Abstract
In this video, we describe an improved transoral endoscopic thyroidectomy technique designed to reduce postoperative oral and mandibular discomfort while effectively lowering surgical complexity. Authors have received and archived patient consent for video recording and publication in advance of video recording of the procedure. The running time of the video is nine minutes and 27 seconds.
Inclusion Criteria:
(1) Benign thyroid tumors (e.g., thyroid cysts, nodular goiter, follicular adenomas) with maximum diameter ≤60 mm; (2) Malignant tumors (follicular carcinoma, papillary carcinoma) with diameter <2 cm, no invasion of trachea, esophagus, recurrent laryngeal nerve, or major vessels, and absence of metastatic lymph node coalescence; (3) Patients with explicit cosmetic requirements.
Background:
The combined transoral and transaxillary endoscopic approach for thyroid surgery represents a minimally invasive technique that offers superior cosmetic outcomes by avoiding visible neck scars.
Surgical Procedure:
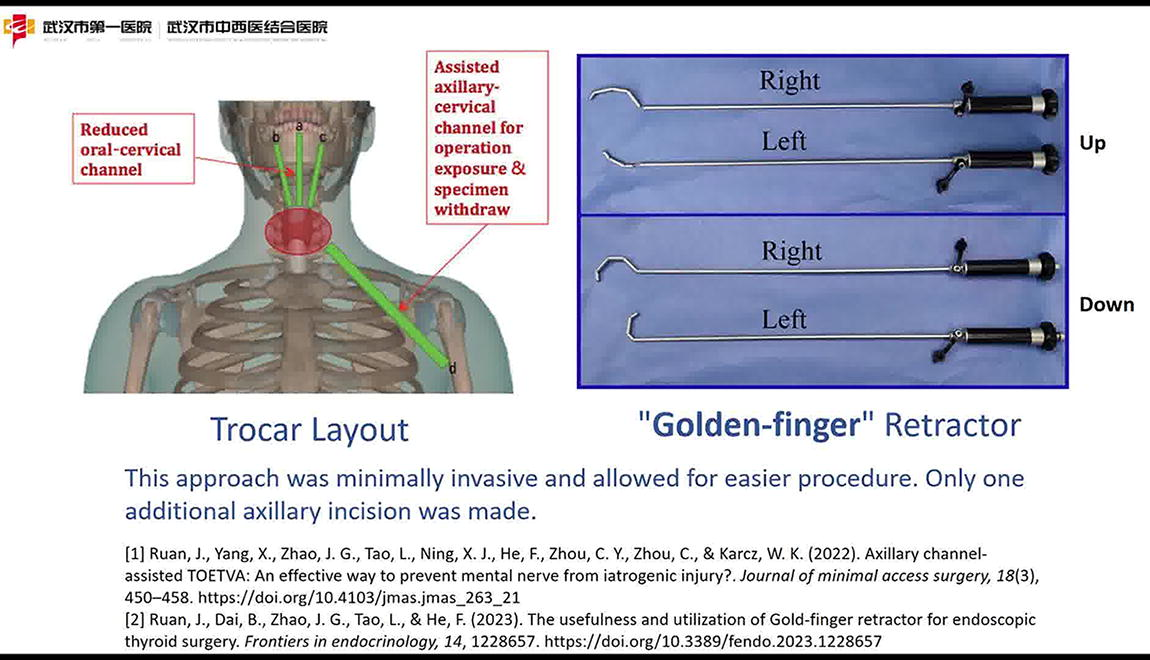
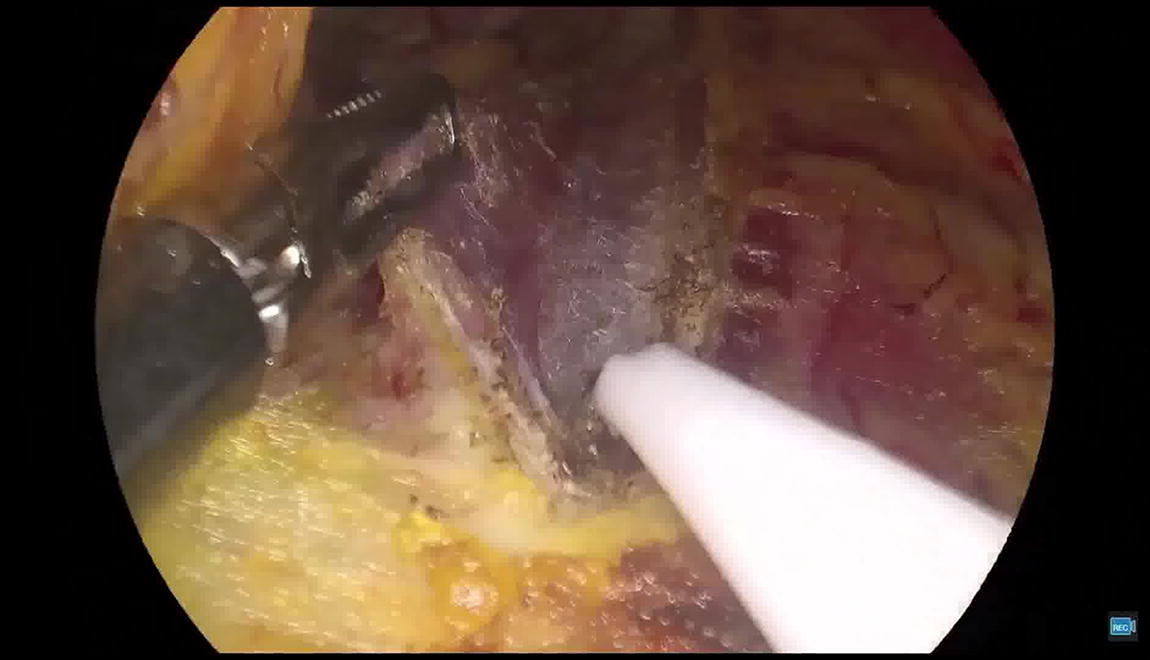
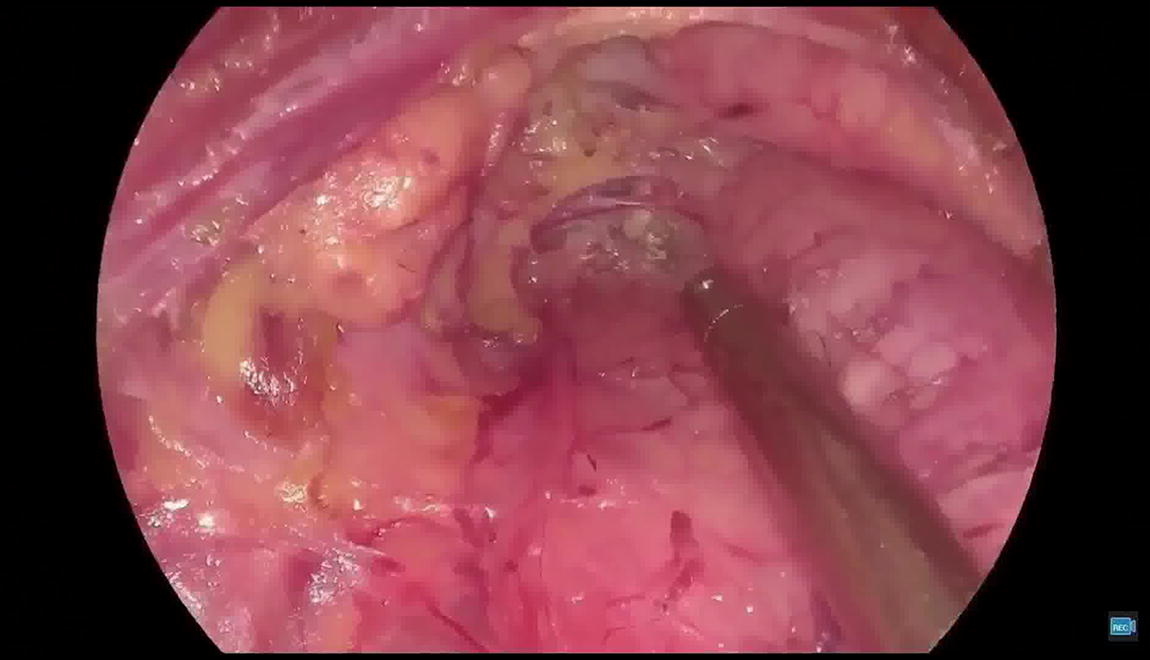
Three 5-mm vertical incisions are created in the oral vestibule, followed by placement of trocars at the midline and bilateral vestibular regions. A subcutaneous working cavity is established from the oral mucosa to the neck using a puncture method. An additional 1-cm incision is made in the left axillary crease to form a subcutaneous tunnel via the same method. Intraoperatively, a “golden finger” retractor is inserted through the tunnel to enhance surgical exposure, maintain tissue tension, and facilitate smoke evacuation.1-2 The remaining steps align with the conventional transoral vestibular approach for thyroid cancer surgery.
Outcome:
The small oral incisions promote rapid healing, lower infection risk, and enhance patient comfort. Utilizing a 5-mm high-definition endoscope instead of a 10-mm scope decreases the likelihood of lip muscle strain and vestibular mucosal tears caused by upward angulation of the larger endoscope during superior pole dissection, thereby reducing lip and chin numbness. The smaller endoscope also minimizes instrument interference during operation. The “Goldfinger” retractor in the assistant’s hand significantly aids the primary surgeon during challenging phases of the operation. Our team has clinically validated the utility of the “Goldfinger” retractor in transoral vestibular thyroidectomy, demonstrating its superior ability to flexibly retract the strap muscles, providing enhanced exposure and tension—particularly beneficial for exposing superior pole tumors. The blunt-tipped, articulated “metal finger” at the front of the Goldfinger retractor facilitates precise placement lateral to the thyroid superior pole. Applying adequate push-pull force effectively separates the strap muscles from the thyroid surface, optimizing exposure of the superior pole and facilitating its dissection and management. The use of the “golden finger” retractor significantly improved surgical exposure and tissue tension during the procedure, enabling smooth and efficient completion of the surgery. The technique effectively reduced intraoperative challenges and enhanced visualization, contributing to a successful outcome with minimal complications.
Conclusion:
The “golden finger” retractor proved to be a valuable tool in the combined transoral and transaxillary endoscopic approach for thyroid surgery. Its ability to optimize exposure and simplify the procedure makes it a promising innovation worthy of adoption and broader clinical application. While adding an axillary auxiliary port increases the total trauma area, it concurrently reduces trauma to the critical oral and maxillofacial region. Given the superior aesthetic importance of the maxillofacial area compared to the axilla, utilizing a minor trauma in a less critical area to mitigate trauma in a highly significant area offers net advantages to the patient. Preoperative assessment for axillary incision placement holds clinical significance, enabling its early utilization for surgical assistance and maximizing the clinical value derived from this incision beyond specimen retrieval alone. 3
The authors gratefully acknowledge Professors Wang Ping and Wang Yong (Department of Thyroid Surgery, Second Affiliated Hospital, Zhejiang University School of Medicine) for their expert mentorship in endoscopic techniques. We extend appreciation to Dr. Zhao Jianguo and colleagues (Department of Thyroid and Breast Surgery, Wuhan First Hospital) for clinical implementation support. Special thanks to Professors Zhao Wenxin and Wang Bo (Fujian Medical University Union Hospital) for procedural guidance and video documentation expertise.
All authors declare that there are no commercial associations that might create a conflict of interest in connection with this video.
Get full access to this article
View all access options for this article.
