Abstract
Fanconi-Bickel syndrome (FBS), also known as glycogen storage disease type XI (GSD XI), is a rare autosomal recessive disorder of carbohydrate metabolism. It is caused by mutations in the gene SLC2A2, which encodes for the facilitative glucose transporter GLUT2. Diagnosis of FBS is often delayed since the clinical features and laboratory markers often overlap with other disorders whose characteristic features include short stature, fasting hypoglycemia, postprandial hyperglycemia, hepatomegaly, hypophosphatemic rickets, and proximal renal tubular dysfunction. In this article, we present a case of FBS and its management in an African American female who initially presented with persistent proximal tubulopathy, hypercalciuria, and metabolic acidosis. We also include a recent literature review on FBS and discuss other metabolic disorders that should be considered in the differential diagnosis.
Keywords
Introduction
Fanconi-Bickel syndrome (FBS; OMIM #227810), also known as glycogen storage disease type XI (GSD XI), was first described in 1949. 1 It is caused by a deficiency in GLUT2 transporters, a member of the facilitative glucose transporter family, secondary to mutations in SLC2A2. GLUT2 transporters are expressed in hepatocytes, pancreatic β cells, basolateral enterocytes, and renal tubular epithelial cells. 2-4 Fanconi-Bickel syndrome is characterized by failure to thrive, chronic diarrhea, fasting hypoglycemia, postprandial hyperglycemia, hepatomegaly, and glucosuria, along with other features of renal tubular dysfunction. Due to the protean nature of the symptoms, the diagnosis of FBS is often missed or delayed. Patients often present with chronic liver and kidney disease as well as significant short stature. Chronic bone disease can occur, and patients can have significant morbidity. In this article, a case of FBS first diagnosed and treated as isolated renal tubular acidosis is presented. However, a comprehensive reevaluation of symptoms led to a late diagnosis of FBS and an adequate therapy promoted good clinical response.
Clinical Presentation
A 5-year-old African American female child was born at 32 weeks of gestational age. Her birth weight was 2.09 kg (88th percentile) and birth height was 43.1 cm (62nd percentile). She was born to a 13-year-old gravida 1, para 1 mother and was later adopted at 2 weeks of age. The newborn screening panel was reported to be normal at birth. During infancy, she underwent numerous hospitalizations for diarrhea and dehydration in the setting of poor weight gain. These episodes were concluded to be intermittent unrelated illnesses, and no further investigations were deemed necessary. At the age of 9 months, a more extensive evaluation was performed due to the presence of severe failure to thrive. The patient was found to have an anion gap metabolic acidosis (total CO2 of 17 mmol/L), elevated hepatic transaminases (aspartate aminotransferase 84 U/L, alanine aminotransferase 58 U/L), and hypercalciuria (urine calcium/creatinine >0.5 mg/mg). However, these findings were attributed to a result of a nonspecific food allergy by her pediatricians. The hypercalciuria was treated briefly with chlorothiazide, but this was abandoned after 2 weeks due to a presumed drug allergy. At her 18-month routine follow-up encounter, the patient was diagnosed with renal tubular acidosis in the setting of poor growth and persistent metabolic acidosis. Bicarbonate therapy was initiated, but poor growth, chronic diarrhea, and developmental delay in cognition, speech, and motor skills persisted.
At the age of 5 years 11 months, she was referred to our pediatric nephrology division for reevaluation on the management of refractory hypercalciuria. On the initial visit, she weighed 12.7 kg (z score −4.17 standard deviations) and her height was 94 cm (z score −4.50 standard deviations). She had frontal bossing, micrognathia, protuberant abdomen with mild hepatomegaly, hypotonia, exaggerated lumbar lordosis, and reduced musculature and subcutaneous fat in the extremities. Her examination was negative for splenomegaly, rachitic rosary, or bowing of the legs.
Review of prior blood work revealed persistently low bicarbonate level (17-18 mmol/L), despite alkali supplementation and mildly elevated hepatic transaminases. Urinalysis was notable for persistent glucosuria (>1000 mg/dL), 1+ ketones, and 1 to 2+ protein. Renal sonography demonstrated medullary nephrocalcinosis. Dual-energy x-ray absorptiometry (DEXA) scan of the total body skeleton revealed a bone mineral density z score of −1.08 after correction for her height. Ophthalmology consultation did not reveal evidence of corneal abnormalities.
Clinical Course
Management of acidosis and hypercalciuria
The initial mineral metabolism profile at 6 years 8 months of age (after having been on 3 months of vitamin D therapy) revealed phosphaturia, hypercalciuria, and a suppressed parathyroid hormone (PTH; Table 1). To prevent bone loss and to enhance growth velocity, we gradually increased the sodium bicarbonate supplementation from 9 to 22 mEq/kg/d, which led to a reduction in the urinary calcium excretion (13 to 4.4 mg/kg/d).
Clinical and Laboratory Findings Over 3 Years.
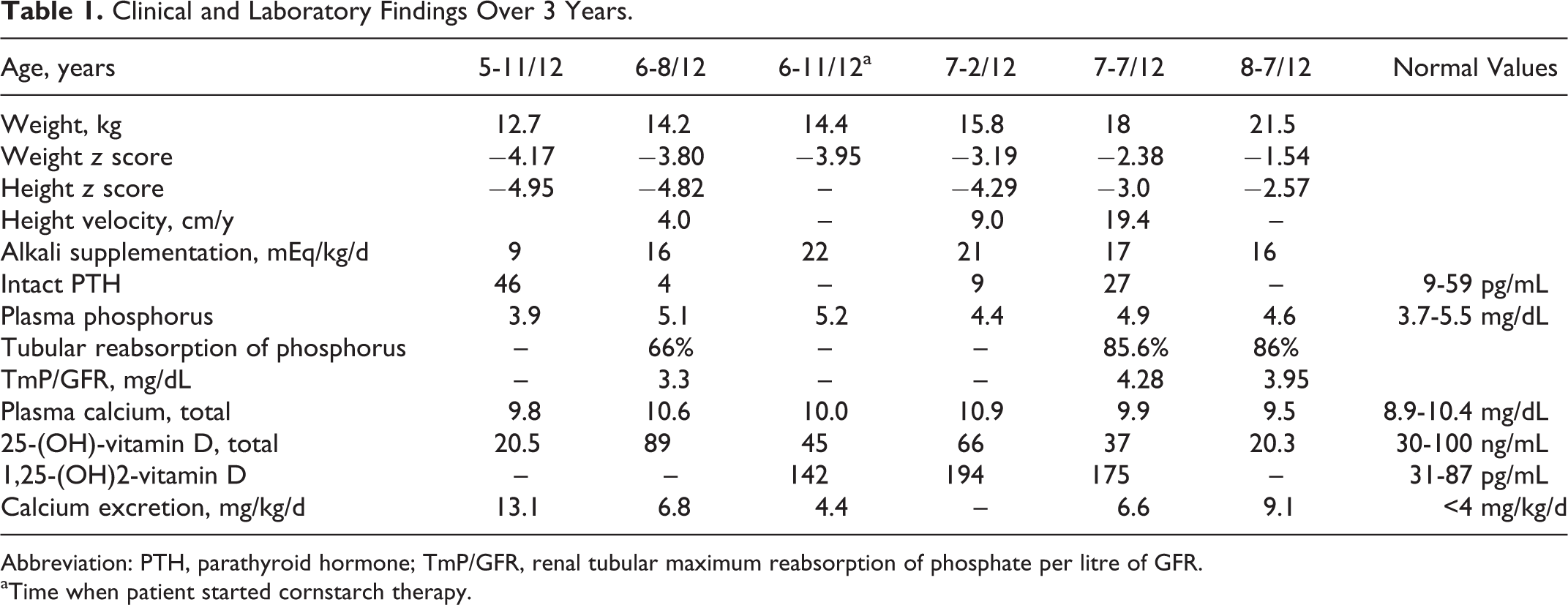
Abbreviation: PTH, parathyroid hormone; TmP/GFR, renal tubular maximum reabsorption of phosphate per litre of GFR.
aTime when patient started cornstarch therapy.
Diagnostic evaluation
Due to the persistence of her symptoms, an evaluation was commenced to investigate for genetic causes of her renal tubular acidosis. The single-nucleotide polymorphism array revealed 631-kb 16p11.2 deletion of uncertain significance, and approximately 20% of the genome had regions of homozygosity, which was concerning for consanguinity. Whole-exome sequencing was recommended but not performed by genetics. While the genetic workup was ongoing, hypoglycemia to 38 mg/dL was documented. When a recurrent pattern of hypoglycemia was appreciated, the patient underwent additional testing in an attempt to identify an underlying metabolic disorder that could unify her clinical (growth restriction, hepatomegaly) and laboratory findings (hypoglycemia, glycosuria, ketonuria, and elevated liver enzymes). Retrospective revision of anamnesis was positive for “maple syrup” urine odor, particularly upon awakening, and sporadic nighttime “shaking” episodes. The patient regularly complained of abdominal discomfort and diarrhea with milk and yogurt products, but she tolerated consumption of fruit.
Formal metabolic monitoring revealed a pattern of fasting hypoglycemia (39 mg/dL), postprandial hyperglycemia ranging between 200 and 400 mg/dL, elevated fasting β-hydroxy-butyrate 3.47 mmol/L (range: 0.04-0.18 mmol/L), normal lactate 15 mg/dL (range: 4-16 mg/dL), and uric acid 1.6 mg/dL. Her baseline lipid profile showed normal total cholesterol (173 mg/dL) and high-density lipoprotein 65 mg/dL, but hypertriglyceridemia was present (261 mg/dL). Urine organic acids were negative for succinylacetone. Mild hepatomegaly and medullary nephrocalcinosis were found on abdominal ultrasound. The constellation of persistent glycosuria, postprandial hyperglycemia, fasting ketotic hypoglycemia, chronic diarrhea, and proximal tubulopathy was most consistent with FBS (GSD XI), and the diagnosis was confirmed genetically when sequencing of the SLC2A2 gene revealed that the patient was homozygous with a deletion of a cysteine residue (position 670 on codon 224) in exon 6.
Therapy for presumed FBS was then started at age 7 years, which involved frequent, small quantities of cornstarch to maintain euglycemia. A high-protein diet was prescribed aimed at normalizing her prealbumin concentration, and intake of sugars (particularly glucose and galactose) was restricted. On follow-up, 3 months later, her energy and cognitive behavioral function (attention span, comprehension skills, following directions, and memory) at home and school had markedly improved. Her speech became more articulate and clear. Catch-up growth in height and weight was also observed. Her liver enzymes normalized on repeat blood work 8 months later. Since her phosphorus levels were always in the normal range, she did not require phosphorus supplementation. Her hypercalciuria decreased to <6 mg/kg/d, but chronic bicarbonate therapy continued to be required.
Literature Review
Genetics
Fanconi-Bickel syndrome is an autosomal recessive disease caused by mutations in SLC2A2, a 30-kb pair gene localized to chromosome 3q26.1-q26.3 that encodes for the GLUT2 glucose transporter. 2 The gene spans 11 exons and 10 introns, 5 and the protein product composed of 524 amino acids is expressed in hepatocytes, pancreatic β cells, enterocytes, renal tubular epithelial cells, and in the central nervous system. 2,3,4 More than 50 SLC2A2 mutations have been found in humans, scattered in all exons. About half of the newly diagnosed cases of FBS are due to novel mutations. Many of these mutations are private and confined to a single family. A genotype–phenotype correlation in FBS has been difficult to establish.
Epidemiology
The true incidence and prevalence of FBS is unknown. About 109 cases from 88 families worldwide were identified from 1949 to 2002. 6 This disorder is predominantly observed in the Middle East, with higher frequency in consanguineous families. SLC2A2 mutations have been described in many ethnic groups in the world. 6,7
Clinical Presentation
Affected patients usually develop signs and symptoms of FBS during infancy, 8 but the diagnosis is often delayed due to the protean nature of the symptoms. 9 Of note, the phenotypic features of FBS are heterogeneous and the constellation of sign and symptoms demonstrate an interfamily and intrafamily variability. 3,10- 12
The initial symptoms include chronic diarrhea, vomiting, growth failure, and hypophosphatemic rickets, which typically manifest between 3 and 10 months. The clinical signs and symptoms of FBS result from the impairment of both glucose and galactose utilization. Carbohydrate malabsorption with glucose or dairy products leads to the diarrhea. Impaired glucose transport out of the hepatocyte results in fasting hypoglycemia, 2 whereas the decreased glucose uptake by the liver and hypoinsulinemia due to the altered sensitivity of pancreatic β cells to glucose contribute to postprandial hyperglycemia. 13 The accumulation of hepatorenal glycogen results in hepatorenomegaly and a protuberant abdomen. Although hypoglycemia is frequently present in patients with FBS, hypoglycemic seizures and mental retardation are rare since the hypoglycemia is associated with prominent ketosis. 8 With glycogen accumulation and failure to export intracellular glucose from the basolateral membrane of the proximal tubule, features of renal Fanconi syndrome manifest (glycosuria, impaired bicarbonate reabsorption, generalized aminoaciduria, phosphaturia, and hypophosphatemia).
Metabolic bone disease in FBS resulting in demineralization with or without rickets is attributable to several causes that are indirectly related to aberrant GLUT2 function. Specifically, ketosis, diarrhea, and proximal renal tubular dysfunction can result in chronic or recurrent acidosis that leads to skeletal buffering and demineralization. Marked phosphaturia will also promote rickets in children with hypophosphatemia. Lastly, calciuria and osteopenia (in the absence of acidosis or exogenous vitamin D) may result from the aberrant regulation of a complex endocrine network that ties calcium and phosphate homeostasis to fibroblast growth factor 23, klotho, PTH, and vitamin D metabolism (CYP27b1 activation and CYP24 inactivation). 14 Accordingly, our patient had suppressed PTH and an elevated 1,25-OH-Vitamin D level, despite normal plasma phosphate concentration, a constellation previously observed in patients with Dent disease.
Diagnosis
There are no specific sonographic or biochemical criteria to diagnose FBS in the prenatal period. Postnatally, some cases may be detected following the evaluation for a positive neonatal screen result for galactosemia. 10,15 All reported patients have had glycosuria at diagnosis; hence, the absence of glycosuria makes the diagnosis of FBS unlikely. 11 Fanconi-Bickel syndrome is confirmed by mutation analysis of the SLC2A2 gene. Biopsies are not routinely performed; a liver biopsy shows increased glycogen deposition in the hepatocytes with steatosis, whereas a renal biopsy shows glycogen deposits in tubular epithelial cells. 9
Differential Diagnosis
Due to phenotypic variability, FBS may be confused with other metabolic conditions (Table 2). Features that FBS shares with GSDs include hepatomegaly, renomegaly, fasting ketotic hypoglycemia, postprandial hyperglycemia, and short stature. 16 Fasting hypoglycemia and postprandial hyperglycemia are also characteristics of GSD 0. 17 Myopathy (skeletal or cardiac) and central nervous system symptoms have not been described in patients with FBS, and their presence should suggest an alternate diagnosis. The presence of renal Fanconi syndrome will distinguish FBS from all GSDs except GSD I. Additional distinguishing features present in GSD I and absent in FBS include hyperuricemia, hyperlactatemia, and the presence of severe hyperlipidemia.
Differential Diagnosis of FBS.

Abbreviations: ARPTH, autosomal recessive proximal tubulopathy and hypercalciuria; FBS, Fanconi-Bickel syndrome.
Clinical findings related to proximal tubulopathy may dominate with concomitant growth restriction and hepatic abnormalities. As with the case presented in this report, FBS can easily be misdiagnosed as renal tubular acidosis. Fanconi-Bickel syndrome may also be confused with other causes of renal Fanconi syndrome (Table 2). Galactosemia and tyrosinemia share these features, yet both should be detected by neonatal screening programs. Rarely, FBS may also screen positive for galactosemia, but further metabolic or genetic evaluation will distinguish these.
The presence of chronic glycosuria, postprandial hyperglycemia, and morning ketosis also leads to misdiagnosis of FBS as type 1 diabetes. Patients can have insulinopenia, but pancreatic antibodies are negative. When diabetes is diagnosed, insulin therapy can result in severe hypoglycemia overnight leading to seizures and possible neurologic damage. The large liver and poor growth can be misattributed as Mauriac syndrome, but a relatively normal hemoglobin A1c can help distinguish these disorders. 18
Pathognomonic physical examination or biochemical findings can help distinguish FBS from several of the metabolic disorders. Congenital cataracts, with or without glaucoma, is found in Lowe syndrome, and acquired anterior ocular abnormalities develop in patients with cystinosis (corneal crystals), galactosemia (cataracts), and Wilson disease (corneal Kayser-Fleischer rings). Distinguishing laboratory findings include elevated white blood cell cysteine levels in cystinosis; urinary succinylacetone in tyrosinemia; and blood and urine copper, as well as blood ceruloplasmin in Wilson disease. Fructosuria will be detected in urine during crises in patients with hereditary fructose intolerance, and galactose will be present in urine from patients with galactosemia after milk feeding. In both, the urinary sugar will yield a high level of urine-reducing substance. Cytochrome c oxidase deficiency is a rare cause of renal Fanconi syndrome that is associated with skeletal muscle and central nervous system abnormalities. Central nervous system abnormalities are also associated with undetected or poorly managed galactosemia and Wilson disease.
Besides proximal tubule dysfunction, Dent disease and Lowe syndrome share many features of dysregulated mineral metabolism with our patient, including nephrocalcinosis, hypercalciuria, and high calcitriol levels. 19 Unlike our patient with FBS, their phenotype is limited to boys and does not include fasting hypoglycemia, ketosis, or postprandial hyperglycemia.
Dent disease (X-linked hypercalciuric nephrolithiasis) refers to a group of X-linked inherited disorders characterized by phenotypic variability in severity of hypercalciuria, proximal tubulopathy, metabolic bone disease, and progression to renal failure. Hypercalciuria, the earliest and cardinal manifestation, is associated with lower than expected levels of PTH and phosphate, while calcitriols are elevated. 19,20 There is also genotypic variability—45% to 60% of cases have genetic mutations in CLCN5, which encodes a voltage-dependent electrogenic chloride/proton exchanger; 15% have OCRL1 mutations, the gene responsible for Lowe syndrome; and in the remaining 25% to 35% of patients, neither CLCN5 nor OCRL1 mutations were detected. 19 Interestingly, proximal renal tubular acidosis is not reported in patients with Dent disease having CLCN5 mutations, whereas it is common in those with mutations in OCRL1. 21
Recently, autosomal recessive proximal tubulopathy with hypercalciuria (ARPTH) was described as a unique disorder that mimics Dent disease but was inherited in an autosomal recessive pattern. 22,23 Further genetic testing revealed a SCL2A2 mutation; hence, ARPTH is now considered an allelic variant of FBS. Prior to genetic testing, our patient also resembled ARPTH. This further highlights the heterogeneity and complexity of clinical and biochemical findings in FBS and the overlap with other metabolic disorders.
Treatment
Currently, dietary modification remains the primary treatment for FBS. Glucose and galactose must be removed from the diet, and small doses of cornstarch administered frequently can stabilize the glucose concentration. Uncooked cornstarch provides a substrate for slow enteric absorption of carbohydrate, thereby prolonging the duration of euglycemia between meals. 24 Although there is no published literature on the use of high-protein diet (2.0-2.5 g/kg/d) in FBS, it is the standard treatment for the other ketotic forms of GSD. Unlike the other ketotic forms of GSD, gluconeogenesis is impaired in FBS, but protein can serve as an alternative energy source for the muscles, which helps to preserve blood glucose concentrations. In our experience, children with FBS often have low prealbumin concentrations, and protein supplementation leads to less gastrointestinal issues, lower postprandial glucose concentrations, and decreased glycogen formation. Protein often is administered 3 to 4 times per day, and dosing is adjusted to normalize the prealbumin concentration. The hypercalciuria can be minimized with the treatment of the underlying disorder and alkali supplementation. While postprandial hyperglycemia can occur, insulin should be avoided unless marked hemoglobin A1c elevation is present.
Prognosis
With early and appropriate treatment, the overall prognosis is very good and survival to adulthood is favorable. Missed or late diagnosis of FBS has been associated with higher rates of death related to liver failure and respiratory distress. 3,10,25 However, even in cases that are diagnosed late, proper dietary intervention should result in the reduction in the liver size and glycogen content 7,9 and avoidance of liver transplantation. 26 Importantly, early diagnosis and proper treatment in young children accelerate growth in height and weight and improve cognitive function. The long-term benefits include successful fertility in affected males and females. 27,28 Unlike the other forms of GSD, hepatic adenoma, malignancies, or cirrhosis has not been reported.
Conclusion
Fanconi-Bickel syndrome should be suspected in children with the supportive history, examination, and laboratory findings, since early diagnosis and treatment are important in improving the quality of life and reducing end-organ damage. The diagnosis can now be confirmed by mutation analysis for the GLUT2 gene. This report demonstrates that appropriate alkali therapy and diet modification including cornstarch supplementation can result in increased growth rates, healing of renal and hepatic injury, and improved activity level and well-being.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the following philanthropic funds managed through the University of Florida Office of Development: Scott miller GSD Program Fund and the GSD Dream Fund. The support was also provided in part by the NIH/NCATS Clinical and Translational Science Award UL1 TR000064 granted to the University of Florida.
