Abstract
The glycogen storage diseases (GSDs) comprise a group of rare inherited disorders of glycogen metabolism. The hepatic glycogenolytic forms of these disorders are typically associated with hypoglycemia and hepatomegaly. For GSD I, secondary metabolic disturbances include fasting hyperlactatemia, hyperuricemia, and hyperlipidemia. Glycogen storage disease III is caused by reduced activity of the debrancher enzyme, GSD VI by phosphorylase, and GSD IX by phosphorylase kinase. It has often been reported that the non-GSD I group of disorders have a benign course. However, myopathy, cardiomyopathy, and cirrhosis have been reported significant clinical morbidities associated with GSD III and IX in particular. There have been a range of reports indicating high-protein diets, high-fat diets, medium chain triglyceride (MCT), modified Atkins diet, and therapeutic ketones as rescuing severe phenotypes of GSD III in particular. The etiology of these severe phenotypes has not been defined. Cases presented in this report indicate potential harm from excessive simple sugar use in GSD IX C. Review of the literature indicates that most interventions have reduced the glycemic load and provide alternate substrates for energy in rescue situations. Prevention of complications is most likely to occur with a mixed balanced low glycemic index diet potentially with relative increases in protein.
Introduction
Glycogen storage diseases (GSDs) are a heterogeneous group of inherited disorders caused by inborn errors of glycogen metabolism. These disorders most commonly affect the muscle and liver where glycogen is the most abundant. 1 For GSD I, secondary metabolic disturbances include fasting hyperlactatemia, hyperuricemia, and hyperlipidemia. Glycogen storage disease III is caused by reduced activity of the debrancher enzyme, GSD VI by phosphorylase, and GSD IX by phosphorylase kinase. The physiology of GSD III, VI, and IX is different to GSD I. 2,3 There is fundamental impairment to gluconeogenesis and mitochondrial beta oxidation in severe forms of GSD I. 4 -7 Fat oxidation is not inhibited in GSD III, VI, and IX, leading to the ability to generate ketones in the presence of hypoglycemia. Glycogen storage disease III, VI, and IX can therefore be referred to as ketogenic GSDs (KGSDs). For the purpose of this article, this group will not include glycogen synthetic disorders including GSD 0 (glycogen synthase deficiency), plasma membrane glucose transport deficits, or lysosomal glycogenoses. It has often been reported that KGSDs have a benign course, but there are significant clinical morbidities associated with some forms of GSD III and IX in particular. 8 -10 This has led to a variety of approaches to management of these conditions without uniform consensus to identify the best dietetic approach to the treatment of these conditions across the world. This article will review the literature and include practical approaches to clinical scenarios the authors have experienced.
Historical Perspective to Treatment
Carl and Gerti Cori identified the Cori ester—glucose-1-phophate in 1936. This directly led to the discovery of the etiology of GSD I, namely glucose-6-phosphatase (G6Pase) deficiency. 11 In 2 of the 10 pathological samples examined at the time in the 1950s, abnormal glycogen structure was shown—one with “longer inner and outer chains than normal glycogen.…resembled amylopectin,” and the other “had very short outer branches… resembling a phosphorylase limit dextrin.” 12 They demonstrated that limit dextrinosis (GSD III) was caused by amylose 1,6 glucosidase (debrancher) deficiency. This enzyme is unusual as it has 2 catalytic sites. Oligo-1,4-1,4-glucan transferase transfers 3 of the 4 glucose molecules from the branch chain to an adjacent linear chain, whereas amylo-1,6-glucosidase facilitates 1,6-glycosidic cleavage of the remaining glucose residue.
Henri-Géry Hers in the 1960s discovered the enzymatic bases of 2 more GSDs namely GSD II (Pompe disease) and GSD VI (hepatic phosphorylase deficiency), which was named after him. 13,14 Despite the phosphorylase kinase (PhK) being discovered in the 1950s, its relation to disease was only identified in the late 1960s. Phosphorylase kinase is a heterotetramer (α, β, γ, δ)4, and each subunit has different isoforms. 2,15 The catalytic site is located on the γ subunit, whereas the other subunits have regulatory function. 16,17 Several genes, with differing modes of inheritance and tissue expression, have been identified encoding for these subunits, and hence, GSD type IX has significant phenotypic variability. 2,18,19
In parallel with the discovery of these disorders, a series of interesting physiological studies were performed by John Fernandes in the 1960s and 1970s to try and delineate optimal management for the GSDs. 4,20 The short-term physiological studies in a range of disorders tested hypotheses around the processing of simple sugars, disaccharides, fats, and proteins in small numbers of patients. Extrapolation from these studies are summarized below in relation to KGSD.
Fructose and Galactose Restriction
Two patients with GSD VI are studied in the paper of Fernandes and van de Kamer of 1965 using glucose, fructose, and galactose. 21 Although the argument is made that neither sugar is gluconeogenic in GSD I, they are noted to synthesize glucose in these 2 patients with GSD VI. In a subsequent article in 1968, 5 with patients with GSD III were studied with fructose, glucose, galactose, wheat starch, and various proteins. 22 After the glucose was administered, there was suppression of fasting ketosis but a postprandial lactate rise. With the other simple sugars, a similar response was seen, although lactate elevations seemed higher with galactose. The authors conclude that “fructose and galactose are equivalent to glucose, but starch is more preferable because its digestion and absorption is more gradual.”
High-Protein Diet
A high-protein diet in GSD has been mentioned in the literature since 1945 in 1 case that had KGSD. 23 At this stage, the precise diagnosis was unknown but in retrospect appears most likely to have been GSD III. Bridge and Holt demonstrated increased nitrogen turnover and addressed this by given beef and bread late at night, which improved energy levels and dyspnea. This appeared to be standard of care as indicated by the papers of van Crefeld. 24 In the 1980s, Slonim and colleagues thoroughly investigated this line of enquiry, demonstrating decreased levels of plasma alanine in the postabsorptive state, relative to controls and patients with GSD I. 25,26 They developed the hypothesis that this gluconeogenic precursor had a pivotal role to play in a gluconeogenesis, particularly after a protein load. The group subsequently reported improvement in growth when energy from protein increased from about 10% to 13% of total energy to 20% to 25% commensurate with an equivalent reduction in carbohydrate. 27 There have been case reports indicating rescue of cardiomyopathy using a high-protein diet. Because these cases were adults, detailed dietary data are not available in the reports about childhood management. The article by Sentner et al describes the therapeutic diet providing 37% from protein, 61% from carbohydrate, and 2% from fat. 28 The article from Dagli et al indicates an increase in protein from 20% to 30% of total energy. 28 Both report improvement in cardiomyopathy.
High-Fat/Ketones-Based Diet
There are detailed dietary data on siblings that have aggressive cardiomyopathy with GSD III, reported by Valayannopoulos et al. Infantile cardiomyopathy is rare in GSD III.
29
Nonetheless, the authors postulate that because the children had high glucose intake, there was insufficient ketone body production due to insulin-mediated inhibition of lipolysis. They consequently demonstrate that treatment with
Case Report—Glucose Toxicity in GSD IX?
It is difficult to reach a sensible decision on appropriate management if different reports indicate good outcomes with each of a high carbohydrate, fat, and protein diet for KGSD. 7 It is probably the case that there is no single best diet. We will attempt to discuss this in the context of the case study below whereby the intervention implemented led to deterioration in liver function of a child with GSD IX type C.
The older child presented with hepatomegaly and liver dysfunction (aspartate transaminase [AST]: 1006 [10-50] IU/L, alanine transaminase [ALT]: 583 [10-50] IU/L, γ-glutamyl transferase [GGT]: 262 [3-26] IU/L, creatine kinase: 59 [15-180] U/L) with normal synthetic function and short stature at the age of 5 years. Liver biopsy demonstrated portal–portal bridging fibrosis. Positive Periodic acid-Schiff staining was demonstrated with vacuolation after diastase digestion. No prior episodes of hypoglycemia had been documented, but a routine supervised fast demonstrated hypoglycemia and ketosis at baseline (after a 10-hour fast). On the basis of this, he was started on cornstarch to be given prior to bed and at 02:00. Daytime nutrition was not altered. GSD IXC was confirmed by massively parallel sequencing, which identified a homozygous variant (c.451C>T) in the PHKG2 gene. Following initial dietary modification and improved compliance with cornstarch therapy, liver function tests (LFTs) began to improve, and the family noticed an increase in his energy levels. Regular monitoring of LFTs (AST reduced to 383 IU/L) and abdominal ultrasounds has been stable. His diet has improved in both variety and quality, with a current macronutrient distribution of 17% energy from protein (3.1 g/kg/d), 31% from fat, and 52% from carbohydrate.
Sibling 2 was 2 years old when his older brother was diagnosed with GSD. He had been noted to have short stature and deranged LFTs by his local pediatrician. His weight was on the seventh percentile and his height well below the first percentile (Z-score = 3.0). Routine bloods had revealed an elevated ALT (1235U/L) and GGT (197). His cholesterol was 5.5 mmol/L and triglycerides of 3.7 mmol/L. Preprandial ketones were elevated at 3.33 mmol/L when the glucose was 2.0 mmol/L. In order to try to aid growth, sibling 2 was started on a high-energy formula (PediaSure; Abbott Laboratories, Illinois), with carbohydrate constituents predominantly being maltodextrin and sucrose, during the day and twice nightly cornstarch. Daily protein intake was 3.9 g protein/kg and macronutrient distribution 15% from protein, fat 31%, and carbohydrate 45% with 100% reference energy intake. He was subsequently reviewed 2 months after this and, although his activity levels were substantially improved, significant deterioration in his LFTs was noted despite adherence to his dietary plan (Figure 1A). Serology for viral hepatitis infections were negative. We hypothesized that excessive glucose and oligosaccharide delivery could have contributed to this pattern, particularly noting the postprandial lactate elevation. The high-energy formula was substituted for cows’ milk and uncooked corn flour. Review 2 months later demonstrated that his liver function had improved dramatically, and this has been sustained. The macronutrient distribution 2 months after this intervention showed 16% energy from protein (4.1 g/kg/d), 30% from fat, and 49% from carbohydrate with 100% reference energy intake. This report indicates that there is an improvement in liver function only by changing the quality of the carbohydrate (ie, lower glycemic index [GI]) rather than proportion.
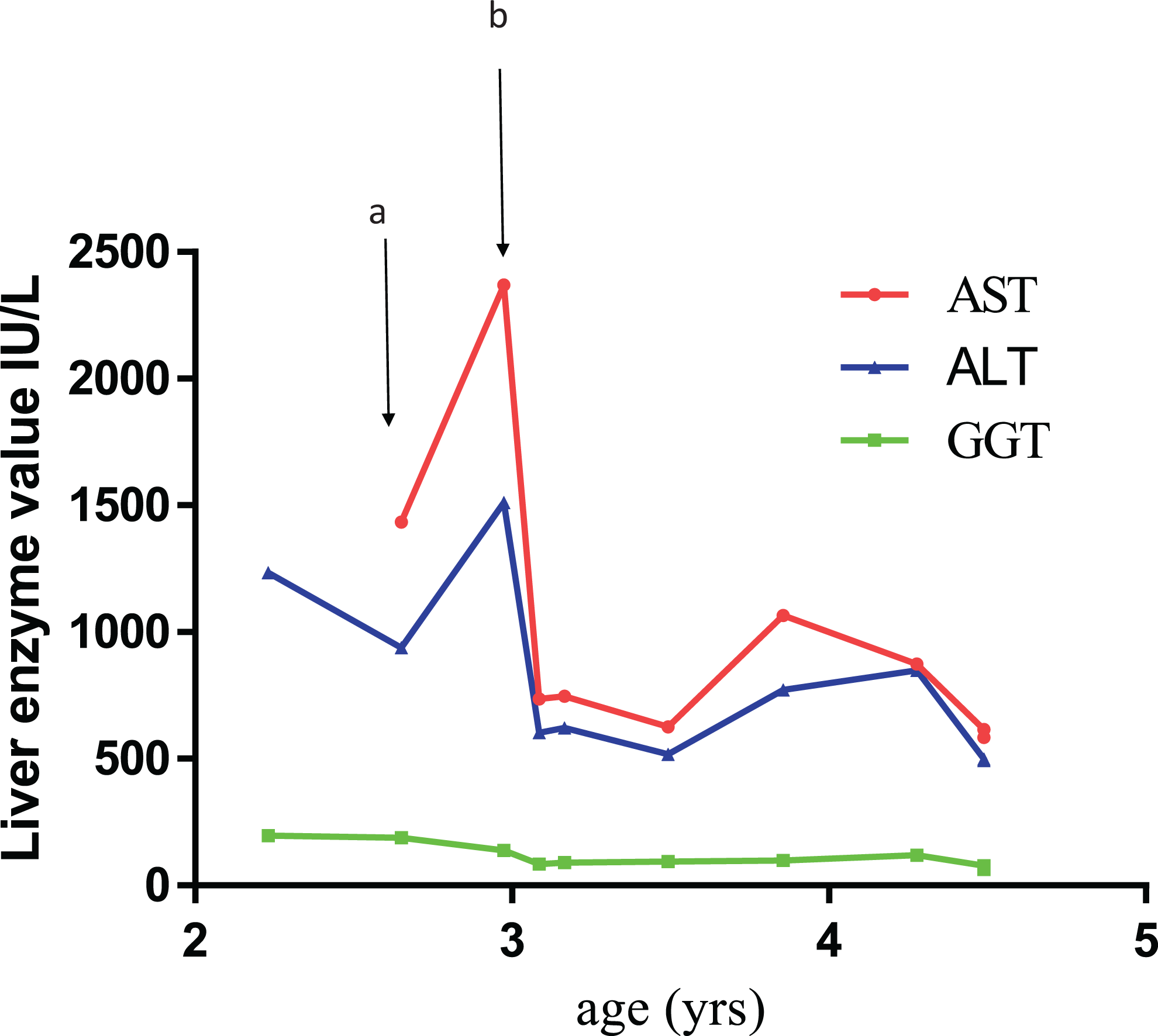
Changes in sibling 2. A, Use of regular high-energy formula during day and night (5 bolus feeds) leading to elevation in liver function tests. B, Substitution of high-energy feed for isocaloric low-fat cows’ milk and uncooked cornstarch leading to the improvement in liver function tests.
Macronutrient Composition of Diet—What Should be Done?
The theme that emerges from all the case reports, mainly in GSD III, but our case with GSD IX C is that problems seem to occur when too much carbohydrate is given. In the reported successful diets, sometimes carbohydrate is reduced and substituted for another macronutrient. In this situation, carbohydrate is displaced from the diet. In other circumstances, the effect of carbohydrate is “diluted” by another macronutrient. This in essence would alter the glycemic load of the administered carbohydrate. Our cases indicate that not only should the macronutrient be considered but the quality. This is not a new concept and specifically was commented on by John Fernandes in his studies in the 1960s in his paper about simple sugars in GSD III.
What was not clear in the 1960s was the extent to which long-term complications could occur with excessive simple sugar use. The variety of case reports referenced indicate rescue by alternative macronutrients enhancing ketogenesis or gluconeogenesis. Using more protein and fat as well as other nutrients in the diet will itself alter the glycemic load of any given meal. 32 Therefore, these interventions are likely to lead to less glucose and lactate excursions in such patients, with the caveat that sufficient carbohydrate remains in the diet to prevent hypoglycemia too. However, the question that needs to be asked is what is the etiology of the worrying complications in the first place?
The body’s metabolic response to glucose loads and high GI foods has been studied in other settings. The GI index is a system for classifying carbohydrate-containing foods according to the glycemic response. 33 Consumption of high-GI foods has been shown to be related to increased risk of cardiovascular disease and type II diabetes. 34 -36 Higher protein intake significantly reduces the relative glycemic response, area under the curve, and peak rise of glucose during a 50-g carbohydrate load, 36 which may partly explain the benefits of increased protein in GSD. Slonim et al have provided additional data to suggest that protein provides a gluconeogenic substrate, and Valayannopoulos et al indicate that ketone body production is also impaired with excessive glucose. 29 Whether these approaches are any better than simply lowering peak glucose excursions and insulin release using complex carbohydrates such as Glycosade (Vitaflo Int Ltd, Liverpool, United Kingdom) or Brazilian cassava starch (sweet polvilho) are yet to be seen. 37 -39
In KGSD, the metabolic responses to hypo- and hyperglycemia are altered. The reciprocal physiological responses of glycogen synthase to hyperglycemia and glycogen phosphorylase kinase to hypoglycemia are indicated in Figure 2. The enzyme activation cascade following glucagon stimulation of the liver usually results in the breakdown of glycogen. Counterregulation is incomplete in patients with KGSD. In response to hypoglycemia, protein kinase A will inactivate glycogen synthase but cannot activate phosphorylase kinase in GSD 9, and consequently, glycogenolysis is impaired. In GSD III and GSD VI, there is proximal and distal inhibition of this pathway, respectively. Rapidly delivering large amounts of glucose immediately after hypoglycemia is unlikely immediately to lead to glycogen synthesis due to sustained inactivation of glycogen synthase by both protein kinase A and glycogen synthase kinase, due to reduced levels of the intermediate protein phosphatase 1 (PP1). 41,42 Free administered glucose is metabolized by alternative pathways such as conversion to lactate. This is one possible explanation for the elevated postprandial lactate levels seen in KGSD. If this occurs every time, there is a significant rise in blood glucose level (after hypoglycemia), chronically elevated lactate may ensue, and this may lead to end organ damage. Over and above this, there will be sustained insulin release. 29 Despite this being a possible mechanism, we can find no other reports linking hyperglycemia or hyperlactatemia to hepatocellular damage in GSD. Elevated lactate levels have been documented in other cases of PHKG2 and GSD III and occasionally in PHKA2 deficiency. 8,43 -45 Physiological data in animal models supporting the hypothesis indicate that PhK and the intermediate PP1 have a crucial role in glucose homeostasis, particularly when there are rapid changes in ambient glucose concentrations. 41,42
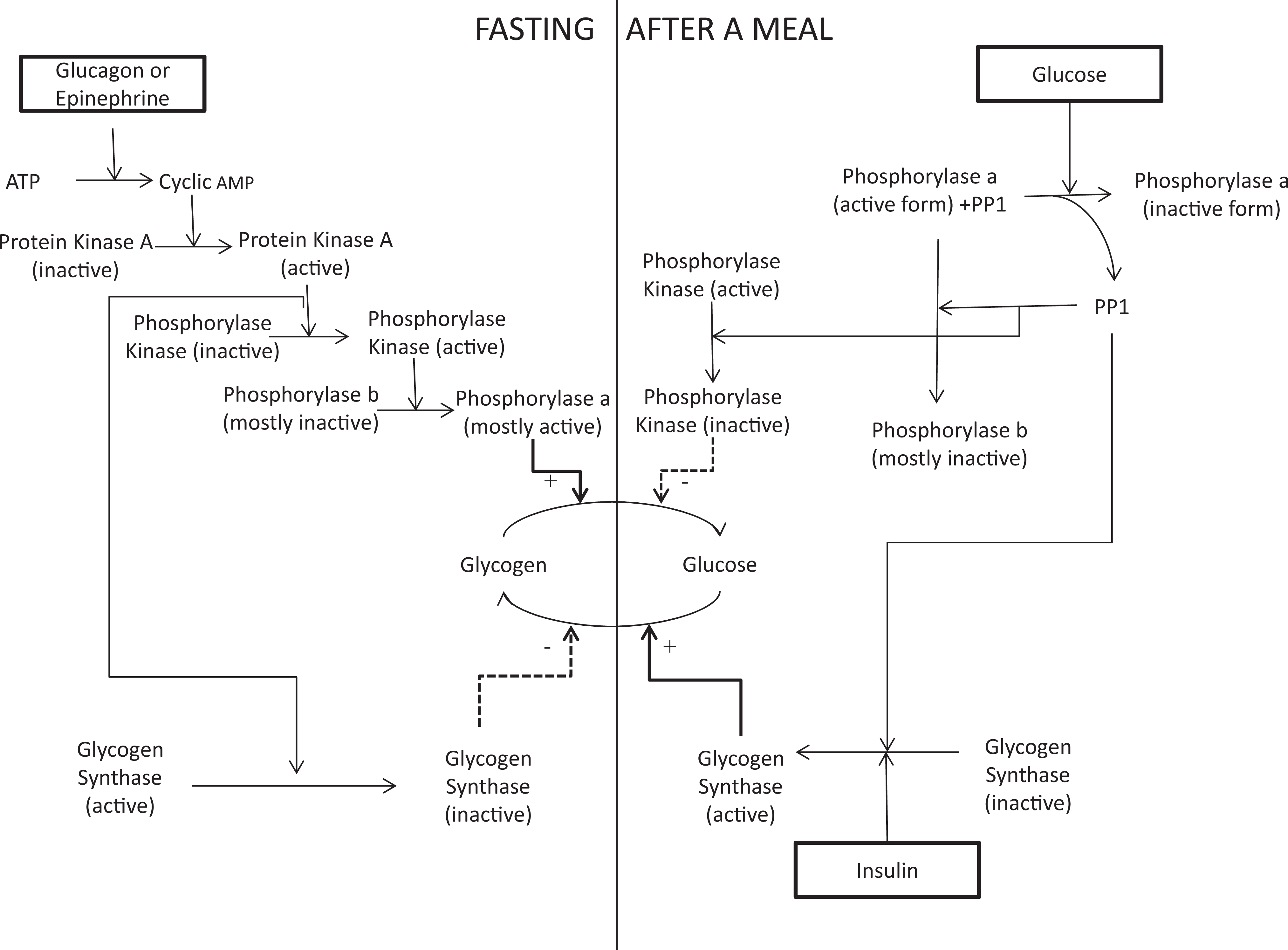
A diagram demonstrating the reciprocal activation and deactivation of glycogen synthase and glycogen phosphorylase via the intermediates protein kinase and protein phosphatase 1. Adapted from Berg et al. 40
There have also been some studies linking hyperglycemia to liver damage in other clinical settings, although again the mechanisms behind this are poorly defined. Good glycemic control has been found to be associated with prolonged survival in hepatitis B patients with cirrhosis, and high serum glucose has been associated with increased liver fibrosis in hepatitis C patients. 46 Adult patients with existing liver disease have also been noted to have exaggerated glucose and insulin profiles following oral glucose loads. 47
Cardiomyopathy is a well-recognized feature of diabetes and is seen in infants of diabetic mothers. The pathophysiology of this complication is not completely understood but starts with dysfunction in glucose and insulin homeostasis. As described, there is also dysregulation of glucose, insulin, and counterregulatory homeostasis in KGSD, which could lead to similar pathological consequences. As a result of altered glucose and insulin homeostasis, in diabetes, there is evidence of mitochondrial dysfunction, decreased lipolysis, microangiopathy, and increased collagen deposition with increased cross-linking. These all remain as plausible mechanisms for cardiomyopathy and end organ damage in KGSD. 48,49
Summary
There is consensus that excessive simple sugars can cause harm as indicated in the paper by Derks and Smit and The American College of Medical Genetics Practice guidelines which states, “Simple sugars are discouraged in favour of a diet higher in complex carbohydrates and protein.” 3,7 Families usually understand simple instructions about hypoglycemia treatment. This type of management is well reported and has been central to GSD literature for decades. 6 However, the shift needs to occur from hypoglycemia treatment for prevention by the use of complex carbohydrates with a mixed diet, possibly with relative increases in protein or fat. There are physiological data to indicate that protein does produce gluconeogenic substrates and several reports of rescue by increasing protein use. The amount of increase has not been defined nor has the type of protein. There are insufficient studies to indicate if any individual amino acid has particular benefit. MCT-based diet, the modified Atkins diet, and the administration of therapeutic ketones have also been used in rescue situations. In some of these reports, the premorbid dietary intake is poorly defined.
A prudent approach for KGSD would be to utilize a low GI-based diet, reducing simple sugar use as much as possible. High biological value protein intake of the order of 30% of standard total energy requirements would seem a pragmatic goal for most families to achieve. Further increase in protein, use of fat, MCT with concomitant carbohydrate reduction, or therapeutic ketones could be utilized if further comorbidities are identified.
Footnotes
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Dr Bhattacharya has received funds for clinical trials sponsored by Glcologic Ltd and Vitaflo Ltd prior to 2008.
Funding
The author(s) disclosed receipt of the following financial support for the research and/or authorship of this article: Dr Bhattacharya has performed consultancy work for Vitaflo Ltd in 2008.
