Abstract
Beta-ketothiolase deficiency is an inherited disorder of ketone body metabolism and isoleucine catabolism. It typically manifests as recurrent ketoacidotic episodes with characteristic abnormalities in the urinary organic acid profile. However, several challenges in the diagnosis of beta-ketothiolase deficiency have been encountered: atypical presentations have been reported and some other disorders, such as succinyl-CoA:3-oxoacid CoA transferase and 2-methyl-3-hydroxybutyryl-CoA dehydrogenase deficiencies, can mimic the clinical and/or biochemical signs of beta-ketothiolase deficiency. A final diagnosis of beta-ketothiolase deficiency requires an enzymatic assay and/or a molecular analysis, but some caveats must be considered. Despite the reported missed cases, screening programs have successfully identified an increasing number of patients with beta-ketothiolase deficiency. Early diagnosis and management of beta-ketothiolase deficiency will enable prevention of its serious acute and chronic complications and ultimately improve the prognosis.
Introduction
Beta-ketothiolase deficiency (Online Mendelian Inheritance in Man [OMIM] 203750) is an autosomal recessive disease caused by a defect of mitochondrial acetoacetyl-CoA thiolase (T2). This disorder affects ketone body metabolism and isoleucine catabolism. Beta-ketothiolase deficiency is also known by other names including T2 deficiency, mitochondrial acetoacetyl-CoA thiolase deficiency, 3-oxothiolase deficiency, 3-ketothiolase deficiency, and 2-methyl-3-hydroxybutyric acidemia. 1 -3 In this review, beta-ketothiolase is abbreviated as T2.
T2 and 3-hydroxy-3-methylglutaryl-CoA (HMG-CoA) lyase (OMIM 246450) deficiencies are the most common disorders of ketone body metabolism. 2 Since the first description of T2 deficiency in 1971, 4 more than 100 cases have been reported worldwide, with no ethnic predisposition. 1 T2 deficiency is estimated to be a very rare disease with an incidence of less than 1 per 1 million newborns. 5
In this review, we provide an overview on T2 deficiency, illustrate challenges in diagnosis, and clarify ways to overcome these challenges; a diagnostic flow chart for T2 deficiency is provided.
Biochemistry
The ketone bodies acetoacetate (AcAc) and 3-hydroxybutyrate (3HB) are important substitutes for glucose. They are produced in the liver and can be utilized as energy sources by most tissues except the liver itself. They are especially important for the brain as the only substitutes for glucose. 1,2
As shown in Figure 1, ketone body metabolism starts in the hepatocytes with β-oxidation of free fatty acids (FFA), supplied from adipose tissues, to produce acetyl-CoA and acetoacetyl-CoA (AA-CoA). T2 can convert acetyl-CoA to AA-CoA and vice versa. Mitochondrial HMG-CoA synthase condenses acetyl-CoA and AA-CoA to form HMG-CoA. HMG-CoA is converted by HMG-CoA lyase to AcAc, which is partially reduced to 3HB by 3-hydroxybutyrate dehydrogenase. AcAc and 3HB are transferred to extrahepatic tissues via the bloodstream, where 3HB is converted back to AcAc. Succinyl-CoA:3-oxoacid CoA transferase (SCOT) activates AcAc to AcAc-CoA, which is then cleaved by T2 into acetyl-CoA. 1,2 Hence, T2 is important in both ketogenesis in the liver and ketolysis in the extrahepatic tissues. Another thiolase, mitochondrial 3-ketoacyl-CoA thiolase, can compensate for T2 deficiency in ketogenesis but to a lesser extent in ketolysis. As a result, deficiency of T2 leads to ketosis. 1 -3 Monocarboxylate transporter 1 (MCT1), a transmembrane transporter, has been shown to transport monocarboxylates, including ketone bodies, into extrahepatic tissues. This is essential for ketolysis, particularly during periods of catabolic stress. 6
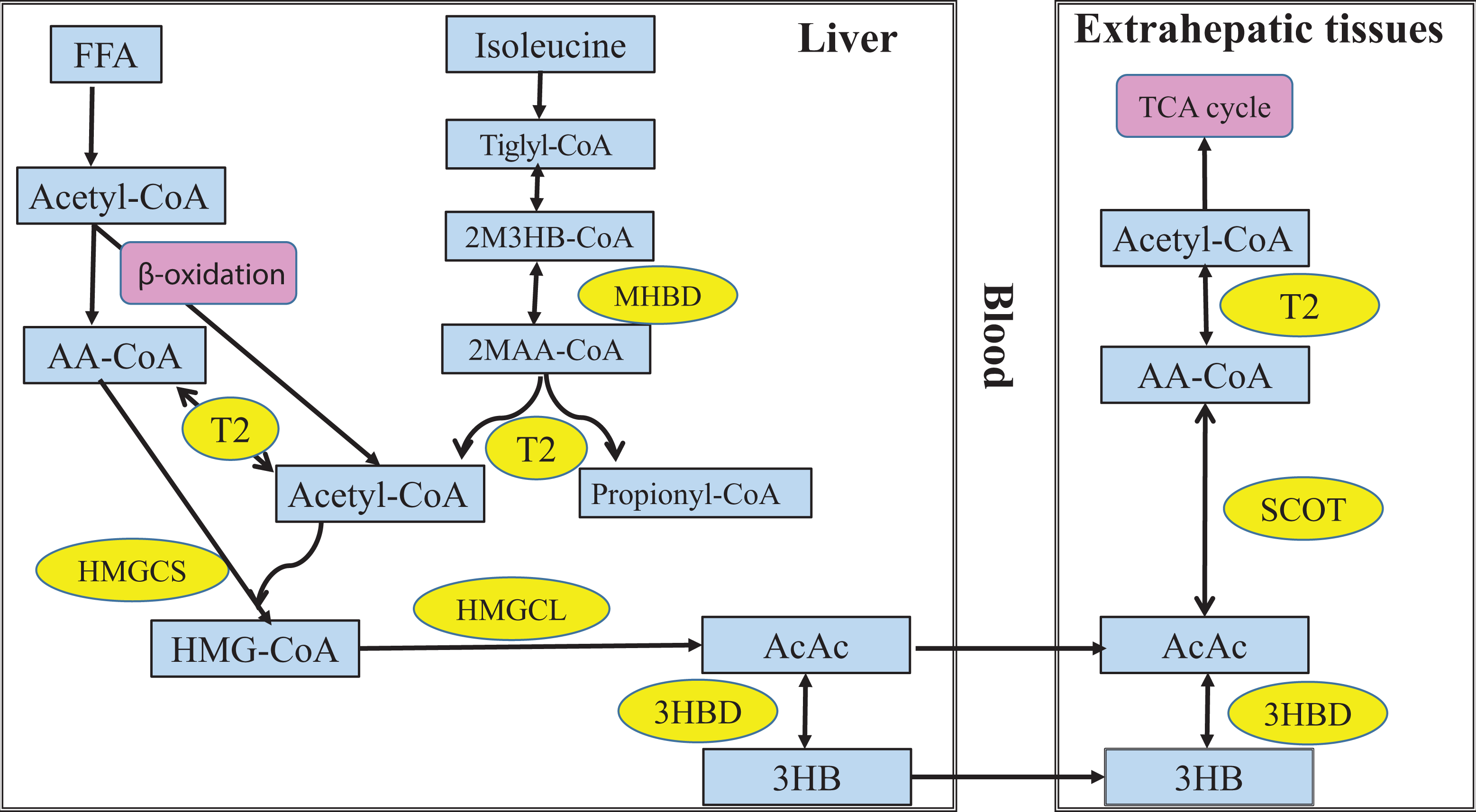
Summary of ketone body metabolism and isoleucine catabolism. 2M3HB indicates 2-methyl-3-hydroxybutyryl; 2MAA, 2-methylacetoacetyl; 3HB, 3-hydroxybutyrate; 3HBD, 3-hydroxybutyrate dehydrogenase; AA, acetoacetyl; AcAc, acetoacetate; CoA, coenzyme A; FFA, free fatty acids; HMG-CoA, 3-hydroxy-3-methylglutaryl-CoA; HMGCL, HMG-CoA lyase; HMGCS, mitochondrial HMG-CoA synthase; MHBD, 2-methyl-3-hydroxybutyryl-CoA dehydrogenase; SCOT, succinyl-CoA:3-oxoacid CoA transferase; T2, mitochondrial acetoacetyl-CoA thiolase; TCA, tricarboxylic acid.
In isoleucine catabolism, T2 is responsible for thiolysis of 2-methylacetoacetyl-CoA (2MAA-CoA) to acetyl-CoA and propionyl-CoA. The 2 upstream reactions, conversion of tiglyl-CoA to 2-methyl-3-hydroxybutyryl-CoA (2M3HB-CoA) and conversion of 2M3HB-CoA to 2MAA-CoA, are reversible; the latter reaction is catalyzed by 2-methyl-3-hydroxybutyryl-CoA dehydrogenase (MHBD). Consequently, T2 deficiency leads to accumulation of 2MAA-CoA, 2M3HB-CoA, and tiglyl-CoA, whereas MHBD deficiency results in accumulation of only the latter 2 metabolites. 1 -3
Clinical Presentation: Diagnostic Challenges
Clinical Presentation
Typical presentation
T2 deficiency classically manifests between 6 and 18 months of age with recurrent ketoacidotic attacks; patients are generally asymptomatic between attacks. Ketoacidotic episodes are often triggered by fasting, fever, infections, or other ketogenic stresses. Coma, convulsions, and even death are possible acute complications, whereas neurodevelopmental impairments are possible long-term complications, mainly as sequelae of severe metabolic decompensations. The severity of the disease varies among cases, but the overall prognosis is usually good. 1,3,7,8
Atypical presentation
Some patients with T2 deficiency having atypical presentation exhibit signs and symptoms at an earlier age, even in the neonatal period, 1 whereas others experience their first attack at an older age. 8 Furthermore, some patients present with neurological symptoms before the onset of ketoacidotic attacks. 9 In contrast, some asymptomatic patients with T2 deficiency have been identified by screening, either because of the existence of an affected family member or as a result of newborn screening (NBS) programs. 10 -14
Diagnostic Challenges
Metabolic disorders should be suspected in ketoacidotic patients. Therefore, critical samples (blood, serum, and urine) should be collected, and routine laboratory tests should be performed before treatment is started 3 ; however, unwary pediatricians may not do so. Symptomatic management of dehydration, acidosis, and hypoglycemia (if present) may lead to improvement in the condition. The patient may then be discharged without receiving a final diagnosis. 15 There are many examples in the literature of failure to diagnose patients with T2 deficiency during their first presentations. Such patients received attention only when they had a second episode or when there was a similar presentation in another family member. 16 -18
A second possibility is that the patient will be seen by a consultant who will order many metabolic investigations (if applicable). Such investigations may lead to the diagnosis of a metabolic disorder, but T2 deficiency might be missed (discussed later). 19 Conversely, the patient may die during the acute attack. An important finding in many cases of T2 deficiency is a positive family history of unexplained sibling deaths. 20 -23 The siblings might have had undiagnosed T2 deficiency as well. 3
The following are some possible solutions for the aforementioned clinical challenges: Education of health-care staff, especially those working in emergency wards, to improve their knowledge of T2 deficiency, ketone body disorders, and metabolic disorders in general, and provision of diagnostic guidelines that identify the circumstances in which ketone body disorders should be suspected and what should then be done.
1,3
T2 deficiency should be considered in the following situations: (a) infants and children with an acute attack of metabolic acidosis following prolonged fasting, acute gastroenteritis, respiratory tract infections, or other febrile states and (b) patients with severe ketosis exceeding predicted values in the context of the clinical circumstances (discussed later); and (c) sick neonates with metabolic acidosis.
1
Establishment of 1 or 2 metabolic centers in countries with a highly consanguineous population, where the incidence of genetic and metabolic diseases, including T2 deficiency, is expected to be high.
24,25
Investigations: Diagnostic Challenges
Investigations
Routine laboratory investigations
During ketoacidotic attacks, a blood total ketone body (TKB) concentration >7 mmol/L is the major finding. Blood sugar is typically normal, but hypoglycemia or hyperglycemia has been reported. 3 Blood ammonia is usually normal, but it may be slightly elevated in some cases. 1,3
Urinary organic acid and blood acylcarnitine profiles
T2 deficiency is usually suspected during acute ketoacidotic attacks when there is increased urinary excretion of 2-methylacetoacetate (2MAA), 2-methyl-3-hydroxybutyrate (2M3HB), and tiglylglycine (TIG). Blood acylcarnitine analysis usually reveals increased tiglylcarnitine (C5:1) and 2-methyl-3-hydroxybutyryl-carnitine. 1
Diagnostic Challenges
When ketosis is associated with hypoglycemia, several disorders are considered, including ketotic hypoglycemia, endocrinal disorders (eg, Addison disease), and metabolic disorders of glucose and glycogen metabolism (eg, glycogen synthase deficiency). 3 The severity of ketoacidosis in T2 deficiency may distinguish this disorder from other causes of ketotic hypoglycemia (Figure 2). 2 The highest reported plasma glucose level in patients with T2 deficiency is 14.1 mmol/L. 15 Ketoacidosis with hyperglycemia, mimicking diabetic ketoacidosis, has been reported in some organic acidemias, although diabetic ketoacidosis is usually associated with much higher plasma glucose levels than ketoacidosis caused by organic acidemias. In such cases, glycated hemoglobin or glycoalbumin levels may help distinguish them (Figure 2). 26 When ketoacidosis is associated with hyperammonemia, organic acidemias are suspected. Such suspicion can be excluded by urinary organic acid analysis. 1,3
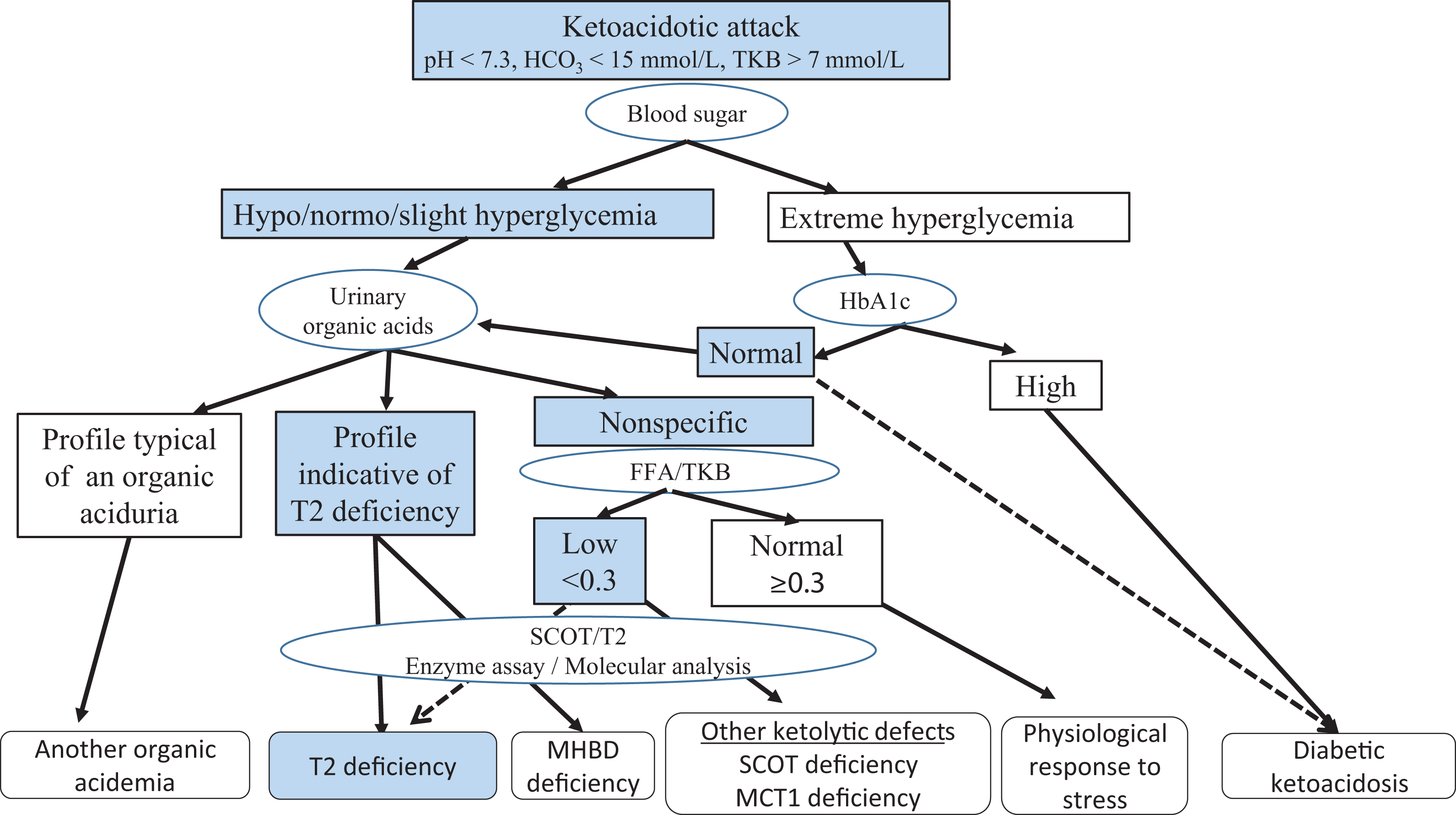
Diagnostic flow chart for beta-ketothiolase (T2) deficiency. An FFA/TKB cutoff of 0.3 is not an absolute value. Fasting for too long may decrease the ratio, and glucose infusion reduces FFA faster than TKB, also decreasing the ratio. Dotted lines indicate rare but possible consequences. Extreme hyperglycemia with elevated HbA1c is usually diagnosed as diabetic ketoacidosis; however, ketoacidosis mimicking diabetic ketoacidosis has been reported in some organic acidemias. Hence, although HbA1c is a good marker for diabetic ketoacidosis, normal HbA1c levels cannot exclude diabetic ketoacidosis conclusively (indicated by a dotted line). If the urinary organic acid profile is nonspecific during ketoacidosis, T2 and SCOT should be analyzed by enzyme assay or gene analysis, since patients with T2 deficiency could have a nonspecific urinary organic acid profile (indicated by a dotted line). FFA/TKB indicates free fatty acids/total ketone body; HbA1c, glycated hemoglobin; MCT1, monocarboxylate transporter 1; MHBD, 2-methyl-3-hydroxybutyryl-CoA dehydrogenase; SCOT, succinyl-CoA:3-oxoacid CoA transferase; T2, mitochondrial acetoacetyl-CoA thiolase.
Individuals with SCOT deficiency (OMIM 245050) may present with ketoacidotic attacks mimicking T2 deficiency. 3 SCOT deficiency has 3 important characteristics: (1) neonatal onset in 50% of cases, (2) permanent ketosis, even postprandially, and (3) lack of a characteristic urinary organic acid profile. 1,2 Given that (1) T2 deficiency may manifest in the neonatal period, 1,2 (2) permanent ketosis is not a feature in all cases of SCOT deficiency, 2 and (3) some cases of T2 deficiency show only subtle biochemical abnormalities in the urinary organic acid profile, 1,19 the 2 conditions may be very similar at both the clinical and biochemical levels. Actually, both conditions should be suspected and investigated in cases of unexplained and/or recurrent ketoacidotic attacks. The conditions can be differentiated by enzymatic assay and/or molecular analysis. 1 -3
MCT1 deficiency (OMIM 616095) is a novel disorder of ketone body utilization. After confirmation of the diagnosis in the index patient, pathogenic mutations, both homozygous and heterozygous, in the MCT1 gene (SLC16A1) were identified in an additional 7 of 96 patients who had unexplained recurrent episodes of severe ketoacidosis. The extent of ketonuria varies during episodes, and the blood pH is normal between episodes. 6
Regarding urinary organic acids, several caveats must be noted: (1) the aforementioned characteristic abnormalities, which are typically present during acute attacks, may be subtle in stable conditions, especially in individuals with mild mutations. 1 -3,19 This can lead to the usual scenario described earlier, in which undiagnosed T2 deficiency is neither suspected nor investigated during the first acute attack. 16,17,27 The results of any subsequent investigations might be inconclusive if samples were obtained after stabilization of the patient’s condition. 2,19,28 (2) In some reported cases, there were only subtle abnormalities in urinary organic acid and blood acylcarnitine profiles during the acute ketoacidotic episode. 10,19 (3) Even in the presence of increased urinary excretion of 2M3HB and TIG, a diagnosis of T2 deficiency cannot be confirmed.
MHBD deficiency (OMIM 300438) is a neurodegenerative disorder with a variable clinical presentation that is usually different from that of T2 deficiency. However, a case of MHBD deficiency mimicking T2 deficiency both clinically and in terms of the urinary organic acid profile (increased excretion of 2M3HB and TIG) has been reported. 2,29 Moreover, MHBD deficiency may produce the same abnormal results as T2 deficiency in a coupled assay. 1,30 Differentiation between T2 and MHBD deficiencies is based on the following: (1) MHBD deficiency is an X-linked disorder; (2) urinary excretion of 2MAA does not increase in MHBD deficiency, even after an oral isoleucine challenge (100 mg/kg body weight), although isoleucine challenge is usually not necessary 3 ; and (3) the potassium-dependent AA-CoA thiolase assay gives a normal result in cases of MHBD deficiency. 28
To overcome the aforementioned challenges, a number of procedures should be followed. Blood gases, electrolytes, glucose, ammonia, TKB (or 3HB if TKB is not available), and FFA are the most important initial investigations during acute attacks. Lactate and pyruvate concentrations should also be measured during the first crises of undiagnosed patients with T2 deficiency to exclude congenital lactic acidosis. 3 The collection of plasma or serum samples for acylcarnitine analysis and aminogram as well as urine samples for organic acid analysis is important at this stage. For accurate evaluation, samples for these analyses should be obtained before glucose infusion. 1,2,19 Enzymatic assays for both T2 and SCOT deficiencies should be performed in suspected cases even in the absence of typical biochemical abnormalities. 1,10
It is worth emphasizing the importance of TKB levels in the diagnosis of T2 deficiency and other ketone body disorders. Total ketone body should be interpreted in light of clinical factors, such as fasting time and any ketogenic stresses, and biochemical factors, especially blood glucose and FFA. The FFA/TKB ratio is a useful tool; being lower than 0.3 in the early fasting stage in patients with T2 deficiency and other ketolytic disorders, it differentiates such conditions from physiological ketosis due to fasting. 31 In the case of associated hypoglycemia, the marked increase in TKB in relation to blood glucose differentiates T2 deficiency (and other ketolytic disorders) from ketotic hypoglycemia. 2 Figure 2 shows a diagnostic flow chart for T2 deficiency.
Molecular Analysis: Diagnostic Challenges
Molecular Analysis
The structure of the human T2 gene (gene symbol ACAT1) was determined in 1991. The gene is located on chromosome 11q22.3 to q23.1 is 27-kb in length and is composed of 12 exons and 11 introns. 32 Genetic mutations resulting in T2 deficiency are highly heterogeneous, with no clear genotype–phenotype correlation. To date, more than 50 different mutations have been discovered and at least 9 novel mutations have been reported in the last 6 years. To our knowledge, apart from the common R208X mutation that has been identified in Vietnamese cases, no other common mutations have been determined. 1,4,7 -15,17,20 -25,28,29,33 -59
T2 deficiency can be confirmed if genomic DNA analysis reveals mutations in ACAT1 gene that were previously identified as causative for T2 deficiency in a mutant complementary DNA (cDNA) expression assay. Screening of other family members for these mutations can identify asymptomatic patients without the need for other sophisticated biochemical or enzymatic assays. Unfortunately, because of the high heterogeneity of mutations in T2 deficiency, this is not the usual scenario. 19
Diagnostic Challenges
DNA analysis of suspected patients with T2 deficiency may reveal novel variants in ACAT1 gene that have never been reported or studied. This is usually enough for a justifiable diagnosis when such variants have not been reported as polymorphisms. However, confirmation of the diagnosis at the molecular level requires mutant cDNA expression assays to verify that these variants are responsible for T2 deficiency. 3 In the absence of any mutations in the coding regions (exons) of the genomic DNA, there are multiple possibilities that must be ruled out before T2 deficiency can be excluded. Although homozygous mutations involving nucleotide substitutions can usually be detected by traditional genomic DNA analysis, heterozygous mutations may be missed. Moreover, copy number variants, small or large heterozygous deletions, and heterozygous or homozygous whole exon duplications cannot be detected by this method. 55,58
Multiplex ligation-dependent probe amplification is a semiquantitative technique by which the relative copy number of multiple DNA sequences can be determined in a single polymerase chain reaction (PCR). By this technique, heterozygous deletions and heterozygous or homozygous exon duplications can be detected. 60 Multiplex ligation-dependent probe amplification for the human ACAT1 gene has already been achieved, and it helped in the detection of a heterozygous deletion including exons 3 to 4 in a patient with T2 deficiency. 58 Real-time PCR can also be used to determine the copy number of each exon. However, neither technique is widely applied. 60,61
Aberrant splicing has been identified in 20% of mutations in the ACAT1 gene. 57,58 Following analysis of genomic DNA, obvious exonic mutations may be reported as silent mutations or polymorphisms if we do not realize their impact on splicing. To discover the effects of mutations on splicing, we have to directly analyze messenger RNA structure. 57
Enzymatic Assay: Diagnostic Challenges
Enzymatic Assay
Enzymatic assay, which is often required to confirm a diagnosis of T2 deficiency, 2 can be performed by different methods: (1) the potassium-dependent AA-CoA thiolase assay is based on the fact that T2 is the only thiolase that is activated in the presence of potassium ions 62 ; (2) the use of 2MAA-CoA as a substrate provides a more sensitive and specific method for the study of residual T2 enzymatic activity 3 ; and (3) the coupled assay for the detection of defects in isoleucine catabolism distal to enoyl-CoA hydratase, using tiglyl-CoA as a substrate, was described as a rapid, straightforward screening test for isoleucine catabolic pathway defects. 30 This procedure has been widely used in the United States and Europe for T2 enzymatic assay. 51
Based on the enzymatic activity detected upon expression of mutant cDNAs, patients have been divided into 2 groups: patients with 2 null mutations and patients in whom at least one of the 2 mutations allows some residual T2 activity. The latter was designated as patients with mild mutations. 7 Patients with T2 deficiency with mild mutations develop ketoacidotic attacks as severe as those in patients with null mutations, but their blood acylcarnitine and urinary organic acid profiles may show only subtle abnormalities even during acute attacks. 1,2,19
Diagnostic Challenges
The potassium-dependent AA-CoA thiolase assay using blood mononuclear cells is possible, but correct evaluation is difficult if the cell preparation includes a lot of erythrocytes. Thus, enzyme assays using fibroblasts are recommended for correct evaluation of T2 enzymatic activity. 3 2MAA-CoA is, unfortunately, neither stable nor marketed. 3 The coupled assay test has 2 substantial flaws: (1) it cannot differentiate T2 deficiency from MHBD deficiency 30 and (2) cases involving mild mutations, where there is residual T2 enzymatic activity, may not be detected by this test. In fact, based on normal results obtained from this test, some patients with T2 deficiency were initially excluded as having the disorder but were later diagnosed with T2 deficiency based on results of the potassium-dependent AA-CoA thiolase assay. 51
Because the coupled assay alone may give false-negative results in cases with residual enzymatic activity and 2MAA-CoA as a substrate is neither stable nor marketed, the potassium-dependent AA-CoA thiolase assay, either alone or combined with the coupled assay, remains the gold standard for T2 enzymatic assay. 3
Screening: Diagnostic Challenges
Screening
Mass screening
Newborn screening programs are invaluable preventive health measures that enable early detection of serious and treatable disorders in the first few days of life before the appearance of any clinical manifestations. 63,64 However, some NBS programs in developing countries are very limited, including only a few disorders. 64,65
Two cases of T2 deficiency were identified by NBS in North Carolina from 1997 to 2005 (by tandem mass spectrometry); however, a missed case (false negative) was identified later, at 15 months of age. That missed case showed an increased C5:1 level only during acute attacks. 13 In a similar NBS program in Minnesota, from January 2001 to November 2010, 1 case was identified, whereas 2 missed cases were discovered later. 10 In an expanded pilot NBS program (liquid chromatography–tandem mass spectrometry) in the Campania region, southern Italy, from 2007 to 2009, 1 case was identified, which led to a diagnosis of T2 deficiency in the patient’s older sister as well. 14 In an interesting study in New South Wales (Australia), an NBS program (April 1998 to March 2002) resulted in a substantial increase in the detection of T2 deficiency to 7 cases compared with only 1 case in the period from April 1974 to March 1998. 66 In that study, there were also 3 missed cases that were discovered later. 67
The results of previous NBS studies have some substantial implications: (1) NBS represents a valuable tool for the detection of T2 deficiency 10,13,14,66 and (2) NBS studies have shown a higher incidence of T2 deficiency than previously reported and provide strong evidence for the underestimation of T2 deficiency. The incidence of T2 deficiency in North Carolina from 1997 to 2005 was nearly 1 per 313 000 newborns, whereas that in Minnesota from January 2001 to November 2010 was 1 per 232 000 newborns. 10,13 Both figures are much higher than the previously estimated incidence of less than 1 per 1 million newborns. 5
Selective screening
Selective screening provides a valuable alternative diagnostic method for the identification of inborn errors of metabolism in developing countries that lack NBS programs. The results may help in preventing further deterioration of the patient and in screening other family members. 65 For example, selective screening of high-risk neonates and children by tandem mass spectrometry in Oman (1998-2008) identified 2 cases of T2 deficiency. 68 In a similar Egyptian study (2008-2013), 6 cases were identified. 25
Diagnostic Challenges
Newborn screening may yield false-negative results, and thus, exclusion of suspected T2 deficiency should not be based on normal NBS results. 2,10 In some countries, such as Japan, where most cases are of the mild genotypic type, the yield of NBS programs is expected to be low, with a high false-negative percentage. 1,28
Selective screening has 2 major flaws. First, if tests are performed under stable clinical conditions, patients with T2 deficiency who lack biochemical abnormalities between attacks will be missed. 1,3 Second, screening may be based on the presence of clinical findings, and some of these findings, such as mental retardation, may be irreversible. In such cases, diagnosis through an NBS program might result in a better prognosis. 25,65,68
Management
The management of T2 deficiency includes prevention of further ketoacidotic attacks, treatment of acute attacks, and screening of other family members.
General Measures for Prevention of Further Ketoacidotic Attacks
Avoidance of prolonged fasting is the cornerstone to prevent further ketoacidotic attacks of T2 deficiency. In case of fever and/or vomiting, increased carbohydrate intake is advised, and intravenous glucose infusion should be considered in such conditions. Monitoring of urinary ketone bodies is advised, and medical advice should be obtained in case of moderate or severe ketonuria. Mild protein restriction, avoidance of a fat-rich diet, and
Treatment of Acute Attacks
In the event of an acute ketoacidotic attack, administration of intravenous glucose should be started—even in cases with a normal blood glucose level—to keep blood glucose at the upper range of the normal level. This will help suppress ketogenesis. Second, appropriate intravenous fluids and electrolytes should be administered to maintain good urine output and keep serum electrolytes within normal limits. Third, if blood pH is < 7.1, a small bicarbonate bolus (1 mmol/kg over 10 minutes) can be given, followed by continuous infusion. This should be guided by frequent monitoring of blood gases and electrolytes to avoid hypernatremia or rapid correction of acidosis.
1
Finally,
Screening of Other Family Members
Screening of family members of a patient diagnosed with T2 deficiency can detect asymptomatic individuals before the development of any acute or chronic clinical manifestations. 3,8
Summary and Conclusions
For 45 years, there have been many challenges in the diagnosis of T2 deficiency and underestimation of its incidence. Improvement in T2 diagnosis together with expansion of NBS programs to more countries will maximize the detection of previously undiagnosed cases. Early diagnosis and management of T2 deficiency enable prevention of its serious acute and chronic complications and remarkably improve the prognosis.
Footnotes
Acknowledgments
The authors thank the Cultural Affairs and Missions Sector, Egyptian Ministry of Higher Education, for their support. They also thank the reviewers for their invaluable comments and suggestions.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The present study was supported in part by Grants in Aid for Scientific Research from the Ministry of Education, Culture, Sports, Science and Technology of Japan (grant numbers 26114708, 24591505); Health and Labor Science Research Grants for Research on Intractable Diseases from the Ministry of Health, Labour and Welfare of Japan; and the Practical Research Project for Rare/Intractable Diseases from the Japan Agency for Medical Research and Development to T.F. [grant number 15AeK0109050h002].
