Abstract
Background:
The use and research of orthobiologics have significantly grown in recent decades, yet patient understanding and perceptions remain largely unexplored. Widespread marketing and potentially misleading claims may skew public understanding of the efficacy and safety of regenerative and orthobiologic therapies.
Purpose/Hypothesis:
The purpose of this study was to examine patient knowledge and perceptions of orthobiologics, identify misconceptions, and understand information sources. It was hypothesized that patients hold significant misconceptions about orthobiologic use and efficacy.
Study Design:
Cross-sectional study.
Methods:
Between October 2023 and April 2024, a cross-sectional, single-center study was conducted at an orthopaedic clinic, engaging all English-speaking patients aged >18 years. A questionnaire was administered covering demographic information, attitudes toward orthobiologic therapies, medical history, and information sources. The survey included multiple-choice questions and Likert scales to assess participants' knowledge and perceptions of the safety and efficacy of orthobiologic treatments. Mean and standard deviation were calculated, and groups were compared using univariate analyses with unpaired t tests.
Results:
A total of 423 responses were obtained, of which 357 met inclusion criteria and were analyzed (response rate, 84.4%). Most respondents were female (56.6%; n = 202) and aged 25 to 34 (33.3%; n = 119), with ages ranging from 18 to 84 years. Among the respondents, 44.0% (n = 157) were familiar with orthobiologics. Within the entire cohort, patients most frequently indicated the belief that orthobiologics could manage pain and inflammation (70.9%; n = 253) and treat cartilage injuries (66.9%; n = 239). Among respondents aware of orthobiologics, the most recognized treatments were platelet-rich plasma (77.1%; n = 121), mesenchymal stromal cells (56.7%; n = 89), and bone marrow aspirate concentrate (38.2%; n = 60). Among these patients, 45.9% (n = 72) believed orthobiologics could reduce pain, and 36.3% (n = 57) believed they could enhance healing rates. Belief in current evidence was mixed, with 37.6% (n = 59) deeming it insufficient and 15.3% (n = 24) considering it adequate. The most influential factors in patients' decisions to use orthobiologics were cost (68.8%; n = 108), recommendations from orthopaedic surgeons (63.1%; n = 99), and potential side effects (57.3%; n = 90). Primary information sources were orthopaedic surgeons (38.2%; n = 60), other physicians (33.8%; n = 53), and friends or family (32.5%; n = 51).
Conclusion:
This study demonstrated that patient familiarity with orthobiologics remains limited, with significant variation in understanding that highlights the need for improved education and communication. Physicians, as the primary source of information, play a critical role in bridging this gap. Financial considerations and potential side effects significantly influence patient decisions and should be emphasized during consultations to support well-informed choices.
Keywords
Musculoskeletal conditions affect >33% of the US population and account for >50% of disabling health conditions among adults.36,39 In 2016, these conditions contributed to 574 million physician visits and 379 million visits to nonphysician providers, underscoring the need for innovative treatment options.36,39 Recent decades have seen substantial advancements in biologic-based therapies across various medical disciplines.6,7,26,28 Orthobiologics, including platelet-rich plasma, stromal cells, and related products, are now used by 66% of sports medicine physicians, both as stand-alone and adjunctive treatments.3,6,10,13,21,40 Research in this field has expanded exponentially over the past 20 years; however, heterogeneity in study designs, outcomes, and treatment protocols underscores the need for higher-quality evidence to more clearly define efficacy.4,5,8,9,20,22,29,38 Therefore, managing patient expectations by engaging in constructive discussions to understand their perspectives, providing education, and guiding them to reliable information sources is crucial.
The biologic-based therapy industry has expanded profoundly, with the orthopaedic sector occupying nearly 60% of this market.17,33-35 A survey of the AOSSM membership reported that 71% of physicians are increasing their use of orthobiologics, while 23% actively advertise these treatments. 21 Commercial growth has paralleled public demand, particularly for stromal cell interventions. Between 2009 and 2014, the number of US businesses offering such treatments doubled annually, and by 2016, 351 companies marketed stromal cell products at 570 clinics nationwide.17,30,34,35 This commercialization, coupled with misinformation and appealing promises, has led to inflated patient expectations and a distorted public perception of these treatments.12,19,23 Consequently, patients may pursue therapies lacking robust safety and efficacy data, thereby assuming unnecessary risks.12,24,25
While research, clinical use, and commercialization of orthobiologics have significantly increased in recent years, there remains a substantial gap in understanding patient knowledge and beliefs about these therapies. Existing research, largely focused on stromal cell therapies, suggests a mix of evidence-based and unsupported beliefs, including pain reduction and tissue regeneration, respectively.2,15 These findings also underscore the critical need for improved patient education, particularly as exposure through advertising grows. To our knowledge, no previous study has comprehensively evaluated patients' foundational understanding of orthobiologics as a whole. Therefore, the purpose of this study was to examine patient knowledge and perceptions of orthobiologics, identify potential misconceptions, and understand the sources from which patients acquire information. The authors hypothesized that patients hold significant misconceptions about the use and efficacy of orthobiologics, underscoring the urgency for meaningful educational interventions.
Methods
Participants
This cross-sectional, single-center study received approval from the institutional review board (IRB) to investigate patients' understanding of orthobiologics. Eligible participants were English-speaking individuals aged ≥18 years. Exclusion criteria included individuals <18, non−English speakers, those unable to complete questionnaires due to cognitive or physical limitations, and individuals declining participation. Incomplete responses were removed from analysis. Patients were not included or excluded based on previous experience with orthobiologic treatments or musculoskeletal issues; however, these data were collected through survey items addressing familiarity with orthobiologics, history of orthopaedic surgery, and history of intra-articular injections. Recruitment occurred in the waiting rooms of Midwest Orthopaedics at Rush, Department of Orthopaedic Surgery, Rush University Medical Center, from October 2023 to April 2024. Following IRB guidelines, participants were presented with a virtual informed consent form detailing the study's aims, methodology, confidentiality of data, and potential risks and benefits. Participants provided electronic consent by selecting "Yes" in response to the statement “Select below if you consent and agree to participate” on the consent form, granting access to the survey. The survey was designed to be discontinued at any point without consequence.
Questionnaire
The survey instrument was meticulously developed to capture a comprehensive range of data—from basic demographic information to nuanced opinions regarding orthobiologic therapies (see Appendix). Content and structure were refined in collaboration with domain experts (A.B.Y., B.J.C., N.N.V. and J.C.) and contemporary literature14,18 to ensure question relevance and clarity. The survey employed a mix of question types, including multiple-choice (with options for single or multiple answers), Likert scales, and open-ended questions to extensively cover topics related to participants' attitudes and understanding of the safety and efficacy of orthobiologic treatments. Demographic questions sought details on age, sex, race, and education level, while health-related queries inquired about insurance status, history of orthopaedic interventions, and current pain levels. The inclusion of open-ended questions was designed to elicit qualitative insights, offering participants the opportunity to express their views and experiences in their own words.
To ensure the confidentiality and protection of participant data, this study employed Research Electronic Data Capture (REDCap) (Version 13.6.1; Vanderbilt University), a secure, web-based application designed for data collection in research studies. REDCap, a Health Insurance Portability and Accountability Act (HIPAA)−compliant application, encrypts and secures participant information, accessible solely to authorized research personnel, thus upholding stringent data privacy and security standards throughout the data collection process.
Statistical Analysis
Data analysis was conducted using R Version 4.3.1 “Beagle Scouts,” provided by the R Foundation for Statistical Computing. Categorical variables were summarized using counts and percentages. Fisher exact test for count data or χ2 was utilized for categorical data analysis where appropriate. For continuous variables, mean and standard deviation were calculated, and groups were compared using univariate analyses with unpaired t tests. Statistical significance was set a priori at P < .05 for all statistical tests. A target sample size of ≥150 respondents was prospectively determined to ensure statistical reliability and practical feasibility, aiming for an acceptable margin of error at a 95% confidence level.1,32
Results
Patient Characteristics
Out of the 423 patients who responded to the survey, 66 incomplete surveys were excluded, resulting in 357 respondents included for analysis, yielding a complete response rate of 84.4%. Among these respondents, a majority were female (n = 202; 56.6%), with the largest proportion falling within the 25 to 34 age group (n = 119; 33.3%) (Table 1). The cohort predominantly comprised Caucasian individuals (n = 257; 72.0%), with most identifying as non-Hispanic (n = 265; 74.2%). Additionally, a majority reported holding a bachelor's degree as their highest level of education (n = 193; 54.1%). Notably, 33.9% (n = 121) reported a history of prior orthopaedic surgery, and 31.9% (n = 114) had previously received an intra-articular injection. On average, participants reported a pain level of 3.4 ± 2.1, with knee pain being the most commonly cited source of discomfort (n = 142; 39.8%).
Baseline Patient Characteristics a
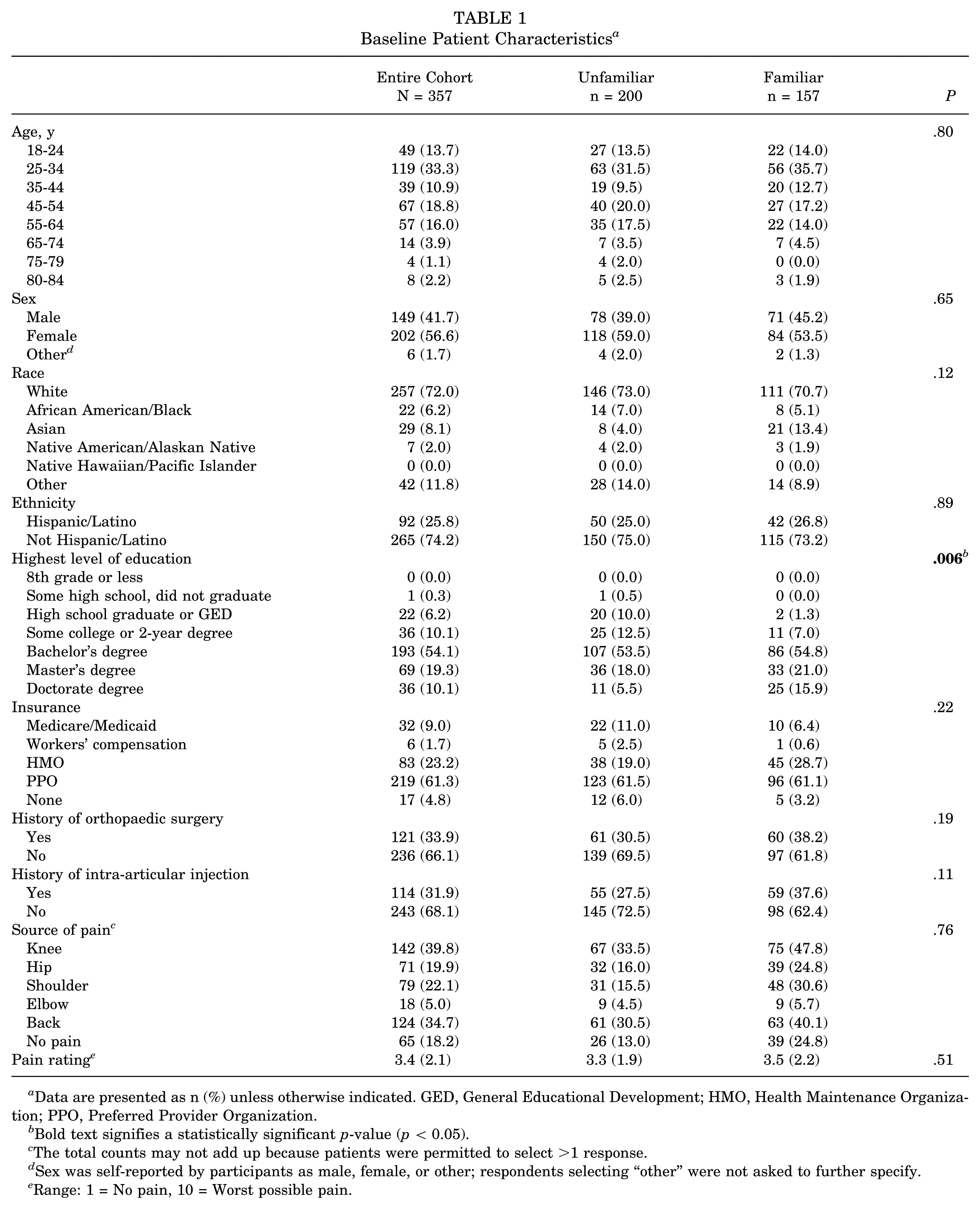
Data are presented as n (%) unless otherwise indicated. GED, General Educational Development; HMO, Health Maintenance Organization; PPO, Preferred Provider Organization.
Bold text signifies a statistically significant p-value (p < 0.05).
The total counts may not add up because patients were permitted to select >1 response.
Sex was self-reported by participants as male, female, or other; respondents selecting “other” were not asked to further specify.
Range: 1 = No pain, 10 = Worst possible pain.
Comparison between respondents familiar with orthobiologics and those unfamiliar revealed no significant baseline differences, except for the highest level of education. Among those unfamiliar with orthobiologics, 10.0% (n = 20) had a maximum of a high school degree or equivalent, compared with only 1.3% (n = 2) of those familiar with orthobiologics. Conversely, a greater proportion of respondents familiar with orthobiologics held a doctorate degree (n = 25; 15.9%) compared with those unfamiliar (n = 11; 5.5%) (P = .006).
Patient Knowledge and Perception of Orthobiologics
Among surveyed patients, n = 157 (44.0%) were familiar with orthobiologics prior to participation (Table 2). When queried about musculoskeletal conditions or symptoms they believed could be alleviated or managed with orthobiologics, pain and inflammation were most frequently selected (n = 253; 70.9%), followed by cartilage injuries (n = 239; 66.9%), shoulder injuries (n = 222; 62.2%), ligament sprains or tears (n = 218; 61.1%), and osteoarthritis (n = 211; 59.1%).
Patient Exposure to and Beliefs About Orthobiologics a

Data are presented as n (%). BMAC, bone marrow aspirate concentrate; BMP-2, bone morphogenetic protein–2; ECM, extracellular matrix; MSC, mesenchymal stromal cell; PRP, platelet-rich plasma.
The total counts may not add up due to patients being permitted to select >1 response.
Of patients who were familiar with biologic-based therapies, a large portion of respondents (n =121; 77.1%) indicated knowing about platelet-rich plasma (PRP), followed by mesenchymal stromal cells (n = 89; 56.7%), and bone marrow aspirate concentrate (n = 60; 38.2%) (Figure 1). Additionally, 2 patients (2%) selected the "other" response, mentioning familiarity with peptides and platelet-rich fibrin in the free-response section.
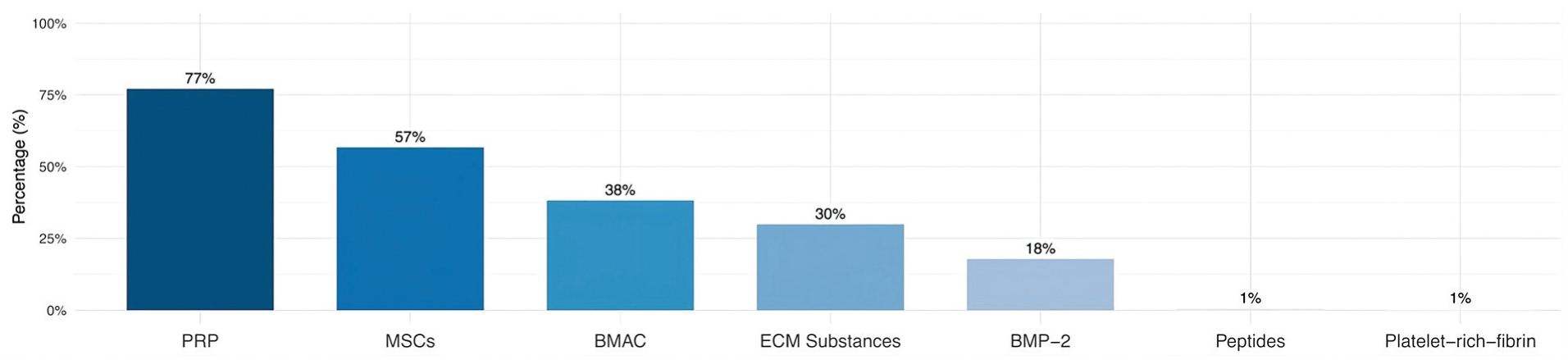
Bar graph illustrating the orthobiologics that patients are familiar with. BMAC, bone marrow aspirate concentrate; BMP-2, bone morphogenetic protein–2; ECM, extracellular matrix; MSC, mesenchymal stromal cell; PRP, platelet-rich plasma.
In terms of general perceptions and influences on views of these therapies, most patients familiar with orthobiologics reported a heightened curiosity after learning about them (n = 107; 68.2%), while smaller proportions noted increased concern (n = 9; 5.7%) or stated they had gained a balanced view of both advantages and disadvantages (n = 41; 26.1%). A large proportion of patients believed that orthobiologics are effective for pain reduction (n = 72; 45%), and 36.3% (n = 57) indicated a belief in their capacity to increase the rate of healing (Figure 2). Of patients who were familiar with orthobiologics, 37% (n = 59) believed that the current evidence supporting orthobiologics was sufficient, while 15.3% (n = 24) expressed uncertainty regarding the current available evidence.
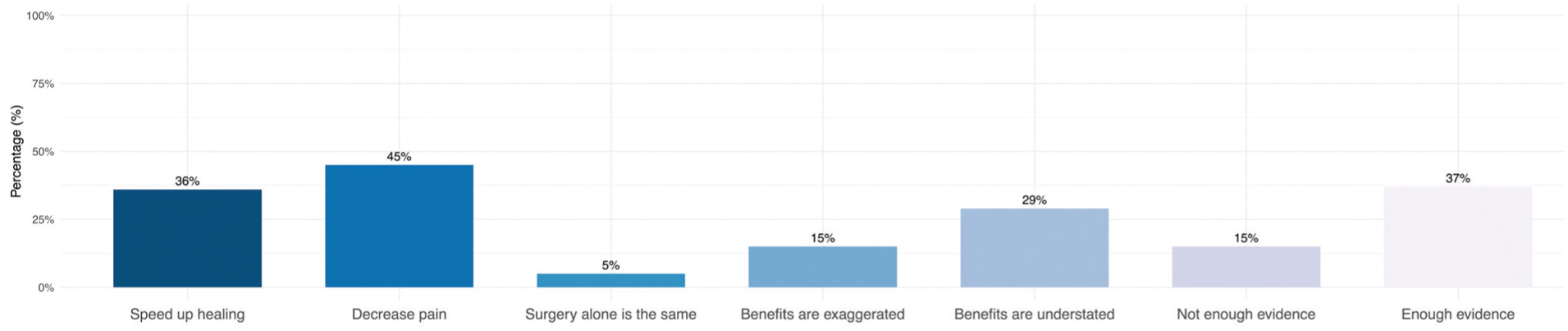
Bar graph illustrating patient beliefs about orthobiologics.
When deciding on the use of orthobiologics in their care, cost (n = 108; 69%) and potential side effects (n = 90; 57.3%) were identified as the most critical factors for a majority of patients who were familiar with orthobiologics. Furthermore, the recommendation of an orthopaedic surgeon played a significant role, with 63.1% (n = 99) considering it an important factor (Figure 3). A large majority (n = 135; 86.0%,) expressed interest in learning more about orthobiologics, while 14.0% (n = 22) indicated no interest. Figure 4 illustrates additional perceptions of the entire cohort (N = 357).
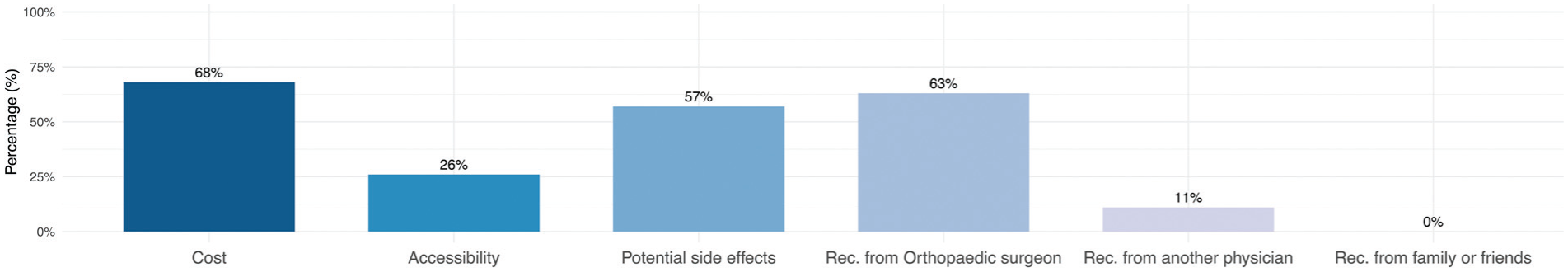
Bar graph depicting factors influencing patients’ decision to consider orthobiologics in their care. Rec, recommendation.
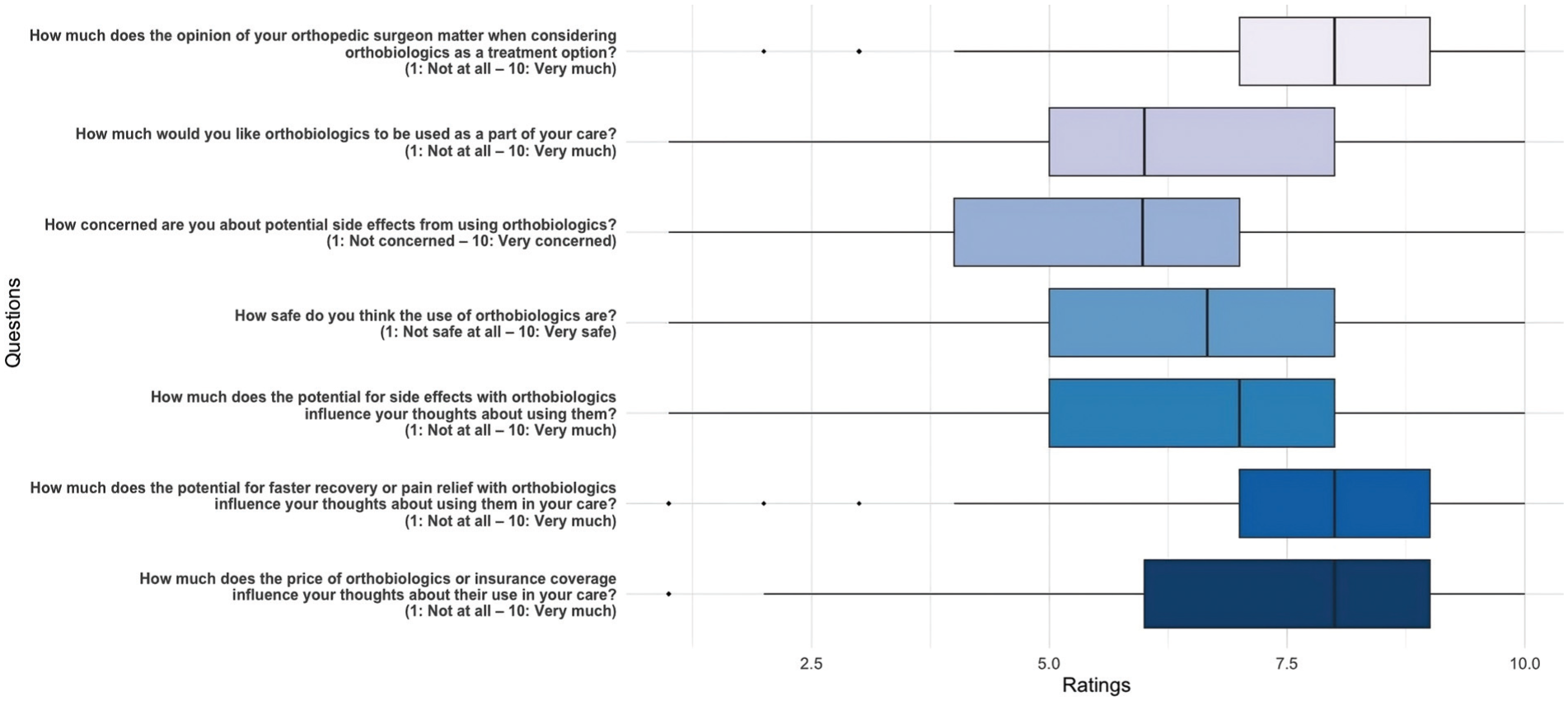
Boxplot illustrating patient perceptions and thoughts about orthobiologics. The distribution of responses is illustrated with boxes indicating the IQR (25th-75th percentile) and whiskers extending to 1.5 times the IQR from the box. Outliers are indicated by diamond-shaped marks (⋄), highlighting responses that lie outside the typical range.
Information Acquisition
Regarding sources of information, patients commonly reported obtaining information about orthobiologics from orthopaedic surgeons (n = 60; 38.2%), followed by other physicians (n = 53; 33.8%), and friends or family (n = 51; 32.5%) (Figure 5). Social media was chosen by 22.3% (n = 35) of patients, with podcasts (n = 21; 13.4%), Instagram (n = 14; 8.9%), and YouTube (n = 14; 8.9%) being the most frequently cited platforms (Table 3). News media was selected by only 7.0% (n = 11) of patients, with the National Broadcasting Company (NBC) (n = 4; 2.5%), Fox News (n = 3; 1.9%), and Cable News Network (CNN) (n = 3; 1.9%) being the most common outlets. Advertisements were noted as sources of information by 7.6% (n = 12) of patients, with social media (n = 7; 4.5%) and radio (n = 6; 3.8%) being the primary platforms through which participants were exposed to advertisements about orthobiologics.
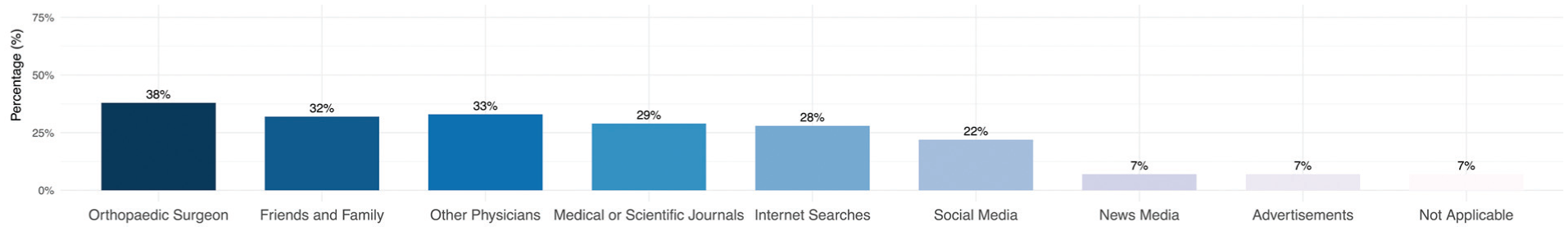
Bar graph illustrating the sources of information from which patients learn about orthobiologics.
Subcategories of Patient Information Sources on Orthobiologics a
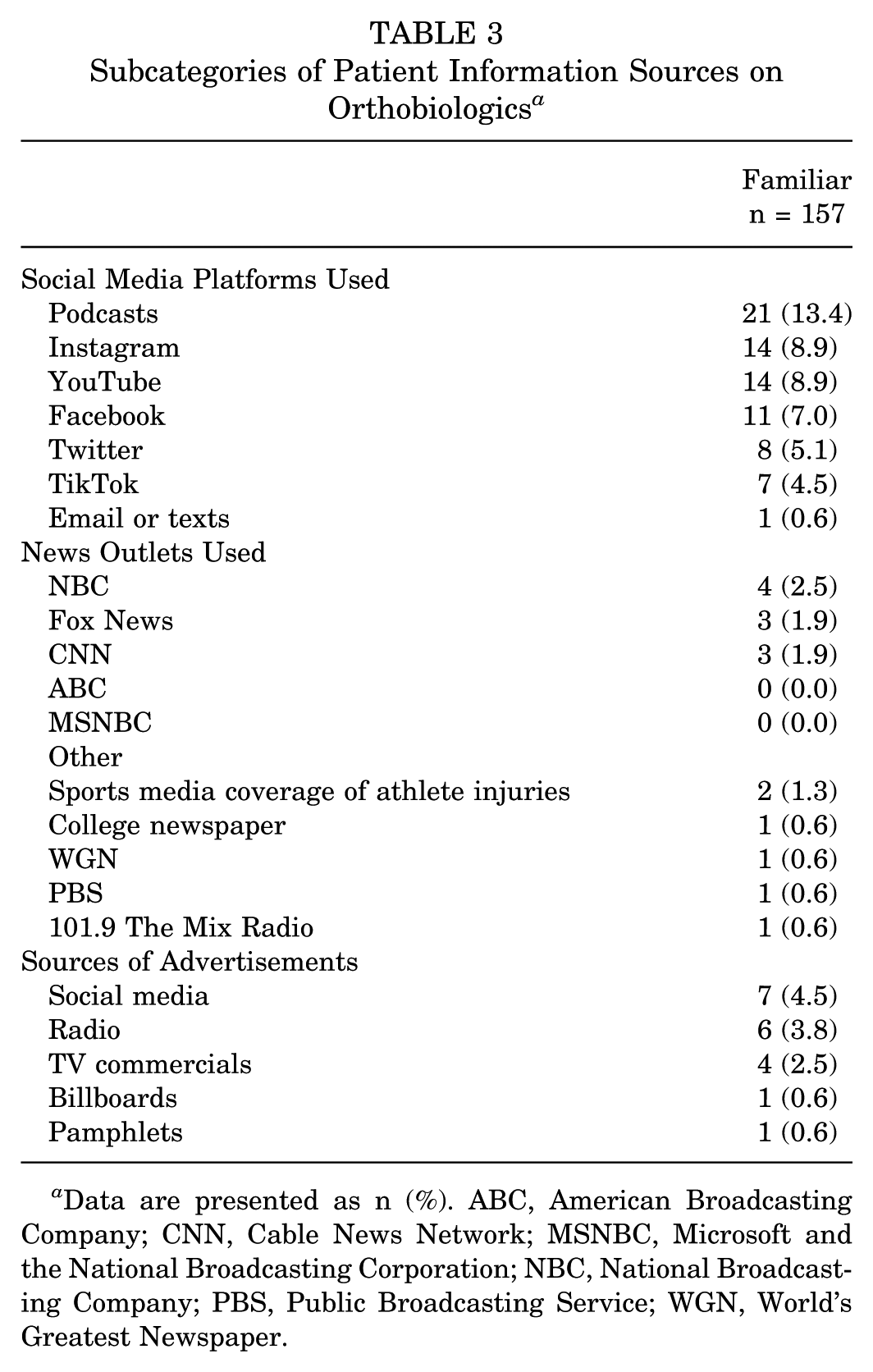
Data are presented as n (%). ABC, American Broadcasting Company; CNN, Cable News Network; MSNBC, Microsoft and the National Broadcasting Corporation; NBC, National Broadcasting Company; PBS, Public Broadcasting Service; WGN, World's Greatest Newspaper.
Discussion
The primary findings of this study indicate that among the surveyed patients, only 44.0% (n = 157) were familiar with orthobiologics. Among these, PRP was the most widely recognized by the public (71.1%). Physicians remained the predominant source of information (72.0%). Patient perception of orthobiologics revealed cautious optimism. Many believed these treatments could accelerate healing (36.3%) and reduce pain (45.9%), but a significant portion also expressed uncertainty about the evidence supporting these treatments. Confidence in the sufficiency of evidence for orthobiologics use was relatively low (37.6%). The most influential factors in the decision to use orthobiologics were cost (68.8%), recommendation from an orthopaedic surgeon (63.1%), and potential side effects (57.3%).
The finding that less than half of surveyed patients were familiar with orthobiologics presents a complex issue with potential explanations on both sides of the patient-physician interaction. This low awareness could indicate a communication gap, where orthobiologics are not adequately explained during consultations, leaving patients uninformed about potential treatment options. Alternatively, it might reflect a cautious approach by physicians, reserving orthobiologics for situations with more robust supporting evidence and established protocols. A recent study of knee osteoarthritis patients found that only 2% were offered the therapy and just 6.5% had even heard of it. 16 It is important to recognize that orthobiologic treatments are not suitable for everyone. Although 66.1% of sports medicine physicians report using ≥1 orthobiologic in their practice, 21 the exact percentage of patients who benefit from these therapies remains unclear. Still, the low awareness found among patients suggests that the market pressure for orthobiologics may be lower than expected,17,30,33-35 which could be considered a positive finding.
Among the evaluated orthobiologics, PRP emerged as the most widely recognized among patients (71.1%). This finding aligns with the growing popularity of PRP among sports medicine physicians, with >70% of those who incorporate orthobiologics into their practice utilizing PRP. 21 This acceptance is likely because of its perceived safety, low complication rate, and ease of preparation and application.11,22,27 However, a concerning trend reported by Noback et al 21 is that approximately 30% of physicians who opted for PRP treatment did so because of competitive pressure rather than compelling scientific evidence. This suggests that the popularity of orthobiologics, both among sports medicine physicians and now among patients, may be driven by factors beyond rigorous scientific evidence.
Another noteworthy aspect is the prevailing confusion among patients regarding the conditions that orthobiologics can effectively treat. When asked about 11 specific conditions where orthobiologics were being used as treatment, only "pain and inflammation" was selected by >70% of patients. For the remaining pathologies and symptoms, responses ranged from 29% to 67%. This suggests that pain and inflammation management may have been the primary reasons cited by physicians when recommending orthobiologics. It could also indicate a lower level of physician confidence in utilizing these therapies for other symptoms and conditions, potentially leading to a hesitancy to present them as options to patients.
Regarding information sources, this study found that physicians remain the primary source of information for patients (38.2% orthopaedic surgeons, and 33.8% other physicians). Although previous studies reported an increase in orthobiologic advertising and a growing direct-to-consumer marketing trend, 35 this research found that advertising accounted for only 7.6% of information sources. This emphasizes the critical role of physicians in staying current on the latest advancements in orthobiologic therapies and their supporting evidence. They must engage in open and transparent discussions with patients, exploring all potential treatment options and ensuring informed decision-making.
Additionally, knowing that cost and potential side effects are paramount concerns for patients, physicians must address these aspects clearly. Many participants in this study had no prior personal experience with orthobiologic treatments, meaning their decision-making may have been shaped more by perceived possibilities or secondhand information than by direct treatment outcomes. 2 This perspective is nonetheless valuable, as it reflects how patients commonly approach these therapies when awareness is informed by external sources. In such circumstances, decisions are especially susceptible to external drivers such as cost transparency, surgeon recommendation, and perceived risk rather than prior personal benefit. 2 This dynamic may help explain why cost and surgeon guidance were ranked so highly in our study, as they represent accessible anchors for decision making among patients both with and without previous experience with orthobiologics.
Among all factors, cost emerged as the most influential, with 69% of patients identifying it as a key driver. This aligns with evidence from other specialties showing that out-of-pocket expenses strongly shape treatment decisions, even for guideline-recommended therapies with proven mortality benefit. 31 If cost can meaningfully influence uptake of therapies with well-established efficacy, 31 it is reasonable to expect that it would play an even more prominent role in decisions about orthobiologics, where uncertainty about effectiveness persists and where patients both with and without previous exposure may weigh financial considerations heavily in the absence of clear long-term evidence. Likewise, physician recommendation and clear communication of risks and benefits have consistently been shown to guide patient choices in shared decision-making studies. 37 Together, these findings underscore the responsibility of physicians to contextualize orthobiologics for patients by providing transparent discussion of financial implications alongside both common and uncommon side effects, to ensure informed and balanced decision-making.
Limitations
This study acknowledges certain limitations that should be considered. The sample was drawn from a single institution, potentially restricting the generalizability of the findings to other populations. Additionally, the study participants were recruited from the waiting room of orthopaedic clinics, suggesting that they may have been more exposed to information about orthobiologics compared with the general population, due to their proximity to health care services and their active interest in seeking information about their conditions and potential therapies. Additionally, because our cohort included both patients with and without previous exposure to orthobiologic treatments, their perspectives may reflect a mixture of direct experience and perceived possibilities derived from external information sources. Furthermore, the study relied on patient self-reports, which may be susceptible to recall bias. Finally, although the cohort of 357 patients with an 84.4% response rate provides meaningful insights, the single-center survey design may limit generalizability and does not allow for the depth of exploration achievable with structured interviews. Larger multicenter studies incorporating both larger populations and complementary qualitative methods may provide a more nuanced understanding of patient knowledge and decision-making.
Conclusion
Our study demonstrated that patient familiarity with orthobiologics remains limited, with significant variation in understanding that highlights the need for improved education and communication. Physicians, as the primary source of information, play a critical role in bridging this gap. Financial considerations and potential side effects significantly influence patient decisions and should be emphasized during consultations to support well-informed choices.
Footnotes
Appendix – Patient Survey
Final revision submitted September 20, 2025; accepted October 19, 2025.
One or more of the authors has declared the following potential conflict of interest or source of funding: R.G. is an editorial or governing board member of Arthroscopy, is a paid presenter or speaker for ENOVIS, and has received other financial or material support from Smith & Nephew. A.B.Y. is a paid consultant for Allo Source, JFR Ortho, and Stryker; is an unpaid consultant for Patient IQ and Sparta Biomedical; has received research support from Arthrex Inc and Organogensis; holds stock or stock options in Icarus Medical, Patient IQ, and Sparta Biomedical; and is a paid presenter or speaker for Stryker. B.J.C. has received research support from Aesculap/B.Braun and National Institutes of Health; is an editorial or governing board member of The American Journal of Sports Medicine and Journal of the American Academy of Orthopaedic Surgeons; receives royalties from Arthrex Inc; receives royalties and financial or material support from Elsevier Publishing; is a paid consultant for Arthrex Inc; has received research support from Arthrex Inc; holds stock or stock options in Bandgrip Inc and Ossio; and receives other financial or material support from JRF Ortho. N.N.V. is a board or committee member of the AOSSM, American Shoulder and Elbow Surgeons, and Arthroscopy Association of North America; has received research support from Breg and Ossur; is an editorial or governing board member of SLACK Inc; has received hospitality payments from Spinal Simplicity; has received consulting fees from Arthrex Inc and Stryker Corporation; and receives royalties or license from Arthrex Inc, Graymont Professional Products IP LLC, and Smith & Nephew. J.C. is a board or committee member of the AOSSM, Arthroscopy Association of North America, and International Society of Arthroscopy, Knee Surgery, and Orthopaedic Sports Medicine; is a paid consultant for Ossur; has received a grant from Arthrex Inc; has received consulting fees from Arthrex Inc, Smith & Nephew, DePuy Synthes Products, Linvatec Corporation, Vericel, and RTI Surgical Inc; has received support for education from Arthrex Inc, Smith & Nephew, and Medwest Associates; has received hospitality payments from Styker and Medical Device Business Services; and has received speaking fees from CONMED Corporation and Linvatec Corporation. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Ethical approval for this study was obtained from Rush University Medical Center (No. ORA23091307).
