Abstract
Background:
Platelet-rich plasma (PRP) has been utilized as adjunctive therapy in arthroscopic rotator cuff repair. However, there is currently limited research available on the efficacy of PRP in arthroscopic repair of full-thickness rotator cuff tears.
Purpose:
This study aimed to perform a cross-sectional analysis of overlapping meta-analyses comparing the clinical efficacy of arthroscopic repair of full-thickness rotator cuff tears with and without PRP to assist clinicians in assessing the most reliable evidence and formulating treatment recommendations accordingly.
Study Design:
Systematic review; Level of evidence, 2.
Methods:
Under PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines, comprehensive searches of meta-analyses were performed in the PubMed, Embase, and Cochrane Library databases until June 1, 2024, and found 63 studies. The methodological quality of the included studies was evaluated using the Assessment of Multiple Systematic Reviews (AMSTAR) and Oxford Centre for Evidence-Based Medicine Levels of Evidence instruments. Data extraction from the included meta-analyses was independently performed by 2 reviewers. The Jadad decision algorithm was employed to identify meta-analyses with the most robust evidence.
Results:
This study included 5 meta-analyses. These meta-analyses had AMSTAR scores ranging from 7 to 9, with a mean of 8. The most reliable evidence, assessed by the Jadad algorithm, included 8 randomized controlled trials and involved 566 patients. It showed that the short-term (≤12 months after surgery) retear rate and visual analog scale score were significantly lower in those with PRP than in those without PRP. The short-term Constant score, short-term University of California, Los Angeles (UCLA) activity score, and long-term (>12 months after surgery) UCLA score were significantly higher in the PRP group, especially in single-row fixation.
Conclusion:
Our study demonstrates that the most reliable evidence suggests that PRP injections can be recommended as adjunctive therapy in single-row repair for enhanced short-term outcomes. Further high-quality randomized controlled trials are imperative to increase the strength of evidence.
Rotator cuff tears are prevalent tendon injuries that lead to enduring shoulder pain and restricted mobility. When nonoperative treatment is ineffective, surgical repair is the primary approach,15,36 offering favorable outcomes, particularly for full-thickness tears.16,34,45 Despite ongoing advancements in instrumentation and surgical techniques, the postoperative retear rate remains notably high, ranging from 8% to 94%.7,11,16,23,30 Additionally, pain and weakness are common concerns after arthroscopic repair and can significantly affect patients’ daily activities. To address this, platelet-rich plasma (PRP) has been explored as adjunctive therapy in rotator cuff repair.20,24,31,50
PRP was initially reported for therapeutic purposes in the 1980s. 19 It is a natural concentration of platelets obtained through the centrifugation of autologous whole blood. PRP is known to reduce inflammation and enhance healing by releasing various cytokines and growth factors such as vascular endothelial growth factor, insulin-like growth factor, transforming growth factor–β, and platelet-derived growth factor.39,46,47 The efficacy of PRP has been validated through basic science and animal experiments.5,25,29,35,42 Yet, several clinical trials and meta-analyses on PRP in arthroscopic rotator cuff repair have produced incongruous results.4,6,12,13,28,41,50,53-55 The inconsistent interpretations from these studies leave clinicians puzzled.
This study addresses the uncertainty by assessing the methodology and reporting quality of intersecting meta-analyses. Cross-sectional analyses of meta-analyses are crucial for decision-makers to optimize treatment strategies by examining overlapping reviews on the same topic.2,3,38,52 The objective of this study was to aid clinicians in evaluating the most reliable evidence from meta-analyses so that they can decide whether to use PRP during arthroscopic rotator cuff repair. We hypothesized that PRP injections can be recommended as adjunctive therapy in arthroscopic repair of full-thickness rotator cuff tears.
Methods
Literature Search
The design of this study is consistent with similar previously published studies and adheres to the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines.2,3,38,52 There were 2 reviewers (X.L. and Z.X.) who independently conducted thorough searches of the PubMed, Embase, and Cochrane Library databases up to June 1, 2024, using keywords such as “arthroscopic,”“rotator cuff tear,”“systematic review,”“meta-analysis,”“platelet-rich plasma,” and “PRP.” We filtered the search results to include only meta-analyses and found 63 studies. The initial screening process included evaluating titles and abstracts, with full texts reviewed when needed. Additionally, references from the included studies were checked, and a manual search was conducted to ensure all pertinent studies were identified. Any discrepancies were resolved through a discussion, with the involvement of a third reviewer (H.T.) when necessary.
Eligibility Criteria
Inclusion criteria for studies were as follows: meta-analyses (1) published in English that exclusively included randomized controlled trials (RCTs); (2) focusing on arthroscopic repair of full-thickness rotator cuff tears; (3) aimed to compare repair with PRP versus repair without PRP; and (4) reporting ≥1 outcome measure, such as the retear rate or visual analog scale. Excluded were narrative reviews, meeting abstracts, case reports, and editorials. Studies involving patients with partial-thickness rotator cuff tears, those with inadequate follow-up (<12 months), or those with a history of injuries or surgery to the same shoulder were also excluded.
Data Extraction
The same 2 reviewers (X.L. and Z.X.) independently extracted data from the included meta-analyses. The collected data encompassed details such as the first author, publication date, search databases, date of the latest literature search, language restrictions, primary study design, number of trials included, software utilized for analysis, Grading of Recommendations Assessment, Development and Evaluation (GRADE) summary, publication bias analysis, conflict of interest disclosure, I2 value, and meta-analysis findings. Outcomes in the studies were evaluated at ≤12 months after surgery and >12 months after surgery.50,54 Any discrepancies were resolved through a discussion, with a third reviewer (H.T.) involved when necessary.
Quality Assessment
Again, 2 reviewers (X.L. and Z.X.) independently evaluated the methodological quality of the meta-analyses using the Oxford Centre for Evidence-Based Medicine Levels of Evidence 51 and Assessment of Multiple Systematic Reviews (AMSTAR) 43 instruments. The AMSTAR is known for its reliability, validity, and responsiveness in assessing systematic reviews. 44 Any disagreements were resolved through a discussion, with the involvement of a third reviewer (H.T.) when required.
Assessment of Heterogeneity
The I2 statistic quantifies the proportion of total variation attributed to heterogeneity, generating values between 0% and 100%. An I2 value of 0% denotes no observed heterogeneity, with higher values indicating greater levels of heterogeneity. 27 Per the Cochrane Handbook, an I2 value ≤50% suggests acceptable heterogeneity across studies in a systematic review or meta-analysis. 26 When significant heterogeneity was present among studies for a variable, we recorded whether the included meta-analyses explored its source. Additionally, we documented whether these studies performed sensitivity analyses and evaluated publication bias.
Application of Jadad Decision Algorithm
Overall, 3 reviewers (S.Y., B.Z., and T.L.) independently analyzed the sources of discrepancies among the meta-analyses using the Jadad decision algorithm and came to a consensus. Discrepancies could stem from variations in clinical queries, inclusion and exclusion criteria, methods of data extraction, assessments of study quality, techniques for data pooling, and statistical approaches for data synthesis. The algorithm facilitated the identification of the most reliable meta-analyses and enabled the formulation of recommendations even in the presence of conflicting outcomes.22,32,56
Results
Literature Search
Figure 1 outlines the study selection process. Among the 63 records reviewed, 5 meta-analyses met the inclusion criteria for this cross-sectional analysis.12,50,53-55 The characteristics of these meta-analyses are outlined in Table 1. These publications spanned from 2015 to 2020, with each meta-analysis encompassing 5 to 15 primary trials (Table 2), all of which were RCTs. Xiao etal 53 conducted the meta-analysis with the highest number of primary studies. Yang etal 54 conducted the most recent meta-analysis, while Zhao etal 55 conducted the earliest one.
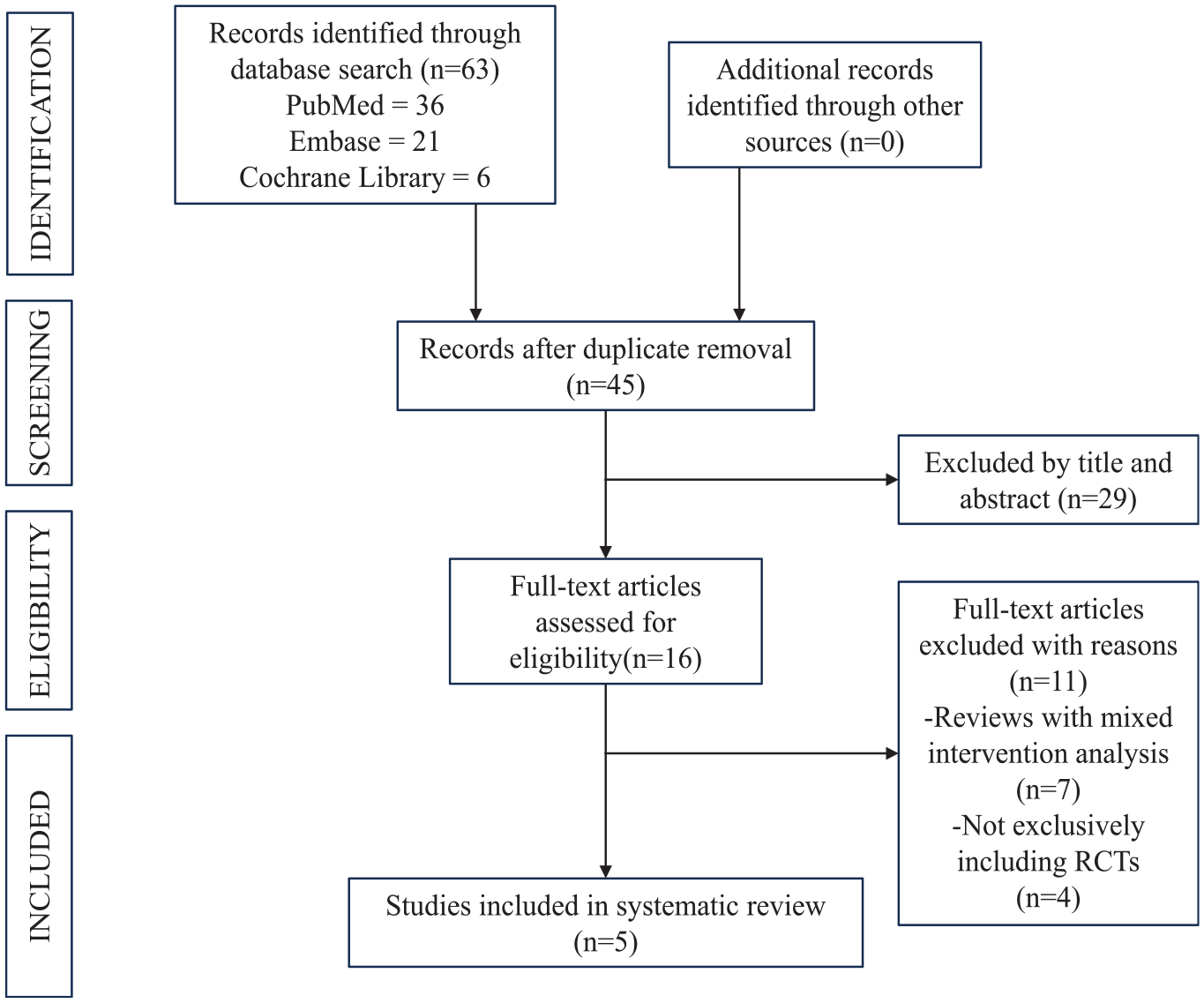
PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) flow diagram of study selection.
Characteristics of Meta-analyses a

RCT, randomized controlled trial.
Primary Studies Included in Meta-analyses

Search Methodology
There were 2 meta-analyses that imposed no language restrictions,53,55 while this information was not specified in the remaining meta-analyses. Only Zhao etal 55 conducted a search for gray literature. All meta-analyses utilized PubMed and Embase as their search databases, but there was variability in the utilization of the Cochrane Library, Google Scholar, and Web of Science. Specific search methodologies are delineated in Table 3.
Search Methodology of Meta-analyses a

NA, not available.
Methodological Quality
As outlined in Table 4, the meta-analyses included were classified as level 2 evidence based on the Oxford Centre for Evidence-Based Medicine Levels of Evidence instrument. All meta-analyses employed RevMan for data analysis. The GRADE method was utilized by Wang etal 50 and Zhao etal. 55 AMSTAR scores varied from 7 to 9, with a mean of 8 (Table 5). The meta-analysis authored by Wang etal 50 attained the highest quality rating.
Methodological Quality of Meta-analyses a
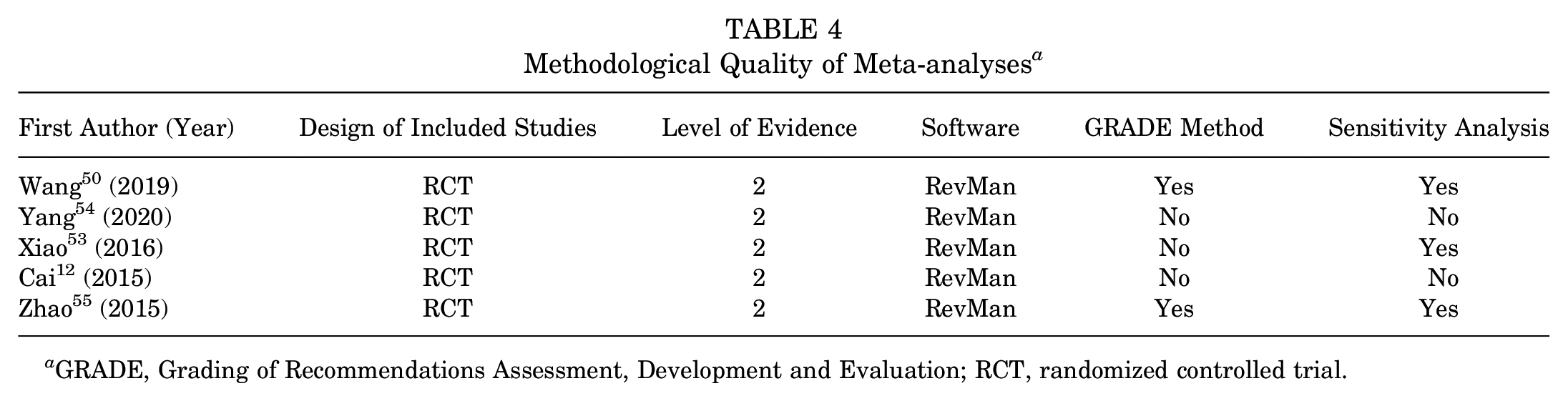
GRADE, Grading of Recommendations Assessment, Development and Evaluation; RCT, randomized controlled trial.
AMSTAR Scores of Meta-analyses a

AMSTAR, Assessment of Multiple Systematic Reviews.
Assessment of Heterogeneity
All the meta-analyses included evaluated heterogeneity, with the I2 values detailed in Table 6. There were 3 meta-analyses that conducted sensitivity analyses focusing on methodological quality (Table 4).50,53,55
I 2 Values of Variables in Meta-analyses a
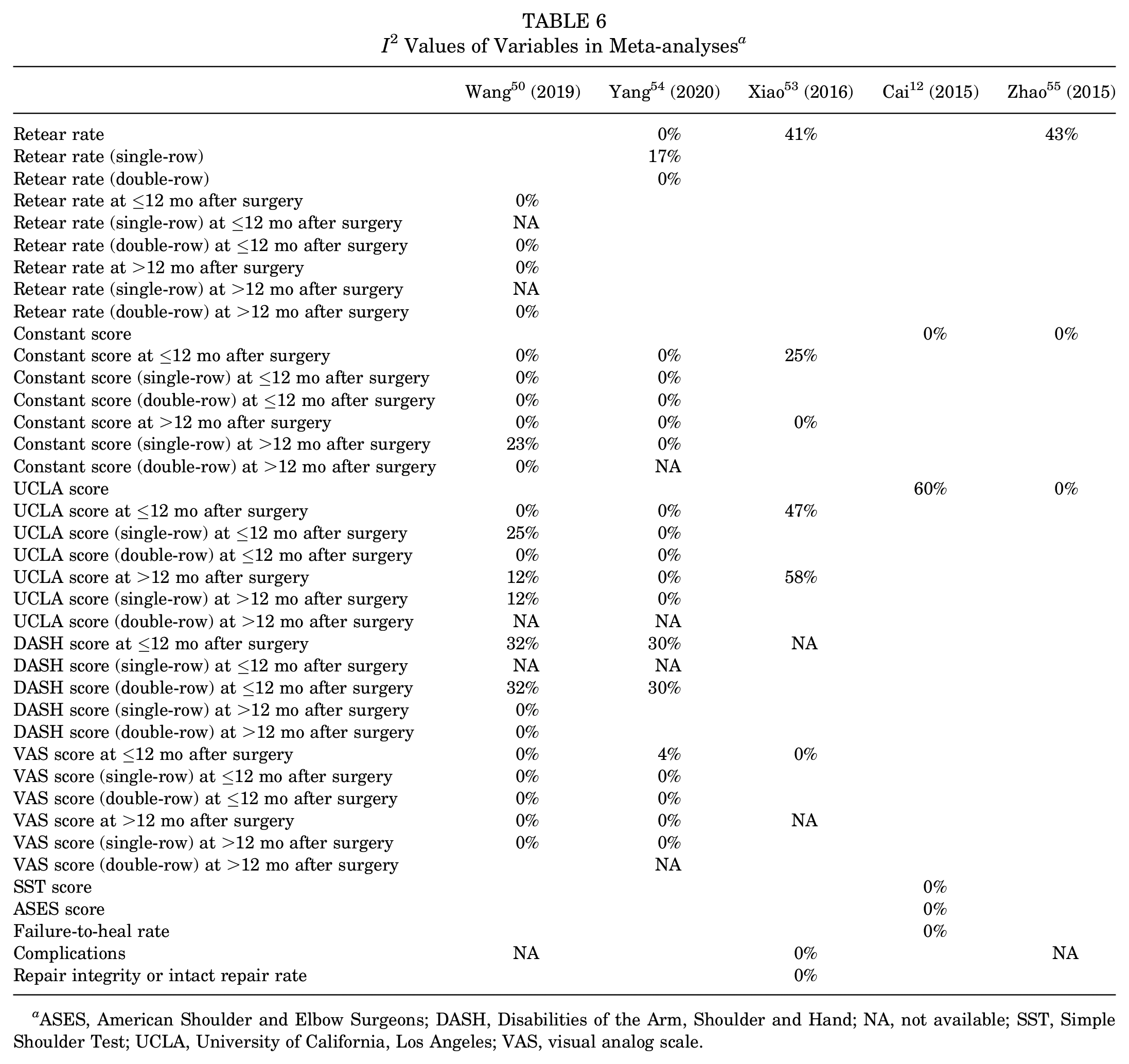
ASES, American Shoulder and Elbow Surgeons; DASH, Disabilities of the Arm, Shoulder and Hand; NA, not available; SST, Simple Shoulder Test; UCLA, University of California, Los Angeles; VAS, visual analog scale.
Jadad Decision Algorithm
The combined findings of the studies included are depicted in Figure 2. The Jadad decision algorithm was utilized to ascertain the most reliable evidence among the 5 meta-analyses included. Despite differences in the selection of primary studies, all meta-analyses addressed the same research question. The algorithm assessed the methodological quality of primary trials, individual patient data analysis, publication status, and language restrictions. In the end, the meta-analysis conducted by Wang etal 50 was determined to be of the highest quality based on the Jadad decision algorithm (Figure 3). This particular meta-analysis concluded that PRP injections effectively enhanced short-term (≤12 months after surgery) outcomes after arthroscopic repair of full-thickness rotator cuff tears, indicating superior clinical results with PRP in single-row fixation compared with other fixation methods.

Results of the included meta-analyses. ASES, American Shoulder and Elbow Surgeons; DASH, Disabilities of the Arm, Shoulder and Hand; SST, Simple Shoulder Test; UCLA, University of California, Los Angeles; VAS, visual analog scale.

Jadad decision algorithm.
Discussion
The major findings of our study demonstrated that the meta-analysis by Wang etal 50 was of the highest quality based on the Jadad decision algorithm among the included meta-analyses. This analysis showed that the short-term (≤12 months after surgery) retear rate and visual analog scale score were significantly lower in those with PRP than in those without PRP, while the short-term Constant score, short-term University of California, Los Angeles (UCLA) activity score, and long-term (>12 months after surgery) UCLA score were significantly higher in the PRP group, especially in single-row fixation. To the best of our knowledge, this study represents the first cross-sectional analysis of overlapping meta-analyses comparing the efficacy of arthroscopic rotator cuff repair with and without PRP.
The retear rate serves as a crucial metric in the treatment of rotator cuff tears, with inadequate tendon healing being a recognized factor in the occurrence of retears. 10 Tendon healing progresses through 3 stages: inflammation, proliferation, and remodeling. 49 Previous research has demonstrated that PRP can expedite wound healing by stimulating cell proliferation and differentiation,1,8,17,33 hence decreasing the short-term retear rate. Noteworthy improvements in short-term outcomes, including the Constant score, UCLA score, and DASH (Disabilities of the Arm, Shoulder and Hand) score, were observed in patients. Based on these results, substantial short-term therapeutic benefits were evident for patients, enabling early-stage functional exercises to mitigate severe joint stiffness.
In contrast to the findings of Wang etal, 50 some researchers12,53,55 revealed no significant differences between groups in the retear rate, Constant score, and UCLA score. This lack of distinction may stem from their focus on long-term outcomes during data extraction. Wang etal’s 50 study demonstrated significant short-term therapeutic benefits but no marked long-term efficacy differences. Similar conclusions were drawn by Yang etal. 54 Previous research has suggested that the long-term effect of PRP might be mitigated by the patient’s inherent healing capacity.18,21,37,40 Furthermore, tendon recovery to maximum strength typically occurs within 12 months after the injury, 9 potentially explaining why the efficacy of PRP application is less pronounced at long-term follow-up.
The efficacy of PRP injections varied across different surgical methods. Subgroup analyses revealed a notable effect of PRP in single-row fixation on both short-term Constant and UCLA scores, whereas only the short-term Constant score was influenced in double-row fixation. The limited auxiliary efficacy of PRP injections in double-row repair may be attributed to the stronger fixation strength with this technique, reducing gap formation and ensuring mechanical stability throughout the healing process. 54 Therefore, PRP injections can be recommended as adjunctive therapy in single-row repair.
The size of the tear plays a crucial role in rotator cuff healing.14,48 Because of insufficient studies reporting these outcomes, most research did not conduct subgroup analyses based on tear size. Cai etal 12 observed a notably lower failure-to-heal rate in the PRP group for mild-to-moderate tears compared with the control group; however, no difference was detected for severe-to-massive tears.
This study’s strengths lie in its emphasis on reviewing the highest quality of evidence by 2 independent reviewers. Additionally, the study excelled in determining optimal results through the utilization of a specific decision algorithm. The study also has some limitations. First, the literature search was restricted to English-language articles, leading to the exclusion of non-English studies, despite thorough searches across multiple databases. Second, our findings are constrained by the quality and inherent limitations of the included meta-analyses. Third, the follow-up duration in the included meta-analyses is short. Few meta-analyses, except for that by Wang etal, 50 discuss outcomes >24 months after surgery. Finally, even with 3 reviewers independently analyzing the selected meta-analyses, the bias is unavoidable in the application of the algorithm.
Conclusion
Our study demonstrates that the most reliable evidence suggests that PRP injections can be recommended as adjunctive therapy in single-row repair for enhanced short-term outcomes. Further high-quality RCTs are imperative to increase the strength of evidence.
Footnotes
Acknowledgements
The authors thank their colleagues for their cooperation with this study. They also thank the reviewers for their constructive criticism and suggestions.
Final revision submitted December 19, 2024; accepted January 21, 2025.
One or more of the authors has declared the following potential conflict of interest or source of funding: Support for this study was received from the Beijing Tongzhou District Science and Technology Plan Project (KJ2023CX067). AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Ethical approval was not sought for the present study.
