Abstract
Background:
Few studies have reported clinical outcomes and tendon healing rates after arthroscopic isolated subscapularis (SSC) repair (AISR).
Purpose/Hypothesis:
The primary purpose of this study was to evaluate clinical outcomes and tendon healing after AISR. It was hypothesized that AISR would result in satisfactory clinical outcomes along with a high rate of tendon healing at the midterm follow-up. The secondary purpose was to assess the influence of tear size and muscle atrophy on SSC tendon healing and patient-reported outcomes. It was hypothesized that both would be negatively correlated with healing but would have no effect on clinical outcomes .
Study Design:
Case series; Level of evidence, 4.
Methods:
A retrospective analysis was conducted on prospectively collected data for 77 patients who underwent primary AISR between 2011 and 2021 at a single institution, with a minimum 2-year postoperative follow-up for all patients. Functional outcomes were assessed using the American Shoulder and Elbow Surgeons (ASES) score, the Subjective Shoulder Value (SSV), and the visual analog scale for pain. Repair techniques and concomitant procedures were also collected. SSC tendon healing was evaluated via ultrasound at the final follow-up. Linear regression analysis was performed to determine factors affecting SSC healing.
Results:
The mean follow-up was 58.1 ± 3.3 months. ASES scores significantly improved from 41.5 to 81.6, and the SSV improved from 38.2 to 80.5 (
Conclusion:
Improved clinical outcomes and an overall high rate of tendon healing were seen at the midterm follow-up after AISR. Smaller tear sizes with less muscle atrophy were correlated with improved tendon healing. However, even when the tendon incompletely healed, the procedure improved functional outcomes.
Combined tears involving the subscapularis (SSC) tendon and other rotator cuff tendons are relatively common, with reported7,8,22 incidences ranging from 19% to 49%. However, isolated SSC tendon tears are less common, with incidences ranging1,24,32 from 6.4% to 10%.
The SSC plays a key role in the internal rotation of the glenohumeral joint. Tendon tearing can disrupt the transverse force couple and lead to shoulder dysfunction and pain.8,39 Since the initial 2002 study by Burkhart and Tehrany, 5 several subsequent articles have reported encouraging clinical outcomes after arthroscopic isolated SSC repair (AISR). 37 However, many of these studies were constrained by limited sample sizes; thus, further research on AISR is needed.9,25,29,37,41 This stands in contrast with the extensive research focused on healing and retear rates after arthroscopic repair of posterosuperior cuff tears.
The present study aimed to evaluate the clinical and structural outcomes after AISR. The hypothesis was that AISR would result in satisfactory clinical outcomes along with a high rate of tendon healing at the midterm follow-up. The secondary purpose was to assess the influence of tear size and muscle atrophy on SSC tendon healing and patient-reported outcomes (PROs). We hypothesized that both would be negatively correlated with healing but would have no effect on clinical outcomes.
Methods
Study Design
A retrospective study was conducted on prospectively collected data on patients who underwent AISR between 2011 and 2021 at a single institution. The inclusion criteria were as follows: primary repair; baseline PROs; preoperative magnetic resonance imaging (MRI) scans ; and minimum 2-year follow-up data. Patients with a history of previous ipsilateral shoulder surgery, concomitant posterosuperior rotator cuff and SSC repair, proximal humerus fracture or glenoid fracture, inaccessible MRI scans or insufficient images for evaluation, inaccessible or incomplete physical examination record, or incomplete intraoperative documentation were excluded from this study. Institutional review board approval was obtained before commencing the study, and all included patients provided written informed consent. Patients who met the inclusion criteria were contacted for a clinical and ultrasound follow-up assessment of rotator cuff healing .
Preoperative MRI Evaluation
All MRI scans were performed at a single institution with a 1.5-T magnet and the arm in a neutral position. No intra-articular or intravenous gadolinium was administered. The Goutallier classification for fatty infiltration was documented preoperatively by a single high-volume fellowship–trained shoulder surgeon (P.J.D.) for each rotator cuff muscle on T1-weighted sagittal MRI using the most lateral image where the scapular spine connects with the body of the scapula.6,45 This classification system consists of 5 grades, scored from 0 to 4, with grade 0 indicating the absence of fat, grade 1 indicating the presence of some fatty streaks, grade 2 indicating a higher proportion of muscle compared with fat, grade 3 indicating an equal presence of fat and muscle, and grade 4 indicating a higher proportion of fat compared with muscle. The SSC was also divided into the upper and lower halves for grading based on the division described by Lädermann et al. 23
The coracohumeral distance was evaluated by measuring the narrowest distance between the cortical border of the coracoid and the cortical border of the humeral head on T2-weighted axial images obtained from MRI scans, following the criteria established by previous studies.27,33 The axial images were set at the point where the subcoracoid space was at its narrowest. Measurements were made by a single orthopaedic surgeon (A.I.K.). Three measurements were recorded, and the mean was taken for analysis.
Surgical Technique and Arthroscopic Findings
All arthroscopic procedures were performed by a single surgeon (P.J.D.). Patients were positioned in the lateral decubitus position, and conventional portals (posterior, anterosuperior, and lateral) were used. SSC tendon integrity was evaluated from the posterior viewing portal with 30° and 70° arthroscopes. SSC tear type was documented intraoperatively according to the Lafosse classification24,35 (types 1-5) and SSC tear size as a percentage (% cephalad to caudal). In addition, the integrity of the long head of the biceps tendon (intact, subluxated, partial tear, or complete tear) was reported.24,35
After an arthroscopic examination of the joint, biceps tenodesis was performed in the bicipital groove on patients with impaired biceps sling or biceps pathology on the physical examination or imaging. The width of the subcoracoid space was evaluated. Coracoplasty was performed if the subcoracoid space was intraoperatively narrowed (<7 mm) or if a coracoid spur was present. In the early phase of the study, a knotted single-row technique was employed for SSC repairs, while a knotless technique was utilized for more recent repairs. In the current technique, a single-row knotless configuration was applied for LaFosse type 1 and 2 tears using either soft or hard anchors. In addition, for LaFosse type 3 and 4 tears, a double-row knotless technique was used, utilizing either soft or hard anchors in the medial row and hard anchors in the lateral row. A limited acromioplasty with preservation of the coracoacromial ligament was routinely conducted, except in patients who were young and had a flat acromion. All tears were fully repairable at the time of surgery.
Postoperatively, the arm was immobilized in a sling for 4 weeks for tears ≤50% of the footprint and 6 weeks for tears >50% of the footprint. After sling discontinuation, patients could engage in passive external rotation and forward flexion. Two weeks after sling discontinuation, self-assisted active range of motion (ROM) exercises were encouraged. Strengthening exercises and passive internal rotation ROM were initiated at 3 months postoperatively, with a full return to activity, including sports activities, allowed at 6 months.
Ultrasound Examination
The ultrasound evaluation was performed by an orthopaedic surgeon (A.I.K.) trained in shoulder ultrasound with 4 years of experience in shoulder surgery, who was blinded to tear size and repair technique. Tendon healing was graded using the Barth et al 2 modification of the Sugaya classification for ultrasound assessment of rotator cuff repair, in which grade 1 designates tendons with sufficient thickness and normal structure, grade 2 indicates sufficient thickness with partial hypoechogenicity, grade 3 indicates insufficient thickness without discontinuity, grade 4 repairs demonstrate minor discontinuity in the tendon, and grade 5 repairs demonstrate major discontinuity. Repairs of grades 1 to 3 were considered healed.2,18
Isometric Muscle Strength Measures
Isometric strength measurements were conducted by the same surgeon who performed the ultrasound evaluation (A.I.K.) using a manual muscle testing dynamometer with the patient in the standing position. The strength of the SSC muscle was evaluated using the belly press (BP) test. The patient was instructed to press the hand dynamometer between the palm and abdomen during the test. To assess external rotation strength, the participants’ elbows were flexed at a 90° angle, their arms were positioned at the side, and strength was measured with the hand dynamometer placed on the dorsal aspect of the forearm, 2 cm proximal to the ulnar styloid process. To determine the constant strength, the patients’ arms were positioned at 90° of forward flexion, with their elbows fully extended and their forearms in a half-pronation position. The hand dynamometer was placed on the dorsal aspect of the forearm, approximately 2 cm proximal to the ulnar styloid process. For each participant, the mean of 3 independent measurements was taken.
Study Variables
Patient characteristics—including age, sex, tobacco use, and length of follow-up—were collected. The status of the traumatic or nontraumatic injuries was collected from patient records. The Charlson Comorbidity Index (CCI), which includes 17 different comorbidities associated with mortality and assigns weights ranging from 1 to 6 points (score range, 0 to 29), was used to standardize comorbidities, and the CCI score as a percentage was calculated 30 by dividing the patient’s score by 29.
Active ROM and PRO values were documented at the baseline and the final follow-up. ROM measurements included forward flexion, external rotation at the side, and internal rotation recorded by the treating surgeon (P.J.D.) or a physician assistant. Internal rotation was numerically scaled based on the nearest spinal level achieved with the thumb (T10 = 10, T12 = 12, L2 = 14, L4 = 16, S1 = 18, and hip = 20). PROs included the American Shoulder and Elbow Surgeons (ASES) shoulder score, the visual analog scale (VAS) for pain, and the Subjective Shoulder Value (SSV). The rates of patient satisfaction with the surgery and return to activity were also recorded at the final follow-up. Complications and revision surgeries were recorded for analysis.
Statistical Analysis
Categorical variables were characterized using absolute and proportional frequencies, whereas continuous variables were described by means and standard deviations. The statistical analysis included the chi-square test to assess associations among categorical variables, and the
PRO scores, ROM measurements, patient satisfaction, and return to activity were compared from pre- to postoperatively for the overall cohort. These variables—as well as postoperative strength—were also compared between SSC tendons considered as healed (modified Sugaya grades 1-3) versus unhealed in the patients who underwent ultrasound assessment at the final follow-up. Linear regression analysis was used to identify which dependent and independent variables influenced SSC healing. SPSS Version 25 (IBM Corp) and MedCalc Version 20 (MedCalc Software Ltd) software programs were used to evaluate the data. A threshold of .05 was used to denote statistical significance.
Results
A total of 163 AISR procedures were performed during the study period, of which 77 patients met the study criteria. In addition, 40 patients were available for postoperative ultrasound assessment of isolated SSC repair integrity (Figure 1). There was a male predominance (63.6%; n = 49). The mean follow-up period was 58.1 ± 3.3 months (range, 23-138 months). Regarding repair constructs, single-row knotted repair was performed on 22 (28.6%) patients, single-row knotless repair was performed on 32 (41.6%) patients, and double-row knotless repair on 23 (29.9%) patients. Baseline characteristics of the study patients are summarized in Table 1.

Flowchart of patient enrollment in the study. AISR, arthroscopic isolated subscapularis repair; US, ultrasound.
Baseline Characteristics of Patients After Arthroscopic Isolated SSC Repair (N = 77 Patients) a
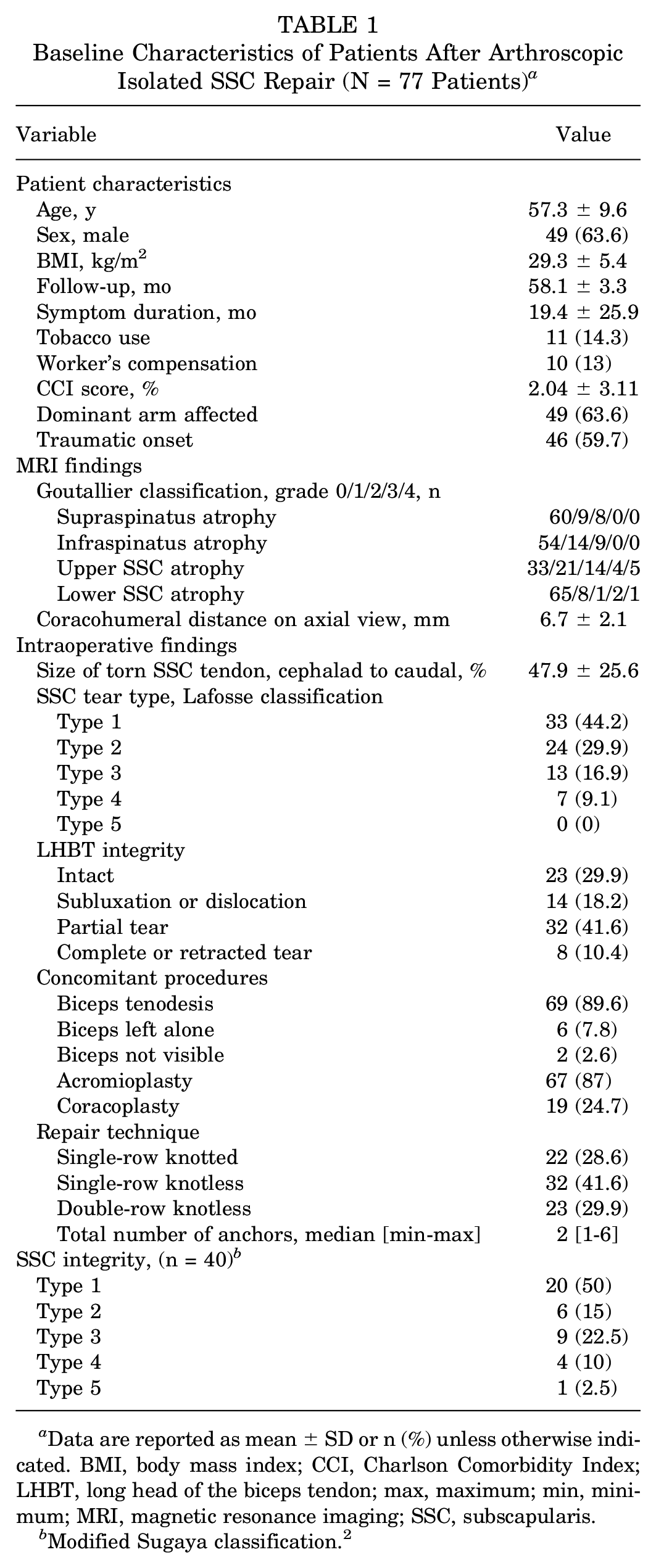

Data are reported as mean ± SD or n (%) unless otherwise indicated. BMI, body mass index; CCI, Charlson Comorbidity Index; LHBT, long head of the biceps tendon; max, maximum; min, minimum; MRI, magnetic resonance imaging; SSC, subscapularis.
Modified Sugaya classification. 2
Functional Outcomes
All PRO scores and ROM measurements improved significantly from the baseline to the final follow-up (
Pre- to Postoperative Changes in PRO Scores and ROM a

Data are reported as mean ± SD or mean (95% CI). Boldface
At the final follow-up, the self-reported patient satisfaction rate was 90.9% (n = 70), and return to activity was reported in 85.7% (n = 66) of patients.
Tendon Healing
Of the 77 study patients, 40 underwent ultrasound assessment at the final follow-up. Within these patients, 35 (87.5%) repairs were classified as healed, and 5 (12.5%) were classified as unhealed (Figure 2). PROs improved significantly from pre- to postoperative periods in both groups (
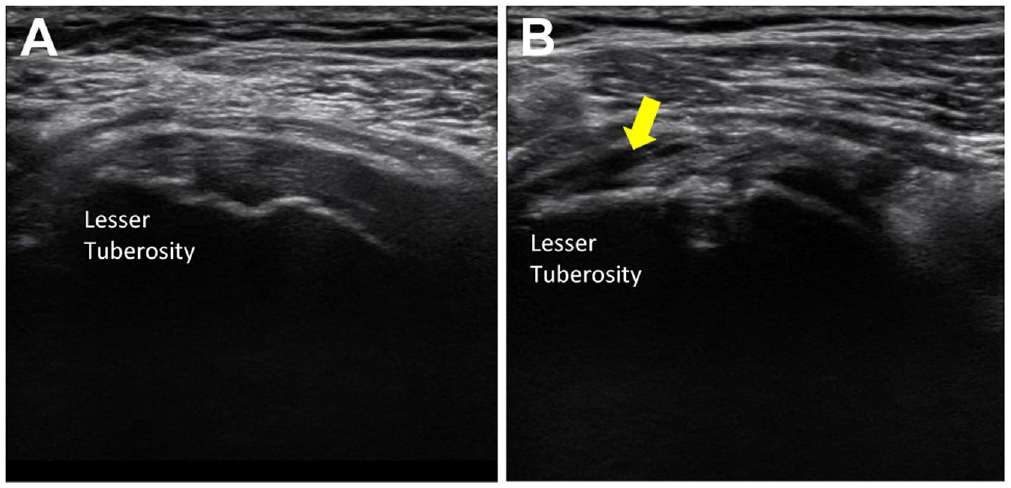
Postoperative images of the SSC tendon with arthroscopic repair. (A) The healed state of the SSC with tendon continuity up to its footprint (lesser tuberosity). (B) The unhealed (retear) state of the SSC, with a monitored hypoechoic field in the lesser tuberosity. The arrow indicates the tear location. SSC, subscapularis.
Comparison of Pre- to Postoperative Changes in PRO Scores and ROM Between the Healed (n = 35) and Unhealed (n = 5) SSC Groups a

Data are reported as mean ± SD or mean (95% CI). Bold
Comparison of Postoperative Strength, Satisfaction, and Return to Activity Between the Healed (n = 35) and Unhealed (n = 5) SSC Groups a

Data are reported as mean ± SD or n (%) unless otherwise indicated. Bold
Factors Associated With SSC Healing
The association of SSC repair healing with Goutallier grade, Lafosse classification, and repair construct are shown in Table 5. As SSC muscle atrophy increased, the healing rate decreased. Furthermore, SSC healing decreased progressively from Lafosse type 1 to type 4 tears. There were no significant differences between the healed and unhealed groups when linking postoperative PROs to Goutallier grades (
Rate of SSC Healing According to Goutallier Classification, Lafosse Classification, and Repair Construct a

Data are reported as mean ± SD or n. Dashes indicate areas not applicable. Bold
Risk Factors for SSC Healing According to Linear Regression Analysis a
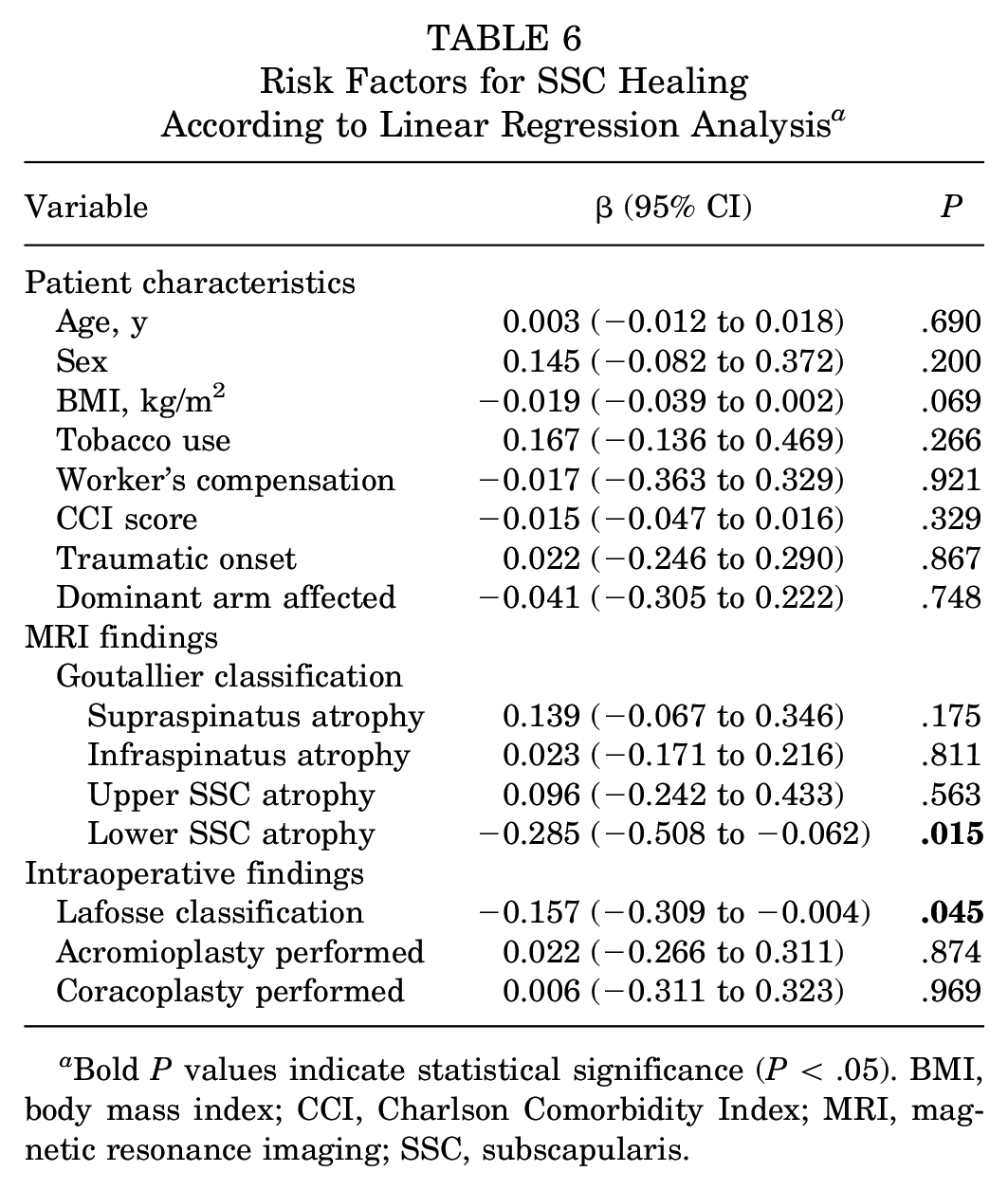
Bold
Complications
Three complications were observed in the study patients. One patient experienced an early anchor pullout, which was arthroscopically revised at 3 months postoperatively. Another patient underwent arthroscopic lysis of adhesions for stiffness at 8 months postoperatively. In the third patient, a subpectoral biceps tenodesis was performed because of a biceps rupture after initial arthroscopic tenodesis at 25 months postoperatively.
Discussion
The major findings of this study were that AISR led to significant improvements in both clinical outcomes and ROM at a mean midterm follow-up. There were no statistical differences in pre- to postoperative PROs and ROM changes between different repair constructs. Postoperative healing was achieved in nearly 90% of patients, although larger tears and greater muscle atrophy were associated with an increased risk of failure. There was no statistical difference in pre- to postoperative PROs changes between the healed and unhealed repair structures.
Isolated SSC tears are relatively rare compared with posterosuperior cuff tears, and there is limited research on isolated SSC repairs in the literature.1,32,36,37 Since the study by Burkhart and Tehrany 5 on AISR, subsequent studies have consistently demonstrated significant improvements in PROs and ROM,4,14,16,24,34 which align with the findings from our study. Among previous studies, Seppel et al 38 and Liu et al 28 presented long-term outcomes after the repair of isolated SSC tears, with mean follow-up times of 98.4 and 120 months, respectively, while our study presents midterm follow-up results (56.7 ± 3.3 months) in the largest sample size36,37,41 of patients (N = 77). In addition, satisfaction and return to activity rates reported by patients in our study were 90.9% and 85.7%, respectively. These results suggest that AISR has consistently shown clinical improvement.
We conducted an ultrasound assessment on 40 of the study patients to assess SSC tendon healing. An 87.5% healing rate was observed, which is consistent with the rates of 83% to 100% reported in the literature.20,21,31,42 Previous studies comparing tear size and healing rates have found higher retear rates in larger tears.19,31 Similarly, in the present study, all Lafosse type 1 and 2 tears healed completely, while approximately 50% of type 3 and 4 tears failed to heal, aligning with previous findings. Yoon et al
44
reported a retear rate of 78.6% in a consecutive case series of isolated SSC repairs with Goutallier grades 3 and 4 atrophy. Despite this high retear rate, they observed significant improvement in the ASES (by 31.6 ± 9.1 points;
Studies have consistently demonstrated an increase in internal rotation force after AISR.3,13,24 Lafosse et al
24
assessed pre- and postoperative BP strength on a scale of 0 to 5 in 17 patients after AISR and noted a significant postoperative increase (2.4 vs 4.5;
Because of the absence of preoperative data, our strength assessment was limited to postoperative comparisons. According to our findings, the group with healed SSC exhibited nearly double the postoperative strength compared with the unhealed group (mean BP strength: 9.4 vs 4.9 kg;
Two studies have compared single- versus double-row SSC repair techniques.17,43 In the study by Yoon et al
43
on patients with isolated full-thickness SSC tears, 31 patients underwent single-row repair and 25 patients had a double-row repair. They did not find any differences in the ASES (91 vs 91.4;
Limitations
There are several limitations to the present study. First, because of its retrospective design, not all patients had complete data for analysis. Second, the ultrasound assessment of tendon healing was only conducted on 40 out of the 77 patients. This may have introduced bias. Furthermore, the sample size might have affected the study’s statistical power to more accurately detect differences in tendon healing and functional outcomes. Tendon healing was assessed using only ultrasound assessments, with no concomitant additional validation using MRI or computed tomography angiography. However, ultrasound has been verified to be equivalent or even superior to MRI in evaluating rotator cuff tears.12,46 The postoperative healing status of only the SSC tendon was assessed; ultrasound was not used to evaluate the final status of the other supraspinatus and infraspinatus tendons. During the follow-up period, new tears may have developed, extending into the other cuff tendons (supraspinatus and infraspinatus), potentially influencing the study results. A single orthopaedic surgeon performed ultrasound evaluations, and the results were subject to the experience and skill of the ultrasound operator. However, ultrasound evaluation in rotator cuff tears has shown high interobserver validity across studies.26,40 This suggests that while the skill and experience of the evaluator can play a role in the accuracy of the results, ultrasound remains a reliable method for assessing rotator cuff tears because of its consistent findings among different observers.11,46
Conclusion
AISR improves clinical outcomes and results in an overall high rate of tendon healing at a mean midterm follow-up. Smaller tear sizes with less muscle atrophy are correlated with improved tendon healing. However, even when the tendon incompletely healed, the procedure improves functional outcomes.
Footnotes
Final revision submitted November 22, 2023; accepted December 6, 2023.
One or more of the authors has declared the following potential conflict of interest or source of funding: T.P. has received education payments from SportsTek Medical. M.E.M. has received education payments from Arthrex and Steelhead Surgical; consulting fees from Arthrex; and hospitality payments from Stryker, Encore Medical, Medical Device Business Services, and Smith & Nephew. P.J.D. has received education payments from Steelhead Surgical; consulting fees from Arthrex, Pacira Pharmaceuticals, and Integer Holdings; nonconsulting fees from Arthrex; and royalties from Arthrex. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Ethical approval for this study was obtained from the Southern Oregon Institutional Review Board (ref No. 22-008).
