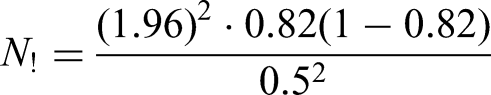Abstract
Introduction
For people living with HIV (PLHIV) who are on second-line antiretroviral therapy (ART), attaining viral resuppression is vital to support immune recovery, avoid antiretroviral resistance, and lower HIV-associated morbidity, mortality, and onward transmission. However, evidence on the level of resuppression and its determinants in Ethiopia is limited.
Objective
To assess the viral resuppression rate and identify predictors among PLHIV on second-line ART at Gondar Comprehensive Specialized Hospital, Northwest Ethiopia.
Methods
An institution-based retrospective cohort study was conducted at the ART clinic of the University of Gondar Comprehensive Specialized Hospital from November 2021 to May 2022. Patient charts of 385 individuals receiving second-line ART were selected with simple random sampling technique. A validated questionnaire adopted from previous studies was used for data collection from patient records at the ART clinic. Collected data were entered into EpiData version 3.1 and analyzed using Stata version 14. Viral resuppression was defined as a viral load of <1000 copies/mL. In the statistical analysis, variables with a P-value < .20 in the bivariate analysis were included in the multivariable Cox proportional hazards regression model to identify independent predictors of viral resuppression.
Results
Out of the 385 patient charts initially selected, five charts were excluded because they had incomplete or missing key variables required for the study analysis. Therefore, the final analysis was conducted on 380 complete patient charts. The median age of the study participants was 41.41 years with an interquartile range (35.0-48.0). In the follow-up period, 297 patients (78.16%; 95% CI: 73.90-82.33) achieved viral resuppression. In multivariable Cox proportional hazards regression analysis, the factors significantly associated with viral resuppression were alcohol consumption (adjusted hazard ratio [AHR] = 1.55; 95% CI: 1.09-2.21), smoking (AHR = 1.49; 95% CI: 1.04-2.13), baseline viral load (AHR = 5.60; 95% CI: 2.07-15.12), good medication adherence (AHR = 1.63; 95% CI: 1.02-2.61), and history of drug substitution (AHR = 1.32; 95% CI: 1.02-1.72).
Conclusion and Recommendations
This study demonstrated that the viral resuppression rate among people living with HIV receiving second-line ART at Gondar Comprehensive Specialized Hospital remains low. Viral resuppression was significantly associated with alcohol consumption, smoking, medication adherence, prior drug substitution, and baseline viral load. Strengthening adherence support, minimizing unnecessary drug substitutions, and providing targeted follow-up for high-risk patients are critical to improving treatment outcomes.
Plain Language Summary Title
How Well HIV Patients Respond to Second-Line Treatment and What Factors Affect Their Recovery at Gondar Hospital, Ethiopia
Plain Language Summary
People living with HIV sometimes need to switch from their first HIV medicines to a second set of medicines when the first treatment stops working. This study looked at patients at Gondar Comprehensive Specialized Hospital in Ethiopia who were on second-line HIV treatment. We wanted to find out how many patients were able to get their virus under control again (“viral resuppression”) and what factors helped or made it harder for them to do so.
We reviewed the medical records of patients who had been on second-line treatment. Our results showed that most patients were able to control the virus again after switching to second-line therapy. Patients who followed their treatment plan well, switched to second-line medicines promptly, and did not have other illnesses like tuberculosis were more likely to achieve viral resuppression.
This information is important because it helps doctors understand what supports patients need to successfully manage HIV on second-line treatment. By focusing on adherence, timely treatment, and managing other health problems, more patients can achieve better health outcomes.
Introduction
HIV remains a significant public health burden in Ethiopia, with prevalence among people of reproductive age ranging from 0.1% to 4.8% in 2018.1,2 The expansion of antiretroviral therapy (ART) has markedly reduced HIV-related morbidity and mortality. 3 However, treatment failure of first-line ART and the subsequent need for second-line regimens are increasingly reported, posing new challenges for long-term HIV care.
What Is Known?
Globally and across sub-Saharan Africa, the demand for second-line ART is rising as ART programs mature. Modeling studies estimate that by 2030, up to one-fifth of people living with HIV (PLHIV) in Africa may require second-line therapy. 4 Viral resuppression following initiation of second-line ART is a key indicator of treatment success, with reported rates ranging from 41% to 83.1%. The World Health Organization (WHO) recommends routine viral load (VL) monitoring as the preferred method for assessing ART response, as unsuppressed VL is associated with increased risks of disease progression, HIV transmission, and mortality.5,6 Previous studies have identified predictors of viral resuppression, including timely regimen switching, higher baseline CD4 count, lower baseline VL, absence of drug substitutions, and selected demographic and clinical characteristics.3,7–9 A 2024 synthesis of 21 Ethiopian studies showed a pooled virological suppression rate of ∼71% and identified poor adherence, BMI, disclosure, and opportunistic infections as predictors.10–14
What Is Unknown?
Despite these insights, much of the existing evidence is derived from settings where VL monitoring is inconsistent or where treatment outcomes are assessed using immunological or clinical failure criteria rather than virological measures. These approaches have limited diagnostic accuracy and may not reflect true treatment response. Furthermore, the influence of nonclinical factors such as behavioral and treatment-related characteristics on viral resuppression has been insufficiently examined, particularly in low-income and resource-limited settings.15,16
For PLHIV who are on second-line ART, attaining viral resuppression is vital to support immune recovery, avoid antiretroviral resistance, and lower HIV-associated morbidity, mortality, and onward transmission.17,18 In settings where routine viral load testing is unavailable or limited, healthcare providers often rely on clinical and immunological criteria to identify antiretroviral treatment failure and guide decisions about switching ART regimens. However, these criteria have low diagnostic accuracy for virological failure, potentially resulting in inadequate adherence support, prolonged use of ineffective regimens, or unnecessary switching to second-line ART. Even in settings where VL testing is available, its clinical utility is compromised if results are not integrated into patient management.5,19,20
However, evidence on the level of resuppression and its determinants in Ethiopia is limited. Available studies are limited in number and often lack a comprehensive evaluation of both clinical and nonclinical determinants using virological outcomes. This gap restricts evidence-based decision-making and optimization of second-line ART management. Therefore, this study aimed to determine the rate of viral resuppression and identify its predictors among PLHIV on second-line ART in Ethiopia, thereby providing context-specific evidence to guide clinical practice and programmatic interventions.
Method
Study Design and Period
An institution-based retrospective cohort study was conducted at the ART clinic of the University of Gondar Comprehensive Specialized Hospital from November 2021 to May 2022. The study included PLHIV enrolled from January 1, 2018, to December 31, 2021.
Study Area
The University of Gondar Comprehensive Specialized Hospital has chronic follow-up centers for managing chronic diseases such as HIV/AIDS, hypertension, and cardiac diseases. HIV care is an integral part of the chronic disease management program, with routine ART services provided by a dedicated care team for over 20 years. The hospital initiated ART services in 2005, enrolling over 7500 adults since then. Currently, more than 4900 adults are actively receiving care at the hospital.
Source Population
All PLHIV who registered at the ART follow-up clinic of the University of Gondar Comprehensive Specialized Hospital were the source population.
Study Population
PLHIV who were on second-line ART who had follow-up visits from January 1, 2018, to December 31, 2021, were the study population.
Inclusion Criteria
All PLHIV who were on second-line ART who were registered in the adult ART follow-up clinic during the study period were included.
Exclusion Criteria
Patients who had been on second-line ART for less than 6 months or who had no viral load measurement after initiating second-line therapy were excluded.
Sample Size Determination
The sample size was determined based on the study objectives. The calculation was informed by a retrospective follow-up study conducted in Dessie, which reported a viral resuppression rate of 82.39% among people living with HIV on second-line ART. In that study, being on anti-tuberculosis treatment and timely switching to second-line ART were identified as statistically significant predictors. For the first objective, the sample size was calculated using a single population proportion formula, assuming a 95% confidence interval and a 5% margin of error:
The final calculated sample size with 10% for incomplete data was 244. For the second objective, the sample size was calculated using a double population proportion formula to assess predictors of viral resuppression. The assumptions included a 95% confidence level, 80% power, and a 1:1 ratio of exposed to unexposed participants:
Using EpiData statistical software version 7, the maximum calculated sample size for the second objective was 385 participants. To ensure adequate power for both study objectives, the larger sample size obtained from the two calculations was selected. Accordingly, the final sample size for this study was 385 participants.
Sampling Technique
Medical charts of patients enrolled in the ART follow-up clinic with HIV/AIDS from January 1, 2018, to December 31, 2021, were used as the sampling frame. The medical registration numbers of all eligible patients were first listed, and then charts were selected using simple random sampling (SRS) to ensure that each patient had an equal chance of being included in the study. Patients with incomplete or missing key information were excluded.
Operational Definitions
Viral re-suppression: Was defined as a viral load of < 1000 copies/mL after at least 6 months of second-line ART. 16
Body mass index (BMI): Was classified per CDC standards as underweight (<18.5 kg/m2), normal weight (18.5-24.9 kg/m2), and overweight (25-29.9 kg/m2). 21
Timely switch: Defined as switching to second-line ART after confirmed virological failure (VL ≥1000 copies/mL) following enhanced adherence support (EAS) per WHO guidelines. Delayed switch refers to switching later than this standard. 5
Medication adherence: Assessed from patient follow-up forms filled by healthcare providers. Good adherence: ≥95% of prescribed medication taken; fair adherence: 85% to 94%; poor adherence: <85%. 5
Censored: Patients who were lost to follow-up, died, or failed to achieve viral suppression during the study period.
Data Collection Tools and Procedures
A validated questionnaire adopted from previous studies was used for data collection from patient records at the ART clinic. The checklist contains socio-demographic, behavioral, baseline clinical, and treatment-related factors. Forms used for laboratory requests, ART registration logbook, and patient cards were reviewed. Data were collected by two BSc nurses who were trained in medical record abstraction and study procedures. A health officer supervised the data collection process to ensure accuracy, completeness, and adherence to the study protocol. To protect patient information, all data were de-identified prior to analysis. Unique codes were assigned to each participant, and personal identifiers (names, medical record numbers, or contact information) were removed. Electronic data were stored on password-protected computers with access restricted to the study team. No identifiable information was shared with third parties. During the data collection period, the medical record number of patients were obtained from the logbook, and charts were selected using a simple random sampling method. Data were then extracted from the selected patient charts using a preprepared checklist. To prevent additional recollection of data, a commonly agreed code by data collectors was given after reviewing and collecting data from each patient's chart. The outcome of each patient was dichotomized as censored or viral resuppressed.
Data Quality Control
For data quality, a validated questionnaire was used. The data collection questionnaire was pretested for consistency and completeness on 38 patient charts at the same hospital before the actual data collection, and these charts were included in the study. Three-day training was given for data collectors for the description of the questionnaire and the way they collect data from the patient chart. Each component of the questionnaire was discussed clearly for the data collectors. The data collection process was monitored closely by the supervisor. Because this study was based on a retrospective review of routinely collected clinical records, missing or incomplete data were anticipated. To account for potential data loss, the initial sample size was increased by 10% when calculating the final sample size. Prior to analysis, the dataset was carefully assessed for completeness. Records with missing outcome variables (viral load resuppression status) or key exposure variables were excluded from the final analysis. For variables with minimal missing values, complete-case analysis was performed. No statistical imputation was conducted, as the proportion of missing data was small and assumed to be missing at random. Data cleaning and consistency checks were undertaken to minimize entry errors and ensure data quality before statistical analysis.
Data Processing and Analysis
Collected data were entered into EpiData version 3.1 and analyzed using Stata version 14. Descriptive statistics summarized socio-demographic, behavioral, clinical, and treatment-related variables. The incidence rate of viral resuppression was calculated using person-time observations and expressed per 100 person-months. The log-rank test and Kaplan-Meier survival curves compared survival probabilities across groups. Model fitness was assessed using Schoenfeld residuals for proportional hazards assumption (P = .7672) and the Cox-Snell residual technique for goodness-of-fit (Figure 1).

Cox-Snell residual plot for the Cox proportional hazards model among people living with HIV (PLWH) on second-line ART at Gondar Comprehensive Specialized Hospital, January 1, 2018, to December 31, 2022 (n = 380).
Potential confounders were identified a priori based on clinical relevance and evidence from previous literature. In the statistical analysis, variables with a P-value < .20 in the bivariate analysis were included in the multivariable Cox proportional hazards regression model to identify independent predictors of viral resuppression. Adjusted hazard ratios (AHRs) with 95% confidence intervals (CIs) were determined, and variables with P-values below .05 in the multivariable analysis were deemed statistically significant.
Ethical Approval
The study was first approved by the Institutional Review Board (IRB) of the University of Gondar, College of Medicine and Health Sciences, School of Medicine (Ref No. 478/14) from the University of Gondar, and ethical clearance was obtained. Upon this clearance, additional written permission to conduct the study on the medical records of PLHIV was obtained from the coordinator of the chronic clinic follow-up of the University of Gondar Comprehensive Specialized Hospital. Confidentiality of information was maintained through refraining from recording the patient's name in the used chart. Written informed consent was obtained from all participants prior to participation in the study, in accordance with COPE guidelines.
Results
Socio-Demographic Related Factors
Out of the 385 patient charts initially selected, five charts were excluded because they had incomplete or missing key variables required for the study analysis (eg, baseline viral load, ART regimen history, or outcome data). Therefore, the final analysis was conducted on 380 complete patient charts. Of these, 53.42% were male. The median age of the study participants was 41.41 years with an interquartile range (35.0-48.0). More than half of the participants (52.63%) were married, and the majority (82.11%) resided in urban areas. Regarding occupation and education, 25% were employed in private jobs, and 32.89% had attained secondary education.
Clinically, 40 participants (10.53%) had a history of psychiatric illness. Substance use was reported as follows: 20.53% had a history of alcohol use, 13.16% had used khat, and 20.53% were smokers. Immunologically, 142 participants (37.37%) had a baseline CD4 count of less than 200, and 77 participants (20.26%) had received FPT (fluconazole prophylaxis therapy). Nutritionally, 69 participants (18.16%) had a BMI below 18.5 kg/m2. Additionally, 143 participants (37.63%) had a history of opportunistic infections (Table 1).
Psychological and Behavioral Characteristics Profile of People Living With HIV (PLHIV) on Second-Line Antiretroviral Therapy at Gondar Comprehensive Specialized Referral Hospital, Northwest Ethiopia, December 2018–January 31, 2021 (n = 380).

Rate of Viral Resuppression
A total of 380 patients were monitored over 5324.93 person-months. The median time to achieve viral resuppression was 10.1 months (SD = 10.74), with follow-up periods ranging from 1.17 to 56.8 months. During the follow-up period, 297 patients (78.16%; 95% CI: 73.90-82.33) achieved viral resuppression. The overall incidence rate was 5.57 per 100 person-months of observation.
Predictors of Viral Resuppression
In the bivariate analysis, variables with a P-value <.2 were selected for inclusion in the multivariable Cox proportional hazards model to identify predictors of viral load resuppression. The bivariate analysis identified several potential predictors, including alcohol consumption, smoking, psychiatric illness, viral load, medication adherence, drug substitution, and history of drug side effects. After adjusting for potential confounders in the multivariable model, the independent predictors of viral load resuppression among people living with HIV (PLHIV) on second-line therapy were: alcohol consumption [AHR: 1.55; 95% CI: 1.09-2.21], smoking [AHR: 1.49; 95% CI: 1.04-2.13], baseline viral load [AHR: 5.6; 95% CI: 2.07-15.12], medication adherence [AHR: 1.63; 95% CI: 1.02-2.61], and history of drug substitution [AHR: 1.32; 95% CI: 1.02-1.72] (Table 2).
Multivariable Regression Analysis on Predictors of Viral Resuppression Among PLHIV Second-Line Therapy at Chronic Follow-Up Clinic of Gondar Comprehensive Specialized Referral Hospital, From January 1, 2018, to December, 2021.

Abbreviations: PLHIV, people living with HIV; CHR, crude hazard ratio; ART, antiretroviral therapy; CI, confidence interval.
* Significant predictors of viral resuppression at P-value <.05.
Discussion
Although numerous studies in Ethiopia and other African settings have investigated virological suppression on first-line ART, few have determined the time to viral resuppression and its predictors after confirmed virologic failure on second-line regimens. This study provides updated real-world evidence from northwest Ethiopia, identifying key clinical and behavioral factors associated with resuppression. These findings offer context-specific insights that can inform targeted adherence interventions and optimize second-line ART management in similar resource-limited settings. Unsuppressed viral load is a major risk factor for morbidity and mortality among PLHIV. This study investigated viral resuppression and its predictors among PLHIV on second-line ART at Gondar Comprehensive Specialized Hospital, Northwest Ethiopia. Five factors were identified as significant predictors of viral resuppression: alcohol consumption, smoking, medication adherence, history of drug substitution, and baseline viral load. Overall, the rate of viral resuppression among participants was 78.16% (95% CI: 73.9%-82.33%), with a median survival time of 10.1 months. These findings align with similar studies conducted in India 77.2% 22 and South Africa. 23
However, the findings of this study showed that the rate of viral load resuppression was lower than reported in studies from Rwanda, 83%, 24 Ethiopia, 82.9%, 3 and South Africa, 83.1. 25 The discrepancy might be, due to the differences in sample size, socio-demographic characteristics, duration of follow-up, and study settings. The finding of the study was higher than in a study done in South Africa 56.5%, 26 South Africa 77%, 27 and Nigeria77%. 28
The rate of viral load resuppression observed in this study (78.16%) reflects both shared and context-specific determinants of treatment outcomes across low- and middle-income settings. While the findings are comparable to those reported from India and South Africa, important contextual differences may explain the observed variations between Ethiopia and other settings such as Rwanda, South Africa, and India. In Ethiopia, limited and sometimes delayed access to routine viral load testing, particularly in resource-constrained and peripheral health facilities, may contribute to slower identification of virologic failure and delayed clinical action. In contrast, countries such as Rwanda and South Africa have more established viral load monitoring systems with broader laboratory coverage, faster turnaround times, and stronger linkage between laboratory results and clinical decision-making, which may facilitate earlier interventions and higher rates of viral resuppression.
Health-system factors may also play a critical role in explaining these differences. Ethiopia's ART program faces challenges related to health-workforce shortages, high patient-to-provider ratios, and interruptions in drug supply chains, all of which can negatively affect continuity of care and adherence counseling. Conversely, South Africa and Rwanda benefit from relatively stronger health-system infrastructure, including differentiated service delivery models, decentralized ART services, and enhanced adherence support mechanisms, which have been shown to improve treatment outcomes. Similarly, in India, structured follow-up systems and integration of community-based support programs may enhance adherence and retention among patients on second-line therapy.
Patient retention and engagement in care further influence viral load resuppression outcomes. In the Ethiopian context, loss to follow-up remains a persistent challenge, often driven by socioeconomic barriers, stigma, transportation costs, and competing livelihood demands. These factors may limit sustained engagement in care following virologic failure, thereby reducing the likelihood of timely resuppression. In contrast, higher retention rates reported in Rwanda and parts of South Africa may reflect stronger patient-tracking systems, community health worker involvement, and social support mechanisms. Collectively, these contextual differences underscore the importance of strengthening viral load testing capacity, improving health-system responsiveness, and enhancing patient retention strategies to optimize viral resuppression outcomes in Ethiopia.
Factors such as alcohol consumption, smoking, medication adherence, drug substitution history, and viral load were found to be significant predictors of viral load resuppression. In this study, we have found that alcohol consumption was independently associated with viral load resuppression. Patients who had no alcohol consumption history were 1.55 times more likely to have viral resuppression at any time as compared to the counterparts [AHR: 1.55 (95% CI: 1.08, 2.21)] after adjusting of multiple confounders (Figure 2).

Kaplan-Meier survival estimates by alcohol status among people living with HIV (PLWH) on second-line therapy at the chronic follow-up clinic of Gondar Comprehensive Specialized Hospital, from January 1, 2018, to December 31, 2022 (n = 380).
The finding is similar with a study done in Morocco. 29 This may be because alcohol consumption is strongly associated with poor adherence, and it may also have direct biological effects on the immune system or influence behaviors such as engagement in care and persistence on ART. 30
Patients who had no smoking history were 1.48 times more likely to have viral resuppression at any time as compared to its counterparts [AHR: 1.488 (95% CI: 1.04, 2.13)] after adjusting of multiple confounders (Figure 3).

Kaplan-Meier survival estimates by smoking status among people living with HIV (PLWH) on second-line therapy at the chronic follow-up clinic of Gondar Comprehensive Specialized Hospital, from January 1, 2018, to December 31, 2022 (n = 380).
The result is comparable with a study conducted in Vietnam. 29 This may be because smoking increases oxidative stress and induces the cytochrome P450 pathway, which can elevate viral load. Additionally, the CYP1A1-m1 enzyme may increase viral load by converting toxins present in cigarette smoke. 31 Smoking has also been independently associated with lower CD4 cell counts, as nicotine can impair immune function in multiple ways, including inhibiting T-cell proliferation by disrupting their ability to interact with antigen-presenting cells. 32
Patients who had good adherence were 1.63 times more likely to have viral resuppression as compared to its counterparts [AHR: 1.63 (95% CI: 1.02, 2.61)] after adjusting of multiple confounders (Figure 4).

Kaplan-Meier survival estimates by medication adherence among people living with HIV (PLWH) on second-line therapy at the chronic follow-up clinic of Gondar Comprehensive Specialized Hospital, from January 1, 2018, to December 31, 2022 (n = 380).
The finding is consistent with a study done in Arba Minch Hospital, Ethiopia. 33 The WHO recommends adherence counseling for PLWH with high viral loads. This counseling is a continuous and repeated process that involves assessing the current level of adherence, identifying specific barriers, assisting patients in finding solutions, and developing an individualized adherence intervention plan. Such interventions can improve viral load suppression and reduce the risk of subsequent treatment failure. 34
Patients without a history of drug substitution were 1.32 times more likely to achieve viral resuppression compared to those with a history of substitution [AHR: 1.324 (95% CI: 1.019, 1.72)] (Figure 5).

Kaplan-Meier survival estimates by drug substitution history among people living with HIV (PLWH) on second-line therapy at the chronic follow-up clinic of Gondar Comprehensive Specialized Hospital, from January 1, 2018, to December 31, 2022 (n = 380).
The finding was consistent with studies conducted in Dessie, Ethiopia. 3 Frequent first-line antiretroviral drug substitutions may reduce subsequent treatment options and necessitate reuse of previously substituted drugs, increasing the risk of drug resistance and failure to achieve viral resuppression. In settings where drug resistance testing is not yet available, appropriate drug selection at the initiation of first-line ART plays a critical role in the effectiveness of subsequent therapy. 5
Patients who had baseline viral load from 1000 to 100 000 were 5.61 times more likely to have viral resuppression as compared with the reference category [AHR: 5.61 (95% CI: 2.07, 15.198)] after adjusting of multiple confounders (Figure 6).

Kaplan-Meier survival estimates by viral load among people living with HIV (PLWH) on second-line therapy at the chronic follow-up clinic of Gondar Comprehensive Specialized Hospital, from January 1, 2018, to December 31, 2022 (n = 380).
The finding was consistent with studies conducted in Dessie, Ethiopia, 3 Uganda, 35 and Morocco. 36 This finding is consistent with studies conducted in Dessie, Ethiopia, Uganda, and Morocco, suggesting that a lower baseline viral load is an important determinant of successful viral resuppression.
Limitations
This study did not assess social or facility-level determinants of viral resuppression. Additionally, clinical factors like comorbidities and organ function were not included in the analysis, which may introduce confounding due to unmeasured variables. As with many retrospective studies using secondary data, incomplete documentation may have affected the availability of some variables. Exclusion of records with missing key variables may have introduced selection bias; however, this was necessary to ensure the validity of the regression analyses.
Conclusion and Recommendations
This retrospective cohort study demonstrated that the viral resuppression rate among people living with HIV receiving second-line antiretroviral therapy at Gondar Comprehensive Specialized Hospital remains low. Viral resuppression was significantly associated with alcohol consumption, smoking, medication adherence, prior drug substitution, and baseline viral load. These findings highlight that virologic recovery on second-line ART is not solely dependent on regimen potency but is strongly shaped by patient behavior, continuity of care, and treatment management practices.
From a public health perspective, suboptimal viral resuppression threatens progress toward national and global HIV control targets, particularly the UNAIDS 95-95-95 goals, by increasing the risk of drug resistance, ongoing HIV transmission, and the need for costly third-line therapies. The results underscore the need for differentiated, patient-centered HIV care models that integrate adherence support and behavioral risk assessment into routine second-line ART management.
Recommendations
Strengthen adherence support by implementing routine, structured adherence assessments and intensified counseling for patients on second-line ART, particularly those with detectable viral load. Integrate substance-use screening and counseling into HIV care services to identify and manage alcohol consumption and smoking behaviors that negatively affect viral resuppression. Minimize unnecessary drug substitutions by ensuring regimen changes are guided by clinical and virological evidence, supported by national treatment guidelines. Enhance viral load monitoring and clinical response by ensuring timely viral load testing and prompt follow-up interventions for patients with unsuppressed viral load. Prioritize high-risk patients, including those with high baseline viral load or prior treatment modifications for closer follow-up using differentiated service delivery approaches.
In conclusion, improving viral resuppression among patients on second-line ART requires coordinated interventions at patient, provider, and health-system levels. Strengthening adherence-focused, behavior-responsive, and guideline-driven HIV care is essential to optimize treatment outcomes and sustain long-term HIV control in resource-limited settings.
Supplemental Material
sj-docx-1-jia-10.1177_23259582261439620 - Supplemental material for Rate of Viral Resuppression and Predictors Among PLHIV on Second-Line Antiretroviral Therapy at Gondar Comprehensive Specialized Hospital, Northwest, Ethiopia: A Retrospective Cohort Study
Supplemental material, sj-docx-1-jia-10.1177_23259582261439620 for Rate of Viral Resuppression and Predictors Among PLHIV on Second-Line Antiretroviral Therapy at Gondar Comprehensive Specialized Hospital, Northwest, Ethiopia: A Retrospective Cohort Study by Getaw Wubie Assefa, Tesfaye Yesuf Yimer and Worku Chekol Tassew in Journal of the International Association of Providers of AIDS Care (JIAPAC)
Supplemental Material
sj-docx-2-jia-10.1177_23259582261439620 - Supplemental material for Rate of Viral Resuppression and Predictors Among PLHIV on Second-Line Antiretroviral Therapy at Gondar Comprehensive Specialized Hospital, Northwest, Ethiopia: A Retrospective Cohort Study
Supplemental material, sj-docx-2-jia-10.1177_23259582261439620 for Rate of Viral Resuppression and Predictors Among PLHIV on Second-Line Antiretroviral Therapy at Gondar Comprehensive Specialized Hospital, Northwest, Ethiopia: A Retrospective Cohort Study by Getaw Wubie Assefa, Tesfaye Yesuf Yimer and Worku Chekol Tassew in Journal of the International Association of Providers of AIDS Care (JIAPAC)
Footnotes
Acronyms and/or Abbreviations
Acknowledgments
We would like to thank the University of Gondar Referral Hospital administrative bodies and card room workers for their cooperation and permission to conduct the study. We are also thankful to the data collectors who participated in the study for their commitment
Ethical Approval and Consent
The study was first approved by the Institutional Review Board (IRB) of the University of Gondar, College of Medicine and Health Sciences, School of Medicine (Ref No. 478/14) from the University of Gondar, and ethical clearance was obtained. Upon this clearance, additional written permission to conduct the study on the medical records of PLHIV was obtained from the coordinator of the chronic clinic follow-up of the University of Gondar Comprehensive Specialized Hospital. Confidentiality of information was maintained through refraining from recording the patient's name in the used chart. Written informed consent was obtained from all participants prior to participation in the study, in accordance with COPE guidelines.
Author Contributions
GWA: conceptualization, data curation, formal analysis, funding acquisition, investigation, methodology, project administration, resources, software, supervision, validation, visualization, writing–original draft, and writing–review and editing. WCT and TYY: helped in methodology and writing–review and editing.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Availability of Data and Materials
The datasets used and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Supplemental Material
Supplemental material for this article is available online.