Abstract
Empyema is a complication of pneumonia, characterized by pus accumulation in the pleural space. It is more common in patients with comorbidities such as older age, diabetes, cancer, or immunocompromised states. Aspiration or oral cavity infections are more common in older adults with significant risk factors; therefore, the pathogen
Introduction
Empyema refers to infection and pus accumulation in the pleural cavity and is a well-known complication of pneumonia. It usually develops in patients with predisposing factors such as old age, diabetes, cancer, or immunodeficiency.1,2 Empyemas are usually polymicrobial and depend on the clinical scenario; however, oral bacteria are involved in aspiration-related ones.
3
This article describes a case of a 58-year-old previously healthy immunocompetent female who developed a left-sided empyema due to
Case Presentation
A 58-year-old woman with no known past medical history was admitted to the emergency room with a 2-week history of presenting weakness, fatigue, anorexia, nausea, as well as diarrhea. She also complained of occasional subjective fevers without rigor, with no shivering. Her overall health status has worsened in the last 48-72 hours, which prompted her to seek medical attention. She worked as a jeweler with frequent exposure to dust and reported that a coworker had recently been diagnosed with pneumonia. She denied tobacco use, alcohol use disorder, intravenous drug use, or other risk factors for immunosuppression. HIV and diabetes testing were not performed during this admission.
Her initial vital signs included a temperature of 98.2 °F, heart rate of 117 bpm, blood pressure of 169/93 mmHg, and SpO₂ of 85% on room air, which improved to 98% on 3L nasal cannula. Laboratory results revealed a white blood cell count of 29.5 × 103/µL, normocytic anemia with a hemoglobin level of 10.3 g/dL, sodium level of 134 mmol/L, and potassium level of 3.5 mmol/L. Computed tomography (CT) of the chest (Image 1) demonstrated a substantial, loculated pleural fluid accumulation on the left side, strongly consistent with empyema.
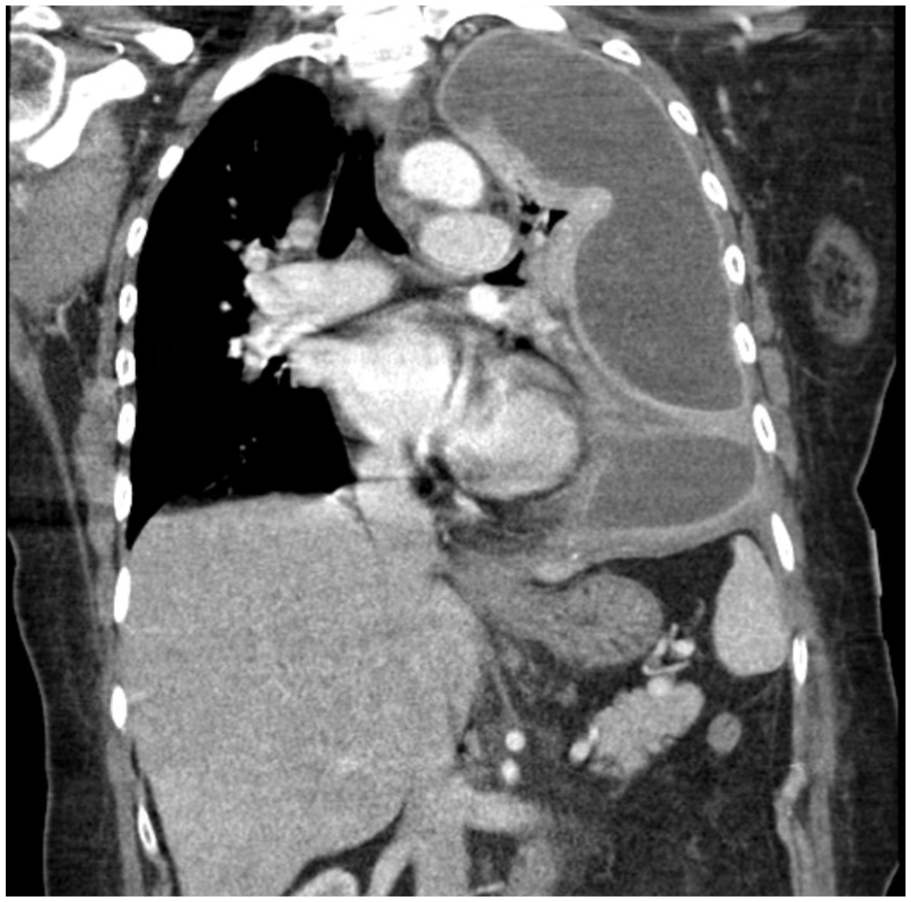
CT chest of empyema preoperatively.
The patient was started on empiric ceftriaxone, metronidazole, and linezolid, chosen to provide broad-spectrum coverage against community-acquired, anaerobic pathogens, and methicillin-resistant

Postresolution CT chest.
Discussion
An empyema develops when infection spreads from the lung parenchyma into the pleural cavity, progressing through the stages of exudative, fibrinopurulent, and organized.
High-resolution CT imaging is conventional for assessing pleural infections and planning for interventional therapy. Diagnostic thoracentesis is crucial, as pleural fluid usually exhibits low pH, low glucose, and elevated LDH levels in empyema cases. Conventional cultures, unfortunately, may not always identify causal organisms, while newer diagnostic techniques such as next-generation sequencing have demonstrated potential in certain contexts. 6
Empiric therapy should initially be broad spectrum, covering both aerobic and anaerobic organisms, then narrowed based on susceptibilities.
Delayed diagnosis and management of empyema may lead to significant consequences, such as chronic fibrothorax, sepsis, bronchopleural fistula, and respiratory failure. Mortality may reach up to 20% 5 in patients with substantial comorbidities or postponed therapy. In our patient’s case, early identification, commencement of antibiotics, and appropriate surgical intervention led to clinical improvement and discharge in a stable state.
Conclusion
This case underscores the necessity of preserving a comprehensive differential diagnosis when assessing pleural infections, especially in individuals lacking traditional risk factors.
Footnotes
Ethical Considerations
Our institution does not require ethical approval for reporting individual cases or case series.
Consent for Publication
Verbal informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
