Abstract
Brain abscess is a life-threatening infection that can occur secondary to contiguous or hematogenous spread. Several underlying conditions can lead to brain abscesses, such as dental infection, otitis media, sinusitis, and immunosuppression. Esophageal perforation leading to brain abscesses is extremely rare. We report a rare case of a 32-year-old man who presented to the emergency department with progressive headaches and upper-extremity weakness. Upon further evaluation, computed tomography (CT) revealed multiple brain abscesses secondary to Streptococcus intermedius infection. The patient eventually underwent esophagogastroduodenoscopy (EGD), which showed a perforation in the middle third of the esophagus. This case highlights the importance of considering esophageal perforation as a predisposing condition for brain abscesses.
Introduction
Brain abscess is a focal infection of the central nervous system, representing 8% of intracranial masses in developing countries and 1% to 2% of intracranial masses in Western countries.1,2 Brain abscess is commonly caused by the spread of nearby infections, including dental infection, otitis media, mastoiditis, and sinusitis. 3 The most frequent microbial pathogens isolated from brain abscesses are Staphylococcus and Streptococcus.4,5 Streptococcus anginosus are gram-positive, catalase-negative facultative anaerobic cocci that are part of the normal flora in the respiratory, gastrointestinal, and genitourinary tracts.6,7 The Streptococcus anginosus group includes anginosus, intermedius, and constellatus, which are subgroups of viridans Streptococci. 2 Although those organisms are part of the normal microbiota, they can become invasive and lead to brain abscesses, as in our case. Esophageal perforation is an uncommon condition, and its association as a predisposing factor to brain abscesses has been rarely reported in the literature. When reported, brain abscesses were linked to esophageal dilation and esophageal cancer which could be a result of microperforations and loss of mucosal integrity. We report a rare case of esophageal perforation presenting initially as multiple brain abscesses secondary to Streptococcus intermedius infection.
Case Report
A 32-year-old man with a medical history of hypertension and recent pneumonia presented to the emergency department with headaches, right upper-extremity weakness, and aphasia. He was noted to be hypertensive at 162/107 and tachycardic at 116, but vital signs were otherwise within normal limits. Laboratory data showed a white blood cell count (WBC) of 15.5 K/CUMM. A head computed tomography (CT) scan showed multiple intracranial masses with surrounding vasogenic edema (Figure 1). Two sets of blood cultures were drawn and showed negative results. The patient was admitted to the neurosurgical unit and was treated with dexamethasone, with gradual improvement in his symptoms. CT angiogram (CTA) was also done to rule out pulmonary embolism and showed patent proximal pulmonary arteries but poor visualization of the distal ones. CTA also showed esophageal wall thickening and lymphadenopathy. Magnetic resonance imaging (MRI) of the brain revealed multiple ring-enhancing lesions within the left temporal lobe, left frontal lobe, and left insula concerning for malignancy or abscesses (Figure 1). Consequently, the patient underwent a CT abdomen and pelvis to search for a potential primary malignancy source. The CT scan revealed an esophageal thickening; therefore, gastrointestinal evaluation was recommended as an outpatient (Figure 2). Image-guided craniotomy with brain biopsy and aspiration was performed, confirming abscesses. The patient was empirically started on intravenous vancomycin, ceftriaxone, and metronidazole, and Gram staining showed gram-positive cocci in pairs and chains. A culture later grew Streptococcus intermedius; cytology was negative for malignant cells. The patient remained clinically stable and was feeding well throughout this period. Given his condition, his antibiotics were narrowed down to ceftriaxone and rifampin for Streptococcus intermedius coverage. In addition, given the cultured organism is a normal flora of the oropharyngeal cavity and esophagus, further workup was done to find the source of the infection. A maxillofacial X-ray showed dental caries, which is a suspected source. However, the patient did not have any active dental symptoms, prior history of dental manipulation, or findings suggestive of dental abscesses, so further workup was requested. A transthoracic echocardiogram (TTE) was done and did not show any vegetation that suggests the presence of endocarditis. Due to his prior incidental CTA finding that raised suspicion of pulmonary embolism, a CTA was performed which revealed a gas collection around the esophagus (Figure 3).
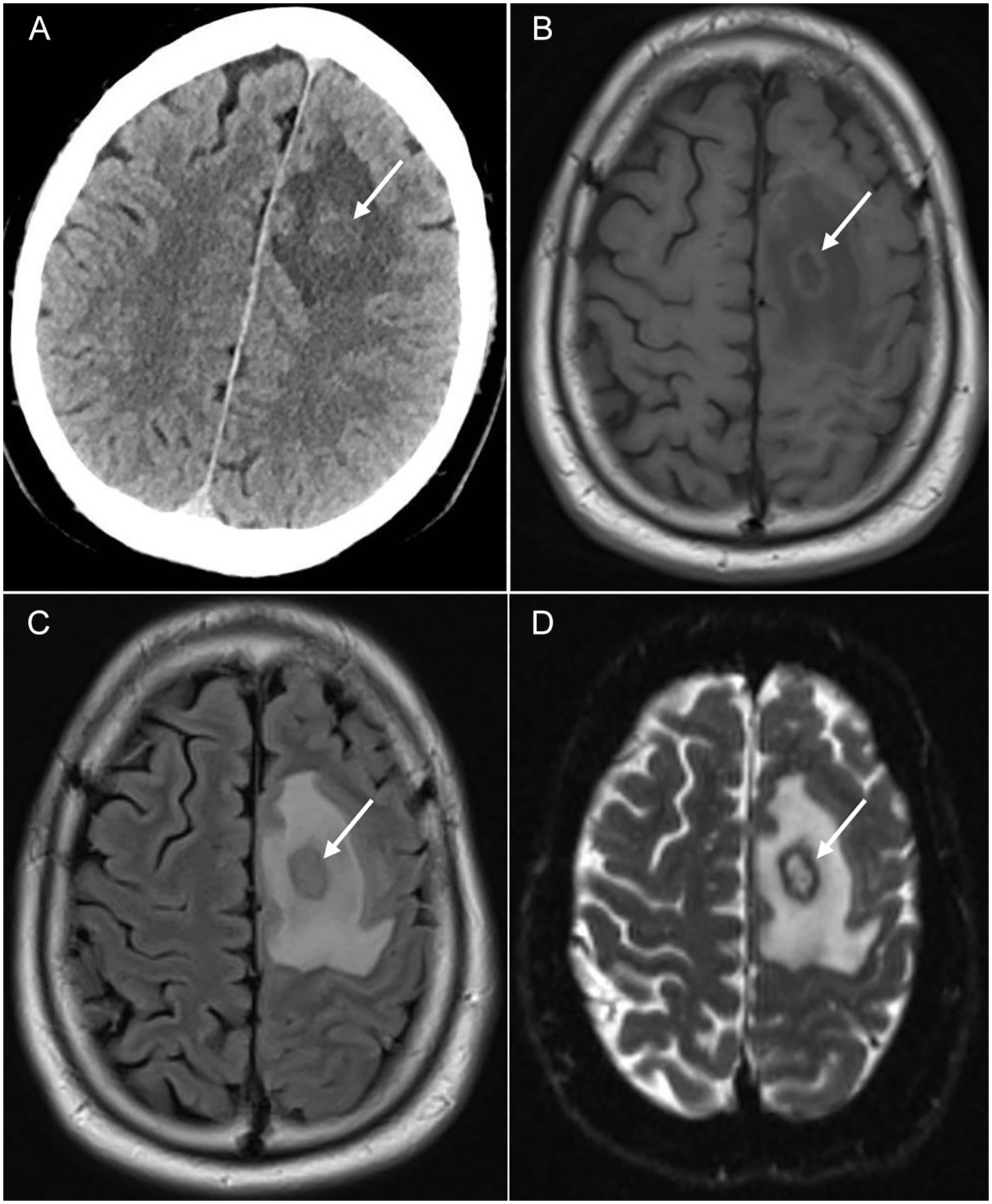
(A) Axial section of the head CT without contrast showing an approximately 1.5-cm mass in the left frontal lobe with surrounding vasogenic edema (white arrow), (B) MRI T1, (C) MRI T2, and (D) MRI DWI showing a ring-enhancing lesion within the left frontal lobe with surrounding vasogenic edema (white arrow).
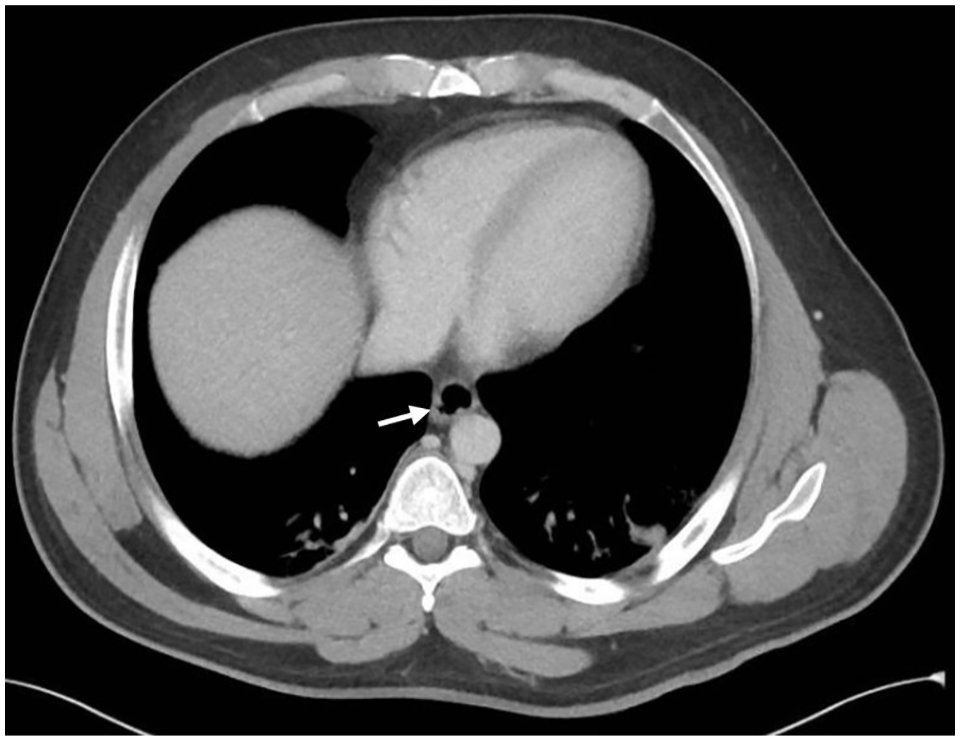
Axial section of the abdominal and pelvic CT showing distal esophageal thickening (white arrow).

Axial section of the chest CT angiogram showing a gas collection around the esophagus (white arrow).
A CT esophagography with oral contrast was done and showed an esophageal leak (Figure 4). The patient underwent urgent esophagogastroduodenoscopy (EGD), which revealed a 2-mm perforation of unknown etiology in the middle third of the esophagus, located at 28 cm from the incisors (Figure 5). Extravasation outside the esophageal lumen was confirmed under fluoroscopy by injecting 10 ml of water-soluble contrast into the fistula orifice. De-epithelialization of the fistula tract and orifice, along with tissue destruction using argon plasma, was successfully performed (Figure 5). Closure was achieved using an Over-The-Scope Clipping Device (OVESCO), which was deployed successfully over the fistula orifice (Figure 5). The patient was able to tolerate food intake and was discharged to continue the same antibiotics as an outpatient to complete 4 weeks of therapy. Two weeks after discharge, the patient presented with worsening headaches. Brain MRI showed interval worsening of the left temporal abscess. The patient underwent craniotomy for resection of the left temporal intracranial abscess and tolerated the procedure well. He was discharged on ceftriaxone, rifampin, and metronidazole to complete 4 weeks of therapy. One-month follow-up brain MRI showed complete resolution of the abscess, and the follow-up chest CT scan showed no persistent esophageal leak (Figure 6).

Axial section of the CT esophagram obtained after administration of oral contrast material showing an esophageal leak (white arrow) with a small amount of mediastinal gas (yellow arrow).
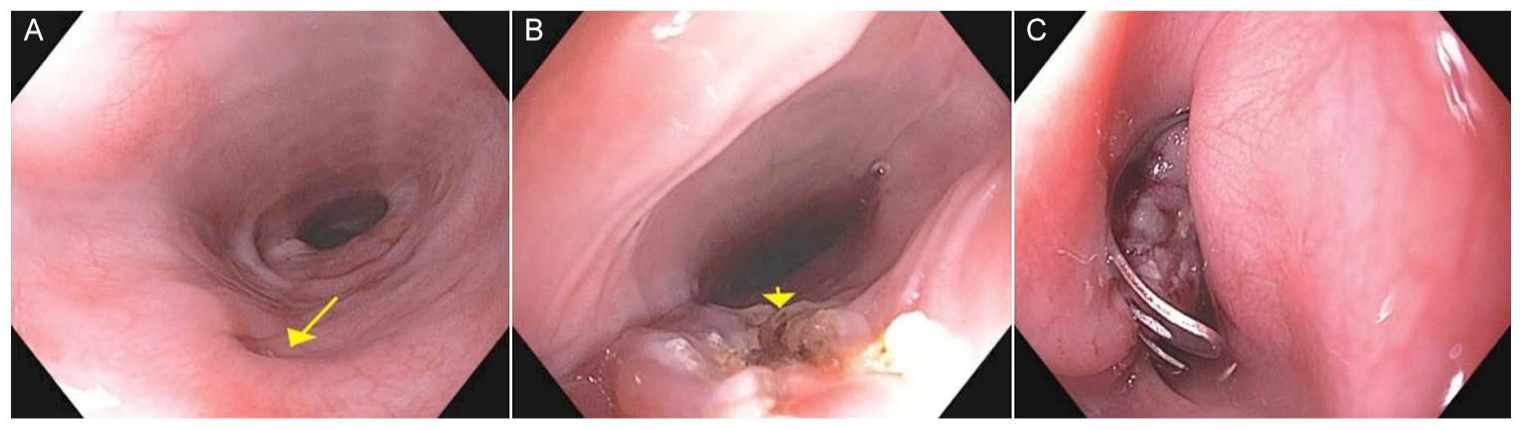
(A) EGD showing a 2-mm perforation at 28 cm from the incisors (yellow arrow). (B) EGD showing a fistula status after de-epithelialization with argon plasma coagulation (yellow arrow). (C) Post-clipping EGD showing successful closure of esophageal perforation.

Axial section of the chest CT showing an esophageal clip (white arrow) without any esophageal leak.
Discussion
Esophageal perforation is a challenging life-threatening condition that can present with a wide range of symptoms, delaying the diagnosis. 8 Patients with esophageal perforation can present with neck pain, chest pain, dysphagia, dysphonia, and odynophagia, depending on the location of the perforation. 8 Interestingly, our patient presented with neurological symptoms without the typical esophageal perforation symptoms. Several risk factors for esophageal perforation have been identified, such as a history of esophageal perforation, esophageal surgery, balloon dilation, severe esophagitis, radiation, caustic ingestion, and malignancy. In our case, the patient did not have any known risk factors for esophageal perforation.
Although most esophageal perforations are iatrogenic or traumatic, they can happen spontaneously. Esophageal perforation can cause the normal flora to leak from the esophagus, which can result in infection that can lead to mediastinitis and sepsis. 9 In our case, the patient had a spontaneous esophageal perforation of unclear etiology that could have contributed to the development of multiple brain abscesses.
Bacterial migration from esophageal dilation and cancer has been reported as a cause of brain abscesses.10-12 Hanna and Das 10 and Nayfe et al 11 reported 2 cases of brain abscesses caused by Streptococcus intermedius in association with esophageal adenocarcinoma and squamous cell carcinoma, respectively. To the best of our knowledge, our case is the first in the literature to describe brain abscesses caused by Streptococcus intermedius in association with esophageal perforation of unknown etiology. Due to these different associations, the loss of esophageal mucosal integrity may be the main reason for brain abscess formation rather than the underlying disease. 11 The loss of mucosal integrity may have allowed gut flora to enter the bloodstream and cause bacterial spread to the brain. 11
The process of how abscesses form involves bacteria spreading by direct or hematogenous dissemination to the brain. 2 One study found that 28% of brain abscesses resulted from bacterial hematogenous spread from distant sites such as the heart, lungs, or gastrointestinal tract. 13 In the previously reported esophageal dilation–associated brain abscess cases, esophageal microperforation likely resulted in bacteremia that led to brain abscesses by allowing the gut flora to enter the bloodstream. In our case, given the identified organism, the source of infection could have originated from the oral cavity or esophagus. In addition, although dental caries were noted on the maxillofacial X-ray, the patient had no dental or oropharyngeal symptoms or a history of dental manipulation. On the other hand, the patient had an active esophageal pathology on admission. The hematogenous spread could have caused the bacteria to migrate to the brain, and given that our patient was treated for community-acquired pneumonia as an outpatient with a 1-week course of amoxicillin/clavulanate and doxycycline 3 weeks before presentation, this could have affected the blood culture results by eradicating any potential bacteremia that could have resulted in brain abscesses. Therefore, we think that dental caries and esophageal perforation are potential sources of brain abscesses.
In conclusion, we report a rare case of esophageal perforation presenting initially as multiple brain abscesses secondary to Streptococcus intermedius infection. Our case suggests that esophageal perforation can be the source of infection for brain abscesses. Clinicians should be aware of esophageal perforation–associated brain abscesses and consider it a potential underlying cause.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed Consent
Verbal informed consent was obtained from the patient for their anonymized information to be published in this article.
