Abstract
Homeopathic remedies made primarily from eggshells, and therefore calcium, can be marketed for treatment of back pain and vaginal discharge. We present a case of a 23-year-old otherwise healthy woman who presented with acute liver failure (ALF) ultimately requiring liver transplantation as a result of taking increased doses of a homeopathic product with the primary ingredient of eggshells. Although relatively uncommon compared with medications such as acetaminophen, herbal supplements have been reported to cause drug-induced liver injury (DILI), thought to be primarily due to contaminants. This is the first known report of DILI resulting from a homeopathic product with the primary ingredient of eggshells, and it demonstrates the importance of early ALF recognition and treatment, as well as the importance of practicing caution when using homeopathic supplements.
Introduction
Drug-induced liver injury (DILI) is the leading cause of acute liver failure (ALF) in the United States, with as many as 20 new cases of DILI per 100 000 persons each year and constitutes more than half of ALF cases.1,2 Acute liver failure is most often associated with dose-dependent toxicity from acetaminophen, but a vast range of drugs can cause idiosyncratic DILI including herbal supplements or homeopathic medicines (up to 16%). 3 Homeopathic remedies made primarily from eggshells (main ingredient therefore being calcium) have reported indications including back pain and vaginal discharge and have not previously been reported to be associated with liver injury or ALF. This report describes a new observation of ALF related to ingestion of a homeopathic product with the primary ingredient of eggshells.
Case
We present a case of a 23-year-old otherwise healthy woman with body mass index 32.3 and a history of polycystic ovarian syndrome who presented with ALF ultimately requiring orthotopic liver transplantation (Figure 1). The patient is originally from India where she reported taking homeopathic medications for various indications for several years without known toxicity. She had no history of alcohol, tobacco, or other drug use. At the time of her presentation, she was living and working in the United States and reported she was unable to refill her homeopathic product with the primary ingredient of eggshells from India. She was off of all medications and supplements with the exception of Berberis vulgaris for approximately 1 month before obtaining a similarly named homeopathic product with the primary ingredient of eggshells from Amazon.com. She reports originally taking 4 pills/d for 10 days, and then increased to 10 pills/d for 10 days as she was unsure of the appropriate dose. She subsequently developed orange discoloration of her urine and nausea, reportedly without any preceding muscle-related effects or symptoms, and she discontinued all of her medications/supplements. Approximately 2 weeks later, she presented to the emergency department for nausea and malaise, where she was found to have the following lab results:

Mononucleosis screen and hepatitis panel were negative. She had no evidence of hepatic encephalopathy at that time. Ultrasound of the abdomen was notable for hypoechoic liver parenchyma only. She was discharged home with gastroenterology telehealth follow-up. She was seen 1 week later at which time she endorsed worsening nausea, vomiting, anorexia, jaundice, and fatigue. She presented to a local emergency department where she received intravenous vitamin K and underwent further laboratory evaluation. She was transferred to another hospital for higher level of care and admitted with acute liver injury. There she received intravenous N-acetylcysteine per institutional protocol, ursodiol, albumin, vitamin K, and fresh frozen plasma transfusions given for coagulopathy. Magnetic resonance cholangiopancreatography was performed and demonstrated no evidence of biliary obstruction or chronic liver disease (no ascites, contour nodularity, mass, or lymphadenopathy), though liver size noted to be small (11.5 cm in span). At approximately 21 to 28 days after the onset of symptoms, her lab results were as follows:

and her mental status deteriorated. She was intubated for airway protection given severe encephalopathy, “cooling protocols” were initiated, and she was transferred again to a higher level of care at our center for emergent liver transplant evaluation. She was evaluated and listed as status 1A for acute liver failure. Her clinical status continued to decline and her labs continued to worsen:

as she waited for an appropriate organ, which became available approximately 28 hours after listing. At the time of her surgery, her explanted liver was noted to have massive parenchymal loss with hemorrhage, and pathology confirmed near complete collapse of the organ’s framework with only small foci of steatotic hepatocytes remaining. After her initial operation, her hospital course was complicated by coagulopathy, hypotension, leukocytosis, kidney failure requiring temporary dialysis, and multiple operations for completion of biliary anastomoses and delayed complex abdominal wall closure with mesh given large donor size. She was discharged from the hospital 2 weeks after transplant and her outpatient course continues to go well over 1 year after liver transplantation.
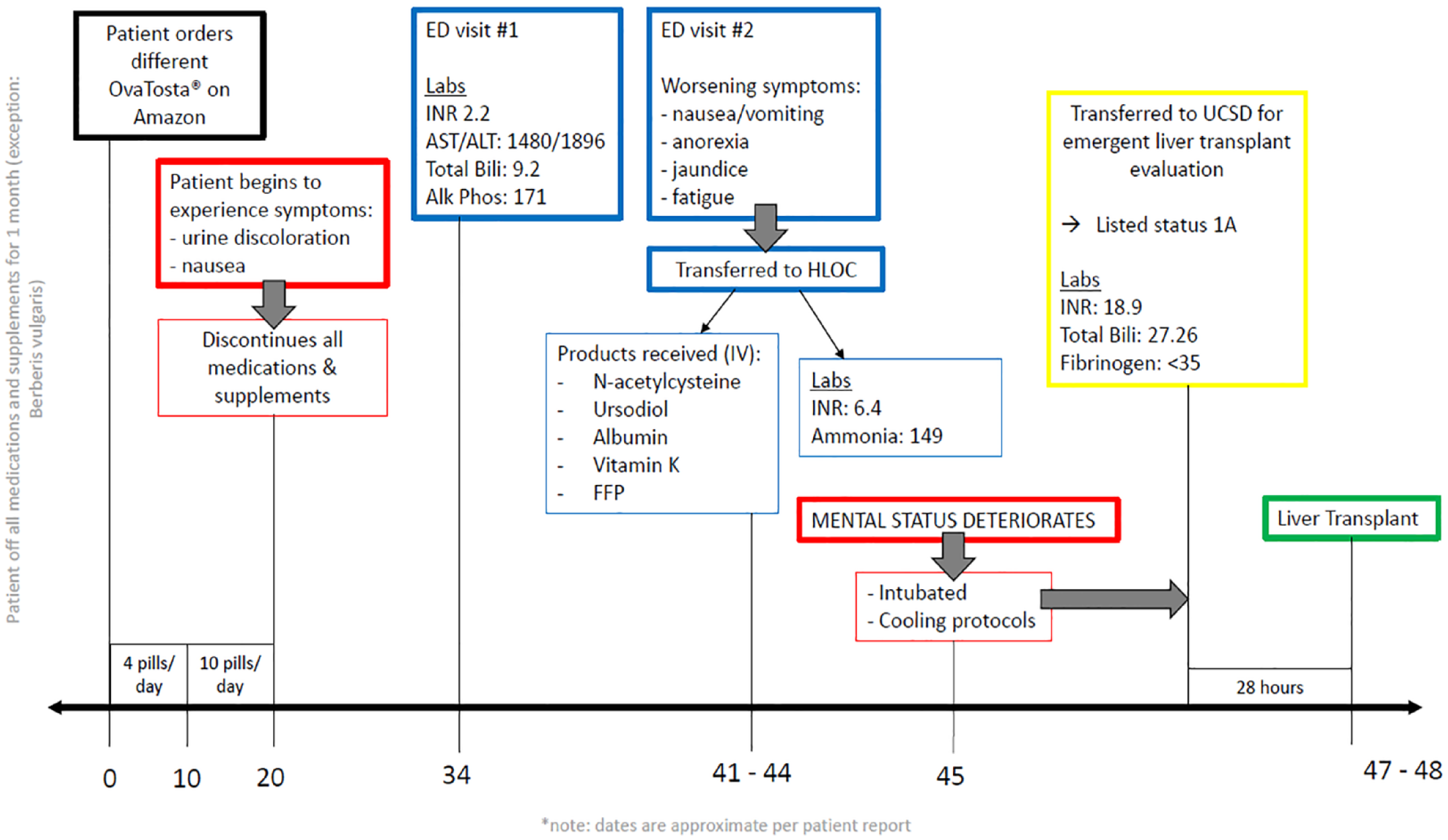
Timeline of patient case trajectory.
Discussion
Drug-induced liver injury can lead to ALF warranting urgent liver transplantation. The most common causes of DILI requiring liver transplantation are acetaminophen (40%-50%), anti-tuberculosis medications (8%-20%), anti-epileptics (7%-15%), and antibiotics (6%); however, herbal supplements have been reported to cause approximately 3% to 16% of cases.3-5 In this case report, an herbal supplement with the primary ingredient of eggshells was unintentionally consumed in doses far greater than intended and was the only identifiable potential cause of ALF necessitating status 1A liver transplantation.
Homeopathic medicine is becoming increasingly popular given their “more natural” reputation. Many are nonregulated. To the author’s knowledge, the product in this case has not been previously reported to contain known toxins. Its primary ingredient is calcium from “toasted eggshells,” which is also not generally known to contain any mechanism of toxicity to cause liver failure or disease. However, it is not uncommon for herbal supplements such as this one to contain other potentially toxic agents that are not specifically listed on the bottles’ ingredients label. For example, toxic metals including lead, mercury, and arsenic have reportedly been discovered in many (almost 20%) naturopathic medicines manufactured in India, particularly those sold by US websites. 6 As such, we hypothesize that this patient’s ALF was likely caused by a contaminant (also consumed in higher quantities than intended) in her homeopathic product with the primary ingredient of eggshells.
The patient in this case did also report taking B vulgaris, another homeopathic supplement, on a regular basis. This medicinal plant, also known as barberry, contains antioxidants and alkaloid compounds, is commonly found in Iranian cuisine and has been used as a remedy for fever, cough, depression, inflammation, hyperlipidemia, and hyperglycemia among other ailments. 7 It has been studied in far greater depth compared with this homeopathic product with the primary ingredient of eggshells and has not been shown to cause liver injury or disease. On the contrary, B vulgaris has been used as a remedy for liver disease as it is believed to have “hepato-protective” properties. 7 This patient had not changed her supply, practice, or dosing regarding B vulgaris in the time course leading up to her ALF, therefore making it an unlikely cause. The timeline does, however, point more definitively toward her homeopathic product with the primary ingredient of eggshells (or more specifically, a contaminant in at least her specific batch) as the etiology for her ALF, given the patient obtained a new supply of the supplement and additionally changed the amount consumed leading up to the onset of her symptoms.
This case is another example of the burden of ALF secondary to homeopathic and naturopathic supplements. Fortunately, the patient had access to and sought medical care in time, and the liver failure was identified and managed efficiently and effectively enough to prevent her imminent demise. As soon as it became clear alternate treatments were not effective and the patient’s clinical status was rapidly deteriorating, she was transferred, swiftly listed for status 1A liver transplant, and just over 24 hours after listing, she underwent successful orthotopic liver transplantation. The pathology results with almost complete parenchymal volume loss reinforce the importance of early recognition and efficient management of DILI causing ALF. Physicians should instruct their patients to practice caution when using homeopathic supplements as there may be unintended, and sometimes fatal, consequences.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: VA is supported by NIDDK (K23DK119460).
Ethics Approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed Consent
Verbal informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
