Abstract
Leukocytoclastic vasculitis (LCV) is an idiopathic small vessel vasculitis. Leukocytoclastic vasculitis can be found in a spectrum of diseases and is noted as a rare extraintestinal manifestation of Crohn disease. This case report examines a 55-year-old man with a previous diagnosis of Crohn disease who was admitted after 5 days with a persistent rash. A biopsy confirmed LCV, and the patient followed up with dermatology for outpatient treatment. This study adds to the sparse medical literature on LCV cases relating to Crohn disease.
Keywords
Introduction
Inflammatory bowel disease (IBD) is an umbrella term that refers to 2 chronic inflammatory disorders of the gastrointestinal tract: ulcerative colitis and Crohn disease. These diseases have different characterizations on location and extent of gastrointestinal involvement, but up to 40% of patients may experience extraintestinal manifestations, which are more commonly associated with Crohn disease than ulcerative colitis. One of the rarest dermatological manifestations is leukocytoclastic vasculitis (LCV).1,2 Leukocytoclastic vasculitis is a small vessel vasculitis that affects the cutaneous postcapillary venules.3,4
The majority of the current literature reporting on the relationship between LCV and Crohn disease portrays LCV primarily as a presenting symptom. 3 The underlying diagnosis of IBD, more specifically Crohn disease, is discovered through the patient’s workup. However, the current literature is devoid of information reporting the relationship of LCV in patients with a prior diagnosis of IBD or Crohn disease. This case is of a 55-year-old man who has a previous diagnosis of Crohn disease and presented with palpable maculopapular purpuric rash found to be LCV.
History and Physical
A 55-year-old man with normal body mass index, a history of Crohn disease in remission, and no significant family history or known allergies presented to the emergency department (ED) with a diffuse, severely pruritic rash. The patient had a painful rash for 5 days that originated on his back and progressed to his extremities (Figures 1 and 2). Associated symptoms include fever, chills, body aches, headaches, cough, sore throat, loss of appetite, and possible isolated oral lesions. His primary care physician prescribed prednisone, loratadine, and famotidine. As minimal relief was experienced, the patient sought medical care from the ED and was admitted to the hospital for further evaluation and treatment.
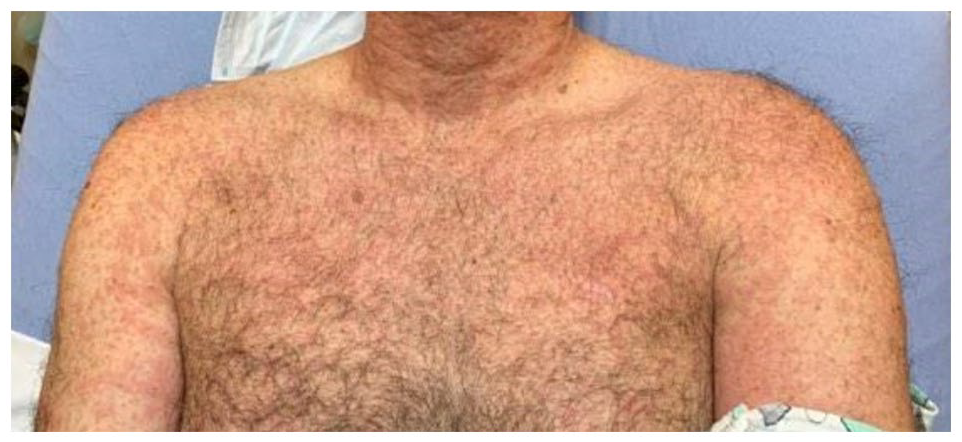
Maculopapular rash originated on the patient’s back and trunk.

Maculopapular rash spread to the patient’s lower extremities.
While obtaining a history, the patient denied common triggers to rashes, including changes in medications, environmental exposures, living arrangements, drug use, and risky sexual behavior. He denied taking any medications relating to his Crohn disease as he was currently in remission. The patient further stated he was up to date on his vaccinations (hepatitis A and B; influenza; anthrax; typhoid; and measles, mumps, and rubella), and he thought he had chickenpox as a child but was not completely certain. Upon admission, many of the symptoms at the onset of the rash resolved except for itching and burning sensation with a diffuse rash and isolated painful mucosal lesion on the lower lip.
On physical examination, he appeared alert, oriented, healthy, and in mild distress. His heart was in regular rate and rhythm without murmurs, and no peripheral edema was present. Lungs were clear to auscultation bilaterally. No focal findings or movement disorders were noted, and there was no significant deformity or tenderness to palpation on his extremities and joints. The patient’s physical examination was significant for a diffuse erythematous maculopapular purpuric rash spanning from the trunk to all 4 extremities, including a few isolated spots on the palms but excluding webs of the fingers. Some fine vesicles in different stages of healing were also present. There was a possible lesion of the lower lip, but no other mucosal involvement was noted.
Diagnostics and Assessment
From the history, most drug-related causes and hypersensitivities were ruled out, so inflammatory and infectious causes were the primary focus of the workup. His laboratory results showed a leukocytosis present upon admission (15.57 K/μL), along with a transaminitis (alkaline phosphatase of 253 U/L, aspartate transaminase of 85 U/L, and alanine transaminase of 96 U/L), trace ketones, and elevated C-reactive protein (69.5 mg/L). Further infectious causes were evaluated with his chest x-ray showing no infiltrate, and COVID-19, influenza A and B, and rapid strep were negative with no β-hemolytic streptococcus group A isolated on culture. Two blood cultures were obtained and yielded no growth after 5 days. Syphilis antibody, human immunodeficiency virus antibody, Epstein-Barr virus viral capsid antigen IgM antibody, and varicella zoster IgM antibody were all negative with varicella zoster antibody IgG showing he had immunity. A shave biopsy was obtained from lesions on his right thigh.
While in the hospital, the patient’s treatment focused on symptomatic treatment with hydroxyzine, but he also received intravenous acyclovir because of the initial concern for varicella infection. The patient’s symptoms and lab values improved, and he was eventually discharged home with outpatient follow-ups with dermatology, his primary care physician, and gastroenterology for his biopsy results and further management.
Biopsy results confirmed acute and chronic dermatitis with vasculitis. Per the pathology report, the biopsy showed perivascular inflammation with a major component of neutrophils present in walls of vessels, extravasation of erythrocytes, focal fibrinoid deposition, and inflammatory infiltrate comprising lymphocytes and few eosinophils. The Grocott methenamine silver (GMS) stained negative for fungal organisms. The biopsy was suggestive of LCV. The patient’s care was transitioned to an outpatient dermatologist, where 2 more biopsies were obtained, and a prednisone taper was prescribed.
Discussion
In the literature, there is a lack of consistency with the use of the term LCV. Leukocytoclastic vasculitis, also known as hypersensitivity vasculitis, is a type of small vessel vasculitis that occurs in about 30 to 45 cases per million people annually.3,5 Although LCV can affect all ages, it is most common in adults and does not discriminate based on sex. 6 However, LCV is a pathological or histological finding, not a diagnosis, and is commonly confirmed with a biopsy. This case is in line with current recommendations to confirm the diagnosis with a biopsy, but there is some evidence that direct immunofluorescence should be the cornerstone of diagnosis, which was not performed in this case. 6
Leukocytoclastic vasculitis is characterized histologically by Drs Russell and Gibson as a “neutrophilic perivascular infiltrate affecting cutaneous postcapillary venules with fibrinoid deposits in and around the vessel wall, endothelial swelling, and extravasation of red blood cells,” 4 which is consistent with the biopsy results discussed in this case.2,4 This is a characteristic feature of multiple forms of cutaneous small vessel vasculitis, which can be related to a wide spectrum of diseases such as recent infections, drug exposure, connective tissue disease, systemic inflammatory conditions, and malignancies.4,5 These conditions serve as inciting factors that create immune responses that lead to LCV. 3 Perhaps, this immune dysfunction is the connection between LCV and IBD, but there is a poor understanding of their relationship.
About 30% to 60% of cutaneous LCV cases lack a clear clinical etiology or identifiable inciting factor.4,6,7 In these cases, primary cutaneous small vessel vasculitis (PCSVV) is used to refer to the clinical manifestation of the pathological or histological finding of idiopathic LCV; therefore, it is a diagnosis of exclusion. 4 These cases are considered “idiopathic,” but the presentations may be the initial symptom of an underlying disease. Therefore, a full workup and close monitoring are recommended in case further symptoms develop that could point to a new underlying diagnosis.
In this patient’s case, his only risk factor was his history of IBD, which is commonly found to be the underlying disease of LCV. The patient was diagnosed with vasculitis as a diagnosis of exclusion, and the diagnosis was later confirmed as LCV when biopsy results were obtained. The inciting event for the vasculitis remains unidentified. The most likely trigger was an unknown viral agent that was not identified during the patient’s workup, an extraintestinal manifestation of his Crohn disease, or an idiopathic cause. 1 Primary cutaneous small vessel vasculitis is a presentation of LCV, and thus, possibly a more appropriate diagnosis for this case. For consistency with terminology used in current literature, idiopathic LCV or PCSVV will be referred to as LCV in the remainder of this article.
The number of cases that connect LCV and Crohn disease is limited, but the cases where Crohn disease is the inciting event for LCV are rare. Leukocytoclastic vasculitis can occur at any time during the course of Crohn disease.1,3,6 Most cases in the current literature contribute the onset of LCV to an inciting drug, and only about 8 histologically confirmed cases were found that attributed the onset of LCV to Crohn disease without another identifiable inciting factor.1,2 Out of these cases, more than half of them found an association of LCV with flares of Crohn disease. Two cases did not report any association between LCV and a flare, 2 but only one case explicitly stated LCV was found in a patient who was in remission for Crohn disease, similar to this case. 1 Furthermore, this is the only case reported where the rash associated with LCV initially started on the trunk and back. Most commonly, the rash starts on the lower extremities and sometimes ascends to the trunk and back.1,3,6
Due to the rarity, diverse etiologies, and variable manifestations of LCV, documented and guided management is lacking, but treatment should be proportional to the severity of the disease.8,9 About 90% of cutaneous vasculitis, including LCV, are self-limited and resolve spontaneously over 3 to 4 weeks, so most patients do not need systemic treatment.6,8 However, if an identifiable trigger was found on the workup, the underlying cause should be treated. This may include stopping the inciting drugs or treating an underlying infection. For more severe or chronic disease states, systemic treatment should be considered. For severe diseases, oral glucocorticoids can be used for short periods of time, along with ice packs and antihistamines for symptom relief.3,8 Other long-term management options are available, such as colchicine, dapsone, azathioprine, or hydroxychloroquine. More studies are needed for the most effective therapies. Treatment must balance risks and benefits on an individualized basis. 8
Most LCV cases are self-limiting, so symptom management takes priority to provide the patient with some relief. The treatment regimen used in this case included an initial dose of steroids with the continuing treatment of acyclovir/valacyclovir and hydroxyzine, which has shown to be effective.1,6,8 Although this treatment was sufficient, the literature suggests altering this treatment regimen by adding ice packs for patient comfort,3,5 continuing steroids until outpatient dermatology follow-up,1,3,5,6,8 and stopping acyclovir/valacyclovir after varicella infection was ruled out. In addition, colchicine could have been beneficial 4 as the patient reported both skin and joint involvement (myalgias).5,8 Fortunately, the prognosis for LCV is very good with minimal risks. There is a low mortality rate (about 2%) and only about 10% of cases become chronic and last 2 to 4 years after onset. 6
Conclusion
There is a limited number of documented cases relating to LCV in patients with a history of Crohn disease. This case highlights the importance of taking a good history, exploring a patient’s risk factors, and the importance of a thorough workup to exclude life-threatening or easily treatable causes and lead to a diagnosis of exclusion. Leukocytoclastic vasculitis is most commonly idiopathic, and the etiology is commonly unidentifiable, especially in patients with previous risk factors like Crohn disease. Based on the literature review conducted, this case is a unique presentation of LCV because it is the only case that reports a patient in remission of Crohn disease with the rash starting on his back/trunk and spreading to his extremities.
Footnotes
Acknowledgements
Dr Rodney Kusumi and Dr Dorvan Byler were vital in diagnosing and managing the patient presented in this case report.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The Ohio University’s Heritage College Office of Research and Grants supported this work by covering the article processing charge for this publication. The authors received no additional financial support for the research and/or authorship of this article.
Ethics Approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed Consent
Written informed consent was obtained from the patient for their anonymized information to be published in this article.
