Abstract
Oral melanin pigmentation is a ubiquitous presentation in the oral cavity. It could be a cause of psychological distress to many subjects due to aesthetic reasons.
Aims and Objectives:
This study attempts to compare the laser and scalpel depigmentation techniques. It also includes a comparison related to the Visual Analog Scale, patient comfort, healing response and time taken for the procedure and recurrence of pigmentation.
Materials and Methods:
A total of 10 patients were included in the study. A split-mouth approach comparing the scalpel technique with that of the diode laser technique was planned.
Results and Conclusion:
The results of the present study revealed that both laser and scalpel techniques are equally effective for depigmentation, yielding aesthetic results.
Introduction
Oral melanin pigmentation has been observed in all races 1 and is usually limited to the keratinized mucosa. It can become an aesthetic issue for many a patient, especially when it is located in the anterior labial gingiva, is not uniform in appearance, and is associated with a high smile line. Gingival depigmentation is a periodontal plastic surgical procedure whereby the gingival hyperpigmentation is removed or reduced with the help of various techniques. The first and foremost indication for depigmentation is the patient demand for improved aesthetics. In medical sciences, various depigmentation techniques have been employed with similar clinical results. In 2017, a similar study was carried out by Mahajan et al 2 in which they compared depigmentation by the scalpel technique on one side and by the diode laser technique on the other side, and concluded that, on surgically treated sites, all cases showed repigmentation of the gingiva, but those treated with the laser technique did not show repigmentation of the gingiva even at the end of the 9-month observation time. The selection of a technique should be based on clinical experience and individual preferences. The purpose of the study was to evaluate clinical outcomes with respect to color change obtained by depigmentation by employing and comparing the surgical blade and diode laser therapies. According to the previously published data,3-8 attempts at depigmentation of gingiva have already been made.
The surgical methods of depigmentation include the scalpel surgical technique, 3 cryosurgery, 4 and electrosurgery. 5 Recently, lasers of different varieties such as neodymium, aluminum-yttrium-garnet (Nd-YAG) lasers [6], diode lasers, erbium-YAG lasers, 7 and carbon dioxide (CO2) laser 8 have been introduced.
Also, bur abrasion chemical methods 9 of depigmentation, referred to as chemoexfoliation, have been employed which use agents such as 90% alcohol and 95% phenol. 10 Other techniques aimed at masking the pigmented gingiva from the less pigmented area have used free gingival grafts 11 and acellular dermal matrix allografts. 12
Aims of the Study
The aims of the study are to compare the clinical outcome pertaining to change in color between the surgical blade and diode laser, leading to a decrease in the appearance of gingival melanin pigmentation, and also to evaluate the patients’ comfort following these 2 procedures using a Verbal Analog Scale which includes the VAS Pain Scale, 9 the duration of the procedure in minutes, any untoward complications, discomfort during and after the time of surgery with the dichotomous option, and the reoccurrence of repigmentation in the study period of 90 days.
Materials and Methods
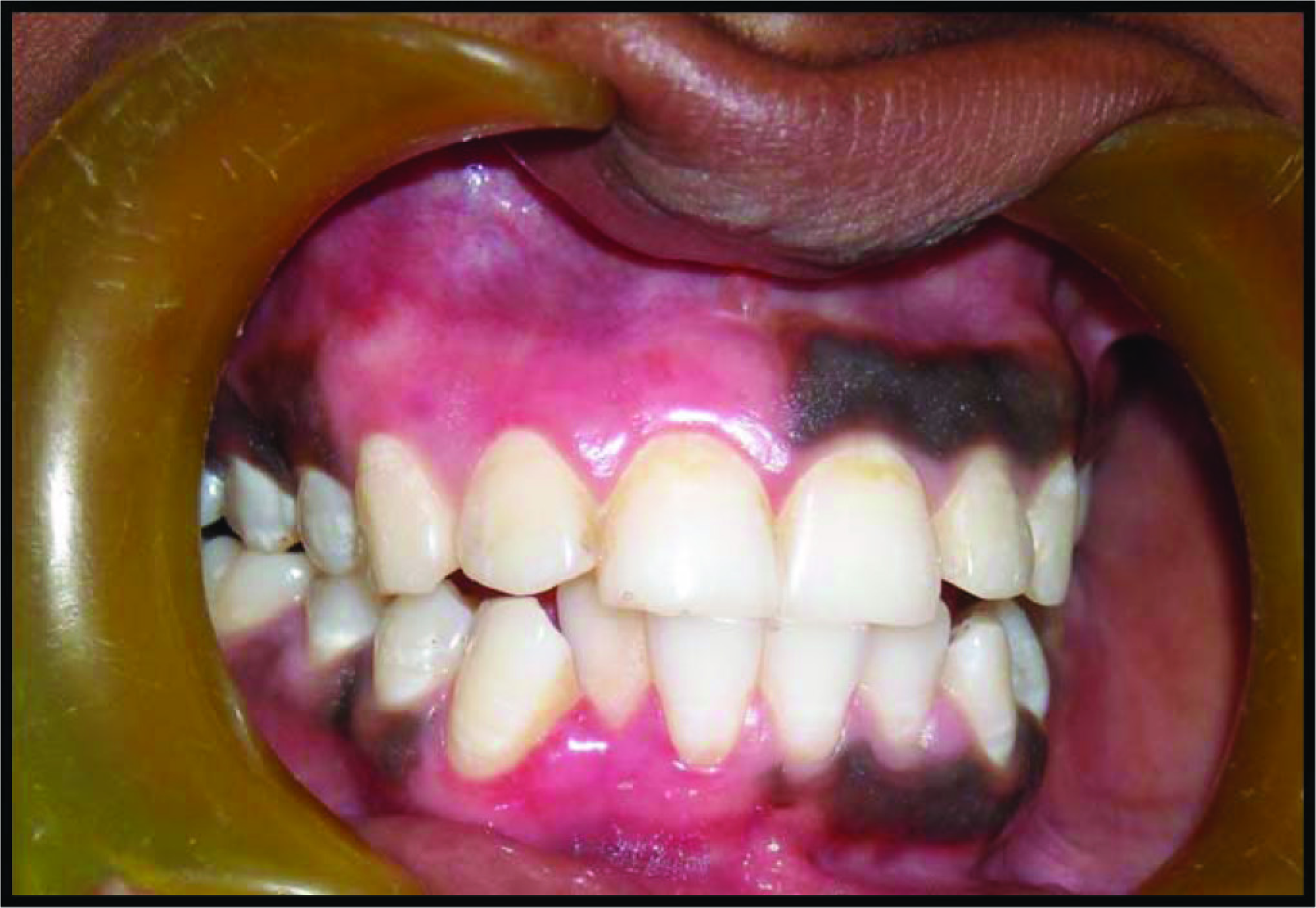
The study was conducted in 2015. Patients reporting to the Department of Periodontics, complaining of discoloration of gums and an unaesthetic appearance with a desire for aesthetic correction were enrolled. Those with physiological melanin pigmentation, acceptable level of oral hygiene, systematically healthy, with no reported adverse habits, and willing to undergo surgical intervention were included in the study. A total of 10 patients (5 males and 5 females) in the age range of 18 to 40 years with the Dummett oral pigmentation index 1 score 3 formed the study cohort (Figures 1 and 2). The sample size was calculated based on the pilot study results. It was carried out on 4 subjects who were excluded from the final study. The parameter assessed included the mean difference in the VAS from the baseline to immediate postsurgical intervention among the test and the control groups. 13
An informed consent was received and the patients were also explained about the possibility of reappearance of pigmentation. The study was conducted after an approval was obtained from the ethics committee of the researchers’ institution (cf. the ethical clearance letter number-IEC/PERIO/22-B/12), and all ethical principles were followed. The parameter assessed included the mean difference in the VAS from the baseline to immediate postsurgical intervention among the test and the control groups. The test arm VAS score was 1.9 ± 0.28 and the control arm VAS score was 0.6 ± 0.78.
The α error was set at 0.05%, whereas the β error was set at 80%. The sample size was calculated at 8 per treatment arm. To rule out the fall-out sample, the size of 10 per treatment arm was set.
Preoperative.
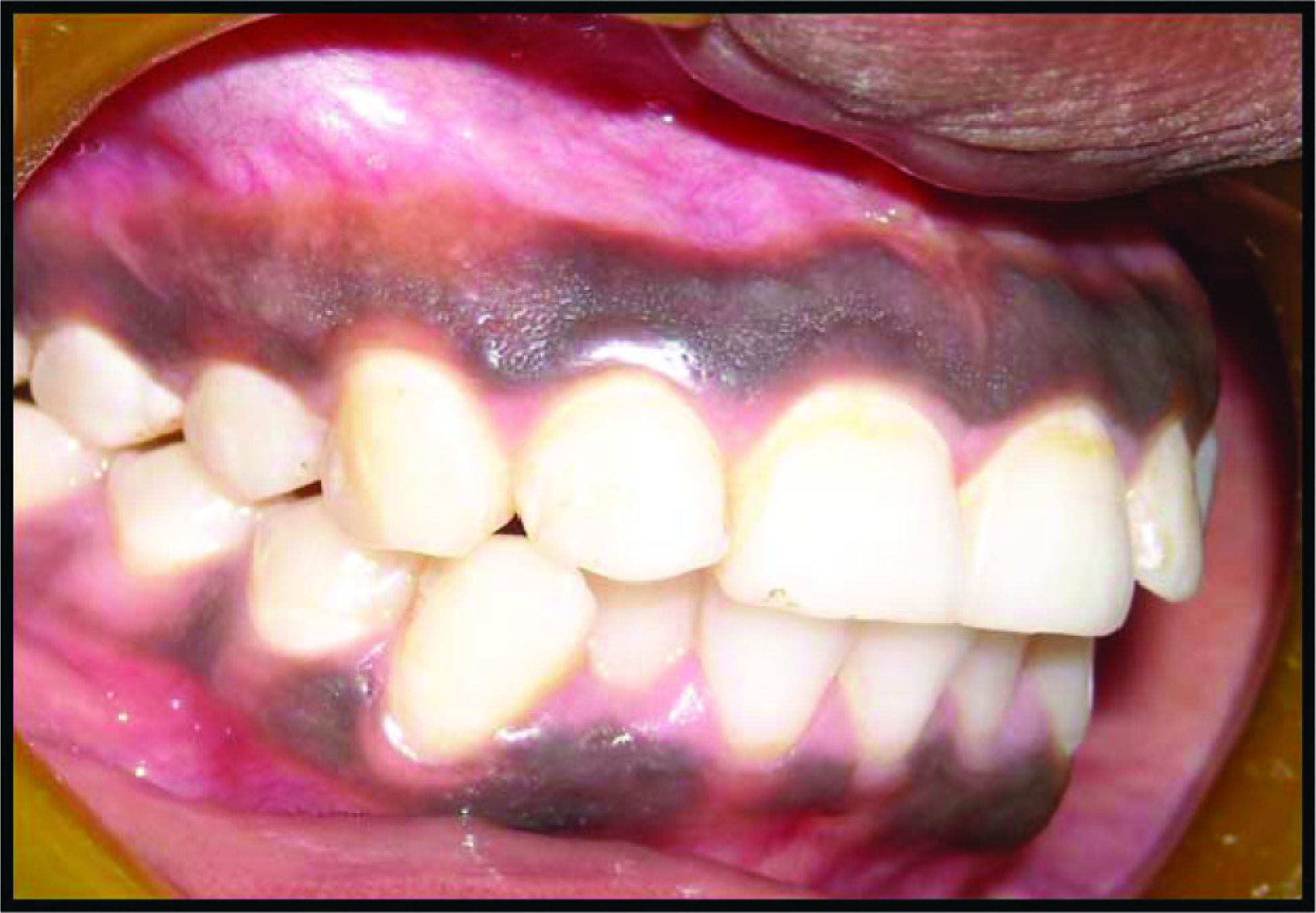
Demarcation of Surgical Site
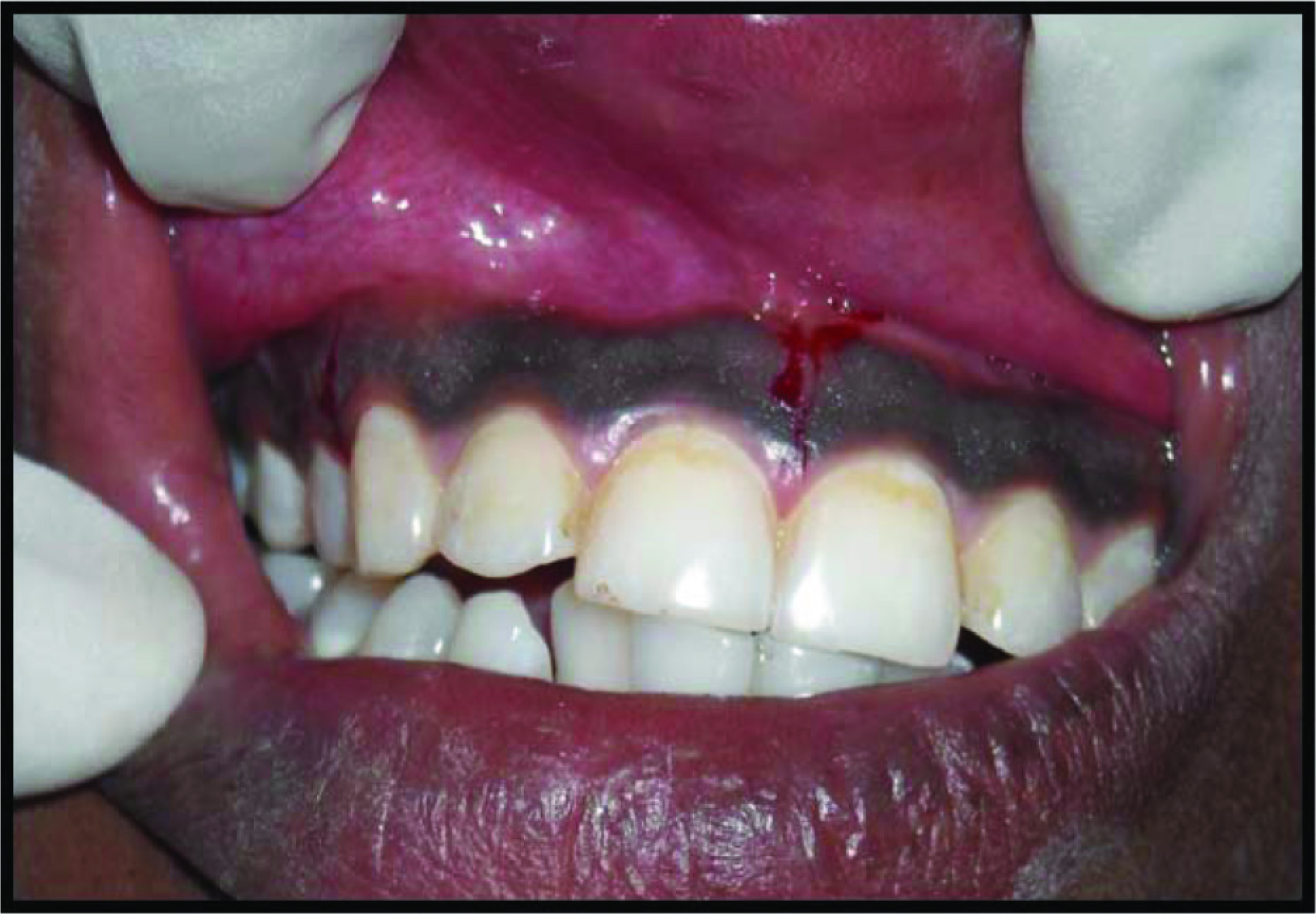
Phase I therapy was carried out prophylactically during the initial visit. A split-mouth approach comparing the scalpel technique with that of the diode laser was planned. Prior to surgery, local infiltration of 2% lignocaine was administered.
The maxillary or mandibular anterior regions extending from the central incisors to canines on the left side and on right side were randomly allocated based on the computer-generated random table for treatment by the diode laser and by the surgical scalpel technique on the same day.
In the region allocated for laser treatment, a diode laser (Zolar Photon Plus® 10 W) with the “depigmentation” mode was used for depigmentation. Exposure parameters were set using the recommended guidelines, followed by the careful removal of epithelium containing the melanin layer. When the diode laser technique was used, intraoperatively, the VAS score was 0. There was absolutely no bleeding during the procedure. The mean time consumed during maxillary and mandibular left arch depigmentation by the laser was (12:46:15 + 10:24:15 mins) 11:12:15 mins.
On the other side, the conventional scalpel technique was performed wherein a #15 blade was used for depigmentation (Figures 3 and 4).
Scrapping of Gingival Epithelium With No.15 Blade
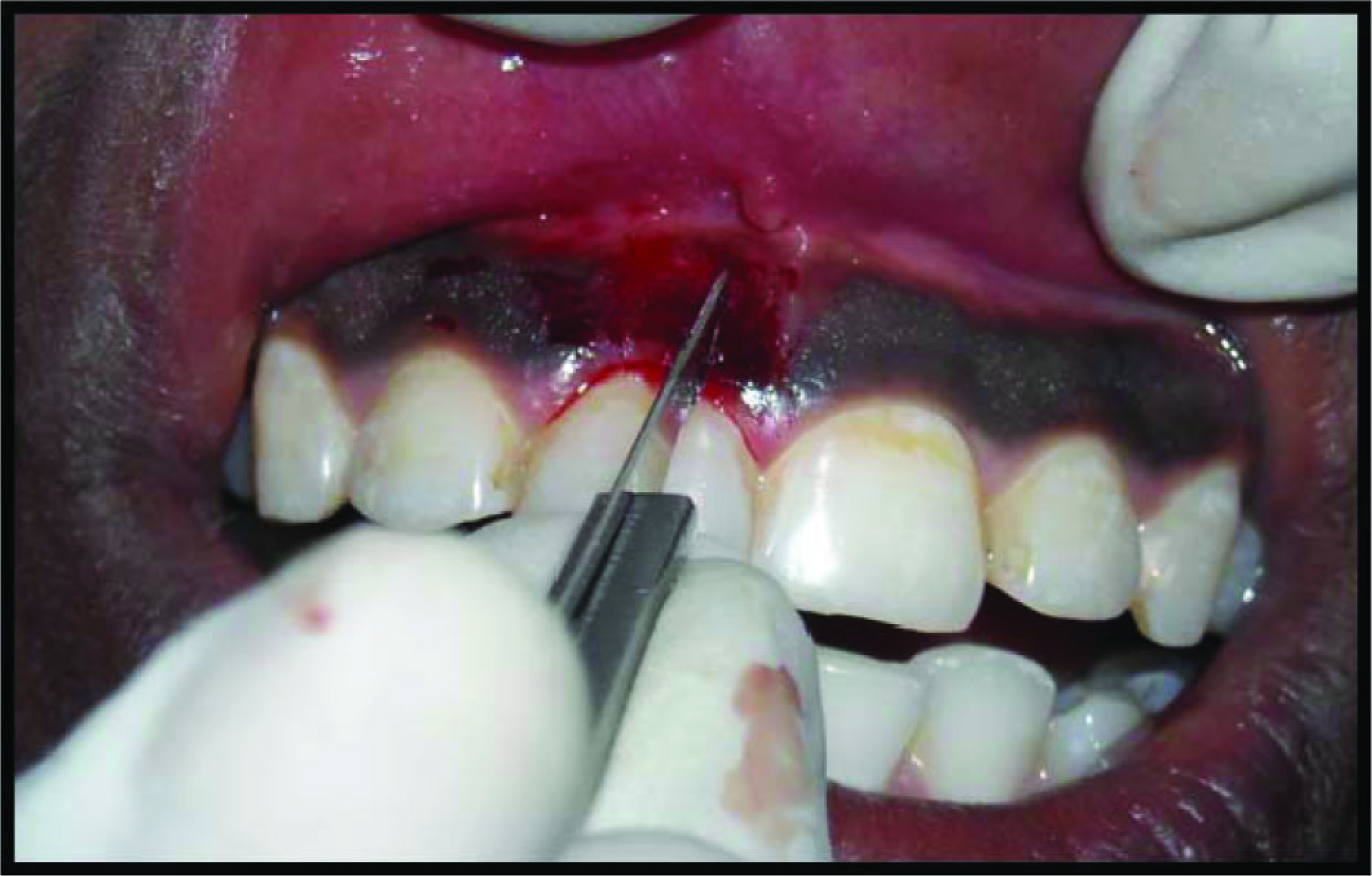
Postoperative
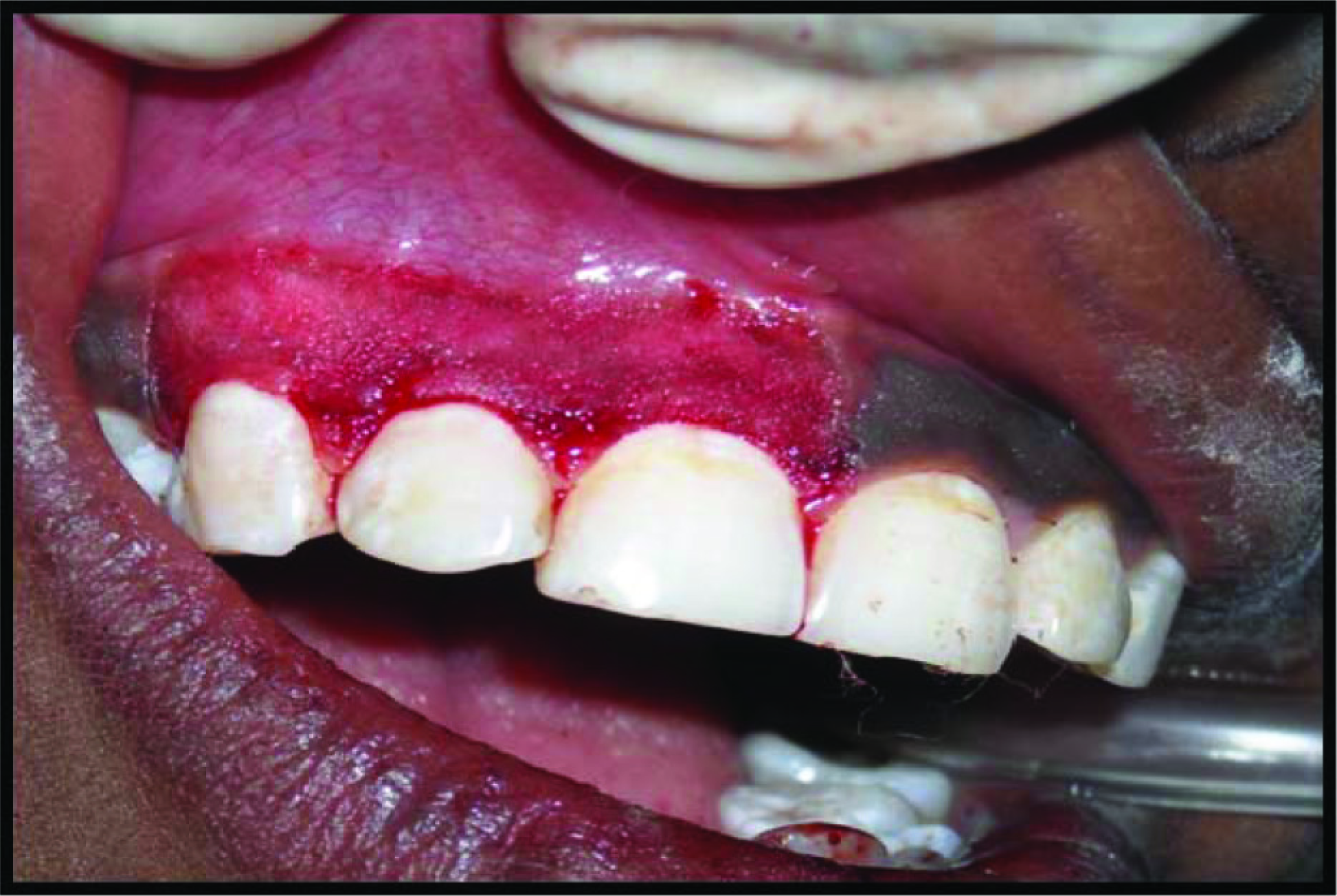
The VAS Pain Scale consisted of a 10-cm-long (100 mm) horizontal line, anchored at the left end by the descriptor “no pain” and at the right end by the descriptor “unbearable pain.” The patients were asked to mark the severity of the pain. The distance between these points, in centimeters, from the left end of the scale to the right end, were recorded and used as the VAS score: 0 = No pain;10 = Severe pain.
Upon completion of depigmentation, a periodontal dressing was placed over the surgical area. Written postoperative instructions were provided to the patients. Ibuprofen (300 mg) thrice daily for 3 days was prescribed to the patients for taking care of any postoperative discomfort. No postoperative complications were observed at sites treated by either of the techniques. Patients were recalled after 1 week for reevaluation. Healing of surgical wound was uneventful on both the sides (Figures 5 and 6). Patients experienced no discomfort and pain after 1 week on the side that was operated with the diode laser technique and slight discomfort on the side treated by conventional scalpel therapy. On 1 month postoperative follow-up, the areas were completely free from pigmentation and no discomfort was observed. The patients were recalled after 90 days for the reevaluation of repigmentation on both the surgically treated and laser treated sites.
Statistical Analysis
The mean and standard deviation (mean ± SD) values were calculated for VRSs for difference in pain experienced after 1 day and 7 days both on the laser and scalpel treated sites. Intragroup comparison was made using the t value, whereas the intergroup comparison of these indices was made using Tukey’s honestly significant difference test. Also, the Mann-Whitney nonarametric test was used to assess repigmentation appearance by the laser and scalpel techniques at 30 and 90 days postevaluation. The data were analyzed using SPSS version 11.
Periodontal Dressing Placed
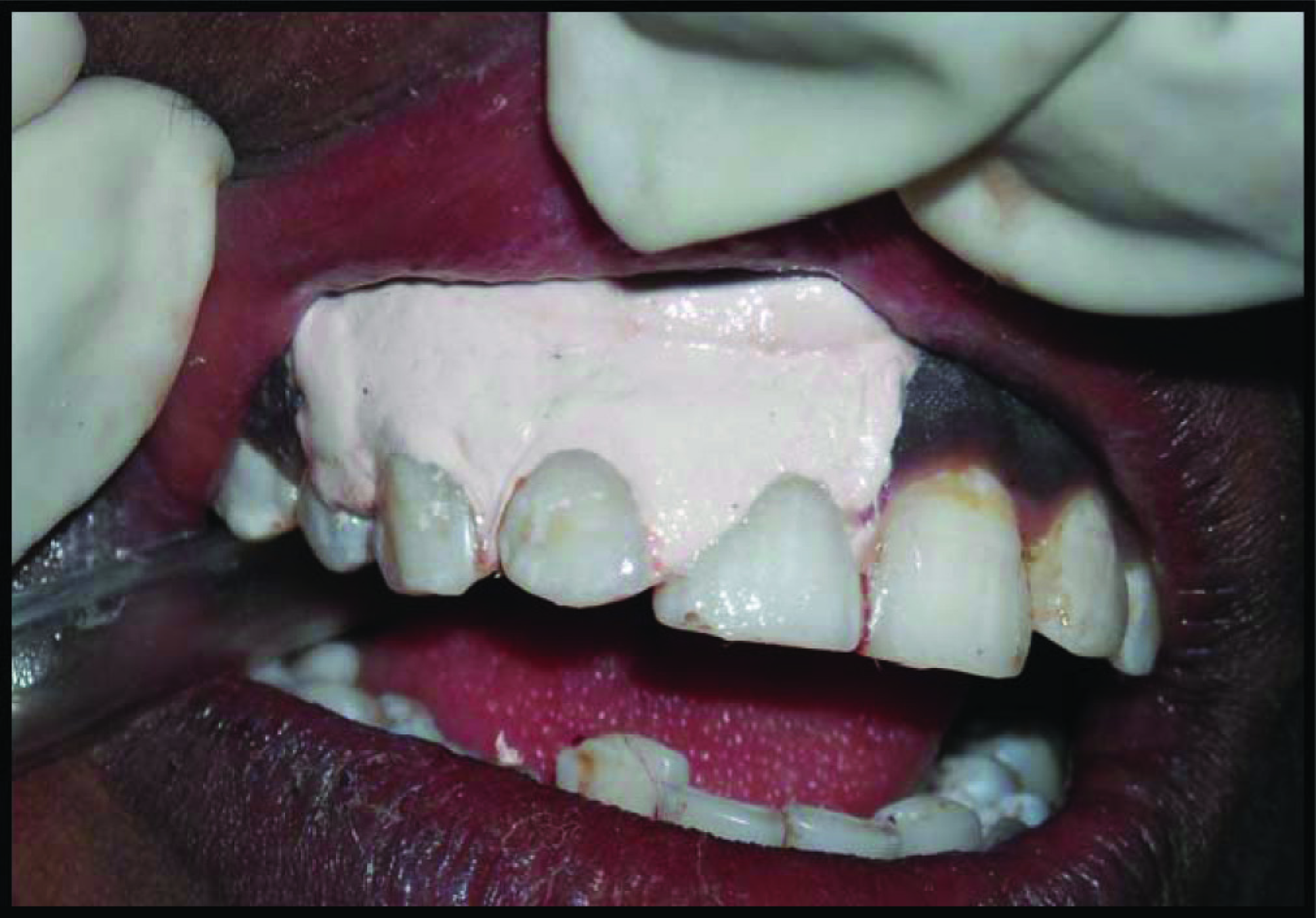
Postoperative After 6 Weeks
Results
Table 1 shows the VAS scores evaluated at days 1 and 7 of surgical intervention for depigmentation. Table 2 indicates the evaluation of Dummett Index for reappearance of melanin pigmentation at 30 and 90 days. Table 3 shows the time evaluation for depigmentation procedure.
VAS Scores to Evaluate Pain at Days 1 and 7
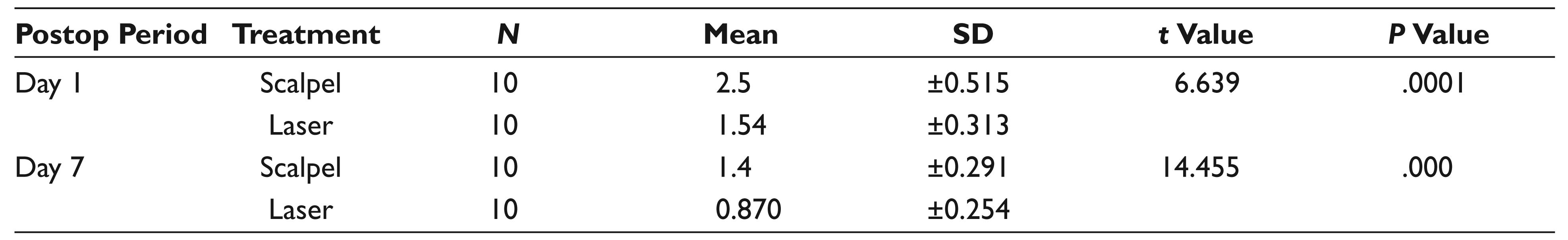
Abbreviation: SD, standard deviation.
Reappearance of Melanin Pigmentation Using the Dummett Index at Days 30 and 90
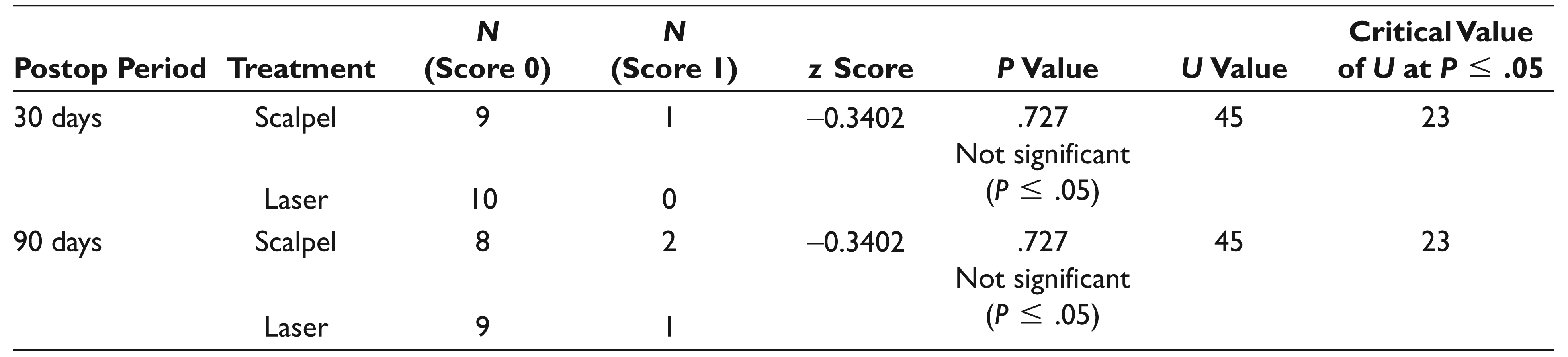
Time Taken for the Depigmentation Procedure
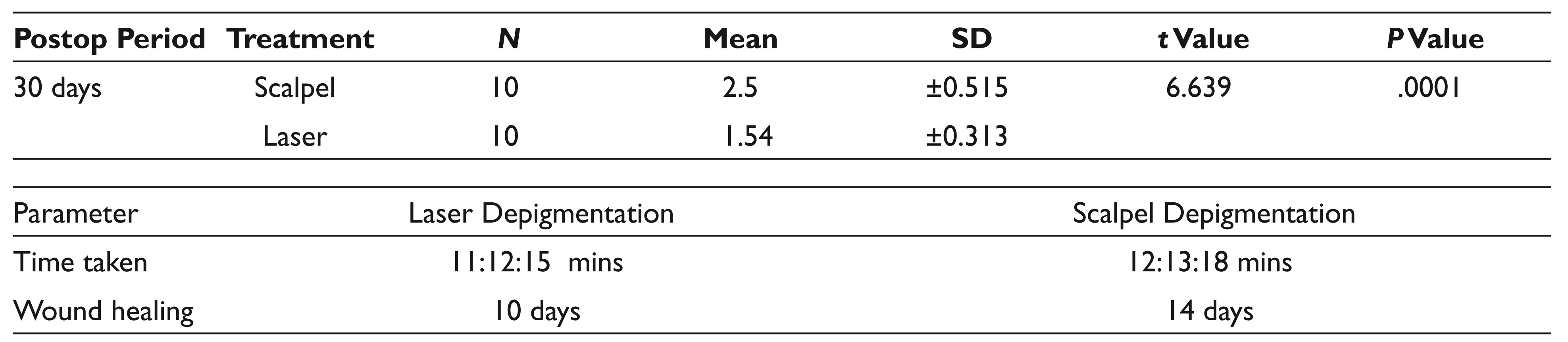
Abbreviation: SD, standard deviation.
Discussion
The scalpel surgical technique is a pioneering technique and is very popular till date due to the ease of application, easy availability of armamentarium, and affordability. 2 The procedure involves the surgical removal of gingival epithelium along with a layer of the underlying connective tissue, thereby allowing the denuded connective tissue to heal by secondary intention. The new epithelium that forms is devoid of melanin pigmentation.2,3 Laser techniques have, however, replaced the conventional surgical stripping.14,15
The present study was carried out to compare the depigmentation techniques of surgical stripping and diode laser.
The parameter assessed included the mean difference in the VAS from the baseline to immediate postsurgical intervention among the test and the control groups. The test arm VAS score was 1.9 ± 0.28 and the control arm VAS score was 0.6 ± 0.78.
In a split-mouth study in 2009, Lagdive et al 16 compared gingival depigmentation using the scalpel and diode laser techniques. There was no sign of bleeding at the depigmentation areas that were operated with the diode laser technique in any patient. Compared to scalpel blade depigmentation, diode laser depigmentation showed delayed healing. Pertaining to sites operated on with the scalpel blade, 2 out of 3 patients complained of moderate pain, and 1 patient complained severe pain on the VAS. In contrast, sites treated with the diode laser were rated as only slightly painful. All patients were satisfied with the aesthetically significant improvement in the gingival color with both the techniques. The study concluded that the application of the diode laser appears to be a safe and effective alternative procedure for the treatment of gingival pigmentation. Our study results corroborate with the results of the above studies.
Our result is supported by the study conducted by Mani et al 17 in 2009. They compared 3 different surgical techniques for gingival depigmentation: lasers, scalpel, and abrasion with the diamond bur on the same patient with the follow-up of 3 months. Compared with the scalpel blade and bur abrasion depigmentation, the diode laser technique showed delayed healing. At the VAS evaluation site operated on with the scalpel blade and bur abrasion, the patient complained of moderate pain, but at the site treated with the diode laser, only slight or no pain was recorded. However, the pain had reduced considerably 1 week after the surgery. The melanin pigmentation index score also showed that there was no recurrence of pigmentation at 3 months in the region operated by the diode laser technique. This was supported by the biopsies that were taken preoperatively and then at 3-month postoperatively.
Lee et al 18 in 2011 compared 2 different gingival depigmentation techniques using an erbium:yttrium-aluminum-garnet (Er:YAG) laser and rotary instruments using a split-mouth study design. The patients were satisfied with the aesthetically significant improvement with each method. The visual analog scale did not yield much difference between the 2 methods, with slightly more pain on the Er:YAG laser-treated site. The results of these cases suggest that the ablation of the gingiva by an Er:YAG laser and abrasion with a rotary round bur are good enough to achieve aesthetic satisfaction and fair wound healing without infection or severe pain. Prudent care about the gingival condition, such as the gingival thickness and degree of pigmentation along with appropriate assessment, is needed in ablation by the Er:YAG laser procedure. The study concluded that both depigmentation methods showed satisfactory results with regard to aesthetics, safety, and effectiveness. The results of the present study also showed that both lasers and scalpel are equally effective for depigmentation yielding aesthetic results.
The VAS score is an often used technique to elicit pain in clinical settings and is amenable to statistical evaluation. Perception of pain was reduced in laser-treated sites as compared with surgical stripping. This is in accordance with a study conducted by Karthikeyan and co-workers 19 and another study by Grover et al. 20
A similar study was conducted by Houshmand et al 21 and Ghoumand et al. 22
The results of our study revealed no discomfort postoperatively on the laser-treated sites and comparatively patients felt slight discomfort on the sites treated by the conventional scalpel method. Complete healing was observed on average at 10 days with the laser and 14 days with the scalpel. The mean time consumed in both the techniques was almost the same.
Strengths
– An alternative and plausible technique for depigmentation
– Split-mouth study with 2 treatment arms
Limitations
– Larger sample size could have been taken with a longer duration of observation period.
Future Research Directions
– Histological assessment could be included.
Conclusion
Gingival hyperpigmentation occurring due to local, systematic, environmental, or hereditary factors could be a major aesthetic concern for most patients. It is imperative to delineate the etiology before attempting to eliminate the gingival pigmentation. The present study revealed that aesthetic results by both techniques were excellent and comparable. Lasers offered less postoperative pain when compared with the scalpel technique. However, randomized controlled studies with larger study cohorts and longer follow-up periods to study the recurrence of repigmentation are required to establish the comparative efficacy and applicability of these techniques to ensure success and predictability.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
