Abstract
Purpose:
To evaluate the quality of reduction and clinical outcomes by using Percutaneous Distractor and Subtalar Arthroscopy Closed Reduction followed by Internal Fixation (PDSA-CRIF) in the intra-articular calcaneal fracture.
Methods:
A consecutive case series of 453 patients with 507 displaced intra-articular calcaneal fractures was recruited in this retrospective study. We performed PDSA-CRIF to treat intra-articular calcaneal fractures. The quality of reduction was assessed by early postoperative Computed Tomography (CT) scans and measurement of serial Bohler’s angles during follow-ups. Clinical outcomes were evaluated by Visual Analogue Scale (VAS) and the American Foot & Ankle Society ankle-hind foot scale (AOFAS) scoring system.
Results:
Fifty-nine patients (68 fractures) who had complete clinical data and follow-up of at least 12-months (mean: 14 months, range: 12–59 months) were finally included. Anatomical and near-anatomical reduction in subtalar articular surface which had less than 2 mm gap or step-off was found in 93% fractures. Unsatisfactory reduction was found in 7%.
Conclusion:
Arthroscopic-assisted percutaneous fixation using a distraction device is effective in achieving positive short-term results in the displaced intra-articular calcaneal fractures. A multicenter, large sample, randomized control trial is needed to fully evaluate the long-term effects of PDSA-CRIF in comparison to other methods.
Introduction
Intra-articular calcaneal fracture is relatively common and challenging to manage with adverse socioeconomic effects. 1 With increased understanding of its pathoanatomy and classifications, surgical reduction and internal fixation have become more common with better clinical outcomes 2 –5 in the last decade. Open reduction and internal fixation (ORIF) by extended lateral L-shaped incision has advantages of sufficient exposure for reduction and stable fixation. However, this approach suffers from high risk of postoperative soft tissue complications, occurring in up to 32% of cases, which can be difficult to manage. 6 –9 Alternatively, minimally invasive surgery (MIS) techniques in foot and ankle surgery including the sinus tarsi approach 10 –12 and arthroscopy are becoming more and more popular, which are proving to be effective techniques in treating intra-articular calcaneal fractures, with soft tissue complications only in 0–6% of cases. 12 –14
Here, we reported the clinical outcomes and experiences of using an MIS technique, percutaneous distractor and subtalar arthroscopic-assisted closed reduction followed by internal fixation (PDSA-CRIF) for intra-articular calcaneal fracture.
Materials and methods
In this study, we retrospectively reviewed a consecutive case series of patients with surgically treated intra-articular calcaneal fractures from April 2012 to July 2017 in the University of Hong Kong-Shenzhen Hospital and Shenzhen Pingle orthopedics Hospital. All records datasets were managed and maintained by the authors.
Our study was approved by the Medical Research Ethics Committee of The University of Hong Kong-Shenzhen Hospital Institutional Review Board with the approval number 202090. All patients included in the study had signed a paper of informed consent, and all patients had authorized their imaging data to be used in scientific research.
The inclusion criteria were: 1) adults aged >18 years old, 2) displaced intra-articular calcaneal fractures (≥2 mm displaced or gap), and 3) managed by Percutaneous distractor and subtalar arthroscopy closed reduction followed by internal fixation (PDSA-CRIF).
A consecutive case series of 453 patients with 507 displaced intra-articular calcaneal fractures was recruited in this retrospective study.
CT was performed for preoperative planning. The injured foot was elevated and temporarily immobilized in cast. Ice therapy was given three times per day. Surgical operations were performed within 2 weeks after the injury, provided that soft tissue conditions were optimal. 15
All patients received PDSA-CRIF by the same group of surgeons under general or spinal anesthesia. Patients were placed on a radiolucent operating table in a prone position with a cushion below the involved limb, creating a flat and stable surface for the surgery. To set up the distracting system, two 2.0 mm Kirschner wires (K-wires) were placed from lateral to medial; the first K-wire was inserted into the talus, and the second into the distal plantar region of the calcaneal tuberosity. With these two pins, a customized distractor was placed laterally and medially, allowing for disimpaction and partial restoration of the depressed subtalar primary fracture and realignment of the calcaneal body. For posterior tuberosity upper displaced fractures, we used tibio-calcaneal distraction methods to reduce calcaneal high and Bohler’s angle 16,17 (Figure 1). We used the distraction device (I.T.S., Lassnitzhöhe, Austria) described by Fröhlich. 18 The distractor also facilitated arthroscope insertion by widening the subtalar joint (Figures 2 –4).

For posterior tuberosity upper displaced fractures, we used tibio-calcaneal distraction methods to reduce calcaneal high and Bohler’s angle.

Intraoperative photo shows the calcaneus distractor.

Calcaneal distractor device (I.T.S., Lassnitzhöhe, Austria) described by Fröhlich. 10

Calcaneal distractor on the model.
A 2.7 mm arthroscopy was inserted into the subtalar joint through the anterolateral portal. Hematoma, bone and chondral fragments were removed with a shaver through the mid-lateral portal.
Firstly, we reduced the calcaneal articular surface under arthroscopy. Based on the appearance under arthroscopy, the fractures of the posterior articular facet were divided into three categories: big stable type fragments, small unstable fragments and comminuted fragments.
For big stable type fragments, reduction was achieved by using either the Essex-Lopresti technique or percutaneously using a hemostat to push the posterolateral joint fragment back to the same level as the sustentaculum tali with a step less than 1 mm. With the talar surface as a template, the anterior, lateral and posterior points of the subtalar joint were used as reference points to ensure a satisfactory reduction. After reduction was confirmed by arthroscopy, 1–2 screws were placed from lateral side across the posterior facet fracture lines into sustentaculum tali solid bone. We used 1–2 metal cannulated screw or absorbable subchondral screws as lag screws to maintain the reduction of posterior facet fragment (Figures 5 and 6). The screws must be within and not inferior to the sustentaculum tali.

We used one metal cannulated screw subchondral screws as lag screws to maintain the reduction of posterior facet fragment.

Postoperative CT shows anatomic reduction. We used one absorbable subchondral screws as lag screws to maintain the reduction of posterior facet fragment.
For small unstable fragments, the free fragment is elevated using a 2 mm K-wire or small joystick through an accessorial incision 2 cm below the lateral malleolus.
For comminuted fragments, percutaneous reduction and elevation of depressed lateral fragments through accessorial incision was attempted for each fragment. The articular surface is rechecked via arthroscopy prior to suturing the wound. If the free fragment was too small or failed for reduction so as to be unfixable by screw, a K-wire was considered for final fixation as early as possible to avoid further iatrogenic fracture.
Then, restoration of calcaneal body (the medial wall reduction and correction of hindfoot varus) were performed by distraction and monitored under fluoroscopy. We shorten the lateral side of the distractor, while maintaining traction on the medial side. Medial extension of the distractor between the talus and calcaneus raises the calcaneal medial wall, which can further aid the correction of the calcaneus varus. First, we use a talocalcaneal or tibio-calcaneal distractor 16,17 to expand the calcaneus length. Secondly, manual reduction was done to correct the posterior calcaneal part lateral displacement and varus deformity. Finally, use the intraoperative C-arm fluoroscopy of the lateral and axial positions of the calcaneus to confirm the reduction of the calcaneal body. If the body of the calcaneus and the medial wall are still significantly displaced, we insert the vascular forceps or a freer from the medial side for further reduction (Figure 7). Then, back to front screws are used to maintain reduction. Finally, we used intraoperative C-arm fluoroscopy to confirm fracture reduction (Figures 8 –14).

The body of the calcaneus and the medial wall are still significantly displaced, we insert a vascular forcep from the medial side for further reduction.

Preoperative lateral X-ray demonstrating a displaced intra-articular calcaneal fracture.
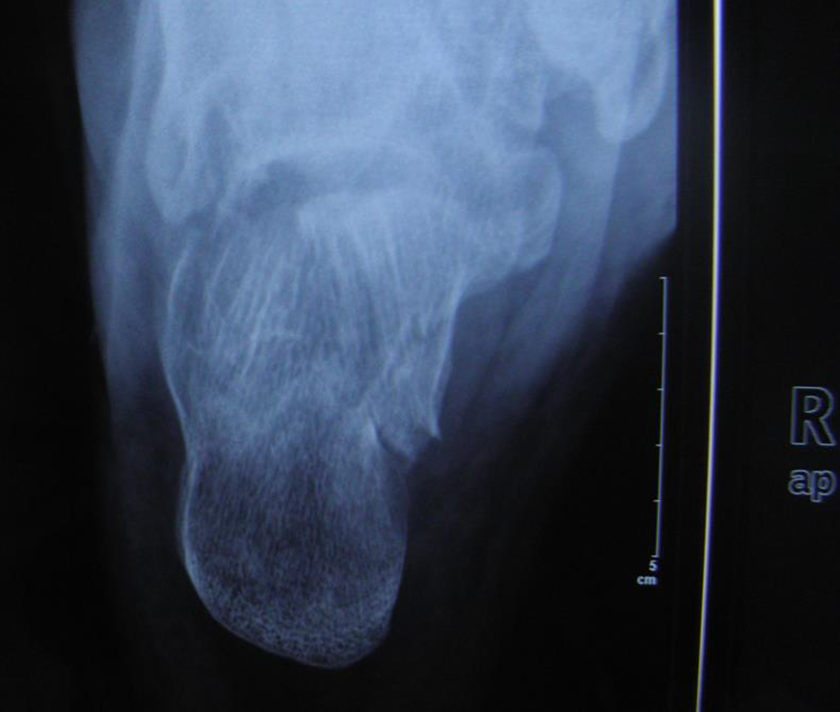
Preoperative axial X-ray shows calcaneal varus deformity.

Preoperative CT demonstrating a displaced intra-articular calcaneal fracture.

Intraoperative arthroscopy shows a big stable fragment with articular step-off before reduction.

Intraoperative arthroscopy shows anatomic reduction.
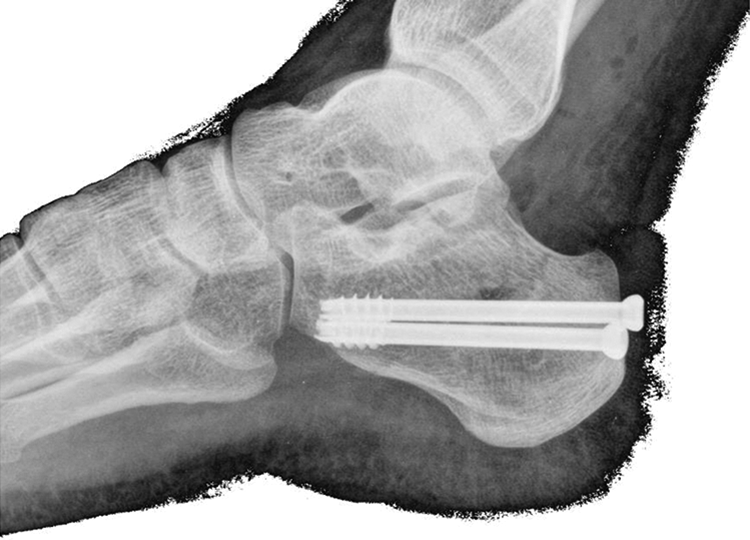
Postoperative lateral X-ray show anatomic reduction.

Postoperative axial X-ray shows no varus after calcaneal reduction.
For rehabilitation protocol, active ankle mobilization was allowed 1 week after surgery. Non-weight-bearing walking exercise was started at first 4 weeks, followed by partial weight-bearing for 6 weeks and then full weight-bearing walking exercise.
Complications were recorded after surgery and postoperative CT scans were obtained to further assess the quality of reduction (Figure 6). Bohler’s tuberosity-joint angle was measured on preoperative, postoperative, and periodic follow-up X-rays. Records of all imaging data were measured and verified by two independent senior doctors. VAS and AOFAS scored were obtained at final follow-up.
Data were analyzed using the SPSS 17.0 software packet. All materials carry on statistical processing, the measurement material were expressed as mean values and standard deviation. Data comparison at different time points before and after the operation was performed using paired t-test. Results of statistically significant differences were taken as P < 0.05.
Results
Because logistical and health-care policy limitations in our region, many patients were migrant workers from other regions of the country. There were 370 cases with a follow-up period of less than 1 year, and 294 of them had undergone postoperative CT examination. We have been following up for more than 1 year in 83 cases, of which only 59 patients (68 fractures) who had complete clinical data and follow-up of at least 12-months (mean: 14 months, range: 12–59 months) were finally included (Table 1). Postoperative complications were found in three cases (4%).One case had transient sural nerve palsy (1%). The other two patients complained of chronic foot pain (3%), which mainly localized to the lateral or plantar aspect of the hindfoot, but did not affect the patients’ daily activity. None of the patients had joint degeneration, arthritis, and no patients required secondary surgical fusion. All complications were treated successfully by nonoperative treatment. We extracted the data of preoperative Bohler’s angle for intra-observer and inter-observer reliability test. Intra-class correlation coefficient (ICC) was used for test. ICC less than 0.20 indicate poor consistency, from 0.20 to 0.40 means fair, from 0.40 to 0.60 means moderate, from 0.60 to 0.80 means good, more than 0.80 means excellent. 19 The mean ICC for different cord levels for intra-observer variation for MD was 0.832, and for inter-observer variation was 0.766, both of which indicated good and excellent reproducibility.
Baseline characteristics of patients and fractures.

There was significant difference in the Bohler’s tuberosity-joint angle between preoperative and immediate postoperative X-rays (2.029 ± 6.870 degrees vs. 16.382 ± 9.787 degrees) (P < 0.05). There was no significant reduction loss of Bohler’s tuberosity-joint angle between immediate postoperative and the final follow-up X-rays (16.382 ± 9.787 degrees vs. 15.647 ± 9.552 degrees) (P > 0.05) (Table 2).
Bohler’s angle on X-rays.

Postoperative CT scans were performed on all 59 patients (68 fractures). There was significant correction of subtalar joint and calcaneal body (medial wall) reduction based on comparison between preoperative and postoperative CT (Paired t-test, P < 0.05, P < 0.05) (Table 3).
Subtalar joint and calcaneal body (medial wall) fracture displacement on postoperative CT scans.

According to Sanders criteria for subtalar joint reduction quality on CT scan, 20 there was good or excellent reduction quality (≤2 mm gap or step-off) in 93% (63/68) of fractures (Table 4).
Subtalar joint reduction quality according to Sanders criteria on postoperative CT scans.

When we used postoperative CT scans to evaluate the reduction of subtalar articular surface fractures, we found that 63/68 (93%) of fractures achieved good or excellent reduction quality (≤2 mm gap or step-off) on immediate post-operation CT.
Discussion
In recent years, the use of arthroscopy in the treatment of intra-articular calcaneal fractures has achieved better clinical results than other MIS techniques. 21 Arthroscopy can achieve precise reduction of the articular surface while protecting the soft tissue. 22 In 2002, Gavlik et al. 23 reported the use of an arthroscopic MIS technique to treat 15 cases of calcaneal fractures, with a mean 1-year AOFAS score of 93.7 and a mean Maryland Foot Score of 95.8. In 2009, Schuberth et al. 24 described the use of this technique in 10 calcaneal fractures, and found that Bohler’s angle, articular surface reduction, and calcaneal body alignment, significantly improved without any soft tissue complications. Our study obtained similar results as we were able to significantly restore subtalar articular surface reduction and obtain good AOFAS and VAS scores using an arthroscopic technique.
Although the normal Bohler’s angle is 25–40°, the recovery of Bohler’s angle after calcaneal fracture is often not full anatomic reduction. 25,26 By comparison with the literature. 14,15,21,22 although the Bohler’s angle is less than 25° in many cases, in our case report, the Bohler’s angle is only 16° on average, which is indeed relatively small. First of all, in some early cases, although we restored the articular surface, the posterior calcaneal tubercle with upward displacement did not achieve full anatomic reduction, which resulted in a small Bohler’s angle. Later, for this type of fracture, we used the tibio-calcaneal instead of talocalcaneal distractor, which is helpful to restore the Bohler’s angle (Figure 1). Secondly, the measurement error caused by factors such as individual differences 27 and the quality of imaging films such as calcaneal rotation 28 needs to be taken into consideration. Gonzalez reported that the average measurement error was ±6°. 29
Regaining the height of the calcaneus and the Bohler’s angle is very important. 30 –32 However, the specific correlation between postoperative Bohler’s angle and clinical function is still inconclusive. 33 Paul believed that if the Bohler’s angle is greater than 10°, the clinical function is good. 34 Buckley et al. reported that if Bohler’s angle is greater than 15°, the clinical function at long-term follow-up is good. 35 This is consistent with our report. Although the Bohler’s angle was 16° after surgery in our patients, functional scores such as AOFAS and VAS were similar with literature (Table 5).
Compared with some studies using arthroscopy to treat calcaneal fractures.

As arthroscopy can only be used to monitor the reduction of the articular surface of the calcaneum, many authors proposed that the extra-articular portion of the calcaneus should be reduced by intraoperative fluoroscopy, especially when we treat joint depression type fractures. 15,21,23,36,37 The optimal reduction method for the extra-articular portion of the calcaneus remains controversial; Gavlik et al. 23 and Woon et al. 15 elevated the tuberosity fragment with a posterolateral percutaneous Schanz pin via the Westhues maneuver reduction method, while Schuberth et al. 24 used a posterolateral Schanz pin to perform reduction. Sivakumar et al. 21 used the Forgon and Zadravec three-point external fixator in their initial cases but found that it was inconvenient for arthroscopic insertion. In our study, we used the Fröhlich two-point distractor, which made tuberosity reduction simpler and made the arthroscope easier to insert and manipulate. 38
Our surgery time was 60 (45–155) minutes. This is shorter than that in Woon’s 15 study which is 95 (60–165) minutes, where arthroscopy plus the Westhues maneuver reduction method was used. The factor contributing to our shorter surgery time is that the two-point Fröhlich distractor is simpler to operate than Westhues maneuver methods. However, many other similar two-point distractors are also available. Some authors have used the Caspar Cervical Distractor (CCD) System to perform intraoperative temporary distraction, 39 while other author applied the two-point linear distraction method using specially designed traction devices. 18 Some author use a three-point distractor, which affects the reduction procedure under fluoroscopy. 40 So we do not advise to use a three-point distractor.
Improper operation of the distractor can result in vascular nerve damage, broken pins, ligament damage, and talus fractures. 41 However, when used properly, this risk can be greatly reduced. Beals was able to use a talocalcaneal distractor in 52 cases of subtalar arthroscopic surgery without any such complications. 42 In our study, we used a distractor without any of the above complications. The key to avoid complications is correct installment and gentle manipulation of the distractor.
We are in agreement with other authors, who emphasize the importance of reduction of the calcaneal body (medial wall) fractures. 43 Some author suggests that the reduction is unsatisfactory on intraoperative Harris-Beath view X-ray, they may convert to medial modified McReynolds approach. 43 But, there is no medial incision performed in our cases. We used a distractor to reduce calcaneal body fractures. Conventionally, we perform extension with the distraction device at first. Then, we focus on reduction of the subtalar joint under arthroscopy. After satisfactory joint reduction is achieved, we reduce the calcaneal body by use of the distractor under fluoroscopy. In our study, there was significant correction of calcaneal body reduction (medial wall) from 5.691 ± 2.469 mm preoperatively to 1.662 ± 1.589 mm postoperatively based on CT (Paired t-test, P < 0.05).
When we used postoperative CT scans to evaluate the reduction of subtalar articular surface fractures, we found that63/68 (93%) of fractures achieved good or excellent reduction quality (≤2 mm gap or step-off) on immediate post-operation CT. Our results are comparable with those of Sivakumar, where 7 of 8 (88%) patients had a reduction less than 2.5 mm. 21
Arthroscopic MIS is not without risk. A common complication of subtalar arthroscopy is nerve damage. Arthroscopy through the posterolateral portal is prone to damaging the sural nerve, and arthroscopy through the anterolateral portal is prone to damaging the lateral branch of the superficial peroneal nerve. 41 The literature reports that the nerve damage rate is 0.87% to 6.12% in subtalar arthroscopic surgery. 44 The “nick and spread” technique is important to avoid the nerve damage. In our study, we found a neurological injury rate of 1.47%.
Calcaneal reduction loss is another common complication after surgery. Some authors report an incidence of around 17%. 45 Singh and Vinay 46 recommend bone grafting as a possible solution. In their study, the reduction loss in patients given bone grafts (6.5 degrees on average) was significantly higher than patients without bone grafts (3.5 degrees on average). Backes et al. 45 believe that loss of reduction is associated with postoperative wound infection and substance abuse. Some authors try to find whether bone loss is related to the fixation material. 47 In a study by DeWall et al. 13 no correlation between bone loss and internal fixation material was found. After 4 months follow-up, they found no significant difference in bone loss between ORIF with plate fixation and percutaneous surgery with screw fixation only. In our study, when compared with immediate postoperative X-ray, there was no statistically significant reduction loss in the final follow-up (Paired t-test, P = 0.10).
Compared with the literature in Table 5, we found that the follow-up time is shorter in our data. However, our fracture reduction quality, surgery time and functional scores were similar or better than those reported in the literature.
This study has a number of advantages. Firstly, this is the first time to report the technique of combining a distractor with arthroscopy. Although some authors report the use of arthroscopy to treat intra-articular calcaneal fractures, the reduction of the calcaneal body still depends on manual traction reduction. 15,21,22,48 In our study, we used a distractor to open the calcaneus-talar joint space which is easy to insert arthroscopy to reduce the articular surface, and on the other hand, it is easier and faster to reduce the calcaneal body. Secondly, we use more restrictive postoperative CT examination to assess the quality of posterior facet fragment reduction.
There are three limitations in the present study. Firstly, the follow-up period was relatively short, and only 13% (59/453) of patients had a minimum 12-month follow-up. Longer follow-up periods and more complete follow-ups will be necessary to fully evaluate clinical outcomes. Secondly, there was no control group that used traditional ORIF treatment methods. Thirdly, although our case had good clinical function, the postoperative Bohler’s angle was small. This technique under-reduced the posterior facet. The height was not easily obtained and maintained by using this technique.
Conclusion
Arthroscope-assisted percutaneous fixation using a distraction device is effective in achieving positive short-term results of displaced intra-articular calcaneal fractures. A multicenter, large sample, randomized control trial is needed to fully evaluate the long-term effects of PDSA-CRIF in comparison to other methods.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
