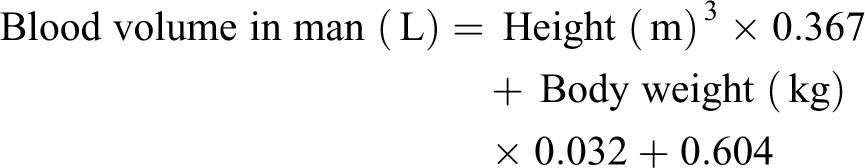Abstract
Introduction:
Although intraarticular tranexamic acid (IA-TXA) administration or drainage clamping are popular methods used to reduce blood loss after total knee replacement (TKR), the protocol remains controversial. We aimed (1) to establish new protocols through investigating whether two methods, that is, low-dose (500 mg) IA-TXA plus 30-min drain clamping and drainage clamping for the first 3 h without IA-TXA, can reduce blood loss and blood transfusion after unilateral TKR and (2) to make recommendations related to clinical application.
Materials and Methods:
This study, conducted from September 2014 to June 2016 related to enrolled 95 patients with primary osteoarthritis who were to have a unilateral cemented TKR, was nonrandomized and retrospective. In group A, the drain was released following tourniquet deflation. In group B, 500-mg TXA was injected into the knee joint via a drain tube after fascia closure and the drain was clamped for the first 30 min to prevent leakage. In group C, the drain was clamped for the first 3-h postoperation. Demographic characteristics and clinical data were collected, including the levels of hematocrit (Hct), the total blood loss (TBL), drained blood volume (BV), the amount of blood transfused, and any complications that developed.
Results:
We found a significantly lower postoperative TBL, drained BV, decreasing Hct level, and less transfused BV in the IA-TXA injection group (group B) and the 3-h drainage clamping group (group C) compared to the conventional negative drainage group (group A; p < 0.001). There was no significant difference between groups B and C (p = 0.99).
Conclusions:
The drainage clamping method can be safer than IA-TXA administration in patients with risk factor of venous thromboembolic complication. Furthermore, the IA-TXA administration can be more optimal than drainage clamping in patients with high bleeding tendency or lateral retinacular release during TKR, who would be concerned about postoperative wound complication.
Introduction
Total knee replacement (TKR) is a major surgery associated with considerable blood loss, and a transfusion may be necessary in some cases. 1 –3 Recently, there have been many attempts to reduce postoperative bleeding and avoid the risks of transfusion-related complications, such as additional costs, viral disease, bacterial contamination, as well as serious acute and delayed noninfectious transfusion reactions. 2
Tranexamic acid (TXA) has demonstrated the ability to decrease postoperative bleeding and the proportion of patients requiring postoperative blood transfusion. 1 The either intravenous (IV) or intraarticular (IA) injection is applicable. However, IV-TXA may be dangerous, exposing patients to an uncertain risk of drug-induced venous thromboembolism (VTE) complication from prolonged high systemic drug level. 3 There has been a growing interest in using TXA as an IA agent in TKR. 4 –9 Several studies have reported a significant reduction in blood loss and transfusion requirements with IA-TXA injection plus drainage clamping for 30 min to 1 h. 6,10,11 Sa-Ngasoongsong et al. developed a new IA-TXA method that combines low-dose TXA (250 mg) with 2-h drain clamping for reducing blood loss and transfusion in TKR without any significant complications. 4 Roy et al. reported that 500-mg IA-TXA plus 1-h drain clamping significantly reduced the drain output at 48-h postoperation and blood transfusion after primary unilateral cemented TKR compared to the control group (5 ml of 0.9% saline).5 Therefore, we postulated that the IA-TXA following TKR may decrease postoperative blood loss and decrease the need for blood transfusions without adversely affecting the overall treatment protocol.
Temporary drainage clamping after TKR has also been attempted to reduce postoperative bleeding. There are various treatment regimens for the management of suction drains in TKR, including immediate clamping, 1-, 4-, and 24-h clamping, respectively, free drainage and their variations. 2,12 –15 Shen et al. suggested that drainage clamping within the first 4-h postoperation reduced postoperative blood loss without causing excess morbidity after TKR compared to conventional drainage, and there was the wound problem of severe bruising with limited skin-edge necrosis in 2.3% of the drainage clamping group. 13 Kiely et al. concluded that drain clamping for 2 h has no benefit in routine TKR, and a longer period of drain clamping may be required. 14
To date, there remain no guidelines for implementing IA-TXA, such as the TXA dosage which varies from 250 to 3000 mg and the optimal drain clamping time after joint injection. We presumed that the IA-TXA (500 mg/5 ml) administration within a narrow and restricted joint cavity would be sufficient to create a high drug concentration without resulting in increased postoperative thromboembolic events and that the first 30 min after joint injection is the optimal clamping time to prevent leakage of TXA solution from the IA space and eliminate confusion with the tamponade effect by drainage clamping. Furthermore, no consensus has been realized for defining a clamping protocol, such as the period of clamping. 1,16 We also assumed that the most critical time zone forming the tamponade effect is 3 h after the operation when most bleeding occurs, and clamping for more than 3 h can lead to increased wound complications. The purpose of our study was (1) to investigate whether two methods, that is, low-dose (500 mg) IA-TXA plus 30-min drain clamping and drainage clamping for the first 3 h without IA-TXA, can reduce postoperative blood loss and blood transfusion after unilateral TKR in severe osteoarthritis (OA) and (2) to make a recommendations related to clinical application.
Methods
This study, conducted from September 2014 to June 2016 related to enrolled 95 patients with primary OA who were to have a unilateral cemented TKR, was nonrandomized and retrospective. We excluded patients with secondary OA (e.g. rheumatoid arthritis, gouty arthritis, postseptic arthritis), history of thromboembolic disease, bleeding diathesis, previous open knee surgery, and revision TKR. The 95 patients were allocated to one of three groups. In group A (n = 30), or the conventional negative drainage group, the drain was released following tourniquet deflation. In group B (n = 30), or the IA-TXA injection group, 500 mg of TXA was combined with physiologic saline to create a 25-ml total volume, and then, this solution was injected into the knee joint via a drain tube after fascia closure and the drain was clamped for the first 30 min to prevent leakage. In group C (n = 35), or the 3-h drainage clamping group, the drain was clamped for the first 3-h postoperation. In our calculation of numbers, 30 cases were enough to compare mean value among three groups at the level of power analysis (0.8) and significance value (0.05). Our study was focused on blood loss, the need for blood transfusion, and postoperative complications among the three groups.
The surgery was performed by one of the authors, an experienced arthroplasty surgeon. The prostheses used in this present study were the NexGen total knee system (Zimmer Inc, Warsaw, Indiana, USA). The same surgical technique was performed in all cases. Under spinal anesthesia, a pneumatic tourniquet was placed around the upper thigh and inflated to a pressure of 350 mmHg after the extremity had been drained of blood by applying a rubber bandage. The knee joint was exposed through a midline skin incision and a medial parapatellar arthrotomy. All prosthesis components were inserted with full cementation (Optipac® 80, Biomet Orthopaedics GmbH, Switzerland). At the end of the surgical procedure, a standard drain tube with an external diameter of 3.2 mm was inserted into the knee joint. The tourniquet was deflated just before we started to close the wound, and then we confirmed hemostasis of wound through the cauterization of visible bleeding point. All patients were screened for complete blood count, platelet count, prothrombin time, and partial thromboplastin time. All patients had antithrombotic prophylaxis with rivaroxaban (Xarelto®, Bayer Pharma AG, Leverkusen, Germany, Janssen Pharmaceutica) and intermittent pneumatic compression device until their discharge date. Antibiotic prophylaxis was given at the start of surgery and continued for 5 days. All drains were removed within 48-h postoperation, and the drainage volume was recorded at 24- and 48-h postoperation. Thromboembolic complications, such as clinical deep vein thrombosis (DVT) and pulmonary emboli, and other complications (e.g. wound complications) were noted during the hospital stay. All patients were discharged from the hospital at 14 days after surgery.
We compared postoperative change of hematocrit (Hct), volume of blood loss, volume of drained blood, volume of hidden blood loss, and amount of packed red blood cell (RBC) transfusion among three groups. The indications for blood transfusion were hemoglobin (Hb) <9.0 g/dl and/or clinical criteria were syncope, dyspnea, tachycardia, hypotension, angina pectoris, and transient ischemic attack. The dates and times of transfusions and the number of units of transfused RBC concentrates were recorded. The intraoperative blood loss was not measured, but Hb and Hct levels were assessed at the preadmission visit and at 06:00 of 1, 2, and 5 days after surgery to calculate total blood loss (TBL). The TBL was calculated 5 day after surgery using the Mercuriali formula. 17 This formula required the patient’s blood volume (BV), calculated through the Nadler formula (in milliliters of blood) 18 , and the volume of RBCs transfused. If a transfusion was performed, a unit of RBC concentrate containing the standard 200 ml of RBCs was used.
The Mercuriali formula is expressed in milliliters of RBC
Nadler’s formula is as follows:
The IBM Statistical Package for the Social Sciences version 19.0 (Chicago, Illinois, USA) was used for statistical analyses of indices. Quantitative data were presented as the mean ± standard deviation. Differences in the mean among the three groups were analyzed using one-way analysis of variance. A significant difference was considered at p value < 0.05.
Results
The three groups were homogenous in their demographic characteristics (Table 1). The mean Hct decrease for the 5-day postoperation was significantly lower (p < 0.001) in group B (5.2 ± 3.3%) and group C (6.2 ± 2.3%) compared to group A (9.0 ± 3.5%; Table 2 and Figure 1(a)). There was no difference (p = 0.56) between groups B and C. The TBL was significantly lower (p < 0.001) in groups B (603.6 ± 192.6 ml) and C (633.1 ± 141.7 ml) compared to group A (1158.6 ± 223.2 ml; Table 2 and Figure 1(b)). Furthermore, no significant difference between groups B and C was evident (p = 0.99). The volume of drained blood in groups B (353.3 ± 172.2 ml) and C (376.9 ± 147.3 ml) was also significantly lower (p < 0.001) than in group A (862.7 ± 143.2 ml; Figure 1(c)). The volume of blood transfused in groups B (416.7 ± 111.7 ml) and C (422.9 ± 135.2 ml) was significantly lower (p < 0.001) than in group A (823.3 ± 150.1 ml; Table 2 and Figure 1(d)). Also, no significant difference in drained BV (p = 0.99) and transfused BV (p = 0.99) existed between groups B and C. Meanwhile, the volume of hidden blood loss revealed no significant difference (p = 0.87) among the three groups. Regarding complications, no wound infections or clinical VTEs were detected in either group during a minimum 1-year follow-up.
The patients' preoperative characteristics data.

Hct: hematocrit.
aThe values were presented as mean (standard deviation).
bThe values were presented as number of patients having that condition (percentage of this group).
Blood loss and blood transfusion outcome in three groups.

Hct: hematocrit; RBC: red blood cell.
aThe values were presented as mean (standard deviation).

(a) Results of decreasing Hct (%) that compared each groups. (b) Results of volume of total blood loss (ml) that compared each groups. (c) Results of volume of drained blood (ml) that compared each groups. (d) Results of packed RBC transfusion (ml) that compared each groups. Hct: hematocrit; RBC: red blood cell.
Discussion
Blood loss and transfusion are important postoperative features that must be considered in TKR. 16 The various methods have been suggested to reduce blood loss following TKR, such as autotransfusion, hypotensive anesthesia, IV-TXA administration, 19 IA-TXA injection, and temporary drain clamping. 2,12
Recently, IA-TXA application has become one of the most popular methods for reducing blood loss and transfusion requirements in conventional TKR. 4 –8 TXA is a synthetic antifibrinolytic drug used to prevent bleeding. 20 Several methods including intramuscular, IV, and IA administration of TXA have been used to reduce blood loss in patients undergoing TKR for severe OA. 21 The time before maximum TXA plasma levels are attained is reportedly 30 min for intramuscular and 5−15 min for IV administration. 22,23 An IV injection for patients undergoing TKR is the best method to rapidly increase and maintain the therapeutic concentration of TXA. Orpen et al. suggested that a single TXA injection of 15 mg/kg, given at the time of cementing the prosthesis in TKR, before deflation of the tourniquet, significantly decreases the amount of blood loss in the early postoperative period and is not associated with an increase in thromboembolic complications. 19 However, due to safety concern of the VTE complication, there has been a growing interest in using TXA as an IA agent in TKR. 4 –9 Sa-Ngasoongsong et al. suggested that combining a low-dose IA-TXA (500 mg) with 2-h drainage clamping is effective for reducing postoperative blood loss and transfusion in conventional TKR, and VTE complication, DVT, was developed in 4.0% of the IA-TXA group. 1 Mutsuzaki and Ikeda concluded that IA injection of TXA (1000 mg) plus 1-h drainage clamping is effective for reducing TBL and transfusion rates compared to the control group. 10 First of all, VTE complications must be taken into consideration for IA-TXA administration protocols, although safer than the IV-use method. There was no case of VTE complications in our study, but it cannot be concluded that it will not happen. Hence, clinical thromboembolic events such as DVT and pulmonary thromboembolism need to be monitored. Second, we also thought that if the drain clamping time for preventing TXA solution from leaking from joint cavity is longer than 1 h, it can be confused with the tamponade effect. In our study, low-dose (500 mg) IA-TXA plus 30-min drain clamping is advantageous for reducing TBL and blood transfusion requirements without thromboembolic complication.
Drainage clamping is also a simple method that reduces blood loss after TKR. The technique induces temporary hemostasis by creating an IA tamponade, 13 which, when released, allows for blood removal through drains, preventing wound hematoma. Most of the blood loss in TKR occurs during the first few postoperative hours (37% and 55% at 2 and 4 h, respectively). 24 Thus, it seems reasonable to clamp the drain tube in the first few hours after TKR to create a tamponade effect for bleeding control. While some authors have reported a significant reduction in blood loss through drainage clamping, others have found no difference either in calculated blood loss or transfusions. 16,25 –27 The drain clamping technique can be classified into two main patterns. The first pattern is a single period of temporary clamping ranging from 1 to 24 h after surgery. 12 –15,27 Stucinskas et al. suggested that in patients with severe OA undergoing TKR, 4-h clamping of the drain reduces postoperative blood loss without increasing clinical thromboembolic events and wound complications. 2 The second is an intermittent or interval clamping pattern that switches back and forth between clamped and unclamped periods. Raleigh et al. concluded that drainage clamping for 115 min and releasing for 5 min every 2 h until 6-h postoperation results in significantly less external blood loss with no change in morbidity or mortality. 28 On the contrary, Tai et al. concluded that drain clamping after TKR does not effectively reduce blood loss or significantly improve any outcomes based on current evidence, and there were wound problems such as acute infection, bruising, and severe oozing in 2.9% of the drainage clamping group. 29 First of all, wound complications such as hematoma and acute infection must be taken into consideration for long-period drain clamping protocols. Yamada et al. demonstrated that the hemostatic effects are similar between the 1- and 24-h drain clamping methods after TKR, though there were significantly more complications in the 24-h drain clamping method. 27 Therefore, the balance between creating a tamponade effect and reducing wound complications is important in patient’s prognosis. An optimal protocol for the number of hours needed for drain clamping has not been established. 16,29 In this study, a postoperative 3-h drain clamping is advantageous for reducing TBL and blood transfusion requirement without wound complication compared to conventional drainage.
As described above, the results show that the two methods have safety and efficacy related to hemostatic changes compared to the control group. However, IA-TXA administration may not be a good method for patients with a risk factor of VTE complication, such as previous DVT history. VTE is a complication that can occur after total hip replacement or knee replacement surgery, despite prophylaxis such as medication or an intermittent pneumatic compressive device. The literature reports an incidence of VTE events that reaches 2.7%. 30,31 Although there was a limitation related to comment potential complication of IA-TXA due to small numbers of our study, drainage clamping method can be safer than IA-TXA administration in patients with a risk factor of VTE complication. It is also thought that drainage clamping may be not a good method in patients with a high bleeding tendency, who are concerned about wound complication postoperatively. Drainage clamping can be a dangerous approach, if the patient has a history of preoperative aspirin use or prothrombin time [PT] prolongation in the laboratory examination. In addition, lateral retinacular release is performed to improve patellar tracking during TKR, which can also be a factor in causing subcutaneous hematoma through postoperative bleeding at the released site. Molyneux and Brenkel demonstrated that lateral release patients had higher transfusion rates (20.3% vs. 10.1%) than nonlateral release patients. 32 The IA-TXA administration can be more optimal than drainage clamping in patients with high bleeding tendency or lateral retinacular release during TKR, who would be concerned about postoperative wound complication.
Conclusions
We propose that two methods, that is, low-dose (500 mg) IA-TXA plus 30-min drain clamping and drainage clamping for the first 3 h without IA-TXA after unilateral TKR, can be secure protocols for reducing postoperative blood loss and the need for blood transfusions. We confirmed that these methods could reduce TBL, drained BV, decreasing Hct for 5-day postoperation, and volume of transfused RBCs compared to conventional negative drainage. Clinical thromboembolic events or wound complications such as hematoma and acute deep infection after TKR need to be monitored. The drainage clamping method can be safer than IA-TXA administration in patients with a risk factor of VTE complication. Furthermore, the IA-TXA administration method can be more optimal than drainage clamping in patients with high bleeding tendency or lateral retinacular release during TKR, who would be concerned about postoperative wound complication.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by Inha University grant.