Abstract
A large number of materials with different compositions and shapes have been proposed and studied for the purpose of bone tissue regeneration. Collagen-based materials have shown promising results for this application, with improved physicochemical properties. The aim of the present in vivo animal study was to evaluate and compare two commercially available collagen-based biomaterials for bone regeneration, with these being implanted in circumferential bone defects created in the calvarium of rabbits. Twenty rabbits received bilateral parietal osteotomies, performed with the aid of a 6.5 mm diameter trephine. Two groups were created: the BC group, where the defect was filled with a scaffold composed of 90% bovine bone particles and 10% porcine collagen, and the EG group, where the defect was filled with a scaffold composed of 75% hydroxyapatite particles of bovine origin and 25% bovine collagen. Ten animals were sacrificed at 30 days and another 10 at 45 days after implantation, and the samples were processed and histologically analyzed. In the evaluations of the samples at 30 days, no important differences were found in the results. However, in the samples at 45 days after surgery, the EG group showed better results than the BC group samples, mainly in terms of the amount of bone matrix formation (
Introduction
Due to their predictability, dental implants have become a safe alternative for the rehabilitation of missing teeth; despite their success rate being quite high, micro-, and macrogeometric alterations are continually proposed.1–3 However, for the installation of these implants, it is essential that there is adequate bone structure, which is normally affected after tooth loss, as the alveolar bone loses a large part of its volume during the healing process. To recover the bone volume needed for implant placement, regenerative bone grafts are often used. Among the types of grafts, autogenous bone (taken from the patient) is obviously considered the best material, due to its osteoconduction, osteoinduction, and rapid remodeling properties, resulting in better-quality neoformed bone tissue.4–6 However, the morbidity resulting from the removal of the graft in the donor area presents inconveniences such as pain, paresthesia, hematoma, hemorrhage, risks of bone fractures in the donor area, and limited bone graft amount, among others.7,8 Therefore, there is a growing search for alternative bone substitutes that have physicochemical properties and biological behavior similar to those of autogenous bone.
Different materials with different forms, composition, and methods of production have been researched and proposed. However, the most used and researched are materials in particles form.8–10 These particulate materials, depending on the morphology of the defect and location, may present problems for transport, accommodation of the graft in the receptor site, and adequate stability of this material to that the repair process can occur adequately. Thus, new materials were developed using the benefits found in these particulate materials and by adding collagen to facilitate the accommodation of the material in the grafted bed and improve its stability.
Materials made from collagen have shown low antigenicity, excellent biocompatibility, and osteconductive and osseointegrative properties much better than those of systems made from synthetic polymers, such as lactic polyacid, glycolic polyacid, and polyethylene terephthalate.11,12 In their function as scaffolds, materials based on collagen, in their sponge form, are considered three-dimensional scaffolds with the best properties for tissue regeneration.13–15 Collagen is easily degraded and is reabsorbed by the body, allowing good cell adhesion, migration, proliferation, and differentiation; however, its mechanical properties are relatively weak compared to those of bone,16–18 for this reason, particles of other more resistant compounds are incorporated in order to improve their mechanical properties and absorption time, especially when used for bone regeneration. At present, it is known that there are 29 different types of collagens have been discovered; however, type I is the most used for applications in bone tissue engineering.19,20
Scaffolds of hydroxyapatite (HAp) and collagen have been shown to have an accelerated bone healing effect and better osseointegration due to the use of a mixture of both materials. In HAp/collagen compounds, the latter has the function of regulating the distribution of the particles of the ceramic part, avoiding their agglomeration.21,22 Thus, the objective of the present in vivo study was to evaluate and compare two commercially available collagen-based biomaterials for bone regeneration, which have the same indication for clinical use. Both materials tested have bovine HAp particles in their composition, but from different portions of the bone (cancelous and cortical), different morphologies (porous and dense) and submitted to different treatments (sintered at low and high temperature). In addition, they have different amounts of collagen (10% and 25%). The evaluations were carried out at two different times (30 and 45 days) after implantation in defects created in the calvarium of adult rabbits.
Materials and methods
The present study was conducted in accordance with ARRIVE guidelines (https://arriveguidelines.org). Twenty adult rabbits of both sexes from the vivarium of the University of Rio Verde (Rio Verde, Brazil) were used. The project was approved by the animal ethics committee of the University of Rio Verde under protocol number 08/2020. The animals received all care in accordance with current national and international legislation for this type of study.23,24
Materials and group formation
Two biomaterials for bone grafting in blocks with particles aggregated by collagen in different formulations were tested and compared, forming two experimental groups: Extra Graft group (

Photographic images of both collagen-based biomaterials for bone grafting tested in the present study.
A sample from each group was used to obtain images by scanning electron microscopy (SEM) in the microscopy laboratory of the Pontifical Catholic University of Rio Grande do Sul (Porto Alegre, Brazil). The images were obtained using an SEM-FEG JSM-7100F (JEOL Ltd., Tokyo, Japan) and used to describe the morphological characteristics of each material.
Surgical procedures and sample distribution
The animals received anesthetic procedures and pre- and postoperative medication following protocols used in previous studies by our research group.1,2 First, an incision was made to the bone level and a total flap was opened, exposing the dorsal calvarium bone. In each animal, two bone defects were created (right and left sides of the midline) in the posterior (dorsal) portion of the skull, in which the total bone thickness was removed using a 6.5 mm external diameter trephine (Hager & Meisinger GmbH, Neuss, Germany), under intense irrigation with saline solution at room temperature (23 ± 2ºC). After preparing the bone defects, both materials were deposited, completely filling the defects. By prior drawing, the samples from the EG group were always placed on the left side of the animals, and the samples from the BC group were always placed on the right side of each animal. The materials were handled as recommended by each manufacturer. A porcine collagen membrane (30 × 15 mm) was positioned to cover both materials.
Finally, an internal and external plane suture was performed with simple stitches using 5-0 nylon suture. The animals were sacrificed 30 and 45 days after the graft surgery was performed (
Radiographic images and sample preparation
The samples remained in the fixative solution for a period of 10 days after their removal. Firstly, radiographs of the samples were taken using an IriX-ray DX 3000 digital radiography system (Dexcowin, Seoul, Korea), and the images were passed directly to Trophy imaging software (Toulouse, France), where the radiopacity of the materials was observed and described qualitatively. Afterward, the samples were dehydrated using a progressive sequence of ethanol (50%–100%), remaining for 48 h in each solution. Then, the collected pieces were embedded in a plastic embedding system based on Methyl methacrylate (MMA) Technovit 9100 (Kultzer & Co, Wehrhein, Germany), cured, and subjected to cutting using an Isomet 1000 machine (Buehler, Illinois, USA). Afterward, they were submitted to sanding and polishing with abrasive disks, and the histological slides were mounted. Finally, the sections were rehydrated (100%–50% ethanol) and stained using the hematoxylin and eosin technique for analysis.
Histological analysis and histomorphometry
Images of the slides were taken at different sizes using a Nikon E200 light microscope (Tokyo, Japan). Initially, all histological sections of each sample were qualitatively evaluated, describing the characteristics of the healing reaction at each proposed time. Then, a histomorphometric analysis was performed to evaluate the following aspects of the materials and healing events: (1) fibrous tissue (FB); (2) newly formed bone matrix (BM); (3) medullary spaces (MS); and (4) remaining material particles (RP). All these parameters were measured in three predetermined areas of 1 mm2 in each defect, as shown in Figure 2. The values were calculated as the percentage occupancy in relation to the total area.
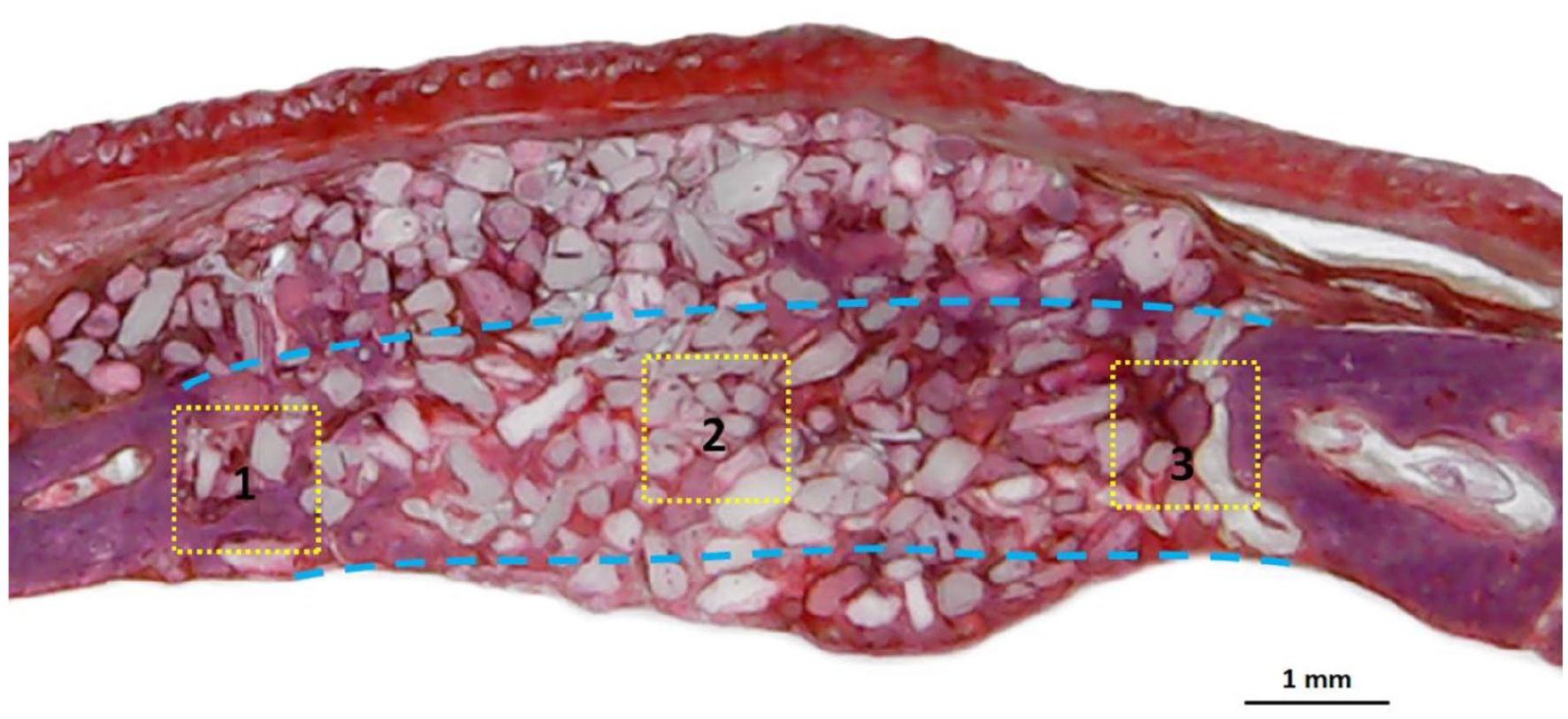
Histological section showing the three local points (with an area of 1 mm2) selected in each sample to measure the predetermined parameters. Yellow Squares 1 and 3 correspond to the areas closest to the native bone (lesion edges), and Yellow Square 2 corresponds to the central area of the defect.
To facilitate statistical comparison, and because they present similar conditions for healing, from the values measured at Positions 1 and 3, an average was calculated for each group at each proposed evaluation time.
In addition, the visible area in each histological section was measured, as shown in Figure 3. All measurements were performed using Image
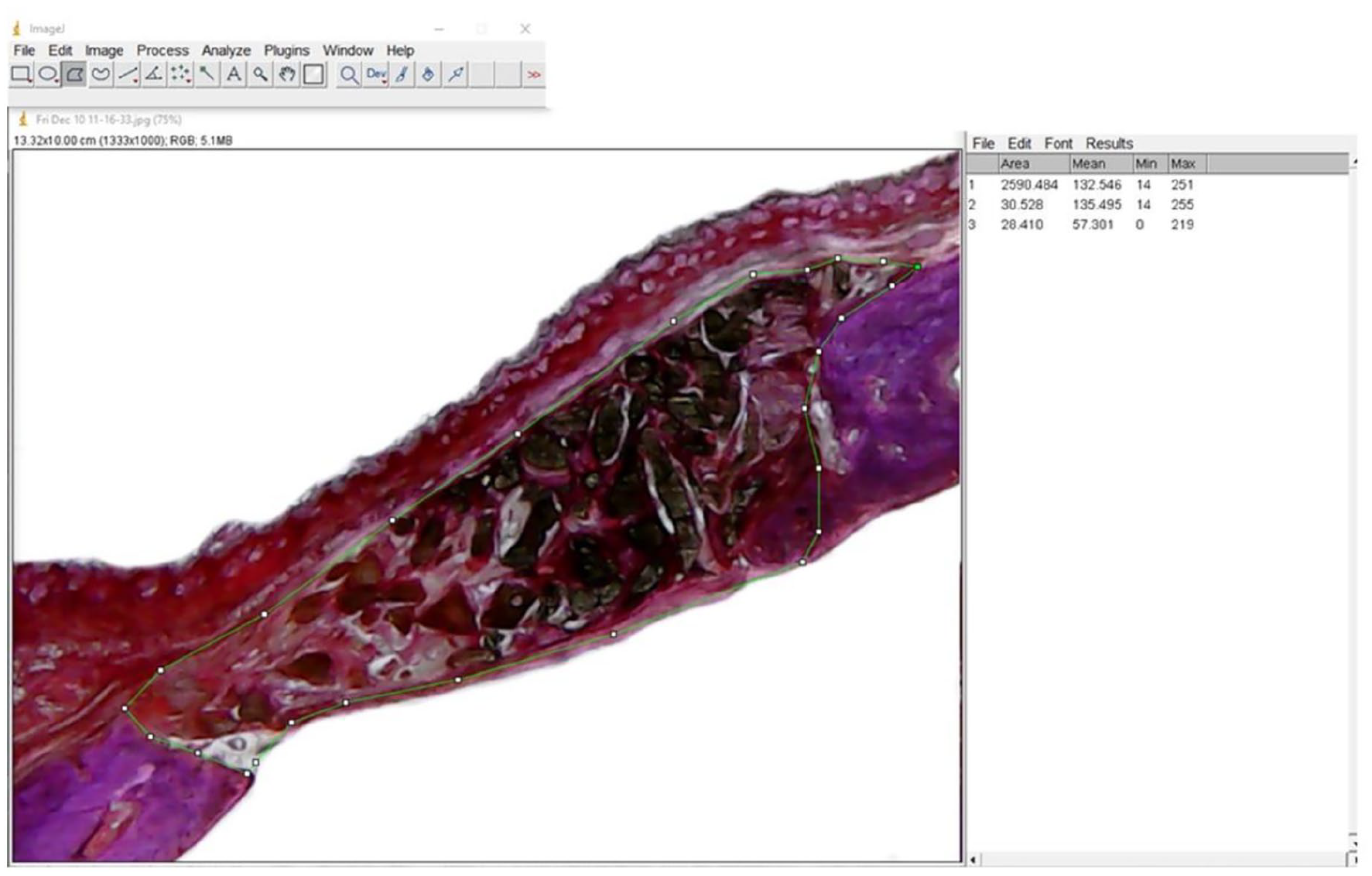
Image showing measurement of the area with the presence of bone material in each sample using the software Image
Mechanical properties
To standardize this test, the standard ASTM F1538-03(2017)
25
were used. Testing was conducted on the blocks (

Illustrative image of the mechanical test applied (
Dissolution analysis and pH alteration
These analyzes were carried out in accordance with the standard ISO 13175-3:2012.
26
Nine samples of each group BC and EG were individually large in buffer solution containing Tris hydrochloride solution in pH 7.4 (Merck KGaA, Darmstadt, Germany), being the ratio between the mass of test material and the average volume of dissolution in 4.0 mg/mL−1. The vials with the samples and dissolution medium were kept on a shaker table at 200 rpm for 24, 48, and 72 h (
Statistical analysis
The animal number was determined for a power level of 85% to obtain a
Results
The images obtained by SEM showed that the BC group particles were much more involved by collagen compared to the EG group particles, as shown in Figure 5. Furthermore, in the images of the sample from the EG group, we can observe more open spaces between the HAp particles as compared to the BC group images, where we observe fewer open spaces in the material structure.

Representative image of both materials evaluated. The first column shows Bio-Oss® Collagen (BC group), and the second column shows Extra Graft XG-13® (EG group).
Regarding the surgical procedures performed, all occurred without major complications and/or unexpected events. In two sites, the trephine surpassed the internal cortical bone, but these animals did not show any difference in postoperative reaction from the other animals. In general, the animals’ postoperative period was normal for this type of procedure (within expectations), without significant inflammatory and/or infectious complications. In two animals, the external suture was opened (suture dehiscence), exposing a small part of the membrane, but both were monitored and administered antibacterial Organnact Prata spray (Curitiba, Brazil) daily, and the wounds healed by second intention approximately 10 days after the surgery.
Radiographically, significant differences were observed in the images of both groups, with the EG group showing a much greater radiopacity at the two proposed evaluation times compared to the BC group (Figure 6). Furthermore, samples from the BC group showed faster resorption in the period between 30 and 45 days, because in the second evaluation period (45 days), few areas of material particles were visible on the radiographs. However, in the samples from the EG group, at both times, we observed greater radiopacity of the material, indicating slower resorption compared to the BC group.
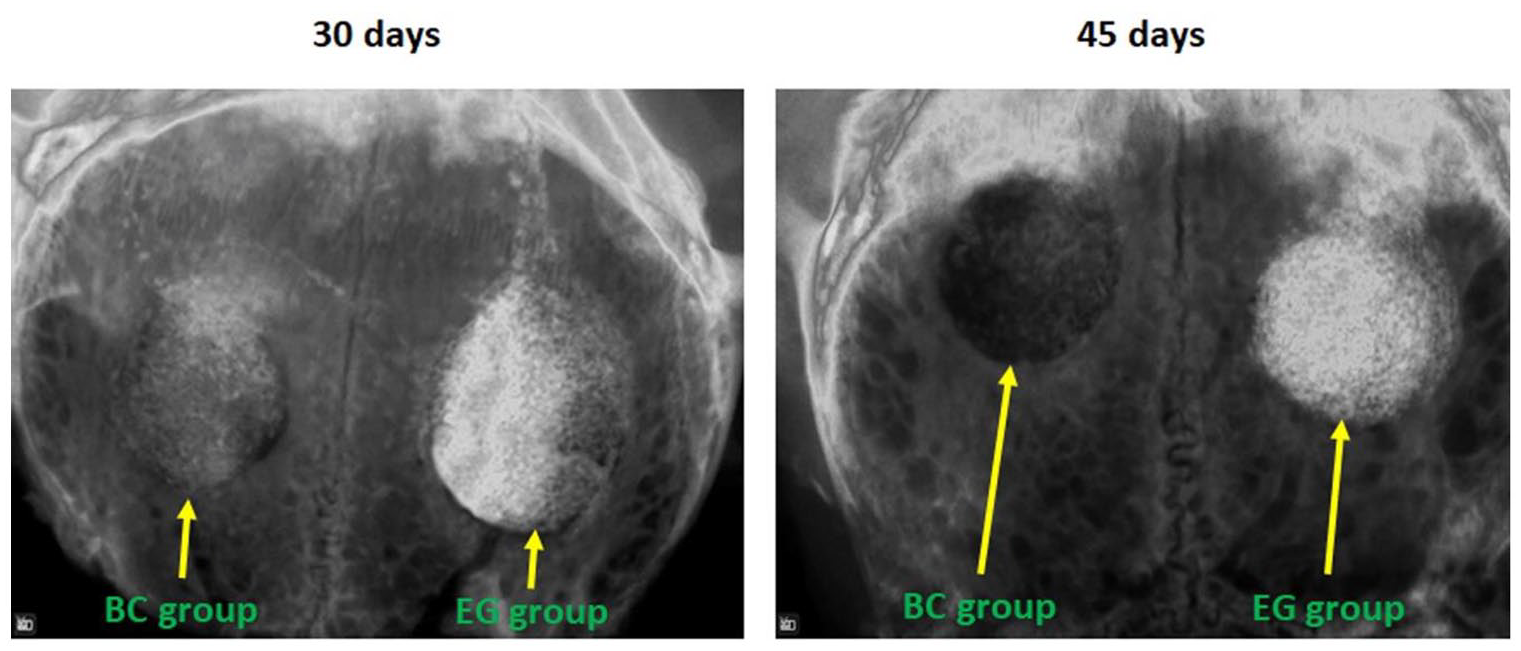
Radiographic images of the defects filled with both materials. In the first image (at 30 days), the radiopacity for the EG group is more evident than that for the BC group. In the second image (at 45 days), we can observe minimal radiopacity in the BC group defect and large radiopacity in the EG group defect.
In the histological evaluations, the BC group, at both evaluation times (30 and 45 days), showed little bone growth and intense formation of fibrous tissue, suggesting that it has lower osseoconductive potential. However, the EG group showed different reactions at the two evaluation times. In samples with 30 days of healing, little bone matrix formation was observed, and a large fibrous formation was observed between the HAp particles. Within 45 days after the graft, the samples from the EG group showed a large amount of neoformed bone between the material particles (HAp), with a low rate of resorption of the volume of the grafted material. Figure 7 shows a representative image of the reaction observed in each period of both groups and, in each predetermined observation points previously shown in the Figure 2.
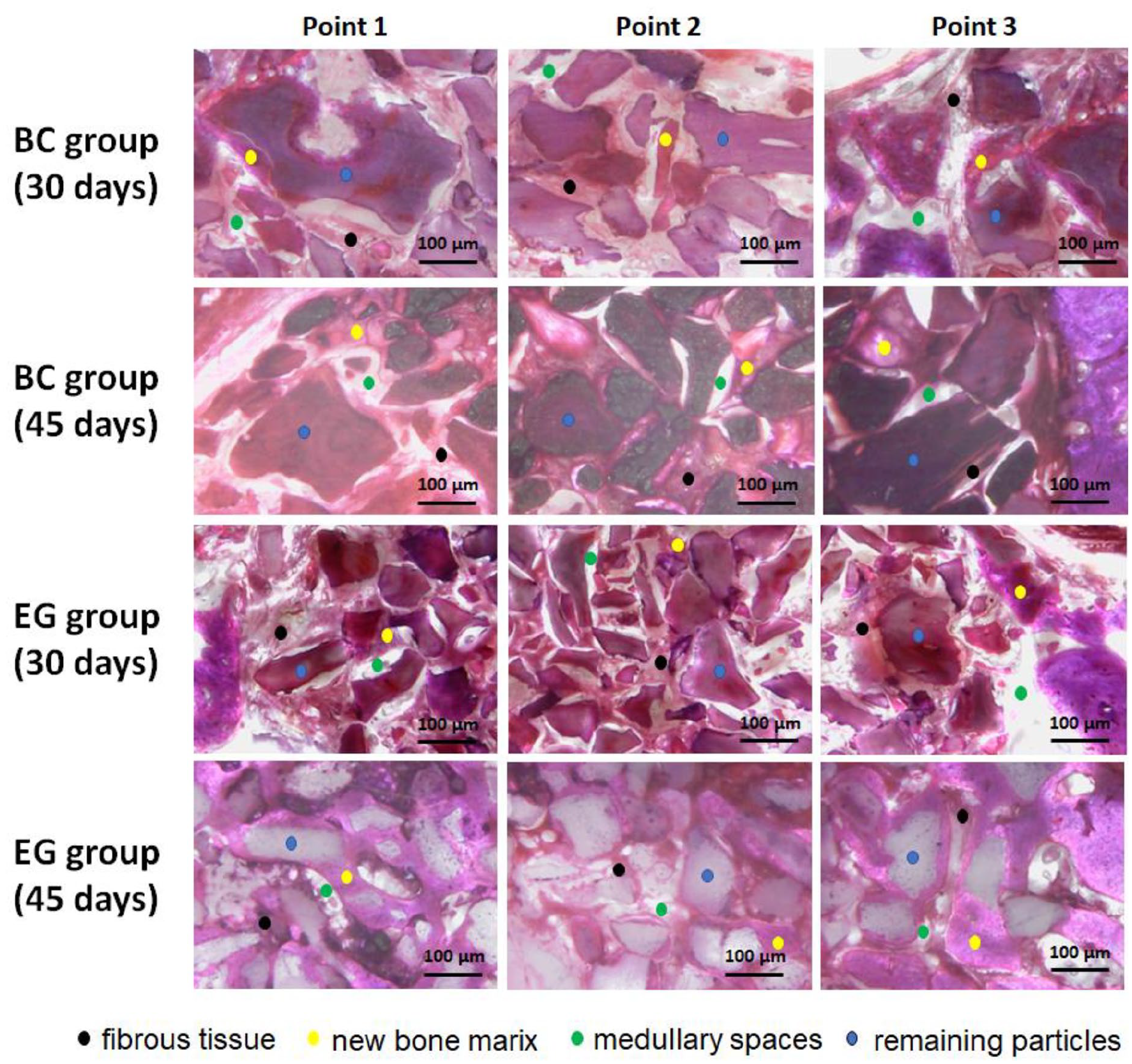
Representative images of a histological section of both groups at 30 and 45 days after the graft in the three predetermined points analyzed. In all samples of both groups was observed a less bone formation in the point 2. Stained using the hematoxylin and eosin technique.
In the histomorphometric analysis of the samples from each group, distinct reactions were observed, and the measured parameters are presented in graph form in Figure 8 (BC group) and Figure 9 (EG group). A statistical comparison within each group between the values obtained at the positions close to the native bone and in the center of the graft area for each parameter analyzed at each proposed time is presented in the table attached to each graph in Figures 7 and 8. However, when parameters were compared between groups, all comparisons, in both areas evaluated (the central area and in the edge areas) and both times, showed statistical differences between groups (
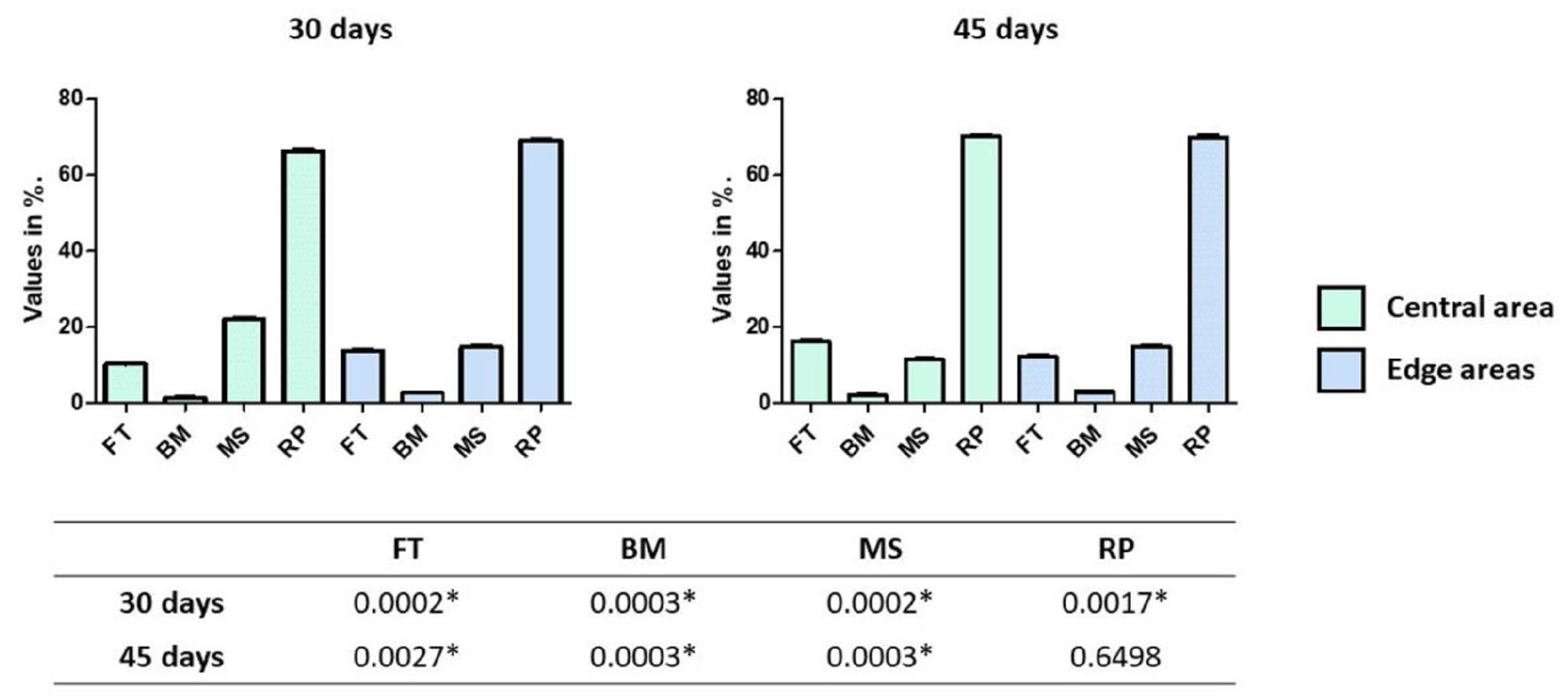
Bar graph showing the values obtained at each evaluation time measured in the central area and in the edge areas to the native bone, with a statistical comparison (
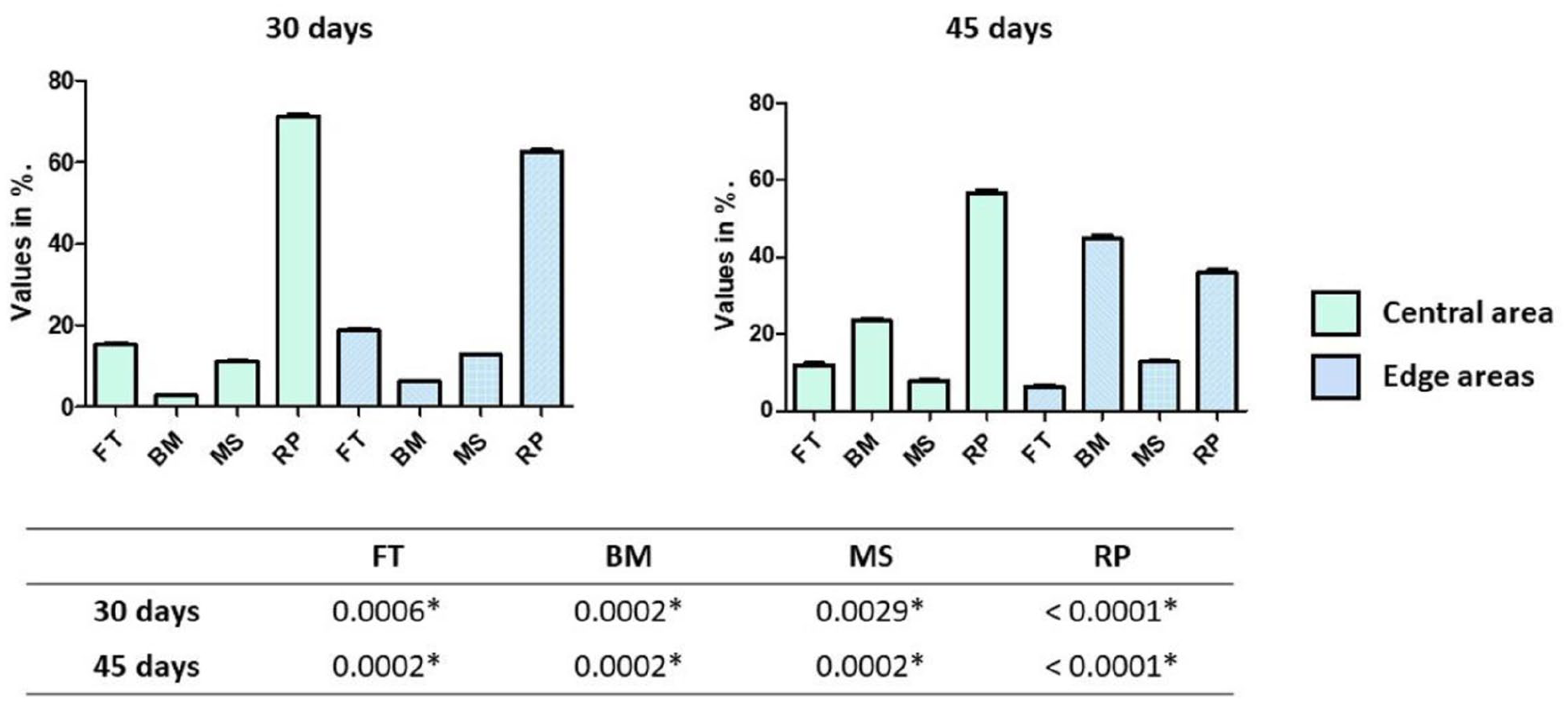
Bar graph showing the values obtained at each evaluation time measured in the central area and in the areas close to the native bone, with a statistical comparison (
The areas measured for both materials at the two proposed evaluation times are presented comparatively in Figure 10. The greater volume of graft area measured at both times in the samples from the EG group corroborates the results obtained through the radiographic images, as compared with the results obtained for the BC group.
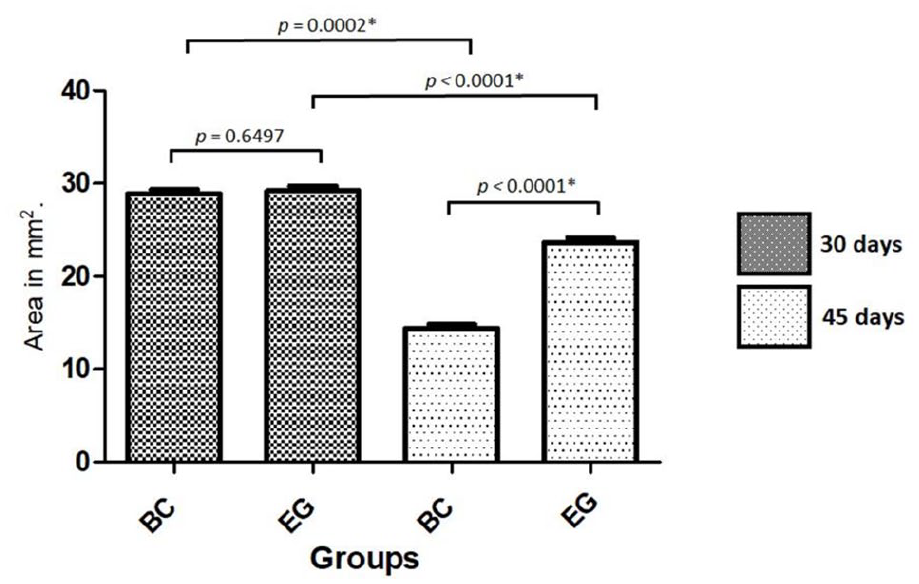
Bar graph showing the values obtained at each evaluation time when measuring the volume of the graft area, with a statistical comparison. *Statistically significant difference.
Regarding the mechanical strength test of both materials, the Young’s modulus calculated for both groups was 19.66 ± 1.06 (Mpa) for BC group and, 20.30 ± 1.18 (Mpa) for EG group. No significant difference was observed between the groups (
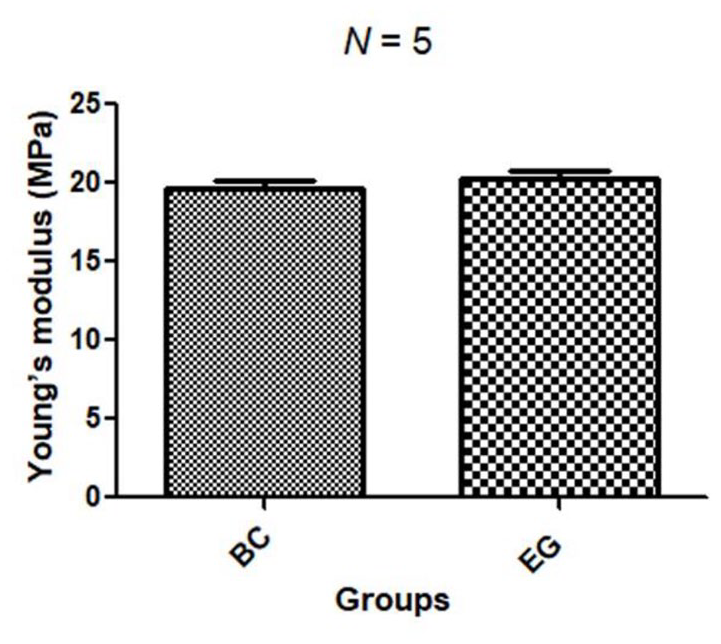
Bar graph comparing the Young’s moduli of BC and EG groups.
Finally, in the degradation analysis, the samples from the EG group showed an average mass loss of 18.5% at 24 h, 20.3% at 48 h and 23.1% after 72 h. In the BC group, the mean mass loss was 2.4% at 24 h, 2.7% at 48 h, and 4.3% after 72 h. The mean pH values at each predetermined time (24, 48, and 72 h, respectively) were 7.35, 7.30, and 7.28 for the BC group and 7.42, 7.45, and 7.50 for the EG group. Figure 12 shows the graphs of the degradation of the analyzed samples and changes in pH value.
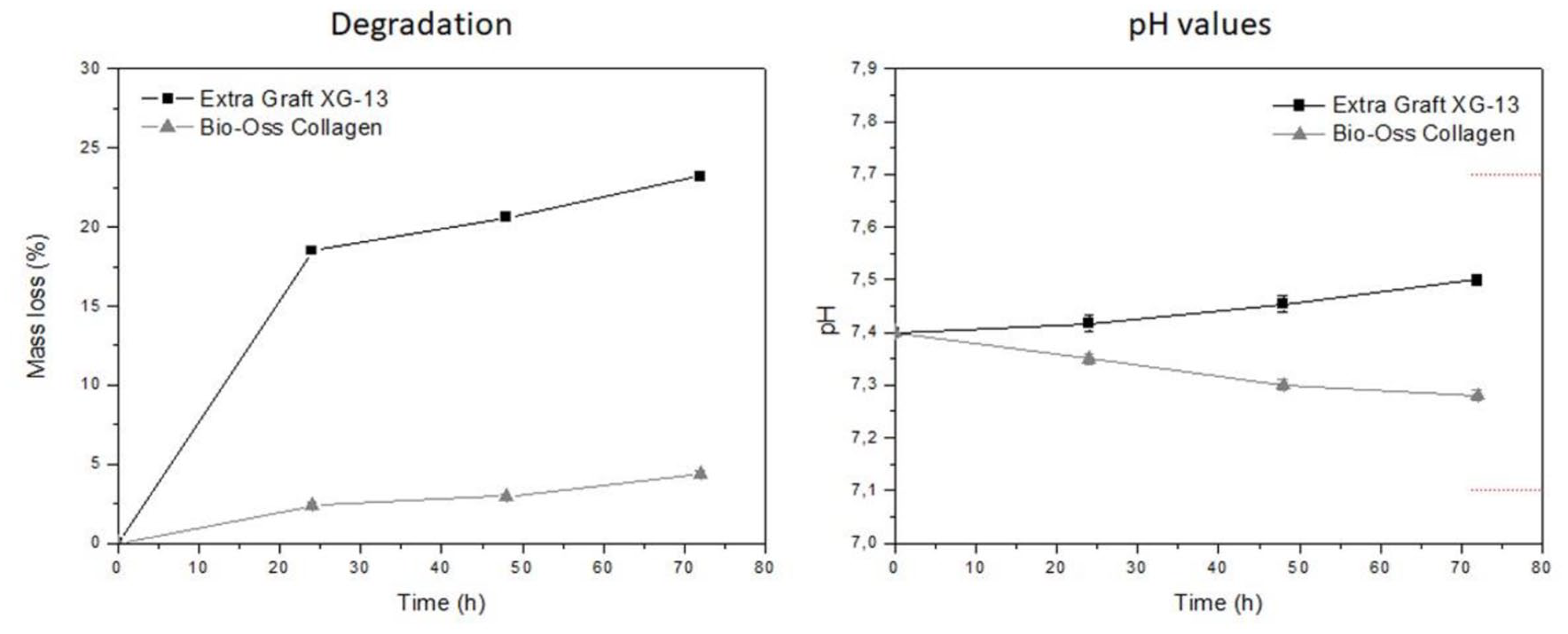
Graphs shows the degradation and pH values of both groups at 24, 48, and 72 h.
Discussion
Structured materials for bone regeneration in different forms have been constantly sought by researchers and industry in recent decades. 27 Such biomaterials can facilitate surgical manipulation and aid in the healing process by supporting cells and improving tissue growth and regeneration.28,29 In this context, in the present in vivo animal study, we analyzed and compared two different commercialized collagen-based biomaterials used for bone grafting and their effects on the early healing process at 30 and 45 days after their insertion into defects created in the calvarium of adult rabbits. The results showed that the composition presented by the material used in the EG group (25% collagen + 75% hydroxyapatite particles) promoted greater bone neoformation compared to the BC material (10% collagen + 90% particulate bovine bone) at the 45-day evaluation. Bone defects filled with biomaterials, which are used as a scaffold to stimulate and direct the growth and neoformation of this tissue, are dependent on several factors, including the physical–chemical composition of the material used; this is one of the main subjects of current research in this area.29–32
Regarding the animal model used and the selected zone, rabbits were one of the first animals used in biomedical studies and are considered laboratory animals of easy access and handling, as well as good economic viability.33,34 In addition, New Zealand rabbits are preferred for their uniformity of reactions in experimental tests. 35 The calvaria was the surgical region chosen because it is an area of easy surgical access, it offers low morbidity, and the interference of muscle forces is reduced in this location, in addition to being widely used for the study of the behavior of biomaterials. 5 Several previous studies related to bone healing have already shown good results from the use of rabbit calvaria to observe the events involved in this process. 36 Regarding the size of the defects created in the calvaria, which was 6.5 mm in the present study, this can be considered critical, considering the short periods of time selected for the evaluation of healing. 37 However, evaluation at 6–8 weeks is the clinical follow-up generally recommended in veterinary orthopedic surgery. 38 Some authors even reported that 8 weeks could be an adequate time to evaluate late repair, with bone neoformation and resorption of the grafted material. 39 In the present study, we used two similar times, at 30 and 45 days, to verify the evolution of the tissue reaction, but other future studies with longer time periods should be proposed for these materials.
We opted to use Bio-Oss® Collagen as a comparison material due to the fact that this biomaterial is already used on a large scale in dentistry and in an extensive number of publications in the world literature. The material used in the EG group (Extra Graft XG-13®) is a commercialized material but with few published studies.40,41 In addition, few studies were found assessing the influence of the amount of collagen in scaffolds developed for bone regeneration. 42 Our results showed that the samples from the EG group, which presented a higher quantity of collagen in the material’s composition (25% collagen), performed better than those from the BC group, for which the material presented 10% collagen in its composition. Among the parameters evaluated histologically—the presence of fibrous tissue, bone matrix formation, medullary spaces, and residual particles—the values obtained in measurements of the amount of bone matrix formed inside the grafted areas in samples of the EG group after 45 days were the determining factor for us to conclude that the amount of collagen can directly influence the performance of collagen-based biomaterials used for bone grafting. Furthermore, the presence of collagen in the scaffolds helps in cell adhesion, proliferation, and differentiation, as well as improving the mechanical/physical factors of these biomaterials. 43
Although type I collagen has several biological advantages, it is a material that is very easily degraded, mainly because it is the target of several collagenase enzymes that are expressed by a variety of cells. Therefore, the association with other materials is important in the elaboration of collagen-based scaffolds to reduce the natural biodegradation process and increase mechanical strength and stability.43,44 In this context, different materials have been proposed, researched, and tested.11,12,17,20–22,31,40–42 In the present study, two commercially available collagen-based materials were tested, both with HA particles of bovine origin but of different sizes and obtained by different processes. Hydroxyapatite of bovine origin is more commonly used because it is easy to obtain and has been frequently reported in the literature, in addition to having physico-chemical properties similar to those of human bone tissue. 45 Engler et al. 28 showed that the osteogenic influence of substrate stiffness is of fundamental importance within these materials (scaffolds), and the use of biocompatible and osteoinductive HA has significant advantages in bone tissue engineering applications. Moreover, Gleeson et al. 42 found in an experimental study that a combination of osteoinductive HA particles and collagen promoted an increase in scaffold stiffness, resulting in an increase in mineral deposition within the scaffolds and excellent bone regeneration. In the comparison made in our study, at the time of 30 days, no major differences were observed in the results obtained for both groups in all parameters observed. However, at 45 days, in the samples from the BC group, there was great resorption of the implanted material and little formation of bone matrix between the particles (average 2.6%) compared to that in the samples from the EG group (average 34.3%). Regarding the size of the area measured at the time of 45 days, the difference was 65% (EG group > BC group). This event can be explained by the reason that the material that has less collagen (BC group) has particles that are more rapidly reabsorbed, while the material that has more collagen (EG group) has particles that are little reabsorbed, so this difference occurred in the amount of resorption (volume) between the groups.
Regarding the type of collagen used as a base, porcine in the BC group and bovine in the EG group, studies have shown that both have similar physical and mechanical properties.46,47 However, when we analyzed the particles used in each material, the medullary bovine bone of the BC group and the sintered cortical bovine bone of the EG group, both HAp of animal origin, it was possible to observe a different behavior between them. Studies have shown that bovine medullary bone can be more easily absorbed due to its physicochemical characteristics, 48 especially when compared to HAp of bovine cortical origin, which has a very low absorption potential, especially when it is sintered, because this process modifies its structure.49,50 However, HAp may have a better impact on bone formation by maintaining its structure for a longer time. 51 Figure 13 shows a SEM image of the particles used in both materials.

SEM images of the structure of the particles without the presence of collagen used in both materials. We can see that the Bio-Oss particles have a porous structure, while the Extra Graft particles are smaller and compact (denser).
Regarding the mechanical proprieties (Young’s modulus calculated) by the two materials tested (BC group and EG group), both showed a low strength in the compression test. Recent studies have shown that rigid bovine bone blocks, with high compressive strength, can enable their fixation using screws, but they have physical characteristics that affect and/or hinder bone neoformation.5,8 On the other hand, when these materials were submitted to the degradation test, the EG group showed a much higher rate of degradation in vitro than the BC group samples, which may be related to the dissolution of the type I collagen composition and moisture loss during the drying process to measure the mass loss, since the material from the EG group is not lyophilized. Esse resultado da degradação in vitro foi completamente diferente dos resultados obtidos in vivo, corroborando os achados de outros autores que demonstraram haver uma pobre correlação entre esses ensaios. 52 However, the pH in both groups presented a low variation, staying within the parameters required by the standard used to perform the test, which determines that the pH could not vary more than 0.3 in relation to the initial value during the test. 26
Among the limitations of this in vivo study, the place where the defects were created for the implantation of the studied biomaterials (calvarium) is different from most places where they will be clinically applied to patients, so the results should be interpreted with some caution. In addition, the times for regeneration in animals are different from those in humans, and this relationship is not well defined in the literature. The sample size used, despite being within the ideal calculated sample size for this study, was limited by ethics considerations, and this must be taken into account. Further studies on the relationship between the ideal amount of collagen and particles in these types of scaffolds should be carried out to evidence the role of each component in the formation and regeneration of bone tissue, as well as the methods of incorporation of these materials.21,53
Conclusions
Through the results obtained in the present study, we conclude that the amount of collagen and the particle characteristics present in the composition of the scaffolds can directly influence the amount of neoformation and/or bone regeneration. The samples from the EG group showed a lower volume of resorption in the total area of material implanted to fill the defects when compared to the samples from the BC group during the 45-day evaluation, fact that can be explained by the type of particles used in each material. Further studies using this type of biomaterials with different collagen concentrations should be carried out to verify the ideal proportion and the ideal particle characteristics.
Supplemental Material
sj-pdf-1-jbf-10.1177_22808000221119650 – Supplemental material for Comparative evaluation of two collagen-based biomaterials with different compositions used for bone graft: An experimental animal study
Supplemental material, sj-pdf-1-jbf-10.1177_22808000221119650 for Comparative evaluation of two collagen-based biomaterials with different compositions used for bone graft: An experimental animal study by Sergio Alexandre Gehrke, Jaime Aramburú Júnior, Tiago Luis Eliers Treichel, Fernando Rodriguez, Piedad N de Aza and Berenice Anina Dedavid in Journal of Applied Biomaterials & Functional Materials
Supplemental Material
sj-xlsx-2-jbf-10.1177_22808000221119650 – Supplemental material for Comparative evaluation of two collagen-based biomaterials with different compositions used for bone graft: An experimental animal study
Supplemental material, sj-xlsx-2-jbf-10.1177_22808000221119650 for Comparative evaluation of two collagen-based biomaterials with different compositions used for bone graft: An experimental animal study by Sergio Alexandre Gehrke, Jaime Aramburú Júnior, Tiago Luis Eliers Treichel, Fernando Rodriguez, Piedad N de Aza and Berenice Anina Dedavid in Journal of Applied Biomaterials & Functional Materials
Footnotes
Acknowledgements
The author Sergio Alexandre Gehrke was funded by post-doctoral grant nº 2021/PER/00020 from the Ministerio de Universidades under the program “Ayudas para la recualificación del sistema universitario español de la Universidad Miguel Hernandez” modalidad “Margarita Salas para la formación de jóvenes doctores.” The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author contribution statement
Sergio Alexandre Gehrke: Conceptualization, Methodology, Investigation, Data curation, Software, Writing—original draft, Writing—review and editing. Jaime Aramburú Júnior: Investigation, Data curation. Tiago Luis Eliers Treichel: Investigation, Data curation. Fernando Rodriguez: Investigation. Piedad N. de Aza: Methodology, Data analyzes, Validation. Berenice Anina Dedavid: Conceptualization, Methodology, Supervision, Writing—review and editing.
Availability of data and materials statements
All data generated or analyzed during this study are included in this published article and its Supplemental Information files.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by MCIN/AEI/ 10.13039/501100011033, Grant PID2020-116693RB-C21.
Ethical approval
The present study was approved by the Animal Experimentation Committee (UniRV nº08/2020), University of Rio Verde (Rio Verde, Brazil). All applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
Informed consent
For this type of study, formal consent is not required.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
