Abstract
Background:
Orthodontic treatment with fixed appliances involves sliding of brackets along archwires. These movements involve friction, which causes resistance to sliding. In addition, moments cause teeth to tip until binding occurs between the bracket and archwire. The manufacturer of a new TiMolium®Titanium archwire claims material properties superior to β-Titanium, potentially leading to reduced resistance to sliding.
Objective:
To compare TiMolium archwires with β-Titanium and stainless steel archwires as the current gold standard for sliding mechanics under application of an increasing moment.
Materials and methods:
A total of 120 stainless steel (Smartclip, 3M, Monrovia, CA) and ceramic self-ligating 0.022″-slot brackets (Clarity SL, 3M) were divided into six equal-sized groups. Resistance to sliding was tested with 0.019″ × 0.025″ TiMolium (TP Orthodontics, La Porte, IN), β-Titanium (3M), and stainless steel (3M) archwires using a custom-designed apparatus to simulate sliding mechanics and application of moments of 1000, 2000, and 3000 g-mm.
Results:
Using stainless steel brackets, the TiMolium archwires had significantly higher resistance to sliding than stainless steel archwires at all moments tested while there was no difference between TiMolium and β-Titanium. Using ceramic brackets, the resistance to sliding with TiMolium archwires was no different than with stainless steel archwires. Both TiMolium and stainless steel archwires showed significantly lower resistance to sliding than β-Titanium.
Conclusion:
TiMolium archwires have resistance to sliding intermediary to stainless steel and β-Titanium archwires when clinically relevant moments are applied. Used with the stainless steel brackets, they behave like β-Titanium, whereas used with the ceramic brackets, they behave more like stainless steel.
Introduction
In orthodontic treatment with fixed appliances, brackets and archwires are used to move misaligned teeth into corrected positions. Over the past few decades, orthodontic therapy has evolved in response to rising demands to provide more efficacious treatment modalities. For instance, the introduction of novel bracket systems has provided an array of selections in orthodontic appliances, including conventional and self-ligating bracket systems. Conventional brackets are suggested to have increased frictional resistance to sliding caused by the ligatures used to hold the archwire in place, resulting in reduced treatment efficacy.1–3 Conversely, self-ligating brackets are suggested to have reduced frictional resistance to sliding as they do not require additional ligatures. 4
Fixed orthodontic appliances have traditionally used stainless steel brackets together with a variety of archwire materials. An aesthetic alternative to stainless steel brackets are ceramic brackets; however, ceramic brackets have unfavorable resistance to sliding due to their high friction coefficient. Several investigations comparing the resistance to sliding of ceramic brackets with stainless steel brackets have shown that ceramic brackets are associated with greater resistance to sliding.3–5
Appropriate choice of archwires aids in providing the most efficient tooth movement to optimize treatment time. Sliding of brackets along archwires, especially in extraction cases, may necessitate extended treatment time as frictional resistance to sliding may hinder orthodontic tooth movement. Frictional resistance to sliding at the bracket-archwire interface is determined by a combination of mechanical and chemical factors, including the mode of ligation, and accounts for about 12% to 74% of applied force lost.1–3,6–9
In general, resistance to sliding is characterized by three phenomena: classic friction, binding, and notching.3–5 Factors that influence static friction include archwire material and dimensions, bracket material, surface roughness, mode of ligation, moisture, and bracket displacement. Binding and notching are dependent on archwire dimension and surface properties. A combination of static friction, binding, and notching influences tooth movement. Tooth movement is initiated when the applied force exceeds the static friction. Binding occurs as the applied force increases and the wire starts to bind against the bracket corners.2,4 Notching is indicative of plastic deformation of the wire, causing cessation in tooth movement.2,4 Resistance to sliding, characterized by the three phenomena, exhibits variability dependent on archwire material.
Traditionally, archwires made from β-Titanium or stainless steel alloys have been used for orthodontic sliding mechanics. 4 A novel archwire material, TiMolium®Titanium, may have material properties superior to β-Titanium paired with smoother surface finish, potentially leading to reduced resistance to sliding and shorter treatment times. However, evidence is scarce to support the manufacturer’s claims of improved efficacy.
The aim of this in vitro study was to quantify frictional resistance to sliding of the novel TiMolium archwire in comparison to the β-Titanium and stainless steel archwires of similar dimension during archwire-guided retraction with self-ligating brackets. The null hypothesis was that the TiMolium archwire would show no difference in frictional resistance to sliding compared to β-Titanium archwires of similar dimension.
Materials and methods
Three different archwires types with identical size but different alloy compositions were tested in combination with two different types of maxillary canine brackets. The archwire types included 40 stainless steel (3M Unitek, Monrovia, CA, USA), 40 β-Titanium (3M), and 40 TiMolium®Titanium (TP Orthodontics, La Porte, IN, USA) archwires with 0.019″ × 0.025″ cross-sectional areas. The alloy compositions of these archwires are shown in Table 1.
Alloy compositions of the archwires used.

The bracket types included 60 stainless steel (SmartClip, 3M) and 60 ceramic (ClaritySL, 3M) passive self-ligating bracket with 0.022″ slot size. Maxillary canine brackets were chosen to simulate canine retraction because the maxillary canine undergoes the most frequent translational movement during orthodontic treatment with premolar extractions. A total of 120 bracket-archwire samples were prepared and subdivided into six equal-sized groups, each consisting of 20 test samples (Table 2) thereby doubling the sample size of previous studies.1,2,12 The archwires were held in the bracket slots using the brackets’ SmartClip self-ligating mechanism. A new bracket-archwire sample was used for each test run as detailed below.
Test groups.

Sample preparation
A custom-made mounting jig, along with 0.021″ × 0.025″ stainless steel guiding wires, was used to standardize the bonding process (Figure 1). Brackets were bonded to the center of a Dura-Green stone bur (Shofu Dental Corporation, San Marcos, CA, USA) using the guiding wire in order to diminish root torque programed in the bracket prescription by creating an uneven layer of adhesive under the bracket base. 2 A light-cured adhesive for orthodontic bracket bonding (Transbond XT, 3M) was applied to the bracket base and the bracket was then placed on the stone bur. Upon centering the bracket on the bur, the adhesive was light cured with an Elipar DeepCure curing light (3M) with a 3-s curing cycle.

Custom-made mounting jig.
Sample testing
The mechanical properties of the archwires were evaluated in a custom mechanical test apparatus (Figure 2) bound by a universal testing machine (Instron Corporation, Model 4204, Canton, MA). A bur with a bound bracket-archwire combination was mounted onto a frictionless rotary unit in the testing apparatus. The unit housed the bur throughout the duration of the experiment using a setscrew. The rotary unit had two nylon rollers mounted 10 mm above and below the axis of rotation of the bur to simulate adjacent brackets during canine retraction. The archwire was centered on the rollers and locked into a straight, on-axis position by tightening a setscrew on the rotary unit to minimize off-axes forces.

Experimental mechanical apparatus simulating canine retraction.
Two 5-kgf load cells (model LCM703-5, Omega Engineering, Stamford, CT, USA) were used to record two different forces in the experimental setup. The first load cell measured the resistance to sliding and the second load cell measured the lateral force that generated a moment on the bracket-archwire combination as it underwent rotation. After the bur had been tightened into the rotary unit, the archwire was clamped at a straight, on-axis grip that was in alignment with the bracket-archwire interface. After clamping the wire, it was vertically displaced for 10 mm at a rate of 5 mm/min. Simultaneously, the bracket could be rotated by the mechanical testing unit to simulate the application of a moment. The rate of rotation was set to 0.08325°/s.
Data acquisition
Data acquisition began for 5 s without rotation of the bracket to acquire the normal force, which is the frictional resistance without the application of a moment. After 5 s, rotation of the bracket was started. Data output from the load cells was processed using a custom-made algorithm within LabVIEW 2015 Data Acquisition and Process Control software (National Instruments, Austin, TX, USA). Data were acquired at a rate of 100 Hz and imported into Microsoft Excel™ (Microsoft, Redmond, WA, USA) for subsequent analysis.
Data analysis
The emulated tipping moment by the lateral force was calculated by addressing the distance between the line of action of the force and bracket, which corresponds to the radius of the rotary unit. The normal force was obtained by averaging recorded data points during the first 5 s of a test. To normalize data sets, the normal force was subtracted from the measured frictional resistance to sliding. Resistance to sliding was calculated for clinically relevant moments of 1000, 2000, and 3000 g-mm.
Statistical analysis
Mean values and standard deviations of the resistance to sliding were calculated for each test group to summarize the data. Differences among the archwires were tested for statistical significance, separately for each bracket type, using Kruskal–Wallis ANOVA on ranks with Tukey’s method as a post hoc pairwise comparison procedure after the data had been tested for normality (Kolmogorov–Smirnov test). Statistical analyses were performed using SigmaStat for Windows (Systat Software, San Jose, CA, USA), with p-values of less than 0.05 considered statistically significant.
Sample imaging
After the quantification of the frictional resistance to sliding, a qualitative comparison of surface smoothness of the novel TiMolium archwire to the β-Titanium and stainless steel archwires was attempted. For this, the archwires were imaged using a stereomicroscope (Olympus Life Sciences, Waltham, MA, USA) at 10× magnification at four characteristic regions: (1) a region that had not undergone mechanical testing, (2) region of initial engagement, (2) region of final engagement, and (4) the transitional region between final engagement and no engagement. The bracket slot surface was also imaged for comparative purposes.
Results
The frictional resistance to sliding using stainless steel and ceramic self-ligating brackets and the three archwires tested is shown in Figure 3. When used with stainless steel brackets, the frictional resistance to sliding of the TiMolium archwire was significantly greater than that of the stainless steel archwire while there was no significant difference when compared to the β-Titanium archwire at each applied moment. When used with ceramic brackets, the frictional resistance to sliding of the TiMolium archwire was significantly less than that of the β-Titanium archwire at each applied moment while there was no significant difference when compared to the stainless steel archwire.

Frictional resistance to sliding at 1000, 2000, and 3000 g-mm for the stainless steel bracket and the ceramic bracket with the archwire types tested.
A quantitative comparison of the frictional resistance to sliding among the archwire alloys in the stainless steel and ceramic brackets is shown in Figure 4. The greatest resistance to sliding at each applied moment was observed with the β-Titanium archwire. Conversely, the least frictional resistance was observed with the stainless steel archwire, except with the ceramic bracket at 1000 g-mm where the TiMolium archwire showed the least frictional resistance.
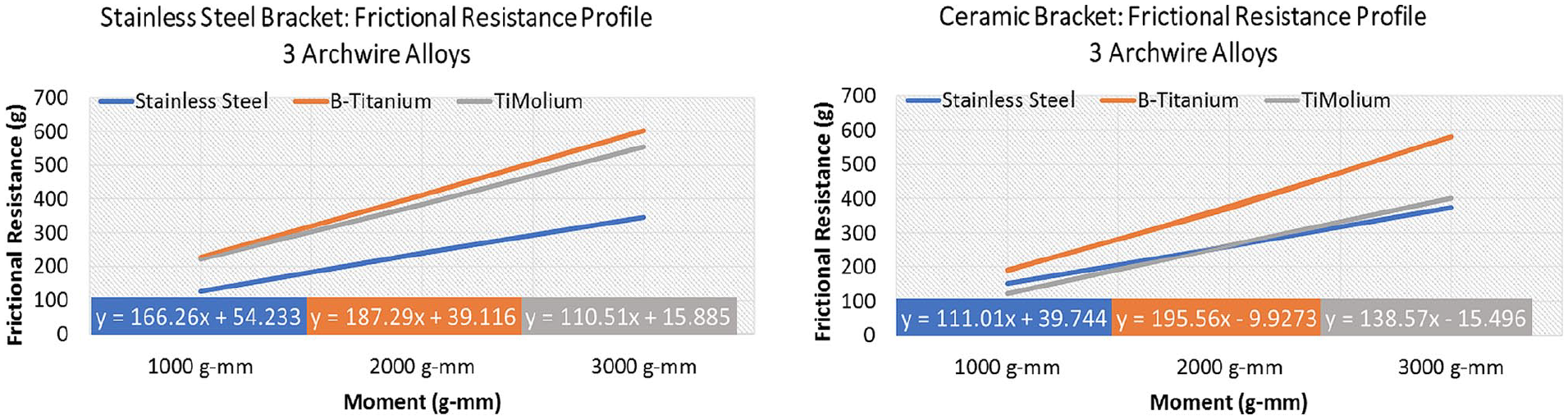
Frictional resistance to sliding profile of archwire alloys for the stainless steel bracket and the ceramic bracket.
Representative samples of the archwire surfaces at transition stages of testing with the stainless steel and ceramic brackets including a 10° rotation are shown in Figure 5. The TiMolium archwire showed the greatest abrasion area, suggesting the greatest surface interaction uniformity as it was pulled along the bracket slot. Conversely, the β-Titanium archwire had the least abrasion area on its surface.

Archwire surface abrasion at the transition sites after interaction with the two bracket types used. Upper row: (a) stainless steel, (b) β-Titanium, and (c) TiMolium archwires used with stainless steel bracket. Lower row: (d) stainless steel, (e) β-Titanium, and (f) TiMolium archwires used with ceramic bracket. 10× magnification.
Representative samples of the bracket types are shown in Figure 6. Focusing on the leading edge of the bracket’s slot, the ceramic bracket has rounder transitions between surfaces when compared to the sharper transitions in the stainless steel bracket.

Maxillary right canine bracket slots showing mechanical surface abrasion after interaction with archwire. (a) Stainless steel bracket and (b) ceramic bracket. 5× magnification.
Discussion
The resistance to sliding of three different archwire alloys was evaluated in vitro within clinically relevant parameters. The resistance to sliding in orthodontic systems in vitro depends on a multitude of factors such as the alloy type, surface texture, bracket type, as well as size and geometry of the archwire.13–15 In the present study, the resistance to sliding was directly proportionate to the applied moment exerted by the testing apparatus as the bracket was rotated throughout each test.
For maxillary canine retraction, Lee concluded that the optimum force level is between 1.5 and 2.6 N, which is roughly equivalent to150 and 260 g of force, respectively.16,17 In clinical application, this means that it requires at least 150 g of force to initiate canine retraction in addition to the force necessary to exceed resistance to sliding in the bracket-archwire system. The force may increase to 260 g of force based on patient-related factors including bone remodeling behavior, periodontal ligament width and compressibility, and salivary flow. Assuming an average distance of 10 mm between bracket and the center of resistance of an average-sized canine, the resulting moments during retraction of maxillary canines would correspond to 1500 and 2600 g-mm; therefore, values of 1000, 2000, and 3000 g-mm were considered clinically relevant in the present study.
Resistance to sliding can be directly correlated to the percentage of force lost due to friction. Force lost due to friction is not available for canine retraction, but stresses teeth that are used as anchorage units. Stresses on anchorage units can cause undesired tooth movement, as they overload the anchorage units.5,18,19 Of interest, the manufacturer claims that the TiMolium archwire outperforms β-Titanium in smoothness and polish, and that it has high stiffness similar to stainless steel, which are all constituent factors of lower resistance to sliding. 20 From this it can be inferred that TiMolium will exhibit lower resistance to sliding when compared to β-Titanium wires, resulting in less force lost due to friction and less stresses on teeth used as anchorage units.
When the findings with ceramic brackets and stainless steel brackets are taken together, this claim is supported by the present results, which suggest that the percentage of force lost due to friction was less for the TiMolium archwire compared to the β-Titanium archwire. Therefore, the null hypothesis of there being no difference between the TiMolium and β-Titanium archwires of similar dimension was rejected. The present results also suggest that the percentage of force lost during canine retraction is greatest using the β-Titanium archwire as it showed the highest resistance to sliding. Conversely, the least percentage of force is lost during canine retraction using the stainless steel archwire. It is noteworthy, however, that when used with stainless steel brackets, the TiMolium archwire behaved similarly to the β-Titanium archwire as it had had significantly higher resistance to sliding than the stainless steel archwire. In contrast, when used with ceramic brackets, the TiMolium archwire had significantly lower resistance to sliding than the β-Titanium archwire.
The archwire surface was abraded by the bracket slot wall during each test run. Different test groups demonstrated qualitative differences in their archwire surfaces, potentially related to their resistance to sliding. For instance, the β-Titanium archwire showed surface interaction on the least surface area, which would explain its high resistance to sliding. In contrast, the TiMolium archwire demonstrated the most uniform surface interaction profile with the bracket slot wall. Interestingly, the behavior of the TiMolium archwire was significantly different between the ceramic and stainless steel brackets. The coefficient of friction of each bracket slot is expected to be similar since the slots of both bracket types have inserts of the same alloy. However, interfacial properties also depend on a variety of other factors, including the dimensions and shape of the bracket slot. The ceramic bracket used has round corners to accommodate for the brittle nature of the material, and this roundness may result in less stress placed on the archwire since the surface area of engaging the wire is greater. In contrast, the stainless steel bracket slot has sharper corners, which may apply greater stress on the archwire surface and increase the level of frictional resistance to sliding as well as the probability of notching.
Limitations of this in vitro study include the lack of simulation of situations that occur in the oral cavity during orthodontic treatment. For instance, orthodontic bracket-archwire systems are subject to masticatory forces that were not simulated in the experimental setup. Similarly, salivation, water hardness, and toothbrush abrasion may impact the surface properties of orthodontic brackets and archwires throughout the duration of treatment. Therefore, the clinical efficacy of bracket-archwire systems will depend on a variety of other factors, including ease of use and clinician experience.
Conclusion
TiMolium archwires showed resistance to sliding intermediary to stainless steel and β-Titanium archwires when clinically relevant moments were applied. Used with the stainless steel brackets, they behaved like β-Titanium, whereas used with the ceramic brackets, they behaved more like stainless steel.
Footnotes
Acknowledgements
The authors are grateful to 3M Unitek and TP Orthodontics for donating the materials used in this study.
Authors’ contributions
A.Y.: Data collection, drafting of the manuscript. C.D.: Data collection. J.B.: Study design, data interpretation, and critical revision of the manuscript. T.G.: Study design, data analysis, and interpretation; drafting and critical revision of the manuscript. All authors reviewed the manuscript, gave final approval, and agree to be accountable for all aspects of the work.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
