Abstract
Despite modern advances, a broad range of disorders such as cancer and infectious diseases continually afflict the global population. Novel therapeutics are continuously being explored to address these challenges. Therefore, scalable, effective, and safe therapies that are readily accessible to third-world countries are of major interest. In this article, we discuss the potential advantages that the nanomedicine field may harness toward successful implementation against some of the major diseases of our generation.
Introduction: Opportunities for Nanotherapy to Address Global Health Challenges
Although the average life expectancy has increased globally in the past decade, the prevalence of communicable and noncommunicable diseases continues to be a challenge for global health. 1 Noncommunicable diseases alone are already responsible for two-thirds of all deaths globally, killing more than 36 million people each year. 2 The Grand Challenges in Global Health (GCGH) initiative has presented seven goals in hopes of overcoming the current disadvantages of modern medicine. 3 Under the goal of improving vaccines, the GCGH seeks to alleviate the cost of treatment, increase therapeutic efficacy, and develop alternative ways to administer treatment drugs to eliminate the chance of reusing needles.3,4 In situations in which new drug compounds are developed, their scalability, ability to modulate the release rate, and targeted release are some of the many properties that can have a direct effect on their clinical relevance.5,6 Furthermore, finding safer methods of treatment has also become relevant, considering that some treatments, such as chemotherapy, have been shown to have both long-term and short-term harmful side effects. 7 Given these challenges, novel technologies are necessary to improve patient treatment outcomes on a global scale.
The evolving use of nanotechnology in medical studies has resulted in several promising applications under the field known as nanomedicine.8–15 According to the European Science Foundation, nanomedicine is “the science and technology of diagnosing, treating, and preventing disease and traumatic injury, of relieving pain, and of preserving and improving human health, using molecular tools and molecular knowledge of the human body.” 16 More specifically, the structures used in nanomedicine are made up of components between 1 and 100 nm in size.12,15 Although the range of dimensions of the nanomaterials used have extended beyond these parameters, clear benefits to therapeutic delivery have been realized through the application of nanomedicine ( Fig. 1 ). These include improved drug circulation times, enhanced intratumoral retention, and enhanced therapeutic efficacy. 17 Such capabilities have generated interest in how nanotechnology can overcome treatment challenges in diseases such as HIV/AIDS. 18 In addition, nanomedicines carrying cancer drugs may be safer and more efficient than conventional chemotherapy because they prevent harmful interactions with normal tissues by preventing early drug release while mediating improved specificity, among other improvements.12,19 Consequently, the versatile physical, chemical, and mechanical characteristics of nanomaterials explain the reason why many of the studies related to nanomedicine are focused on its effects on the delivery of therapeutic agents.10,13 The nanomedicine field is not limited to applications in drug therapy but can also be instrumental in diagnosing and monitoring diseases.9,11 This article will briefly highlight three examples of where nanotechnology can further play a role in accelerating the translation of novel therapeutic strategies toward improving global health.
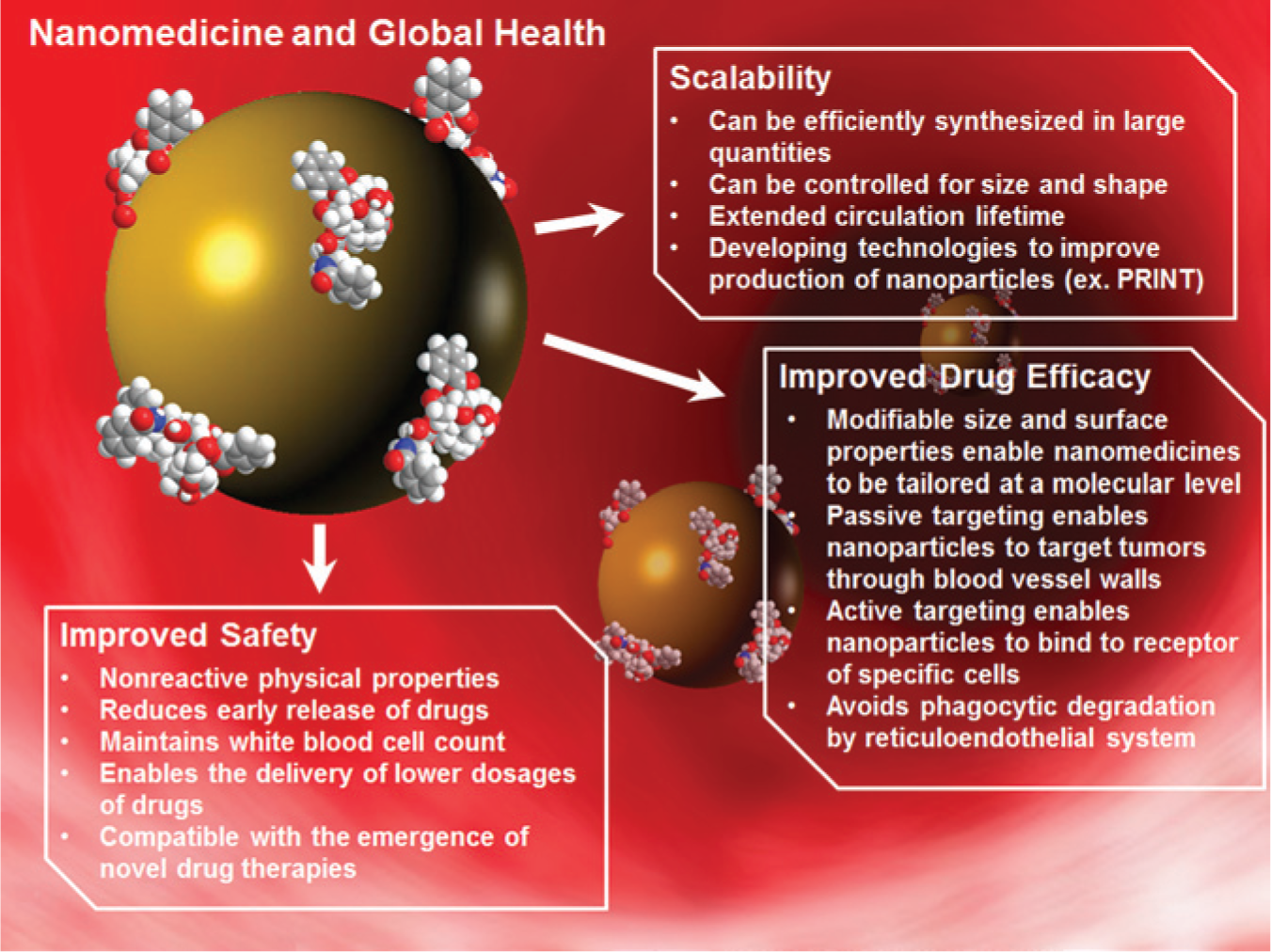
Nanomedicine and global health.
Material Scalability and Efficacy: PRINT
Novel therapeutics, including those that are nano-modified, are often developed to overcome specific challenges in disease treatment. 20 However, if there are insufficient resources or difficulties in manufacturing these therapeutics consistently for those affected, then resolving these global health challenges becomes difficult to achieve. 21 The ability to produce novel therapeutics uniformly at a large scale is not only important for research trials but also necessary for regulatory approval and clinical use. Researchers in the nano-field have recognized this and have devoted their attention toward finding new ways to improve the production of nanoparticles. 22
The Particle Replication in Non-wetting Templates (PRINT) technique is a soft lithography approach developed by Desimone et al. 23 to produce nanoparticles that are uniform in size, shape, chemistry, and composition. PRINT involves the use of a fluorinated perfluoropolyether (PFPE) mold and subsequent casting of nanoparticles with remarkable control of sizes and shapes, which can markedly improve the production of carriers for a spectrum of diseases. Significant advantages of the PRINT technique come from its use of PFPE; it is compatible with a range of different solvents, and its physical traits make the fabrication process more efficient. Another key feature of the PRINT technique is its scalability, which enables nanoparticles to be created with greater precision and control. 23 Being able to create uniform nanoparticles of varied dimensions has allowed Desimone and other scientists to conduct important studies pertaining to the effects of size, shape, and chemistry on the ability of cells to internalize nanoparticles. 24
Desimone and a team of scientists from Liquidia Technologies used the PRINT technology to study the development of a nanoparticle-based influenza vaccine. Their approach predicted that antigen presentation from a biodegradable particle would increase vaccine effectiveness by inducing a more efficient immune response. Vaccines composed of cylindrical nanoparticles containing a solution of poly(lactic-co-glycolic acid) mixed with different cationic additives were prepared using the PRINT technique and administered to mice and rabbits intramuscularly. Animal sera were then assessed for antibodies, and the animals themselves were also evaluated for toxicologic effects. Depending on the cationic additive that was used, the nanoparticles showed different levels of binding to the vaccine antigens; particles with a positive surface charge displayed more efficient binding compared with particles with a negative surface charge. Furthermore, immunogenicity studies revealed that PRINT particles with the cationic additives resulted in greater positive surface charges and yielded the most improved immune responses. Another immunogenicity study was done to compare the efficacy of nanoparticle-modified antigens to unmodified antigens. The study revealed a markedly stronger immune response for vaccine antigens delivered via bioabsorbable nanoparticles. Finally, toxicology studies indicated no apparent effects on mortality, body weight, food consumption, and other parameters. 25
Nano for HIV/AIDS
As one of the world’s leading causes of death, human immunodeficiency virus (HIV)/acquired immune deficiency syndrome (AIDS) persists as a global health challenge. As deadly as it is on its own, HIV/AIDS has also been linked to terminal blood cancers such as lymphoma. 26 Although modern antiretroviral drug therapies have improved, there are still several limitations; many HIV localization sites are inaccessible by the majority of drugs, and most drugs cannot be maintained in their active state for very long. Furthermore, the poor solubility of some antiretroviral drugs can compromise the efficacy of HIV treatment. However, nanotechnology-modified drug delivery to specific sites with controlled release rates may counteract many of these limitations. 27
Elechiguerra et al. 28 previously examined how silver noble-metal nanocrystals of different sizes interacted with the HIV type 1 (HIV-1) virus. Silver nanoparticles were chosen out of consideration for their antimicrobial properties. Prepared samples of HIV-1 cell-free virus were exposed to varying sizes of silver nanoparticles coated with carbon, poly(n-vinyl-2-pyrrolidone) (PVP), or bovine serum albumin (BSA) and later observed with an electron microscope. The spatial arrangement of the silver nanoparticles interacting with the gp120 glycoprotein knobs on the HIV-1 virus indicated that nanoparticles that were too big (greater than 20 nm) could not attach to the virus. However, silver nanoparticles that were less than 14 nm in diameter mediated the most stable surface interactions with the viruses. The silver nanoparticles were then mixed directly with the HIV-1 virus, diluted, and then added to cultures of target cells to observe their antimicrobial properties. For the carbon, PVP, BSA-coated nanoparticles, viral infectivity was markedly reduced. However, when the silver nanoparticles were coated with PVP or BSA, the inhibitory effects were not as prominent as those observed with the carbon-coated particles. 28
Nanomedicine and Cancer
Cancer is a global health concern that is independent of socioeconomic status. In 2012, cancer was responsible for 8.2 million deaths—more than HIV/AIDS, tuberculosis, and malaria combined. The American Cancer Society estimates that in 2030, cancer will be responsible for 13 million deaths worldwide. 29
Many global health organizations are continually trying to find improved ways to combat the growing threat of cancer by focusing on advances in cancer treatment. 30 The popular approach of chemotherapy is limited by its toxicity to normal cells and the acquisition of drug resistance by cancer cells, among others. 31 Furthermore, the presence of cancer stem cells can induce tumor growth, even with chemotherapy, which renders these toxic treatment courses impractical. 32 However, a growing number of studies have been focused on addressing these limitations by combining conventional cancer therapy with the advantageous features of nanotechnology.33,34 For example, nanoparticle-modified therapeutics can use the enhanced permeability and retention effect to improve drug delivery outcomes, as nanoparticle uptake is increased and retained within solid tumors due to faulty lymphatic drainage systems. 33 The size adaptability of nanostructures allows them to penetrate tumors from the blood stream without being filtered by the kidneys. 13 In addition, nanoparticles can be synthesized in a variety of forms such as lipid-based vehicles, polymer carriers, metals, carbon structures, and other inorganic particles, enabling their use in a wide spectrum of specific applications in clinical medicine.35,36 For example, Gao et al. 37 used polymeric nanobubbles to deliver doxorubicin, a small-molecule chemotherapeutic, to tumor tissues surrounding epithelial cells more effectively. Beyond drug delivery, nanoparticles themselves have also been harnessed as the cancer therapeutic. For example, gold nanoshells were used in photothermal cancer therapy as nanoscale heat sources to induce cancer remission in hypoxic tumor areas where there was minimal blood flow.38,39
Among the many nanomaterial platforms that have been explored as drug delivery carriers, nanodiamonds are gaining more attention because of facile drug modification procedures that have mediated improved efficacy and safety in the treatment of multiple tumor models. Although different methods of nanodiamond synthesis are still being explored to yield both fluorescent and nonfluorescent particles with favorable properties, the general process for detonation nanodiamond synthesis involves the harvesting of uniform, truncated octahedral particles following processes such as acid washing, ball milling, and ultrasonication. 40 Several breakthroughs have been made identifying nanodiamonds as a well-tolerated nanoparticle that can be produced in large volumes. 41 Moore et al. 42 identified the enhanced performance of nanodiamond-lipid hybrid particles that successfully targeted triple negative breast tumors to induce regression. Chow and colleagues 41 demonstrated the use of nanodiamond-modified doxorubicin particles to improve circulatory half-life of the drug, improve intratumoral drug retention, and markedly enhance chemotherapeutic efficacy with no apparent myelosuppression. 42 Additional studies have shown that the nanodiamonds can be rapidly loaded with chemotherapeutic agents such as epirubicin at a high loading capacity, as shown in Figure 2 . Furthermore, nanodiamonds have been used as both epidermal growth factor receptor (EGFR)–targeted imaging and therapeutic agents. Figure 3A demonstrates enhanced targeting efficiency of liposome-nanodiamond hybrids, which is quantified in Figure 3B . Figure 3C demonstrates that EGFR-targeted nanodiamond-epirubicin complexes can improve treatment efficacy and safety. Figure 3D shows that these targeted complexes can markedly improve the tolerance of even lethal epirubicin doses while mediating tumor regression. 42 The ability of nanodiamonds to bind a wide range of drug compounds makes them a promising vehicle for drug delivery. 43
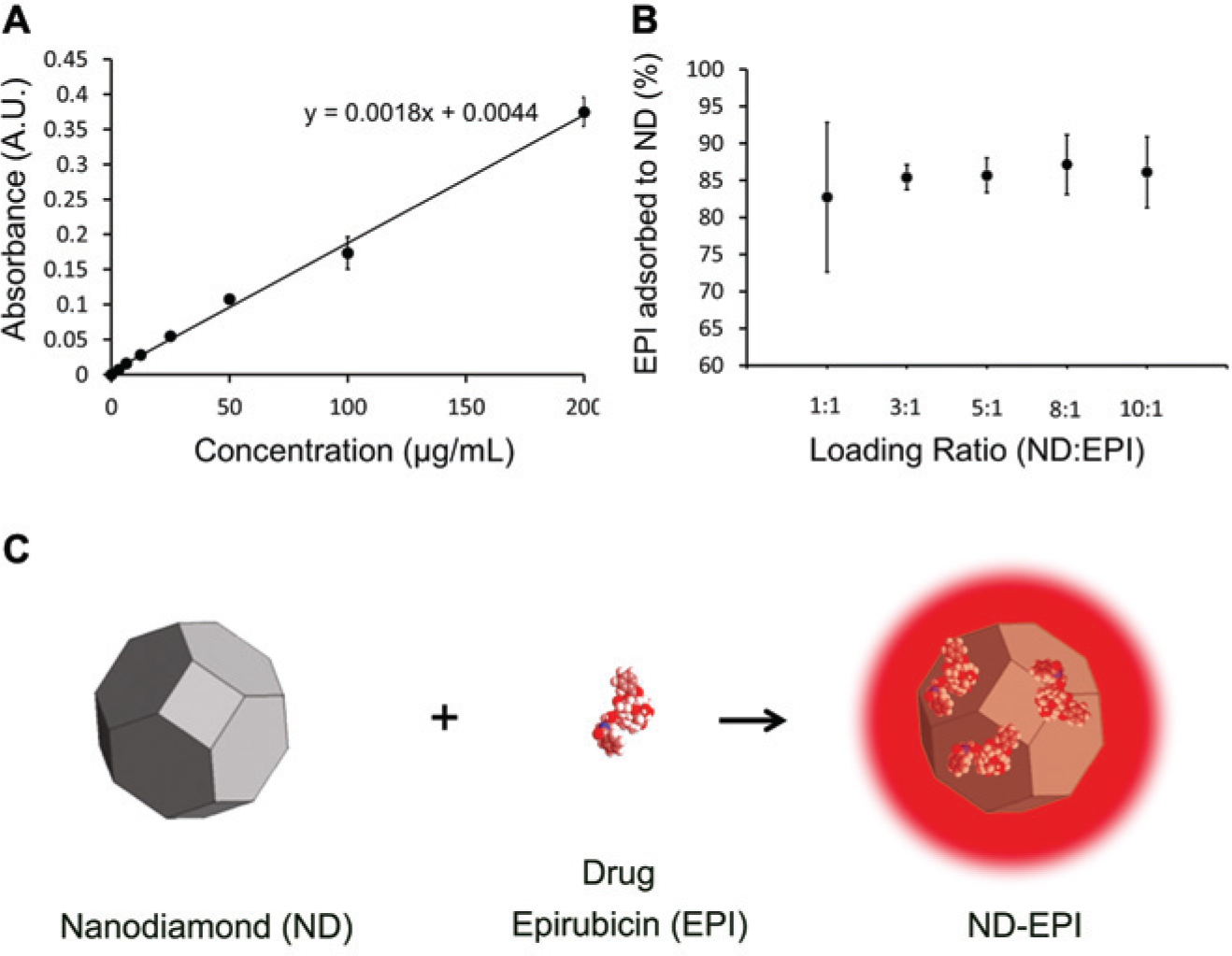
(
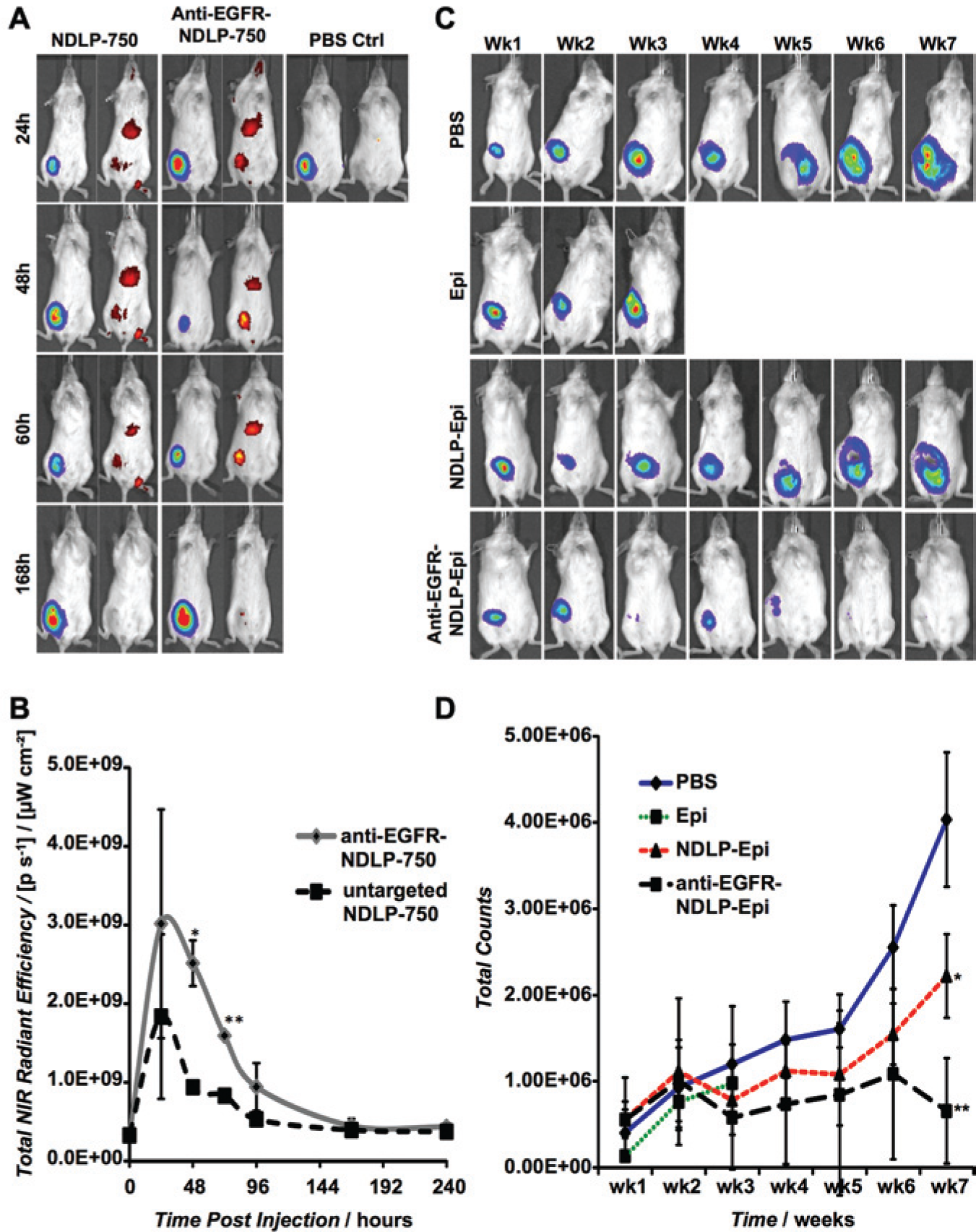
(
In conclusion, nanomedicine has the potential to address many of the pressing challenges in global health in the near future. Many studies have already shown how nanotechnology can be used to increase the efficacy and safety of treatment compared with conventional approaches. Although human clinical studies to assess the efficacy and safety of nanomedicine agents have started to emerge, 44 there are many challenges to address before further commercialization or widespread implementation and clinical acceptance can occur. These barriers include the need for long-term material/therapeutic storage, the availability of substantial clinical trial funding, social and ethical issues, potential health and environmental impacts, regulatory requirements (e.g., manufacturing and controls, safety and toxicity validation, etc.), and a continually evolving intellectual property landscape. Fortunately, there has been an emergence of Food and Drug Administration–approved platforms that are forging the broader use of nanotechnology in the clinic.9,45 Future cooperative efforts in nanomedicine will bring about a positive impact on society. As the biomedical research community continues to make significant breakthroughs in the field of nanomedicine, the future of global health looks to improve considerably.
Footnotes
Acknowledgements
Edward K. Chow gratefully acknowledges support from the National Research Foundation Cancer Science Institute of Singapore RCE Main Grant, National Medical Research Council (NMRC CBRG-NIG BNIG12nov017) and Ministry of Education Academic Research Fund (MOE AcRF Tier 1 T1-2012 Oct-11). Dean Ho gratefully acknowledges support from the National Science Foundation CAREER Award (CMMI-0846323), Center for Scalable and Integrated NanoManufacturing (DMI-0327077), CMMI-0856492, DMR-1105060, V Foundation for Cancer Research Scholars Award, Wallace H. Coulter Foundation Translational Research Award, Society for Laboratory Automation and Screening (SLAS) Endowed Fellowship, Beckman Coulter Life Sciences, and National Cancer Institute grant U54CA151880. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Cancer Institute or the National Institutes of Health.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: National Research Foundation Cancer Science Institute of Singapore RCE Main Grant, National Medical Research Council (NMRC CBRG-NIG BNIG12nov017) and Ministry of Education Academic Research Fund (MOE AcRF Tier 1 T1-2012 Oct-11) to E.K.C, and National Science Foundation CAREER Award (CMMI-0846323), Center for Scalable and Integrated NanoManufacturing (DMI-0327077), CMMI-0856492, DMR-1105060, V Foundation for Cancer Research Scholars Award, Wallace H. Coulter Foundation Translational Research Award, Society for Laboratory Automation and Screening (SLAS) Endowed Fellowship, Beckman Coulter Life Sciences, and National Cancer Institute grant U54CA151880 to D.H. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Cancer Institute or the National Institutes of Health.
