Abstract
Study Design
An Exploratory Study.
Objectives
To estimate the prevalence of scoliosis and associated factors among adolescents, and to evaluate the clinical utility of an electronic scoliometer in school screening.
Methods
The scoliosis school screening was conducted in Xinyang City, Henan Province, in 2024. Students’ study habits and daily routines were collected via questionnaires. Manual and electronic scoliometers were used for primary screening and compared using receiver operating characteristic (ROC) curves and agreement statistics. Three-dimensional ultrasound provided a provisional diagnosis. Multivariable logistic regression identified factors associated with scoliosis.
Results
A total of 1874 students were enrolled in this study. The positive screening rates using manual and electronic scoliometers were 4.97% and 2.87%, respectively. Among these cases, 102 students were referred for 3D ultrasound examination, with 74 students showing an ultrasound Cobb angle ≥10°. The prevalence of scoliosis was 4.55% in seventh-grade students and 4.04% in eighth-grade students. The prevalence of scoliosis was 2.99% in males and 5.96% in females. In the paired sample (n = 39), the electronic device had an AUC of 0.844 (95% CI 0.718-0.971) vs 0.751 (95% CI 0.596-0.907) for the manual device (ΔAUC = 0.093, P = 0.033). Agreement for continuous ATR showed moderate absolute agreement (ICC(3,1) = 0.614; 95% CI 0.373-0.777). Multinomial regression identified sitting with crossed legs and lack of sports participation as potential risk factors.
Conclusions
The prevalence of scoliosis among seventh and eighth-grade students in Xinyang City, Henan Province, was 4.33%. We recommend ATR ≥5°be triaged with 3D ultrasound before radiography; cases with UCA <20°should be rechecked at 3 months. Schools/parents should promote correct seated posture and more physical activity.
Keywords
Introduction
Scoliosis is a complex three-dimensional torsional deformity, characterized by a diagnostic criterion of a Cobb angle of≥10°, as measured by X-ray. 1 It is reported that the positive rate via primary scoliosis school screening (SSS) is 3.97% and the prevalence of scoliosis is 1.20% in Mainland China. 2 Scoliosis is prevalent but sometimes overlooked due to the absence of periodic SSS. 3 Consequently, these adolescents are diagnosed and receive treatment during the progressive phase of scoliosis rather than at an early stage, which is accompanied by a significant financial burden.
For primary SSS, the most frequent approach is a physical examination followed by the forward bending test, with measurement of the angle of trunk rotation (ATR) using a manual scoliometer. While practical, this approach generates false positives and can lead to unnecessary radiography, exposing children to potentially harmful ionizing radiation. Recently, to enhance the efficiency of SSS, an electronic scoliometer featuring automatic data upload capability has been developed. Although this electronic scoliometer has been deployed in some regions as an alternative to a manual scoliometer, its accuracy and consistency remain debated. 4
To date, established protocols typically comprise primary school-based screening followed by radiographic confirmation in a hospital. 5 However, the primary concern regarding X-rays is radiation exposure in students, which is a challenging yet inevitable aspect of the diagnostic process for scoliosis. 6 As a three-dimensional (3D) ultrasound imaging system, the Scolioscan was developed to lead the trend in radiation-free spine imaging using the technique of volume projection imaging. Although studies have validated the reliability of Scolioscan for measuring coronal spinal curvature against radiographic standards, its adoption in SSS remains limited.7,8
Therefore, a meticulously designed SSS was performed in Xinyang City, Henan Province, China, involving the application of manual scoliometers and electronic devices (electronic scoliometers and Scolioscan). This study aimed to determine scoliosis prevalence and associated risk factors among adolescents in Xinyang City, while evaluating the clinical utility of electronic devices within school-based programs. The findings are intended to inform practical choices for school screening programs seeking to reduce unnecessary radiography.
Methods
Study Design and Subjects
Based on national guidelines and available international methods, the SSS was conducted among junior school students from grades 7 to 8 in HuaiBin County Experimental School (East Campus), Xinyang City, Henan Province, in March 2024. The students with spine and chest deformities, musculoskeletal disorders, neurological disorders, and a history of spinal operation were excluded. A total of 1874 students were enrolled, and 1710 (91.2%) students completed the SSS. Classes participating in the screening were selected in collaboration with the local education authority, which coordinated school participation and logistics.
Study Objectives
The primary objective of this study was to estimate the prevalence of scoliosis and to identify associated risk factors among seventh and eighth-grade students in Xinyang City. The secondary objective was to evaluate the clinical utility of electronic devices used in school screening, specifically an electronic scoliometer and a three-dimensional ultrasound imaging system, focusing on their diagnostic performance, measurement agreement, and practical suitability for routine school screening.
Sample Size
No formal sample size or power calculation was performed because the screening was conducted as a school-based activity in collaboration with the local education authority. This approach allowed estimation of local prevalence and assessment of device performance under field conditions. The findings are exploratory and should be confirmed in larger, population-representative studies.
Ethics Approval and Consent to Participate
The study protocol was reviewed and approved by the Institutional Ethics Review Board of Peking University People’s Hospital (IRB No. 2024PHB100-001). The school-based screening was organized with the local education authority. Written informed consent was obtained from parents/guardians before participation, and assent was obtained from all students at the time of screening. The study adhered to the Declaration of Helsinki and applicable national/local regulations. Ultrasound is a non-ionizing technology; no radiographs were performed for research purposes, and any clinically indicated imaging followed routine care pathways.
Questionnaire Investigation
Prior to SSS, all students were required to complete the questionnaire, which contained the items referring to basic information, habitual posture, backpack style, daily activities, dietary behavior, learning environment, the history of pain and disease. The questionnaire could be acquired by scanning the QR code using the WeChat application, and the students were requested to finish the questionnaire in 30 minutes. If the students failed to understand any question, he/she would consult the teachers or parents. Prior to field use, the questionnaire underwent content review by a multidisciplinary expert panel convened by the Chinese Center for Disease Control and Prevention (CDC) Nutrition Group and the China CDC Center for Chronic Disease Prevention and Control, and was subsequently pilot-tested to refine item wording and skip logic. The original questionnaire is provided as Supplementary 1.
The Criteria and Procedure of Primary SSS
According to the pre-established plan, the male and female students would be separately screened class by class in a private space. To mitigate the impact of incorrect posture, all students underwent a spinal motion test—consisting of flexion, extension, lateral bending, and rotation of the spine—before screening. The primary step of SSS was simplified as a forward bending test, during which the examiner inspected asymmetries of the thorax, scapula, waist, and pelvis lean, as well as the spinous process line, and then the ATR was measured using a scoliometer. Specifically, tests were performed with students standing feet together, knees extended, and bending forward to 90°, arms hanging, with the examiner viewing from behind. For each suspected level (thoracic/thoracolumbar/lumbar), the examiner recorded ATR in degrees; each level was measured twice, and the mean value was used for referral decisions. Examiners were trained in a standardized protocol prior to fieldwork. In our study, the ATR for each student was measured twice—once with a manual scoliometer and once with an electronic scoliometer. There were six examining groups with two examiners in each group (a doctor/nurse plus a school doctor/gym teacher). In the screening process, the manual scoliometer (Jiansheng ST-201) was used by one examiner, and the ATR was recorded by another examiner. In contrast, only one examiner could complete the screening process using an electronic scoliometer (Zhuoyong ZY-CW01), since the data could be automatically recorded. Students with ATR ≥ 5° measured by either a manual scoliometer or an electronic scoliometer would be examined by the 3D ultrasound system.
The Procedure of 3D Ultrasound Examination
In this study, a 3D ultrasound imaging system (Scolioscan, Model SCN201, Telefeld Medical Imaging Ltd, Hong Kong) with a linear probe (central frequency of 7.5 MHz and 7.5 cm width) was utilized to acquire ultrasound images of the spine. During ultrasound scanning, students maintained a standing position with arms resting naturally, achieving an average scan duration of 30-40 seconds. The manual ultrasound Cobb angle (UCA), similar to the radiographic Cobb angle, was acquired by the ultrasound volume projection image technique. UCA ≥ 10° was regarded as a scoliosis case (either in the thoracic or lumbar spine), and a false-positive case was defined as students with ATR ≥ 5° (by either method) while UCA < 10°.
Students with a UCA of 20° or greater were referred for radiographic confirmation. Those with a UCA between 10° and 20° received prescribed spinal exercises and were scheduled for ultrasound follow-ups at 3 and 6 months. Intervention was initiated if progression exceeded 5° within 6 months or 10° within 1 year from baseline. Individuals with ATR ≥5° and UCA <10° were recommended for re-examination 3 months later. The procedure of entire SSS was shown in Figure 1. Flowchart of scoliosis school screening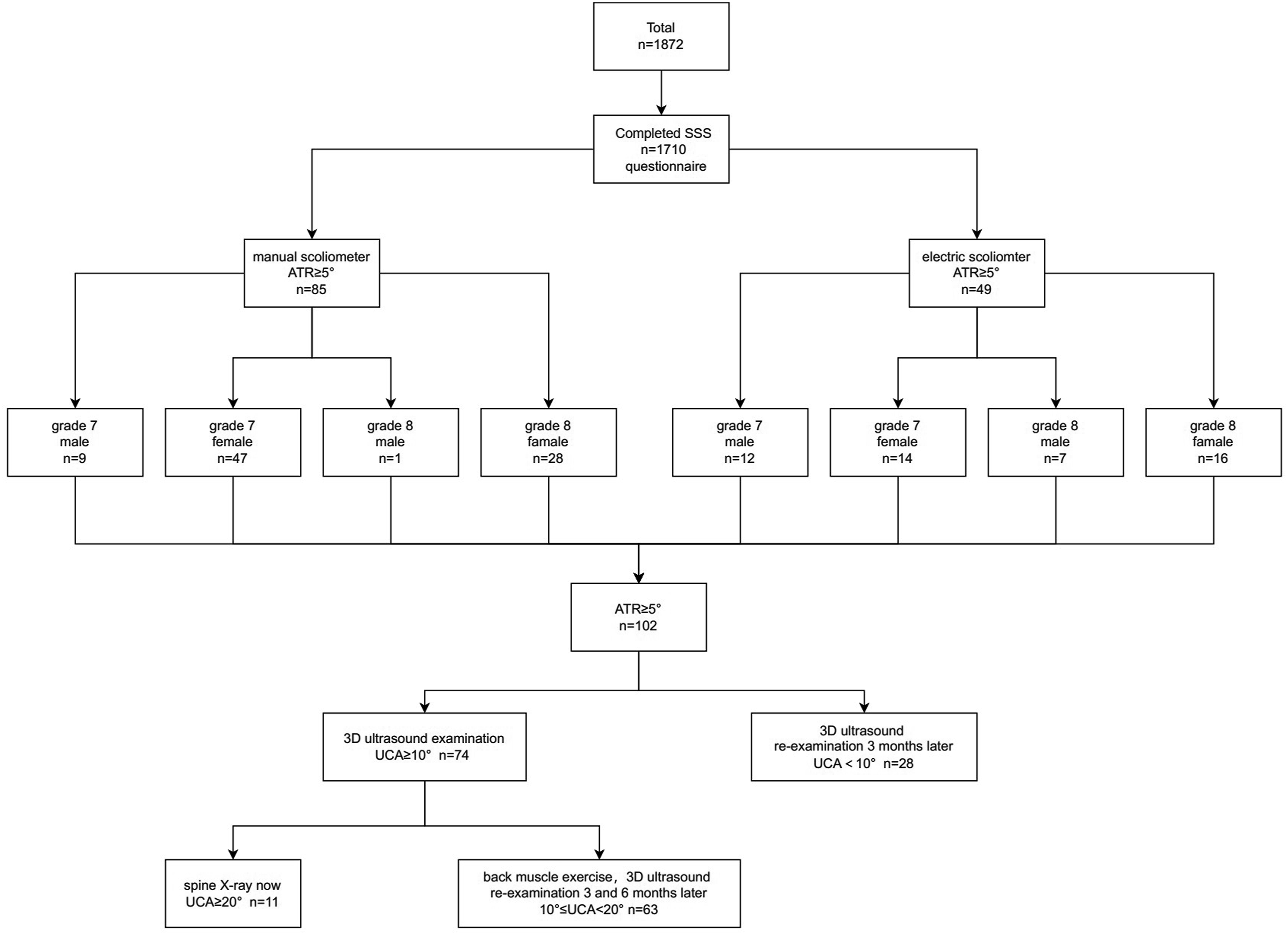
Statistical Analysis
Results were presented as percentages or mean ± standard deviation. Continuous variables were analyzed using independent sample t-tests, while categorical variables underwent chi-squared tests. For questionnaire-based analyses, we modelled ultrasound-confirmed scoliosis (UCA ≥10°) as a binary outcome using multivariable binary logistic regression. Device discrimination was assessed with receiver-operating characteristic (ROC) curves and area under the curve (AUC) with 95% confidence intervals. In participants who had same-visit measurements by both instruments, AUCs were compared using the DeLong test for correlated ROC curves. The agreement for continuous ATR between devices was quantified using the intraclass correlation coefficient (ICC) with a two-way mixed-effects, single-measure, absolute-agreement model (ICC(3,1)). The 95% confidence intervals for ICCs were calculated using the F-distribution. Statistical Analyses were performed by using IBM SPSS Statistics 24.0 and R (version 4.4.2). All tests were two-sided, and P < 0.05 was considered statistically significant.
Results
The Distribution of Students From Grade 7 and 8 Underwent SSS
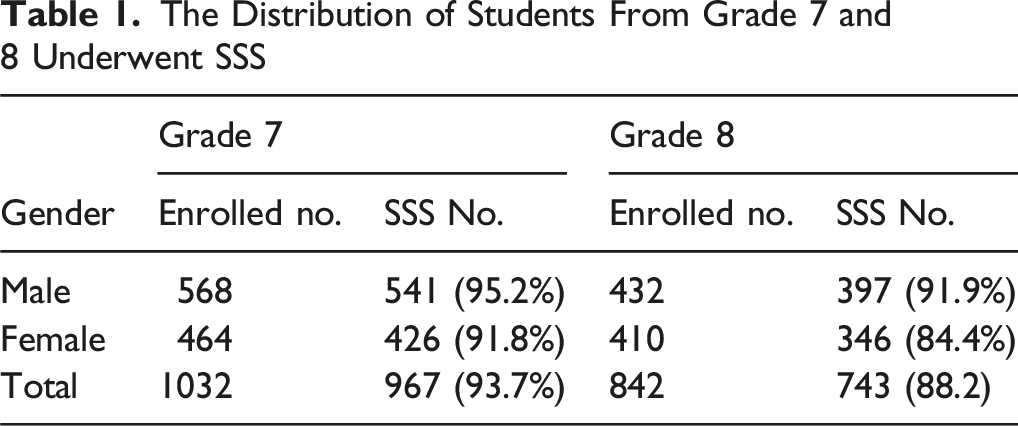
The Positive Rate of Primary Screening by Both Manual and Electric Scoliometer
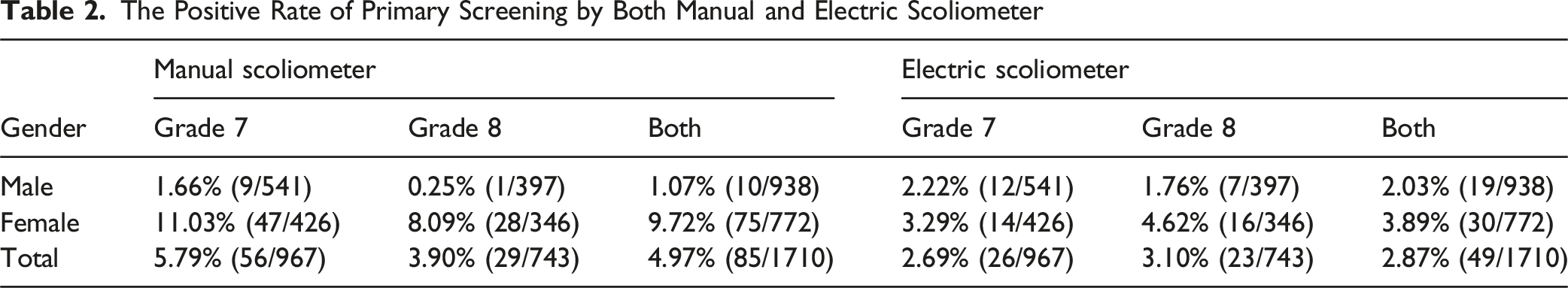
Using manual and electronic scoliometers, ATR ≥5° was detected in 85 and 49 students, respectively. As 32 students tested positive on both devices, the actual cohort with ATR ≥5° comprised 102 individuals. In the manual scoliometer group, 64 cases were diagnosed with scoliosis (thoracic/lumbar curves), with a 24.71% false-positive rate in SSS screening. The electronic scoliometer group had 40 scoliosis diagnoses and an 18.37% false-positive rate. Overall, among 102 cases that screened positive by either device, 74 were confirmed to have scoliosis, resulting in a 31.37% aggregate false-positive rate.
In the paired subset of students who had same-visit measurements by both devices (n = 39), ROC analysis predicting ultrasound-confirmed scoliosis yielded an AUC of 0.751 (95% CI: 0.596-0.907) for the manual scoliometer and an AUC of 0.844 (95% CI: 0.718-0.971) for the electronic scoliometer. The paired DeLong test indicated a modest but statistically significant difference favoring the electronic device (ΔAUC = 0.093, 95% CI: 0.007-0.179; P = 0.033) (Figure 2). Agreement for continuous ATR between devices indicated moderate absolute agreement, as indicated by a two-way mixed-effects single-measure ICC (ICC(3,1) = 0.614 (95% CI 0.373-0.777). The corresponding average-measure ICC was ICC(3,k) = 0.761 (95% CI 0.544-0.875). Receiver operating characteristic (ROC) curves for manual and electronic ATR measurements predicting ultrasound-confirmed scoliosis (UCA ≥10°) in the paired subset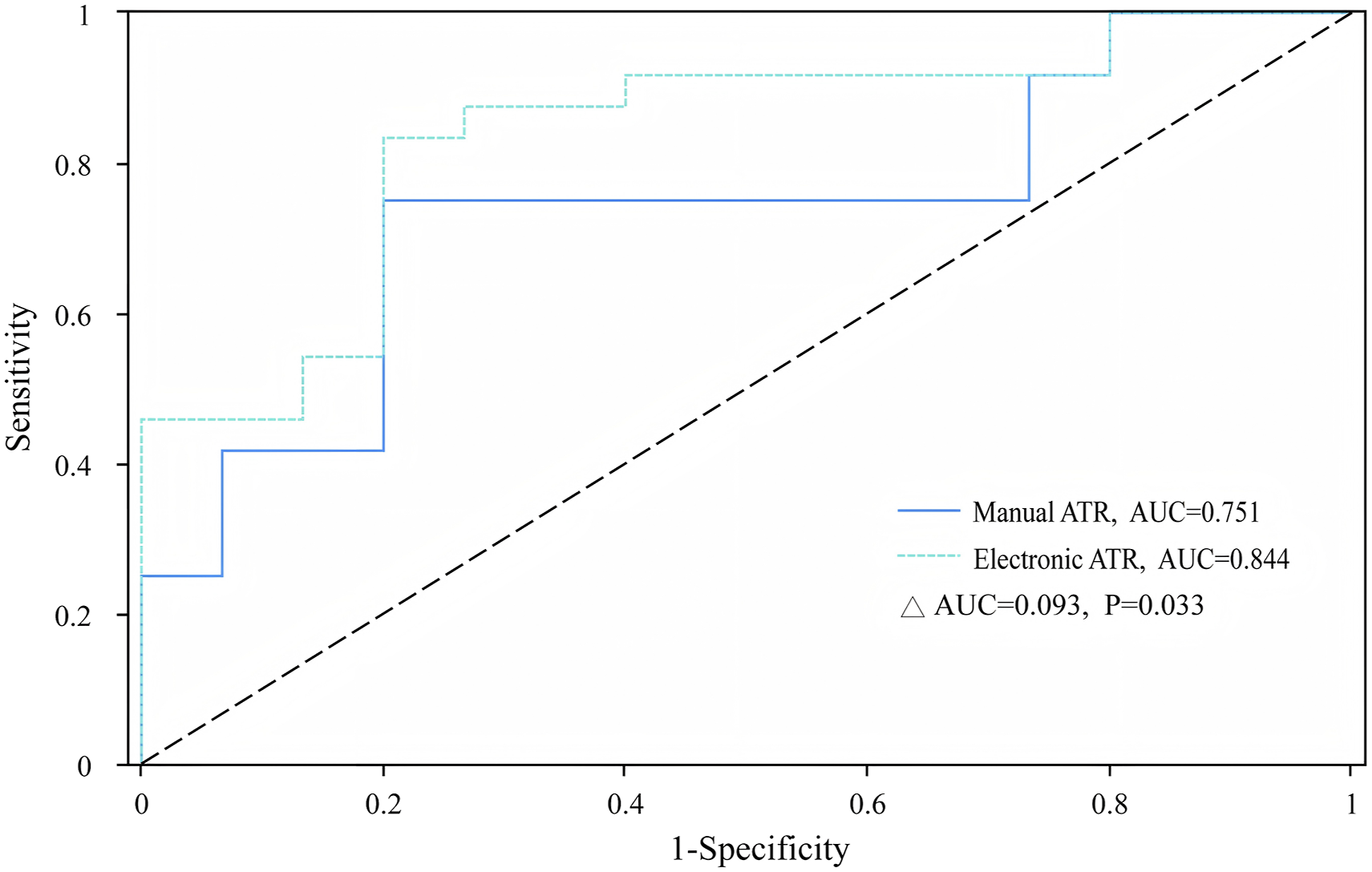
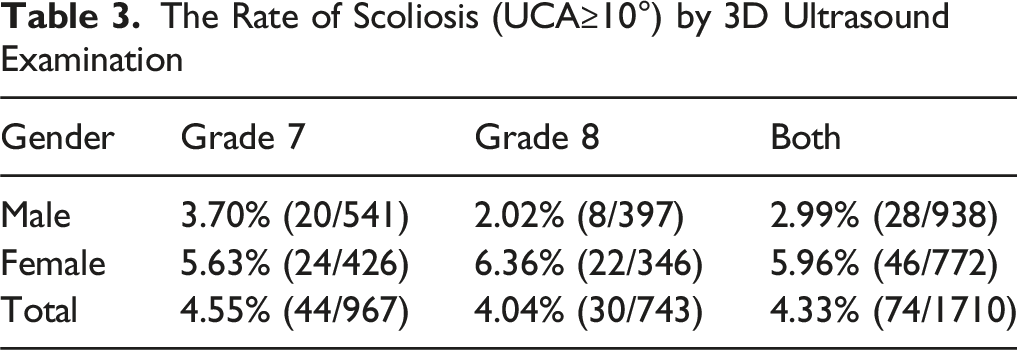
The Rate of Scoliosis (UCA≥10°) by 3D Ultrasound Examination
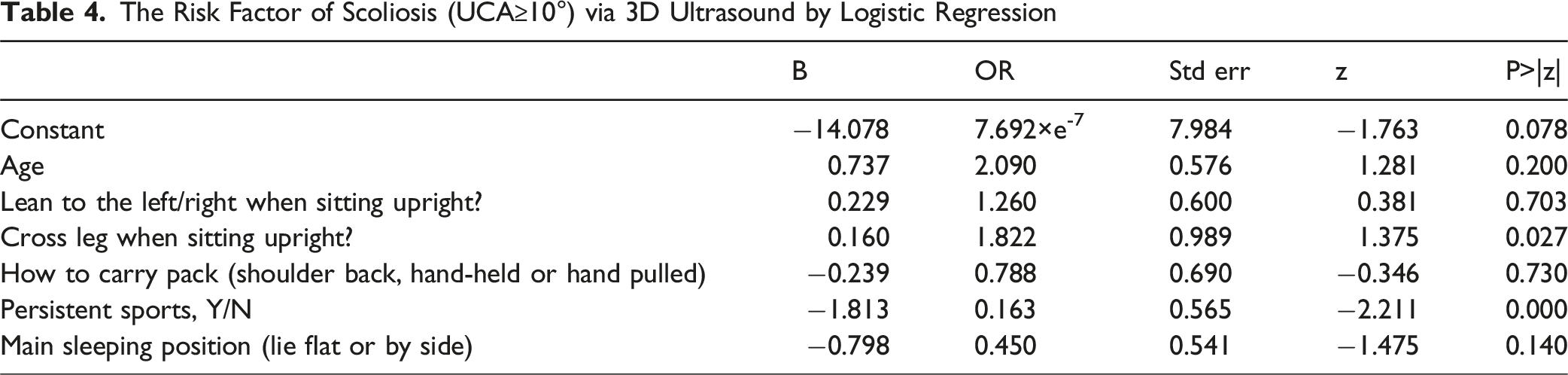
The Risk Factor of Scoliosis (UCA≥10°) via 3D Ultrasound by Logistic Regression
Discussion
This city-level implementation study evaluated a pragmatic, radiation-sparing school-screening workflow in Xinyang, Henan Province, that combined forward-bend ATR measurement with 3D ultrasound triage, and concurrently examined the field performance of manual and electronic scoliometers, as well as questionnaire-based associations. The positive screening rates in Xinyang, using a manual scoliometer and an electronic scoliometer, were 4.97% and 2.87%, respectively. Females demonstrated a higher rate of positive screening for scoliosis compared to males. Among 102 students with an initial positive screening result, approximately 72.55% were diagnosed with scoliosis through 3D ultrasound assessment. Questionnaire analysis identified sitting with crossed legs while upright and lack of regular sports participation as possible risk factors for the occurrence or progression of scoliosis.
A study of 2.22 million adolescents in mainland China reported an average scoliosis prevalence of 1.2% using X-ray, which is lower than the 4.33% rate identified by 3D ultrasound in our study. 2 This discrepancy may be attributed to our focus on the high-risk age group for scoliosis. Consistent with other research, females showed a higher prevalence of scoliosis than males, with positive rate ratios (girls: boys) ranging from 1.1:1 to 18:1 across studies, aligning with our observed ratio of 1.99:1.9,10 Multiple studies have associated incorrect posture with scoliosis.11,12 Our prior research demonstrated that the spinal motion test reduced the false-positive rate by correcting incorrect posture. 13 In the current study, the implementation of the spinal motion test for all students prior to screening yielded a false-positive rate of 31.37%. In contrast, Yılmaz et al. reported that among 2515 students who screened positive via ATR measurement and forward bend testing, only 380 were subsequently confirmed to have scoliosis by X-ray, resulting in a significantly higher false-positive rate of 84.89%. 9
Common scoliosis screening methods include physical examination, ATR measurement, and Moiré topography, with subjects showing suspicious results typically referred for radiographic confirmation. 5 However, unnecessary radiation exposure occurred due to false positives. Furthermore, patients with radiographic Cobb angles exceeding 20° require interventions, while those with angles of 10°-20° require periodic X-ray monitoring. 1 Studies indicated that idiopathic scoliosis patients faced up to 5 times higher overall cancer incidence than age-matched peers. 14 The emergence of 3D ultrasound may address this concern. Ultrasound Cobb angles derived from anatomical landmarks (spinous/transverse processes) demonstrated strong linear correlation with radiographic Cobb angles (R2≥0.90).15,16 In this study, 3D ultrasound confirmed scoliosis at a 4.33% positivity rate. We recommend immediate radiographic evaluation for patients with ATR ≥5° combined with a ultrasound Cobb angle ≥ 20°. Those with an ultrasound Cobb angle <20° should receive back muscle exercises and undergo a 3-month ultrasound follow-up. This protocol may reduce radiation exposure while ensuring diagnostic accuracy.
Multiple studies have shown that study habits and daily routines are correlated with the development of scoliosis.17,18 In our research, we collected the habits and basic information of students through questionnaires prior to scoliosis screening. Logistic regression analysis revealed that sitting with crossed legs while upright increased the likelihood of scoliosis, whereas participation in sports reduced this risk. Consistent with our findings, Zhu et al. demonstrated that adolescents who achieved at least 60 minutes of moderate-to-vigorous physical activity daily exhibited a lower likelihood of developing scoliosis. 17 A Syrian study aligned with our findings in reporting no association between scoliosis development and either leaning laterally (left/right) when sitting upright or backpack-carrying methods. However, this study also identified right-sided sleeping position as increasing scoliosis risk compared to flat position and found no elevated risk from sitting with crossed legs, both of which diverged from our results. 18 These discrepancies may be attributed to factors such as ethnicity, geographical variations, and differences in the age distribution of study cohorts. Given the exclusively recruited cohort of seventh and eighth-grade students with a focused age range, this study observed no association between age and scoliosis.
In paired analyses, the electronic scoliometer demonstrated superior discrimination relative to the manual device. At the same time, agreement testing revealed only moderate absolute agreement for single readings, but improved reliability when multiple measurements were averaged. However, given the small paired sample, these observations are preliminary and should be interpreted with caution; we therefore report them briefly and recommend local validation and larger, radiograph-confirmed paired studies to establish their practical relevance.
This study has several limitations. First, because we enrolled only seventh- and eighth-grade students and performed 3D ultrasound triage only for those with ATR ≥5°, the observed prevalence and device-performance estimates may not generalize to adolescents and are susceptible to partial verification biases. Second, the paired device comparison sample was modest in size, which reduces the precision of AUC and ICC estimates. Importantly, most diagnoses relied on 3D ultrasound rather than universal radiographic Cobb angles; although prior work shows good correlation between these modalities, the absence of routine radiographic confirmation could bias prevalence estimates and affect measures of diagnostic accuracy. Larger radiograph-confirmed paired studies would strengthen these inferences. Finally, the use of questionnaires to collect data on study habits and daily routines may introduce recall bias. Future large-scale, multi-center prospective studies with comprehensive radiographic and ultrasonographic data sets are warranted to validate these findings.
Conclusion
This study demonstrates that both the electronic scoliometer and 3D ultrasound imaging exhibit significant clinical utility in scoliosis screening. Owing to its absence of ionizing radiation, 3D ultrasound achieves markedly higher patient acceptance rates compared to X-ray examinations, suggesting its potential as a primary alternative for future screening protocols. Based on the exploratory regression analysis outcomes, we recommend implementing structured health education interventions to correct postural behaviors and increase physical activity levels, thereby reducing the risk of scoliosis.
Supplemental Material
Supplemental Material - Scoliosis School Screening Using Electronic Devices in Henan Province, China: An Exploratory Study
Supplemental Material Scoliosis School Screening Using Electronic Devices in Henan Province, China: An Exploratory Study by Weiwei Xia, Hongzhen Li, Shuaiqi Zhu, Chong Zhao, Bing Hou, Zhijie Zhu, Yongping Zheng, De Yang, Yanhui Dong, Haiying Liu, Shuai Xu in Global Spine Journal
Footnotes
Ethical Considerations
The study protocol was reviewed and approved by the Institutional Ethics Review Board of Peking University People’s Hospital (IRB No. 2024PHB100-001). The school-based screening was organized with the local education authority. Written informed consent was obtained from parents/guardians prior to participation, and assent was obtained from all students at the time of screening. The study adhered to the Declaration of Helsinki and applicable national/local regulations. Ultrasound is non-ionizing; no radiographs were performed for research purposes, and any clinically indicated imaging followed routine care pathways.
Consent for Publication
All parents provided their written informed consent before they participated in this study, and the consent for publication was obtained from the parents.
Author Contributions
S. X and Hy. L designed and supervised this study. Yh. D and D. Y were involved in the enrollment of all participants. C. Z and B. H participated in measurements. Ww. X, Zj. Z and Yp. Z is involved in the data collection and statistical analysis. Ww. X and Sq. Z drafted the initial manuscript. Hz. L contributed to the revision of the manuscript, including statistical re-analysis and responses to reviewer comments. All authors read and approved the final manuscript.
Funding
This research was supported by (1) Clinical Medicine Plus X-Young Scholars Project Peking University, the Fundamental Research Funds for the Central Universities [grant number PKU2023LCXQ042], (2) the Beijing Natural Science Foundation [grant number 7232182], (3) Peking University Clinical Scientist Training Program (grant number BMU2024PYJH016), (4) China Association for Science and Technology: Innovative Service for Management of Scoliosis in Tibetan Adolescents (grant number: N/A).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data could be obtained by contacting the corresponding author.
Supplemental Material
Supplemental material for this article is available online.
