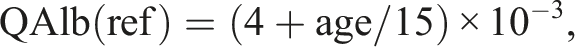Abstract

Dear Editor,
I commend Arora and colleagues for their comprehensive systematic review and meta-analysis of cerebrospinal fluid (CSF) and blood biomarkers in degenerative cervical myelopathy (DCM). 1 Their work provides valuable insight into biochemical correlates of spinal cord pathology. However, I would like to respectfully highlight one methodological issue that may substantially influence a key interpretation—namely, that elevated albumin-, IgA-, and IgG-CSF/serum quotients indicate blood–spinal-cord-barrier (BSCB) disruption. 1
In this meta-analysis, raw quotient means were pooled from cohorts with markedly different ages. DCM groups were predominantly older adults (mean ages approximately 52-70 years), whereas control groups spanned a much wider age range, including adolescents and young adults (with mean ages as low as 17.9 years) as well as older adults. Such pooling of unadjusted quotient values overlooks the well-documented age dependence of CSF/serum albumin and immunoglobulin quotients (QAlb, QIgG, QIgA, QIgM), which increase physiologically with age due to normal microvascular and choroid-plexus changes.
Since Reiber’s seminal description of the age-adjusted hyperbolic reference function
In the two principal studies contributing quotient data (Schmidt 2023; Blume 2020), age matching was based on mean values, but CSF/serum quotients were still interpreted without explicit adjustment to age-dependent reference limits, despite broad age distributions (standard deviations exceeding 10-15 years in some groups). Physiologic aging alone can elevate QAlb by approximately 20%-40%, which is non-trivial and may contribute substantially to the reported pooled increase in CSF/serum quotients (ratio = 2.6; P < .001). Thus, part of the observed effect could plausibly reflect age-related variance rather than true BSCB dysfunction.
Two Key Questions
1. How were differences in participant age addressed when pooling albumin- and immunoglobulin-quotient data? Were quotients normalized to age-adjusted reference limits or expressed as proportions exceeding age-appropriate thresholds? 2. If no age adjustment was performed, on what empirical grounds can the higher quotient values be attributed to pathologic barrier disruption rather than the physiologic rise associated with normal aging?
Clarifying these points would strengthen the reliability of the authors’ conclusions. Prior analyses in other neurological disorders have shown that age correction can nullify apparent barrier abnormalities. 5
I sincerely thank the authors for their important contribution and Global Spine Journal for fostering constructive scientific dialogue on this clinically relevant topic.