Abstract
Study Design
Retrospective quasi-experimental study conducted at two Level I trauma centers over a 6-year-period.
Objectives
Unstable thoracolumbar burst fractures are frequently treated by circumferential (360°) stabilization. Due to ongoing debate, this study aimed to compare whether single- or two-stage 360° stabilization leads to a shorter hospital length of stay in those patients.
Methods
Non-polytraumatized adults (ISS ≤15) with unstable thoracolumbar fractures who underwent 360° stabilization were included. Total hospital length of stay was defined as primary outcome. Secondary outcomes were operative time, intraoperative blood loss and in-hospital mortality. Mann-Whitney U and chi-square tests were applied to compare continuous and categorical variables, respectively, with P < 0.05 as the threshold for significance.
Results
A total of 184 patients was eligible (single-stage, n = 104; two-stage, n = 80). Age, sex distribution, and ASA scores did not differ between both groups. Hospital length of stay was significantly shorter in the single-stage group (9+/−4 days) compared to the two-stage group (11+/−5 days; P < 0.001). Operative time was significantly shorter in the single-stage group (194+/−75 min) compared to the two-stage group (230+/−91 min; P = 0.003). Blood loss was significantly less in the single-stage group (500+/−400 mL) compared to the two-stage group (750+/−635 mL; P = 0.033). There was no in-hospital mortality in both groups.
Conclusions
Single-stage 360° stabilization for unstable thoracolumbar fractures in non-polytraumatized patients is superior to the two-stage approach regarding length of hospital stay, operative time, and intraoperative blood loss. Consequently, a single-stage procedure should be preferred whenever feasible.
Keywords
Introduction
Traumatic thoracolumbar burst fractures (T10-L3) involving neurological deficits, posterior tension band disruption, or fracture dislocation achieve better outcomes with surgical rather than non-operative management, often requiring urgent decompression and stabilization. 1 Commonly, posterior pedicle screw and rod stabilization alone is employed – with or without vertebral body augmentation using an intracoropral device with bone cement (posterior-only stabilization). A (partial) corpectomy with anterior column decompression and cage reconstruction is another option, as is circumferential (360°) stabilization.2-5 Anterior instrumentation offers the potential to stabilize the anterior and middle columns and restore sagittal alignment. 4 In contrast, posterior-only stabilization has been linked to hardware loosening, likely since the anterior column accounts for approximately 80% of spinal stability.3,6,7 Consequently, the use of 360° stabilization has increased since the early 2000s. 3
In procedures combining anterior-posterior stabilization, debate continues regarding the optimal timing or staging of these 2 steps. 8 Obvious factors influencing decision-making regarding single-stage vs two-stage procedures comprise the patient’s fitness for surgery, operating room capacities, and surgical expertise and equipment. Importantly, there is gap of knowledge regarding implications on hospital length of stay, surgical time, and blood loss of single- and two-stage strategies. Thus, the objective of this bi-centric study was to compare single-stage vs two-stage 360° stabilization of unstable thoracolumbar fractures.
Methods
Data Sources and Data Collection
This study was approved by the local ethics committees (Kantonale Ethikkommission Bern, project-ID 2021-02021). This bi-centric, quasi-experimental retrospective study was conducted from January 2012 to January 2018 at two Swiss Level I trauma centers: Inselspital, University Hospital Bern, and Kantonsspital Graubünden in Chur. Medical charts, imaging, operative reports, discharge summaries, anesthesia protocols, and laboratory sheets were retrieved and consolidated in a comprehensive database.
Study Population
Adult patients (≥18 years) with acute thoracolumbar injuries (T10–L3) who underwent 360° stabilization with first treatment within 48 hours of injury and an Injury Severity Score (ISS) ≤15 were eligible. Fractures were classified as AO Spine types A2–A4, with or without posterior tension band disruption (B-type) and fracture dislocation (C-type). A quasi-experimental study design was employed as patients were assigned to one of two groups based solely on the surgical strategy exclusively used at each institution: Patients at one center (Kantonsspital Graubuenden, Chur) received a single-stage procedure, whereas patients at the other center (Inselspital, University Hospital of Bern) were managed by a two-stage procedure. Patients with incomplete outcome data, presenting with non-acute injuries or low-energy trauma, or without general research consent were excluded. Key demographic and clinical parameters included age, sex, ASA score, trauma mechanism, concomitant injuries, neurologic deficits, and the indication for decompression. Neurological status was determined using the AO Spine (N0–N4 or Nx) classification, and cases classified as Nx were excluded unless an unrelated etiology was established.
Surgical Technique
All procedures were performed under general anesthesia. Patients were positioned prone on a radiolucent operating table for the posterior approach, with fluoroscopic guidance used at the surgeon’s discretion. Posterior stabilization typically involved pedicle screw instrumentation, inserted via a conventional open approach or percutaneously, based on fracture morphology and surgeon preference. One center preferred an open approach in all procedures, while the other center preferred a percutaneous approach in cases without decompression. Decompression was performed in patients with neurological deficits or significant spinal canal stenosis.
For the anterior column, a lateral approach was employed. In type A3 fractures, a partial corpectomy (monosegmental anterior fusion), and in type A4 fractures, a complete corpectomy (bisegmental anterior fusion) was performed. A static or expandable vertebral body replacement cage was placed for reconstruction, followed by bone grafting with local autologous bone from the fractured vertebra. In the single-stage group, both posterior and anterior steps were completed in a single operative session including intraoperative repositioning. In the two-stage group, the anterior procedure followed the initial posterior stabilization at a later stage. Standard postoperative imaging with conventional X-ray was obtained to confirm instrument placement and construct alignment (Figure 1). Preoperative CT and Postoperative X-ray of a 28-Year-old Patient With a Burst-Split Fracture at L1 (AO type A4, N0) Fracture After a Skiing Accident. Left: Sagittal and Coronal View of Preoperative CT. Right: a. p. and Lateral Views of Postoperative Standing Conventional X-ray, After Two-Stage 360°-Stabilization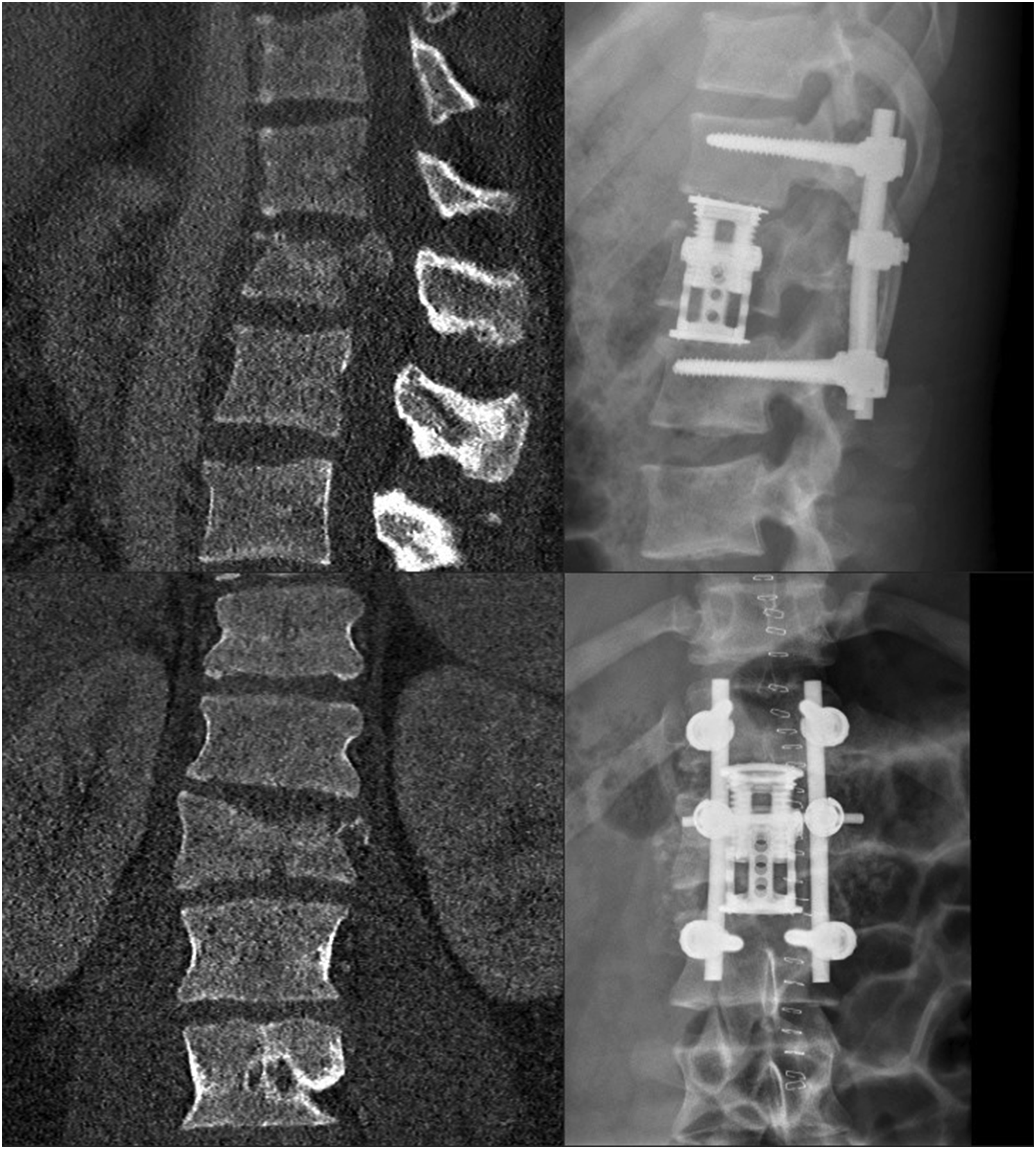
Outcomes
The primary outcome was hospital length of stay, defined as the interval (in days) from admission to discharge, encompassing pre-, peri-, and postoperative time in the general ward. Secondary endpoints included cumulative operative time, intraoperative blood loss and in-hospital mortality. Cumulative operative time (in minutes) was measured from skin incision to skin closure for the spinal procedure. Operative time and blood loss were primarily obtained from anesthesia records, which also provided ASA scores.
Statistical Analysis
All analyses were conducted using R software (Version 4.4.0 “Puppy Cup”; R Foundation for Statistical Computing, Vienna, Austria). Continuous variables were tested for normality using the Shapiro-Wilk test, which confirmed non-normal distributions for operative time, blood loss, and hospital length of stay (all P < 0.05). Consequently, these variables were compared between groups using Mann-Whitney U tests and expressed as median (interquartile range).
For stratified analyses, patients were categorized by procedure type (decompression vs non-decompression), neurological status (deficit vs no deficit), and AO fracture classification. For pooled analyses, patients from both surgical approach groups were combined and stratified by procedure type (decompression vs non-decompression), neurological status (deficit vs no deficit), AO fracture classification, and number of instrumented dorsal levels (≤3 vs >3). For the AO classification, each patient was assigned to a single group based on their highest fracture type (C > B > A) to avoid statistical redundancy when patients had multiple classifications. The Kruskal-Wallis test was used for comparisons involving 3 or more groups (AO classification).
Statistical significance was set at P < 0.05, with Bonferroni correction applied to account for multiple tests. Data processing was performed using base R functions.
A post-hoc power analysis was conducted using R (Version 4.0.2) and the pwr package. For each endpoint, effect sizes (Cohen’s d) were calculated based on the observed differences and pooled standard deviations between groups. A two-sample t-test (two-sided, α = 0.05) was then used to estimate the achieved power. For hospital length of stay, the post-hoc power analysis indicated a power of 88.5% (Cohen’s d = 0.47).
Results
Demographics and Baseline Characteristics
Baseline Characteristics of Study Participants
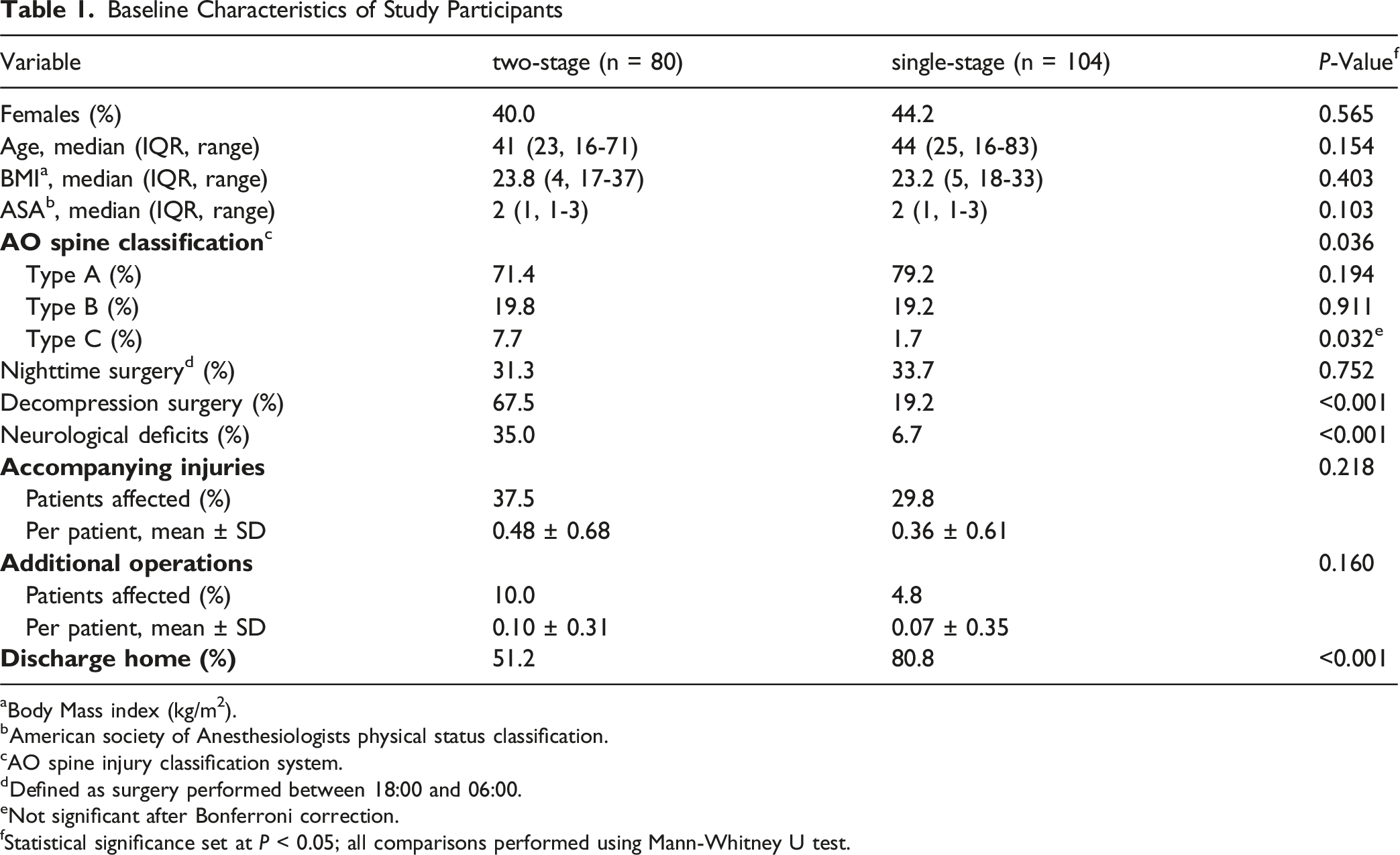
aBody Mass index (kg/m2).
bAmerican society of Anesthesiologists physical status classification.
cAO spine injury classification system.
dDefined as surgery performed between 18:00 and 06:00.
eNot significant after Bonferroni correction.
fStatistical significance set at P < 0.05; all comparisons performed using Mann-Whitney U test.
Mechanism of Injury by Treatment Group
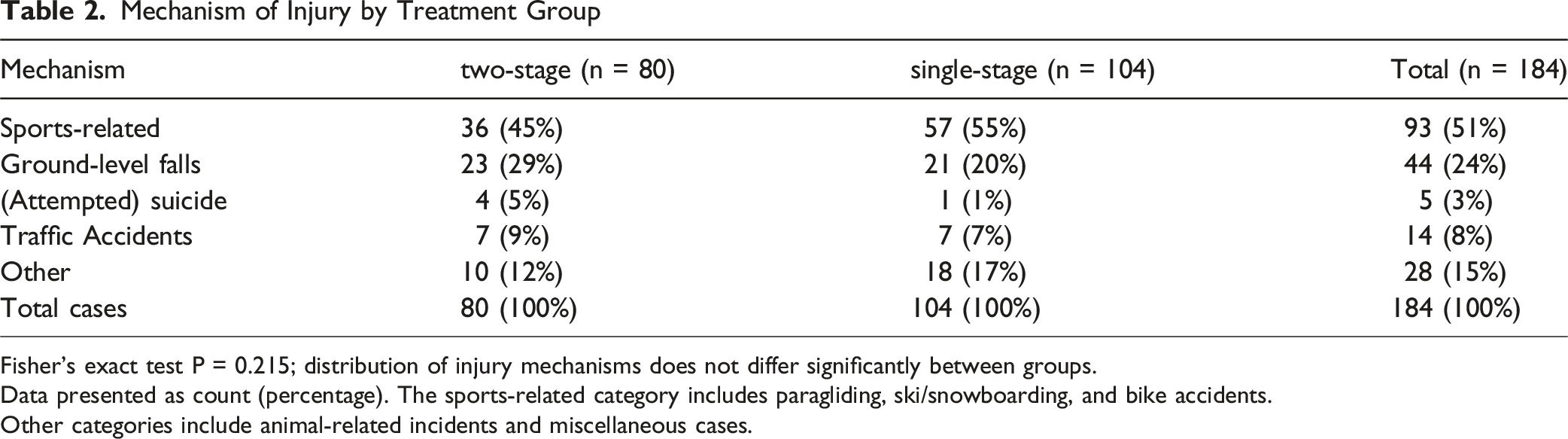
Fisher’s exact test P = 0.215; distribution of injury mechanisms does not differ significantly between groups.
Data presented as count (percentage). The sports-related category includes paragliding, ski/snowboarding, and bike accidents.
Other categories include animal-related incidents and miscellaneous cases.
Clinical Outcomes
Operative and Clinical Outcomes: Primary Analysis and Subgroup Analyses
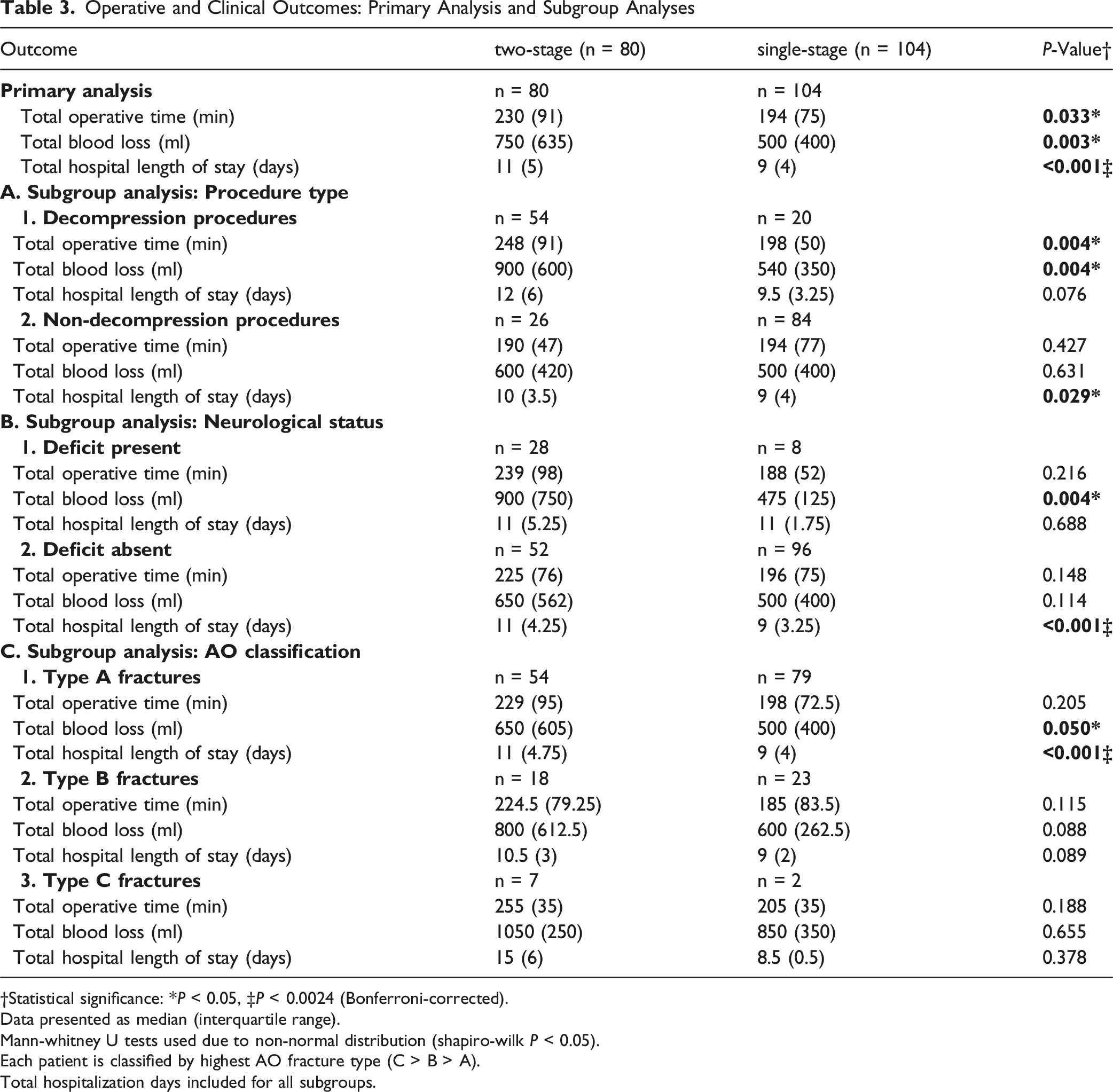
†Statistical significance: *P < 0.05, ‡P < 0.0024 (Bonferroni-corrected).
Data presented as median (interquartile range).
Mann-whitney U tests used due to non-normal distribution (shapiro-wilk P < 0.05).
Each patient is classified by highest AO fracture type (C > B > A).
Total hospitalization days included for all subgroups.
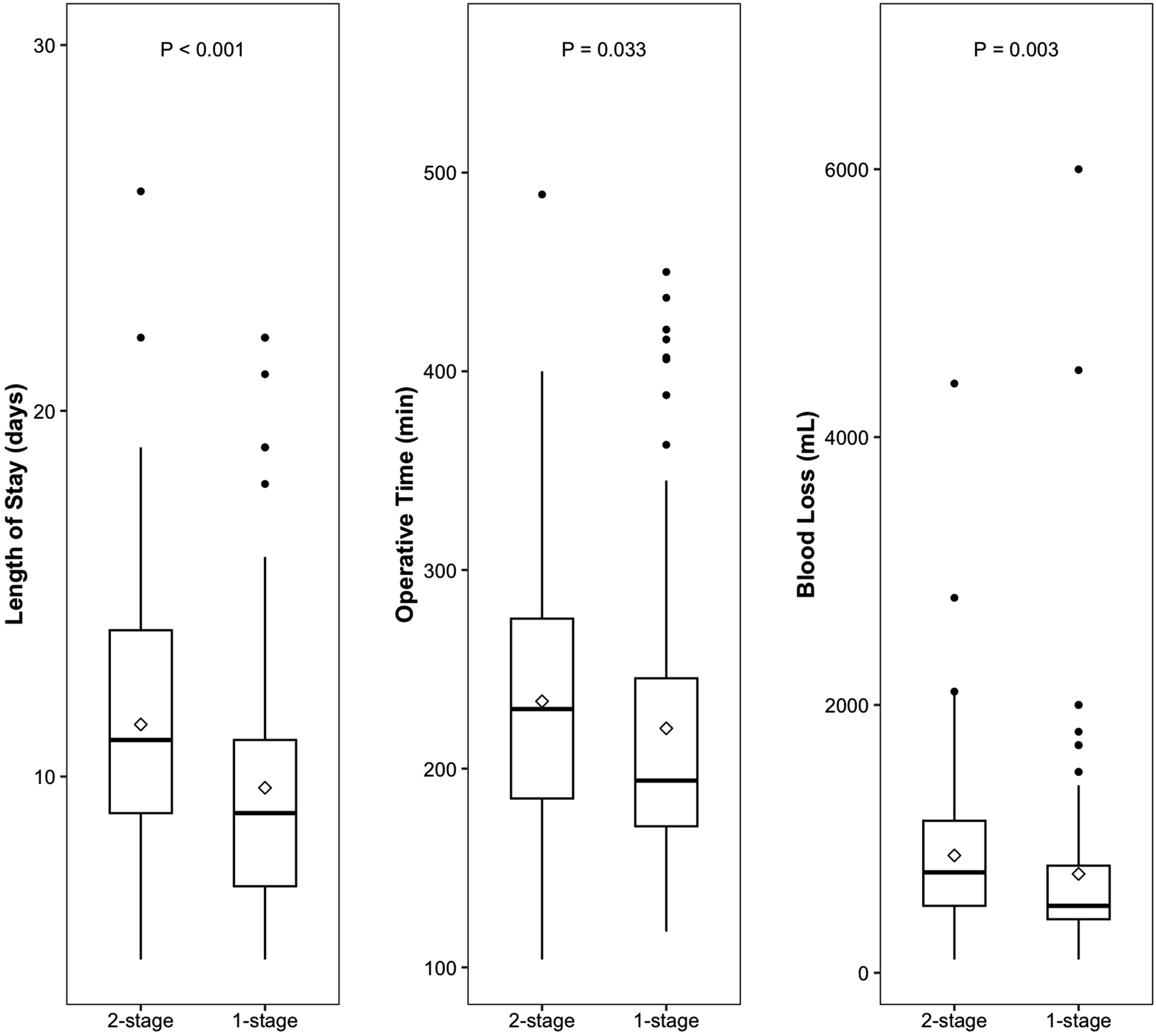
Main Outcomes (1-Stage Versus 2-Stage Group)
Stratified Analyses
Decompression vs Non-Decompression
Among patients who underwent decompression, the two-stage group showed a median operative time of 248 minutes (IQR 90.8) vs 198 minutes (IQR 49.5) in the single-stage group (P = 0.004). Blood loss in decompression cases was higher in the two-stage group (median 900 mL, IQR 600) than in the single-stage group (median 540 mL, IQR 350; P = 0.004). Hospital length of stay showed a trend toward longer stays in the two-stage group (median 12 days, IQR 6) compared to the single-stage group (median 9.5 days, IQR 3.25), though this did not reach statistical significance (P = 0.076). For non-decompression procedures, while operative time and blood loss showed no significant differences between both groups, hospital length of stay was significantly longer in the two-stage group (median 10 days, IQR 3.5) than the single-stage group (median 9 days, IQR 4; P = 0.029).
Neurological Deficit vs No Deficit
Among patients with neurological deficits, the two-stage group demonstrated higher blood loss (median 900 mL, IQR 750) compared to the single-stage group (median 475 mL, IQR 125; P = 0.004). Operative time in patients with neurological deficit did not differ significantly (P = 0.216), nor did hospital length of stay (P = 0.688). Among patients without deficit, hospital length of stay was significantly longer in the two-stage group (median 11 days, IQR 4.25) than in the single-stage group (median 9 days, IQR 3.25; P < 0.001), while no significant differences were observed regarding operative time or blood loss (both P > 0.05).
AO Classification
When subdivided by AO classification, median operative time did not differ significantly between the two-stage and the single-stage group in any fracture subtype (all P > 0.05). For type A fractures, the two-stage group had higher blood loss (median 650 mL, IQR 605) compared to the single-stage group (median 500 mL, IQR 400; P = 0.050) and significantly longer hospital length of stay (median 11 days, IQR 4.75 vs median 9 days, IQR 4; P < 0.001). Type B fractures showed a trend toward longer hospital length of stay in the two-stage group (median 10.5 days, IQR 3) vs the single-stage group (median 9 days, IQR 2), though this did not reach statistical significance (P = 0.089). Type C fractures showed no significant differences in any measured outcomes.
Pooled Analysis
Clinical Outcomes by Pooled Patient Subgroups
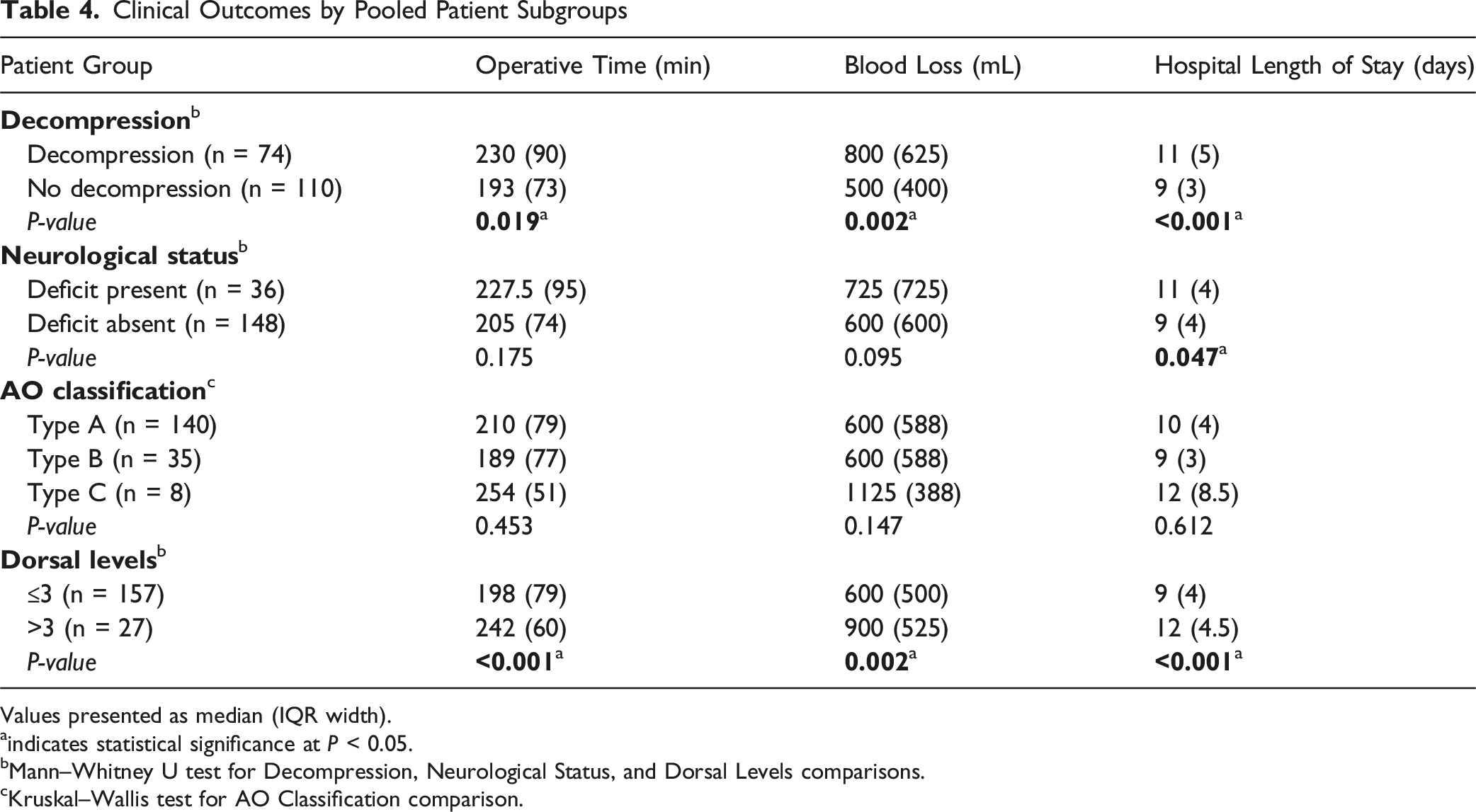
Values presented as median (IQR width).
aindicates statistical significance at P < 0.05.
bMann–Whitney U test for Decompression, Neurological Status, and Dorsal Levels comparisons.
cKruskal–Wallis test for AO Classification comparison.
Discussion
In this retrospective, quasi-experimental bi-centric analysis of 184 patients with unstable thoracolumbar fractures, we observed that a single-stage 360° stabilization significantly shortened hospital length of stay, showed shorter total operative time, and reduced blood loss compared with a two-stage procedure. These advantages persisted even after stratification for decompression procedures and neurological deficits, highlighting the robustness of the findings despite inherent group differences. Notably, in-hospital mortality was absent in both groups. Although patients in the two-stage group presented with more neurological deficits, which may have skewed their surgical risk profile, the overall findings favor a single-stage surgical strategy in appropriately selected patients. To our knowledge, this is the first study directly comparing single-vs two-stage approaches for 360° stabilization in thoracolumbar trauma.
The choice of surgical approach is influenced by the severity and type of fracture. For instance, fractures with significant vertebral body loss may necessitate a 360° stabilization to achieve adequate stability and alignment. 9 Although there is a significant worldwide variation in the treatment of spinal injuries, 360° stabilization remains a common choice for many surgeons. 10 There is evidence from studies that a combined anterior-posterior approach results in a longer total operative time, higher estimated blood loss and a longer hospital stay for the patient than a sole posterior approach. 11 However, the combined 360° anterior-posterior approach has the presumed advantages of allowing short-segment posterior stabilization, better correction of kyphotic deformity, and direct removal of fracture fragments for decompression of the canal. 11
While many studies compare posterior, anterior, and combined procedures, they rarely mention whether they performed single- or two-stage procedures. 12 In this study we found 3 clear advantages of single-stage 360° stabilization: significant shorter hospital length of stay, shorter total operative time, and reduced blood loss.
Hospital Length of Stay: Shorter with Single-Stage
The difference in hospital length of stay between the 2 groups was relatively small, with a median of 9 days in the single-stage group compared to 11 days in the two-stage group. Nevertheless, this finding is clinically relevant, as prolonged hospital stays can increase healthcare costs, delay rehabilitation, and thus contribute to dramatically higher indirect costs due to delayed return to work.13,14 In comparison, most prior studies on combined anterior–posterior stabilization have reported substantially longer hospital length of stay, ranging from 12 days 15 to 22 days, 16 with even higher values of up to 27 days. 17 Older reports similarly found hospital length of stay between 14 and 31 days, underscoring that our observed median stay of 9-11 days is comparatively short.3,4,18 The interval between the 2 surgeries in the two-stage center was primarily influenced by operative capacity. Interestingly, the additional 4 days between surgeries in the two-stage group did not fully account for the overall difference, suggesting the influence of further confounding factors. Notably, the two-stage cohort included more neurologically impaired patients (35% vs 7%) and a higher proportion requiring decompression (68% vs 19%). Neurological deficits may necessitate longer hospitalization, and decompression procedures, requiring open exposure and larger wounds, may also prolong recovery. To address this potentially confounding factor, we performed subgroup analyses and multiple testing. Among patients with neurological deficits, hospital length of stay was similar for both strategies (11 days), suggesting that surgical staging alone did not drive hospital length of stay in this subgroup. In contrast, for patients without deficits, hospital length of stay was significantly longer in the two-stage group (2 days longer). A similar pattern was observed in decompression vs non-decompression cases, where the single-stage procedure was consistently associated with shorter stays, despite the fact that all single-stage cases were performed with open instrumentation rather than percutaneous stabilization. This indicates that larger wounds and muscle dissection may not translate into prolonged hospital length of stay.
Blood Loss and Surgical Time: Favoring Single-Stage
Blood loss and operative time are crucial factors to consider when evaluating surgical outcomes, as they directly impact both patient recovery and the risk of perioperative complications. For instance, Purvis et al demonstrated that every 10% decrease in hemoglobin is associated with a 27% higher risk of perioperative complications and nearly double the risk of hospital-acquired infections. 19 Similarly, prolonged operative times are linked to increased infection rates, thromboembolic complications, and overall costs. 20 In our cohort, the single-stage procedure was associated with clear advantages: median blood loss was reduced by 250 mL and median operative time was shorter by 35 minutes. Reported blood loss for combined anterior–posterior stabilization varies widely across the literature, ranging from relatively low values of 645-748 mL in recent single-stage series15,21 to over 1300 mL in older cohorts 22 and even 2500 mL. 16 Our subgroup analyses highlighted the importance of decompression as a driver of blood loss and operative duration. In the single-stage group, decompression did not significantly increase blood loss compared with non-decompression cases, whereas in the two-stage group decompression was associated with approximately 400 mL greater blood loss. Independent of fracture type, the two-stage strategy consistently resulted in higher blood loss. This may relate not only to surgical exposure but also to perioperative coagulation changes: prior studies have shown that clotting factors II, X, XI, and XII can remain significantly reduced until postoperative day 3, potentially amplifying blood loss when surgeries are staged closely together. 23
Similar patterns were observed for surgical time. In the two-stage group, decompression prolonged surgery by roughly 1 hour, whereas in non-decompression cases the posterior stabilization was performed percutaneous. No such difference was seen in the single-stage group, in which posterior procedure always was performed open. This suggests that staging amplifies the additional burden of decompression, whereas the single-stage strategy mitigates its impact. Blood loss and operative time are often interdependent, and although surgeon experience may also play a role, it was not captured in our dataset. Taken together, our findings suggest that the benefits of the single-stage approach are particularly relevant in patients requiring decompression, while outcomes in non-decompression cases appear similar between strategies.
Study Strengths and Limitations
A potential limitation of our study is its retrospective design, which may introduce bias related to randomization and comparability. However, our research design utilized pre-existing patient groups based on the specific treatments administered at different centers. Importantly, relevant demographic baseline characteristics were similar in both groups. While this approach reflects real-world conditions, the quasi-experimental design enhances the study’s external validity. 24
Nevertheless, by restricting our analysis to acute fractures in non-polytraumatized adults (ISS ≤15), we minimized confounding from major systemic injuries. However, this restriction also means that our findings may not be generalizable to patients with more complex polytrauma.
Although both centers were located within the same country, differences in discharge policies, access to rehabilitation, and perioperative workflows may have influenced outcomes. Peri- and postoperative complications were not analyzed in detail due to inconsistent severity reporting across the 2 centers.
Future prospective trials with standardized complication reporting, long-term follow-up, and cost analysis are needed to determine whether these perioperative benefits translate into sustained patient and health-system advantages.
Conclusion
Our study suggests that a single-stage 360° stabilization contributes to the reduction of hospital length of stay. In addition, a single-stage approach leads to reduced operative time, and minimizes blood loss relative to a two-stage approach in selected patients. The single-stage procedure might be especially beneficial for patients who need decompression. These findings highlight the preference for a single-stage approach whenever feasible, depending on capacity and set-up.
Footnotes
Ethical Considerations
The review and approval by the regional ethics committee (KEK – Kantonale Ethikkommission Bern, ID: 2021-02021) have been successfully completed.
Consent to Participate
All participants provided written informed consent prior to inclusion in the study.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data supporting the findings of this study are available from the corresponding author upon reasonable request.
