Abstract
Study Design
Systematic review.
Objectives
The pre-symptomatic state of Degenerative Cervical Myelopathy (DCM), wherein degenerative changes and spinal cord compression are seen without clinical findings, is poorly understood and inconsistently categorised. Clear identification may elucidate the temporality of DCM development. Therefore, a systematic assessment was undertaken of current terminology for pre-DCM states, with the objective of standardising definitions and informing an AO Spine expert position statement.
Methods
Medline and Embase were searched for all studies on asymptomatic spinal compression or clinical findings preceding DCM, returning 3585 studies. After screening, 96 studies were included in the final analysis. The terminology used for pre-DCM states and their definitions were extracted, along with their frequencies or speciality/country of author in the literature.
Results
Multiple terms were used to represent pre-DCM stages, including “
Conclusion
There is substantial inconsistency in the terms used to describe pre-DCM states. There is no clear relationship between the terms used and the country or speciality of the main author. Standardised definitions for these disease states should be agreed and used in future studies.
Keywords
Introduction
Degenerative Cervical Myelopathy (DCM) is a degenerative condition of symptomatic spinal cord compression. It is an umbrella term introduced by Nouri et al. that encompasses various degenerative spinal pathologies such as cervical spondylotic myelopathy (CSM), degenerative disc disease (DDD), ossification of the posterior longitudinal ligament (OPLL) and ossification of ligamentum flavum (OLF). These conditions are highly interrelated and often manifest concomitantly. DCM is a clinical diagnosis that relies on patient’s symptoms and clinical signs such as upper limb numbness/paraesthesia, loss of manual dexterity, gait abnormalities, hyperreflexia and Hoffman sign to be present alongside radiological evidence of spinal cord compression.1-3
Patients are assessed and stratified using the modified Japanese Orthopaedic Association scale (mJOA), which produces a score dependent on the extent of motor and sensory dysfunction in the upper and lower limbs as well as bladder sphincter dysfunction.3,4 The AO Spine clinical guidelines recommend surgical intervention for patients with moderate to severe or progressive DCM, 5 based on a series of relatively recent papers that provide clear supporting evidence. 6 For patients with mild DCM, there is a lack of high-quality research that limits the strength of recommendation, with either a trial of non-operative management or surgical intervention proposed. 5 These guidelines do not recommend prophylactic surgical treatment of patients with spinal cord compression without signs or symptoms of myelopathy and radiculopathy.
The understanding of the pathogenesis of DCM and its progression from neurologically intact to a myelopathic condition is poorly understood. This may be because from a radiological perspective, various changes can represent pre-DCM pathologies: OPLL or OLF without cord compression and cord compression with or without cord signal change but without clinical myelopathic symptoms.1,2 From a clinical perspective, individuals may present with cervical radiculopathy or upper motor neurone signs such as Hoffman sign or hyperreflexia. The numerous clinical and radiographic findings have resulted in various terminologies that categorize the same population – individuals at risk of eventually developing DCM.
Multiple studies have been conducted on these patients and have demonstrated a significant prevalence of pre-DCM degenerative spinal pathology. Nakashima et al. recruited 1211 healthy neurologically intact volunteers consisting of 100 men and 100 women from each decade between 20 to 70 years. They found a prevalence of 5.3% for spinal cord compression (SCC) and 2.3% for increased signal intensity on MRI 7 . In a meta-analysis of MRI reports, Smith et al found the prevalence of spinal cord compression to be 24.2% in healthy volunteers. Additionally, they found the prevalence of DCM to be 2.3% within a subgroup of the healthy cohort. 8 Martin et al. used objective spinal cord morphology metrics and found that spinal cord deformation (flatting, indentation, torsion, or circumferential compression) occurred in 50% of healthy subjects, increasing linearly with age. 9
However, studies addressing pre-DCM pathology demonstrate inconsistency in descriptive terminology, including in the use of “
The objective of this systematic review was therefore to synthesise the current terminology and definitions used in the literature for pre-DCM pathologies with the aim of forming the basis for an AO Spine expert position statement on standardised definitions for this clinical entity.
Methods
Study Design
A systematic review was conducted with reference to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020 checklists (Online Appendix C).11,12 The protocol was registered on PROSPERO (ID: CRD42022307883).
Eligibility Criteria
Inclusion Criteria
• Human study • Adult (>18 years old) • English language • Full-text available • Primary research paper, review or opinion article • Discussion of pre-symptomatic or early stage of any degenerative cervical spinal pathology or condition within the DCM umbrella • Published in the last 12 years (2012-2024)
Exclusion Criteria
• Animal studies • Cadaveric studies • Case reports • Conference abstracts
Information Sources
MEDLINE and Embase were searched using the Ovid Platform from inception to October 2024.
Search Strategy
Scoping searches were performed to refine the review question. Final search strategies (Online Appendix A) were developed and piloted using an iterative process. The search included multiple possible terms used to describe pre-DCM, as well as subject headings to maximise search sensitivity. During the preliminary research stage, 10 studies were identified as significantly relevant to the study (Online Appendix B). These were used to test the search strategy sensitivity by ensuring all 10 studies were captured by the final search. Only studies published in the last 12 years were included to ensure focus on the most contemporaneous terminology.
Selection Process
Search results were exported and deduplicated using EndNote (Version 20.3.0.17787, Clarivate, London, United Kingdom). 13 Title and abstract screening was completed using Rayyan (Rayyan Systems Inc, Cambridge, MA, United States). All records were screened in duplicate by two blinded reviewers; a pilot of 100 records was screened by all reviewers to ensure concordance. Full-text screening was completed in duplicate.
Data Collection
Manual data extraction from the 96 studies that passed screening was completed in duplicate in Microsoft Excel 2016 (Version 2311, Microsoft 365).
Data Items
Data was independently extracted on the various terminology used and their definitions. Where clinical studies were included, further information was sought regarding their methodology. Specifically, this included the study design, recruitment process, inclusion and exclusion criteria, patient demographics (age, gender, ethnicity), mode of imaging and the overall conclusion.
Risk of Bias Assessment
The quality and bias of included studies were assessed using appropriate Joanna Briggs Institute (JBI) critical appraisal tools depending on the type of literature: systematic review, cohort studies, cross-sectional studies and case-control studies. For review articles, the Scale for the Assessment of Narrative Review Articles (SANRA) was used, with which a score was given for each of its six criteria. To make the data comparable across different appraisal tools, an overall score was given (as a percentage) based on the specific criteria fulfilled by each study. Two authors assessed the quality and bias of these studies independently.
Synthesis Methods
The frequency of different terminology in the literature was calculated using Microsoft Excel and the respective definitions for each of the terms were analysed. As the data was entirely qualitative, the scope for conducting extensive statistical analyses was limited.
Results
A total of 3585 records were identified by the search. Following removal of duplicates, 2566 records were screened against eligibility criteria. A total of 179 were sought for retrieval; 15 of these studies were not retrieved due to unavailability of full texts or because they were non-English language. During full text screening, 52 further studies were excluded as they did not focus on the early stages of DCM,1,14-17 and 16 further studies were excluded for being conference abstracts. A total of 96 studies were included in the final review (Figure 1; Online Appendix D). Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) flow diagram of study selection.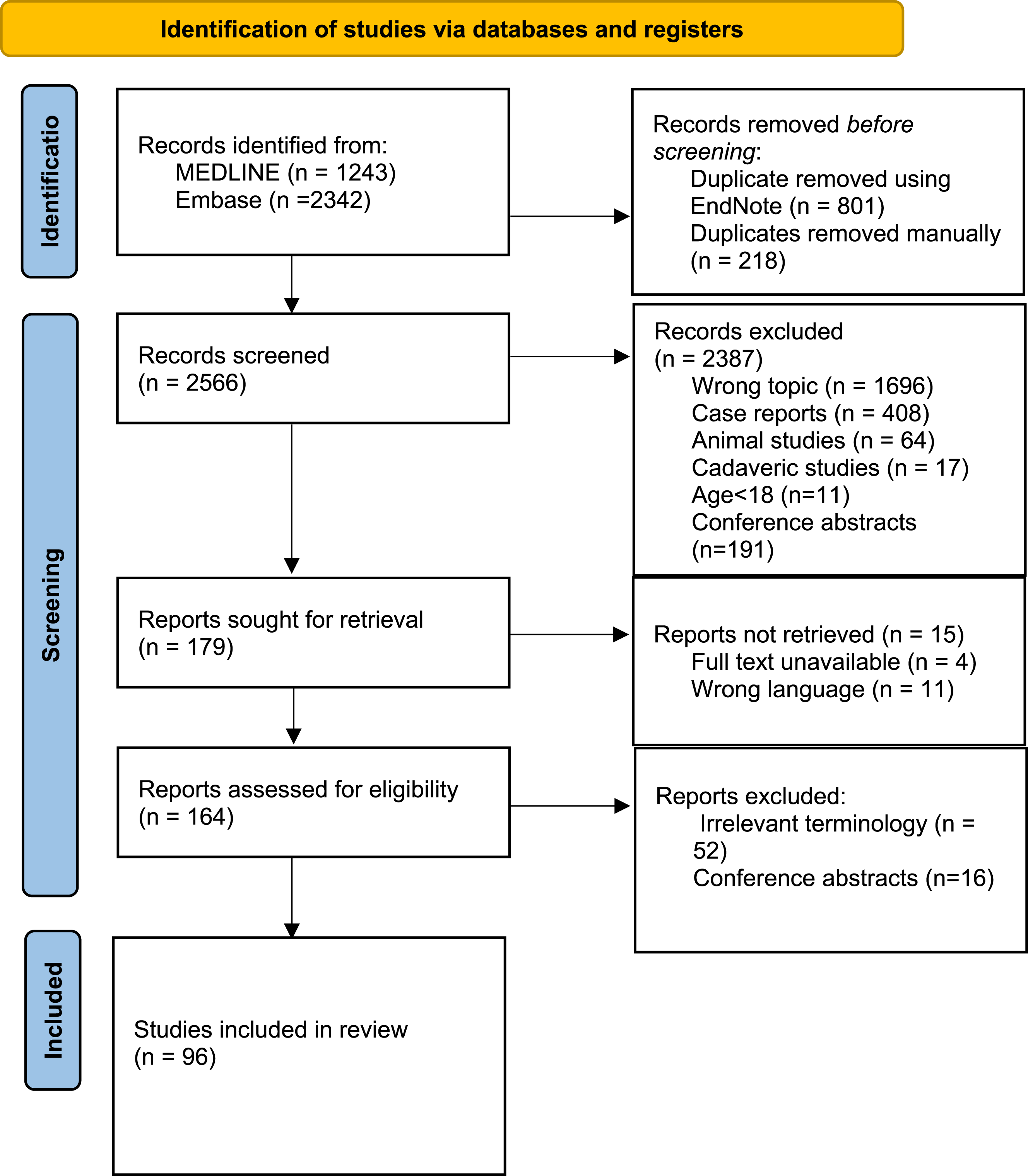
Summary of the Terms Used to Describe Pre-DCM States.

Further Analysis of the Use of the Term Asymptomatic.

Breakdown of the Use of the Term Non-myelopathic.
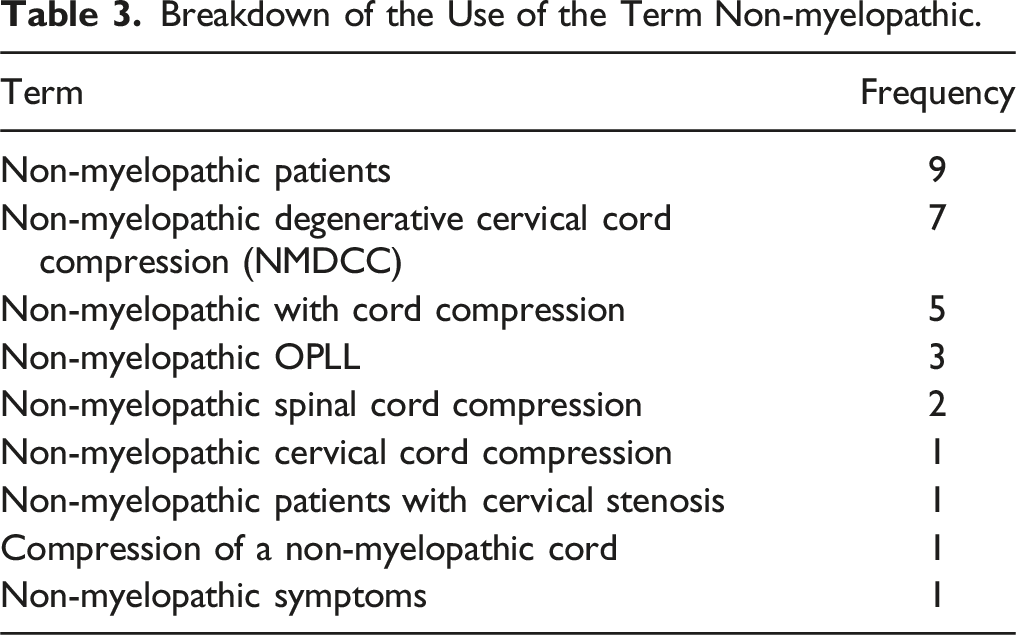
There were no obvious temporal trends in use of terminology during the period studied (Figure 2). The frequency of use of The frequency of different terms used to describe pre-DCM states from 2012-2024.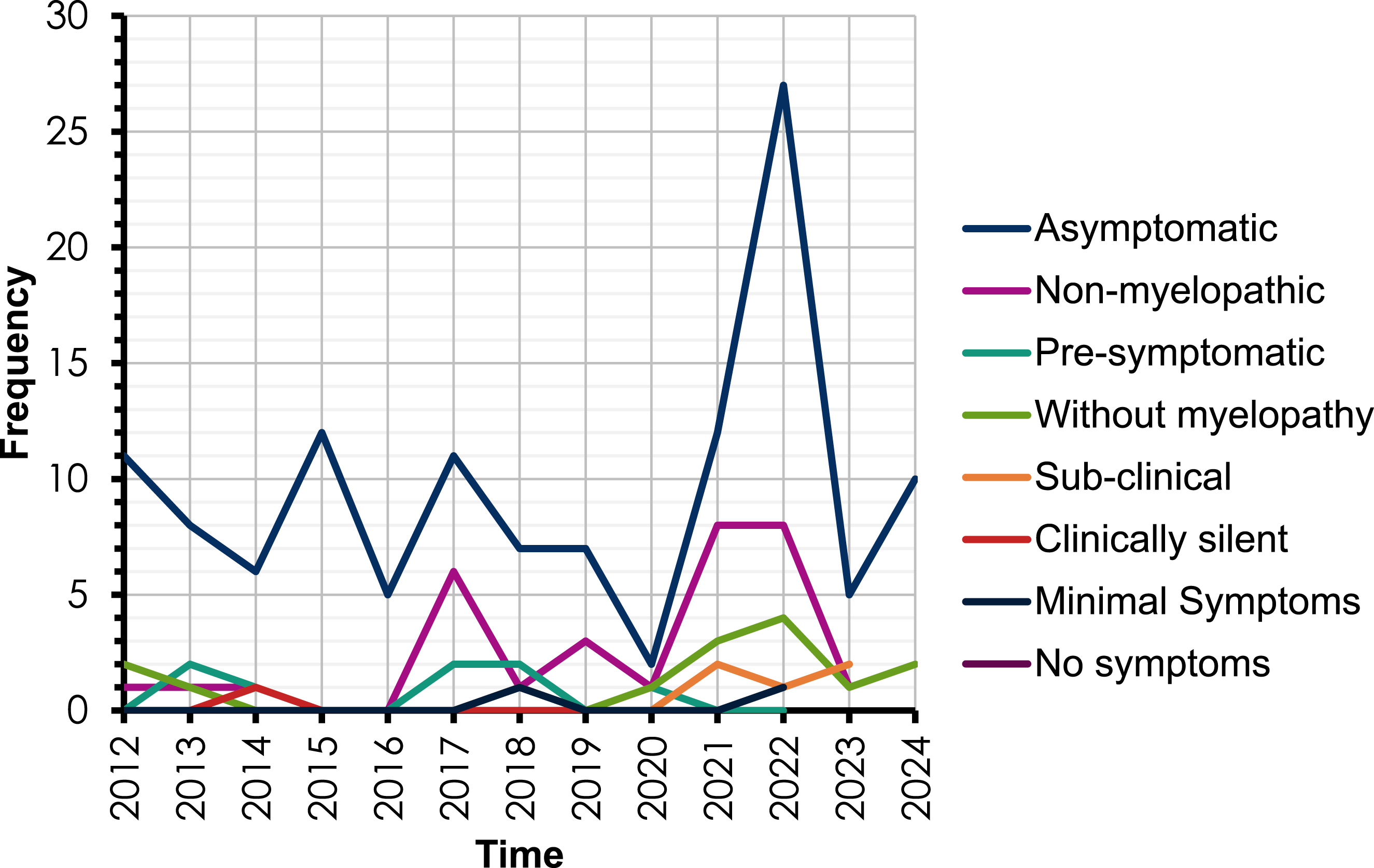
Assessment of pre-DCM terminology geographical variation showed that the United States and Canada produced the greatest volume of literature on the subject. The term The absolute frequency of different terms used to describe pre-DCM states in different countries.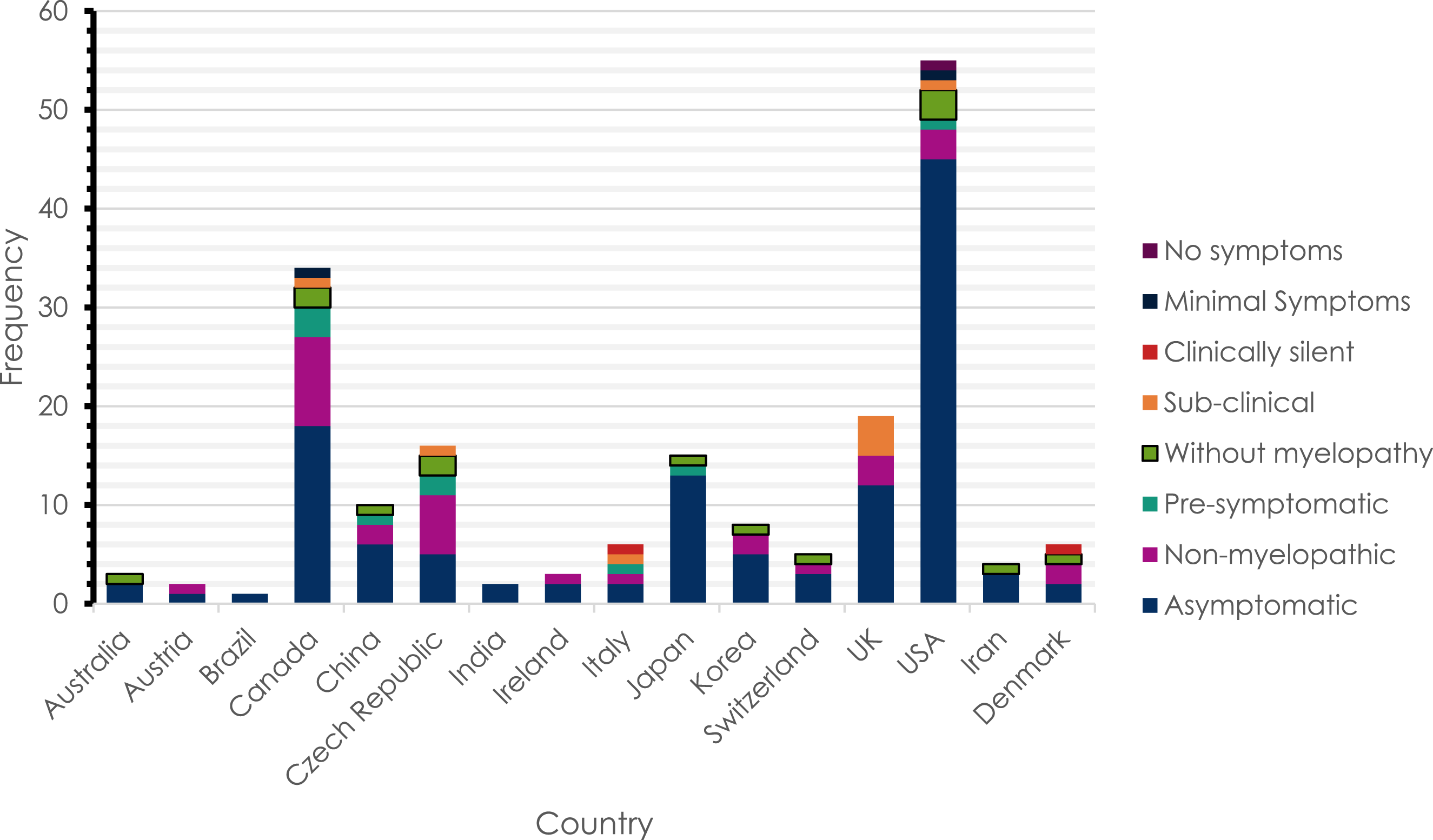
The included literature was found to be written by authors who were primarily from a neurosurgical or orthopaedic background. A broader range of terms were used by neurosurgeons than orthopaedic surgeons (Figure 4). The relative frequency of different terms used to describe pre-DCM states by different specialities. Total numbers of papers from each specialty included in brackets after specialty name.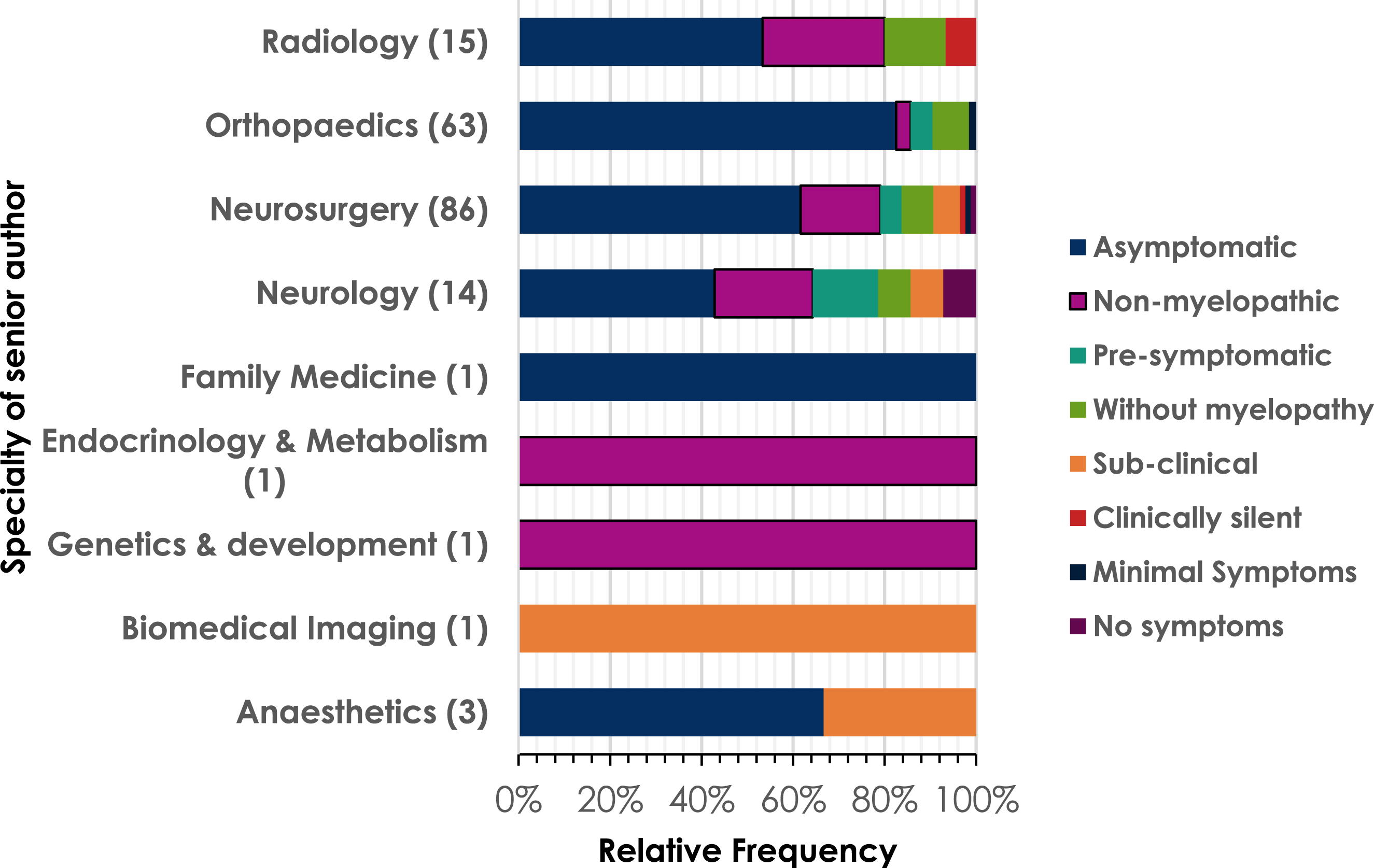
Most studies were high quality with low bias (Figure 5). Studies in the medium risk category were still included in this study because regardless of their quality, the terminology used was still relevant. Frequency table of the quality and bias assessment scores for the studies included in data extraction.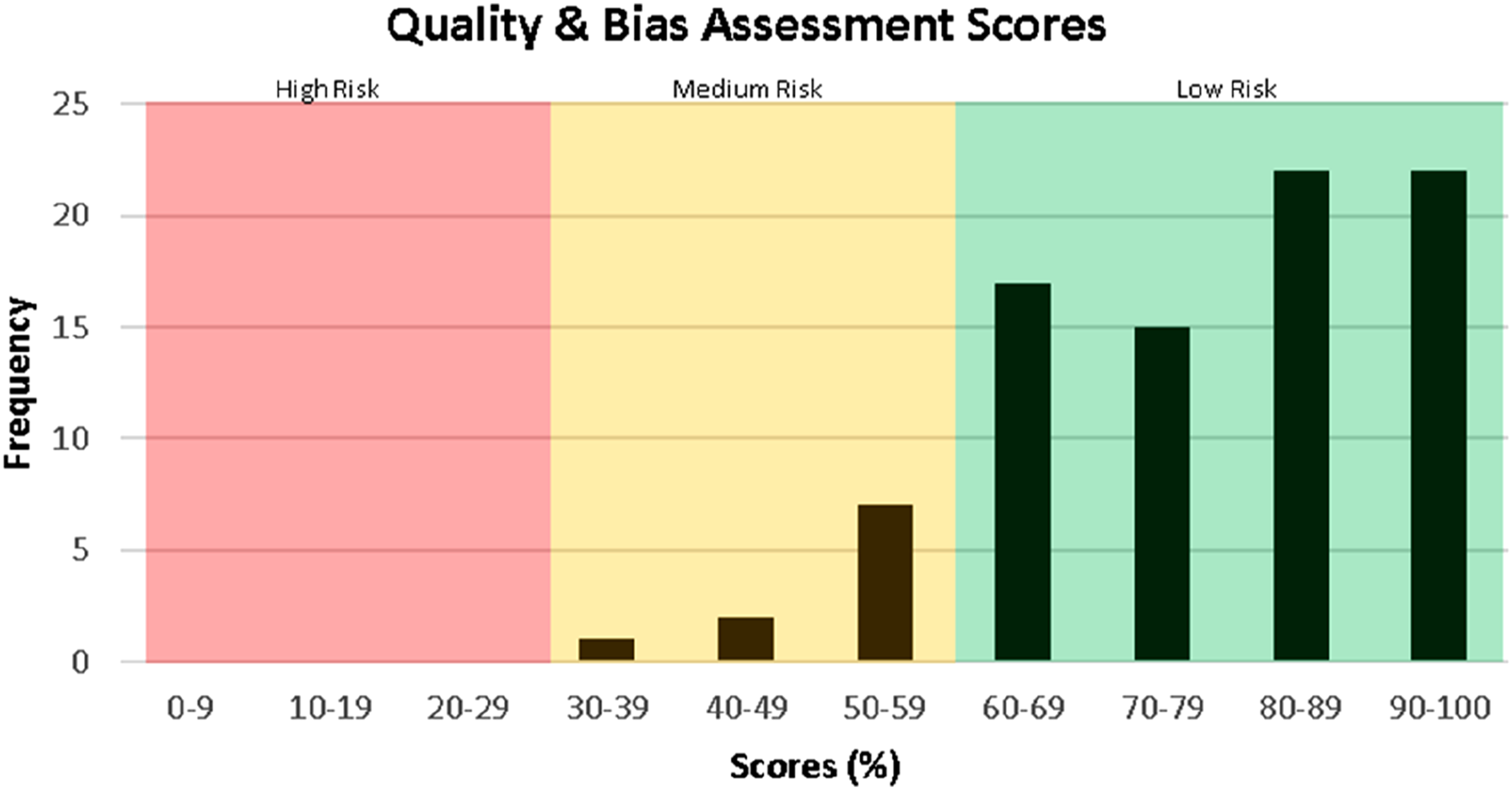
Discussion
Whilst the conditions encompassed by DCM have been the subject of considerable study, there is significantly less literature addressing the stages preceding DCM. Thus far, research on the terminology used to describe these stages has not been conducted. The discussion that does exist around the semantics of the field is brief, and is usually included at the end of papers, with clear definitions of terminology uncommon. The aim of this review was therefore to synthesise the definitions used and identify the inconsistencies in the literature.
The most used term to describe a pre-DCM state was
The second use of
Another term used with variability in the literature was
While there were studies that used the terms
Additional terms that have been used to describe patients in the stage preceding DCM are presented in Table 1. An example is the term
It is possible that the inconsistency found between authors describing pre-DCM states stems from the uncertainty in the meaning of
Moreover, there is variability in patients’ presentations in the pre-DCM state and this influences the terms used to describe these stages. Many clinical studies investigating conditions preceding DCM had different inclusion and exclusion criteria making it difficult to reproduce or compare their findings. For example, in a prospective cohort study of 115 patients with non-myelopathic cervical OPLL, 23 had an absence of symptoms, 44 had axial neck pain, 40 had radiculopathy and eight had tingling sensation of the fingers. 29 In contrast, a retrospective cohort study by Shen et al, 2021, excluded patients from their non-myelopathic group if they had neurological deficits, symptoms of radiculopathy, cervical axial pain, previous spinal surgery, or a diagnosis of either spondylolisthesis or scoliosis. 42 Furthermore, healthy subjects and individuals with DCM frequently report intermittent symptoms (eg, numbness), and most studies do not address how this finding is reported or categorized. Some studies also reported abnormalities in electrophysiological testing in asymptomatic individuals, thus adding to this diversity in pre-DCM conditions.38,43 Nouri et al. argue that both the variations in the diagnostic criteria and differences between ethnic populations may explain the heterogeneity in the prevalence rates of “non-myelopathic spinal cord compression”. 26
Future Directions
The RECODE-DCM Natural History Incubator is leading an AO Spine terminology consensus statement. These standardised definitions will allow better characterisation of the pathology preceding DCM, facilitate more efficient stratification of this large group of patients and promote optimal clinical management and research efficiency. A recent cross-sectional observational study, involving a web-based survey targeted towards surgeons and other health care professionals involved with DCM patients, investigated definitions of DCM and standard practice in DCM management. 44 They found no consensus on the definitions and management of pre- or mild DCM and deficient follow-up assessments. Brannigan et al, 2024 discuss that inconsistent use of diagnostic terms can give rise to ambiguity when exploring diagnoses and interventions for patients. It is important to note that these results were found despite some authors having offered an approach to the management of patients in the pre-DCM stage, such as Fehlings et al, 2017. They suggest counselling these patients about the risks of progression, educating them about the signs and symptoms of myelopathy and ensuring clinical follow-up. 5 For patients with additional symptoms of radiculopathy, they suggest informing them of the increased risk of myelopathy development and offering either surgical intervention, close regular follow-up or a trial of structured rehabilitation. The strength of these recommendations was weak due to being based on limited evidence, thus further highlighting the need for more research in this field with consistent terminology.
Limitations
Limitations of this study include pre-DCM terminology not being clearly defined by many authors and so the meaning of the terms had to be inferred by the context, the study design and the inclusion and exclusion criteria. This was negated somewhat in our methodology by having two independent authors reviewing the literature. Limitations also arose due to the exclusion of non-English literature. This resulted in a lack of data of equivalent terms in other countries, which may have affected the results shown in Figure 3. Finally, this research is limited in that we can only form conclusions about the variable usage of terms describing pre-DCM states in the academic literature and do not specifically capture descriptors employed in clinical practice.
Conclusion
There are many terms in the literature used to describe conditions preceding DCM, with the most common being
Supplemental Material
Supplemental Material - A Systematic Review of Current Terminology for Conditions Preceding Degenerative Cervical Myelopathy: Evidence Synthesis to Inform an AO Spine Expert Opinion Statement
Supplemental Material for A Systematic Review of Current Terminology for Conditions Preceding Degenerative Cervical Myelopathy: Evidence Synthesis to Inform an AO Spine Expert Opinion Statement by Vinisha Agrawal, Mohammed Farhan Ali, Froher Yasin, Daniyal Ashraf, Jamie FM Brannigan, Ratko Yurac, MD, Vishal Kumar, Rory Murphy, Enrico Tessitore, Granit Molliqaj, Joost Dejaegher, Juan José Zamorano, Guy Wynne-Jones, Manjul Tripathi, David B Anderson, Jose Joefrey F Arbatin, So Kato, Ronie Romelean Jayapalan, Nicolas Dea, James S. Harrop, Jefferson Wilson, Brian K. Kwon, Allan R. Martin, Josef Bednarik, Mark R Kotter, Benjamin M Davies, Oliver D Mowforth, and Aria Nouri in Global Spine Journal.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research aligns with the AO Spine RECODE-DCM top research priority
Disclaimer
The views expressed in this publication are those of the authors and not necessarily those of the NHS, the National Institute for Health Research or the Department of Health.
ORCID iDs
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
