Abstract
Study Design
Retrospective Cohort.
Objective
This study aims to assess the easily measurable radiographic landmarks of screw-to-vertebral body ratio and changes in screw angle to identify if they are associated with early subsidence following an Anterior cervical discectomy and fusion (ACDF).
Methods
A retrospective cohort study was conducted on patients undergoing 1-3 level ACDF with allograft or PEEK cages. Preoperative, immediate postoperative, and 6-month postoperative radiographs were analyzed to measure intradiscal height (or distance between 2 vertebral bodies) as an anterior vertebral distance (AVD), middle (MVD), and posterior (PVD), screw angle, screw-to-vertebral body length ratio, and interscrew distance. Multivariate stepwise regression analyses were performed.
Results
92 patients were included (42 single-level, 32 two-level, and 18 3-level ACDFs). In single-level ACDFs, a decrease in the caudal screw angle was associated with a decrease in AVD (=.001) and MVD (P = .03). A decrease in the PVD was associated with a decrease in segmental lordosis (P < .001). For two-level ACDFs, a higher caudal screw-to-body ratio was associated with a lower MVD (P = .01).
Conclusion
Six months following an ACDF for degenerative pathology, a decrease in the caudal screw angle was associated with an increase in radiographic subsidence at the antero-medial aspect of the disc space albeit largely subclinical. This suggests that the caudal screw angle change may serve as a reliable radiographic marker for early radiographic subsidence. Furthermore, a greater screw-to-vertebral body ratio may be protective against radiographic subsidence in two-level ACDF procedures.
Keywords
Introduction
Anterior cervical discectomy and fusion (ACDF) is a widely utilized surgical procedure for addressing radiculopathy or myelopathy in cases of degenerative cervical disease.1,2 This surgical intervention involves the removal of the intervertebral disc, followed by the placement of autologous and allograft bone, alongside a potential interbody cage to serve as a structural support. These materials play crucial roles in maintaining proper disc height and alignment, as well as widening the neuroforamen, ultimately facilitating successful bony fusion. 3 However, a notable concern with the use of any interbody device/material, regardless of whether it is for single- or multi-level disease, is the potential for subsidence. Subsidence, in this context, refers to the settling or sinking of the cage into the vertebral body. This phenomenon can lead to a reduction in foraminal height and cervical alignment, potentially compromising surgical outcomes.4,5
While subsidence is recognized as a known complication, its long-term impact on surgical outcomes remains unclear due to a limited number of studies on this matter. 6 Notably, various factors have been identified as potential risk factors for subsidence including graft type, location, sagittal alignment, number of levels, length of plate used, and screw angle and bone mineral density.7-9 However, potential radiological identifiers for subsidence especially in the early postoperative period are not discussed in literature. Two critical variables: the change in variable screw angle over time and the screw-to-vertebral body ratio have yet to be evaluated in relation to subsidence. Longer screws have been associated with greater pull-out strength and reduced rates of pseudarthrosis, but the impact of the screw-to-vertebral body ratio on subsidence and changes in screw angles in relation to subsidence remains unexplored. 10 Hence, the objective of this study is to assess the influence of the screw-to-vertebral body ratio and changes in the variable screw angles at both the cephalad and caudal aspects of the construct on subsidence; taking into account both interscrew distance and intradiscal heights. This research aims to provide valuable insights into early identification of subsidence for ACDF procedures.
Methods
Patient Data
Consecutive patients who underwent anterior cervical discectomy and fusion (ACDF) at our center, utilizing either allograft or PEEK cages between January 2018 and June 2021, were included in this study after internal review board approval at Virginia Mason Medical Center (IRB 22-067). Informed consent was deemed exempt. Surgeries were performed by 1 of 3 fellowship trained spine surgeons who perform the discectomy and fusion portion of the procedure with similar techniques and instrumentation. Inclusion criteria encompassed: (1) diagnosis of myelopathy or radiculopathy from a degenerative pathology; (2) discernible spinal cord or root compression evident in recent magnetic resonance imaging, at either single or multiple levels (<3); (3) A minimum of 6 months of radiographic and clinical follow-up. Conversely, exclusion criteria comprised: (1) patients necessitating fixation of more than 3 levels; (2) patients requiring a posterior approach; (3) cervical stenosis in the setting of tumor, trauma, or infection.
Surgical Technique
A transverse incision of approximately 4-6 cm was made on the right side. The Smith-Patterson approach was employed, navigating between tissue planes with medial retraction of the tracheoesophageal complex and lateral retraction of carotid sheath contents. A thorough discectomy with curettes and a high-speed burr that includes uncovertebral decompression were carried out, along with the takedown of the posterior longitudinal ligament. Subsequently, a cage size was chosen and trialed before selecting the appropriate 1. An anterior cervical plate of appropriate size is secured with 2 cranial and caudal vertebral body variable angle screws in each and an intermediate fixed angle screw, in multilevel surgery. Intraoperative x-rays were taken to verify the level, ensure the implant’s size adequacy, and confirm its correct (central) positioning.
The techniques utilized by the 3 surgeons are similar in order of steps, instrumentation, and assessment of interbody cage height. A 3 mm matchstick high-speed pneumatic burr is utilized to remove the posterior vertebral body margin and associated osteophytes. The endplates were not removed for the primary purpose of placing a taller interbody cage. However, the anterior osteophytes were removed with a high-speed burr and the disc space was “rectangularized” in order to place a 7-degree lordotic trapezoidal interbody cage. No distraction pins were placed, thus the interbody cage was press-fit into place with a close examination of lateral fluoroscopy imaging to assess for facet joint distraction that may occur. The height of the interbody cages selected were the tallest height in which did not demonstrate facet joint distraction intraoperatively.
Radiographic Assessment
The plain radiographs were stored and accessed through the Picture Archive and Communication System (PACS) software. The pre-operative, initial post-operative (day 0-1) and 6-month post-operative neutral standing lateral radiographic assessments included: intradiscal height/vertebral distances (anterior [AVD], middle [MVD], and posterior [PVD]), intervertebral screw distance, and the screw-vertebral body ratio for both the cephalad and caudal screws (Figure 1). The intradiscal heights were measured as the distance between the lower endplate of the cephalad vertebral body and the upper endplate of the caudal vertebral endplate at the center of the anterior one-third (“anterior”), middle one-third (“middle”), and posterior one-third (“posterior”) of the disc space. The intervertebral screw distance was the distance between the tips of the screws. If the screw tips within the same vertebral body were not parallel, a “center” of the 2 screw tips was used to perform the measurement. The plain radiographs taken at the 6-month follow-up were utilized to determine the presence of subsidence. All analyses were conducted to predict changes in subsidence measurements (anterior, middle, and posterior intradiscal height, interscrew distance) based on alterations in screw angles (cephalad or caudal), postoperative screw angles, screw-to-vertebral body ratios, and postoperative subsidence measurements. (A) Sagittal x-ray showing cephalad and caudal screw angle measurements for single-level ACDF. (B) Sagittal x-ray showing interscrew distance, screw-to-vertebral body length ratio, and anterior vertebral body distance (AVD), middle vertebral body distance (MVD), and posterior vertebral body distance (PVD) measurements for two-level ACDF.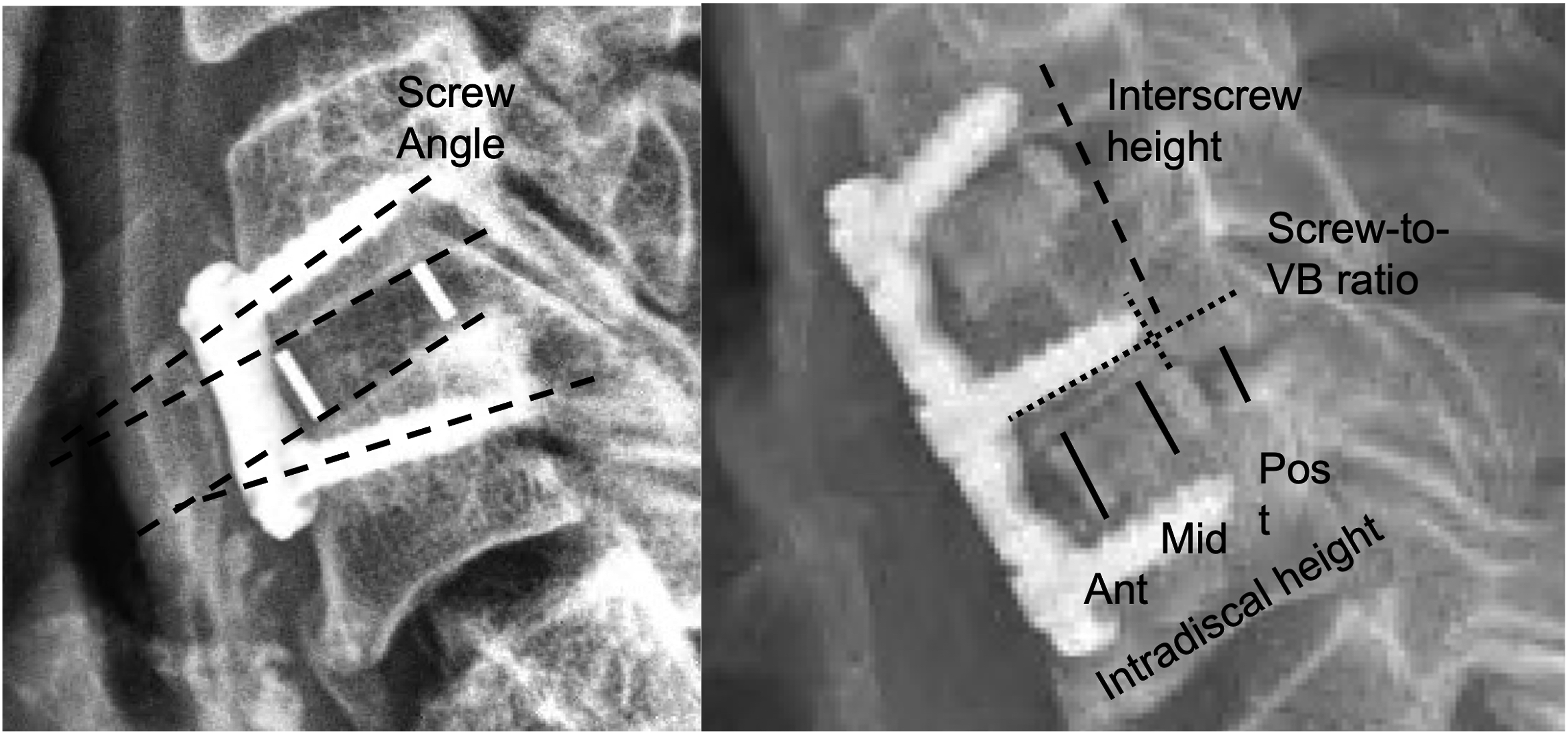
Statistical Analysis
Multivariate stepwise regression assessed the relationship between postoperative changes in AVD, MVD, PVD, and interscrew distance change on screw angle change, C2-C7 sagittal vertical axis (SVA) change, lordosis change at both the fused segment and C2-C7 levels. Linear regression between screw-to-body ratio and subsidence measures was also performed. Wilcoxon rank sum tests compared the change in AVD, MVD, PVD, and Interscrew between graft type (allograft and PEEK) and sex (male and female). Additionally, paired t-tests were performed between immediate postoperative and 6-month for measured parameters.
Results
Patient Demographics.
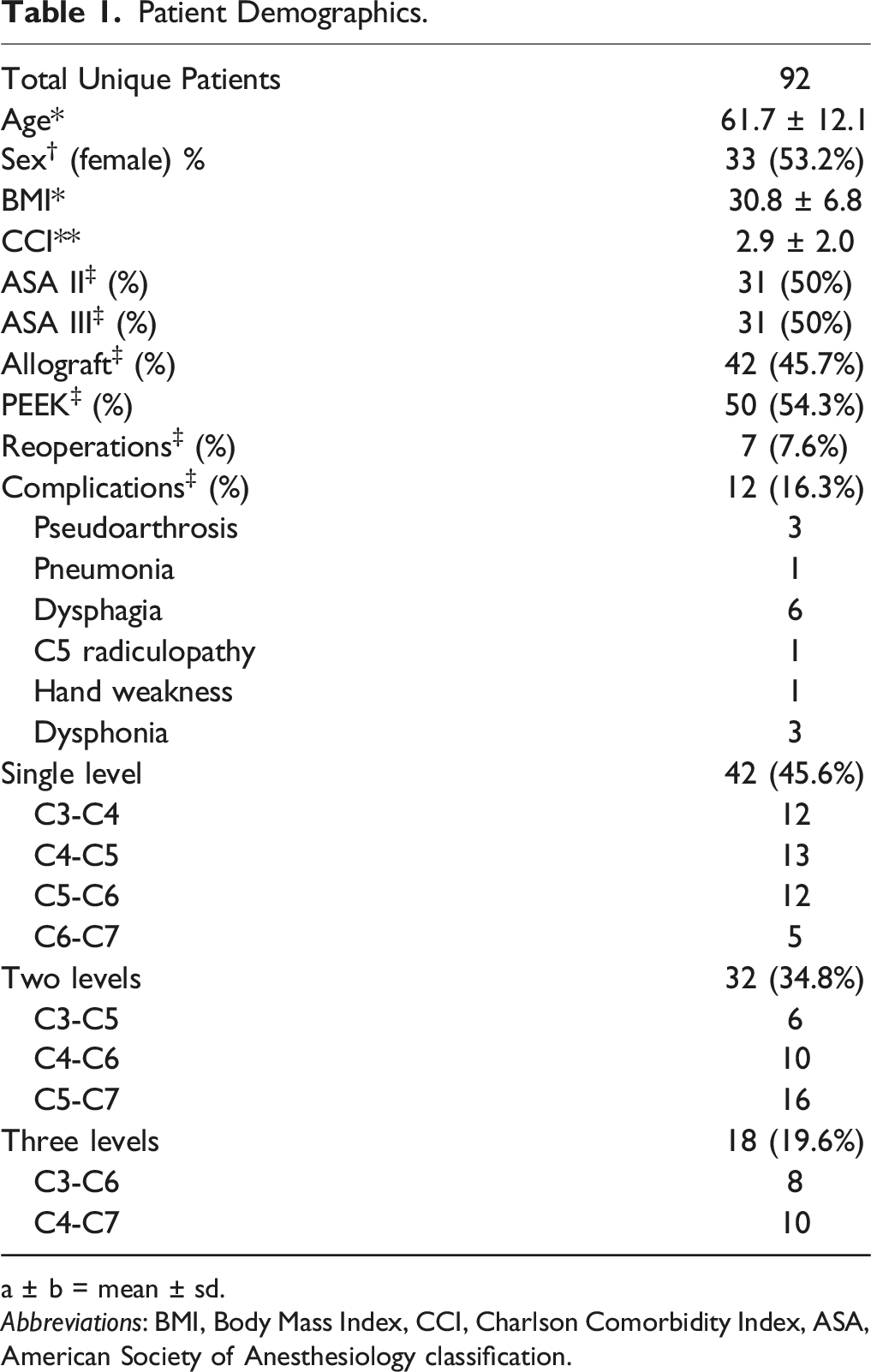
a ± b = mean ± sd.
Abbreviations: BMI, Body Mass Index, CCI, Charlson Comorbidity Index, ASA, American Society of Anesthesiology classification.
Radiographic Measurements.
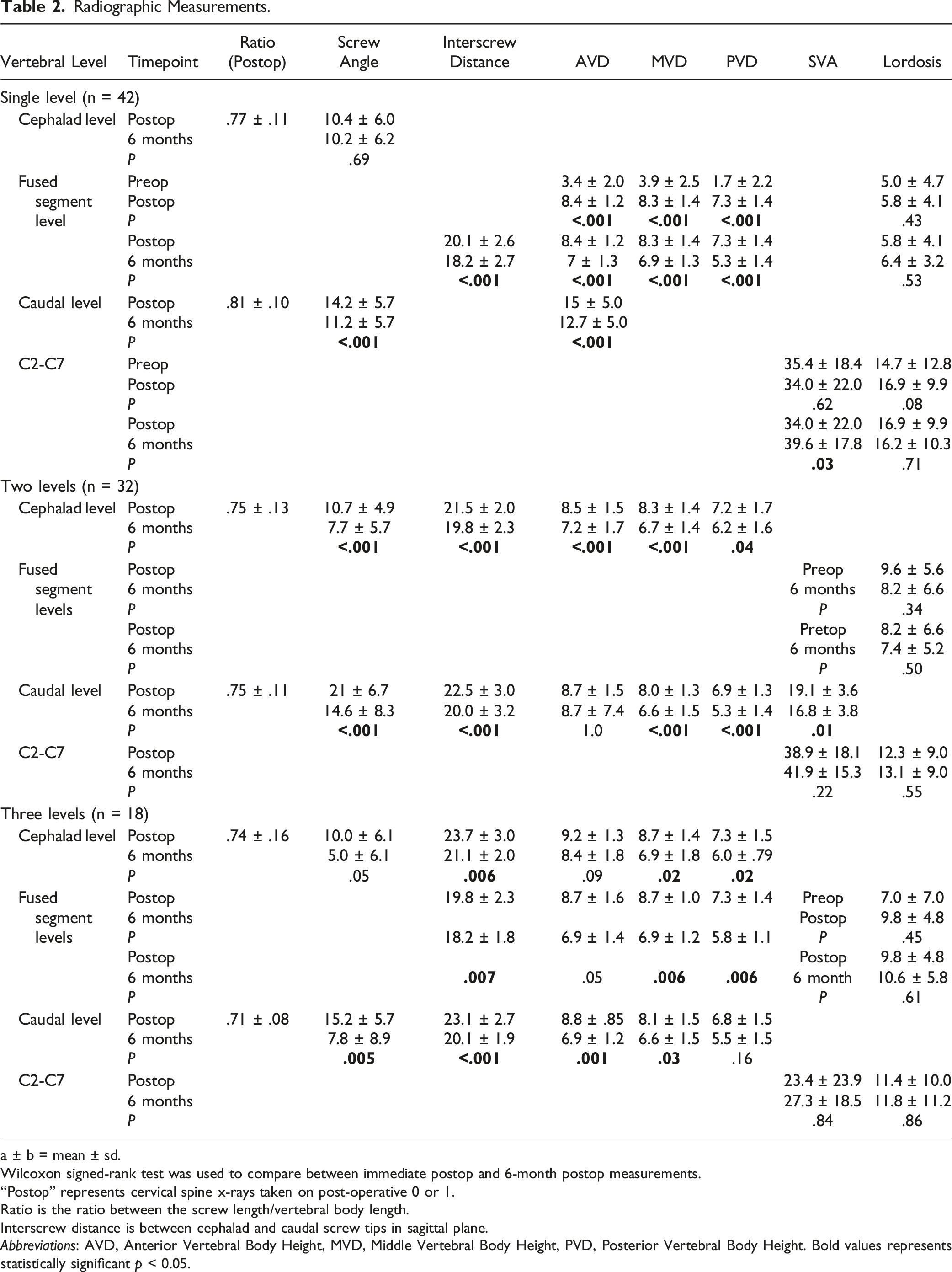
a ± b = mean ± sd.
Wilcoxon signed-rank test was used to compare between immediate postop and 6-month postop measurements.
“Postop” represents cervical spine x-rays taken on post-operative 0 or 1.
Ratio is the ratio between the screw length/vertebral body length.
Interscrew distance is between cephalad and caudal screw tips in sagittal plane.
Abbreviations: AVD, Anterior Vertebral Body Height, MVD, Middle Vertebral Body Height, PVD, Posterior Vertebral Body Height. Bold values represents statistically significant p < 0.05.
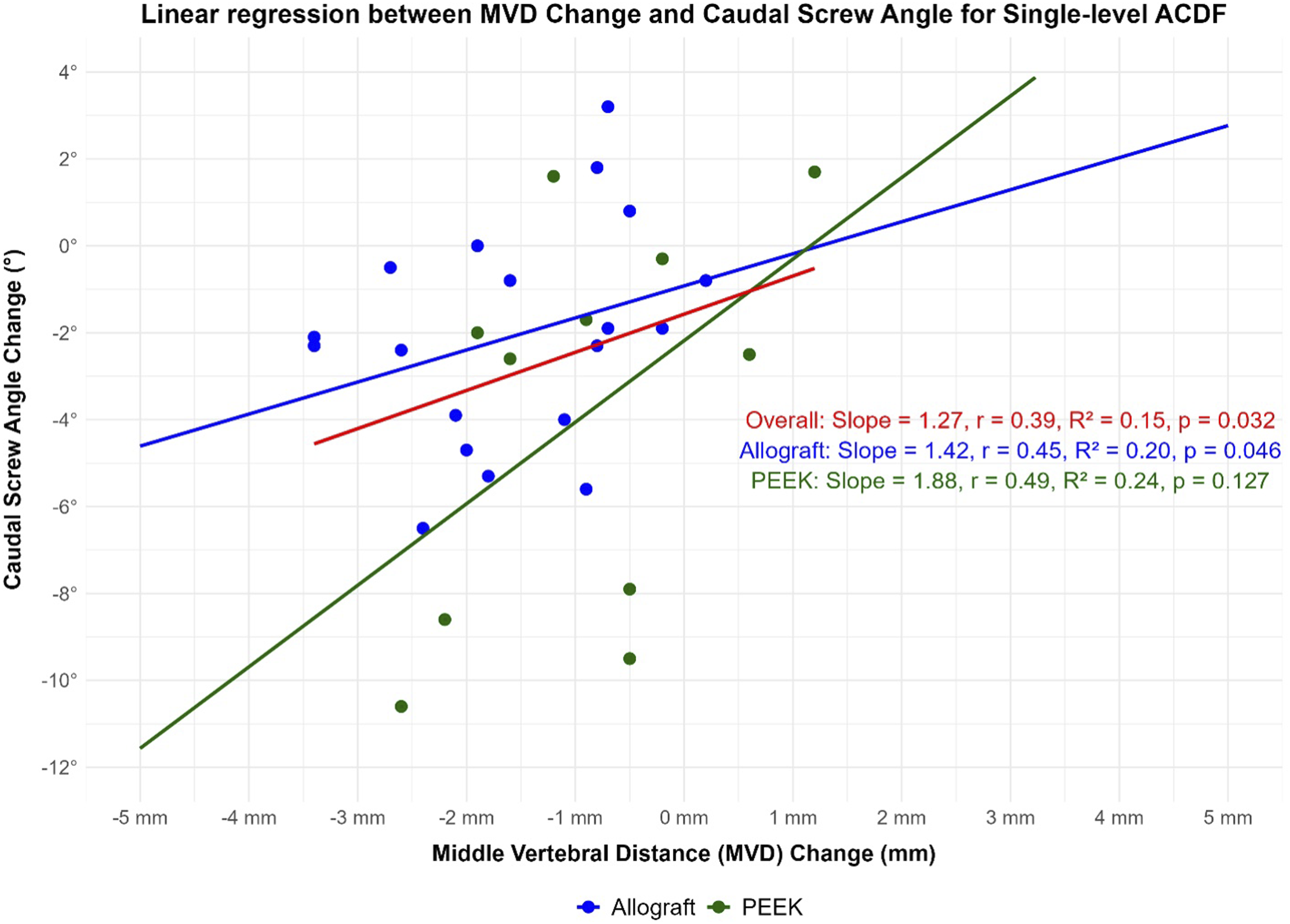
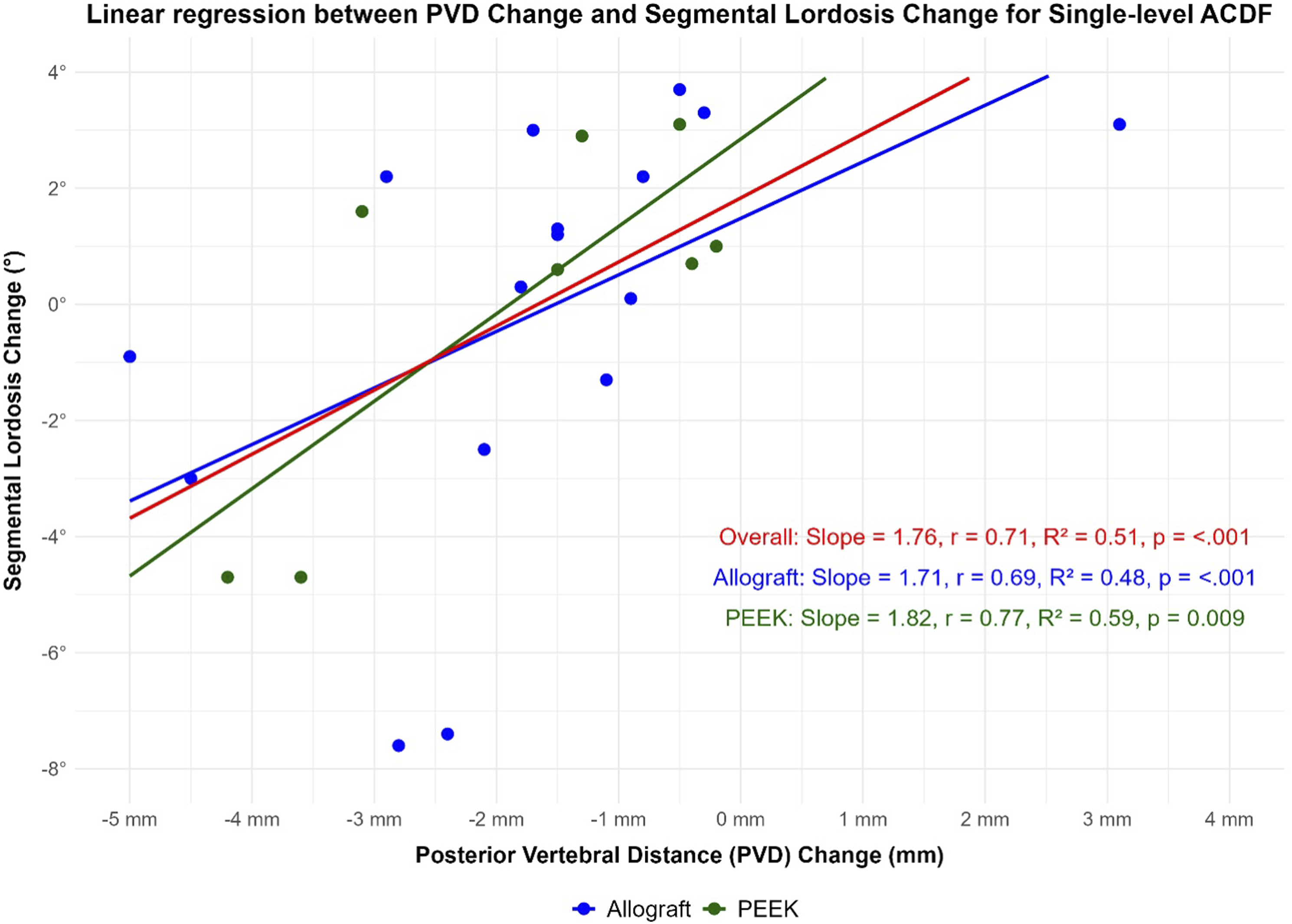
For a single-level ACDF, univariate analyses showed that a decrease in AVD was associated with a decrease in the caudal screw angle (β = 1.5, r = .55, P = .001, Figure 2) and a decrease in the MVD was also associated with a decrease in the caudal screw angle (β = 1.3, r = .39, P = .03, Figure 3). A decrease in PVD was associated with a decrease in segmental lordosis (β = 1.8, r = .71, P < .001, Figure 4). Results of multivariate analyses showed that a decrease in the AVD (β = 3.9, P = .006) and decrease in the MVD (β = 4.1, P = .01) is associated with greater C2-C7 lordosis change (R2 = .24, P = .01). Linear regression between anterior vertebral distance (AVD) and cadual screw angle change in single level ACDF stratified by type of graft. Linear regression between middle vertebral distance (MVD) change and caudal screw angle change in single level ACDF stratified by type of graft. Linear regression between posterior vertebral distance (PVD) change and Fused segmental lordosis change in single level ACDF stratified by type of graft.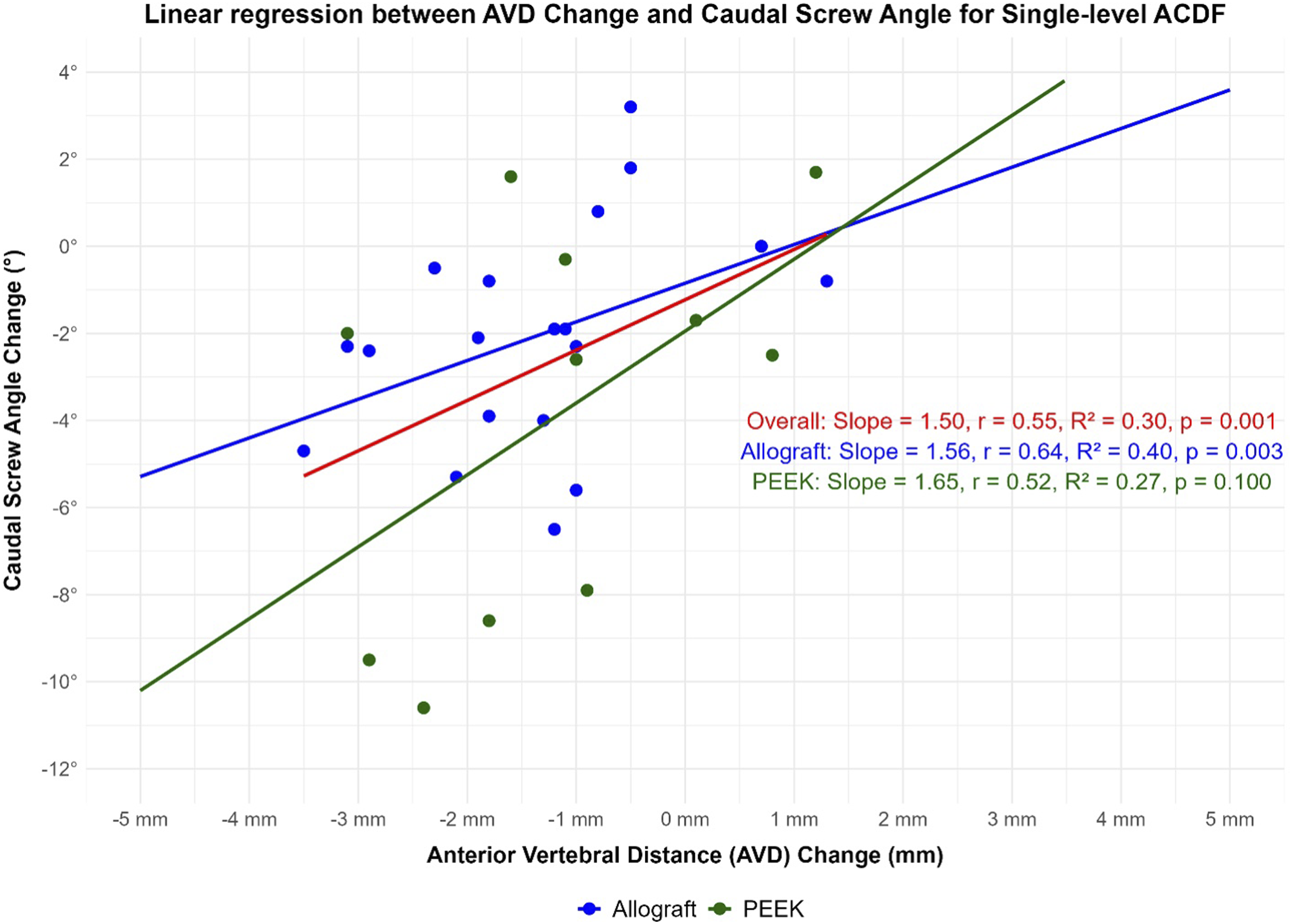
Univariate analyses for two-level ACDF showed that a higher caudal screw-to-body ratio was associated with less subsidence in MVD (β = 10, r = .52, R2 = .27, P = .01). Specifically, for every .1 increase in the caudal screw-to-body ratio, there was 1.2 mm less change in MVD (Figure 5). Linear regression between caudal screw-to-vertebral length ratio and middle vertebral body distance (MVD) in two-level ACDF and single-level ACCF separated by graft type.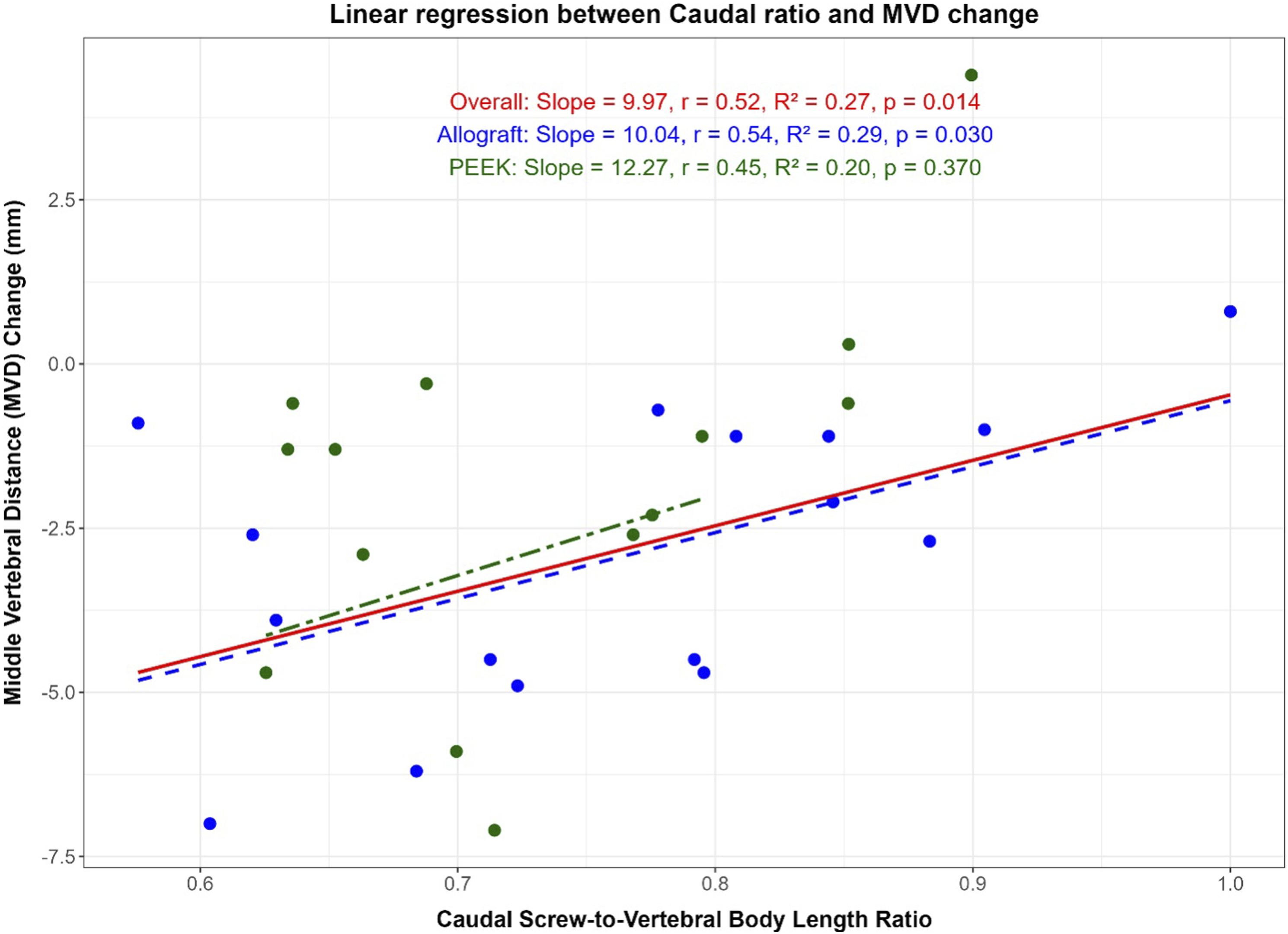
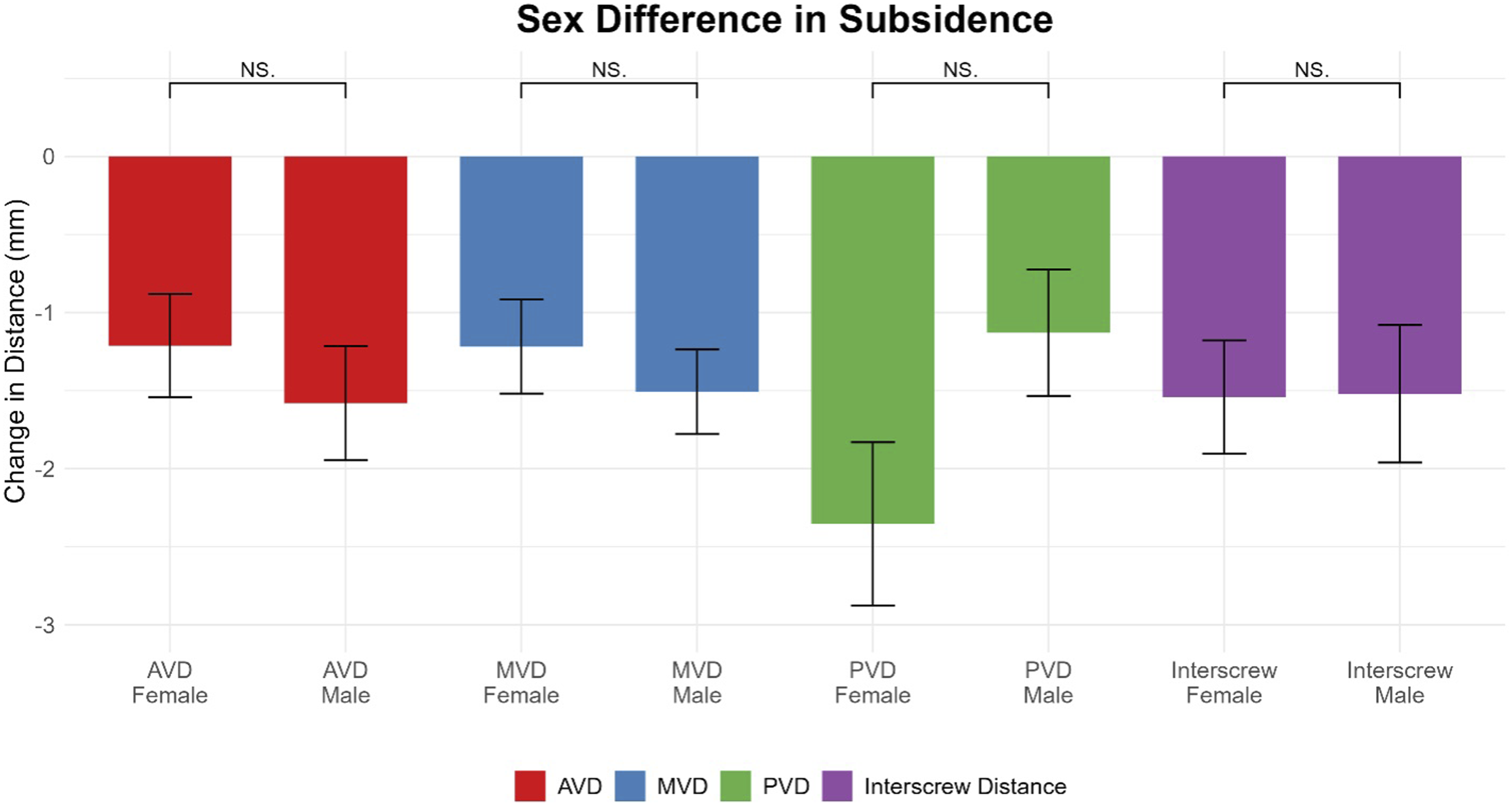
When stratifying by graft type, there was no significant difference found between any AVD, MVD, PVD, or interscrew distance changes between allograft and PEEK groups (Figure 6). There was no significant difference in subsidence between males and females (Figure 7). Comparison of anterior vertebral distance (AVD), middle vertebral distance (MVD), posterior vertebral distance (PVD), and interscrew distance change between allograft and PEEK. Wilcoxon rank-sum tests were used for comparisons. Comparison of anterior vertebral distance (AVD), middle vertebral distance (MVD), posterior vertebral distance (PVD), and interscrew distance change between male and female sex. Wilcoxon rank-sum tests were used for comparisons.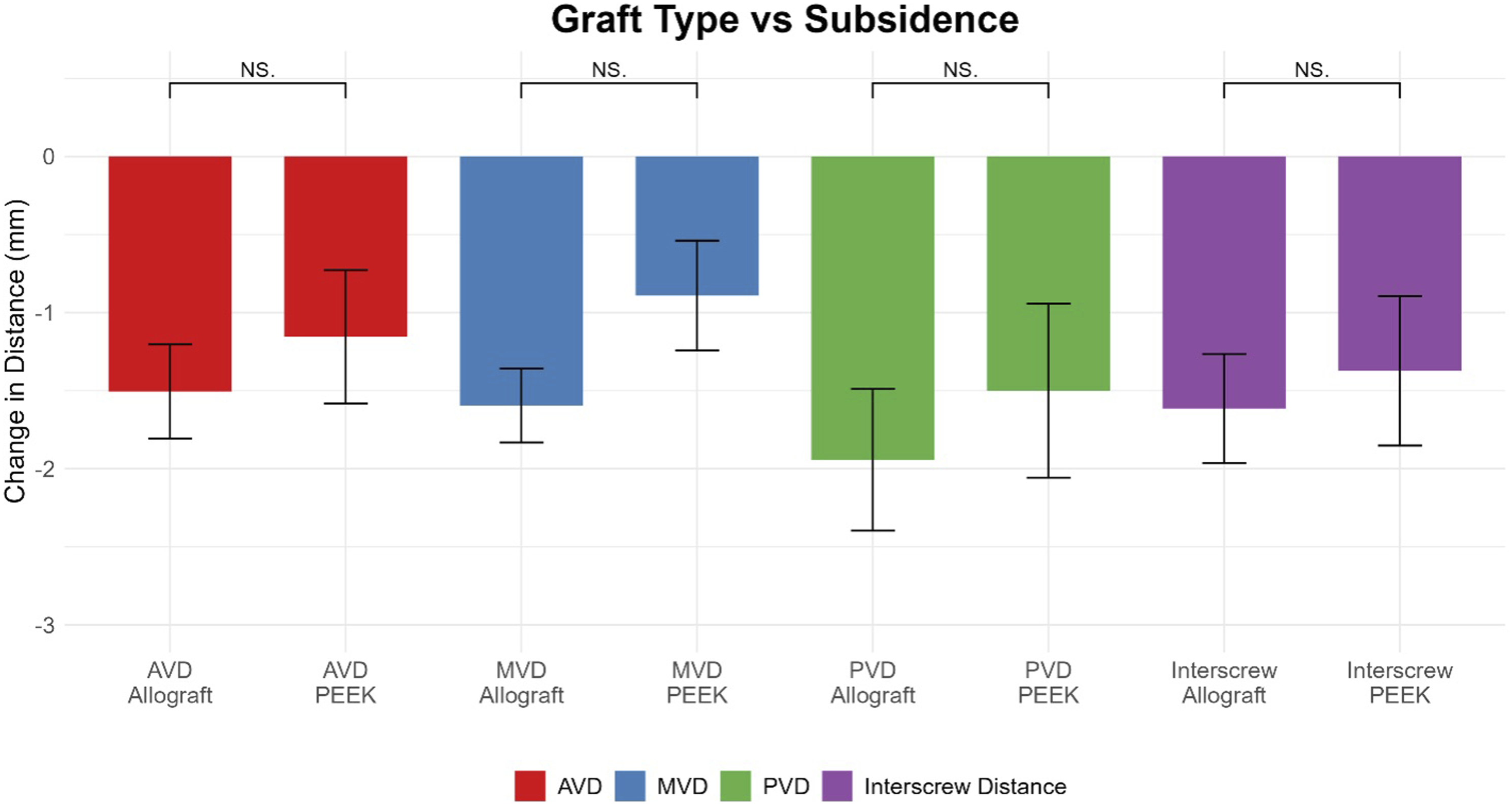
Discussion
Cage subsidence is frequently observed following ACDF procedures (average incidence of 21.1%, ranging from 0 to 83%), with varying definitions and techniques of how subsidence is measured. 11 Subsidence, commonly defined as a reduction of more than 2 or 3 mm in anterior or posterior disc height following ACDF during the postoperative period, is a frequent phenomenon. Prior studies have evaluating subsidence following ACDF have utilized various measurements including the distance between endplates at any location as well as the distance between the tips of screws.4-7 While the clinical implications of subsidence remain uncertain, it can significantly affect cervical sagittal alignment as well. 12 Karikari et al emphasized the necessity for a validated definition and standardized measurement technique to accurately assess the incidence of subsidence and its influence on both radiographic and clinical outcomes. 13 We assessed a combination of changes in variable screw angles at both the cephalad and caudal aspects of the construct as well as the relative length of the screws, factoring in interscrew distance and intradiscal heights (across the anterior, middle, and posterior aspects) for radiological identification of subsidence. In our study, we found that a decrease in the angle of the caudal variable angled screws was associated with subsidence, as measured by AVD and MVD. Prior studies have not specifically focused on the specific location of subsidence along the anterior-posterior spectrum of the disc space. We may be observing an association with the caudal variable angled screws and not the cephalad screws as there may be greater loads experienced at the caudal screws due to the additional cephalad force and longer lever arm of the fused segment, compared to the cephalad screws. As many of our interbody grafts are lordotic and placed closer to the anterior aspect of the disc space (compared to the posterior edge of the disc space), there may greater surface area of interbody graft-to-endplate for subsidence to occur in the anterior and middle aspects of the disc space. These observations require additional investigation in the future.
Several factors have been recognized as potential contributors to subsidence, encompassing graft type, location, sagittal alignment, number of levels, plate length, screw angle, bone mineral density, and excessive resection of vertebral endplates with a lower screw tip to vertebral body height ratio.7-9,14 Nevertheless, the identification of changes in the cephalad/caudal variable screw angles nor the screw-to-vertebral body ratio have been evaluated in the setting of subsidence following ACDF procedures. Some studies have demonstrated an association between severe subsidence (>3 mm) and eventual pseudarthrosis. In that setting, Lee et al have observed greater risks of pseudarthrosis following ACDF when the screw-to-vertebral body ratio is below 75%. 10 And Jimenez et al recommended that placing a “short” anterior plate with screws measuring greater than 20°, may be protective against subsidence. 8 As subsidence may represent an early marker for potential pseudarthrosis, it is important to identify potential radiographic markers, such as changes in screw angles; and surgical technique factors (screw length) that may prevent or identify these complications.
In our study, 18 patients demonstrated subsidence greater than 3 mm, measured with either the anterior/middle/posterior vertebral distances and/or interscrew distance. No patients required re-operation within 6 months of surgery for subsidence-related complications. Similarly, in this patient population, we did not observe adverse clinical outcomes, such as exacerbation of neck or arm pain, or worsening myelopathic symptoms, in patients who experienced cage subsidence and subsequently required revision surgery. All patients underwent the placement of anterior plates with their fusion construct. Here was no significant effect on any of the subsidence measurements based on graft type or the number of levels fused. Previous studies have suggested a higher likelihood of cage subsidence when stand-alone cages are employed compared to the conventional plate and cage construct (CPC) in multi-level ACDF surgeries. In a meta-analysis conducted by Lu et al, no significant disparities were found between the zero-profile self-locking standalone cages (SLSA) and the CPC group in single-segment ACDFs. However, an increase in subsidence was noted in the zero-profile group for multi-segment ACDFs. 15 This pattern was similarly observed by other authors, including Chen and Zhu et al, who reported an elevated cage subsidence rate in stand-alone cages compared to CPC for three-level cervical degenerative spondylopathy.16,17 From a biomechanical standpoint, anterior metal plating aids in distributing the applied loading pressure directly to the endplate/cage interfaces. In multi-segment ACDFs, this effect is more significant compared to single-level discectomies, potentially diminishing the risk of cage subsidence.
This study reveals that for single level ACDF there was no significant association between ratio and radiographic subsidence. However, for 2 level ACDF, a higher caudal ratio was significantly associated with reduced subsidence for MVD.
The present study has several limitations, primarily due to its retrospective design. Specifically, there are noteworthy constraints. Firstly, while linear measurements on a PACS are deemed reliable for CT scans, they may lack accuracy for digital plain radiographs without internal calibration. Consequently, we opted for a ratio-based approach rather than relying on absolute disc height measurements for a more precise analysis. Secondly, the sample size of patients and individual levels that underwent surgery was relatively small, with no patients that require re-operation for subsidence. Therefore, a more extensive follow-up period and a larger cohort of patients are imperative to comprehensively assess changes in subsidence over time, as well as to ascertain its impact on clinical outcomes and cervical alignments. The cohort of patients in this study was relative heterogenous with a combination of single- and multi-level surgeries. There may be a variance in the biomechanical dynamics between one-level and multi-level ACDF procedures. So, the diversity in patient groups could influence the study’s outcomes and interpretations. Therefore, a more extensive follow-up period and a larger cohort of homogenous patients are imperative to comprehensively assess changes in subsidence over time, as well as to ascertain its impact on clinical outcomes and cervical alignments.
Conclusion
In conclusion, our findings suggest that within the confines of a single center utilizing comparable surgical techniques, a decrease in the angle of the variable angled screws placed at the caudal level of the construct is associated with radiographic subsidence measured by anterior and middle disc height changes after an ACDF for degenerative pathology over a 6-month postoperative period. This angle decrease is an indicator of possible subsidence, but is limited to an analysis only at cephalad and caudal levels, and only in cases in which variable angle screws were utilized. The causative relationship between subsidence and this screw angle change remains unclear, and we propose using the screw angle change only as a radiographic marker of subsidence. Longer screws may be protective of subsidence. Thus, changes in variable screw angles may serve as an early identification marker for subsidence.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
