Abstract
Study Design
A retrospective study.
Objective
To develop a new MRI scoring system to assess patients’ clinical characteristics, outcomes and complications.
Methods
A retrospective 1-year follow-up study of 366 patients with cervical spondylosis from 2017 to 2021. The CCCFLS scores (cervical curvature and balance (CC), spinal cord curvature (SC), spinal cord compression ratio (CR), cerebrospinal fluid space (CFS). Spinal cord and lesion location (SL). Increased Signal Intensity (ISI) were divided into Mild group (0-6), Moderate group (6-12), and Severe group (12-18) for comparison, and the Japanese Orthopaedic Association (JOA) scores, visual analog scale (VAS), numerical rating scale (NRS), Neck Disability Index (NDI) and Nurick scores were evaluated. Correlation and regression analyses were performed between each variable and the total model in relation to clinical symptoms and C5 palsy.
Results
The CCCFLS scoring system was linearly correlated with JOA, NRS, Nurick and NDI scores, with significant differences in JOA scores among patients with different CC, CR, CFS, ISI scores, with a predictive model (R2 = 69.3%), and significant differences in preoperative and final follow-up clinical scores among the 3 groups, with a higher rate of improvement in JOA in the severe group (P < .05), while patients with and without C5 paralysis had significant differences in preoperative SC and SL (P < .05).
Conclusion
CCCFLS scoring system can be divided into mild (0-6). moderate (6-12), severe (12-18) groups. It can effectively reflect the severity of clinical symptoms, and the improvement rate of JOA is better in the severe group, while the preoperative SC and SL scores are closely related to C5 palsy.
Level of Evidence
III
Cervical spondylotic myelopathy (CSM) is a neurological disorder caused by degenerative changes in the cervical spine, resulting in compression of the spinal cord. 1 It is a common cause of spinal cord dysfunction or physical incapacity in the aging Chinese population. As time continues, patients go from no clinical symptoms to neurological dysfunction of varying severeeity.2,3 In recent years, it has become commonplace for magnetic resonance imaging (MRI) to detect the benign nature and insidious development of patients. When patients present with severe CSM with neurological complications, surgical treatment is required. However, the best option or most appropriate surgery for asymptomatic or minimally symptomatic patients is controversial. 4 MRI, as the gold standard for detecting spinal cord injury, shows the anatomy and location of the lesion, the degree of spinal cord compression and signal intensity, and the overall state of the cervical spine. 5 Previous studies have evaluated clinical symptoms and MRI may have prognostic value for surgical outcomes, but the conclusive results between MRI, clinical scores and surgical outcomes remain unclear.6-8 On the other hand, MRI only shows form, not function. However, it is significant to explore the association between spinal cord function and MRI, which can also help in forecasting surgical outcomes. 8 In this study, clinical features and neuroradiological data were evaluated to develop a new useful scoring system for assessing cervical spinal cord function and to analyze its relationship with preoperative symptoms, outcomes and C5 paralysis complications.
Materials and Methods
Study Design
This study retrospectively analyzed clinical data collected from 2017 to 2021 on 400 patients with cervical spondylotic myelopathy who underwent spinal surgery and were followed for 1 year. The inclusion criteria were as follows: (1) diagnosis of CSM based on clinical symptoms and data; (2) complete and clear MRI images of the cervical spine that could be accurately measured and evaluated; and (3) detailed documentation of patient visual analog scale (VAS), numerical rating scale (NRS), Japanese Orthopaedic Association (JOA) scores, Nurick and Neck Disability Index (NDI). Exclusion criteria were as follows: (1) history of previous trauma or spine surgery; (2) diseases that severely affected functional scores such as Parkinson’s disease, ankylosing spondylitis, and rheumatoid arthritis; (3) presence of ossification of the posterior longitudinal ligament (OPLL), infection, tuberculosis, tumor, congenital malformation, or other diseases; and (4) incomplete imaging data or functional score information. A total of 366 cases meeting the criteria were enrolled in the study, including 207 males (56.56%) and 159 females (43.44%); patients were divided into 3 groups (mild (0-6), moderate (6-12), and severe (12-18) groups) according to the CCCFLS scoring model.
CCCFLS Scoring System
CCCFLS Scoring System.

The maximum compressed sagittal plane length (a) was measured, compared with the average length of the upper(b) and lower(c) layers of the unaffected spinal cord, CR = 2a/(b + c). The vertebral artery axis and the long axis of the spinal cord were used to evaluate the displacement of the spinal cord for the coronal plane, and the midline of the spinal canal and the short axis of the spinal cord represent the displacement of the spinal cord for the sagittal plane. Therefore, the 2 indicators are synergistic but separate. The T2 signal of the selected lesion was compared with the adjacent unaffected spinal cord.
Outcome Measures
VAS, Nurick, NDI, and JOA scores were obtained from all patients at the initial and final follow-up. (1) JOA scores relates to 3 categories: motor, sensory, and bladder function. The total score is 17. According to the formula (improvement rate (%) = [postoperative score - preoperative score]/[17 - preoperative score] × 100%) is suggested to assess the improvement rate of surgical procedures. (2) The NRS is an 11-point numeric scale ranging from zero (no pain) to ten (the most severe pain). (3) Nurick consists of 6 scales (0-5). (4) The NDI consists of a 50-point scale.
Surgical Procedure for Degenerative Cervical Myelopathy 12
Patients in this study underwent 4 surgical procedures, including grade ≥2 (multilevel) anterior cervical discectomy and fusion (mACDF), anterior cervical corpectomy and fusion (ACCF), and posterior cervical laminectomy and fusion (LF) and cervical laminoplasty (LP).
Statistical Analysis
All radiographic images were transferred to a computer. Measurements were evaluated twice with imaging software by 3 orthopedic spine surgeons independently to verify intra-observer and interobserver reliability and consistency. SPSS (Version 24.0; SPSS Inc., Chicago, IL) was used for statistical analysis when P values were <.05. Continuous variables were recorded as mean ± standard deviation (SD), and categorical variables were expressed as proportions (%). Correlation analysis was used to analyze correlations between functional scores, imaging parameters, age, body mass index (BMI), duration of symptoms and their change parameters. The correlation coefficient r was calculated, linear regression analysis was used to compare scales and multivariate logistic regression analysis was performed to obtain a linear regression model. Multiple ANOVA LSD tests were performed to compare the means or data distributions of continuous variables. Categorical variables were compared appropriately using the χ2 (chi-square) test or Fisher’s exact test. Ordered variables are compared using Kruskal Wallis tests.
Results
Patient Population
Clinical Characteristics of Patients with Different Scoring Models.
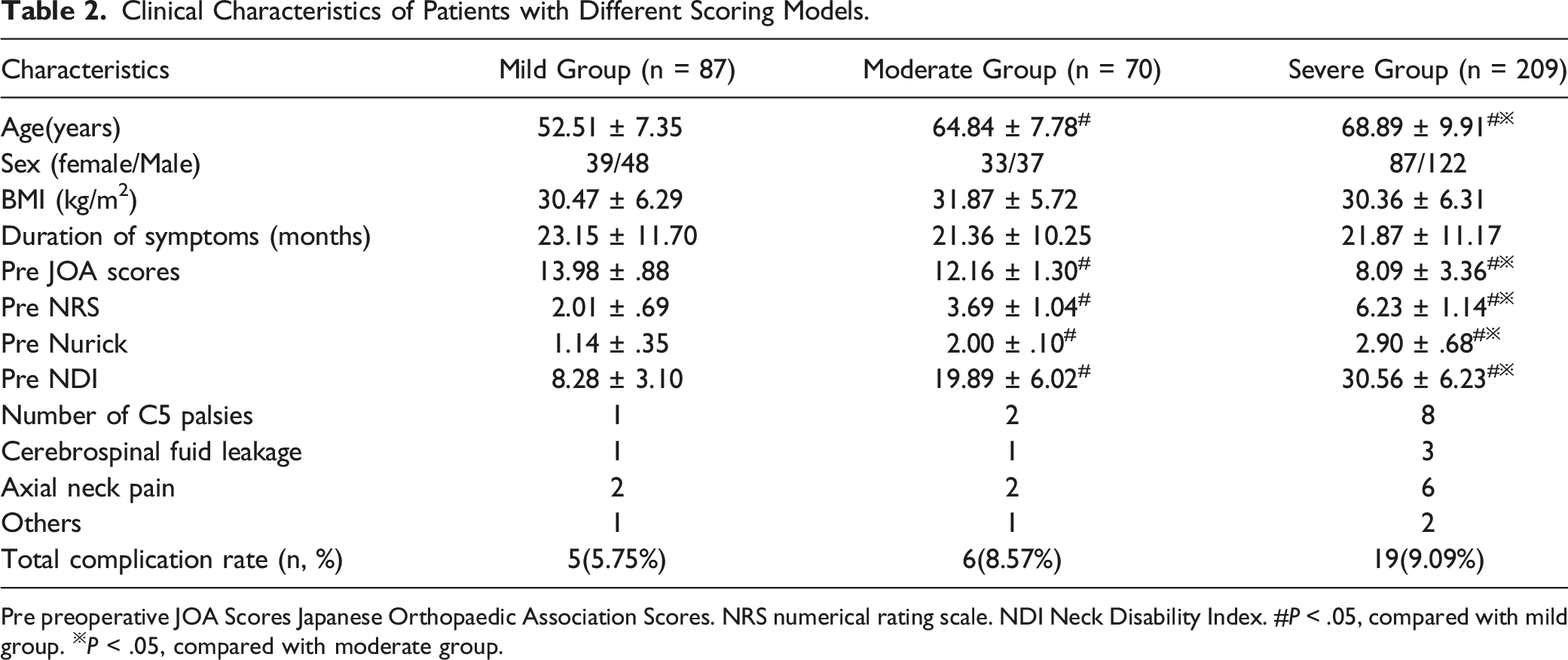
Pre preoperative JOA Scores Japanese Orthopaedic Association Scores. NRS numerical rating scale. NDI Neck Disability Index. #P < .05, compared with mild group. ※P < .05, compared with moderate group.
Reliability
In this study, the Kendall W test was applied to analyze the diagnostic consistency of the CCCFLS scoring system among 3 radiologists for 366 subjects. The results of preoperative and postoperative Kendall W coefficient were .904 and .934, respectively, P < .001, showing a strong consistency.
Correlations Between Functional Scores and Imaging Scoring Models Parameters
Correlation Between Preoperative Clinical Scores and MRI Scores.
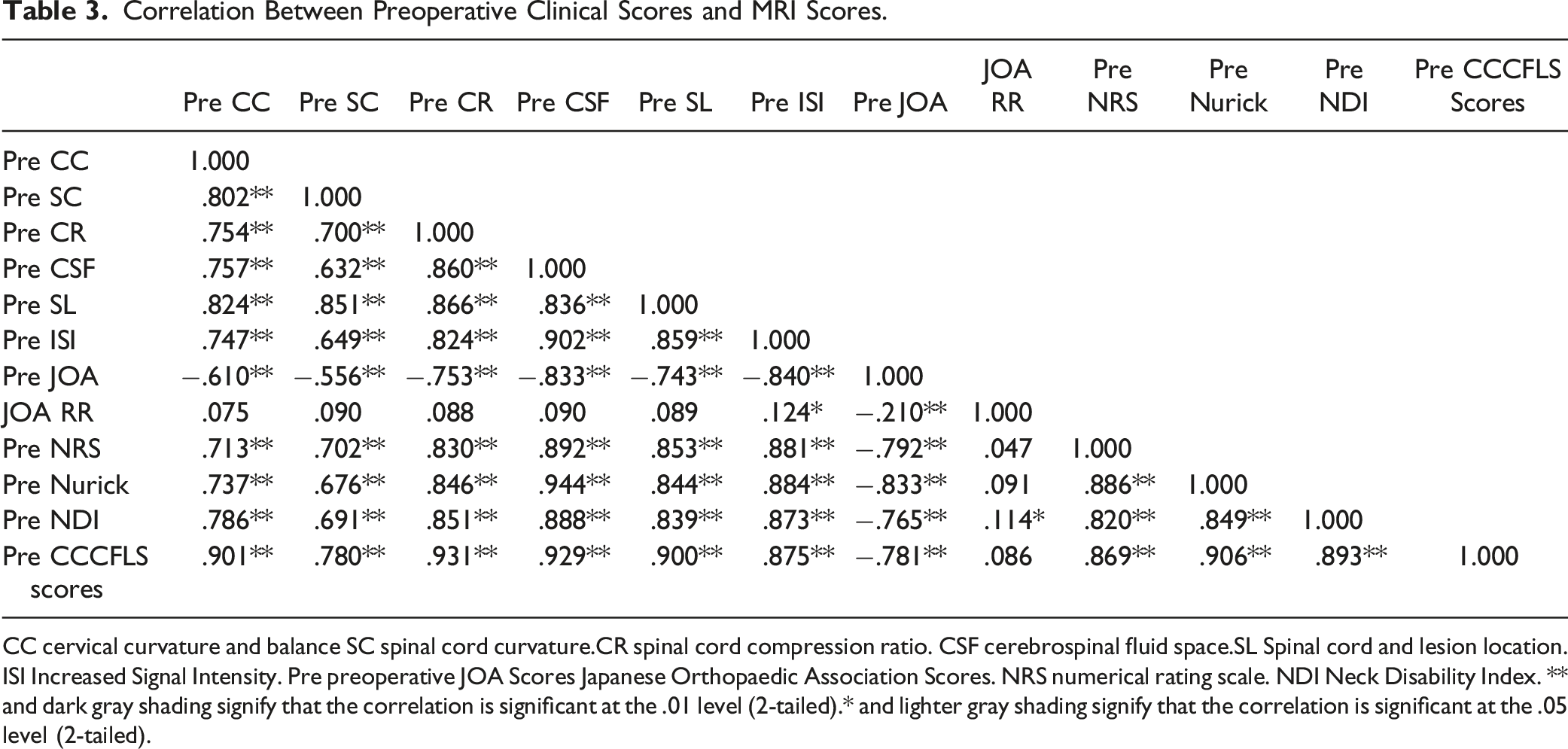
CC cervical curvature and balance SC spinal cord curvature.CR spinal cord compression ratio. CSF cerebrospinal fluid space.SL Spinal cord and lesion location. ISI Increased Signal Intensity. Pre preoperative JOA Scores Japanese Orthopaedic Association Scores. NRS numerical rating scale. NDI Neck Disability Index. ** and dark gray shading signify that the correlation is significant at the .01 level (2-tailed).* and lighter gray shading signify that the correlation is significant at the .05 level (2-tailed).
Regression Analysis to Determine the Independent Risk Factors and Models
Regression analysis revealed that this scoring system was correlated with preoperative JOA, NRS, Nurick and NDI scores. The regression models are Y = −.5113*X + 16.02(R2 = .5521), Y = .3453*X + .8035(R2 = .8101),Y = .1445*X + .6626(R2 = .7314), Y = 1.832 *X + 2.098 (R2 = .8286)respectively. (P < .001). Figure 1 Correlation observed between CCCFLS scores on MRI and clinical scores. This score is closely related to JOA, NRS, Nurick, NDI.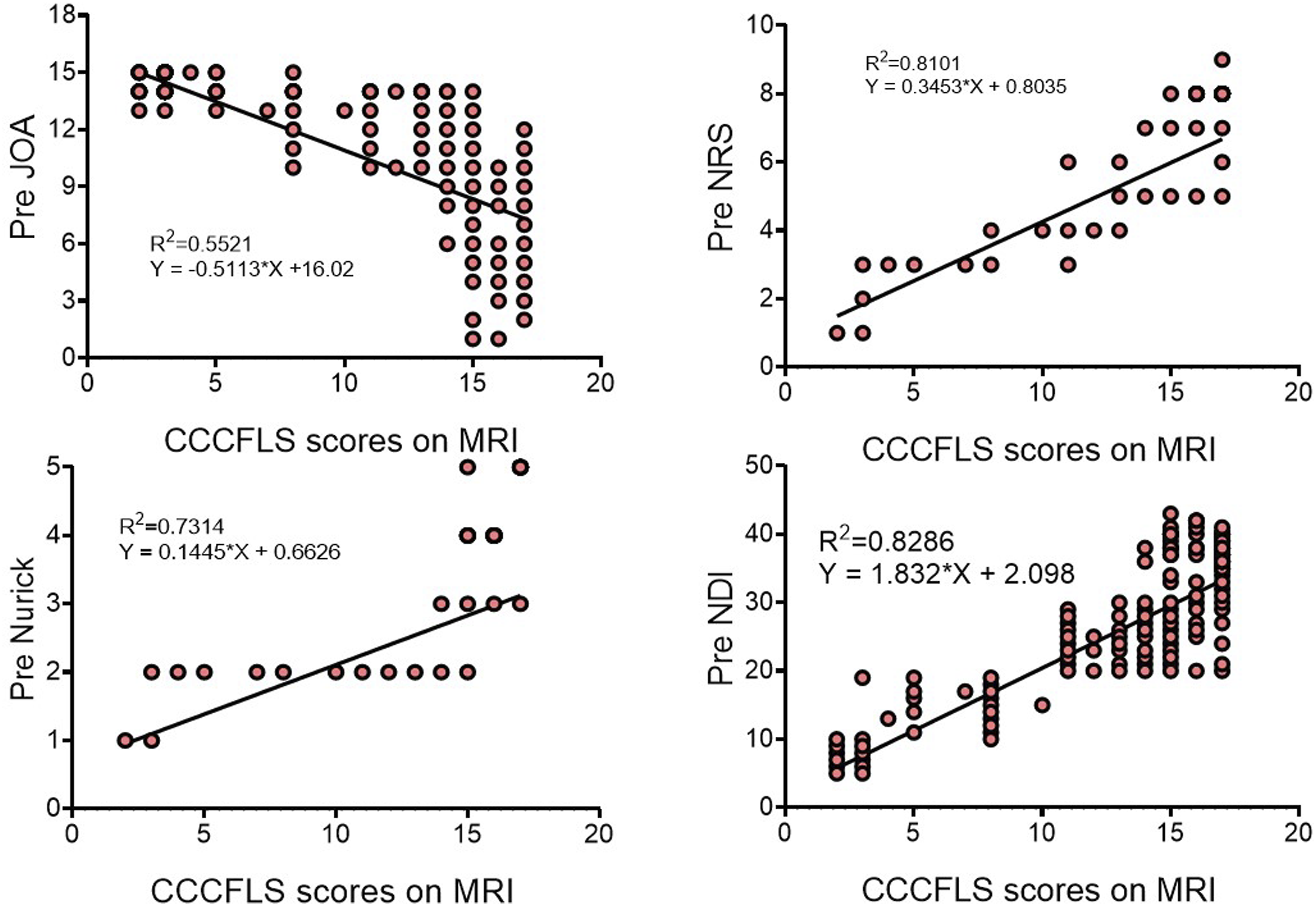
Regression was performed with 6 preoperative scores as independent variables and JOA score and JOA improvement rate as dependent variables. The results indicated that the regression model was statistically significant (F = 207.394, P < .001). The independent variable explained 69.3% of the change in the preoperative JOA score, which had a high degree of explanation and therefore also implied that the effect of the remaining factors except spinal cord position (spinal cord curvature is covariant with cervical curvature) on the JOA score is statistically significant. The regression equation was Y = 17.121 −1.634 XCSF−1.949X ISI+1.249XCC−1.026XCR. However, the score model does not predict the rate of JOA improvement at this time (F = 11.855, P < .05, R2 = 2.9%). We evaluated the relationship between surgical method (ACDF(1)vs ACCF(2) vs laminoplasty (3)vs posterior laminectomy/fusion (4)), number of surgical segments (2-5), and basic data with JOA improvement rate. Although surgical segment and surgical approach were found to be associated with JOA improvement rates, a model to predict JOA improvement rates could not be developed. (F = 6.514, P < .05 R2 = 2.9%). In addition, the weighted linear regression model (Y = .569 + .117 XCSF) does not predict the rate of JOA improvement at this time (F = 3.017, P < .05, R2 = 3.4%).
Surgical approach and decompression operator were the main contributors to the improvement. Figure 2 shows the statistical difference in JOA scores for the different scores (0-3, 4 groups) of the 4 variables (CSF, ISI, CC, CR) (P < .05). Group comparison of main factors affecting JOA score. The difference in JOA scores between Pre CC, Pre CR, CSF, ISI groups was statistically significant.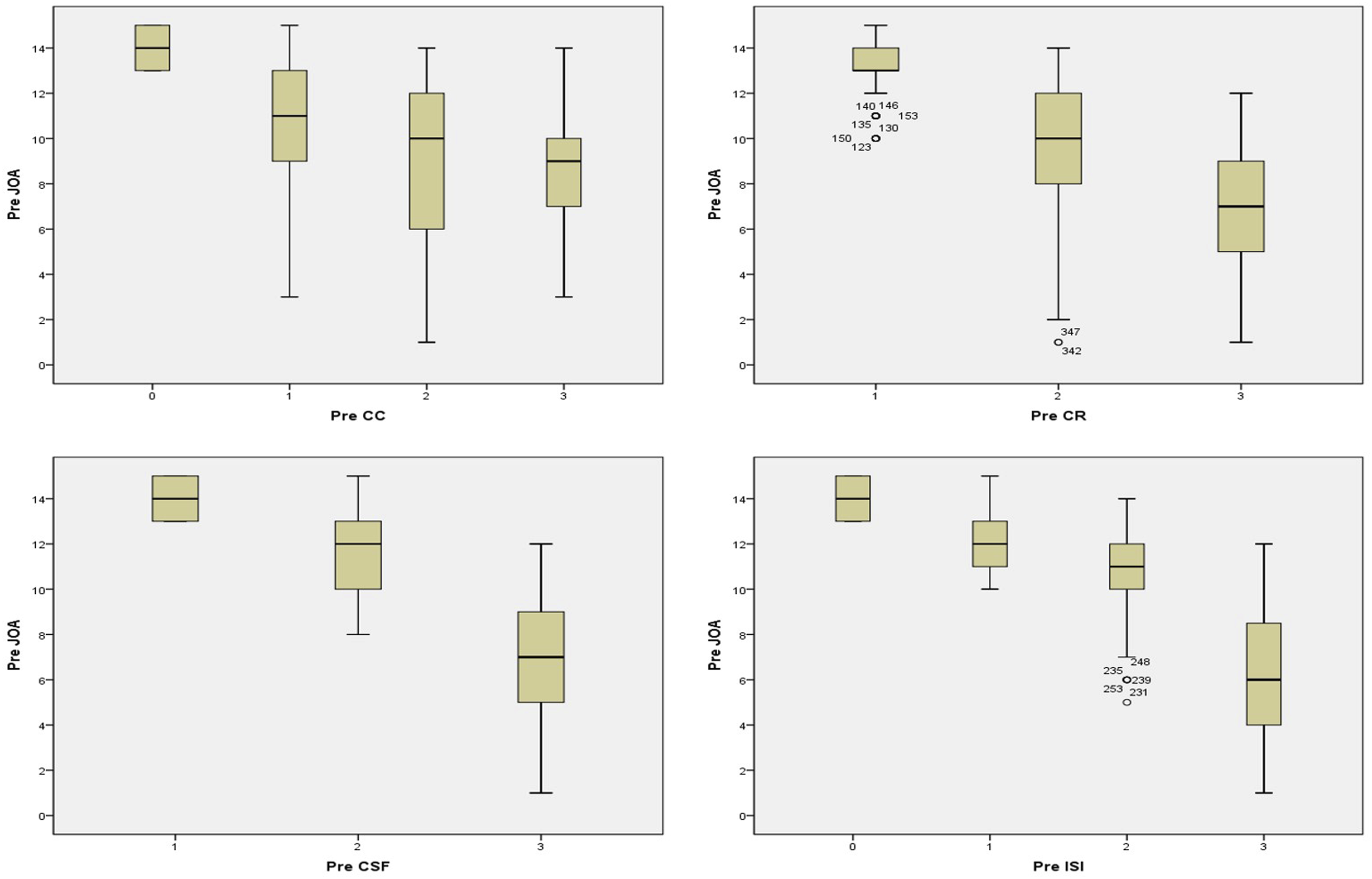
There were statistically significant differences in the mean values of preoperative scores in all 3 groups (P < .05). It indicates that the higher the preoperative scores of patients, the more frequent and severe the clinical symptoms and the poorer the quality of life Table 2.
1-Year Follow-Up Efficacy of Patients with Different Scoring Models in this Study.
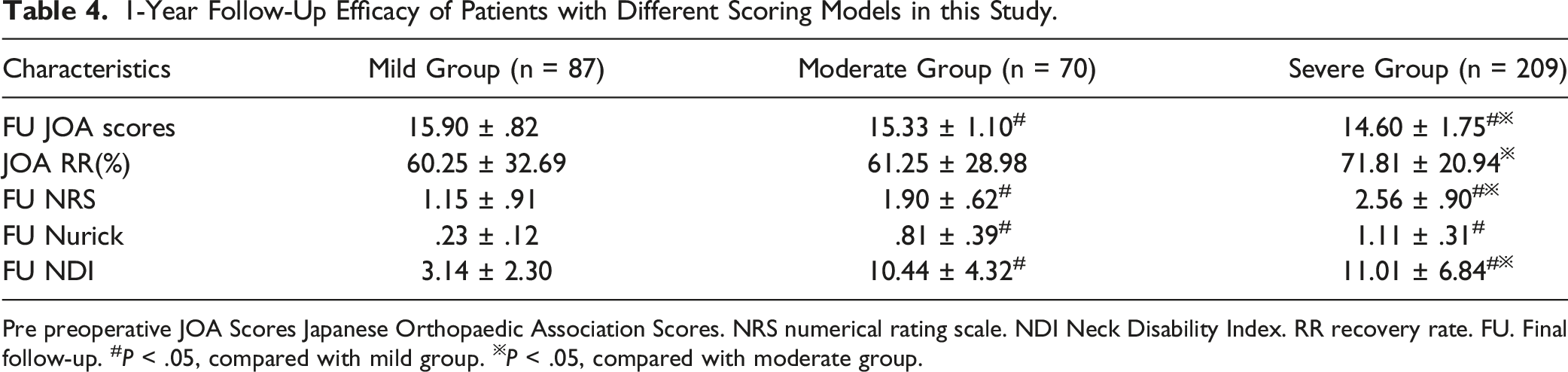
Pre preoperative JOA Scores Japanese Orthopaedic Association Scores. NRS numerical rating scale. NDI Neck Disability Index. RR recovery rate. FU. Final follow-up. #P < .05, compared with mild group. ※P < .05, compared with moderate group.
C5 Paralysis
Comparison of Paralyzed and Non-Paralyzed Patients.
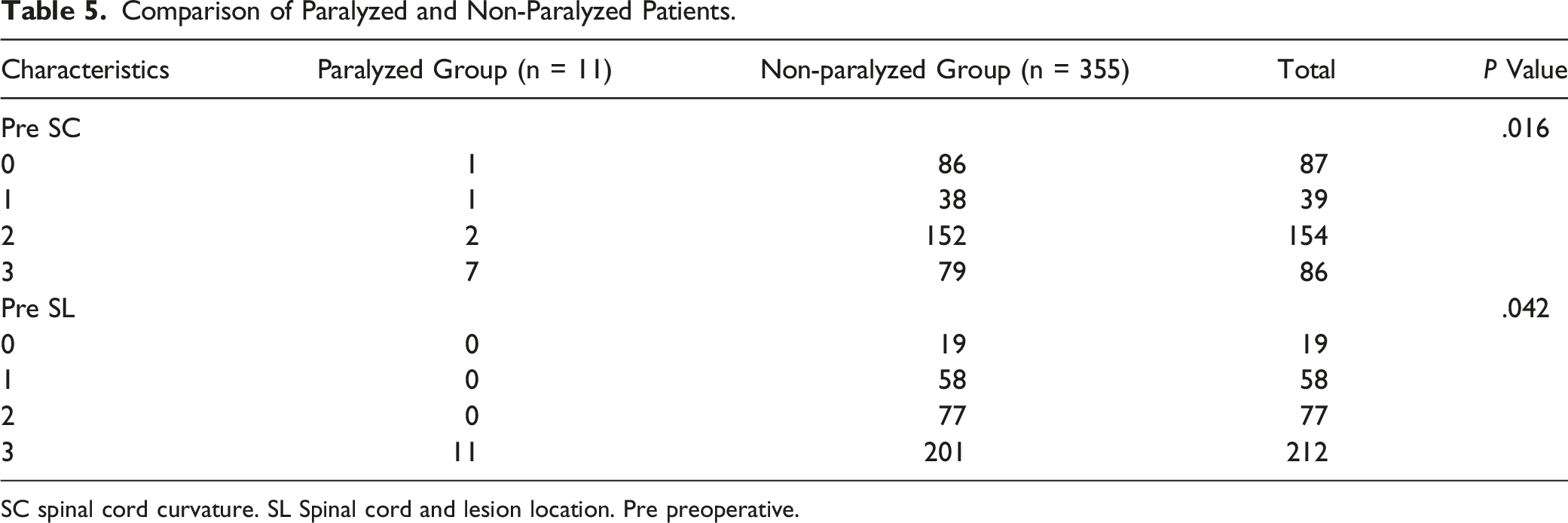
SC spinal cord curvature. SL Spinal cord and lesion location. Pre preoperative.
Discussion
Myelopathy is caused by static compression, spinal misalignment leading to altered spinal cord tone and vascular supply, and dynamic mechanisms of injury. 13 Its natural progression is not well characterized, and gradual MRI changes are not always accompanied by clinical symptoms, but when they do occur, MRI abnormalities often follow them.s, 14 while patient selection and timing criteria are controversial for surgery. 4 Clinical history usually requires periodic review of MRI to assess the rate of disease progression, but it is not consistent with the existence of an optimal time point for surgery.4,15 Early spinal cord compression, with unremarkable clinical presentation and neurological scores, can be assessed by MRI. 16 Also, based on history, signs, and diagnostic tests, MRI may be able to show signs of myelopathy at some point in the time course. 3 This scoring model is closely related to neurological function and may reflect the risk of neurological deterioration or spinal cord injury in patients undergoing non-surgical treatment, with increasing scores representing accelerated disease progression.
Effects of Cervical Curvature and Balance on Spinal Cord Function
The physiological anterior convexity and balance of the cervical spine provides a natural barrier for the spinal cord and nerve roots to maintain a normal physiological state and perform their physiological functions. Regression modeling studies have found a negative correlation between the sagittal angle of the cervical spine on MRI and with JOA scores, reflecting the severity of myelopathy. Patients with high cervical spine scores had severe myelopathy symptoms. 17 Similarly, a correlation between JOA scores and SVA was found using multiple linear regression analysis, with the severity of myelopathy worsening with spinal misalignment. 18 The literature reports that cervical sagittal parameters are important risk factors for CSM and are used to assess cervical spine function and quality of life. Among them, VAS scores and JOA scores are positively correlated with CL and negatively correlated with C2-7 SVA. 19 Because patients have better clinical outcomes when anterior cervical convexity and balance are maintained, the author proposes that the optimal cervical focal angle should be planned preoperatively. 17
Effects of Spinal Cord Curvature and Drift on Neurological Function
Changes in spinal cord curvature are associated with alterations in curvature and balance. The sagittal geometry of the spinal cord is an important biomechanical factor, and the model reflects overall morphological changes in the spinal cord. Lower scores indicate that most of the spinal cord is anteriorly convex. 9 Maintaining normal spinal cord curvature prevents damage to the spinal cord from abnormal or excessive movements of the cervical spine, which increase strain and shear forces within the spinal cord. 20 Kuwazawa et al. reported that the mean midline length of the cervical spinal cord was longer in flexion than in neutral and anteriorly convex positions, and that the spinal cord had minimal axial tension when the cervical spine was in physiological anterior convexity. 21 The compressed spinal cord is more susceptible to distraction injury, especially in cases of combined ligamentous ossification and disc herniation. When the spinal cord is kyphotic or twisted S-shaped, it can lead to a range of neurological dysfunctions. As reported in the literature, the results of this systematic evaluation suggest a higher risk of excessive spinal cord drift and postoperative C5 palsy. 22 Control of dural expansion due to spinal cord kyphosis can prevent C5 palsy. 23 Excessive spinal cord kyphosis also affects spinal cord function and surgical outcomes, 24 and increased total spinal cord displacement is associated with altered spinal conduction, which may lead to worsening myelopathy. 25 Spinal cord displacement is the postoperative occurrence of C5 paralysis the main cause of postoperative C5 paralysis. 26 There is a positive correlation between posterior convex drift of the spinal cord and the risk of C5 paralysis.27,28 Since C5 palsy may be a combination of posterior decompression of spinal drift and relative laxity due to increased anterior spinal convexity, a limited conservative anterior cervical correction is recommended to achieve good spinal drift distances and a low incidence of axial symptoms in patients. 29
Effects of Spinal Cord Compression Rate on Neurological Function
As an independent risk factor for CSM, spinal cord compression has been reported in the literature. The degree of cervical cord compression is a predictor of the severity of the patient’s symptoms. Clinical symptoms are more severe when the degree of spinal cord compression exceeds 30%. 19 Spinal cord compression ratio correlates best with JOA scores. 17
Notably, the spinal cord compression ratio has recently been reported to be significant and has become a major factor in surgical decision making. 30 MRI demonstrates a remarkable correlation between the degree of cervical cord compression and the severity of clinical and spinal cord lesions.31,32 Compression ratio (CR) ≤ .4 is a significant predictor of progression to symptomatic myelopathy. 33 Therefore, the higher the compression ratio, the more severe the myelopathy. The score is also the only independent significant predictor of the presence of clinical myelopathy. 34 Patients with high scores and severe spinal cord lesions recover less well after surgery. 35 The author suggests that the more severe the spinal cord compression, the higher the stress caused by intermediate diffusion compression, as well as the concentration of stress in the circumferential pattern in the posterior gray matter, where biomechanical changes and ischemia may be the underlying mechanism. 36 On the other hand, this higher score and more serious symptoms are associated with reduced spinal cord motion and loss of spinal cord displacement. Compression of the spinal cord leads to a reduction in the flow of cerebrospinal fluid and movement of the spinal cord with clinical symptoms, while spinal cord motion was normal or increased in lower scoring asymptomatic patients. Spinal cord compression results in focal dynamic deformation within the medulla, which may also affect neurological function. 37
Effects of Cerebrospinal Fluid Band on Neurological Function
Decreased cerebrospinal fluid space was the only independent significant predictor of the presence of clinical myelopathy. 34 Shibuya et al. suggested that measurement of cerebrospinal fluid flow disturbances could quantify the degree of spinal cord compression and signal changes. 38 CFS recovery was closely related to the patient’s status of neurological improvement, and there was a high correlation between cerebrospinal fluid flow disturbances, pulsation and flow and the severity of myelopathy.10,39,40 Although CFS may not eliminate spinal cord deformation, it helps to reduce deformation and exerted pressure, acting as a protective cushion. 41 Most importantly, cerebrospinal fluid space facilitates nutrient supply, metabolic and inflammatory waste elimination, and blood circulation, which are crucial for the maintenance of normal spinal cord function. 42
In addition, high preoperative spinal cord CR and CFS band scores, significantly lower CFS velocities and reduced flow continuity are interrupted, and decompression restores CFS and blood circulation around the spinal cord, reestablishes coherence of CFS flow anterior and posterior to the spinal cord, improves CFS flow, and promotes recovery of neurological function.37,43
Effects of Lesions and Spinal Cord Location on Spinal Cord Function
Tethering, spinal cord ischemia and spinal cord reperfusion injury due to spinal cord rotation and displacement are a strong and significant predictor of postoperative C5 palsy.44-46 Preoperative cord rotation was also identified as a significant risk factor for C5 palsy. 47 The nerve root pull theory and spinal cord hyper-drift effect are important causes of C5 nerve palsy. 48 The C5 level is anatomically located at the apex of the anterior cervical convexity, the length of the C5 nerve root is also relatively short, and the angle of the spinal cord is more obtuse, making the postoperative C5 nerve more susceptible to hypertonicity caused by spinal cord drift. 49
This score represents the three-dimensional position of the spinal cord relative to the vertebral body. Asymmetric decompression and displacement of the spinal cord may trigger medically induced spinal cord rotation and increase the risk of C5 paralysis,23,27 while Espander et al. showed that the greater the degree of spinal cord rotation, the higher the C5 nerve root tension and the greater the likelihood of C5 paralysis. 46 In summary, excessive spinal cord drift and spinal cord rotation due to asymmetric decompression is a key factor in the development of C5 paralysis. The present study also revealed that the higher the preoperative spinal cord score, the higher the incidence of postoperative C5 paralysis may be, 46 which has a considerable impact on the clinical prognosis, 50 and although lesions close to the center of the spinal cord are at the greatest risk of damage, lesions on the lateral side, where patients have significant radicular symptoms, may be associated with C5 paralysis. 36 In addition, cervical misalignment and postoperative dural hyper-expansion predict C5 palsy under-recovery. 51
Spinal cord rotation and asymmetric decompression, post-cervical dural hyperextension can trigger coronal and sagittal traction of the nerve roots, while anterior-posterior drift of the spinal cord can cause horizontal traction of the nerve roots. 51 Ultimately, changes in the three-dimensional spinal cord displacement may lead to nerve root tension like a bowstring, resulting in decreased deltoid muscle strength and inadequate C5 palsy recovery, which has an adverse effect on clinical prognosis. 50 For example, after anterior cervical approach, spinal cord displacement is less and direct decompression removes spinal cord rotation caused by compression, but anterior displacement of nerve roots triggered by dural expansion can cause C5 palsy. After posterior cervical surgery, the spinal cord is more posteriorly displaced, and with indirect decompression and the inability to correct spinal cord rotation, the nerve roots are under greater tension, so C5 palsy is highly likely to occur. At the same time, scholars have identified 177 extraforaminal ligaments that connect the spinal nerve to surrounding structures, suggesting that the cervical extraforaminal ligaments may also be associated with postoperative C5 palsy. Whether the posterior expansion of the dural sac and the movement of the spinal cord and nerve roots are found after performing an expanded open-door laminoplasty, or the anterior expansion of the dura and the movement of the nerve roots after an anterior decompression, it may lead to increased nerve root tension. Therefore, changes in the three-dimensional spatial displacement of the spinal cord and nerve roots leading to the pull and displacement of the epidural root may be the main pathological mechanism of postoperative C5 palsy. Also, the bowstring state of the nerve root due to the anchoring effect of the intervertebral ligament and the extradural ligament plays an important role in the development of postoperative C5 palsy. 52 Restoration of rotation and excursion of the spinal cord requires intraoperative attention. 11
Effect of MR T2 Increased Signal Intensity on Spinal Cord Function
Studies have reported that MRI can be used to assess the adequacy of spinal cord decompression and neurological recovery, and that MRI imaging signal changes correlate with clinical severeity. 32 Also, patients with strong spinal cord signal changes have poorer postoperative recovery. 35 Thus, postoperative ISI remission with reduced scores and good postoperative JOA scores and recovery rates have better clinical outcomes. In conclusion, remission of postoperative ISI in patients reflects postoperative symptoms and surgical outcomes. 53 Spinal cord signal intensity progresses from absent to mild and then to strongly progressive, with neurodegenerative changes such as nerve cell loss, gliosis and gray, matter edema corresponding to areas of high signal. High signal is due to intramedullary edema and later it becomes related to demyelination and gliosis. 54 Mild (score 1) ISI represents a reversible stage of intramedullary edema, and reflects mild neuropathological changes in the spinal cord with high recovery potential, with improved CSF environment and microvascular circulation playing a key role in neurological recovery. 55 A score of 3 indicates severe changes and low recovery potential. Both multi-segmental T2W ISI and sharp, intense T2W ISI were associated with poorer surgical outcomes. Postoperative regression of T2W ISI was associated with better functional outcomes. 56 The present study also demonstrated increased ISI scores and progressive deterioration of neurological function, suggesting early surgical decompression and that good neurological recovery and clinical outcomes can be achieved after surgery.
Conclusion
The CCCFLS model can predict clinical symptoms and can be divided into mild (0-6), moderate (6-12), severe (12-18) groups. The improvement rate of JOA is better in the severe group, while the preoperative SC and SL scores are closely related to C5 palsy.
Footnotes
Authors’ Contributions
“SW has contributed to the conception, study design, and was a major contributor in drafting of the study and writing the manuscript. JS, JF, YY, XZ, HY, CG and DH have contributed to the acquisition, analysis, and interpretation of the data. YG and JS finished the final assessment of the manuscript. All authors read and approved the final manuscript.”
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study is supported by the National Natural Science Foundation of China, Grant/Award Numbers: No. 81871828, No. 81702141, No. 81802218.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the Ethics Committee of Changzheng and 910 Hospital.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Data Availability
Data sharing is not applicable to this article as no datasets were generated or analyzed during the current study.
