Abstract
Study Design
clinical study.
Objectives
Loosening of pedicle screws is a frequent complication in patients with osteoporosis. The indication for additional stabilization, such as cement augmentation, is more often based on the subjective intraoperative feeling of the surgeon than on a preoperative bone mineral density (BMD) measurement. Aim was to evaluate the correlation of the intraoperative perceived bone quality in comparison to the objectively measured BMD.
Methods
A total of 62 patients undergoing dorsal stabilization using pedicle screws at a level-1 trauma center were analyzed. The preoperative CT scan measured each instrumented vertebra's pedicle size and BMD. During the surgery, the perceived screw stability was graded by the respective surgeon for each screw.
Results
204 vertebral bodies were evaluated. Looking at all implanted screws a significant correlation between the measured BMD and the perceived screw stability was found (Resident r = .450; R2 = .202; P < .001/Attending r = .364; R2 = .133; P < .001), but there was no significant correlation in the osteoporotic patients (Resident P = .148 / Attending P = .907). The evaluation of the screws implanted in osteoporotic vertebrae showed that the surgeons considered a total of 31% of these screws to be sufficiently stable.
Conclusions
There was no significant correlation between the measured BMD and the perceived pedicle screw stability in the group with osteopenic / osteoporotic bone (<100 mg/cm³). The results indicate that it is not possible to reliably determine the bone quality and the resulting screw stability in patients with reduced BMD. The preoperative measurement of the BMD should become a crucial part of preoperative planning.
Introduction
With an increasing aging society, spine surgery will be more often performed on patients with reduced bone quality and quantity due to different medical conditions. Different indications such as osteoporosis associated vertebral body fractures, 1 secondary kyphosis, spine deformities or tumours and metastases of the spinal column leading to the need of dorsal instrumentation and spondylodesis2-4 despite poor bone quality. Therefore, pedicle screw fixation can be difficult in aged and multimorbid patients. During reduction of the fracture or compression-distraction-manoeuvres, cranial pull-out of the pedicle screw is a common intraoperative complication. However, loosening of pedicle screws is the most frequent cause of failure of posterior stabilization postoperatively.5,6
The screw strength depends on the bone quality, more precisely the bone mineral density (BMD) 7 . In osteoporosis-associated vertebral fractures the incidence of screw loosening is reported up to 60 %. 8
Many biomechanical studies have shown that pedicle screw fatigue load as well as pull-out force are significantly reduced in osteoporotic bone.6,9,10 Most studies have analyzed the effect of pedicle screw augmentation in osteoporotic bone. They have shown a relevant increase in stability after cement augmentation.11-14
In contrast, Weiser et al. examined the impact of cement augmentation in specimen with osteoporotic (< 80-90 mg/cm³) and normal bone mass (>120 mg/cm³). 15 The authors showed that the effect of cement augmentation depends on the BMD - it decreased with increasing BMD. There was nearly no difference between the augmented compared to the non-augmented screws in samples with normal bone mass. Therefore, pedicle screw augmentation with bone cement is recommended to improve screw strength in patients suffering from osteoporosis (BMD below 80-90 mg/cm³).9,11,13
Despite of its advantages, pedicle screw augmentation also carries risks. There is a relevant risk of cement leakage into epidural vessels causing pulmonary cement embolism and into intraspinal space causing radicular compression symptoms and neurological deficits. Furthermore, bone cement can trigger anaphylactic reactions and hemodynamic complications. 16 Due to these risks, the indication for cement augmentation must be carefully evaluated. Consequently, the patient’s bone density should be ideally determined preoperatively and the decision for cement augmentation should be based on the measured BMD. However, in daily hospital routine the preoperative bone densitometry is often dropped.
Many spine surgeons propagate that they can feel bone quality while inserting pedicle screws. This “feeling” should arise both when creating the transpedicular screw channel and when screwing in the screw itself. A high resistance when reaming or drilling and a high screw-in torque should suggest good screw stability. Therefore, in many cases the decision for pedicle screw augmentation is based on the subjective intraoperative feeling of the surgeon. The aim of this clinical study was to investigate the correlation of the intraoperative perceived bone quality in comparison to the objectively measured bone density using QCT.
Methods
The present study was approved by the relevant ethics committee (approval number: AN 8/11/17) in compliance with the Helsinki Declaration. Since only preexisting data and assessments independent of the patient’s treatment were evaluated, this study was deemed exempt from the informed consent requirement.
In 2019, 62 patients, who were undergoing dorsal stabilization using pedicle screws at a level-1 trauma center were analyzed. Indications for surgical stabilization were fractures and degenerative spinal pathologies. A total of 204 screws were implanted and included in the evaluation.
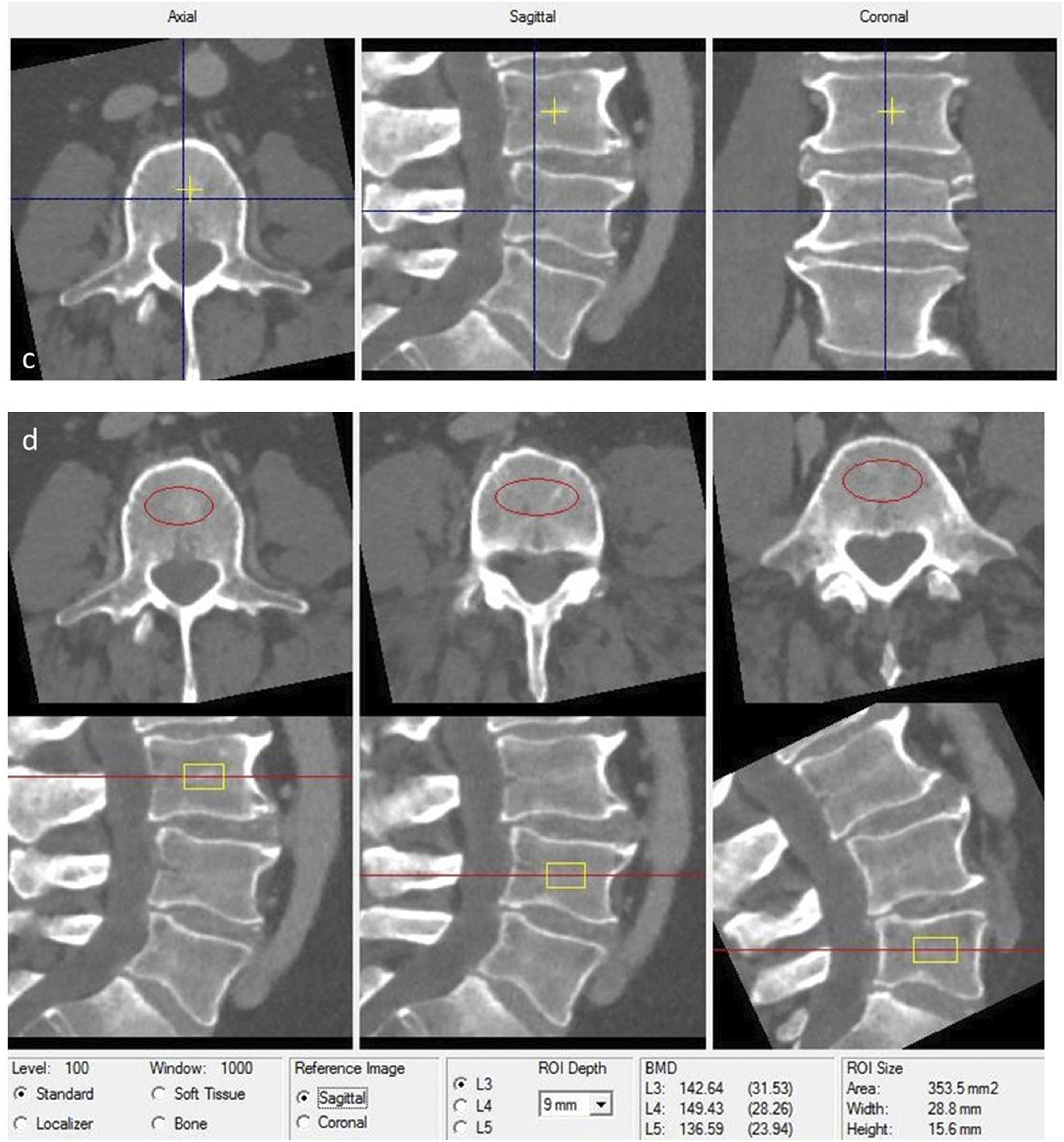
The age and gender of the respective patients were recorded. A computed tomography (CT) of the spinal section to be instrumented was performed preoperatively in all patients. The corresponding pedicle size for each instrumented pedicle was measured in the CT scan using an axial and coronal view (Figure 1). Furthermore, an asynchronous QCT (CliniQCT, Mindways, Austin, TX) was used to measure the bone mineral density in each vertebral body, which was instrumented using pedicle screws (Figure 2). During the surgical stabilization, standard pedicle screws (Expedium / Viper / CFX, DePuy Synthes Inc., West Chester, PA) were implanted into the respective vertebral bodies, percutaneously or via an open access. For the implantation of the respective screws, a transpedicular channel was created using an awl. In all cases, the trajectory ran transpedicularly and parallel to the upper end plate. The screw was implanted using a hand screwdriver without cutting a thread beforehand. All patients were operated by 2 surgeons, with each surgeon implanting the screws on 1 side. Operations were performed by either 2 attending surgeons or 1 attending surgeon together with 1 resident surgeon. During the surgery, the perceived screw stability was graded by the respective surgeon for each screw. CT scan of lumbar spine in sagittal, axial, and coronal plane with measurement of pedicle screw length and thickness. Measurement of the BMD using QCT software. Bone density is measured in a given cube within the cancellous vertebral body.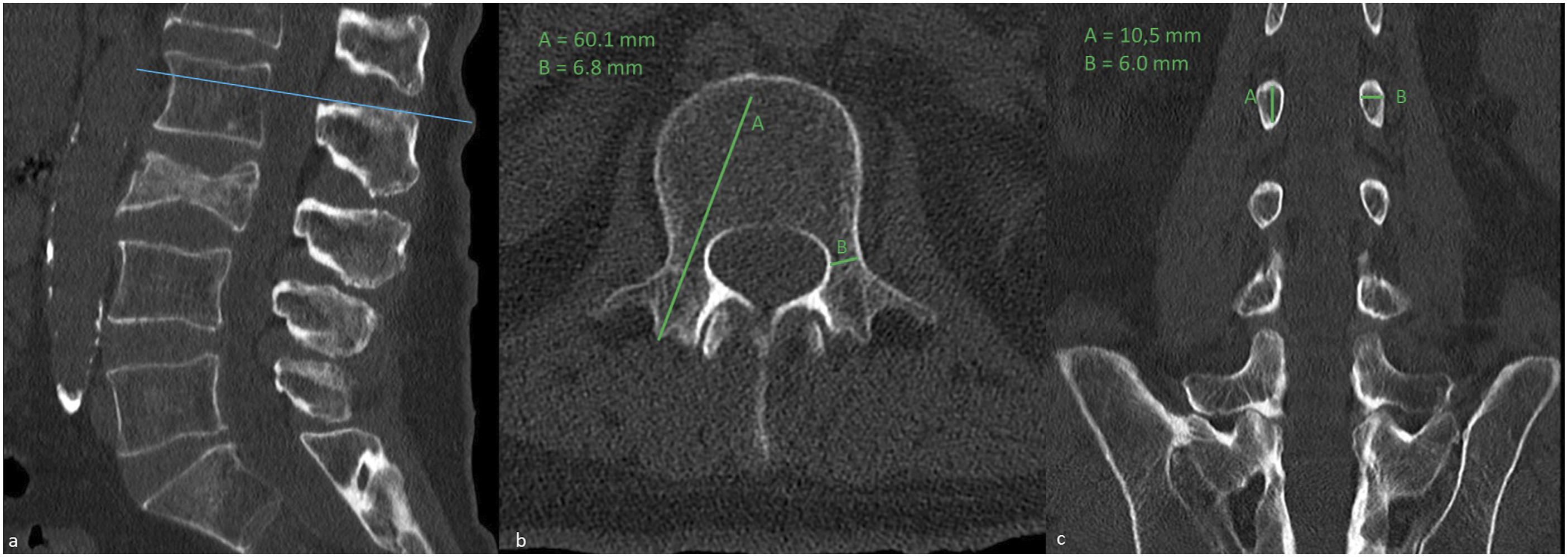

Thus, the respective instrumented pedicle was documented with the corresponding pedicle size and the respective grade for screw stability.
Statistics
For statistical analysis (SPSS, Version 21, IBM, Armonk, USA) the type I error probability was set to a = .05. A linear regression with stepwise reduction was performed to investigate the correlation between perceived screw strength and measured BMD as well as the influence of pedicle width, the difference between pedicle width and screw thickness and age on this analysis. All data is shown as mean value ± standard deviation.
Results
Patient Data and information Giving the Number of Included Patients and Implanted Screws Divided into Male and Female. Overview of Instrumented Spine Levels with Respective Number of Implanted Screws as Well as Age Distribution of the Included Patients.

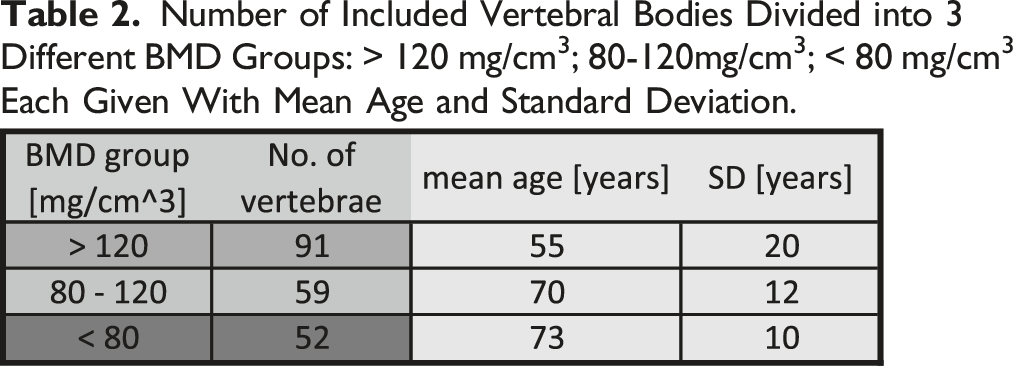
Number of Included Vertebral Bodies Divided into 3 Different BMD Groups: > 120 mg/cm3; 80-120mg/cm3; < 80 mg/cm3 Each Given With Mean Age and Standard Deviation.
There was a significant correlation between the measured bone density (QCT) and the age of the corresponding patient (r = -.507; R2 = .257; P < .001). When looking at all implanted screws, a significant correlation was found between the screw stability felt by the surgeons and the measured bone density (Resident r = .450; R2 = .202; P < .001/Attending r = .364; R2 = .133; P < .001). The difference between the pedicle width and the selected screw thickness was calculated and amounted to 1.28 mm (SD 1.8 mm). Linear regression analyses showed no significant influence of age, pedicle width or the difference between pedicle width and screw thickness on the coefficient of determination and therefore were omitted.
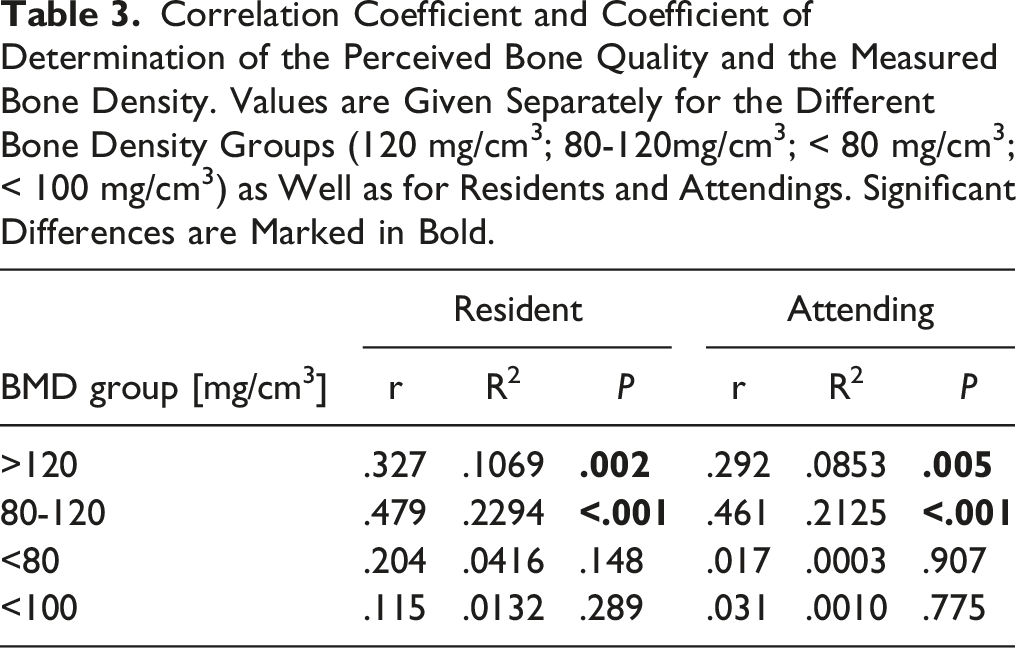
Correlation Coefficient and Coefficient of Determination of the Perceived Bone Quality and the Measured Bone Density. Values are Given Separately for the Different Bone Density Groups (120 mg/cm3; 80-120mg/cm3; < 80 mg/cm3; < 100 mg/cm3) as Well as for Residents and Attendings. Significant Differences are Marked in Bold.
Overview of the Perceived Screw Stability Given by Grade with the Respective Number of Vertebral Bodies for Residents and Attendings. The Associated Bone Mineral Density Range as Well as the Mean BMD with SD and the Number of Vertebral Bodies with a BMD Below < 80 mg/cm3 are Given for Each Selected Grade as Well as for Residents and Attendings Separately.
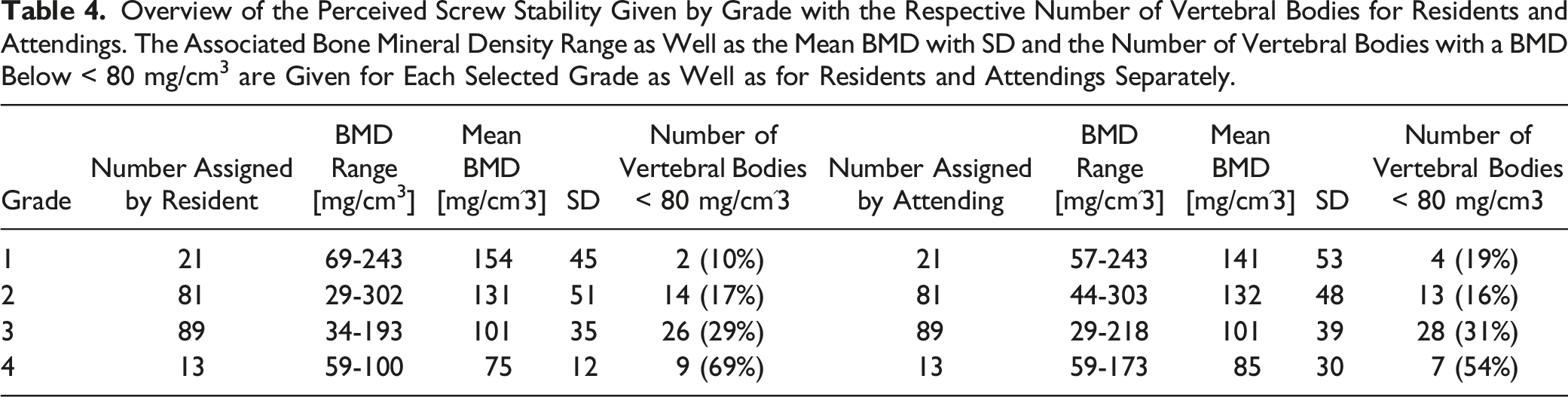
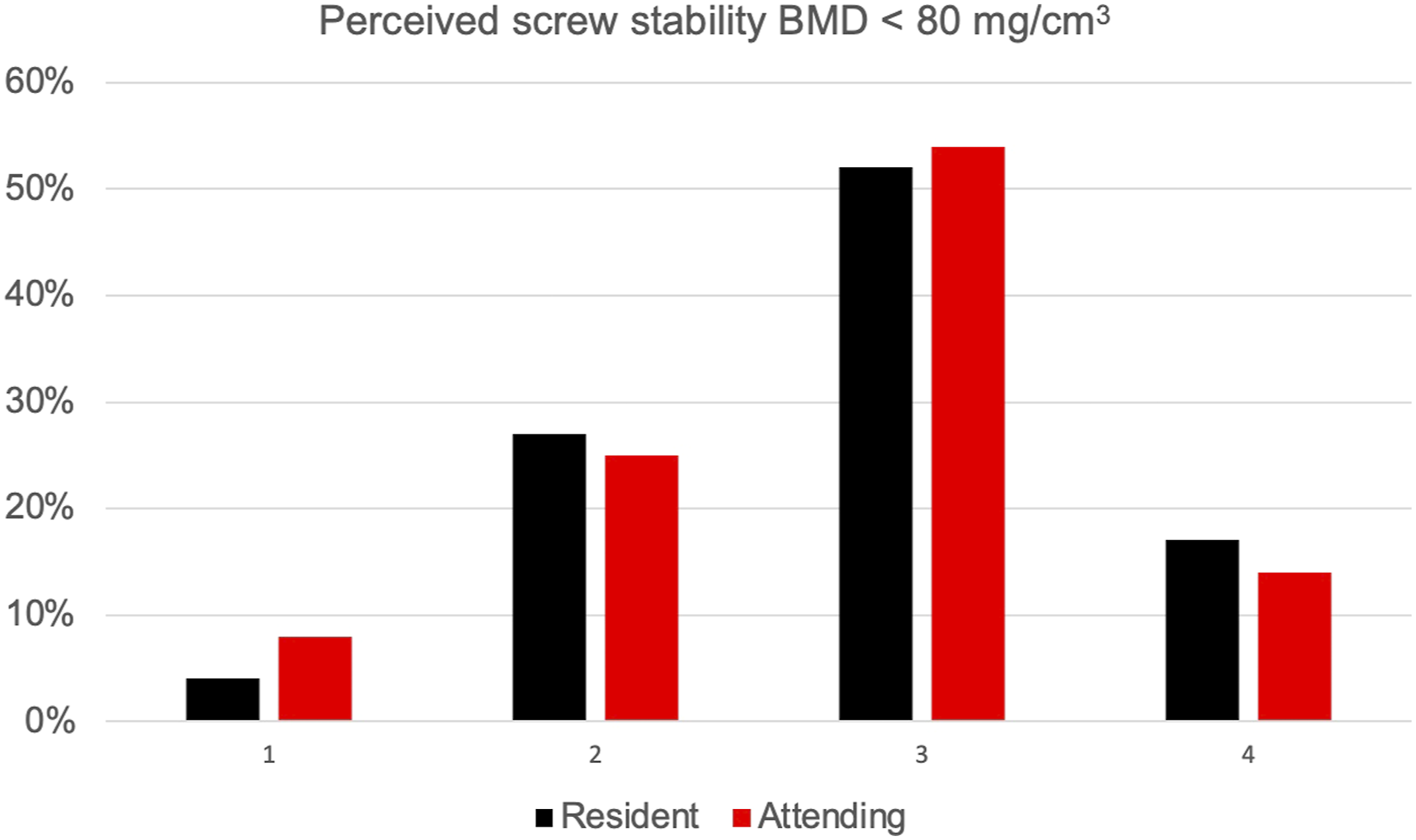
Diagram showing the perceived screw stability in patients with a BMD below 80 mg/cm3 given for residents (black) and attendings (red).
The routinely performed postoperative controls using conventional X-ray or CT did not reveal any screw misalignments requiring revision and no initial loosening of the pedicle screws.
Discussion
Loosening of pedicle screws is a common and relevant complication after posterior stabilization of the spine, especially in patients suffering from osteoporosis.5,6,17 Various factors that influence the stability of pedicle screws have been identified. On the 1 hand there are implant properties including diameter, length, and design of the screws, on the other there are patient specific factors such as pedicle width and bone quality. However, BMD is 1 of the most important factors. Several biomechanical studies have shown that there is a high correlation between pedicle screw stability and BMD.17,18
Augmentation of pedicle screws with bone cement is widely used to improve screw strength. Accordingly, clinical and biomechanical studies have indicated good results with increased screw stability after cement augmentation. 13 Hence, it can be recommended for patients with poor bone quality if the BMD is measured below 80-90 mg/cm³.7,9,18
Various studies have investigated the impact of screw augmentation with bone cement in osteoporotic bone. All were able to show a significant increase in pull-out strength with improved stability of the augmented pedicle screws compared to the non-augmented screws.19,20 In contrast, other studies also examined the effect of screw augmentation in specimen with normal bone mass. Wang et al. used the finite element analysis to show that there is a greater impact of cement augmentation on fixation strength of pedicle screws in osteoporotic bone. 21 Weiser et al. evaluated the influence of cement augmentation in samples with osteoporotic bone and with normal BMD. They showed that the benefit of cement augmentation decreased with an improved BMD. 15
By measuring the Hounsfield units in a preoperative CT scan, Bredow et al. demonstrated that calculation of the BMD can predict the risk of screw loosening. 22
Various complications associated with augmentation of pedicle screws have been noted. The incidence of accidental cement leakage is reported up to 94 %, but in most cases, it remains clinically asymptomatic. 23 Severe complications, such as pulmonary cement embolism, radicular compression symptoms and neurological deficits or anaphylactic reactions and hemodynamic complications, 16 are rare but have serious consequences for the patient. Due to these mentioned risks and because of the decreasing benefit of cement augmentation with increasing BMD, the indication for augmentation of pedicle screws should always be critically evaluated.
Nevertheless, in clinical routine surgeons often forego the preoperative bone density measurement. Many spine surgeons claim that they can feel the quality of the bone while inserting pedicle screws. Instead of a reliable measured BMD, surgeons evaluate bone quality by determining the amount of strength required to insert the pedicle screws. Thus, in many cases the indication for cement augmentation of pedicle screws is based on a subjective assessment of the surgeon.
Intraoperatively there is no possibility to reliably determine the quality of the bone so far. Mizuno et al. examined the correlation between insertion torque of the inserted screws and the BMD measured by QCT prior to surgery. 24 There was no significant correlation between the insertion torque and the stability of the pedicle screws. Lee et al. investigated the correlation between BMD (using DXA) and the magnitude of the torque which is required to insert the pedicle screws. 25 The authors were able to show a positive correlation between BMD and inserting torque and proposed the measurement of the insertion torque with a torque meter. Furthermore, the study by Popp et al. tested a device called DensiProbe Spine in patients with pedicle screw instrumentation. 26 The breakaway torque strength within the vertebral body was assessed intraoperatively by using the DensiProbe Spine. They proposed that the DensiProbe Spine might be a method to determine bone quality intraoperatively, but further studies are needed to verify these findings. However, none of these methods have been established so far. Yet, these results underline the importance of preoperative measurement of bone density.
The results of this study show a significant correlation between the measured BMD and the perceived screw stability (Resident / Attending) looking at all implanted screws (n = 408). Thus, at first sight, it seems to be possible to estimate the bone quality by inserting pedicle screws. However, when considering the different groups of bone densities, there is no significant correlation between the screw strength felt by the surgeon and the appraised BMD in the osteoporotic group (Resident P = .148 / Attending P = .907).
A separate analysis of the group with bone density below 100 mg/cm³ also demonstrates no significant correlation between the measured BMD and the perceived quality of the screw (Table 3). These findings already indicate that it seems to be impossible to reliably determine the bone quality in patients with reduced BMD.
A further examination of the screws implanted in vertebral bodies with a BMD below 80 mg/cm3 shows that the residents correctly evaluated 69 % and the attendings 68 % of these screws with a grade 3 or 4 (Table 4, Figure 3). Accordingly, this implies that more than 30 % of the implanted screws in vertebrae with osteoporotic bone were rated too good. Keeping in mind that pedicle screw augmentation is recommended in patients with osteoporotic bone (BMD below 80 – 90 mg/cm³), an error rate of more than 30 % means that a corresponding large number of patients might be treated insufficient with pedicle screws without cement augmentation. Furthermore, the present study shows that there is no relevant difference between the residents’ or the attendings’ assessment of screw stability. This conclusion conflicts with the widespread opinion of spine surgeons who claim that they can determine the bone quality due to their experience and therefore do not need the preoperative measured BMD.
Thus, our findings are in accordance with previous studies which also strongly recommend the preoperative measurement of BMD to assess the risk of screw loosening and to confirm the indication for cement augmentation.
Besides the already mentioned importance of preoperative measurement of the BMD, osteoporosis in general should become a priority in everyday surgical practice. Because vertebral body fractures are 1 of the most common osteoporotic fractures, spine surgeons should be responsible for initiating the osteoporosis diagnostic and therapy. After surgery, it is essential to ensure that patients with a fracture due to osteoporosis receive an appropriate osteoporosis therapy. Special programmes, such as a Fracture Liaison Service, might be useful to improve the quality of care for these patients.
In this study the BMD is measured using QCT, even though the guidelines for osteoporosis and its therapy recommendation are based on DXA-Scans. Some studies indicate a significant correlation between DXA and QCT, although the QCT examination is not equivalent to DXA. 27 Nevertheless, because of its greater availability in clinical routine, the present study used QCT to measure the BMD. As most patients with spinal diseases are examined with a CT scan before surgery, no extra examination is necessary to determine the bone density. Moreover, the QCT might be more precise because it is not so much affected by surrounding structures such as calcifications of the aorta, facet joint arthrosis or the patient’s weight.15,28,29 Regarding the measurement of BMD using QCT, a BMD between 80 – 120 mg/cm³ characterises osteopenia while a BMD below 80 mg/cm³ is defined as osteoporosis. 28
However, this clinical study has some potential limitations. Firstly, it is a monocentre study with a relatively small sample size. Secondly, the BMD is only measured using QCT. To receive more precise results, the measurements using both QCT and DXA-Scans could be compared in future studies. The operating surgeons were not blinded to the preoperative CT, so that the perceived bone density could have been falsified, since the surgeons could have been biased due to the CT. Furthermore, the evaluation of the surgeons could have been influenced by other factors such as the age of the patient, other patient-specific factors, or unrecognized breaching of the pedicle wall during screw implantation. There was no long-term follow-up with regard to any screw loosening that might occur, and there was no evaluation of any cement augmentation that might have been used. In addition to bone density, other aspects such as screw thickness, pedicle size and screw design are responsible for pedicle screw stability. In our investigation, there was no significant influence on the results in this regard, but these points should always be taken into account, since a change in stability can occur independently of the bone quality.
In summary, according to the results of this study, it is not possible to determine bone quality reliably while inserting pedicle screws, especially in case of reduced bone quality. However, the decision for cement augmentation depends on the bone density. Therefore, the preoperative measurement of the BMD, for example using QCT, and its establishment as a standard procedure should become an essential part of preoperative planning to verify the indication for cement augmentation and thereby prevent the risk of screw loosening.
Footnotes
Acknowledgment
The authors thank Majd Hamdoun for assistance in collecting the data for the study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.