Abstract

Keywords
Citation: Devereaux PJ, Marcucci M, Painter TW, et al; POISE-3 Investigators. Tranexamic Acid in Patients Undergoing Noncardiac Surgery. N Engl J Med. 2022 May 26;386(21):1986-1997.
Visual Abstract
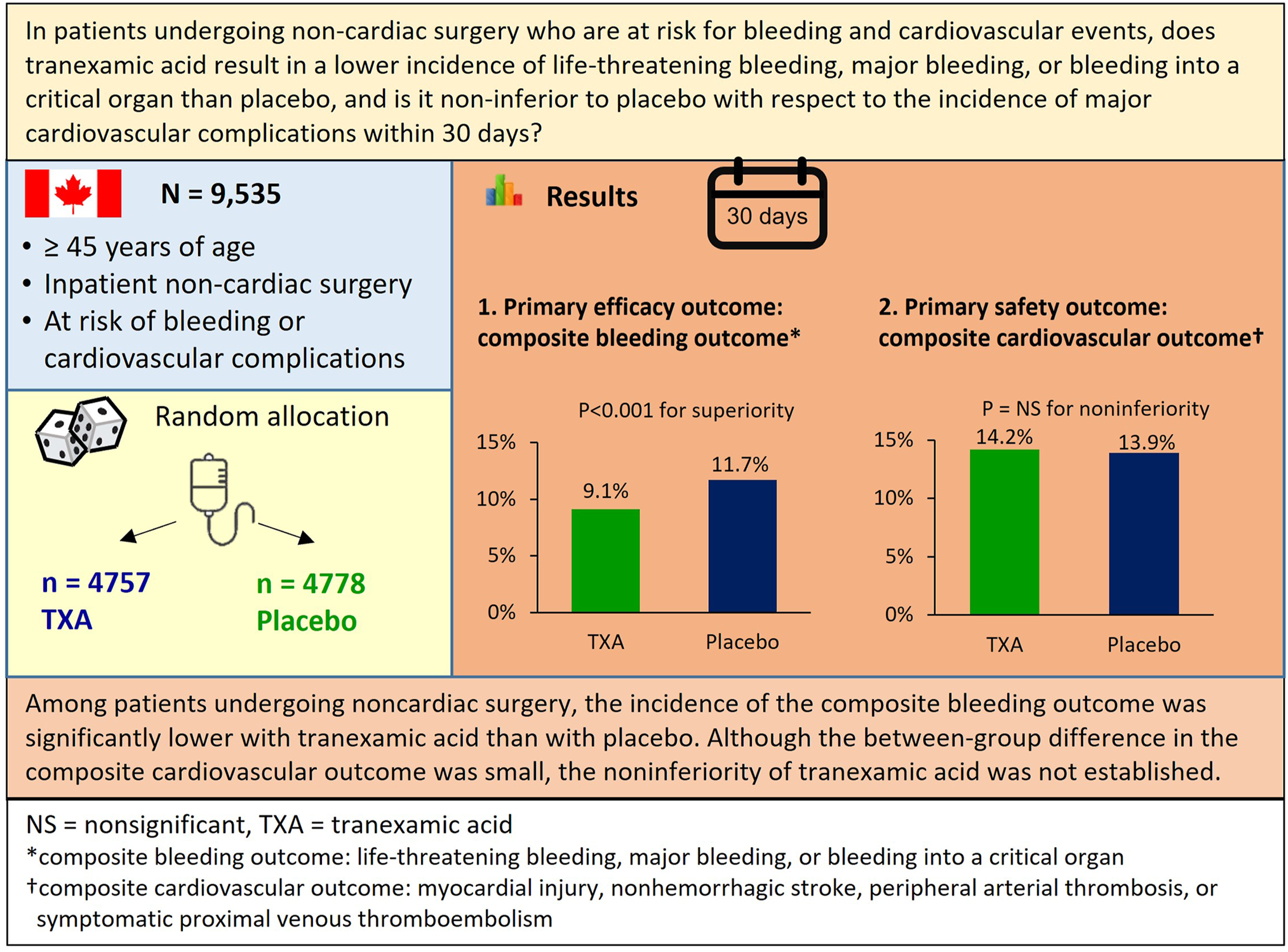
Why is This Study an Important Topic?
In non-cardiac surgeries, perioperative bleeding can lead to serious complications including death. Tranexamic acid is used to reduce bleeding during non-cardiac surgery. However, there is limited evidence of its effectiveness and safety in non-cardiac surgery such as spinal and orthopedic procedures. This study aimed to determine whether tranexamic acid can provide a reduction in bleeding events with a level of safety that is non-inferior to placebo in patients undergoing non-cardiac surgery.
What are the Primary Clinical Questions?
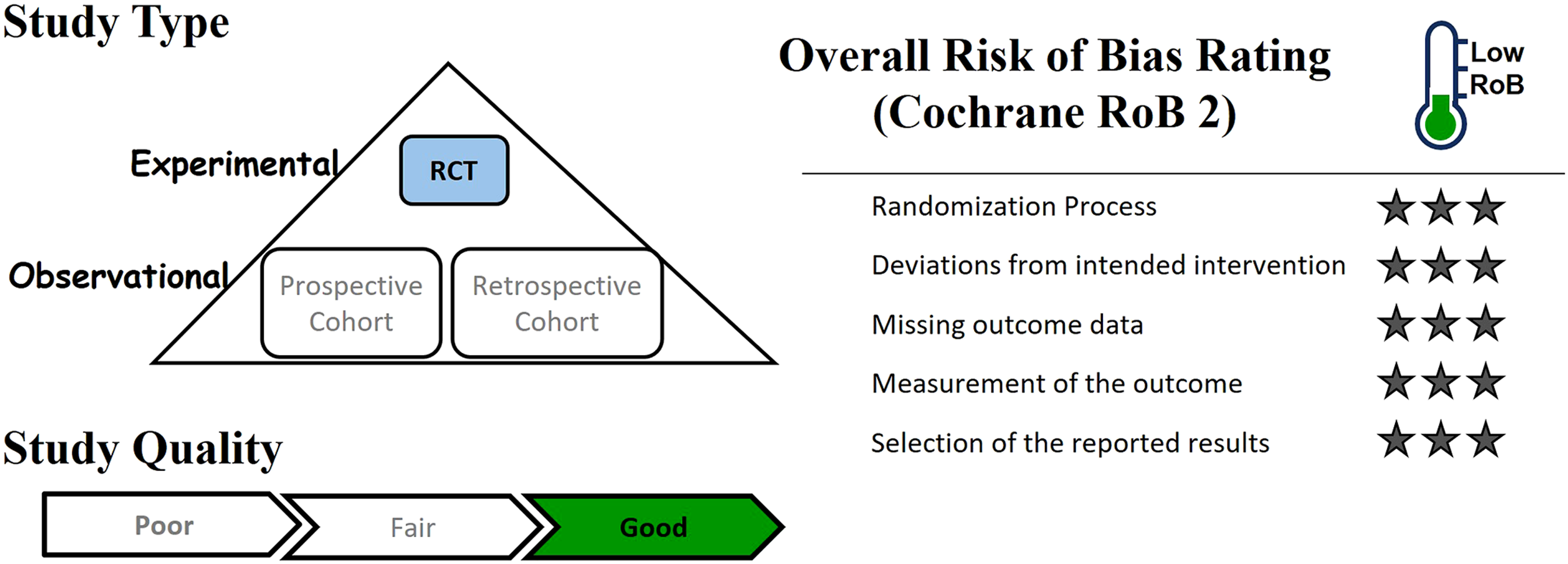
In patients undergoing non-cardiac surgery who are at risk for bleeding and cardiovascular events, does tranexamic acid result in a lower incidence of life-threatening bleeding, major bleeding, or bleeding into a critical organ than placebo, and is it non-inferior to placebo with respect to the incidence of major cardiovascular complications within 30 days?
Study Characteristics
Population:
Male (56%) and female (44%) adults, mean age 69years following non-cardiac surgery and at risk for bleeding or cardiovascular complications.
Intervention:
Tranexamic acid, 1-g intravenous bolus at the start and end of surgery.
Control:
Placebo administration at the start and end of surgery.
Outcomes:
Time:
Within 30days
Results
Result 1. Percent of an Event (A) and Kaplan-Meier Estimates (B) of Primary Efficacy Outcome (Composite Bleeding)
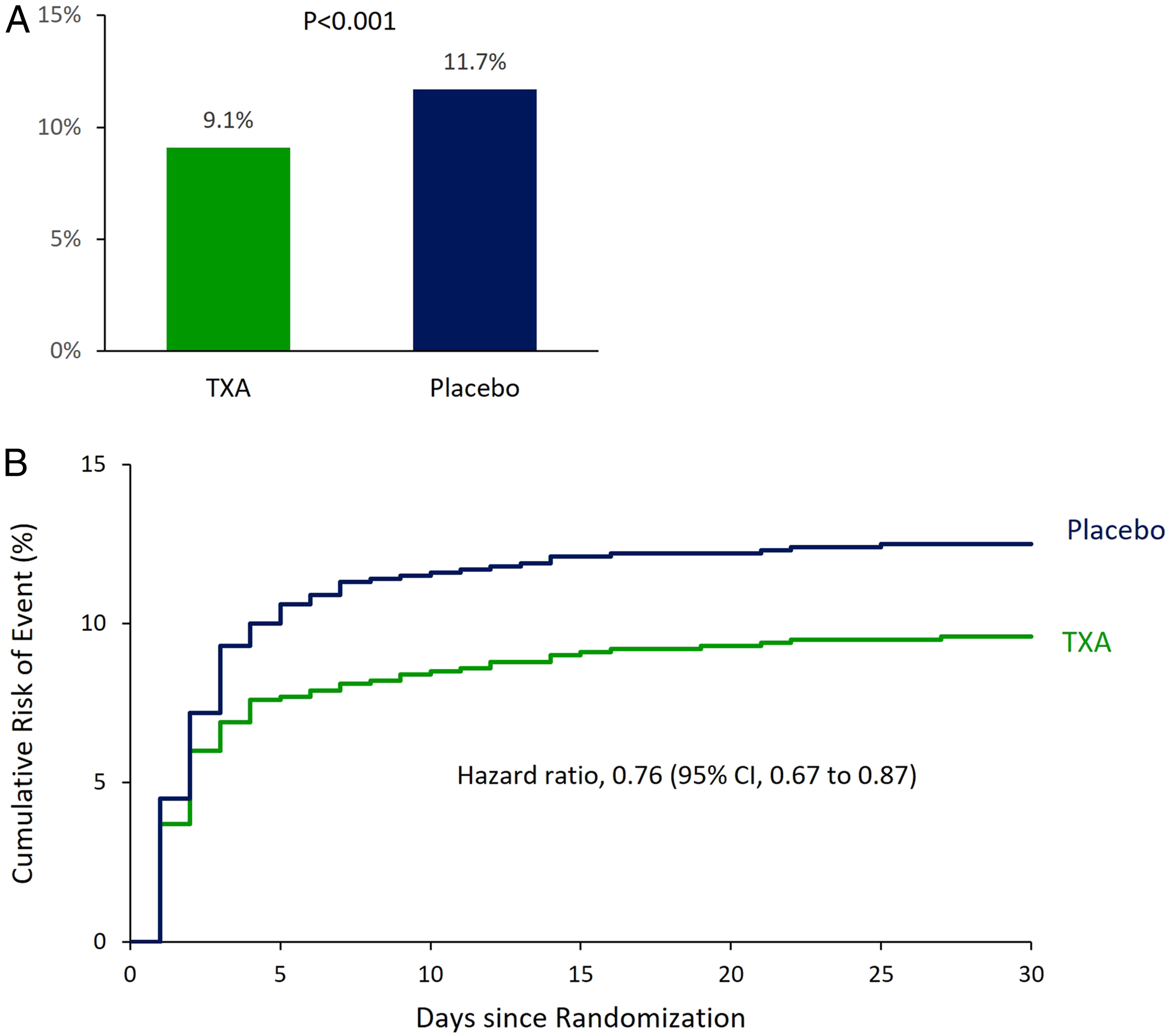
Result 2. Percent of an Event (A) and Kaplan-Meier Estimates (B) of Primary Safety Outcome (Composite Cardiovascular)
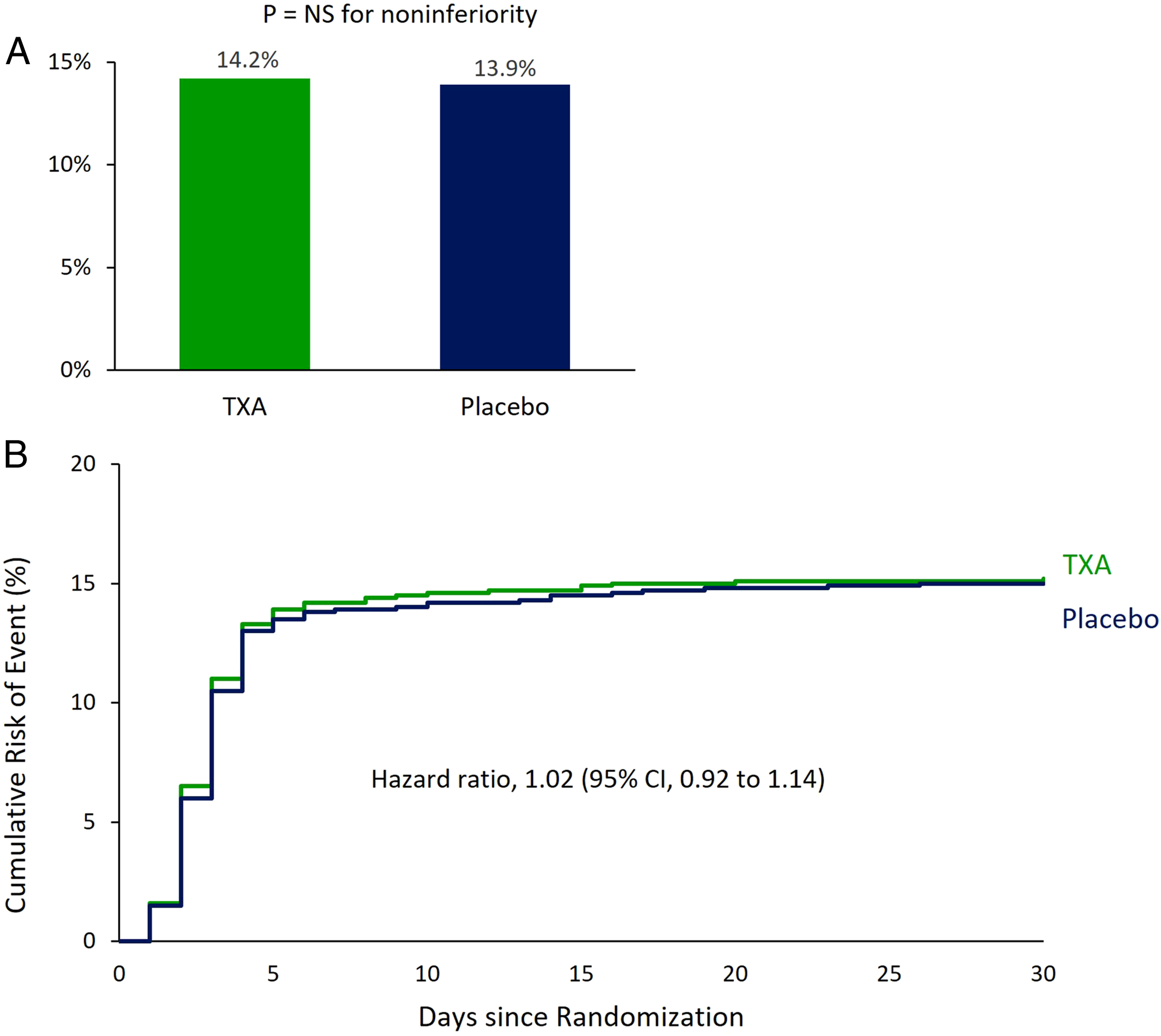
How Will This affect the Care of My Patients?
Among patients undergoing non-cardiac surgery, the incidence of the composite bleeding outcome was significantly lower with tranexamic acid compared with placebo (absolute difference, −2.6 percentage points; 95% CI, −3.8 to −1.4). Although the difference between groups in the composite cardiovascular outcome was small, the noninferiority of tranexamic acid was not established (absolute difference, .3 percentage points; 95% CI, −1.1 to 1.7). Health care providers and patients will have to weigh the beneficial reduction in the incidence of composite bleeding outcome events against the low probability of a small increase in the incidence of composite cardiovascular outcome events.
