Abstract
Objective
A systematic review and meta-analysis was conducted to explore the efficacy of tranexamic acid (TXA) in reducing transfusion events in patients undergoing percutaneous nephrolithotomy (PCNL).
Methods
PubMed, Web of Science, Embase, EBSCO, and Cochrane library databases from January 1980 to October 2019 were searched for randomized controlled trials (RCTs) that assessed TXA efficacy in reducing transfusion events during PCNL. Intervention treatments include using TXA compared with placebo (or no intervention) for patients who underwent PCNL. The search strategy and study selection process were managed in accordance with the PRISMA statement.
Results
Six RCTs are included in the meta-analysis. Overall, TXA intervention groups showed a significant reduction in blood transfusion events (RR = 0.34; 95% confidence interval [CI] = 0.19 to 0.62), hemoglobin decrease (MD = −0.80; 95% CI = −1.32 to −0.28), operative time (MD = −12.62; 95% CI = −15.62 to −9.61), and length of hospital stay (MD = −0.73; 95% CI = −1.36 to −0.10) compared with control groups after PCNL. However, TXA had no substantial impact on the rate of stone clearance (RR = 1.10; 95% CI = 1.00 to 1.21).
Conclusions
TXA can effectively reduce the transfusion rate and blood loss during PCNL.
Keywords
Introduction
Urinary stone disease is a highly prevalent disease worldwide. It is also the third most common disease, closely following infections and prostate disease in the urinary tract. 1 Compared with flexible ureteroscopy, shock wave lithotripsy, and other alternative choices, percutaneous nephrolithotomy (PCNL) is the best choice to treat bulky urinary stones because of its cost-effectiveness, higher stone clearance rate, and lower resulting morbidity.2,3 Although the efficacy and safety of PCNL have been confirmed in previous studies, complications may still occur. 4 Establishment of access to the renal collection system and lithotripsy are two critical steps in this procedure. However, this system is surrounded by a high-flow arteriovenous network, which accounts for 20% of the cardiac output, in terms of anatomy. 5 Thus, during puncture, dilation, and lithotripsy processes, trauma to this vascular network might lead to serious bleeding. 6 Based on previous studies, 3% to 23% of patients with this significant complication need a blood transfusion. 7 Blood transfusions cause a heavy economic burden and are associated with other risks including coagulopathy, hemolysis reaction, acute lung injury, mis-transfusion, non-immune hemolysis, and blood transfusion-related infections. 8 Therefore, prevention of post-surgical bleeding to reduce blood transfusion rates has become a current hot topic.
Tissue plasminogen activator, which converts plasminogen to the fibrinolytic enzyme plasmin plays an important role during the surgical bleeding process.9,10 Tranexamic acid (TXA) is an antifibrinolytic derivative of the amino acid lysine that acts by binding to plasminogen and blockers the interaction between plasmin and fibrin, thereby preventing fibrin clot dissolution. Specifically, it inhibits plasminogen by blocking the lysine binding sites in the Kringle domain.11,12 TXA is effective in reducing postoperative blood transfusion in surgery, which has been known for many years; this was validated by Ker et al. 13 In their study, a systematic review of seven types of surgery (cardiac, orthopedic, urological, vascular, gynecological, cranial, and orthognathic) with 129 trials from 1972 to 2011 was conducted, and they showed that TXA administration can significantly reduce the rates of blood transfusion by one-third (RR = 0.62, 95% CI = 0.58–0.65; p < 0.001) and mortality from surgical bleeding by a similar proportion (RR = 0.61, CI = 0.38–0.98; p = 0.04). 9 However, when trials that used adequate concealment were assessed in that review, the impact of TXA became unclear (RR = 0.67, CI = 0.33–1.34). Additionally, only two studies about urological surgery were included their report. More recently, Mina et al. 14 and Longo et al. 15 reported that TXA significantly reduced bleeding in prostate surgery in their respective meta-analyses. The high plasminogen concentration contained in urine and in the urothelium is beneficial for destroying blood clots. 16 Consequentially, this increases urinary fibrinolysis, which is often associated with postoperative bleeding in urology surgery. 17 However, TXA can disrupt fibrinolysis, thereby reducing bleeding and rates of transfusion. 14 Similarly, TXA significantly reduced bleeding and transfusion rates in PCNL. Such results have also been reported in other recent studies.
To date, there is a lack of high-level evidence available, supporting the need for this systematic review and meta-analysis. We anticipate that our results may support future routine use of TXA for PCNL.
Materials and methods
The systematic review and meta-analysis were performed based the Preferred Reporting Items for Systematic Reviews and Meta-analysis (PRISMA) statement and the Cochrane Handbook for Systematic Reviews of Interventions. No ethical approval and patient consent were required because all analyses were performed using data from previously published studies.
Literature search and selection criteria
We systematically searched several databases including PubMed, Embase, Web of Science, EBSCO, and the Cochrane library from January 1980 to October 2019 using the following keywords: tranexamic acid, hemostatic, blood loss, stone, and percutaneous nephrolithotomy. The reference lists of retrieved studies and relevant reviews were also hand-searched and the process above was performed repeatedly to include additional eligible studies.
The inclusion criteria are presented as follows: (1) study design is an RCT; (2) intervention treatment was TXA compared with placebo (or no intervention) for patients who underwent PCNL; (3) adequate reported data for analysis were provided; and (4) all languages were included (translated into English if necessary).
Data extraction and outcome measures
Some baseline information was extracted from the original studies, including name of first author, published year, number of patients, age, gender, description of the urinary stone, and detailed methods of intervention in each group. Data were extracted independently by two investigators. If the extracted data (mainly for data estimation of missing data, data merging, and data exclusion) were different, the data in question were jointly reassessed, and the final decisions were determined by all authors during a meeting.
The primary outcome was the number of patients receiving a blood transfusion. Secondary outcomes included hemoglobin difference, operative time, average length of hospital stay, and stone clearance.
Quality assessment in individual studies
The methodological quality of each RCT was assessed using the Jadad Scale. 18 An article with a total Jadad score that is less than or equal to 2 is considered to be of low quality. A study is thought to be of high quality if its total Jadad score greater than or equal to 3. 18 Only high-quality studies were included in the current meta-analysis.
Statistical analysis
We assessed standard mean differences (Std. MDs) using 95% confidence intervals (CIs) for continuous outcomes and relative risk (RR) with 95% CIs for dichotomous outcomes. Heterogeneity was evaluated using the I2 statistic, and I2 > 50% indicates significant heterogeneity. 19 A sensitivity analysis was performed to detect the influence of a single study on the overall estimate via omitting each study in turn or performing subgroup analysis. The random-effects model was used for all meta-analyses. Because of the limited number of included studies (<10), publication bias was not assessed. Results were considered to be statistically significant at P < 0.05. All statistical analyses were performed using Review Manager Version 5.3 (Copenhagen: The Nordic Cochrane Centre, The Cochrane Collaboration, 2014).
Results
Literature search, study characteristics and quality assessment
Overall, 373 articles were initially identified in the databases. After removing duplicates, 202 articles were retained. Then, 193 studies were excluded from our study after checking the abstracts and titles. Three articles were also excluded from our analysis because of their study design (not RCT). Finally, six RCTs that satisfied the inclusion criteria were included in this meta-analysis.20–25 The article selection process was completed in accordance with the PRISMA statement (Figure 1).

Flow diagram of the study search and selection process.
The baseline characteristics of the six RCT studies are shown in Table 1. These studies were published between 2013 and 2019, and the total sample size is 965. Patients from all studies received 1 g of TXA before surgery or at anesthesia induction. Kumar et al. 20 administered three 500-mg doses of TXA orally every 8 hours while Cauni et al. 23 used the same dose regimen, but repeated it every 12 hours post-surgery. Sichani et al. 25 administered 1 g of TXA at the start of the procedure followed by 1 g of TXA every 8 hours for the first 48 hours. All six of the included RCTs reported blood transfusion events, but data from only three of the RCTs was adequate to determine the change in hemoglobin (Hb).20,21,25 Four RCTs reported the length of hospital stay and operative time.20,21,23,25 Two RCTs reported stone clearance.20,21
Characteristics of the included studies.

a, mean±SD; b, mean, IQR; c, number of patients with Staghorn stones (n), mean ± SD of the stone surface area (cm2); d, Stone size (cm) mean, IQR. TXA, tranexamic acid, IQR, interquartile range; SD, standard deviation
Jadad scores for five of the studies varied from 3 to 5, and all six studies were high-quality RCTs based on the quality assessment.
Primary outcome: Blood transfusion
A random-effects model was used for the primary outcome analysis. The results indicated that compared with the control group, TXA administered to patients in the intervention group significantly reduced the need for blood transfusion (RR = 0.34; 95% CI = 0.19 to 0.62; P = 0.0004), and heterogeneity among the studies was insignificant (I2 = 19%, Figure 2).

Forest plot for the meta-analysis of blood transfusion events.
Secondary outcomes: Hb decrease, operative time, length of hospital stay, and stone clearance rate
Compared with the control intervention after percutaneous nephrolithotomy, TXA was associated with a decrease in Hb levels (MD = −0.80; 95% CI = −1.32 to −0.28; P = 0.002; Figure 3), operative time (MD = −12.62; 95% CI = −15.62 to −9.61; P < 0.00001; Figure 4), and length of hospital stay (MD = −0.73; 95% CI = −1.36 to −0.10; P = 0.002; Figure 5), but it had no substantial impact on the stone clearance rate (RR = 1.10; 95% CI = 1.00 to 1.21; Figure 6).
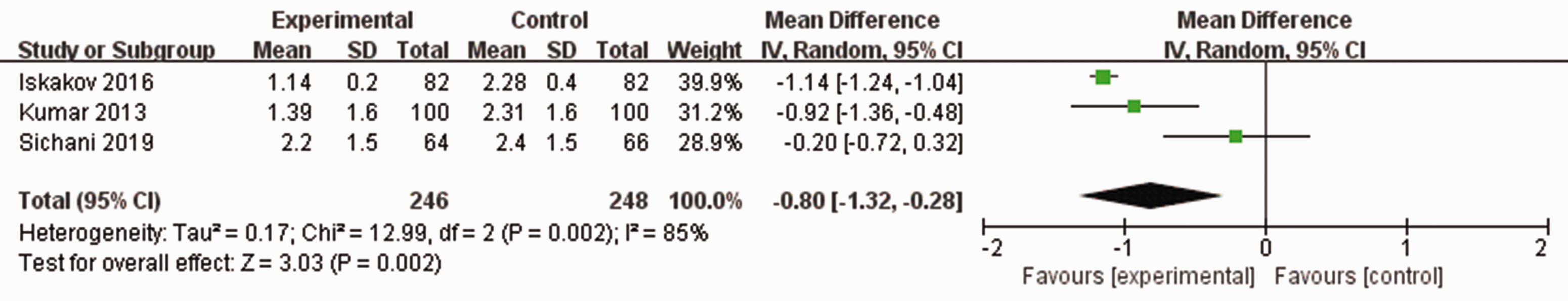
Forest plot for the meta-analysis of Hb difference.

Forest plot for the meta-analysis of operative time.

Forest plot for the meta-analysis of length of hospital stay.

Forest plot for the meta-analysis of stone clearance.
Sensitivity analysis
There was no significant heterogeneity in the primary outcome. Among all secondary outcomes, length of hospital stay showed significant heterogeneity (I2 = 99%, P < 0.00001). A sensitivity analysis was performed to evaluate the stability of the results. After removing one study at a time, the heterogeneity was I2 = 95%, 99%, 99%, and 95%, which indicates that the heterogeneity was stable. Difference in Hb levels also showed significant heterogeneity (I2 = 85%, P = 0.002). After removing the study by Sichani et al., 25 the heterogeneity was I2 = 0%, which was not significant.
Discussion
PCNL is considered the gold standard for removal of large upper urinary tract stones. Because of technical improvements, much progress has been made in this procedure, but many complications still occur.4,26 Among them, hemorrhage is the most common complication that usually requires blood transfusion and angiographic embolization after conservative treatment fails. 27 Severe damage such as renal failure, myocardial infarction, and cerebral ischemia may be caused by uncontrollable blood loss. Additionally, surgical morbidity and mortality will be significantly improved.27,28 Many modifications have been extensively investigated to determine a non-surgical and inexpensive way to control excessive hemorrhage. 25 TXA has been widely used in many types of surgeries such as orthopedic; cardiac; cranial; hepatic; ear, nose, and throat; and gynecological surgery, where it was shown to be safe and effective in several studies.29,30 Its clinical effectiveness was also shown by significantly reducing the intensity of intraoperative bleeding.29,30 Kumar et al. 20 first reported that TXA is well tolerated and associated with reduced blood loss and fewer complications in PCNL. However, these findings are in contrast to another recent study. Sichani et al. 25 showed that TXA is not associated with a significant reduction in blood loss. Therefore, we conducted this systematic review and meta-analysis of RCTs to determine the efficacy of TXA in PCNL surgery.
In our study, blood transfusions were given to 4.4-fold more patients in the control group compared with the TXA group. TXA administration can, therefore, reduce the transfusion rates significantly (2.7% vs. 11.5%). A previous study indicated that the need of blood transfusion during PCNL is approximately 10%. 21 This result shows that TXA has a positive effect on reducing the blood transfusion rate during PCNL. In practice, the transfusion threshold level must also be taken into consideration. Typically, this is dependent upon the decisions made by different surgeons and the individual patient’s condition. It is unfortunate that the transfusion thresholds are not reported in all five studies.
Although only two studies provided adequate data about the Hb measurements for analysis in our systematic review, Hb differences following surgery have been characterized in other studies. Siddiq et al. 22 reported a change in Hb of 1.6 (interquartile range [IQR], 4) in the placebo group 1.3 (IQR, 7.8) in the TXA group (P < 0.05), and Cauni et al. 23 reported that Hb was 1.1 in the TXA group compared with. 2.3 in the control group (P < 0.05). Using TXA, the decrease in Hb can be significant, which is the main reason that TXA radically reduces the rate of blood transfusion after PCNL in patients.
In the current study, the use of TXA was also associated with a reduction in the average operative time and length of hospital stay. Reduced bleeding leads to better intraoperative visualization and a shorter duration of irrigating fluid use. Thus, TXA could help to achieve a shorter mean operative time. 15 However, studies by Iskakov et al. 21 and Siddiq et al. 22 showed no significant difference in the length of hospital stay. This might be because surgeons often adhere to constant time limits for removing nephrostomy tubes and urinary catheters to avoid additional complications. However, in clinical practice, fewer complications that result from a lower volume of blood loss is reflected in the length of hospital stay. Different discharge thresholds may account for the high heterogeneity of the outcome.
Finally, stone clearance was not different based on our results. However, poor visibility when there is bleeding might increase the risks and difficulties of the PCNL procedure. Severe bleeding can even lead to termination of the procedure. However, we suggest that the stone clearance rate is a particularly complex indicator that is influenced by many factors such as the size of the stone, the location of the puncture, and the skill of the surgeon. Thus, the effect on stone clearance rate using TXA remains unclear.
To the best of our knowledge, our study is the first systematic review and meta-analysis to investigate the effectiveness of TXA in reducing the rate of blood transfusion in PCNL. However, there are some limitations in our study. First, the data on adverse effects that are associated with the intervention are not sufficient for analysis. Second, the bias introduced by differences in the stone size, access for puncture, method of dilatation, and ectopic vessels that can cause unpredictable bleeding during the procedure requires future studies. Finally, there are some unpublished data and missing negative data in the original RCT reports, and because of this publication bias, the accuracy of our summary may be skewed.
In conclusion, TXA can reduce the need for transfusion and blood loss in PCNL. Because of the limitation of a small number of studies and incomplete outcome measures, more clinical trials with a large number of patients are required in future research.
Footnotes
Research involving human participants and/or animals
Not applicable.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
