Abstract
Study Design
Retrospective Cohort Study
Objectives
Postoperative ileus (POI) is a common complication following elective spinal surgeries. The aim of this study was to determine the incidence of POI and identify demographic and surgical risk factors for developing POI after elective instrumented fusion of the thoracolumbar spine.
Methods
The University of Utah Institutional Review Board (IRB) approved this retrospective study. The study does not require informed consent given the data reviewed was deidentified and collected in accordance with the institution’s standard of care. A designated IRB committee determined that study is exempt under exemption category 7. IRB approval number 00069703. Patients undergoing instrumented thoracolumbar fusion for one or more levels were retrospectively identified from an internal spine surgery database. Cases performed for trauma, infection, or tumors were excluded. Demographics, medical comorbidities, surgical variables, and opioid medication administration (morphine milligram equivalents, MME) were abstracted from the electronic medical record. Univariate analysis was used to identify variables associated with POI. These variables were then tested for independent association with POI using multivariate logistic regression.
Results
418 patients were included in the current study. The incidence of POI was 9.3% in this cohort. There was no significant relationship between development of POI and patient age, gender, BMI, diabetes mellitus, thyroid dysfunction, lung disease, CKD, GERD, smoking status, alcohol abuse, anemia, or prior abdominal surgery. Univariate analysis demonstrated significant association between POI and fusion ≥7 levels compared to fusions of fewer levels (P = .001), as well as intraoperative sufentanil compared to other opioids (35.9% vs 20.1%, P = .02). POI was not significantly associated with total intraoperative MME, approach, use of interbody cage, or osteotomy. Multivariate logistic regression confirmed total 24-hour postoperative MME as an independent risk factor for POI (OR 1.004, P = .04), however, intraoperative sufentanil administration was not an independent risk factor for POI when controlling for other variables.
Conclusions
This retrospective cohort study demonstrates that greater postoperative MME is an independent risk factor for POI after thoracolumbar spine fusion when accounting for demographic, medical, and surgical variables with multiple logistic regression. Prospective studies are warranted to evaluate clinical measures to decrease the risk of POI among patients undergoing instrumented thoracolumbar spinal fusions.
Introduction
Postoperative ileus (POI) is a transient loss of coordinated bowel motility after surgical intervention, 1 which can result in abdominal distension, pain, nausea and vomiting, delayed passage of flatus and stool, and an inability to tolerate oral intake.2,3 The estimated incidence of POI after spine surgery has varied widely in the literature, with reported rates of 1.9%–23.1%.4-9 POI is one of the most common reasons for delayed hospital discharge and is associated with significantly longer length of stay (LOS), higher hospitalization costs and hospital readmission rates, and may place patients at increased risk of developing deep venous thrombosis, myocardial infarction, sepsis, and aspiration pneumonia.1,4-6,10,11 Despite the considerable amount of published research related to POI, the pathogenesis, risk factors, and treatment strategies still remain incompletely understood. This represents a potential area for quality improvement, including clinical care algorithms for risk reduction and management of patients with ileus after undergoing spine surgery.5,7,12-15 Several factors have been linked to increased risk of postoperative ileus among patients undergoing spine surgery, including male gender, chronic constipation, electrolyte disorders and postoperative fluid imbalances, history of gastroesophageal reflux disease (GERD), history of alcohol abuse, and the type of spine surgery performed.4,9,12
Although the effect of opioid medications upon GI motility is well understood,16-18 there are, interestingly, few studies in the spine literature evaluating the association of peri-operative opioid consumption with development of POI.6,12 The purpose of this study was to determine the postoperative incidence of POI and identify potential risk factors for developing POI in patients undergoing instrumented posterior fusion in the thoracic and/or lumbar spine; in particular we aimed to evaluate the association between intra- and postoperative opioid administration with the development of POI after spine surgery.
Methods
The University of Utah Institutional Review Board (IRB) approved this retrospective study. The study does not require informed consent given the data reviewed was deidentified and collected in accordance with the institution’s standard of care. A designated IRB committee determined that study is exempt under exemption category 7. IRB approval number 00069703. Patients who underwent instrumented posterior arthrodesis of one or more thoracic or lumbar vertebral levels between January 1, 2017 and August 31, 2019 were eligible for inclusion. Surgeries were performed by one of four attending spine surgeons at a single academic institution. Patients were excluded if they underwent surgery for trauma, tumor, or infection. Surgeries were performed as open posterior instrumented posterolateral fusions with bilateral pedicle screw fixation at each level with very few exceptions using local autograft and allograft material placed in the posterolateral gutters.
Demographics and Comparison Between Groups.
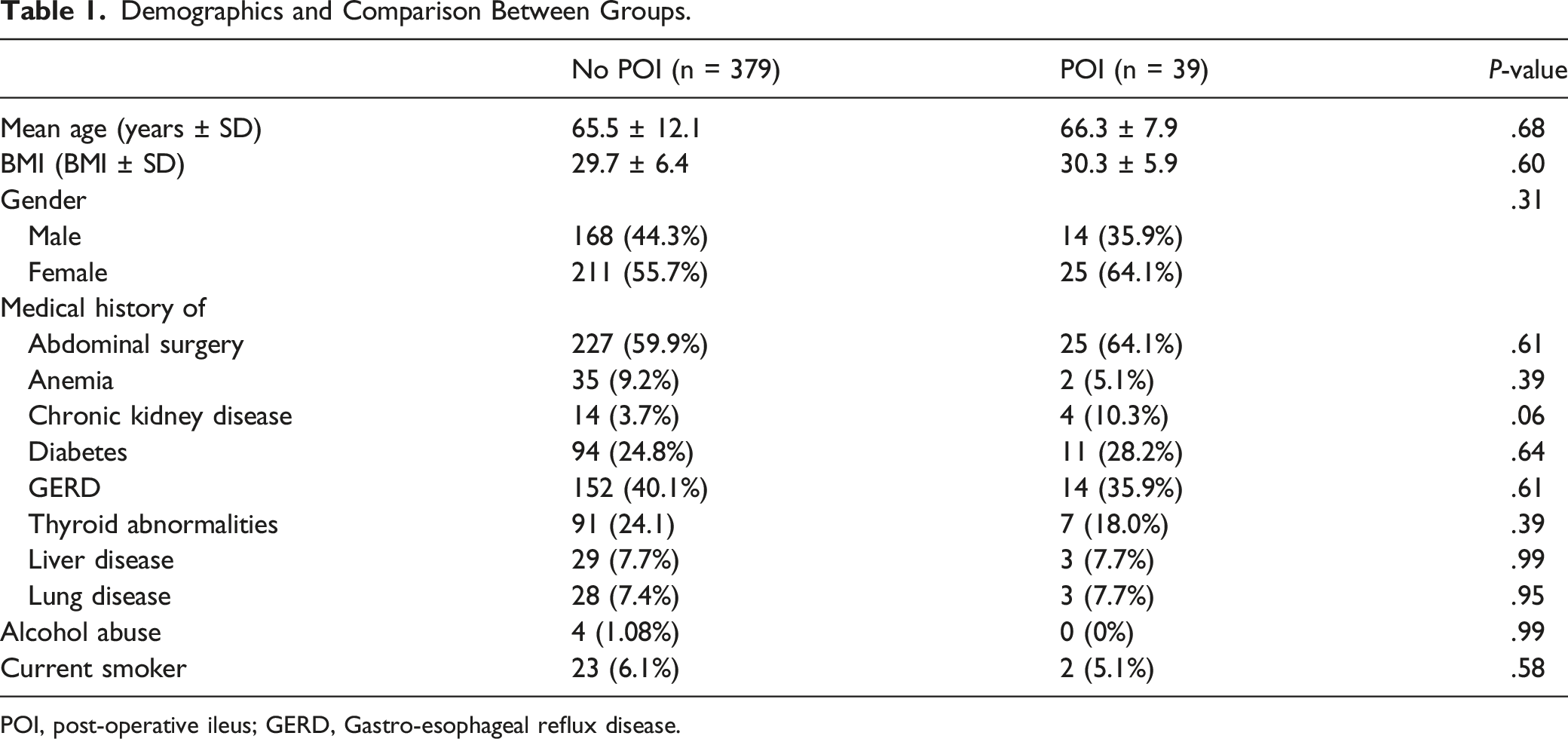
POI, post-operative ileus; GERD, Gastro-esophageal reflux disease.
Postoperative pain control consisted of scheduled Tylenol and omeprazole, and had as-needed oral and intravenous opioid medications. Patients were mobilized with a physical therapist on the day of surgery or the first day after surgery. Post-operative bowel regimen began on the day of surgery, and included scheduled daily doses of sennosides-docusate sodium, magnesium hydroxide, polyethylene glycol, in addition to as needed naloxegol, bisacodyl suppository, or mineral oil enema.
The primary outcome measure was the development of POI, which patients were considered to have if they developed at least two of the following symptoms: abdominal pain, distension or bloating, nausea or vomiting, absence of passing flatus or stool, or an inability to tolerate oral intake at any point after the completion of surgery. This determination was made on careful review of each patient’s records, in addition to a review of abdominal x-rays obtained postoperatively to ensure there was no obstruction.
Statistical analyses consisted of univariate analyses using Student t-tests for continuous variables and Chi-square for categorical variables. If the given variable was sparse in any cell (≤5 cases) a Fisher Exact test was used. A P-value < .05 was considered significant for all analyses. Multivariate logistic regression analysis was then performed for all variables found to be significant in the univariate analysis.
Results
A total of 418 patients met inclusion criteria and were included in analyses. Of these, 39 patients (9.3%) developed POI. There was no statistically significant difference in age, gender, BMI, diabetes, thyroid dysfunction, lung disease, CKD, GERD, smoking status, alcohol abuse, anemia or history of prior abdominal surgery between POI and no POI groups (Table 1).
Surgical Factors and Comparison Between Groups.
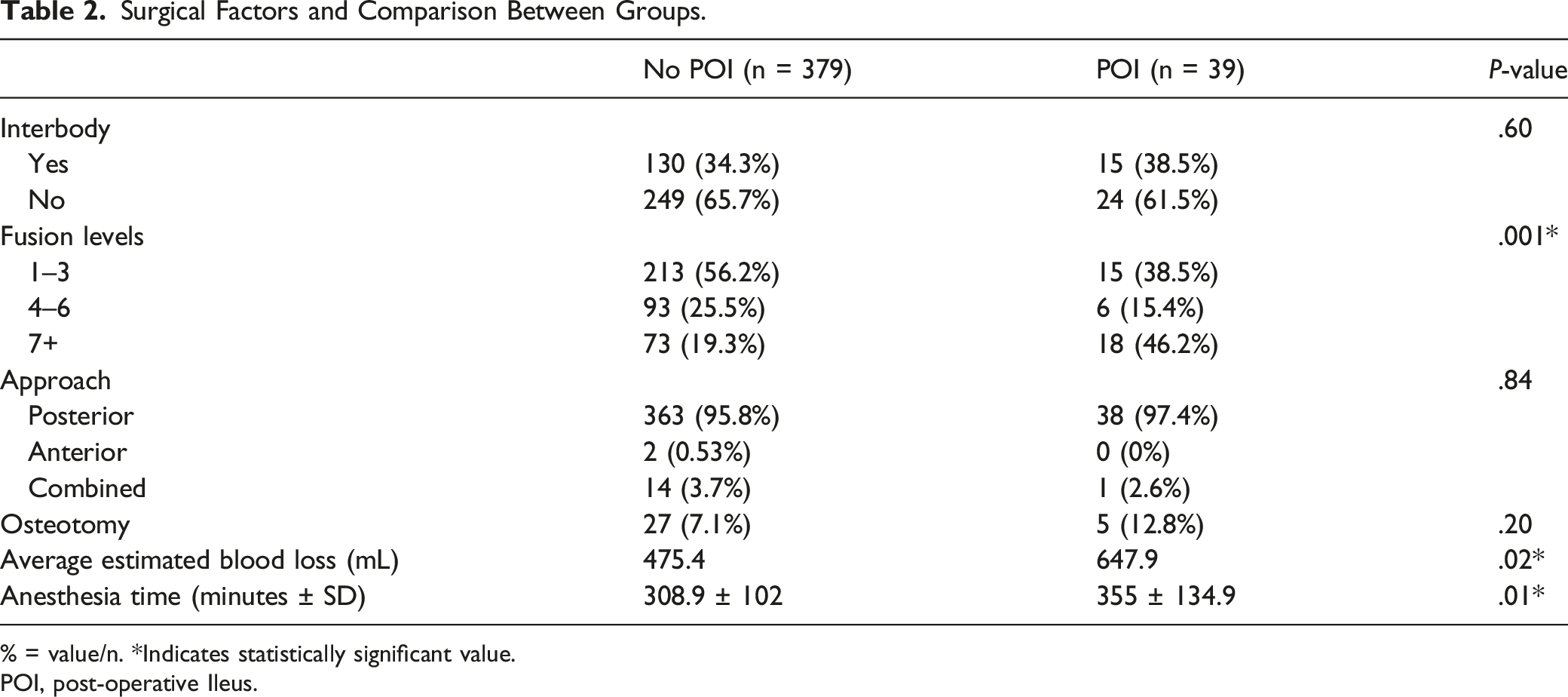
% = value/n. *Indicates statistically significant value.
POI, post-operative Ileus.
Opioid Consumption.
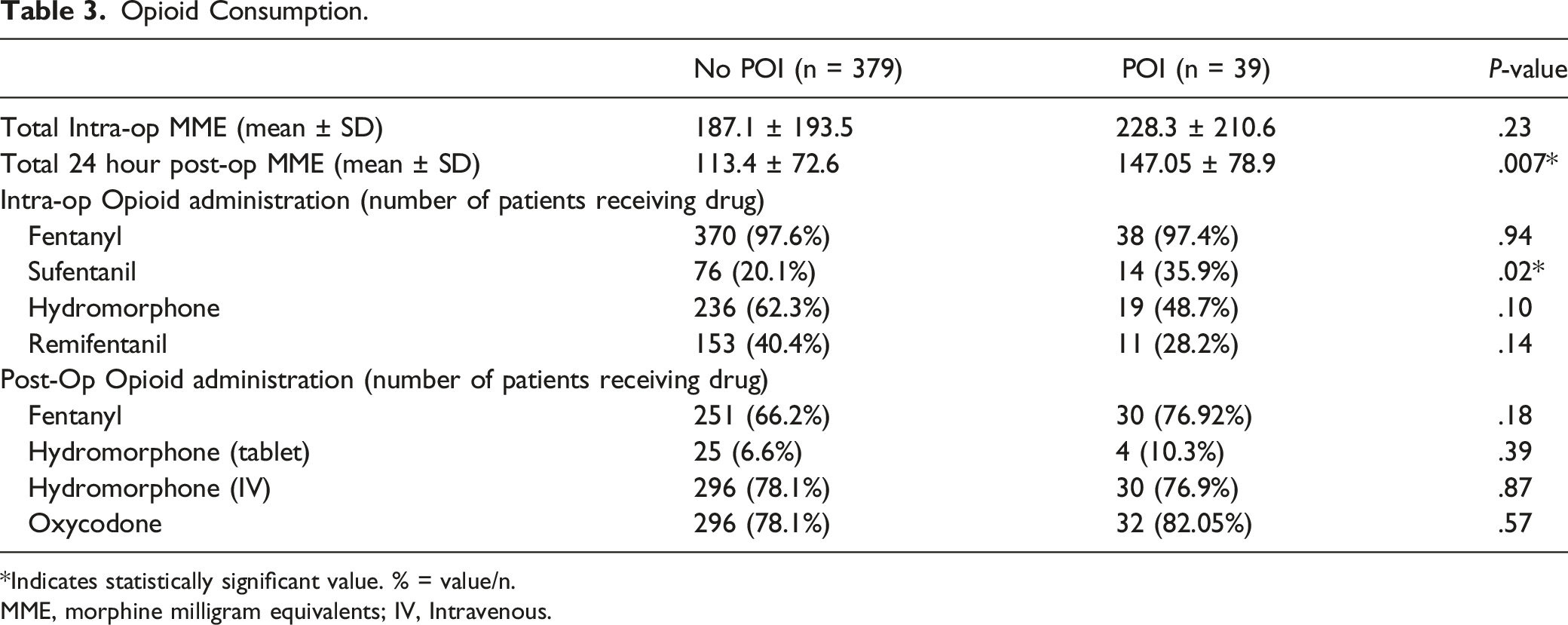
*Indicates statistically significant value. % = value/n.
MME, morphine milligram equivalents; IV, Intravenous.
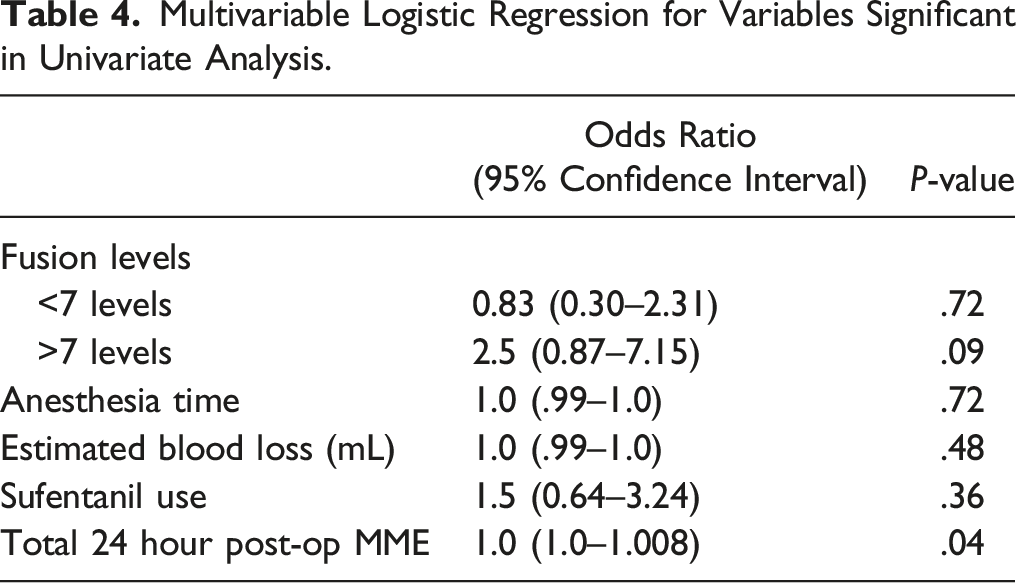
Multivariate logistic regression analysis showed that number of fusion levels, anesthesia time, estimated blood loss, and sufentanil use were no longer significant (Figure 1). Total 24-hour post-op MME remained significant when all other factors were controlled for (OR 1.004, P = .04) (Table 4). Probability for Ileus with Total 24-Hour Post-Op MME. Brackets indicate 95% confidence interval. Multivariable Logistic Regression for Variables Significant in Univariate Analysis.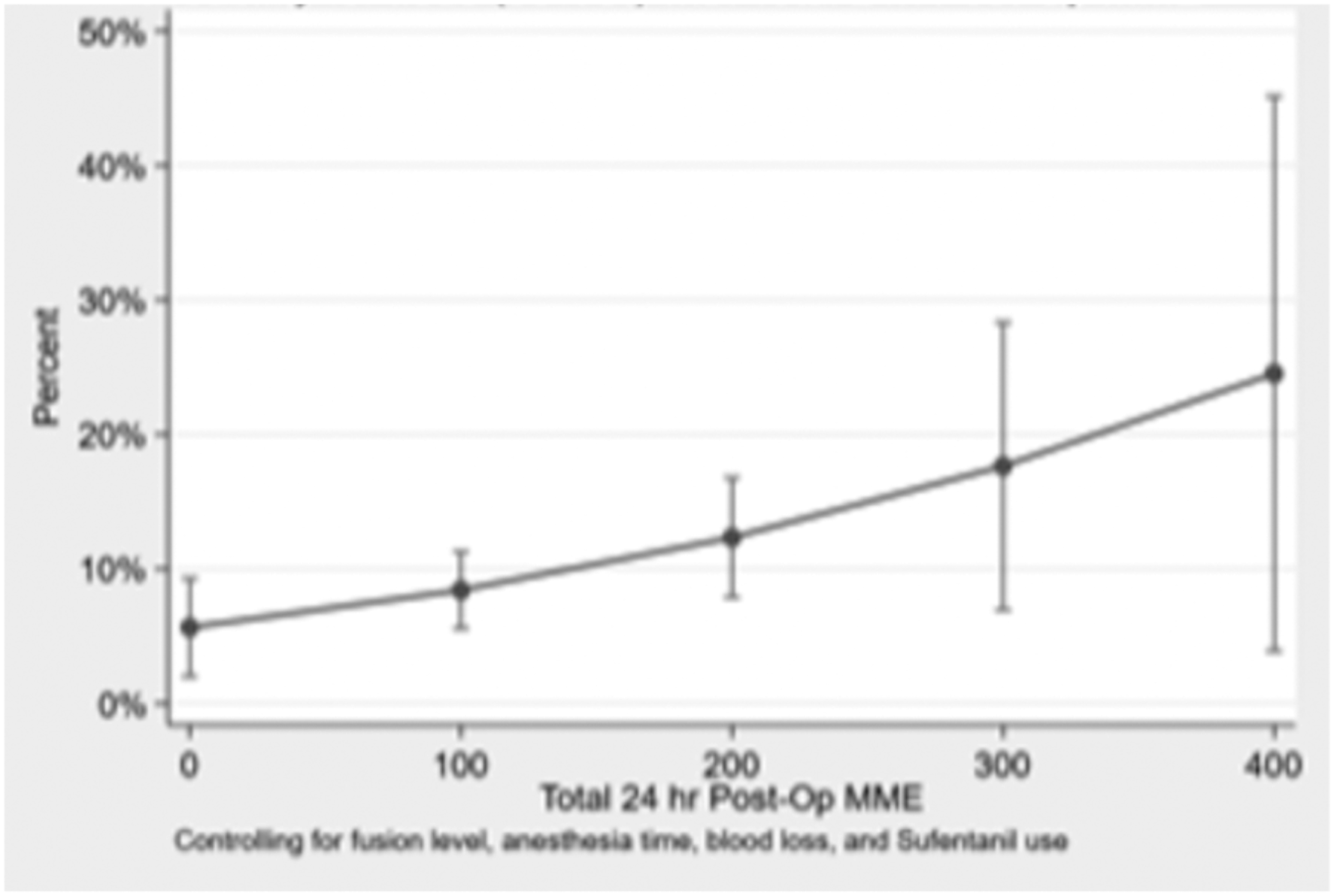
Discussion
This retrospective cohort study of 418 patients undergoing thoracolumbar instrumented fusion found that total postoperative opioid administration is an independent risk factor for the development of POI. Surgeons and anesthesia providers should carefully consider multimodal analgesia agents to maintain appropriate pain control while minimizing perioperative opioid administration. The effect of POI is manifold—in addition to patient discomfort POI increases costs to the medical system,19,20 increases length of stay, and can increase the risk of DVT, PE, and other medical complications.20,21 There are few studies in the spine literature examining the effect of opioids upon development of POI in this patient population. The current study, which is the largest of its kind, is the first to demonstrate that the amount of opioids a patient takes postoperatively has a direct impact on the development of POI. Gifford et al 12 found that postoperative opioid administration did not influence the development of POI. However, in contrast to our study they did find that intra-op opioid administration affected the development of POI. The overall effect of total MME, both intra-operatively and postoperatively is difficult to separate and likely both contribute to the development of POI. The results of these two studies reporting association between POI and the amount of opioids administered in the perioperative period supports the well-described associations between opioid medications and decreased GI motility.22-24 It is possible that opioids given after 24 hours postoperatively also play a role in developing POI. Our study, however, could not detect this as we accounted for opioid administration within a 24-hour period after surgery.
The observed incidence of POI in the current study was 9.3%, which is within the range of previously reported POI incidence of 1.9%–23.1% after spine surgery.4-9 Our incidence is toward the lower end of this range, which may be due to our typical postoperative protocol, which includes early mobilization and scheduled bowel regimen starting on the day of surgery. Several studies have found that aggressive bowel programs postoperatively can decrease the rate of postoperative ileus, though none of these studies were specific to spine surgery.25,26 The use of nalexgol, as used routinely at our institution, as well as methylnaltrexone and alvimopan, have proven efficacious in opioid induced ileus,27-30 but no studies have investigated their potential positive role after spine surgery. These are potential low-cost interventions that could be utilized to decrease the risk of POI in prospective studies.
While univariate analysis demonstrated a significant difference in POI rates with fusion of ≥7 levels, this difference was no longer significant when controlling for MME with multivariate regression analysis (P = .09). Post-hoc power analysis estimated a total sample size of 316 patients to detect a significant difference with 80% power at the predetermined significance level of alpha = 0.05, suggesting this was not due to type II error. Similar results were seen for anesthesia time and higher EBL, where univariate analysis demonstrated significant association with POI which was no longer a significant relationship after controlling for other factors with multivariate regression analysis. These three factors are clearly interrelated, as patients who undergo fusion at more levels will also have longer anesthesia time, higher EBL, potential for increased post-operative pain leading to increased opioid administration and may be slower to mobilize postoperatively. Although there was no significant relationship between number of levels fused and POI with multivariate analysis of the current study, other studies have reported significant association between increasing number of levels fused and POI.4,12 In the current study, fusion of ≥7 levels approached significance when controlling for other variables in multivariate analysis (P = .09).
There are several limitations to this study. The retrospective nature of the study introduces inherent biases and limitations. Identification of POI through chart review may underestimate the true incidence following thoracic and/or lumbar spinal fusion. The generalizability of this study is limited, as this was done at a tertiary care academic institution. These patients may have a higher level of complexity but are also managed in the same manner postoperatively in terms of a bowel regimen, pain control, and early ambulation. Furthermore, this study only applies to thoracic and lumbar spine surgery with instrumented fusion, and therefore may not apply to cervical spine patients or patients only undergoing decompression without fusion. Lastly, we only accounted for post-op 24-hour MME, and, as such, cannot exclude the possibility that calculating MME over a longer duration with accumulation of opioids in a patient’s system may also be an independent risk factor for POI.
Conclusion
This retrospective study is the largest study to date investigating risk factors for POI after elective thoracolumbar spinal fusion. We observed a 9.3% rate of POI, and have identified postoperative opioid consumption as a significant risk factor for POI development. Further studies are warranted to examine clinical strategies to decrease the incidence of this common postoperative complication.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Author’s Note
Work was performed at the University of Utah, Salt Lake City, Utah.
