Abstract
Study Design:
Prospective non-randomized single-center cohort study.
Objectives:
To analyze the quality of postoperative magnetic resonance imaging of 2 structurally different cervical disc arthroplasty devices at the index and adjacent levels.
Methods:
A non-randomized, comparative, prospective, single-center study included 40 patients (23 men and 17 women) aged 32 (26-40) years. Two study groups were utilized: in the first (n = 20), a titanium prosthesis was used; in the second (n = 20), a cobalt-chromium implant was used. Evaluation of MRI studies before and after surgery was performed using sagittal and axial T2 weighted images by 2 specialists who were blinded to the prosthesis that was used. To determine the quality of an MRI image, the classification of Jarvik 2000, the radiological and orthopedic scales for assessing artifacts were used.
Results:
There was good-to-excellent inter-observer agreement for all of the MR parameters used for the titanium and satisfactory-to-good for the cobalt chromium group. The analysis of the quality of postoperative imaging using the Jarvik 2000 scale showed a statistically significant deterioration in MR images in the cobalt chromium group (P < 0.001), compared to the titanium (P = 0.091). Following a single-level total arthroplasty, the titanium group had better MRI images according to radiological and orthopedic scales (P < 0.001).
Conclusion:
Titanium cervical disc arthroplasty devices result in superior postoperative MR imaging, as compared to cobalt chromium prostheses, as the latter significantly reduces image quality due to the pronounced ferromagnetic effect.
Keywords
Introduction
Total disc arthroplasty of the cervical spine has become a popular alternative to ACDF, as it preserves motion at the operated segment,1,2 while allowing for fast recovery and potentially reduced rates of adjacent segment pathology compared to ACDF. 3
Currently, structurally different single-component and 2-component CDA (cervical disc arthroplasty) prostheses with metal-on-metal and metal-polymer contact surfaces have been developed. 4 For the metal element, stainless steel, titanium or cobalt-chromium-molybdenum alloys are used; the polymer part consists mainly of polyether-ether ketone, polyurethane or ultra-high-molecular weight polyethylene.5,6
Following total disc arthroplasty, the necessity for revision surgery has been reported to be between 2-4%.7,8 A common cause of such intervention is the degeneration of an adjacent segment, and therefore, full visualization of the operated and adjacent levels is a desirable characteristic for CDA devices. 9 Given the low percentage of revision surgery following a CDA, postoperative imaging should be comprehensive and must include both magnetic resonance imaging (MRI) and computed tomography (CT). 10 CT remains the preferred and most informative method for assessing the status of the implant. 5
MRI is considered the definitive screening method for postoperative examination of the spinal cord and roots, and is preferable to CT, with or without myelography. 10 In addition, perioperative assessment of the state of the spinal cord is important, even without obvious clinical manifestations, and therefore MRI is preferable over CT for imaging. 10 Most implantable devices create distortion on MRI images, from minimal to severe. 11 The use of metal-subtracting MRI protocols are not routinely obtained and provide only a partial improvement in the quality of neuroimaging. 12 Some studies indicate a lower ferromagnetic effect of titanium CDA devices compared to cobalt-chrome ones.13,14
In Europe, M6-C (Spinal Kinetics, Switzerland) and Active-C (B-Braun, Germany) are 2 popular CDA devices. We first began using the M6-C, a titanium prosthesis, at the Neurosurgery Center…………in 2013. The Active-C (B-Braun, Germany), a cobalt-chromium prosthesis was introduced in 2018. To our knowledge, the MRI characteristics of these 2 structurally different prostheses have not been previously reported. We undertook this study to conduct a comparative analysis of the quality of postoperative magnetic resonance visualization of 2 structurally different CDA prostheses: the M6-C and the Active-C.
Materials and Methods
Study Design
From May 2013 to April 2020, 492 decompression-stabilization cervical spine procedures were performed at the Neurosurgery Center………Of these, 140 were performed using CDA prostheses: 73 at 1 segment, 42 at 2 levels and 25 in combination with an interbody fusion.
A non-randomized, comparative, prospective, single-center study included 40 patients (23 men and 17 women) aged 32 (26-40) years. All of the cases that met the inclusion and exclusion criteria for a single level CDA and the patients were willing to give informed consent were included. This study was approved by the ethics committee of the…………(Protocol No. 1 dated 17.12.2017). Each patient signed a voluntary consent to be included in the study.
Patient Inclusion/Exclusion
All patients had to have persistent radicular symptoms resistant to conservative therapy for 4-6 weeks due to a single-level cervical disc pathology between C5 to C7. The disc degeneration had to be grade I or II by the Pfirmann classification 15 and the facets joints had to be grade I or II by the Fujiwara classification. 16 The disc height had to be no less than 50% of an adjacent normal disc height. The segment had to be stable with no posterior osteophytes.
Patients were excluded if they had 2 or more level clinically significant degenerative diseases of the cervical spine, or if they had symptoms from above C4 or below C7. They could not have had previous surgery at the index level, myelopathy, inability to have an MRI due to any reason, a decrease in bone mineral density of 2.8 or more according to the T-criterion (WHO, 1995), traumatic injury to the disc, systemic connective tissue disease, infectious or inflammatory etiology, tumor, segmental instability, facet arthrosis, disc height loss greater than 50%, congenital stenosis or lack of informed consent. Patients with cervical myelopathy were excluded from the study due to the fact that when we were designing the study, we did not believe there would be very many eligible patients with myelopathy and therefore decided to keep the group as uniform as possible.
Operative Procedures
The operations were performed by one surgical team under general anesthesia using standard techniques via a left-sided retropharyngeal Cloward approach. In all cases, a total discectomy was performed with bilateral foraminotomies and the posterior longitudinal ligament was resected. The first group (n = 20) was treated with a single-component titanium prosthesis, M6-C (Spinal Kinetics, Switzerland) (Figure 1A-D) consisting of 2 titanium endplates with a polyurethane core. The second group (n = 20) was treated with a 2-component cobalt-chromium prosthesis, Active-C (B-Braun, Germany) (Figure 2A-D), consisting of cobalt-chromium endplate with an ultra-high-molecular weight, low-pressure polyethylene liner.
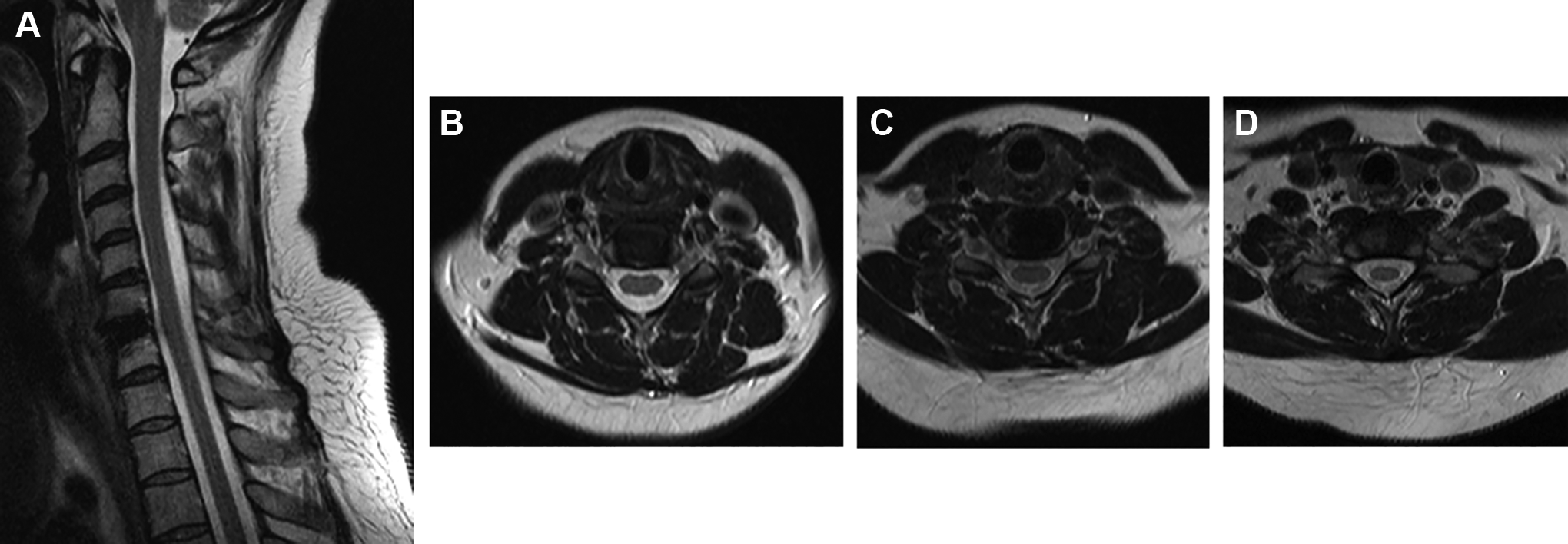
Clinical case: Female, 39 y.o. with degenerative disc disease at C6-7 treated with a titanium CDA. (A) Postoperative sagittal MRI; (B-D) postoperative axial MRI images, respectively, of C5-6 (upper adjacent level); C6-7 (index level); and C7-T1 (lower adjacent level)
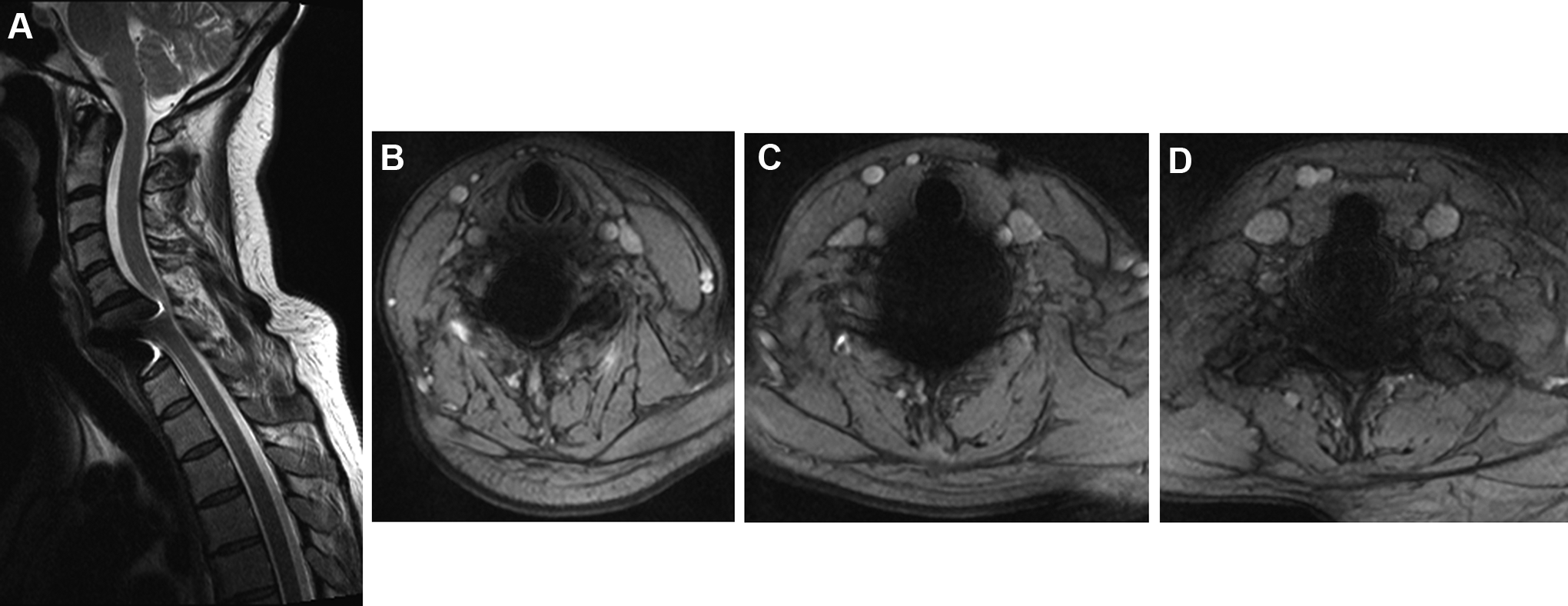
Clinical case: Female, 38 y.o., with degenerative disc disease at C6-7 treated with a titanium CDA. (A) Postoperative sagittal MRI; (B-D) postoperative axial MRI images, respectively, of C5-6 (upper adjacent level); C6-7 (index level); and C7-T1 (lower adjacent level)
Follow-Up Outcomes
Pre and post-operative T2-weighted sagittal and axial MRI images (Siemens Magnetom Essenza 1.5 T, Germany) were evaluated. The MRIs were obtained using the following parameters: matrix 384 × 288, TR (repetition time) = 4000, TE (echo time) = 43, NEX (number of excitations) = 1, slice thickness = 4 mm, FOV (field of view) = 30 × 30. Postoperative MRIs were obtained from 4 to 12 weeks after surgery.
The MRI images were evaluated independently by 2 specialists who were blinded to the type of implant utilized. Deidentified JPEG images were analyzed in 7 regions: (1) the spinal cord at the operated level, (2) the operated disc level, (3) the central canal at the operated level, (4) the right foramen, (5) the left foramen, (6) the superjacent disc, and (7) the subjacent disc. To evaluate the quality of the MRI image, the Jarvik Classification 2000 17 was used: grade 1—marked blurring without definable margins; grade 2—blurring but definable margins; grade 3—minimal blurring; grade 4—sharp definition. The general image quality rating was the average of all 7 evaluated areas; the image quality rating at the operated level was calculated as the average value from 5 regions (spinal cord at the operated level, the operated disc level, central canal at the operated level, right and left foramina); the rating for the adjacent segments was the average value of the superjacent and subjacent disc levels. Statistical evaluation of experts’ agreement was carried out using Kappa statistics (Graph Pad Software, Inc., USA).
The radiology grading scale for the operated and adjacent levels are outlined MRI artifact assessment by Radiology grading (grade 1—no significant artifact, grade 2—mild artifact measuring 1 mm or less surrounding the implant; grade 3—moderate artifact measuring greater than 1 mm but less than 3 mm; grade 4—severe artifact measuring greater than 3 mm surrounding the implant) and Orthopedic grading (grade 1—no reduction in diagnostic quality because of artifact, grade 2—some artifact with a reduction in diagnostic quality; grade 3—severe artifact with loss of diagnostic ability) scales. 18
Statistical Analysis
Statistical data processing was performed using Statistica for Windows software version 6.0. Descriptive statistics are presented as M ± SD, where M is the mean value and SD is the standard deviation. Comparison of continuous variables in the groups of respondents was performed using the t-test. P values less than 0.05 were considered reliable.
Results
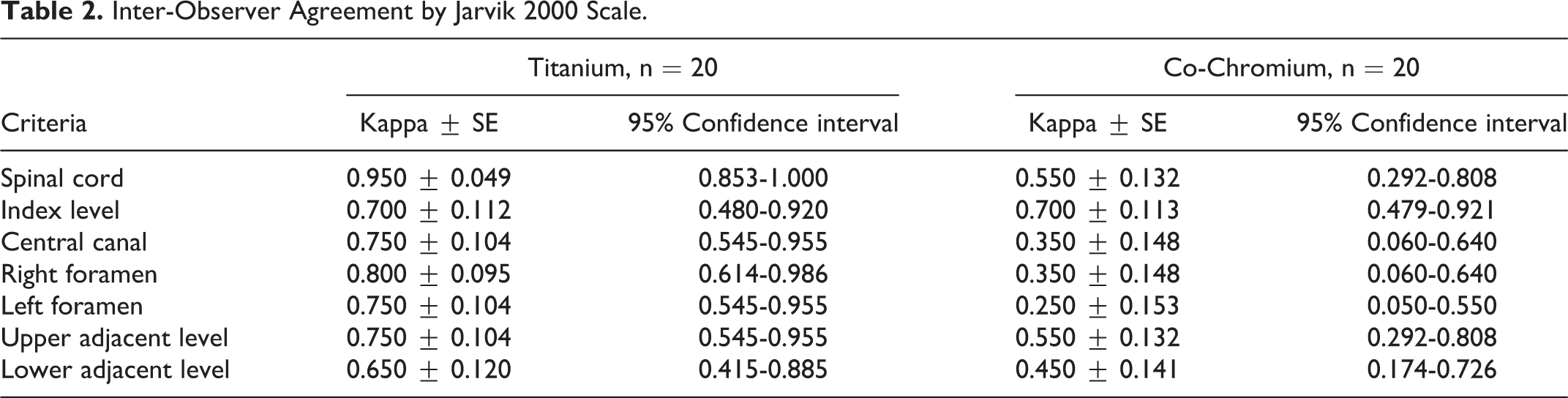
Information about the patients included in the study is shown in Table 1. There were no intergroup differences in gender and age (P > 0.05). The average follow-up was 98 months in group I and 28 months in group II.
Characterization of Patients of the Studied Groups.
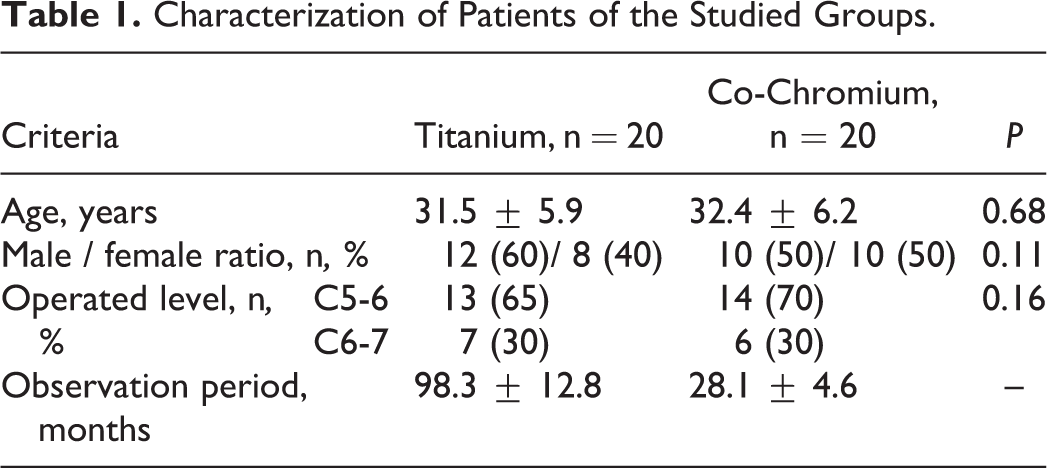
The inter-observer agreement was evaluated based on the kappa statistics for each of the measured parameters on the Jarvik 2000 scale 17 (Table 2). It was found that the quality of agreement for the titanium group was good and excellent, for the cobalt-chromium group—satisfactory and good.
Inter-Observer Agreement by Jarvik 2000 Scale.
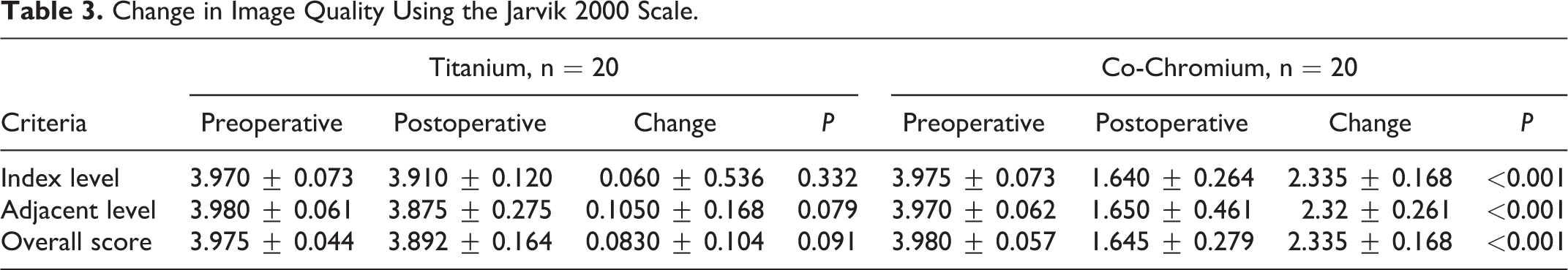
The quality of postoperative imaging using the Jarvik 2000 scale 17 showed a statistically significant deterioration of MR images in the cobalt-chromium group for all analyzed areas (Table 3).
Change in Image Quality Using the Jarvik 2000 Scale.
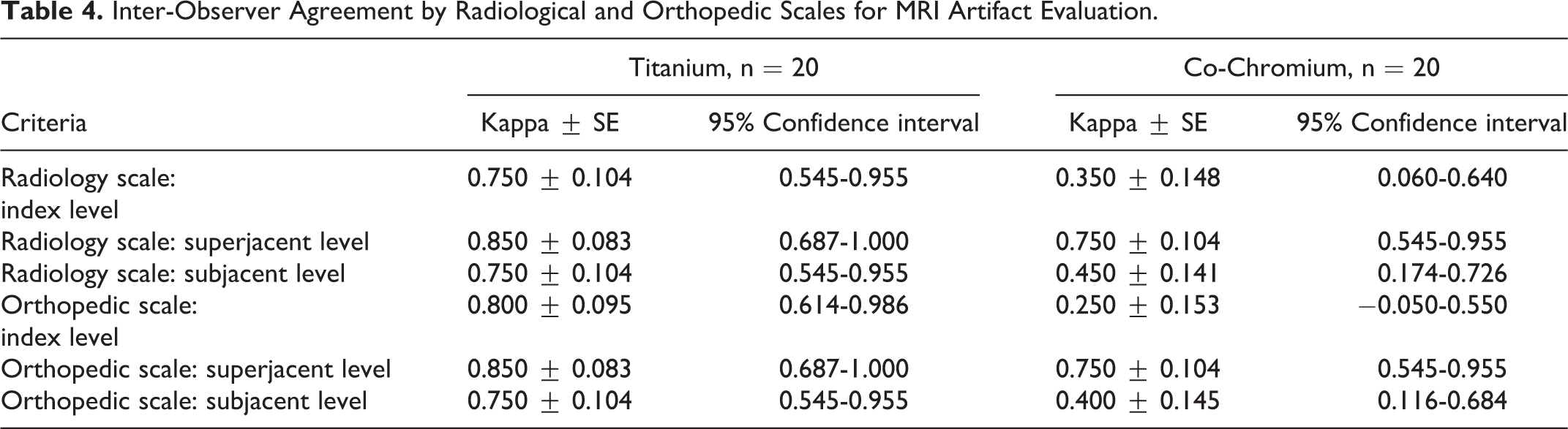
Inter-observer agreement based on the kappa statistics for the operated and adjacent segments on the radiological and orthopedic scales for MRI artifact evaluation 18 showed good and excellent quality for the titanium group and satisfactory and good for the co-chromium group (Table 4).
Inter-Observer Agreement by Radiological and Orthopedic Scales for MRI Artifact Evaluation.
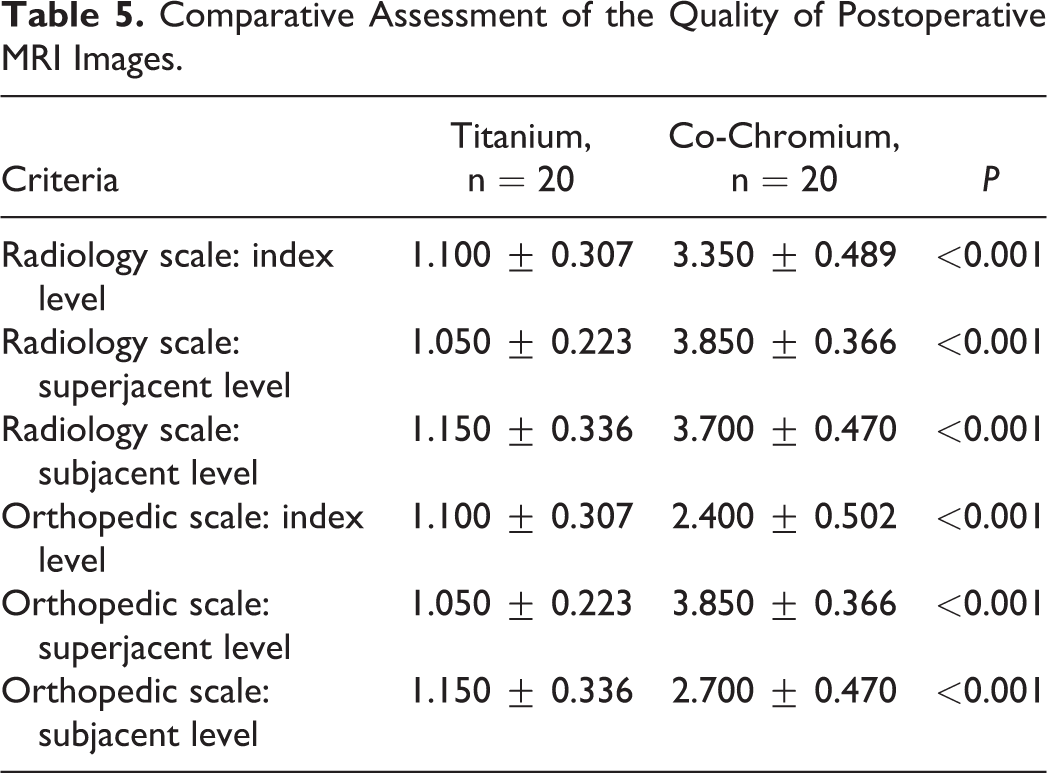
A comparative analysis of the quality of MRI images on radiological and orthopedic scales for evaluating artifacts at the operated and adjacent segments revealed a statistically significantly better postoperative neuroimaging for the titanium group (Table 5).
Comparative Assessment of the Quality of Postoperative MRI Images.
Evaluation of the quality of MRI images following a single-level CDA showed that the titanium prostheses had better postoperative neuroimaging at both the operated and adjacent segments than the cobalt-chromium implants.
Discussion
It is not uncommon for patient to develop symptomatic adjacent segment pathology following CDA. Routine workup for these symptoms includes MR scanning of the operated and adjacent segments to determine the state of neural structures and adjacent segments. 13 It is well-known that the degree of MR image distortion and artifact directly depends on the implanted material: from severe (stainless steel) to moderate (cobalt-chromium-molybdenum alloys) to minimal (titanium). 19 However, the amount of material utilized for a CDA is small and might not have a significant effect on MR images. We undertook this study to determine the MR imaging characteristics of 2 CDA devices that are popular in Europe.
We found that the cobalt-chromium disc produces pronounced artifacts on postoperative MRIs, which complicates the evaluation of neural compression at both the operated and adjacent segments. On the other hand, the titanium prosthesis resulted in much better post-operative MR images.
There are advantages and disadvantages to both types of metals. Titanium has high strength and biocompatibility and osseointegration due to a low Young’s modulus of elasticity. 20 At the same time, titanium products are characterized by increased wear at the contact surfaces, which requires additional alloying with aluminum or vanadium. 4 Cobalt-chromium metal alloy, usually containing up to 7% molybdenum, also possesses high biocompatibility but it has been associated with allergic reactions and an immune response. 21 At the same time, cobalt-chromium-molybdenum alloy is more wear-resistant than titanium. 22
All modern artificial cervical disc prostheses are safe and compatible with postoperative MRI evaluation. 23 A comparative analysis of the results of titanium and cobalt-chromium artificial CDA prostheses showed a significant deterioration in image quality and the presence of artifacts with the latter. 24 Thus, according to Sekhon et al. 14 the titanium Bryan disc prosthesis (Medtronic Sofamor Danek, Memphis, USA) and Prestige LP (Medtronic Sofamor Danek, USA) did not significantly affect postoperative imaging, while the cobalt-chromium Prodisc-C (Synthes Spine, USA) and PCM (Cervitech, Rockaway, USA) significantly impaired the quality of MR images. On the other hand, not all titanium prostheses may have the same MRI characteristics. Sundseth et al. 12 , in a study of postoperative MRI following implantation of the titanium Discovery (Depuy Spine, USA) prosthesis reported that the presence of artifacts impeded the interpretation of foramina and made it impossible to assess the state of the spinal cord. Gerigk et al. 25 also found impaired visualization of the foramen after implantation of titanium cages. Similar data were obtained by Elliott et al. 26 in patients after ACDF with titanium cages. Therefore, not all titanium implants result in minimal MRI distortion.
Comparative analysis of clinical postoperative results is beyond the scope of the study aimed solely at assessing the MR characteristics of cobalt-chromium and titanium implants. At the same time, the study of clinical data after the installation of 2 constructively different IVD prostheses, in our previously published studies, did not reveal significant intergroup differences. We would like to emphasize that MRI compatibility is but one determining factor for which implant should be chosen. In fact, mechanical properties, ease of implantation, longevity, wear characteristics, sizing alternatives, heterotopic bone induction, speed of integration into the endplates, ease of explantation, stability, long-term utility and other factors may equal or even far supersede MRI compatibility as important determining factors.
Limitations
As with any study, there are a number of potential limitations with this study. First, we used only 2 different implants and they may not be representative of all titanium or cobalt-chromium implants. However, our goal was to test 2 of the most popular devices used in Europe. Second, we used only 1.5 T magnet MRIs with standard T2-weighted images. It is possible that other sequences or protocols might have yielded very different results. For example, there are a number of techniques to reduce the severity of postoperative ferromagnetic artifacts. First, one can use an MRI with a smaller magnet. Antosh et al. 27 , demonstrated a reduction in artifacts following implantation of cobalt-chromium PCM (NuVasive, Inc., USA) and Prodisc-C (Synthes Spine, USA) prostheses by using a 0.2 T MRI. Similar data were obtained in the evaluation of adjacent segments after total arthroplasty of the lumbar spine using an MRI tomograph with a magnetic field strength of 0.3 T. 28 As one might suspect, a 3 T magnet MRI had worse artifact production following implants than 1.5 T magnets. 29 In addition, the direction of frequency encoding, slice thickness, throughput, and echo time also affect the severity of artifacts.30,31 There is active research attempting to improve neuroimaging after implantation of spinal prostheses. The “slice encoding for metal artefact correction” (SEMAC) technique improves the quality of postoperative MRI neuroimaging by increasing the angle of inclination of the spin echo with additional z-phase encoding, although it lengthens the scan time. 32 The “iterative decomposition of water and fat with echo asymmetry and least-squares estimation” (IDEAL) technique is a technique that reduces metal artifacts following pedicle screws. 33 Therefore, it may be possible that with some of the above techniques, one can subtract out much, if not most, of the metal artifacts from post-operative MRIs. However, most surgeons do not routinely ask for these sequences or they are not usually offered in many radiology departments without a specific request. Therefore, we feel that our protocol represents a more clinically relevant scenario.
Strengths of the Study
Our study also has several strengths. First, we had 20 patients in each of the 2 groups and all of the MRIs were read in a blinded fashion by 2 experts. Second, we restricted the level of surgical intervention to the C5-C6 and C6-C7 segments in order to keep the study as uniform as possible. The novelty of the study is that, to our knowledge, this is the first evaluation of 2 CDA devices that are popular in Europe. In addition, we used a combination of different methods for assessing MR imaging (the classification of Jarvik 2000, as well as radiological and orthopedic artifact evaluation scales) following CDA that have not been used before.
Conclusion
Postoperative MR imaging to assess neural structures and adjacent segments depends not only on the type of instrumentation used, but also on its material composition. Cobalt-chromium devices adversely affect post-operative MRI evaluation, whereas titanium devices have a much less of an effect on MRI images.
Footnotes
Authors’ Note
Each author made significant individual contributions to this manuscript. VAB (0000-0003-4349-7101)*, AAK (0000-0001-9039-9147)* and KDR (0000-0003-2083-9375)* were the main contributors to the drafting of the manuscript. VAB and AAK performed the surgery and patient follow-up, and gathered clinical data. AAK and MAA (0000-0002-7676-1127)* evaluated the data from the statistical analysis. VAB, AAK and MAA performed the literature search and review of the manuscript, and contributed to the intellectual concept of the study. *ORCID (Open Researcher and Contributor ID).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
