Abstract
Study Design:
Narrative literature review.
Objective:
The numbers of low-energy cervical fractures seen in patients suffering from ankylosing spondylitis (also known as Bechterew disease) or diffuse idiopathic skeletal hyperostosis (also known as Forestier disease) have greatly increased over recent decades. These fractures tend to be particularly overlooked, leading to delayed diagnosis and secondary neurological deterioration. The aim of the present evaluation was to summarize current knowledge on cervical fractures in patients with ankylosing spinal disorders (ASDs).
Methods:
The literature was analyzed through an extensive PubMed search focusing on cervical fractures, especially with delayed diagnosis.
Results:
In ASDs, it was mainly the cervical spine that was found to be affected by fractures. Fifty percent of ASD patients had neurological deficits at admission, with a high probability of secondary deterioration due to an initially missed diagnosis. Multislice high-resolution imaging techniques should be the radiological standard of care if a vertebral fracture is suspected. Nevertheless, many of these spinal fractures are overlooked, leading to feared secondary deterioration of existing unstable fractures. Long posterior instrumentations were found to be the treatment of choice, followed by anterior and combined anterior-posterior instrumentations.
Conclusions:
Delayed diagnosis of cervical fractures in ASDs contributes to initially misinterpreted clinical symptoms, inadequate imaging techniques, and a lack of knowledge about this disease entity due to its peculiarities. Thorough assessment of the patients’ neurological morbidity at admission might reduce the occurrence of the associated fractures. The biomechanical behavior of ASD fractures is completely different from that of non-ASD fractures, so that the treatment strategy for these patients should be at least surgical, in combination with long dorsal instrumentations or combined anterior-posterior approaches.
Keywords
Introduction
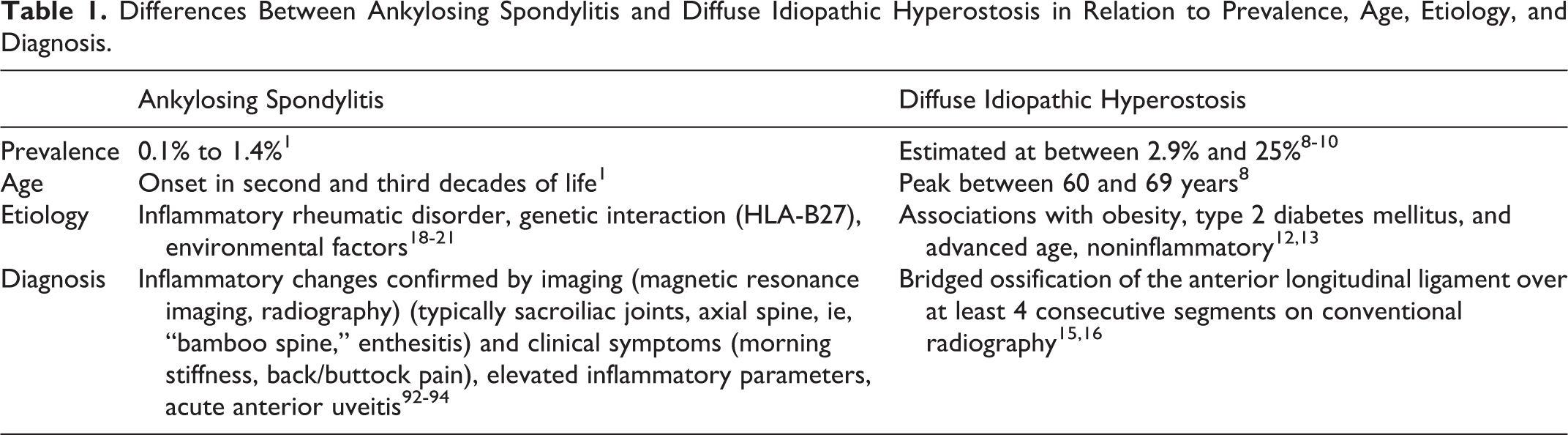
Ankylosing spinal disorders (ASDs) lead to progressive ossification of the spinal column. 1 These ossifications entail bridging bone formations (syndesmophytes) in the spinal segments involved, with a high susceptibility to trauma even after low-energy impacts. 1 –5 This is a result of long ankylosed lever arms combined with a reduced capability for deformation, resulting in unstable spinal fractures, especially in the lower cervical segments. 6,7 The most common entities involved in ASDs are ankylosing spondylitis (AS; also known as Bechterew disease) and diffuse idiopathic skeletal hyperostosis (DISH; also known as Forestier disease). These 2 types share essential clinical features. The current prevalence of DISH is estimated at between 2.9% and 25%. The prevalence of DISH peaks in the 60- to 69-year-old age group and rises progressively with increasing age. 8 –10 Interestingly, DISH tends to be more common in men, although the etiology of the condition is still unknown. 8 –11 There may be a strong association with obesity, type 2 diabetes mellitus, and higher age, as described in the literature (Table 1). 12,13 Despite the increasing number of DISH cases, as a result of its association with traits involved in the modern Western affluent lifestyle, the prevalence of AS is still stable at 0.% to –1.4% and it mainly affects males. 1 In contrast to AS, DISH is regarded as a noninflammatory disorder in which the spinal longitudinal ligaments and entheses slowly develop ossification over time in the segments involved, ultimately ending in complete rigid ankylosis. 14 The diagnosis of DISH is established when bridged ossification of the anterior longitudinal ligament is present over at least 4 consecutive segments on conventional radiography. It was first defined as “senile ankylosing hyperostosis of the spine” by Forestier and Rotes-Querol. 15,16 A progressive chronic inflammatory component is assumed to be the cause of Bechterew disease. The clinical characteristics of the disease consist of progressive stiffness, combined with pain as a result of advanced inflammation of the spinal and sacroiliac joints, occurring approximately around the 25th year of life. 17 Complex interactions between genetic (HLA-B27) and environmental factors are involved in the etiology of the disease, but it continues to be one of the most puzzling mysteries among the rheumatic disorders. 18 –21 Due to improvements in the medical treatment available for AS and DISH, associated with increased life expectancy, the incidence of complicated spinal fractures among these patients can be expected to rise dramatically during the coming decades. 2,7 The cervical spine is the region that is most susceptible to these fractures. 2 –4,22 The reason for this may be the hypermobility of the cervical spine in combination with the weight of the skull, small vertebral bodies, and the position of the cervical facet joints. 23,24 In addition, patients suffering from AS frequently present with concomitant osteoporosis, especially in the early stages of the disease. 20,25 –27 There is also often a delay in the diagnosis of cervical spine fractures as a result of initially mild symptoms and the use of standard fluoroscopic imaging. 2,10,20,21,26,28,29 Finally, delayed diagnosis of cervical fractures may lead to severe secondary deterioration as a result of unstable spine fractures. 30 –33 The analysis of the literature presented here reports on cervical spine fractures in ASD, their diagnosis, neurological symptoms, and therapy, as well as complications and mortality.
Differences Between Ankylosing Spondylitis and Diffuse Idiopathic Hyperostosis in Relation to Prevalence, Age, Etiology, and Diagnosis.
Methods
The authors performed a narrative literature review based on an extensive PubMed search. Three authors searched independently, using the following key words with the “advanced” searching option in PubMed without limit, based on the publication year: (ankylosing spondylitis (Title)) OR (ankylosing spinal disorders) OR (diffuse skeletal hyperostosis) OR (bechterew’s disease) OR (forestier’s disease) AND (cervical) AND (spine) AND (spinal fractures) AND (trauma) AND (spinal) AND (injury) AND (injuries). All studies published in English with full-text availability were considered for inclusion. A total of 241 articles were found (230 records identified through PubMed and 11 records manually added after screening of reference lists). The articles collected were screened initially for relevance by title and abstract (182 articles excluded). After all appropriate articles had been compiled, 59 articles were checked by the authors (Figure 1). Thirty articles were not appropriate for inclusion due to inappropriate language, lack of full-text availability, and missing information according to our inclusion criteria and were therefor rejected. A total of 29 articles were included in the narrative literature review presented (Table 2). The majority of the reviewed articles are evidence level “3” and “4” (case-control studies, retrospective comparative studies, case series). The information presented focuses on the following results in summarized form:
Cervical spine fractures in ASD
Delayed diagnosis of cervical fractures in ASD
Surgical therapy of cervical spine fractures
Complications
Mortality
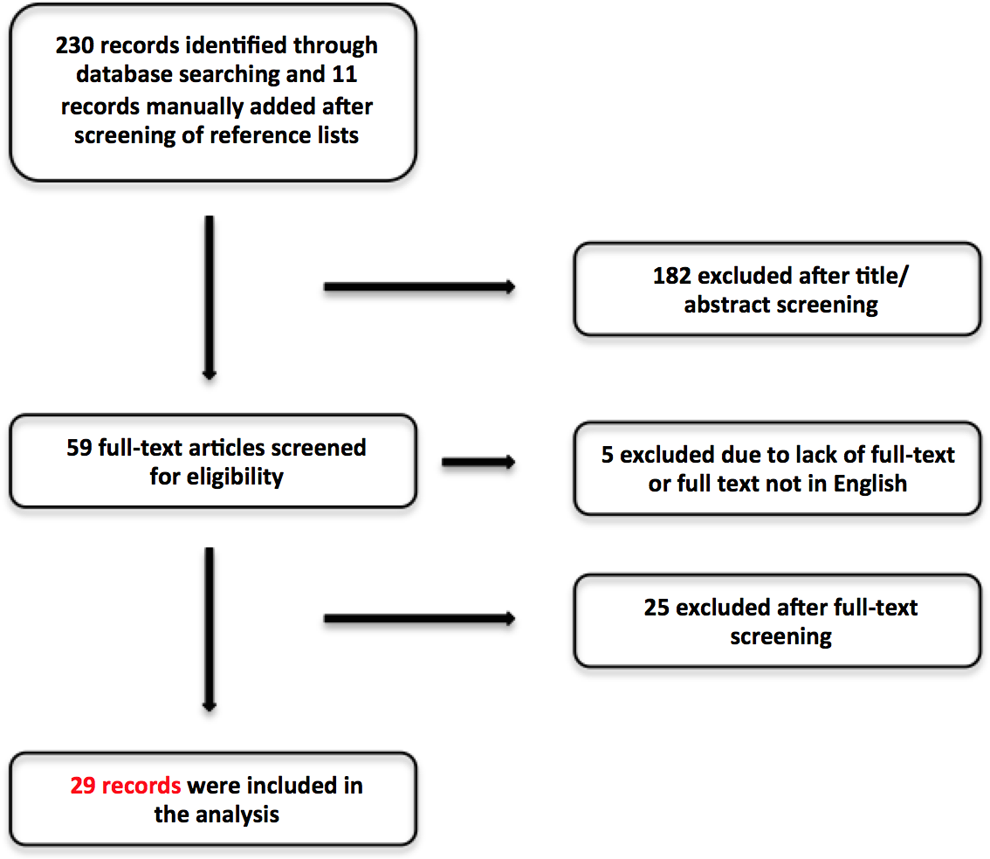
Flow chart for the literature search and study selection.
Important Studies Identified in the Literature Review Relative to the Numbers of Patients Treated, Treatment Option, Summarized Results, and Delayed Diagnosis of Ankylosing Spondylitis (AS) and Diffuse Idiopathic Skeletal Hyperostosis (DISH) (Oxford Centre for Evidence-Based Medicine; Available at http://www.cebm.net).
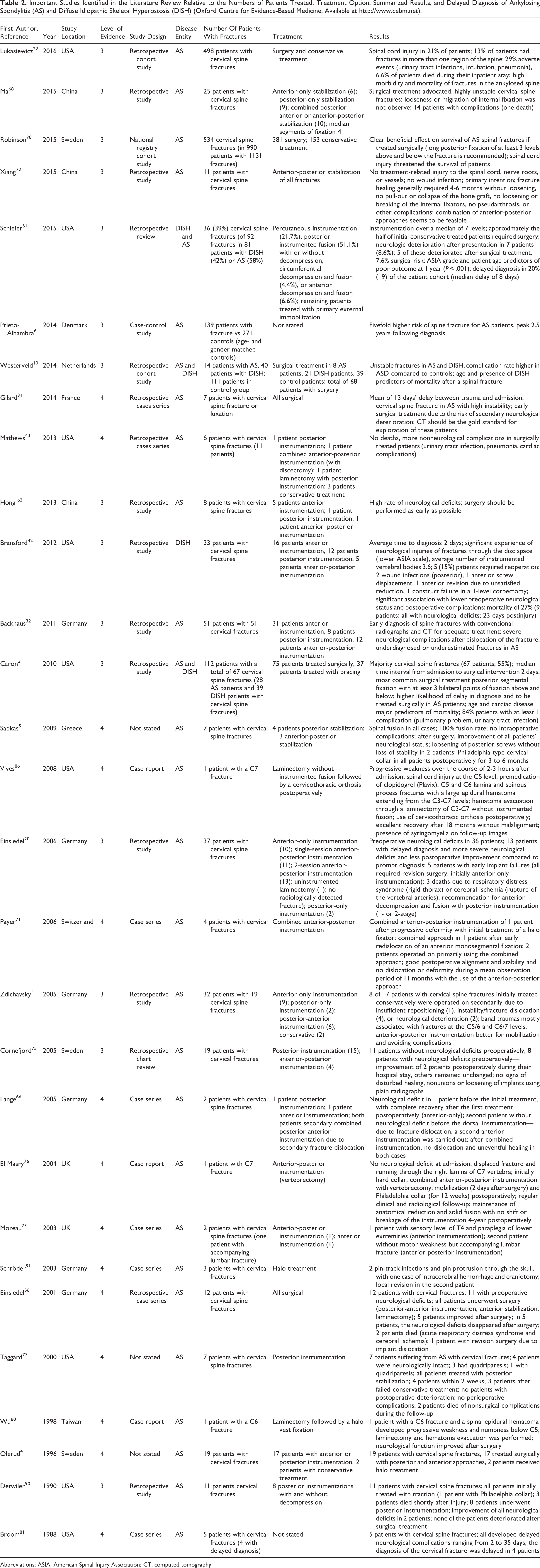
Abbreviations: ASIA, American Spinal Injury Association; CT, computed tomography.
Cervical Spine Fractures in ASD
The characteristic feature in both AS and DISH is progressive ankylosing of the spinal segments involved. Inevitably, an ankylosed spine reacts differently to spinal trauma than a healthy one. The prevalence figures for vertebral fractures and osteoporosis in patients with AS are reported in the literature to be approximately 10% to 30% and 20% to 60%, respectively. 34 –39 The cervical spine in particular is prone to fractures, and more than 50% of AS and DISH patients present with fractures of the cervical spine. 2,22 In addition to the frequently reduced bone mineral density in these patients, there is controversy over whether AS is also associated with increased bony formations due to ankylosing joints and syndesmophytes in the more advanced stages of the disease. 35 Osteoporosis appears to be associated with AS activity, but spinal fractures appear to be more related to the duration and severity of AS rather than bone mineral density. 36 In contrast to AS, there is still a lack of information on coexisting osteoporosis in patients with DISH. Nevertheless, some investigators have reported a possible relationship between DISH and a greater risk of vertebral fractures. 14 Patients with both AS and DISH are considered to be highly susceptible to cervical spine fractures resulting from low-energy impacts. 2 –5,22 These fractures tend to be unstable and may lead to secondary deterioration after initially mild symptoms, often as a result of displacement. 2,33,40,41 An initial presentation with mild symptoms may mask severe cervical fractures, leading to delayed diagnosis. The mechanism of injury commonly involves a fall from standing or sitting positions, with hyperextension of the cervical spine, but injury can also occur merely after rotating the head. 3 –5,42,43 According to Caron et al, cervical fractures in ASDs can be classified into disc injuries (type I), body injuries (type II), anterior body or posterior disc injuries (type III), and anterior disc or posterior body injuries (type IV). 3 The typical transverse fractures of the spine are known as “carrot stick fractures.” 44 Due to the functional deprivation of the intervertebral disc (IVD) in patients suffering from AS, the IVD represents the weakest point in the spine in these patients, which may be the reason for the typical fracture location through the IVD. 45 In contrast to AS, DISH fractures are prone to occur through the vertebral body. 45,46 Calcifications, especially at the level of the IVD, combined with stress shielding due to load transfer through the calcified/ossified anterior ligaments, prevent fractures through the IVD by weakening the vertebral body and strengthening the IVD. 45,46 In healthy individuals, increased forces lead to elastic distortion of the cervical spine until rupture of ligaments or fractures of the vertebrae occur. These compensatory mechanisms of elastic distortion in ASD patients fail much earlier due to a significantly decreased range of motion (ROM) as a result of ankylosed spinal segments. The lower cervical spine, especially levels C5-7, is highly susceptible to these low-energy fractures. 3,20,42,47 The age range during which fractures develop is approximately 60 to 70 years, with a significantly higher age at onset for DISH, as stated in the review by Westerveld et al. 2,3,20
Delayed Diagnosis of Cervical Fractures in ASD (Table 3)
The annual numbers of cervical spine fractures occurring due to AS have increased dramatically over the past 20 years. 7 Improved diagnosis and greater awareness of spinal fractures, combined with increased levels of activity particularly in older patients as a result of modern medical therapy, provide a reasonable explanation for these increasing numbers. 48 Despite the increase, the numbers of missed fractures are decreasing due to better visualization and the preference for computed tomography (CT) and magnetic resonance imaging (MRI) instead of conventional methods. 49 In most of these cases, mild injury patterns result in a delayed diagnosis. 2,3,20,33,50 –52 Several studies have reported a delay in diagnosis among patients with AS and DISH, ranging from approximately 10% to 50% of the patients presenting. 2,3,51,53 One possible explanation for the delayed diagnosis of cervical fractures might be the fact that minor trauma with only moderate pain is combined with insufficient radiodiagnostic examinations, in which osteoporosis and fractures in the cervicothoracic junction may be overlooked. 54 In addition, the physiological anatomy of the spine is sometimes substantially altered in patients with ASD, so that even with advanced imaging techniques it can still be challenging to identify the fractured levels. 55
Recent Literature on Ankylosing Spinal Disorders (ASDs) in Relation to Delayed Diagnosis, Second Neurological Presentation With Associated Postoperative Recovery, and Overall Mortality Rate.
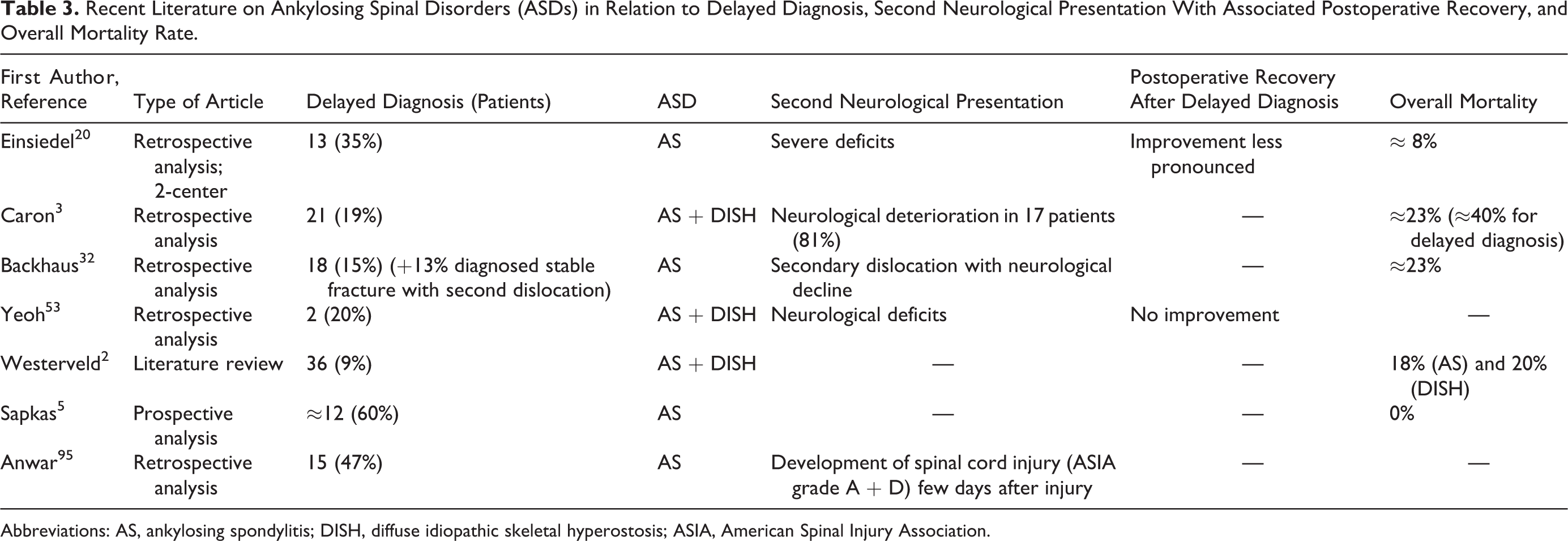
Abbreviations: AS, ankylosing spondylitis; DISH, diffuse idiopathic skeletal hyperostosis; ASIA, American Spinal Injury Association.
Delayed diagnosis often leads to secondary deterioration, with an associated decline in neurological function. 2,3,40,51 The initial lack of symptoms in patients with AS has been described as the “fatal pause” before neurologic deterioration occurs. 56 The delay in diagnosis of cervical fractures in AS contributes to initial misinterpretation of the clinical symptoms by physicians (52%), as well as by patients (48%), and this was described as the “doctor’s and patient’s delay” in the review by Westerveld et al. 2 In contrast to AS, patients with DISH did not misinterpret their symptoms, so that delayed diagnoses were only caused by doctors’ delays, as stated by Westerveld et al. 2
The use of standard imaging alone is also insufficient, and advanced imaging techniques should be used if there is a strong suspicion of fracture. 2,57,58 Due to the thin fracture lines, high-resolution multislice CT imaging is preferable as one of the most reliable tools for identifying the fractured levels. 54,59 –61 Since the risk of concomitant spinal cord injury in patients with AS is 10 times higher than in the healthy population, additional MRI scans are strongly recommended and should be available for all patients. 5,22,43,62,63 Concomitant epidural hematomas, with bleeding from ruptured epidural veins or cancellous bone due to displacement of unstable fractures, can be adequately visualized or excluded using an MRI scan. 64 –66
In conclusion, suspected fractures justify the use of high-resolution imaging techniques for the entire spine, to evaluate concomitant injuries in other spinal regions and to avoid overlooking fractures with initially mild symptoms. 22,55,67
Surgical Therapy for Cervical Spine Fractures
Ankylosed cervical spine segments result in long lever arms, with a 5-fold higher risk of clinical spine fractures in comparison to the normal population with spine fractures, as reported by Prieto-Alhambra et al. 6 Particularly in patients with AS, this excessive increased risk peaks in the first 2.5 years after the onset of the disease. The combination of long lever arms with the comorbidity of osteoporosis indicates the problems faced in the surgical treatment of these patients using anterior, posterior, or combined procedures. 26,68 –71
Following the introduction of the anterior cervical approach by Smith and Robinson in the 1960s, the conventional discectomy was expanded into an anterior cervical corpectomy, including one or more cervical levels, in order to decompress the neural structures and accomplish fusion, or at least reconstruct the cervical spine using special cage systems. High rates of implant-related failures were observed with the use of anterior-only instrumentations. This can be explained by the accompanying fractures of the dorsal spine elements, which are characteristically transverse and often remain undetected, as mentioned above. 20 Anterior-only instrumentation may then cause implant failures, so that circumferential instrumentation would be preferable. 69,71 –73 Due to the accompanying comorbidities in the patients affected (especially cardiovascular and pulmonary problems), a circumferential approach might lead to a high level of perioperative risk among the patients affected. If a circumferential approach is not feasible, a posterior-only approach should be considered. 5,74
Most of the research groups identified in the literature search used a dorsal approach to treat patients with cervical fractures, but without accurate descriptions of the rationale behind this treatment strategy. 2,10,41,51,75 However, several groups also used an anterior or combined anterior-posterior approach with satisfactory results, either planned after the index procedure or after implant failure. 41,63,68,69,71 –73,76
In conclusion, most of the patients described in the literature have been treated with multilevel posterior segmental fixation, using bilateral fixation points above and below the affected cervical levels. 2,3,5,32,68,74,77 Surgical stabilization may also improve the survival among patients with spinal fractures related to AS. 74,78 In patients with anterior cervical decompression, especially in corpectomy approaches, additional dorsal instrumentation is advocated in order to reduce implant-related complications. 20 As reported in the literature, good neurological recovery is observed in many surgically treated patients. 56,74,77 –80
Complications
The complication rates for AS and DISH reported in the literature range from approximately 30% to 50%, with a trend toward increased complications due to DISH. 2 One of the most feared complications is secondary deterioration due to an initially overlooked and delayed diagnosis of cervical fractures. 2,3,20,33,40,43,81 The mortality rate among patients with surgically treated spine fractures in AS and DISH is reported in the literature to be approximately 18%. The higher mortality rate among trauma patients suffering from DISH, especially during the course of follow-up and regardless of the treatment option, may be explained by the etiology of the disease, associated with disorders of the metabolism, obesity, and advanced age. 82 –85
Finally, concomitant epidural hematomas, lacerations of the aorta (lower spine), and ruptures of the trachea in patients with AS have also been reported. 64,65,80,86,87 In contrast to AS, cervical spine complications among DISH patients consist of myelopathy with spinal canal stenosis, dysphagia, and difficult endotracheal intubation when anesthesia is being administered. 2,88,89
In general, the overall complication rate appears to be greater among conservatively treated patients. 2 Most patients selected for conservative management have been treated with a cervical collar (DISH) or cervical traction devices (AS). 3,90,91 The high proportion of brace therapy among DISH patients may possibly reflect the high incidence of thoracic fractures in this disease entity. 2 In general, based on the published data, the overall morbidity and mortality appear to be greater among patients treated conservatively than among their surgical counterparts. 2,91
Pneumonia and respiratory insufficiency, postoperative deep venous thrombosis, and wound infections are frequent postoperative complications among ASD patients. 2,3,77 Pulmonary infections and associated respiratory insufficiency in particular lead to fatal outcomes in both disease entities. 2,3,22
Mortality
The mortality associated with spine fractures among surgically treated patients with ASD is approximately 7% to 25%, based on our analysis of the literature. 2,3,10,22,51,68,77 Regression analyses show that age, the presence of DISH, neurologic deficits, cardiac diseases, the number of additional comorbid conditions, and also a low-energy mechanism of injury are predictive of increased mortality. 2,3,10 In particular, lacerations of the aorta or trachea and pneumonia with or without respiratory failure appear to be the severe complications mostly associated with fatal outcomes. 2 For both entities (AS and DISH), pulmonary complications appear to be the most common cause of death. The mortality rate among surgically treated patients is reported to be lower than among those receiving conservative treatment. 2
Conclusions
Ankylosing spinal disorders lead to progressive ossification of the spinal column, due to bridging bone formations in the spinal segments involved. An increased incidence of cervical spine fractures, particularly due to low-energy trauma, is observed among patients suffering from AS and DISH. This high susceptibility to trauma even after low-energy impacts may lead to a delay in the diagnosis of these fractures, contributing to initially misinterpreted clinical symptoms and inadequate imaging investigations, partly due to the lack of knowledge of the peculiarities of the disease. Secondary deterioration due to initially unstable fractures with neurologic compromise, associated with low recovery rates, is a frequent problem with these diseases. Thorough assessment of the patients’ neurological morbidity and additional radiography, MRI, and CT at admission should reduce the prevalence of overlooked fractures. The overall complication rate appears to be higher among conservatively treated patients. Conservative treatment usually involves cervical collars (DISH) or cervical traction devices (AS). In patients who receive surgical therapy after cervical spine fractures, a multisegmental posterior approach is preferable, followed by anterior instrumentation or circumferential approaches.
Key Points
There is an increased incidence of cervical spine fractures (after low-energy impacts) in patients suffering from AS and DISH.
There is a high risk of delayed diagnosis, with secondary deterioration due to unstable fractures.
Patients suffering from AS and DISH are at high risk of neurologic compromise, associated with low recovery rates.
If a fracture is only suspected, multislice high-resolution imaging techniques are advocated.
Posterior instrumentation or circumferential approaches are recommended, due to high failure rates with anterior-only fixations.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
