Abstract
Background:
Hand sanitizer use increased dramatically during the COVID-19 pandemic, yet knowledge about its safe use and potential health impacts remains limited, particularly across different occupational groups. There is a need to better understand the frequency and health effects of hand sanitizer use, especially when comparing healthcare professionals and non-healthcare professionals.
Methods:
This cross-sectional study included 305 adults from a central district of Türkiye, with 48.5% being healthcare professionals. Data were collected on participants’ knowledge of sanitizer contents, frequency of use, and any health problems experienced. Regression analysis was performed to identify factors associated with sanitizer-related health problems.
Results:
Only 28.4% of healthcare professionals and 12.1% of non-healthcare professionals reported full knowledge of the contents of the sanitizers they used. Daily use of hand sanitizer 10 or more times was reported by 53.4% of healthcare professionals and 33.8% of non-healthcare professionals. Regression analysis indicated that female gender and being a healthcare professional were significantly associated with sanitizer-related health problems (p < .01). Despite frequent use, both groups demonstrated insufficient knowledge regarding safe sanitizer use, which may contribute to increased health risks such as skin irritation or allergic reactions.
Conclusions:
These findings highlight the importance of implementing targeted, evidence-based educational interventions and developing clear guidelines on the safe use of hand sanitizers for both healthcare and non-healthcare professionals. Future studies should focus on the effectiveness of these interventions in reducing healthcare-associated infections and improving hygiene practices.
Application to Practice:
Occupational health and public health professionals can use these results to design workplace and community-based training programs, promote safer hygiene practices, and minimize sanitizer-related health risks across diverse populations.
Background
The COVID-19 pandemic has emerged as a challenging global public health issue, profoundly affecting public health and daily life. According to the World Health Organization (2025), approximately 775 million people worldwide have been infected, and more than 7 million deaths have been reported. With the pandemic, hand hygiene has become the cornerstone of preventive strategies against viral transmission. The World Health Organization (WHO) and the U.S. Centers for Disease Control and Prevention (CDC) recommend the use of alcohol-based hand sanitizers containing at least 60% alcohol when soap and water are not available (CDC, 2024) and for their ease and effectiveness in reducing microbial presence (Ambrosino et al., 2022; Bayer et al., 2023).
This increased use of hand sanitizers during the pandemic has raised questions about their effectiveness and potential health effects, especially in different occupational groups (W. Chen et al., 2023; Dhama et al., 2021). Healthcare professionals, who have been at the forefront of the pandemic response, have been subject to rigorous hygiene protocols requiring frequent use of hand sanitizers (European Centre for Disease Prevention and Control, 2020). In this context, there has been a marked increase in hand sanitizer use among healthcare professionals. Similarly, the general population has also increased the use of these products due to public health recommendations and personal safety concerns. The U.S. CDC has stated that, unlike soap and water, sanitizers do not eliminate all microorganisms, are less effective when hands are visibly dirty, and cannot remove harmful chemicals (CDC, 2024). The CDC recommends that, when applied, the sanitizer cover all hand surfaces rubbing in the sanitizer until dry (CDC, 2024).
Despite the widespread use of hand sanitizers, there is a notable gap in the current literature regarding their composition and the potential health risks associated with overuse or misuse (F. Chen & Xu, 2024; Rianto et al., 2024). Repeated exposure to the chemical components of hand sanitizers can lead to adverse health effects such as skin irritation, contact dermatitis, and respiratory symptoms (European Centre for Disease Prevention and Control, 2020; Hashemi et al., 2023). Lack of knowledge about proper hand sanitizer use may exacerbate these side effects (Hashemi et al., 2023; Rianto et al., 2024).
This study aims to investigate the frequency of hand sanitizer use among adults during the pandemic, with a specific focus on comparing the frequency, knowledge, and health outcomes associated with its use between healthcare professionals and non-healthcare professionals. By examining frequency of use, knowledge of sanitizer ingredients, and associated health outcomes, this research aims to provide a comprehensive understanding of the effects of hand sanitizer use. Understanding these dynamics is crucial for developing targeted educational interventions and guidelines to ensure safe and effective hand hygiene practices.
The findings of this study are expected to contribute to the existing body of knowledge by underlining the need for evidence-based education and policy-making in hand hygiene practices. Such measures are necessary not only to reduce potential health risks but also to improve the overall effectiveness of hand hygiene practices, both in healthcare settings and in the wider community. As the world continues to navigate the challenges posed by the pandemic, understanding the nuances of hand sanitizer use will be vital in shaping future health policies and practices.
Methods
Study Design
This study was designed as a cross-sectional investigation to evaluate the frequency of hand sanitizer use among adults (heathcare and non-healthcare professinals) during the pandemic and its impact on health outcomes. The reporting of the study was conducted in accordance with the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines.
Study Participants, Sampling and Recruitment
Study Participants
The participants of this study were individuals aged 18 and older residing in the Gölbaşı district.
Sample Sampling and Recruitment
A simple random sampling method was employed to ensure that the sample was representative of the population in the Gölbaşı district. The sample size was calculated using the Epi-Info program, based on the 2024 population of Gölbaşı (165,201). Parameters used in the calculation included a 95% confidence interval, a 5% margin of error, and an expected frequency of hand sanitizer use of 90%.
Stratification was carried out according to profession to create two strata’s: healthcare professionals and non-healthcare professionals.
Sampling strata’s;
Healthcare professionals (HCP): An official roster of all actively working healthcare professionals in Gölbaşı was obtained from the District Health Directorate. The roster included physicians/dentists, nurses/midwives, home-care workers, and public-health workers involved in patient-facing services.
Non-healthcare professionals (Non-HCP): Adults (≥18 years) registered in district population records who were not listed as non-healthcare professionals. Reported occupations included education (teachers/academics), service sector (waiters, cleaners, barbers/hairdressers), self-employed, unemployed/housewives, retired, and other.
Recruitment procedure
For the healthcare professional (HCP) stratum (N = 2,800), an official roster of all HCPs actively working in the Gölbaşı district during the pandemic was obtained from the District Health Directorate. For the non‑healthcare professional (non‑HCP) stratum (N = 128,400), the sampling comprised adults registered in the district population records who were not listed as HCPs (N = 2,800). Within each stratum, individuals were assigned unique identification numbers and selected using computer‑generated simple random numbers to meet the target sample sizes (HCP n = 148; non‑HCP n = 157).
Selected participants were contacted by trained research staff via face-to-face and/or telephone, informed about the study, and invited to participate.
If a person selected from the sample could not be reached or declined, the next person on a pre-established random backup list from the same process was invited to continue the random sampling.
Inclusion and Exclusion Criteria
Inclusion Criteria
Individuals residing in the Gölbaşı district.
Adults aged 18 and over during the study period.
Individuals who voluntarily agreed to participate in the study.
Exclusion Criteria
Individuals under the age of 18.
Individuals with pre-diagnosed chronic health issues directly related to hand sanitizer use, such as dermatological or respiratory diseases.
Pregnant or breastfeeding women during the pandemic.
Instrument
The data collection tool was developed by the researchers based on a comprehensive literature review (Ambrosino et al., 2022; F. Chen & Xu, 2024; Hashemi et al., 2023; Rianto et al., 2024). The tool consisted of three main sections:
Descriptive Characteristics: This section included five items covering demographic information, including age, gender, education level, occupation, and income status. These variables were included to understand the participants’ background and to enable stratified analyses.
Hand Sanitizer Use During the Pandemic: This section included four items focusing on participants’ hand sanitizer use. The questions addressed:
Hand sanitizer content knowledge
Type of hand sanitizer used (e.g., alcohol-based, solid-liquid antimicrobial soap, or corrosive substances).
Frequency of daily hand sanitizer use (e.g., once, 2–3 times, 4–6 times, 7–9 times, or 10 or more times).
Change in use during the pandemic.
Health Outcomes Related to Hand Sanitizer Use: This section included 12 items designed to assess health issues potentially associated with hand sanitizer use. These items were developed by researchers based on the most commonly reported side effects in the literature (Hashemi et al., 2023; Rianto et al., 2024). Each item was scored on a 5-point Likert scale, ranging from 1 (never) to 5 (always). The total score ranged from 12 to 60, with higher scores indicating greater severity of health problems related to hand sanitizer use. The items included:
Does your skin peel after each use?
Do your hands feel dry after each use?
Do you get redness on your hands after each use?
Are your eyes sensitive and itchy after each use?
Do your eyes get red after each use?
Is your nose irritated and itchy after each use?
Does your nose run after each use?
Is your throat itchy and irritated after each use?
Do you cough and sneeze after each use?
Do you get red, itchy, or burning skin after each use?
Do you experience headaches and dizziness after each use?
Do you feel nausea after each use?
A pilot study was conducted with a small group of participants (n = 30) prior to the main study. Pilot study feedback was used to refine the questions, ensuring they were understandable and aligned with the study questions. While the tool was not validated in a traditional sense, the pilot study helped establish questionnaire face validity for the specific context of this research. Reliability was not tested. The questionnaire used in the study is included as Supplemental Appendix.
Data Collection Procedure
Using the questionnaire, data collection was carried out between September and November 2024 in the Gölbaşı district. After informing participants verbally about the purpose and scope of the research, they were asked to participate voluntarily, and written consent was obtained. The data were collected through structured face-to-face interviews by Gölbaşı district health directorate personnel. After the interviewers had contacted the participants at their addresses, the questionnaire was administered in a private and comfortable setting, either in the participants’ homes or workplaces, depending on their preference and convenience. If face-to-face interviews were not possible, an online option was offered.
All interviewers received training on the questionnaire and data collection procedures prior to the study including such areas as:
Written informed consent, standardized script for study introduction, and protocols for privacy and confidentiality
Addressing questions about hand‑sanitizer safety without giving advice and providing referral information for dermatologic/respiratory complaints when needed
Using pre‑specified neutral probes; checking completeness before leaving/resolving inconsistencies immediately
Bias minimization (no interpretation or coaching)
Infection‑prevention measures (e.g., hand hygiene, mask use when requested, and maintaining physical distance during interviews
Security and data protection
During the interviews, participants were encouraged to provide honest and accurate responses. The interviewers ensured that all questions were clearly understood by the participants and provided clarifications when necessary.
At the end of each day, the collected data were reviewed and verified for completeness and accuracy by the authors. Any missing or unclear responses were followed up with participants by phone, if possible, to ensure data quality.
Data Analysis
This research analyzed data using licensed IBM SPSS software (IBM SPSS Statistics for Windows, Version 30.0). Demographic variables were summarized with descriptive statistics, including frequencies, percentages, means, and standard deviations. Group comparisons were conducted using independent t-tests for two groups (e.g., gender, profession) and one-way ANOVA for more than two groups (e.g., economic status) to assess whether outcome scores differed significantly between the groups. Multiple linear regression modeling was then applied to identify predictors of health outcomes related to hand sanitizer use, examining the contribution of independent variables such as profession, gender, economic status, and frequency of use. Effect sizes were calculated using Cohen’s d, interpreted as small (0.2), medium (0.5), and large (0.8). Statistical significance was set at p < .05 with a 95% confidence interval.
Ethical Considerations
Ethical approval was obtained from the Ankara University Ethics Committee (Approval No: 2024/468). Written institutional permission was also obtained from the institution where the research was conducted. Participants were informed about the study, and written consent was obtained by completing an informed consent form, ensuring voluntary participation. Data collected during the study were stored in accordance with confidentiality and anonymity principles and were used solely for research purposes. The study was conducted in accordance with the principles of the Declaration of Helsinki.
Results
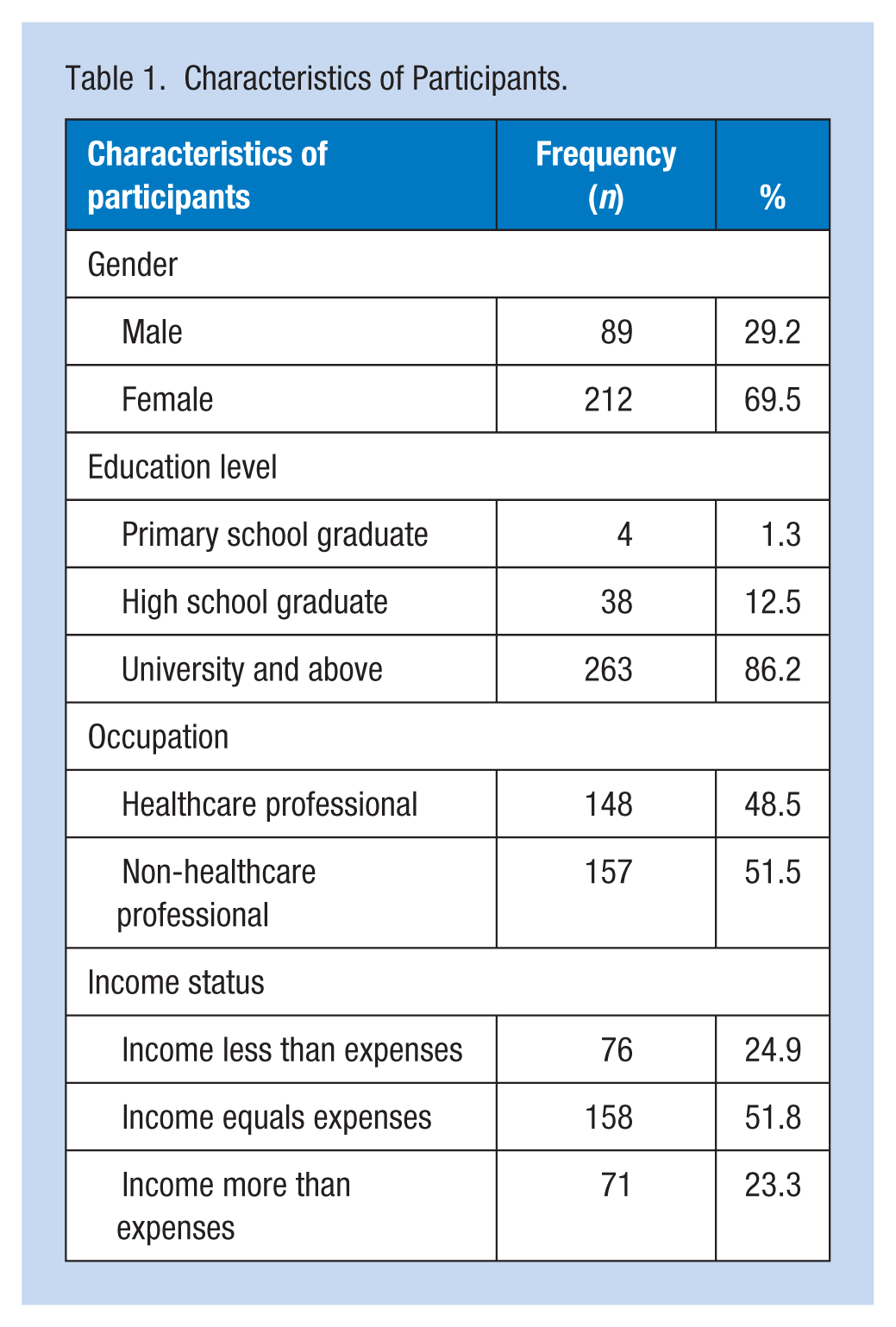
Among the participants, 29.2% were male and 69.5% were female, with 86.2% having a university education or above. It was determined that the income status of 75.1% of the participants was equal to or above their income and expenses. In addition, 48.5% of the sample consisted of healthcare professionals (Table 1).
Characteristics of Participants.
In the study, 100% of healthcare professionals and 99% of non-healthcare professionals used hand sanitizer. As shown in Table 2, 28.4% of the healthcare professionals and 12.2% of the non-healthcare professionals completely knew the content of the hand sanitizers. When asked about the types of hand sanitizers used, 85.8% of the healthcare professionals used solid-liquid antimicrobial soap, 84.4% used alcohol-based hand sanitizers, and 35.1% used corrosive substances (tincture of iodine, Lugol’s solution, povidone iodide, etc.), detergent, hydrogen peroxide, and sodium hypochlorite. Among non-healthcare professionals, 86.6% used solid-liquid antimicrobial soap, 88.5% used alcohol-based hand sanitizers, and 46.4% used corrosive substances. Daily hand sanitizer use of 10 or more times was reported by 53.4% of healthcare professionals and 34.0% of non-healthcare professionals.
Hand Sanitizer Content Knowledge, Types of Hand Sanitizer Used, and Frequency of Hand Sanitizer Use by Profession.
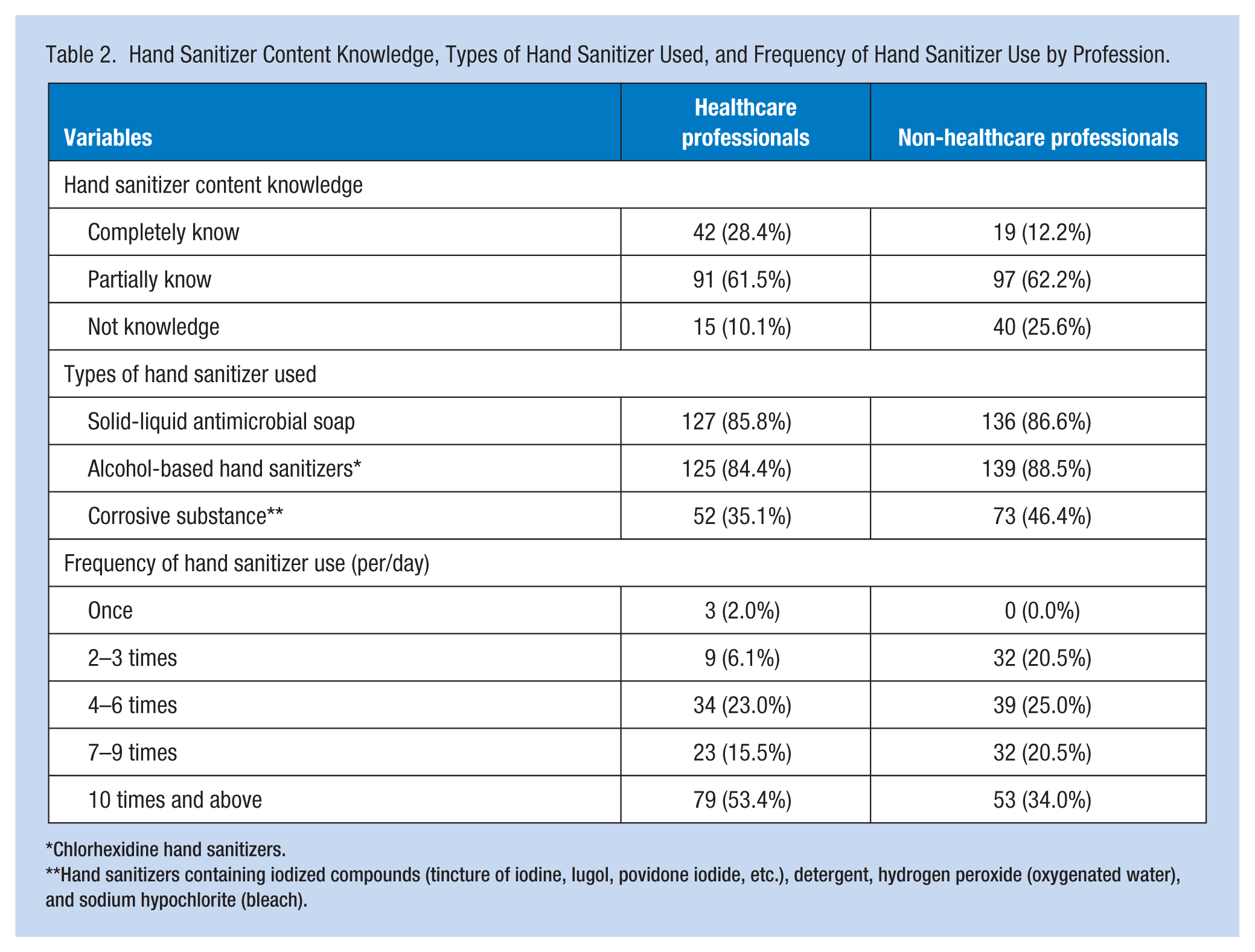
Chlorhexidine hand sanitizers.
Hand sanitizers containing iodized compounds (tincture of iodine, lugol, povidone iodide, etc.), detergent, hydrogen peroxide (oxygenated water), and sodium hypochlorite (bleach).
As shown in Table 3, significant relationships were found between health outcome scores associated with hand sanitizer use and several participant characteristics, including profession (t = 4.75, p < .001), gender (t = −5.53, p < .001), economic status (F = 3.44, p = .033), hand sanitizer usage frequency (t = −1.99, p = .047), and solid-liquid antimicrobial soap usage (t = −2.04, p = .045). However, no significant relationships were observed for hand sanitizer content knowledge (F = 0.21, p = .81), hand sanitizer use (t = −1.34, p = .18), and corrosive substance use (t = 0.07, p = .946).
Examination of Outcome Scores Associated With Hand Sanitizer Use According to the Characteristics of Participants and Hand Sanitizer.
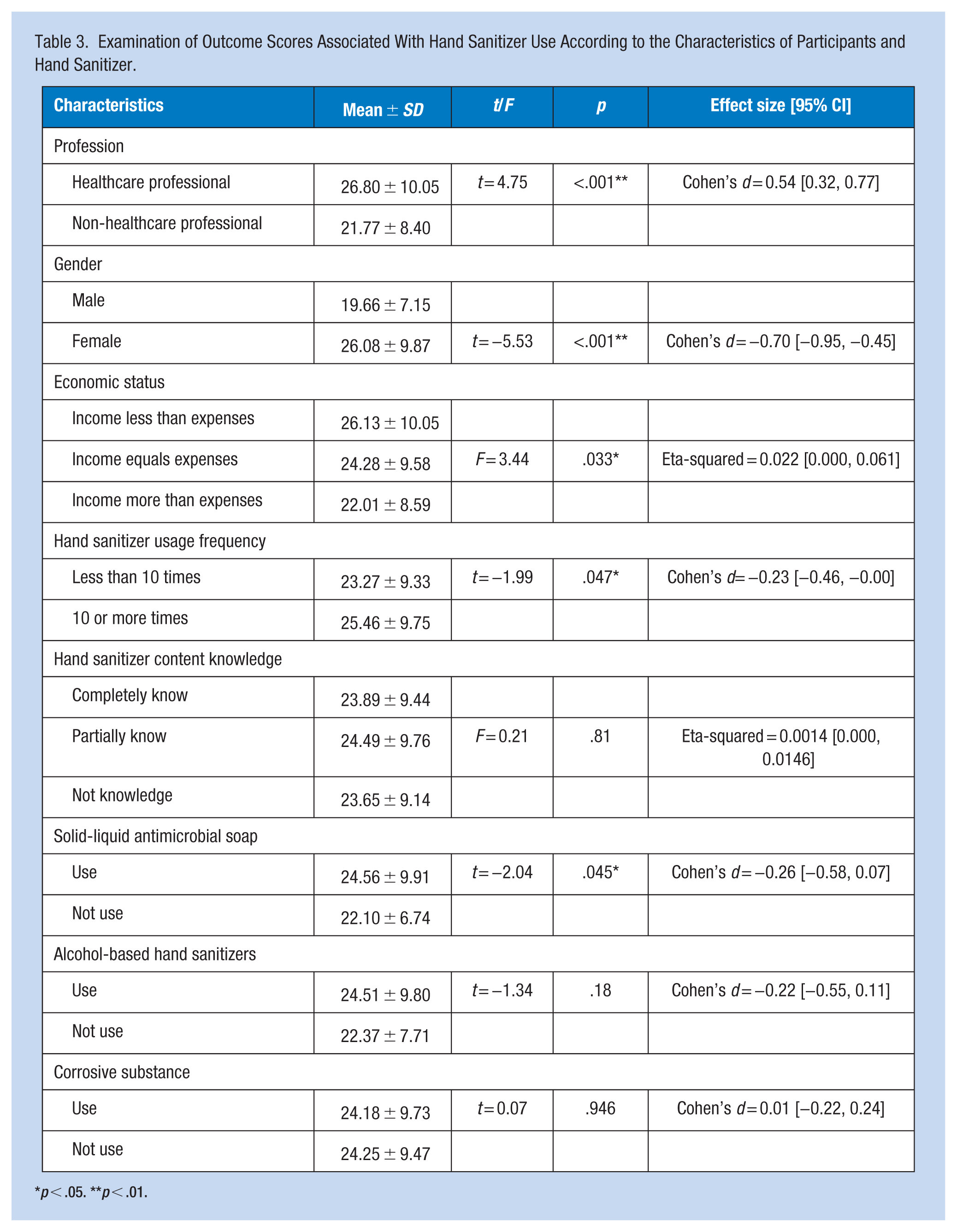
p < .05. **p < .01.
Multiple linear regression analysis revealed that female gender (β = .22) and being a healthcare professional (β = .16) significantly predicted adverse health outcomes associated with hand sanitizer use (p < .01). These outcomes primarily involved dermatological issues, such as skin irritation or dryness, and respiratory symptoms related to frequent use. However, income status, frequency of hand sanitizer use, and soap use were not significant predictors. Overall, predictive factors accounted for 14% of the variance in health outcomes (R² = .14, p < .001), as determined through multiple linear regression analysis using the data presented in Table 4.
Predictive Factors of Health Outcomes Associated With Hand Sanitizer Use.
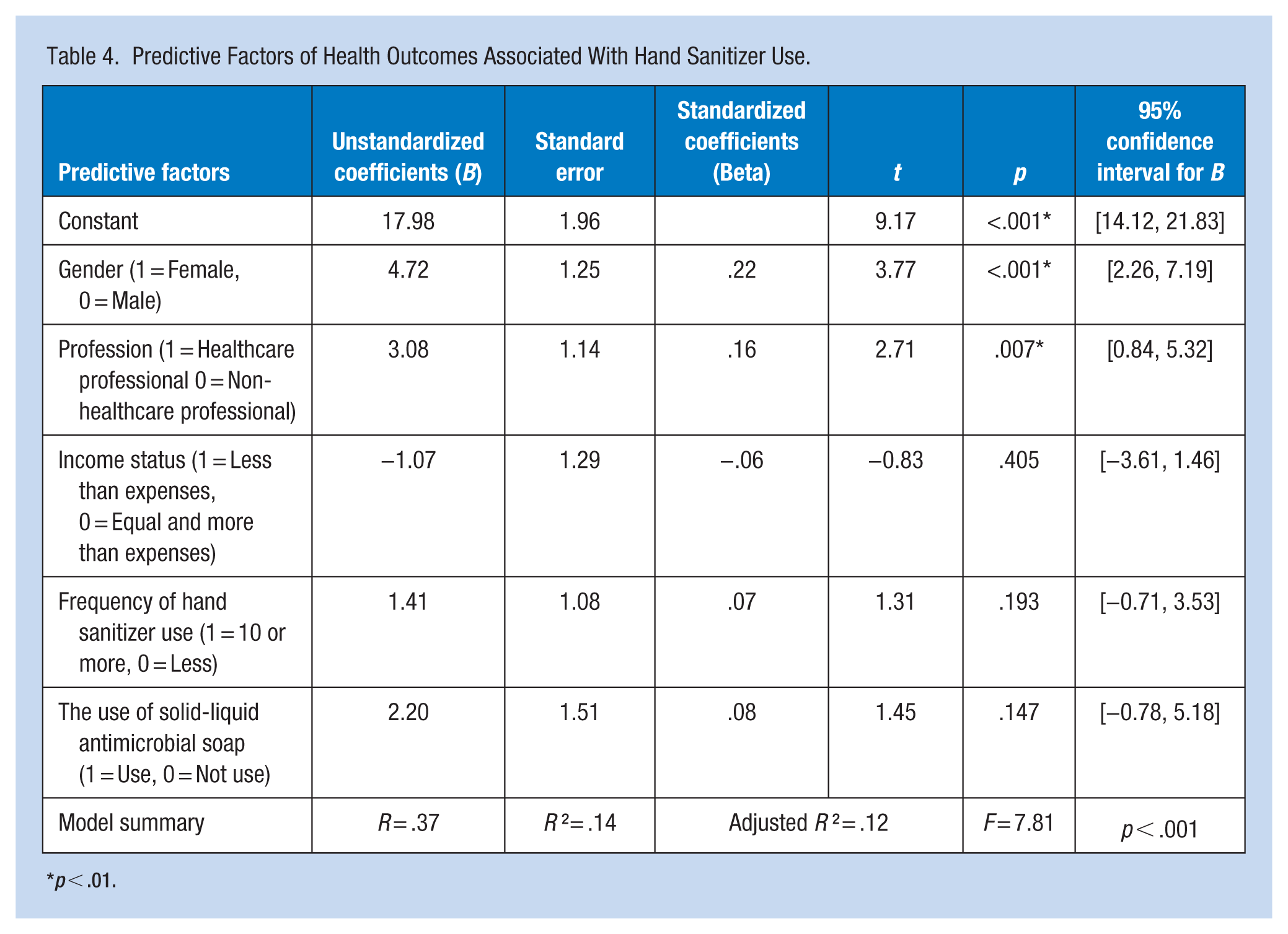
p < .01.
Discussion
The COVID-19 pandemic has highlighted the critical role of hand hygiene in prevention infection, making hand sanitizer use an essential and widespread practice globally. However, while these measures have been pivotal in controlling the spread of infections, the unintended consequences of improper or excessive use of hand sanitizers have emerged as a growing public health concern (Mahmood et al., 2020). This study provides valuable insights into the frequency of hand sanitizer use and health impacts, focusing on healthcare and non-healthcare professionals. The findings reveal gaps in knowledge about the content and safe use of hand sanitizers, emphasizing the urgent need for focused education and evidence-based guidelines to mitigate associated health risks.
The high frequency of hand sanitizer uses among both healthcare professionals (100%) and non-healthcare professionals (99%) found in our study was in line with global trends reported during the pandemic (Assefa et al., 2021; Czeisler et al., 2020). A study conducted in Italy reported that use in hospitals increased by 105%, and the increase was also seen in the general population (Mengato & Di Spazio, 2022). Although the use of hand sanitizers has become an important issue for both healthcare professionals and the general population during the pandemic period, the lack of knowledge about the ingredients of hand sanitizers, especially among non-healthcare professionals, is of concern. This finding is consistent with previous research showing that the general population often lacks adequate knowledge about the chemical composition and potential risks of hand sanitizers (Alwan et al., 2023; Aridi et al., 2024). Limited knowledge among healthcare and non-healthcare professionals about the content of the hand sanitizers underscores the need for targeted education and training.
Our study revealed that low socioeconomic status and frequent hand sanitizer use were associated with adverse health outcomes, and that female gender and being a healthcare professional were important determinants. In a similar study, it was reported that while healthcare professionals had better quality hand hygiene facilities and more focused education compared to the public, adherence to the recommended actions by WHO guidelines on hand hygiene remained at a low level (Horng et al., 2016). Previous research has shown that healthcare professionals are at higher risk of developing skin-related problems such as dermatitis and irritation from repeated use of alcohol-based hand sanitizers and other disinfectants due to occupational exposure. In one study, hand dermatitis in healthcare professionals was reported to be 3% in the pre-pandemic period and 83% during the pandemic period (Abhishree et al., 2023). Roy et al. (2022) revealed that healthcare professionals experienced 3.5 times more skin symptoms related to hand sanitizer use than the general population, with those using alcohol-based sanitizers experiencing more itching and those using soap experiencing more skin peeling and redness. Alsaidan et al. (2020) provided data for the general population during the pandemic period and found that 34.8% reported hand dermatitis and 15.3% reported facial dermatitis, with more skin problems in women and those who worked in jobs requiring frequent hand hygiene, like healthcare professionals. In another study conducted on healthcare professionals, it was reported that 23.2% of healthcare professionals experienced skin problems due to the use of hand sanitizers, and the use of hand sanitizers 10 or more times a day was significant (El-Hadidy et al., 2022). In light of these findings, it should be considered that healthcare professionals, due to their occupational exposure, may be at higher risk of developing skin-related problems such as dermatitis and irritation from repeated use of alcohol-based hand sanitizers and other disinfectants.
The finding that female participants reported more health problems could be attributed to biological differences in skin sensitivity as well as potential differences in hand hygiene practices between genders. While frequency of hand sanitizer use was significantly associated with health outcomes in the univariate analysis, it did not emerge as a significant predictor in the multivariate model. This suggests that other factors, such as the type of hand sanitizer used and individual susceptibility, may play a more critical role. Of particular concern is the frequency of use of corrosive substances. These substances, including hydrogen peroxide and sodium hypochlorite, are known to cause skin and respiratory irritation (Clausen et al., 2020; Goh et al., 2021), but their use continues to be widespread. This situation may be due to misunderstanding about their effectiveness.
Conclusions
In conclusion, this study highlights the urgent need for improved education, regulation, and awareness regarding the safe use of hand sanitizers, particularly in the context of a pandemic. The findings show gaps in knowledge and practice, with healthcare professionals and women disproportionately affected by reported adverse health impacts of frequent hand sanitizer use. These results highlight the importance of targeted interventions to protect at-risk groups and promote safer practices. By addressing these gaps with evidence-based education and stricter regulations, public health authorities can not only reduce the health risks associated with hand sanitizer use but also increase the overall effectiveness of infection control measures. Moreover, these efforts will strengthen preparedness for future pandemics and ensure that infection prevention strategies are both effective and safe for everyone.
Implications for Occupational Health Practice
The findings of this study underscore several critical implications for occupational health practice. First, the high prevalence of hand sanitizer uses among both healthcare and non-healthcare professionals, coupled with significant gaps in knowledge regarding product content and safe usage, highlights the urgent need for comprehensive, evidence-based educational interventions in the workplace. According to the Centers for Disease Control and Prevention (CDC), alcohol-based hand sanitizers containing at least 60% alcohol are recommended when soap and water are not available. However, CDC also emphasizes that hand sanitizers are not effective against all microorganisms, are less effective when hands are visibly dirty, and cannot remove harmful chemicals. These recommendations align with the findings of this study, which revealed a lack of knowledge about hand sanitizer use among participants.
Occupational health professionals should prioritize the development and implementation of targeted training programs that address not only the importance of hand hygiene but also the potential risks associated with improper or excessive use of hand sanitizers. These programs should incorporate CDC guidelines to ensure that employees are educated on the appropriate use of hand sanitizers, including when and how to use them effectively, and the importance of using soap and water when hands are visibly soiled. By aligning workplace training programs with CDC recommendations, organizations can promote safer and more effective hand hygiene practices, ultimately reducing the risk of adverse health outcomes associated with improper hand sanitizer use.
Given that healthcare professionals and women are disproportionately affected by adverse health outcomes such as dermatitis and skin irritation, occupational health policies should include regular risk assessments and proactive monitoring of skin health, especially for high-risk groups. The provision of skin protection products, such as moisturizers and barrier creams, should be integrated into workplace safety protocols, and employees should be educated on their correct use.
Furthermore, the widespread use of corrosive substances like hydrogen peroxide and sodium hypochlorite, possibly due to misconceptions about their effectiveness, points to the necessity of clear, accessible guidelines on the selection and safe use of disinfectants. Occupational health practitioners should collaborate with management to ensure that only approved, safe products are available in the workplace and that employees are trained to read and understand product labels.
Institutions should also establish reporting and follow-up mechanisms for adverse reactions related to hand sanitizer use, enabling early intervention and continuous improvement of workplace hygiene practices. Finally, these findings highlight the importance of integrating occupational health considerations into broader public health campaigns, ensuring that both healthcare and non-healthcare workers receive consistent, accurate information and support. By adopting a proactive, education-focused approach and fostering a culture of safety and awareness, occupational health professionals can help reduce the risk of sanitizer-related health problems, enhance overall workplace well-being, and improve preparedness for future public health emergencies.
Applying Research to Occupational Health Practice
This study found frequent sanitizer use but limited knowledge of product contents with sanitizer‑related symptoms more common among women and healthcare workers. To translate these findings into practice, occupational health programs should deliver brief, targeted education on when to choose sanitizer versus soap and water, application (adequate volume, 20–30 seconds of rubbing, allow to dry), avoidance on damaged skin, and basic label literacy emphasizing compliant alcohol levels and potential irritants such as fragrances or additives. Organizations should standardize procurement to low‑irritant, regulation‑compliant formulations and place compatible moisturizers near dispensers to prevent irritant dermatitis. Routine skin‑health screening in high‑use areas, coupled with a simple adverse‑event reporting and follow‑up process, can detect problems early. Posting concise job aids at points of use and providing periodic refreshers will reinforce correct technique. Messaging tailored for higher‑risk groups and ensuring convenient access to handwashing alternatives will maintain hygiene without increasing skin reactions. These low‑cost strategies can reduce dermatitis and allergy complaints while sustaining effective hand hygiene.
Supplemental Material
sj-docx-1-whs-10.1177_21650799251392217 – Supplemental material for Hand Sanitizer Use During the Pandemic: Frequency and Health Effects Among Healthcare and Non-Healthcare Professionals
Supplemental material, sj-docx-1-whs-10.1177_21650799251392217 for Hand Sanitizer Use During the Pandemic: Frequency and Health Effects Among Healthcare and Non-Healthcare Professionals by Burak Kurt and Hazal Ozdemir Koyu in Workplace Health & Safety
Footnotes
Acknowledgements
We would like to thank the Gölbaşı District Health Directorate team and Dr. Ülgen GÜLLÜ for their support in fieldwork and data collection.
Author Contributions
Burak Kurt: Conceptualization, Methodology, Data analysis, Writing-Original draft preparation, Writing-Reviewing and Editing. Hazal Ozdemir-Koyu: Conceptualization, Methodology, Data analysis, Writing-Original draft preparation, Writing-Reviewing and Editing.
Conflict of Interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Ethical approval was obtained from the Ankara University Ethics Committee (Approval No: 2024/468).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
