Abstract
The objective of this study was to assess work-related hygiene practices and the frequency and location of skin rashes due to cutaneous contact with crop-associated materials (e.g., pesticides) for female nursery and fernery workers in Central Florida. A cross-sectional, community-based participatory research study of 237 female nursery and fernery workers between the ages of 19 and 43 years with significant cutaneous contact with foliage crops was conducted using a self-report questionnaire and a skin rash chart assessment tool. Of the 237 farmworkers surveyed, 37.1% (n = 88) reported a rash on at least one area of their bodies. Women who were pregnant during the study were 4.7 times more likely to report more than 30% total body surface area (TBSA) covered by rash compared with non-pregnant fernery workers (p = .045; 95% confidence interval [CI] [1.04, 21.35]). Further research is needed to better understand the development of skin rashes among farmworkers, to generate effective prevention strategies.
Keywords
Occupational exposures affecting the skin are the second most frequent cause of occupational health disorders in the world with contact dermatitis (CD) being the most common occupational skin disorder (Centers for Disease Control and Prevention [CDC], 2013). Contact dermatitis is the inflammation of the upper layers of skin and may appear as dryness, redness, itching, flaking, scaling, cracking, or blistering (Behroozy & Keegel, 2014; CDC, 2013). Physical and environmental factors are the primary causes of CD, followed by skin irritation due to an allergic reaction (Behroozy & Keegel, 2014). Chemical pesticides (i.e., insecticides, fungicides, and herbicides) are commonly used in agriculture. Health effects of pesticide exposure can vary depending on the chemical, the individual, and the working environment (e.g., route, duration, and chemical concentration of exposure; the workers’ age and use of skin care products; and ambient temperature and humidity; MacFarlane, Carey, Keegel, El-Zaemay, & Fritschi, 2013). In addition, the individual body part exposed to a pesticide significantly affects the rate of absorption. For instance, absorption occurs more quickly in the genital area, head, and trunk than the forearms (MacFarlane et al., 2013; Poet, 2000).
To protect farmworkers from exposure to pesticides and plants, the use of personal protective equipment (PPE; e.g. gloves, boots, coveralls, hats, and long-sleeved shirts) is highly recommended. United States Environmental Protection Agency (USEPA; 2006) recommended PPE for handler employees who mix and apply pesticides and remove pesticide residue as well as early entry workers. The USEPA (2006) also recommended employers and employees refer to the “Hazards to Humans” section on pesticide labels for specific precautions. Furthermore, the type of material (e.g., cotton vs. polypropylene fabrics), the weight and thickness of the fabric, and how PPE is used can determine the effectiveness of PPE in limiting exposure. However, the use of PPE across all types of agriculture remains low (MacFarlane et al., 2013); limited PPE use can be due to lack of employer provision of equipment or lack of proper education on the necessity of PPE use (Flocks, Monaghan, Albrecht, & Bahena, 2007). Heat stress also plays a significant role in PPE use with the National Institute of Occupational Safety and Health (NIOSH; 2016) reporting 423 worker deaths (16% of deaths were crop workers) due to heat stress from 1992 to 2006.
Only a small percentage of farmworkers have direct contact with liquid pesticides when they are mixing and applying pesticides or cleaning equipment used in the application of pesticides (Clarke, Cordery, Morgan, Knowles, & Guy, 2015). Currently, dermal exposure to pesticides is calculated based on a specific dose of the liquid form of a product but is not based on exposure to dried residue that remains on plants and is transferred to the skin (Clarke et al., 2015). For farmworkers, the majority of pesticide exposures are to dried residue found on plants (Clarke et al., 2015). Pesticide residue remains on plants for an unknown amount of time; little is known about the outcome of this exposure.
Nursery workers are a subpopulation of farmworkers who care for ornamental plants (e.g., cut flowers, potted plants, foliage, garden plants, and landscape plants) and perform a variety of work tasks (e.g., planting at conveyor belts, loading pots of plants into trays, and loading and carrying trays, boxes, and bags of soil). In Florida, this work is typically done within enclosed environments, specifically plastic or glass greenhouses. Fernery workers cut ornamental foliage (e.g., florists’ greens) in fields under black mesh shade cloth or large shade trees. The main work task of fernery workers includes bending over to cut fronds at the base and gathering and transporting bunches of 20 to 25 fronds (Flocks, Kelley, Economos, & McCauley, 2012).
This study examined the prevalence of skin rashes on farmworkers related to occupational and environmental exposures, including pesticides used in agriculture. A previous survey with 382 Central Florida male and female fernery and nursery workers showed that nearly 80% of fernery workers and 30% of nursery workers reported experiencing skin rashes they believed to be associated with pesticide exposure (Mayer, Flocks, & Monaghan, 2010). The current study piloted a skin rash diagram to document the frequency and location of self-reported skin rash among female nursery and fernery farmworkers. The analysis of rash frequency and rash location was compared with job activities, workplace practices, work-related hygiene practices, and access to field sanitation facilities and supplies.
Method
This CD study was nested within a larger community-based participatory research project designed to study pregnancy health among childbearing-aged women in Florida (R21OH009830). A cross-sectional design was used to compare workplace characteristics, work-related hygiene practices, and health beliefs of female nursery and fernery workers in Central Florida. The study was a collaboration between Emory University and the Farmworker Association of Florida (FWAF). Human subjects’ protection was reviewed and approved by the Emory University Institutional Review Board.
Participants
Female farmworkers between the ages of 19 and 43 years, having worked a minimum of 20 hours per week over the previous 60-day period in a Florida nursery or fernery operation, were recruited for this study from membership rosters of the FWAF and their friends and relatives. The participants were employed in rural agricultural communities in Orange and Lake Counties near Apopka, Florida, and in Volusia and Putnam Counties near Pierson, Florida.
Instruments
The authors adapted a questionnaire previously developed by the research team to measure pesticide exposure and workplace practices, adding specific sections on musculoskeletal stress and heat exposure (Flocks et al., 2012; Runkle et al., 2013). The questionnaire included items related to (a) participant demographics; (b) job activities, including cutting, trimming, weeding, and moving plants; (c) workplace ergonomic positions, including sitting, standing, and bending; (d) work-related hygiene practices, including the use of PPE, handwashing, and showering after work; and (e) access to proper field sanitation facilities and supplies. The questionnaire was based on discussions with focus groups of female farmworkers about occupational exposure risk and then further developed in partnership with the FWAF who assisted with content development, cultural appropriateness, and translation into Spanish and Haitian Creole.
Focus groups frequently identified skin rash as an occupational health issue. Therefore, a skin rash diagram was developed using two outlines of the human body: one anterior/dorsal plane and one posterior/ventral plane (see Figure 1). Each participant was asked to mark the areas on the anterior and posterior aspects of the diagram where they currently exhibited a rash (see Figure 2).
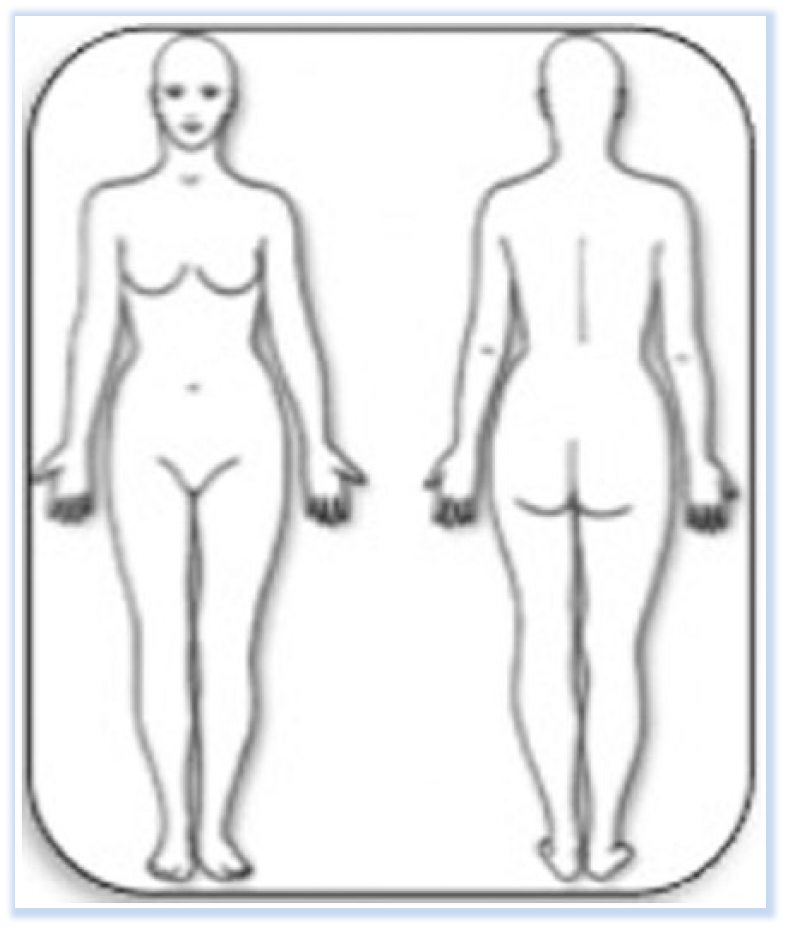
Example of skin rash chart participants used to indicate extent of self-reported rash.

The participant reported rash in the following areas: neck, upper arms, forearms, hands, and genitalia area. Total body surface area covered in rash would be approximately 41%.
Trained community interviewers (promotoras) assisted farmworkers in completing the questionnaire and skin rash diagram (see Figure 1). All consents and instruments were administered in English, Spanish, or Haitian Creole according to the preference of the participant. Research team members reviewed completed questionnaires and skin rash diagrams during data collection to assure consistency and completeness of data. Of the 260 recruited participants, 237 (91.2%) questionnaires and skin rash diagrams were completed.
Analysis
Data were analyzed using both univariate and multivariate test statistics including independent t tests, chi-square test, Fisher’s exact test, and binary logistic regression. The primary dependent variables for these analyses were the following: (a) total body surface area (TBSA) covered by rashes (0%-100%), (b) having at least one rash (rash case Yes or No), (c) anatomical location of the rash, and (d) greater than 30% of body covered by rashes (high rash case Yes or No).
The Lund and Browder (1944) burn chart clinical assessment method is a familiar, easy tool for health care providers; therefore, it was used to estimate the TBSA and the location of rashes in this study (Du Bois & Du Bois, 1916). The Lund and Browder chart assigns values to each anatomical location: head (7%), neck (2%), anterior trunk (13%), posterior trunk (13%), buttocks (5%), genitalia (1%), upper arms (8%), forearms (6%), hands (5%), thighs (19%), legs (14%), and feet (7%). Total body surface area is calculated by adding the percentages associated with each rash area identified by the worker. For example, a worker who reported a rash on the neck, upper arms, forearms, hands, and genital areas would be given a TBSA of 41% (see Figure 2). Upon reviewing the National Burn Repository 2015 Report, 30% was a common cutoff point for severity of burns covering the body (American Burn Association et al., 2015). Therefore, participants who reported a rash on at least one body area were coded as a rash case and any worker who reported having rashes covering greater than 30% TBSA were coded as a high rash case. Background factors such as age, pregnancy, type of work, and use of PPE were examined for their association with rash prevalence, location of the rash, and the likelihood of a worker being categorized as a high rash case.
Results
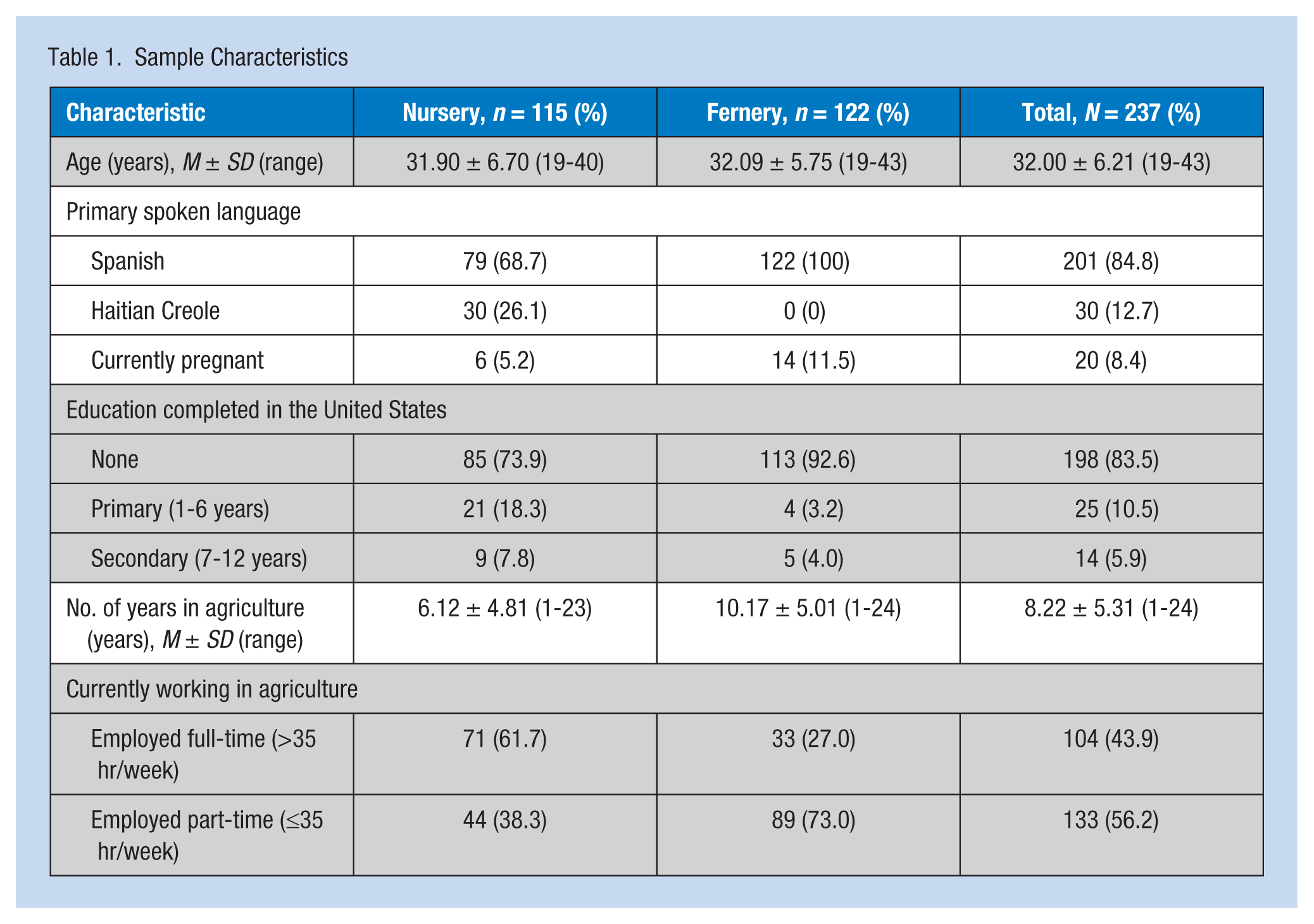
Two hundred thirty-seven women completed the survey; 122 (51.5%) worked in ferneries and 115 (48.5%) worked in nurseries. The majority of these farmworkers (84.8%) spoke Spanish as their primary language; 12.7% spoke Haitian Creole as their primary language. The average age of the farmworkers was 32 years, and they reported an average of 8.22 years working in agriculture. Twenty participants reported they were currently pregnant. See Table 1 for a summary of the characteristics of study participants.
Sample Characteristics
Frequency of Skin Rash
Of the 237 farmworkers surveyed, 37.1% (n = 88) reported a rash on at least one area of their bodies. Of the 88 rash cases, three were excluded because participants reported implausible values. Table 2 displays the association between personal and workplace characteristics and the likelihood of reporting a rash.
Univariate Analysis of Workplace Factors and Personal Factors and the Likelihood of Reporting a Rash
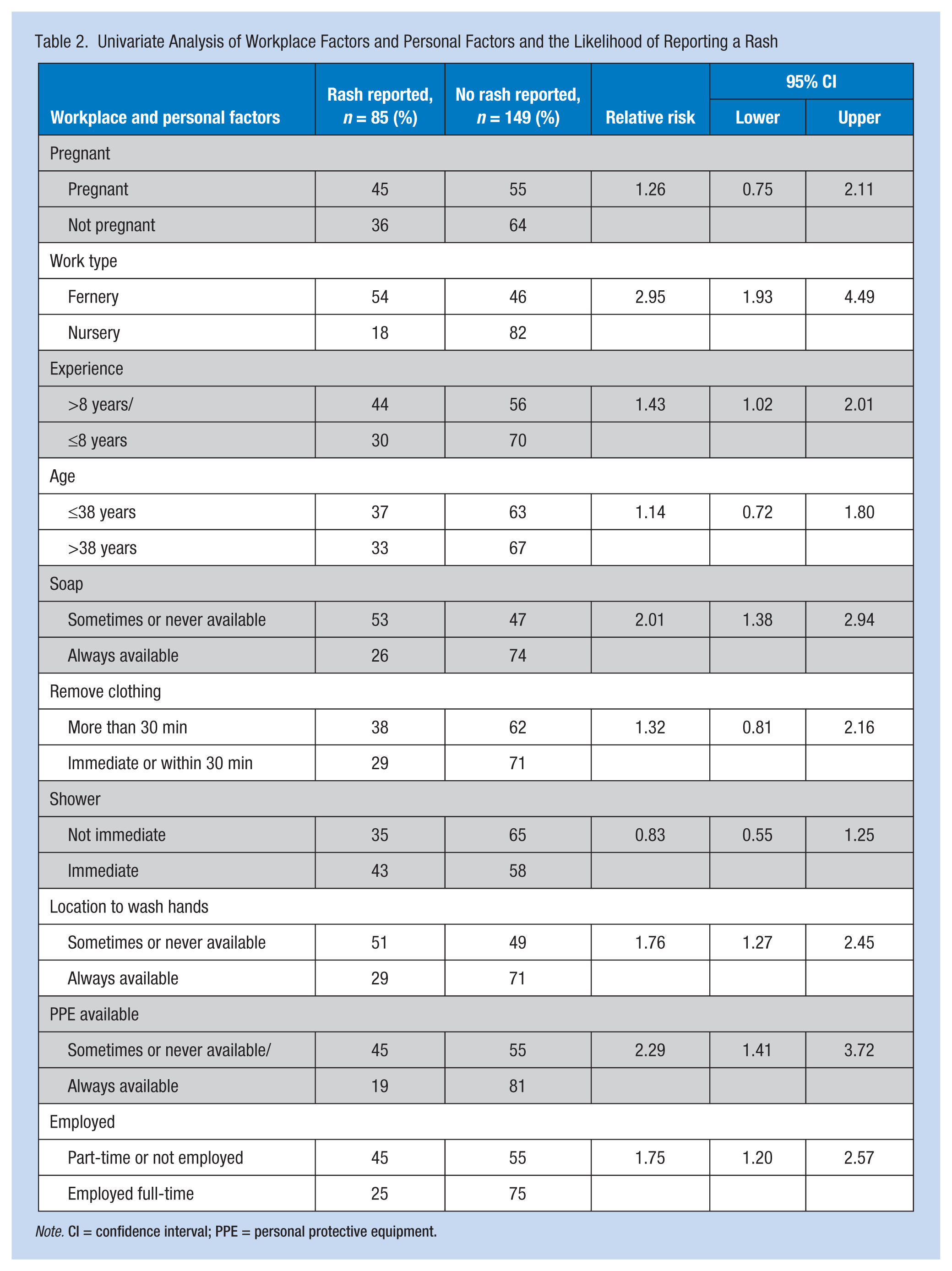
Note. CI = confidence interval; PPE = personal protective equipment.
For this sample (n = 234), the authors used binary logistic regression to determine the extent to which certain individual and work characteristics increased the odds of a rash case. The authors included showering within 30 minutes after work, changing work clothes within 30 minutes of finishing work, the use of PPE, availability of handwashing facilities, availability of soap and towels, pregnancy, years worked in agriculture, and worker age as independent variables.
The model examined the effects of the independent variables on the likelihood that participants reported at least one rash. The logistic regression model was statistically significant (χ2 = 37.09, p = .000). The model explained 14.7% (Cox & Snell R2) of the variance in rash presentation and correctly classified 67.9% of cases. Fernery workers were 4.39 times more likely to report a rash than were nursery workers (p = .000; 95% confidence interval [CI] [2.36, 8.13]). Participants who had no place to wash their hands at work were 2.72 times more likely to report a rash than were participants who reported having a place to wash their hands (p = .054; 95% CI [0.982, 7.54]).
Location of Rash
Table 3 shows the location of the skin rashes and the frequency of reporting a specific rash location by the type of agricultural work performed. Among the 85 participants reporting a skin rash, the most common locations were the forearms (65.9%) and hands (56.5%). The two agricultural groups differed on the likelihood of reporting rashes on different parts of the diagram. Fernery workers were 3.6 times more likely to report a rash on their hands than were nursery workers (p = .000; 95% CI [2.79, 31.38]). Nursery workers were 8.4 times more likely to report rashes on their upper arms (p = .000; 95% CI [4.38, 62.13]) than were fernery workers. Only fernery workers reported rashes on their feet (p < .05). Among nursery workers, forearms (66.7%) and upper arms (52.4%) were the most self-reported rash locations with all other areas being reported less than 19% of the time. Whereas with fernery workers, hands (68.8%) and forearms (65.6%) were the most self-reported rash locations with all other areas being reported less than 30% of the time.
Location of Skin Rash and Percentage of Workers Affected by Type of Agricultural Work
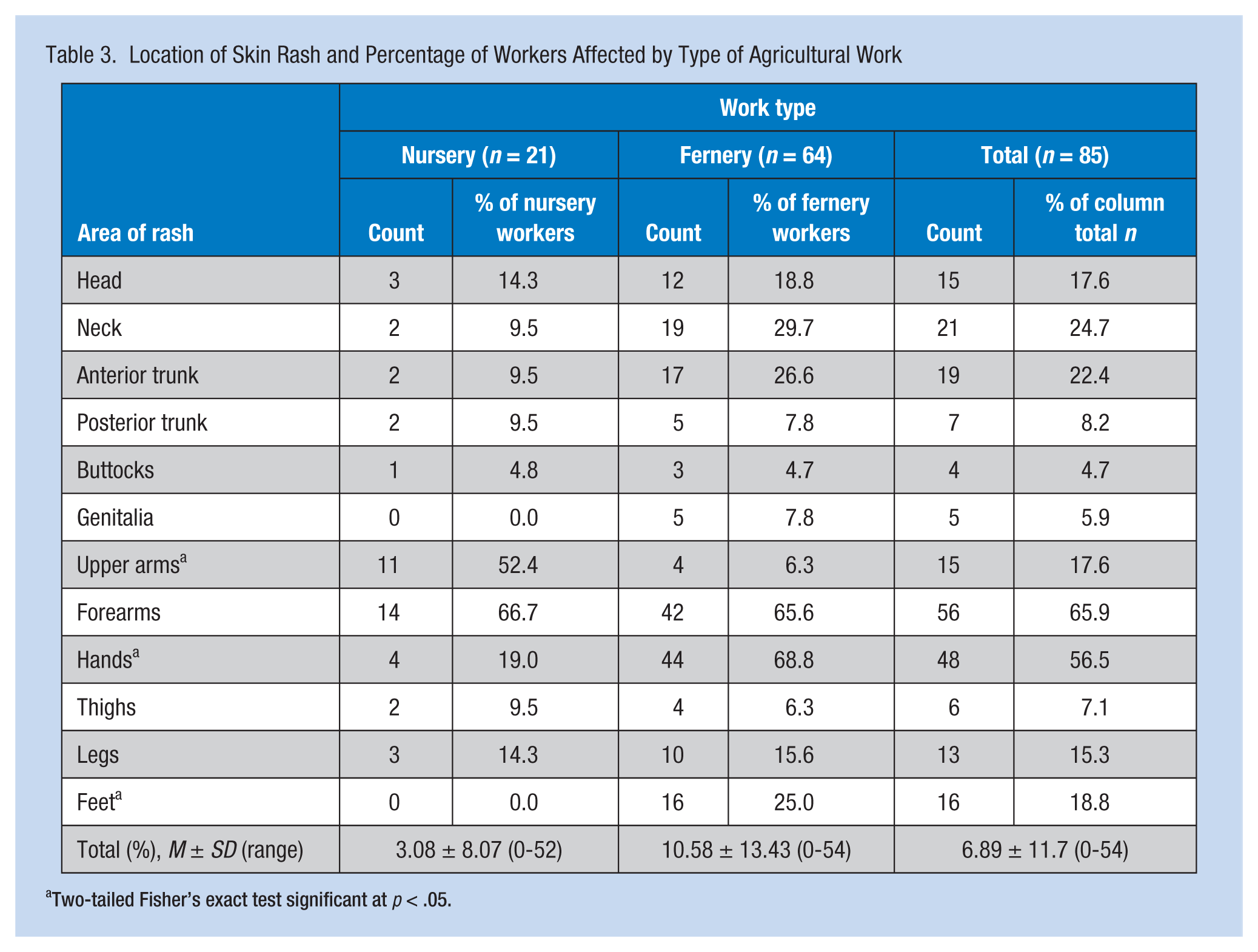
Two-tailed Fisher’s exact test significant at p < .05.
Percentage of Body With Rash
The mean percentage of workers’ bodies with rash among the 85 participants who reported rashes was 18.98% ± 12.20%. No statistically significant differences in the mean percentage of body rash reported by nursery workers (16.86% ± 11.29) compared with fernery workers (19.67 ± 12.49%) were found. Among the 85 workers reporting any rash, 71 workers were categorized as reporting less than or equal to 30% TBSA affected; 14 (12 fernery and 2 nursery) workers reported more than 30% TBSA affected. Overall, the odds of reporting more than 30% TBSA were 6.3 times greater for fernery workers than for nursery workers (95% CI [1.38, 28.98]).
Factors Associated With a Rash Over More Than 30% of the Diagram
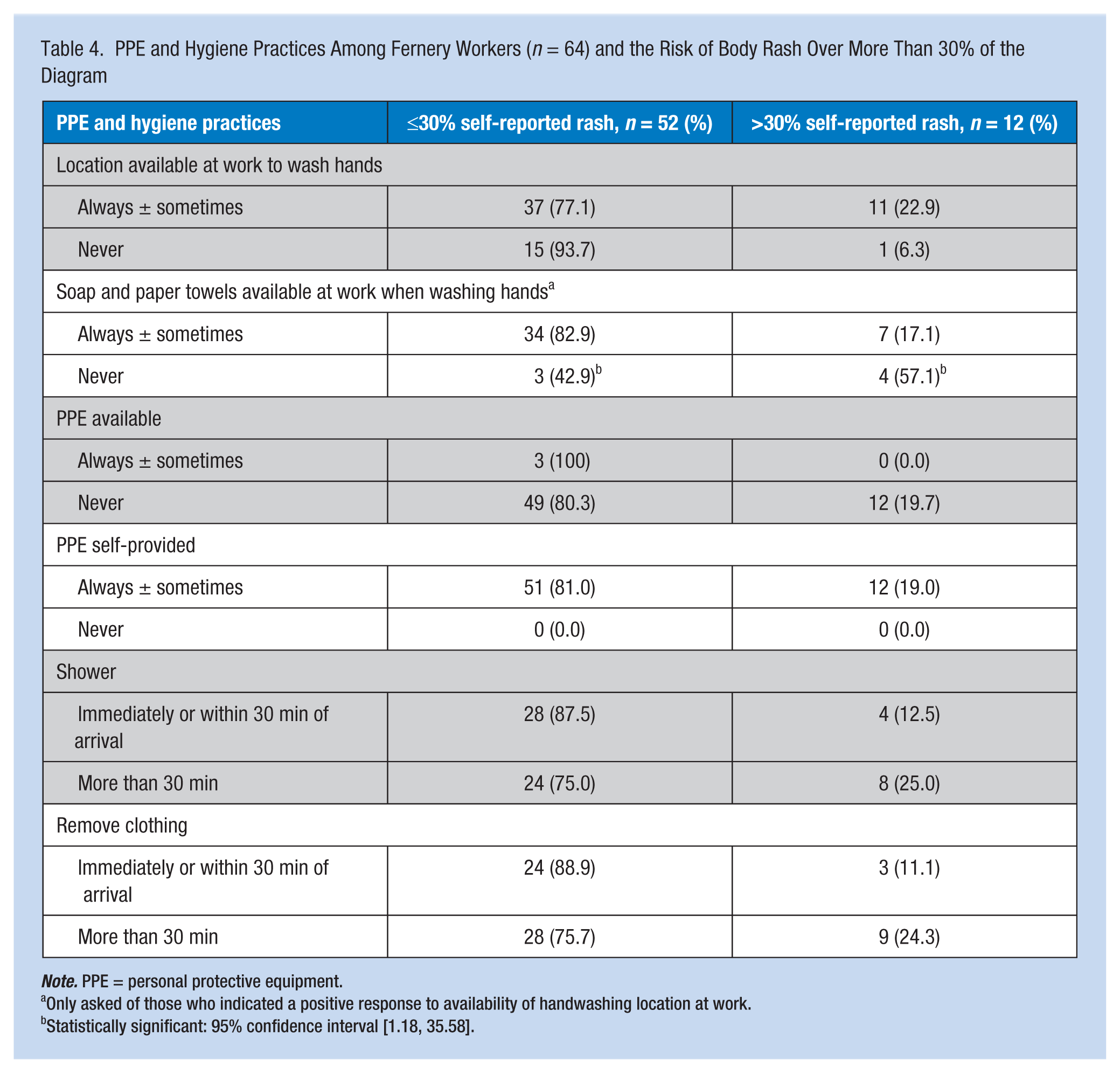
The authors examined factors associated with the likelihood that participants would report more than 30% of their bodies being affected with a rash. Nursery workers were not included in this model because only two reported more than 30% TBSA affected. Table 4 shows the PPE and hygiene practices used by fernery workers (n = 64) and the risk of body rash over more than 30% of the diagram.
PPE and Hygiene Practices Among Fernery Workers (n = 64) and the Risk of Body Rash Over More Than 30% of the Diagram
Note. PPE = personal protective equipment.
Only asked of those who indicated a positive response to availability of handwashing location at work.
Statistically significant: 95% confidence interval [1.18, 35.58].
Table 4 compares the 12 fernery workers with rash over more than 30% of their bodies with fernery workers with less rash (n = 52). Sixteen fernery workers with rash (25.0%) reported having no access to handwashing facilities at work, and 14.6% of those with access to handwashing facilities reported never having soap or paper towels available at the handwashing facilities. Those workers who never had soap or paper towels available were about 3.4 times more likely to report having more than 30% of their body covered by rash than those who did have those items available (95% CI [1.18, 35.58]).
Only 4.7% of fernery workers reported that PPE was available at work locations. Availability of PPE and the use of hygiene practices were compared with the likelihood of workers reporting rash over more than 30% of their bodies. No significant associations were found between self-reported body surface covered in rash and PPE availability or work-related hygiene practices.
Fisher’s exact test was used to analyze the relationship between job activities (weeding, loading, planting) and the likelihood of reporting more than 30% total body rash. No relationship was found between type of work tasks performed by workers and the likelihood of skin rash over more than 30% of the diagram. Work positions (standing, sitting, bending) were analyzed in relation to reporting more than 30% of the body covered in rash, and no statistically significant relationship was found.
For the sample (n = 85) of participants who reported at least one rash, the authors used binary logistic regression to determine the extent to which certain individual and work characteristics increased the odds of reporting a rash that covered more than 30% of their bodies. The authors entered showering, changing work clothes, PPE use, the availability of handwashing facilities, pregnancy, years worked in agriculture, and worker age as independent variables. Note that the type of agricultural work was not included in this model because only two nursery workers reported more than 30% TBSA covered in rash. The model examined the effects of the independent variables on the likelihood that participants reported rashes covering more than 30% TBSA. The logistic regression model was not statistically significant (χ2 = 3.78, p = .052). The model explained 5.7% (Cox & Snell R2) of the variance in rash and correctly classified 81.3% of the cases. However, the odds of reporting a rash covering more than 30% TBSA were 4.7 times more likely for pregnant versus non-pregnant fernery workers (p = .045; 95% CI [1.04, 21.35]).
Discussion
This community-based research program demonstrated the value of developing strong partnerships between community groups and researchers in academic institutions. The community group provided access to conduct research on farmworkers’ occupational and environmental exposures and the benefits of effective mitigation methods. This research method provides practical insights into real-world issues affecting many populations. The authors analyzed the extent to which skin rash affected this community because of the high interest of the population. Although the original study focused on chemical, thermal, and musculoskeletal stressors among childbearing-aged female farmworkers, the information on risk factors for skin rash is applicable to the larger agricultural community. This study found a high frequency of self-reported rash among female farmworkers, particularly on the upper arms, forearms, and hands. Women who work in ferneries were more likely to report rashes on their hands and feet than women working in nurseries, which is most likely due to the hot and damp environment. It is common practice for fernery workers to wear plastic bags over their torsos to protect themselves from the moisture. If their gloves (usually cloth, not rubber) and their shoes (generally athletic shoes) become damp, the frequency of rashes on their hands and feet may increase. The frequency of rash on the forearms of nursery workers was a surprising finding and points to the need for more research in this area. Future studies should compare rash cases in male and female workers from diverse agriculture industries and regions, in combination with pesticide exposure data and history of skin rash.
Although no significant association between rash location and job activity or work position was found, it was determined that availability of handwashing facilities was predictive of whether farmworkers reported any skin rashes. In other words, greater access to handwashing facilities at the workplace lowered the risk of reporting a skin rash. Although this association was not statistically significant based on all factors in the model, this study demonstrated that approximately one in five farmworkers never has handwashing facilities at the workplace and, even if handwashing facilities are available, the facilities may not be stocked with soap and paper towels. Farmworkers’ hands accumulate plant and produce juices, agricultural chemical residues, and pathogenic organisms, all of which may lead to skin rash or be inadvertently ingested or absorbed through the skin if not properly removed (USEPA, 2006). For example, the USEPA (2015) has estimated farmworker exposure for specialty agricultural crops, such as nurseries and ferneries, at 6,050 mg of exposure per pound of active ingredient (µg/lb ai) with no PPE compared with 2,050 µg/lb ai with single layer gloves. In addition, the Occupational Safety and Health Administration (OSHA) has promulgated standard 29 CFR Part 1928.110(b) that requires, among other regulations, that covered employers provide potable water, handwashing facilities, and toilet facilities in the proper ratio to the number of workers present on any given day.
Recent research has discussed the “take-home pathway” as harmful to not only farmworkers but also to their families. Bringing pesticides into the home on clothing allows the residue to persist in the home and on the skin. In the agricultural environment, sunlight, water, and soil breakdown pesticides, but in the home, pesticide residues remain unchanged (Clark & Snedeker, 2006). In the cohort of female fernery workers reporting rashes, 57.8% of participants did not remove their work clothing within 30 minutes of being home.
It is also important to note that cultural and workplace barriers to engaging in safety behavior also exist. For example, Arcury, Marin, Snively, Hernandez-Pelletier, and Quandt (2009) found that many workers viewed mixing “hot” and “cold” substances together as harmful which prevented farmworkers (who are “hot”) from taking showers (considered “cold”). Additional barriers included cramped living conditions, which make it difficult for farmworkers to change soiled clothing after work due to limited space (Arcury et al., 2009). Another factor to consider is whether farmworkers must reuse the same clothing the next day for work. Previous research has shown that employer and supervisor participation in supporting and encouraging farmworkers’ safety behaviors by providing appropriate facilities at the worksite is positively correlated with farmworkers engaging in those behaviors (Mayer et al., 2010).
In addition, the current study results indicate the skin rash diagram is a clinically useful tool for documenting skin rashes. Participants were able to indicate areas of the diagram affected by rash, which removed potential language or literacy barriers. The tool could easily be implemented in the clinical setting to document and track rashes further facilitating conversation between the patient and health care provider about pesticide exposure and methods of prevention. Further validation for clinical utility of the rash diagram is needed, including reliability of the tool and standardization of documenting extent of rash.
This study is the first to examine the risk of skin rash among pregnant farmworkers. Pregnancy results in physiological changes, growth factors, and higher blood flow, leading to more broken blood vessels, dark spots on the skin, rashes, acne, stretch marks, and worsening of existing skin conditions. The authors found that, when controlling for other factors, the odds of reporting a rash over more than 30% of the diagram were 4.7 times more likely for pregnant versus non-pregnant fernery workers. Pregnant agricultural workers should be counseled about the increased risk of skin rash, and employers and health care providers should emphasize the importance of handwashing, changing work clothes, and showering immediately upon returning home after the workday.
The cross-sectional design of this study did not allow for analysis of long-term exposures. Prospective studies of pregnant farmworkers, which describe the incidence of skin rash and other health outcomes, are needed. More research is needed to study the health effects of prolonged exposure, especially considering the average participant reported approximately a decade of work in agriculture. The description of the rash, including color, appearance, severity, and extent of rash, for each body area, could provide additional information on the effects of pesticide exposure on the skin. In future studies, the skin rash diagram should be supplemented with participants’ descriptions or providers’ assessments of the color, appearance, severity, and extent of rash. Height and weight were not available in this data set, which prohibited the incorporation of body mass when determining the percentage of body area covered in rash. Work completed by Neaman et al. (2011) incorporated body mass in calculating patients’ body surface area for burn victims. These additional data could reduce measurement error when incorporated into the evaluation of the rash diagram. Finally, intervention studies are needed to assess the effect of adequate handwashing facilities on the reported incidence of skin rash. A compelling need to examine the extent to which current protective clothing in agricultural settings actually reduces exposure to chemicals, moisture, and other factors associated with the development or exacerbation of skin rash is needed.
Applying Research to Practice
Study results indicate the skin rash chart is a clinically useful tool for documenting skin rashes. By indicating affected areas on the skin rash chart, potential language or literacy barriers were avoided. The tool could easily be implemented in the clinical setting to document and track rashes using skin rash chart to facilitate conversations between the worker and provider about pesticide exposure and methods of prevention.
Footnotes
Acknowledgements
The authors thank Jennifer R. Runkle, PhD, and Joan D. Flocks, JD, for their contributions on concept development.
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funding for this study was made possible by the Centers for Disease Control and Prevention (R21OH009830).
Author Biographies
Kristina Campbell worked as a chemist evaluating the pesticide residue on fruit, water, and soil prior to attending Nell Hodgson Woodruff School of Nursing. She is now a practicing ARNP with Swedish Neurosurgery in Washington State.
Brenda Baker is an Assistant Clinical Professor at Nell Hodgson Woodruff School of Nursing specializing in maternal health and Obstetrics. Dr. Baker’s other areas of research are improving safety for nurses, care of preterm infants, and parent education.
Antonio Tovar is currently an Adjunct Professor at Florida State University and a Pesticide Poison Investigator with the Florida Department of Health. Dr. Tovar has a goal of improving the conditions of farmworkers.
Eugenia Economos is currently employed with the Farmworker Association of Florida and advocates for human rights, civil liberties, and justice. Ms. Economos works to improve living and working conditions through the empowerment of farmworkers.
Bryan Williams is currently a Research Associate Professor at Nell Hodgson Woodruff School of Nursing. His research is primarily focused in the areas of perinatal, pediatric, and environmental epidemiology and policy.
Linda McCauley is Dean and Professor at Nell Hodgson Woodruff School of Nursing. Dr. McCauley’s research focuses on occupational and environmental studies of working populations and children.
