Abstract
Noise-induced hearing loss occurs among workers across a wide spectrum of industries. The purpose of this study was to investigate whether annual hearing testing contributed to a change in employees’ habits and awareness and aimed to evaluate the use of hearing protection at work and at home. Employees enrolled in a university’s hearing conservation program (HCP) were anonymously surveyed regarding their hearing protection habits and awareness of noise exposures on and off the job using a Likert-type scale. Approximately half were “very much” concerned about hearing loss over time. Evidence supports that annual testing, part of the workplace HCP, also led over half of participants to change their habits at work and at home. Awareness of noise exposures increased both at home and at work with annual testing. Overall, the HCP in this particular setting was associated with improved on-the-job and home hearing protection use.
Keywords
One of the most prevalent occupational conditions, noise-induced hearing loss (NIHL), occurs across a wide spectrum of industries in the United States. Thousands of workers every year endure avoidable hearing loss due to workplace noise (Kirchner et al., 2012). Occupational hearing loss is preventable through a hierarchy of engineering and administrative controls and personal protective equipment (Kirchner et al., 2012). Nevertheless, the effectiveness of hearing protection devices (HPDs) depends on workers’ proper use and compliance in wearing the devices. The purpose of this study was to investigate whether annual hearing testing, through a university’s hearing conservation program (HCP), contributed to a change in employees’ habits and awareness on and off the job. Furthermore, the researchers evaluated the use of and attitudes toward using hearing protection at work and at home.
Audiometric testing can identify irreversible hearing loss at a time when early detection and preventive interventions are possible. Testing also serves as an opportunity to educate employees on the lasting effects of noise exposure and can increase awareness of noise hazards present in everyday activities. For example, workers often do not pay close attention to the volume of the sounds in their surroundings at home, because they are not adhering to work rules. The goal of an HCP is to encourage the use of hearing protection as a natural part of everyday life (Schulz, 2014).
The researcher investigated the HCP’s impact by administering an anonymous survey and analyzing the findings. The hypothesis was that workers who participated in annual hearing screening would have a greater awareness of noise exposure on and off the job that would lead to positive changes in habits (i.e., wearing hearing protection more frequently at work and at home). Research has shown that instituting an effective HCP can prevent hearing loss, improve employee morale and well-being, increase quality of production, and reduce the incidence of stress-related disease (Occupational Safety and Health Administration [OSHA], 2008).
According to OSHA, safety managers must provide HPDs, training, and other personal protective equipment to their employees. Employers must also ensure that HPDs are worn by employees where feasible and where administrative and engineering controls fail to reduce excessive noise. Those employees exposed at or above the action level must have access to hearing protection at no cost and have it replaced as needed. More specifically, occupational hearing protection is required by OSHA at 90 dB or higher and is used by most employees who are exposed to noise above 85 dB (OSHA, 2008). One study examined the incidence of a 10-dB standard threshold shift in a group of Canadian lumber mill workers. This study retained the audiograms of 22,376 participants, of which 2,839 had hearing shifts. After adjusting for potential confounding variables, continuous use of hearing protection, and initial hearing tests later in the study period showed that the risk for standard threshold shift was reduced by 30% (Davies, Marion, & Teschke, 2008). Data supported that HPDs are effective in reducing NIHL.
Various studies have investigated not only HPDs but also the impact of education on hearing loss. Griest, Folmer, and Martin (2007) evaluated the effectiveness of a school-based education program for fourth- and seventh-grade students. This study used a baseline and 3-month monitoring questionnaire, concluding that the program was effective at producing long-term knowledge improvements of those participants surveyed (Griest et al., 2007). Fausti, Wilmington, Helt, Helt, and Konrad-Martin (2005) addressed the need for identifying hearing loss and hearing conservation practices among veterans. The study concluded that poor implementation of hearing protection programs and lack of testing caused veterans to have unrecognized hearing loss. Identification often did not occur until speech communication was impaired (Fausti et al., 2005). Another study examined the knowledge and attitudes of British infantry soldiers regarding hearing conservation and explored various factors that might influence behavior. The study concluded that an effective HCP should be comprehensive and incorporate appropriate education, sociological issues, and economic considerations. The findings demonstrated that a well-structured hearing education program which targets appropriate behavior modification is effective and recommended annual educational lectures and videos. Through education and improvements in proper use of HPDs, NIHL could be reduced (Okpala, 2007).
Education as well as worker, supervisor, and HCP manager perceptions affect HPD compliance for those working in elevated noise environments. Morata et al. (2005) aimed to distinguish between the perspectives of workers with normal hearing and those with impaired hearing. Information was collected from workers with self-reported noise exposures and NIHL. Workers perspectives on hearing loss and safety as it relates to job performance showed that awareness is the first step toward providing protective measures for hearing-impaired workers who are exposed to excessive noise (Morata et al., 2005). Svensson, Morata, Nylén, Krieg, and Johnson (2004) assessed the impact of worker beliefs and attitudes regarding HPDs. The authors used a questionnaire developed by the U.S. National Institute for Occupational Safety and Health (NIOSH). The study evaluated workers’ attitudes toward using HPDs as effective tools in occupational NIHL prevention. Key findings included that (a) 95% of respondents were aware that loud noise could damage their hearing, (b) 90% considered hearing loss a serious problem, and (c) 85% believed that HPDs could protect their hearing. However, lower percentage of workers always used HPDs when they were noise-exposed. The study also addressed the issue of safety; 55% of the workers indicated that they could not hear warning signals when using HPDs. Comfort was another factor; 45% of the workers considered HPDs to be uncomfortable. The study provided evidence that these issues must be addressed if HPD use is to be more effective (Svensson et al., 2004).
Although regulations are in place and studies have investigated the effectiveness of HCPs, few studies have focused on the diverse range of occupations typical in a university setting. In turn, this study’s purpose was to investigate whether annual hearing tests contributed to changes in hearing protection use and noise awareness inside and outside the work environment.
Method
Anonymous surveys were distributed to randomly selected employees enrolled in a university HCP per OSHA standards through the Occupational Medicine Department. A total of 44 employees were surveyed of the 132 currently enrolled. Respondent workers ranged in age from 21 to 70 years; they were enrolled in the HCP from 1 to 10 years. Based on the demographics of university employees exposed to excessive noise, those workers enrolled in the HCP had various job descriptions (e.g., groundskeeper, mechanic, electrician, and marching band staff).
A consent sheet was given to employees that described the study. The sheet included the following overview statement: “The purpose of the survey is to gain a better understanding of how annual hearing tests have affected you, if at all. If you wish to participate, a survey will be administered. Please sit outside of the office and place it in the labeled envelope when you are finished. You may also decline or take the survey and place it in the mail. The survey may take 5 to 15 minutes to complete.”
Reassurance that the survey was anonymous and would not be attached to employee health records was provided verbally and in writing. Employees received no benefits for completing the survey; could anticipate no adverse effects from participating in, not participating in, or leaving the study; and were not paid for participation. Workers were reminded not to write their name on the survey. By giving verbal consent, participants gave researchers permission to use the information gathered.
Questions assessed worker concern regarding hearing loss over time and the frequency by which workers think about hearing loss. Another question addressed whether employees were aware that hearing loss was permanent once it occurred. A Likert-type scale was used to gauge whether the HCP had contributed to a change in wearing hearing protection at work and at home. Moreover, the study investigated if the program had increased individuals’ awareness of noise exposure at work and at home. Demographic categories, including age, years of participation in the HCP, and hearing protection usage (both type and frequency), were collected.
Results
Of the 44 workers surveyed, two thirds of workers marked that they use earplugs instead of earmuffs. Many, however, marked both (Figure 1). A relatively even distribution of age ranges spanned 21 to 70 years, with the majority in the 21 to 30 year range (Figure 2).
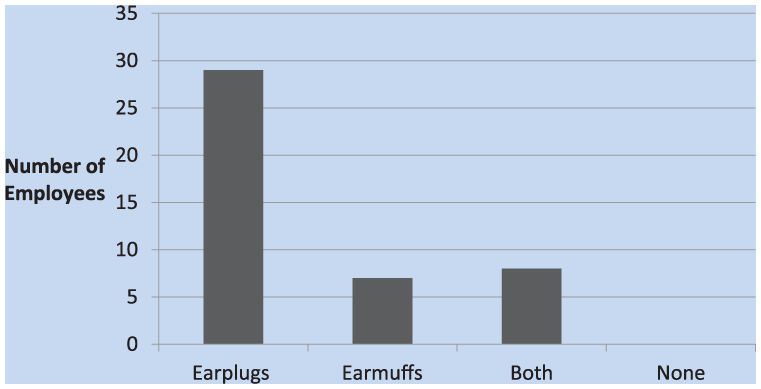
Type of hearing protection used.
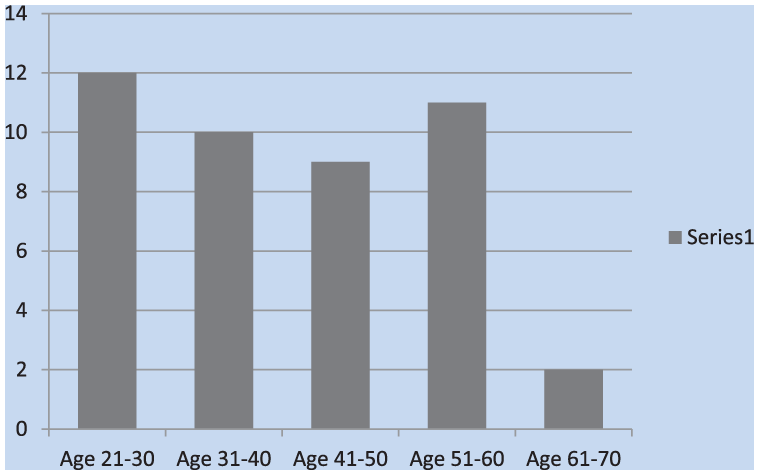
Age distribution of participants in the hearing conservation program (HCP).
Almost half of those surveyed had been in the HCP for between 1 and 5 years; less than half of study participants had been enrolled for 8 or more years (Figure 3). Of those surveyed, almost an even split in responses was found between those who were somewhat (48%) concerned about hearing loss over time and those who were “very much” (46%) concerned. Only a few employees were “not at all” concerned with losing their hearing over time (Figure 4).
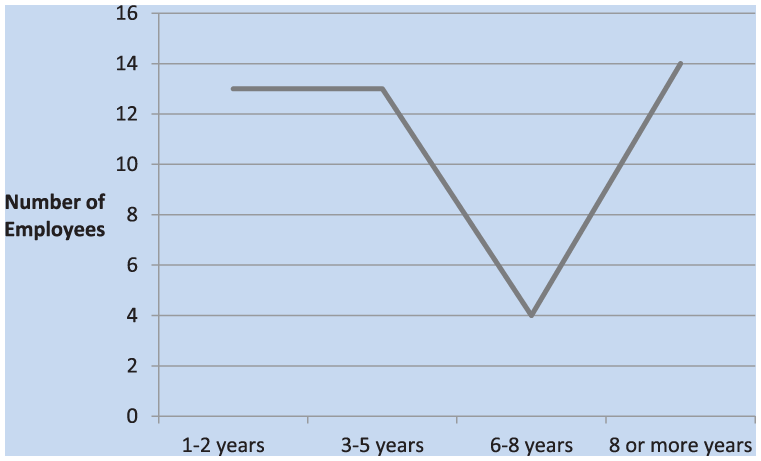
Number of years participants were in the hearing conservation program (HCP).
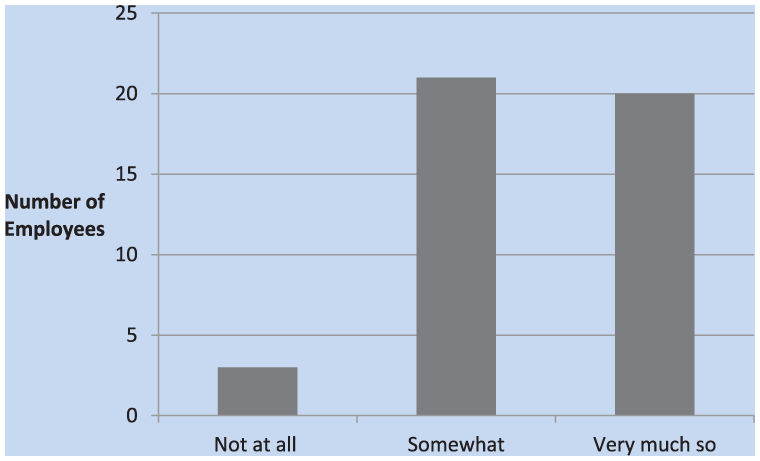
Levels of employee concern about losing their hearing.
Another question addressed how often workers thought about hearing loss. According to Figure 5, the majority reported thinking about hearing loss “once every few months,” and a fourth “many times a month.” Only a few workers thought about hearing loss “every week” and a few workers “never” thought about hearing loss. As seen in Figure 6, the majority of employees were aware that hearing loss is irreversible, although a fourth of employees were unsure if hearing loss was irreversible.
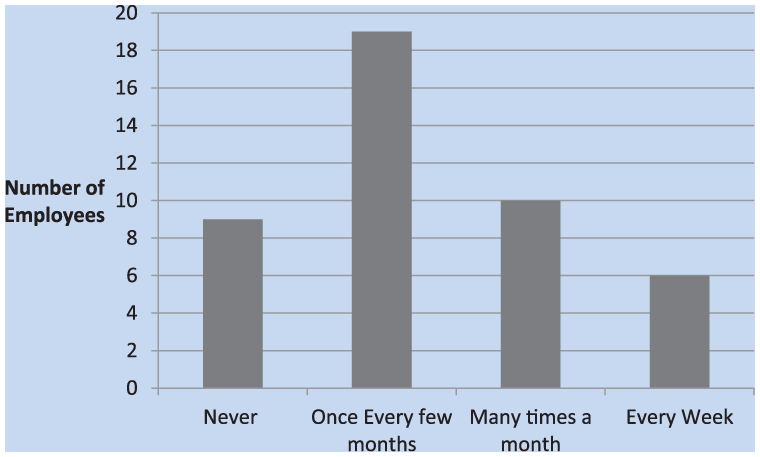
Frequency that participants thought about NIH.
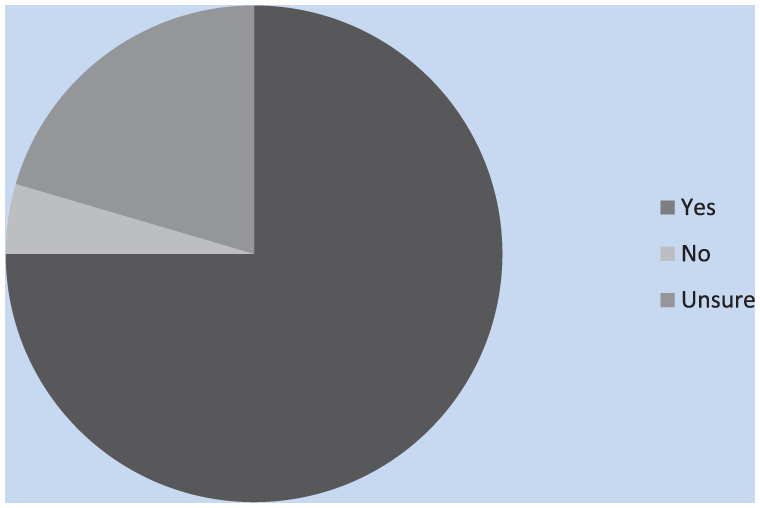
Participants’ beliefs that hearing loss is permanent.
The questionnaire attempted to target noise exposure habits at work and home as well as respondents’ awareness of exposure to noise on and off the job. Of those surveyed, about half answered that annual hearing tests “somewhat” contributed to hearing protection habits at work, approximately a third of respondents answered “very much so,” and a minority stated “definitely” (Figure 7). The next question addressed whether the program contributed to changes in habits at home. Compared with habits at work, more respondents (18.2%) stated the program had “not at all” changed their HPD usage at home. However, half of the workers responded that their home habits “somewhat” changed and 13.6% marked “very much so” (Figure 8). The same number in both groups reported that the HCP “definitely” supported change.
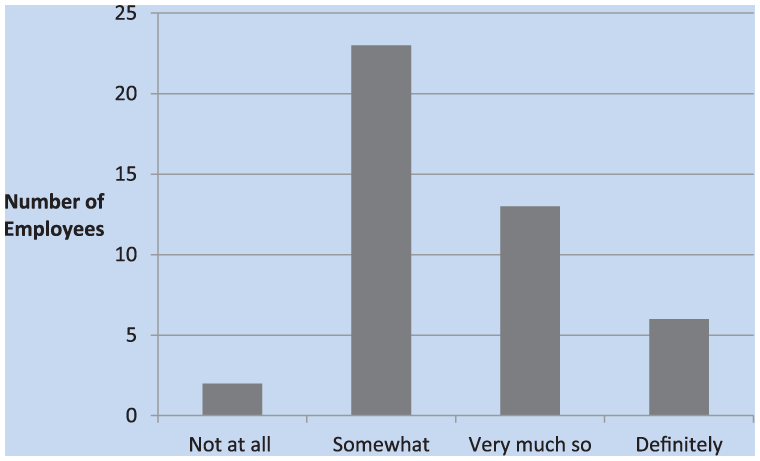
Annual hearing tests contributed to a change in hearing protection habits at work.
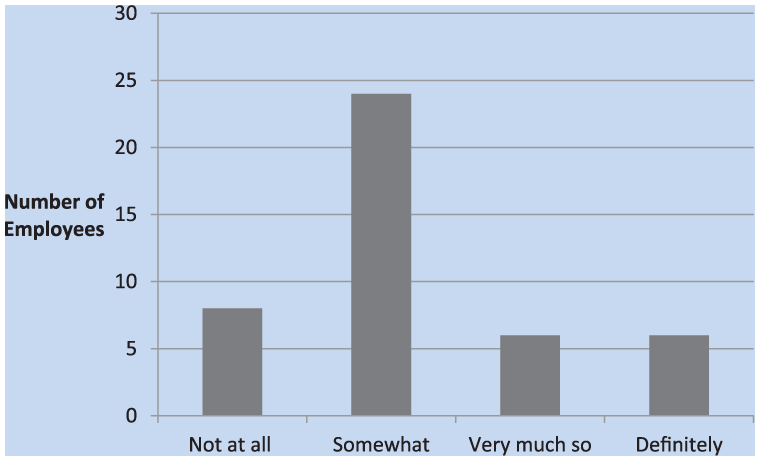
Annual hearing tests contributed to a change in hearing protection habits at home.
The next couple of questions addressed employees’ awareness of noise levels at home and at work. Most employees reported that annual testing increased their awareness of noise at work “very much so” or “somewhat.” Only a few marked that the program did “not at all” increase awareness and a few answered that it “definitely” increased their awareness (Figure 9). As shown in Figure 10, the largest percentage of employees checked that annual testing through the HCP had “somewhat” increased their awareness of noise at home (46.5%). The smallest proportion, 9% of employees, stated the program “definitely” increased their awareness.
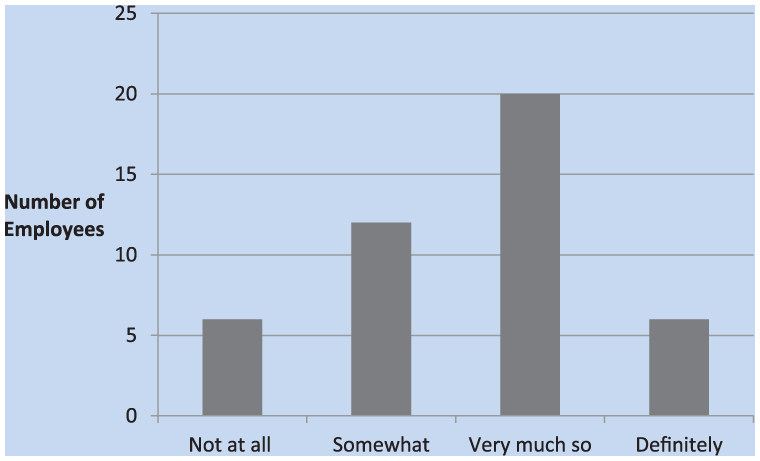
Participants beliefs that annual hearing tests increased awareness about noise exposure at work.
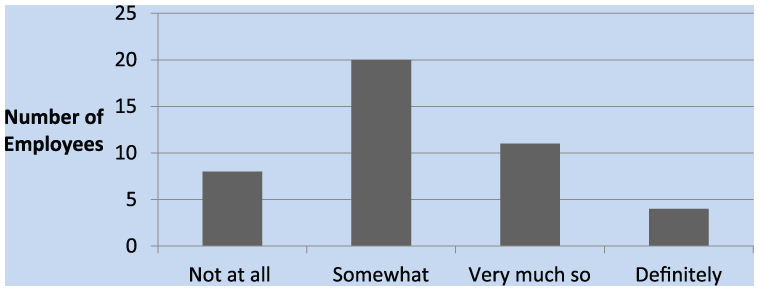
Participants beliefs that annual hearing tests increased awareness about noise exposure at home.
Discussion
Below four of the questions, space was provided for employees to leave comments. A common theme was “awareness.” One worker wrote “more aware” for each answer from 7 to 10 (questions correspond with figure numbers). Another wrote, “we remind each other to use protection” on the job. One employee wrote “more mindful about hearing [
One individual indicated that they were “somewhat” concerned about losing hearing over time and circled that they think about it “every week.” Another wrote that they are “somewhat” concerned and think about it “once every few months” whereas one employee was “somewhat” concerned but “never” thinks about hearing loss. One employee wrote they are “not at all” concerned and “never think” about hearing loss.
Another employee also answered “never” thinks about losing hearing but that it has “definitely” contributed to a change in hearing protection work habits. At home, the same employee wrote that “I wear them when I need them,” and that it has “very much so” contributed to a change. One worker stated that hearing tests “definitely” contributed to changes in habits both at work and at home; hearing tests are “always a good reminder.” One employee’s awareness increased “very much so” and wrote that their department “purchased various hearing protection.” An employee in the 31 to 40 year age range stated, “I think about protection and actually use it” at work; the respondent is more aware at work “by trying to preserve my hearing for as long as I can.”
Based on free responses, the population sampled not only seemed to qualify for the HCP based on noise exposure on the job but also had noisy activities that would be classified as “loud noise” at home. In this study, comments included hobbies like using power tools, shooting firearms, running construction equipment, listening to loud music or movies, and riding motorcycles. Some specific equipment usage mentioned included chainsaws, trimmers, lawn mowers, and vacuums, all typically realizing noise levels above 85 dB.
According to Schulz (2014), discussions on workers’ awareness “grab a worker’s attention and encourage the use of earplugs as a natural part of everyday life,” effectively forming a positive habit. To this effect, one employee in this study wrote, “I use hearing protection while mowing the lawn” and circled “definitely” to a change in habits at home. Another wrote, “I know the lawnmower is too loud and requires ear plugs,” and another, “I don’t drive fast with the windows down anymore.” A total of 34.9% agreed that the program had increased their awareness of noise exposure at home; one specific participant mentioned increased awareness “when working with power tools.” Others indicated, “I now protect when hammering and drilling” and “more aware of my TV volume.” More comments included “I use hearing protection as often as possible when I believe the activity I am engaged in could result in hearing loss. I make sure not to listen to music too loud.”
More workers agreed the program “very much so” and “definitely” increased their awareness of NIHL at work (59.1%) than their awareness of noise at home (34.9%). This finding may be a result of less noise exposure at home or that the program resonated more with on-the-job exposure. One worker reported purchasing custom-fit earplugs and another wrote a supervisor “got us all molded earplugs.” Another commented that the HCP is a “reminder that loud noises can affect you for life.” A total of 79.5% of respondents “somewhat, very much or definitely” agreed that the HCP has increased their awareness of noise at home.
According to results from participants 21 to 30 years of age, 75% of workers reported that hearing protection “somewhat” changed habits at home and half of these respondents reported that hearing protection “very much so” increased awareness at work. Another frequent response was in the 51 to 60 years age range in which 54.5% reported the program “very much so” increased awareness at work and 45.5% at home. An employee in the 17 to 30 years age range stated the HCP “helps me remember to think about using hearing protection before I use tools or equipment.”
In retrospect, one question could have been misleading and affected data analysis. One employee answered in a free response that the hearing program had “not at all” contributed to hearing conservation changes at work and elaborated by writing, “I always am aware of noise and wore hearing protection.” It is unclear where this habit originated before the HCP: whether it was engrained in workplace culture, if there was a family history of hearing loss, or another unidentified reason.
The value of this study could be expanded by repeating the survey every few years. As the older age category retires, it is relevant to determine if the culture of hearing protection is more widely adopted. That is, it would be interesting to assess the transition of the HCP from effectively
Conclusion
Individuals with NIHL may experience morbidity due to hearing loss, tinnitus, or speech discrimination difficulties. On the job, NIHL can affect worker communication and overall safety. However, hearing loss has further-reaching affect on the well-being of employees, not exclusive to the workplace. Loss can be linked to certain conditions such as depression, social isolation, and increased risk of accidents (Kirchner et al., 2012). Individual workers are ultimately responsible for their own hearing protection and conservation. To ensure workers’ safety from NIHL, employees must also take their learned “best practices” home and protect their hearing off the clock as well as on shift (Schulz, 2014).
Supervisors and leaders of HCPs have a responsibility to promote the use of HPDs on and off the job. Each audiogram should be an opportunity to educate and encourage this culture of safety, further reinforcing this positive habit. A combination of providing protective equipment, encouraging a culture of safety, and increasing awareness of excessive noise can contribute to long-term benefits and hearing preservation. Moreover, hearing results can also serve as an indicator of other potential health-related conditions that may be underlying or related to a medication side effect. Overall, the OSHA-mandated HCP appears to be a beneficial service to employees on many levels. The program should be presented in a supportive and nonpunitive manner, without promoting any fear of job loss or repercussions.
Applying Research to Practice
Few studies have focused on the diverse range of occupations typical to a university setting and the effects of a hearing conservation program.
Each audiogram should be an opportunity to educate and encourage the culture of hearing protection on and off the job.
Ideally, by increasing awareness of loud noise in everyday life as well as on the job, more workers use hearing protection out of habit.
Future studies could involve surveying supervisors to gauge their perception of staff awareness and compliance.
Footnotes
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Author Biography
Dedicated to employee health and wellness, Ariel G. Leshchinsky is the lead Registered Nurse for Occupational Health Services at Oregon State University. She is nationally certified as a Clinical Nurse Leader and in Orthopedics.
