Abstract
The Ebola epidemic in West Africa presents a considerable occupational risk to the health personnel involved. The principal mode of virus transmission to health care personnel is through direct contact with the patient, although transmission by aerosols through the air may also occur. Many safety protocols have been suggested relating to personal protection and particularly respiratory protection. It is generally agreed that all health care workers should have easy access to personal protective equipment. However, the degree of respiratory safety escalates from a mask, to an adequate respirator, and finally to a whole body suit with integrated helmet and positive air pressure. Recent publications demonstrate a lack of consensus on the degree of safety necessary. The step from “safe enough” to being “absolutely safe” seems, in most countries, insurmountable because of costs and logistics.
Keywords
As of December 2014, approximately 666 health care workers had been infected with the Ebola virus in Guinea, Liberia, Nigeria, and Sierra Leone. More than half of these workers died (World Health Organization, 2014). This article documents the authors’ concern about the lack of consensus regarding the adequacy of respiratory protection when treating patients with viral hemorrhagic fever (MacIntyre, Chughtai, Seale, Richards, & Davidson, 2014). In particular, what are the standards for respiratory protection during splash-risk and aerosol-generating procedures (AGPs)? The use of personal protective equipment is both a strategy to control disease and protect workers. In this article, the authors emphasize the protection of worker health.
A Norwegian physician, who had just started working in an Ebola clinic in a West African country, contracted Ebola in autumn 2014 and was repatriated to the Oslo University Hospital in Norway for further diagnostics and treatment. The hospital’s guidelines for infection prevention and respiratory protection (Oslo University Hospital, 2014a, 2014b) for personnel entering isolation rooms with Ebola patients encompassed FFP3 half-mask or, for bearded individuals, a full face piece respirator or whole body suit with integrated helmet when the risk of splash or aerosol existed.
When the first Ebola patient to enter Norway was admitted, all personnel involved directly at the bedside were dressed in whole body disposable suits with integrated helmets. Each suit was equipped with a powered air-purifying unit that also created positive air pressure within the suit. In addition, a permanent built-in ventilation system provided negative pressure to patient rooms. Applied correctly, this equipment should prevent any kind of airborne droplets, particles, or splash from entering the respiratory zone. It is likely that no individual health care worker applying this type of protective equipment adequately has ever contracted Ebola. However, the personal protective equipment described above is costly. Health workers in Norway are fortunate because social insurance covers the cost of preventing an occupationally acquired infectious disease.
Respiratory Protection and Transmission
The principal mode of person-to-person transmission of Ebola occurs through direct contact with broken skin, mucous membranes, blood, contaminated needles or instruments, and body fluids including saliva, stomach contents, urine, feces, semen, perspiration, and breast milk. The virus can also be spread through contact with contaminated clothing and through direct contact with the corpses of individuals who have died of Ebola. Transmission can also occur through AGPs (e.g., intubation, suction, and wound revision). Coughing, vomiting, and spraying hemorrhage may also transmit the virus through the air. Martin-Moreno, Llinás, and Hernández (2014a) ascertained in a Lancet correspondence that “Ebola is rarely transmitted via an airborne route” (p. 856). They recommended graded precautionary measures consistent with the risk of a disease spread by direct contact, and criticized health control/provider agencies for widely applying control measures appropriate for airborne diseases (Martin-Moreno, Llinás, & Hernández, 2014b). They stated that “complete respiratory protection is expensive, uncomfortable, and unaffordable for countries that are the most affected” (Martin-Moreno et al., 2014a). In the same comment, these authors stated that “exceptional precautions, such as pressurized suits with oxygen tanks, should be reserved for interventions that generate aerosols (e.g., invasive explorations or intubations), specific situations (e.g. massive hemorrhage), or in laboratories where the virus is cultivated” (Martin-Morene et al., 2014a). MacIntyre et al. (2014) explained the basis for their protection protocol and stated that in the care setting, facemasks (medical/surgical masks) are generally used to protect wearers from splashes and sprays of blood and body fluids and to prevent spread of the infection from the wearer; a respirator is intended for respiratory protection. They stated that the risk of infection with respiratory pathogens increases threefold during AGPs such as intubation and mechanical ventilation. Respirators are generally recommended in these situations for diseases that are known to be transmitted through the droplet route such as influenza and SARS. The fact that respirators are not recommended more broadly for a disease with a much higher case-fatality rate such as Ebola Virus Disease is problematic. In another publication the authors stated that because no certainty exists about Ebola transmission, personal protective equipment (PPE) recommendations are not clear (MacIntyre, Chughtai, Seale, Richards, & Davidson, 2015).
The Pragmatic Standard of Respiratory Protection
A precise “hands-on” manual by the Tanzanian Ministry of Health and Social Welfare (2014) demonstrated a pragmatic approach. The manual recommends the personal protective equipment that should be used by health care personnel working in Tanzania with suspected Ebola patients. “Always put on essential required personal protective equipment (PPE) when handling either a suspected, probable or confirmed case of Ebola. Gather all the necessary items of the PPE beforehand. Risk assess what PPE to wear”:
Standard precautions = hand hygiene
Contact precautions = glove + gown
Droplet precautions* = surgical mask + goggles/face shield + single room
Airborne precautions* = particulate respirator (N95/FFP2) + goggles/face shield + negative pressure room)*
(*depends on resources).
The standards defined above are based on broadly accepted principles and are currently implemented in many countries. The precautions regarding droplets and airborne contamination are not absolute, but depend on available resources.
Surgical Masks and Respirators
Surgical masks provide barrier protection from droplets including large respiratory particles. Most surgical masks do not effectively filter small particles from the air and do not prevent leakage around the edge of the mask when the user inhales. A splash may penetrate the barrier. Simple surgical masks do not provide as much respiratory protection as an N95 surgical respirator (i.e., National Institute for Occupational Safety and Health [NIOSH]–approved and cleared by the Food and Drug Administration [FDA]) or a 3M FFP3 surgical respirator equipped with a filter for fine airborne particles such as viruses or a version supplied with an exhalation valve used in Norwegian hospitals. The application of a whole body suit with integrated helmet and an air-purifying system with positive air pressure (Figure 1) is a significant step in terms of technological development, logistics, and cost. The degree of respiratory protection for health care workers is related not only to the qualities of the mask, respirator, or suit but also to the way it is used and the general health protocols being followed. Ideally, every health care worker should be adequately dressed, equipped, and trained before the actual risk situation arises.
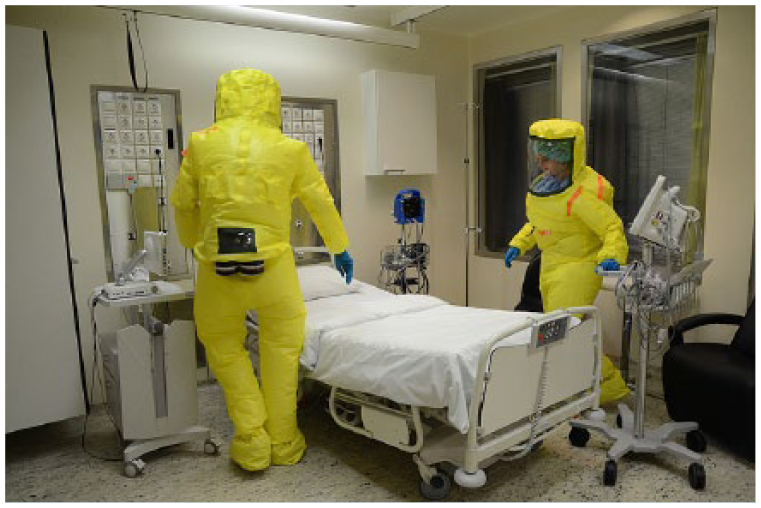
Personal protective equipment used in the care of an Ebola patient: Whole body suit with integrated helmet, each suit equipped with a powered air-purifying unit creating positive air pressure within the suit.
Equipment Relative to Operator Compatibility and Task Complexity
The physical comfort of the health care worker wearing the chosen respirator or whole body suit represents another challenge (Shaffer & Janssen, 2015). The Ebola outbreaks have so far been in hot climates; heat increases worker strain and load. Whether heat provides an impediment to health care workers using appropriate respiratory protection is a question that requires further attention (Kuklane et al., 2015). Better science-based education and information concerning protective equipment that is “safe enough” in various situations might reduce health care providers’ fear and anxiety (MacIntyre et al., 2014).
The degree of task complexity for individual health care workers is another factor that can influence the choice of respiratory protection. During major surgery (e.g., thoracotomy) of an Ebola-suspected patient, full protection would ideally be provided by a whole body suit with integrated helmet and positive air pressure. However, this equipment might not be practical during demanding procedures. Could less respiratory protection during demanding procedures cause distraction among health care providers due to their own health concerns? Such fears may be more prevalent in Western countries where fewer providers have direct experience with the Ebola situation. Further studies are required to learn more about this issue.
Should Standards and Protocols Reflect the Resources Available?
As indicated in the PPE guidelines of the Tanzanian Ministry of Health, the level of personal protective equipment chosen in a given situation depends on the resources available. Some years ago, Hewlett and Hewlett (2005) thoroughly documented the effect of scarce resources, politics, and economics on Ebola eradication. Ansumana, Bonwitt, Stenger, and Jacobsen (2014) documented that health care workers often have limited access to basic personal protective equipment. To many health care providers in developing countries, technically advanced personal protective equipment is unaffordable. In Scandinavian countries, fewer economic limitations affect hospitals’ provision of personal protective equipment. Decisions about equipment should be made with the personnel involved. The relative priority of occupational safety and health depends on the relationship between employees and the health care industry as well as country-specific legislation.
Footnotes
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Author Biographies
R. O. Hanoa, MD, PhD, is working as a professor in occupational medicine at the University of Bergen. He has long experience in this area and has also been a professor of social medicine. He is also a surgeon in neurotraumatology at Oslo University Hospital.
B. E. Moen, MD, PhD, is the head of the Centre for International Health at the Department of Global Public Health and Primary Care, University of Bergen. She is professor in occupational medicine and global health.
