Abstract
In 2008, the work-related injury fatality rate was 3.8 per 100,000 workers in the United States but was 5.2 per 100,000 workers for the southeast region. Work-related fatalities in the southeast were examined for the period 2008 to 2011. Median work-related injury fatality rates are reported for the southeast region, each of the 12 states, and the United States. The percentages of employees in high fatality industries and work-related fatalities by cause were calculated. Finally, the Occupational Safety and Health Administration’s database was searched for fatality reports. States with the highest rates (per 100,000 workers) included Arkansas (7.2), Louisiana (6.8), and West Virginia (6.6). Arkansas, Louisiana, Mississippi, and West Virginia each had more than 20% of their employees in high fatality industries. Forty percent of work-related injury fatalities were from transportation incidents in the southeast and the United States. Future analyses should include work-related injury fatality rates by industry and compare rates with other U.S. regions.
Keywords
In the early morning hours of a summer day in 2012, a 49-year-old male owner-operator of a Kentucky towing company died when he was struck by a driver operating a box truck. While the towing company owner and his two sons were on an interstate returning with an SUV, the operator thought the load felt strange. He parked his tow truck on the right-hand shoulder and was standing on the driver’s side at the rear of the trailer checking the load’s securement, when a box truck in the right lane struck him. Emergency medical services arrived, followed by the coroner who declared the towing operator dead at the scene. The cause of death was due to massive head and chest injuries resulting from being struck by the motor vehicle (Kentucky Injury Prevention and Research Center, 2013).
Each year, more than 4,000 workers die from work-related injuries in the United States (National Institute for Occupational Safety and Health [NIOSH], 2010). A report of work-related injury deaths for 2008 indicated the rate was 3.8 per 100,000 workers in the United States overall, but was higher, 5.2 per 100,000 workers, in 12 southeastern states (Alabama, Arkansas, Florida, Georgia, Kentucky, Louisiana, Mississippi, North Carolina, South Carolina, Tennessee, Virginia, and West Virginia; Southeastern States Occupational Health Network [SouthON], 2012). Because work-related deaths are preventable, the SouthON is focused on developing common priorities for collaborative surveillance and for informing policies. To encourage public health professionals, occupational safety and health professionals, and company safety representatives to identify intervention priorities, the Centers for Disease Control and Prevention’s (CDC) NIOSH and state partners examined work-related injury fatalities in SouthON states, compared with the United States, for the period 2008 to 2011.
Method
To characterize fatal, work-related injuries, methods provided by the Council of State and Territorial Epidemiologists’ Guide for Tracking Occupational Health Conditions and Their Determinants (Council of State and Territorial Epidemiologists, 2013) were used to evaluate data from the Bureau of Labor Statistics’(BLS) Census of Fatal Occupational Injuries (CFOI) and Geographic Profile of Employment and Unemployment. CFOI uses multiple sources, including death certificates, workers’ compensation reports, medical examiner records, news stories, Mining Safety and Health Administration fatality reports, and Occupational Safety and Health Administration (OSHA) fatality reports (BLS, 2012) to provide a census of work-related fatal injuries. The Geographic Profile of Employment and Unemployment includes data from the Current Population Survey, a survey of about 50,000 households, which is used to estimate employment and unemployment numbers for each state (BLS, 2001). Using these data, median fatality rates from work-related injuries are reported for each of the 12 SouthON states, the 12 states as a whole, and the entire United States. Median fatality rates were used rather than the average over the 4-year time period because some states had wide ranges of worker-related injury fatality rates. The percentage of work-related fatalities by cause is also reported: transportation incidents, contact with objects and equipment, assaults and violent acts, falls, exposure to harmful substances or environments, and fires and explosions. Finally, the percentage of employees in high fatality industries, which include agriculture, construction, mining (including oil and gas), and transportation, was calculated by state for the period 2008 to 2011. The OSHA fatality database was also searched for reports from states with higher work-related fatal injuries in high mortality risk industries. No tests for statistical significance were performed.
Results
During 2008 to 2011, the median annual fatality rate for work-related injuries from the 12 states in SouthON was 4.8 per 100,000 workers; the rate for the entire United States was 3.5 per 100,000 workers (Table 1). The SouthON states with the highest rates included Arkansas (7.2 per 100,000 workers), Louisiana (6.8), and West Virginia (6.6). An additional 6 SouthON states also had a higher rate than the United States as a whole: Mississippi (6.3 per 100,000 workers), Kentucky (5.7), Tennessee (4.8), Alabama (4.7), South Carolina (4.3), and North Carolina (3.7). Only Virginia (3.4), Florida (3.1), and Georgia (2.7) had rates lower than the United States (Figure 1). The SouthON states with the highest work-related injury fatality rates also had the highest median percentages of employees in high fatality industries for the period 2008 to 2011 (Table 2). The percentage of work-related injury fatalities due to transportation incidents was similar for the SouthON states and the United States, approximating 40% of fatalities. The percentage of work-related injury fatalities due to other causes in the SouthON region differed little from rates in the United States (Table 3).
Median Annual Fatality Rates and Ranges per 100,000 Employees by Location—2008-2011
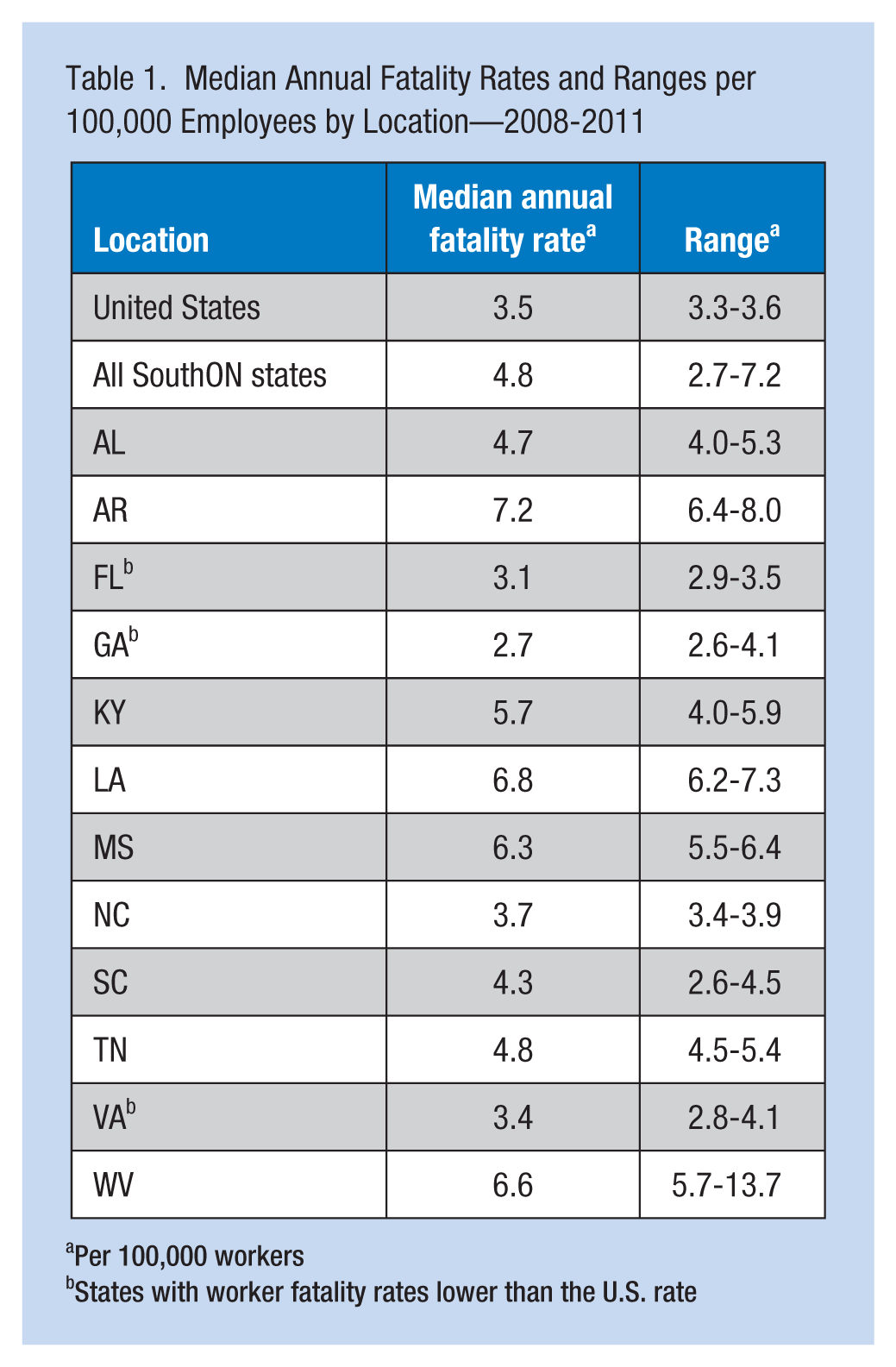
Per 100,000 workers
States with worker fatality rates lower than the U.S. rate
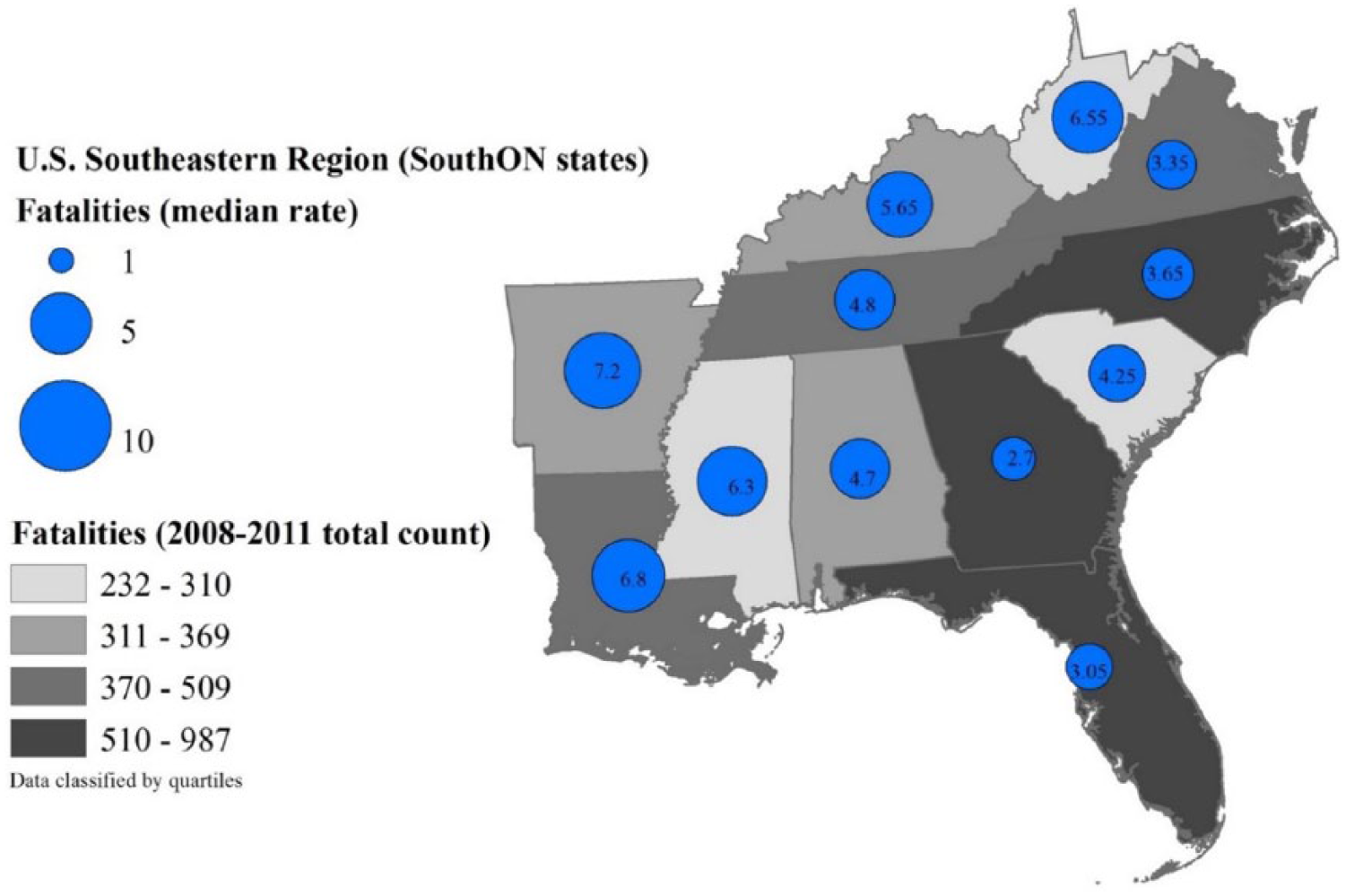
Fatal work-related injuries, 2008-2011.
Median Percentage of Employed Persons in High Mortality Risk Industries by Location—2008-2011
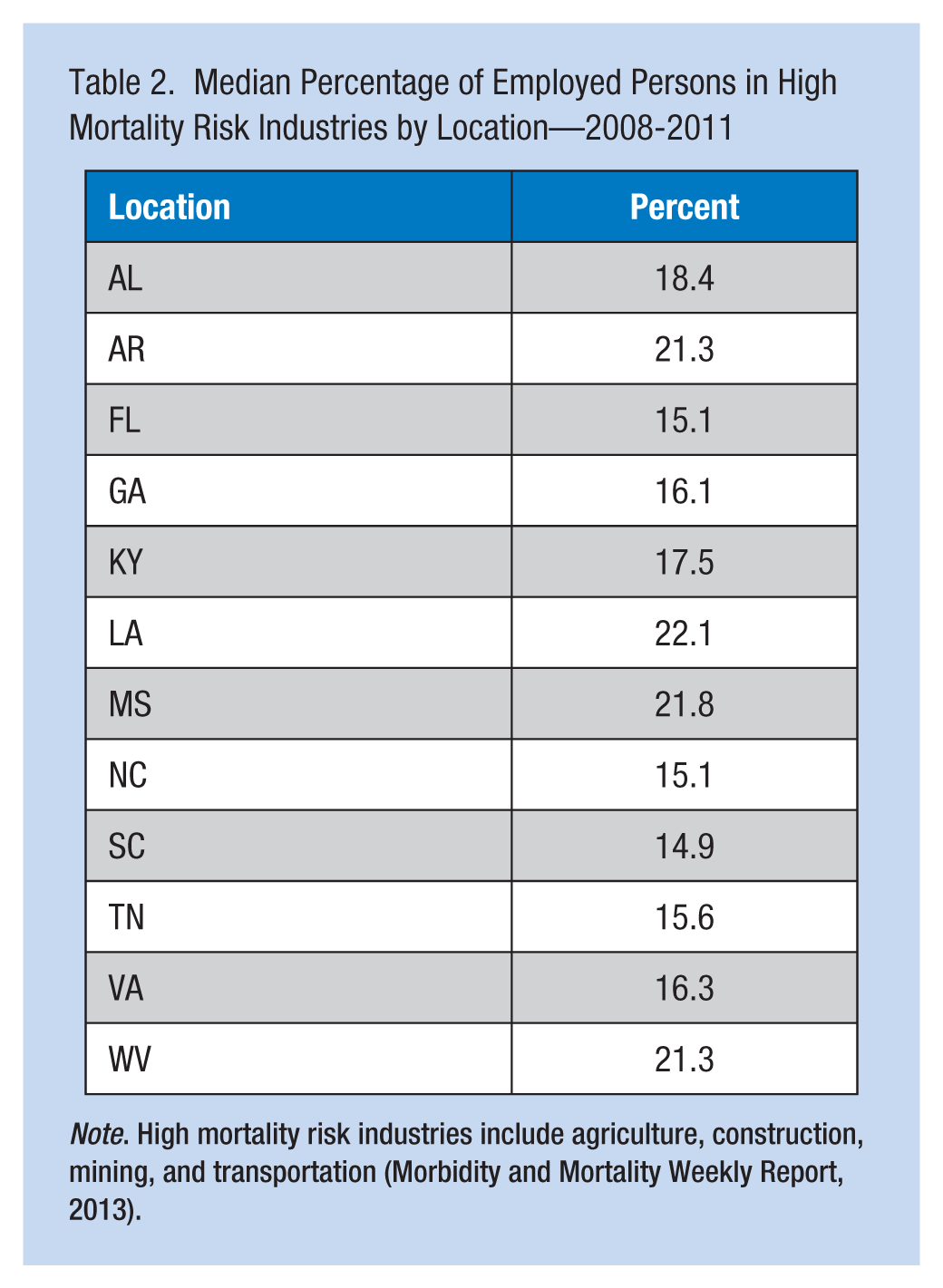
Note. High mortality risk industries include agriculture, construction, mining, and transportation (Morbidity and Mortality Weekly Report, 2013).
Percentage of Work-Related Fatalities by Cause—2008-2011
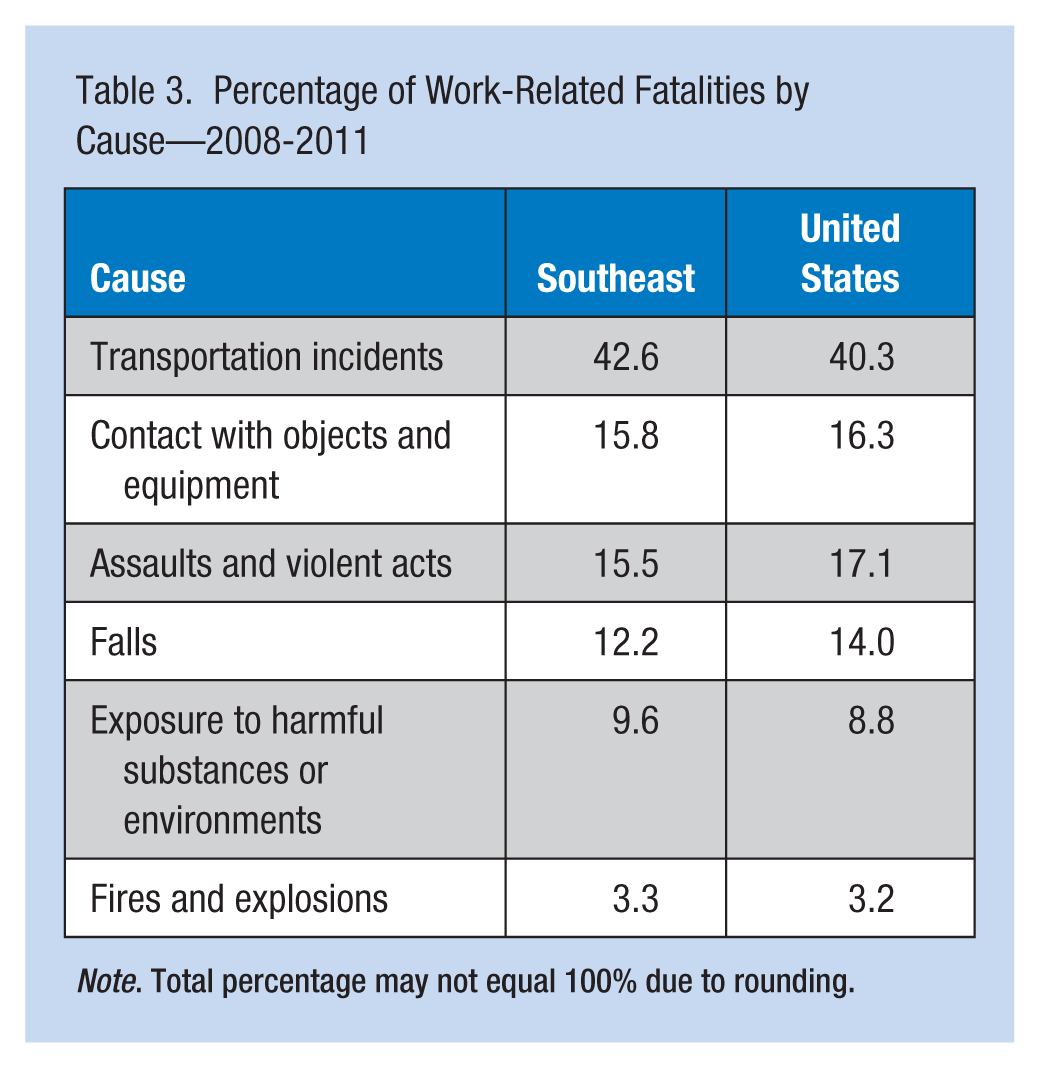
Note. Total percentage may not equal 100% due to rounding.
Work-related fatality reports based on worker fatalities reported to federal and state OSHA can be found on the OSHA website (2015). Following are such reports of work-related injury fatalities from states with higher fatality rates and a high percentage of employees in high fatality industries. One fatality report from 2008 described a work-related fatality in the construction industry in Louisiana. Employees were restarting a recovery boiler under a partial-natural-draft. The power boiler was not online at the time and exploded. One employee was blown over a standard guard railing on the sixth floor. He fell down some 25 feet on a scaffold staging and died from blunt force trauma to the chest. His injuries included lacerations to his lungs, diaphragm, liver, and thoracic aorta (OSHA, 2008).
Another fatality report described the death of a migrant farm worker in the agriculture industry in Arkansas. In 2010, the employee had been working in a tomato packing warehouse for several months. After a 4-day work period, he was found unconscious in a shaded area. The employee was transported by coworkers to a local hospital, where he arrived with a temperature of 108 degrees. He died from heat exhaustion the following day (OSHA, 2010).
Discussion
Nine of 12 SouthON states had a higher median work-related injury fatality rate than the U.S. rate of 3.5 per 100,000 workers. One of the reasons for this elevated rate might be that workers in the southeastern states work in high fatality industries. The SouthON states with the highest work-related injury fatality rates also had the highest median percentage of employees from high fatality industries. Arkansas, Louisiana, Mississippi, and West Virginia each have more than 20% of employees in these industries. Individuals working in agriculture, construction, mining, and transportation are at higher risk for work-related fatalities than workers in other industries within the United States (Morbidity and Mortality Weekly Report, 2013).
Caution should be used when comparing fatality rates from work-related injuries by state as workforce characteristics (e.g., demographics), and industry employment vary from state to state. For example, a common industry in the southeast in 2011 was health care and social assistance (data not shown). West Virginia, which has a work-related injury fatality rate of 6.6 per 100,000 workers, has 22% of its workforce in this industry. Georgia, which has only 13% of its workforce in health care and social assistance, has a work-related injury fatality rate of 2.7 per 100,000 workers. In this particular instance, industry employment differences might account for variances in work-related fatality rates; however, caution should be used when making these comparisons, because it is possible that no correlation actually exists.
Implications for Practice
NIOSH currently funds four regional occupational safety and health education and research centers (ERC; Kentucky, North Carolina, Florida, and Alabama) and an agricultural center (Kentucky) in the southeast region. Center staff collect industry-specific and total industry injury and illness surveillance data, conduct research, engage in public health practice, and educate the next generation of occupational health researchers and practitioners. The funded SouthON states are addressing the elevated work-related injury fatality rates of these southeastern states by using occupational health indicators to identify and track risk factors and implement priority interventions. North Carolina and Kentucky both have occupational health-related objectives in their states’ versions of Healthy People 2020.
In addition, Kentucky’s Injury Prevention and Research Center has published several epidemiologic studies that identify risk factors associated with transportation incidents to facilitate implementation of prevention measures (Bunn, Slavova, & Hall, 2008; Bunn, Slavova, & Robertson, 2012, 2013). The case study at the beginning of this article described a motor vehicle crash in which the owner-operator of a towing company died when he was struck by a driver operating a box truck (Kentucky Injury Prevention and Research Center, 2013). The report outlined several recommendations based on investigation findings. To prevent similar incidents, the report included recommendations that Kentucky create a law requiring the use of portable emergency warning devices when an emergency vehicle is stopped at the side of the road and that employers and tow truck operators ensure the use of warning devices to alert approaching motorists whenever a worker is outside of the tow truck.
Conclusion
SouthON is developing common priorities for informing collaborative surveillance, research, interventions, and policies in the southeastern region of the United States. Based on current findings, enhanced research and public health practice activities are needed in this region. Future analyses should include work-related injury fatality rates by industry and comparison of these rates with other regions of the United States. States with work-related injury fatality rates higher than the U.S. rates should consider factors unique to these states. SouthON provides a mechanism for diverse partners in the southeastern United States to work together to address these occupational safety and health issues.
Footnotes
Acknowledgements
The authors thank the Alabama Department of Public Health and the South Carolina Environmental Public Health Tracking Program and Office of Research and Statistics for contributions to this report.
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Author Biographies
Lieutenant Kimberly Brinker, US Public Health Service, is a registered nurse and epidemiologist with the National Institute for Occupational Safety and Health (NIOSH), Centers for Disease Control and Prevention (CDC). LT Brinker received her Master of Science in Nursing and Master of Public Health from Emory University in Atlanta, GA.
Teri Jacobs is a PhD Candidate in Environmental Geography, specializing in Conservation Biogeography, at the University of Cincinnati, where she also teaches climatology, geomorphology, biogeography, and conservation as an adjunct professor. At CDC’s National Institute for Occupational Safety and Health, she is an ORISE Research Participant and GIS Analyst.
Jeffrey Shire is a Health Scientist in the Division of Surveillance, Hazard Evaluations and Field Studies, National Institute for Occupational Safety and Health, Centers for Disease Control and Prevention.
Dr. Terry Bunn received her doctorate from Cornell University and is an Associate Professor in the Department of Preventive Medicine and Environmental Health at the University of Kentucky, College of Public Health. She has been the Director of the Kentucky Injury Prevention and Research Center (KIPRC) since 2010. Dr. Bunn conducts research in the prevention of motor vehicle injuries and drug poisonings, in both the general and working populations.
Juanita Chalmers graduated with a BA from Dartmouth College and a Masters in Public Health from the University at Albany, SUNY. Ms. Chalmers is currently employed at the Florida Department of Health as the program coordinator and epidemiologist for the Occupational Health and Safety Program.
Dr. Gregory Dang graduated with his Doctor of Public Health degree concentrating in Health Services Management from the University of Kentucky, College of Public Health in 2012, and earned his Master of Public Health degree in Research Epidemiology in 2008, from the Loma Linda University School of Public Health in California. He is currently the principle investigator and primary epidemiologist for the North Carolina Occupational Health Surveillance Program at the NC Division of Public Health. Dr. Dang’s experiences and interest in public health research and practice span multiple fields of study, which include epidemiology of cancer, infectious diseases, domestic violence, and health program management and evaluation.
Dwight Flammia is the State Public Health Toxicologist for the Virginia Department of Health. He received his undergraduate degree in chemistry at the Virginia Commonwealth University and his doctorate in medicinal chemistry from the Medical College of Virginia.
Sheila Higgins graduated from the University of Connecticut with a Bachelor of Science in Nursing in 1981 and subsequently from UNC Chapel Hill with an MPH, concentration Occupational Health Nursing, in 1992. She currently functions as an Occupational Health Nurse Consultant and surveillance coordinator with the Occupational and Environmental Epidemiology Branch, NC Division of Public Health.
Michelle Lackovic is the project lead for the Occupational Health and Injury Surveillance Program at the Louisiana Department of Health and Hospitals’ Office of Public Health.
Antionette Lavender, MPH is currently the occupational health epidemiologist at the Georgia Department of Public Health, where she surveils occupational injuries, illnesses, and fatalities. She previously served as the suicide epidemiologist and tobacco use epidemiologist for the state of Georgia. She has special interest in how the work environment causes chronic disease and impacts mental health.
Dr. Jocelyn S. Lewis earned her PhD and MSPH in Environmental Health Sciences (concentrations: Industrial Hygiene and Toxicology/Risk Assessment) from Tulane University School of Public Health & Tropical Medicine in New Orleans, LA. She is currently an Environmental Health Scientist Coordinator with the Louisiana Department of Health and Hospitals/Office of Public Health/Section of Environmental Epidemiology and Toxicology and is also an adjunct Assistant Professor with LSU Health Sciences Center.
Dr. Yinmei Li, is an epidemiologist with the Tennessee Department of Health (TDH) who has provided epidemiological support to the Department for more than twelve years. She earned an MD equivalent degree from Shanghai Medical College, Fudan University in China, and both a Master’s degree in Experimental Statistics and a PhD in Veterinary Medical Sciences from Louisiana State University.
Laurel Harduar Morano is an occupational and environmental epidemiologist. She received her MPH in biostatistics from Boston University and is currently a doctoral candidate in epidemiology at the University of North Carolina. Over the last decade she has worked with the Florida Department of Health on numerous projects, most recently those related to occupational health and climate change effects.
Austin Porter, MPH, DrPH candidate, is the trauma registry administrator for the Arkansas Department of Health. Mr. Porter also serves as the Arkansas representative for the SOUTHON network.
Dr. Kimberly Rauscher is Assistant Professor in the Department of Occupational and Environmental Health Sciences at West Virginia University, and is the Assistant Director for Research at the WVU Injury Control Research Center. Her research is in occupational health and safety policy and the prevention of occupational injuries, with a focus on adolescent workers in the US. She teaches a graduate course on occupational injury prevention in the WVU School of Public Health.
Dr. Svetla Slavova is an Associate Professor at the University of Kentucky College of Public Health and a biostatistician for the Kentucky Occupational Safety and Health Surveillance Program. Her research interests are in the areas of occupational safety and health, injury surveillance, and drug overdose research.
Dr. Sharon Watkins is Director of Public Health Research at the Florida Department of Health and has worked in epidemiology in Florida since 1990. She currently serves as the Principal Investigator for NIOSH-funded occupational health efforts in Florida and is serving her second elected term on the Council of State and Territorial Epidemiologists (CSTE) Executive Board as chair for Occupational/Injury/Environmental Health.
Dr. Lei Zhang is Director of the Office of Health Data and Research at the Mississippi State Department of Health and a professor of Biostatistics at the University of Mississippi Medical Center.
Captain Renée Funk, US Public Health Service, is the Deputy Associate Director of the Emergency Preparedness and Response Office (EPRO), Office of the Director, National Institute for Occupational Safety and Health (NIOSH), Centers for Disease Control and Prevention (CDC). Dr. Funk is the NIOSH liaison to the SouthON network.
