Abstract
According to the Centers for Disease Control and Prevention, the number of people 65 years of age or older living in the United States is projected to double by 2030 to 72 million adults, representing 20% of the total U.S. population. Evidence suggests that older Americans are working longer and spending more time on the job than their peers did in previous years. The increased number of older adults working longer is observed not only in the Unites States but also worldwide. There are numerous ramifications associated with the changing demographics and the expanding prevalence of an aging population in the workforce. Dynamics that arise include stereotyping and discrimination, longevity and on-site expert knowledge, variances in workplace behavior, a multigenerational employee pool, chronic disease management, occupational safety, and the application of adaptive strategies to reduce injury occurrences. Occupational health nurses play a pivotal role in implementing best practices for an aging-friendly workplace.
Keywords
Advances in public health and medicine have improved health outcomes and increased life expectancy worldwide while reducing mortality (Global Aging Initiative, Center for Strategic & International Studies, 2017). Acknowledging that the human life cycle is undergoing unprecedented changes, the Global Aging Initiative, Center for Strategic & International Studies (2017) stated that a demographic transformation is now sweeping the world, intersecting with every dimension of public and private life. As a result, nothing is more likely to shape the intercontinental development of financial, social, and political institutions in the 21st century than the simultaneous aging of Asian, European, and American citizens (Global Aging Initiative, Center for Strategic & International Studies, 2017). To preserve economic security, society must adapt to this new reality. Because of willingness, and sometimes fiscal necessity, older adults are working beyond the traditional retirement age of 65 years.
According to the Department of Labor’s Bureau of Labor Statistics (2017), older Americans are working longer and spending more time on the job than their peers in previous years. In 2000, approximately 12.8% of 65 years of age and older Americans, or about 4 million individuals, reported they were working; in 2016, 9 million individuals age 65 years of age and older reported being employed full-time or part-time (Drew, 2016). Not only are more older Americans working, but more are working full-time. The Centers for Disease Control and Prevention’s (CDC) National Center for Chronic Disease Prevention and Health Promotion (2012) reported an increasingly widened gap: 77% of workers aged 55 years or older held full-time employment while 23% held part-time jobs. Although working during their retirement years remains a largely male phenomenon, the percentage of older women working has grown over time (Toossi & Bureau of Labor Statistics, 2015). In this article, the authors examined implications associated with changing population demographics and the increasing prevalence of older workers in the workforce.
Why Are People Working Longer?
The number of individuals aged 65 years of age and older is projected to double by 2030 to 72 million adults, representing 20% of the total U.S. population (CDC, National Center for Chronic Disease Prevention and Health Promotion, 2012). Since 1998, the qualifying age to receive full Social Security retirement benefits has increased and is projected to reach 67 years by 2020 (Toossi & Bureau of Labor Statistics, 2015). As a result, the average age of the workforce has slowly risen. Other crucial factors affecting the working population are the general economic climate in the United States, fertility, the cost of living, international migration, and the need for additional health insurance coverage beyond Medicare (Toossi & Bureau of Labor Statistics, 2015). Furthermore, the availability and design of present-day employer-sponsored benefits packages transfer greater financial responsibility to workers.
Family dynamics and unexpected circumstances force some seniors to remain in the workplace (Toossi & Bureau of Labor Statistics, 2015). Career interest and a desire to continue contributing at the workplace may be the deciding factors for others. Because of advances in health care and technology, some older employees can work longer. Interestingly, a noteworthy contributing factor to workplace longevity may be the desire to remain cognitively healthy. Rohwedder and Willis (2010) conducted cross-nationally comparable surveys of older adults in the United States, England, and 11 other countries. Employees who retired in their early sixties later experienced diminished mental ability. Cognitive decline was due to less engagement in cerebral exercises and stimulating activities provided in the work environment that did not exist in the home after retirement (Bonsang, Adam, & Perelman, 2012; Rohwedder & Willis, 2010). Hence, research indicates a positive relationship between working longer and enhanced cognitive function.
Legislations Against Ageism in the Workplace
Ageism is stereotyping and discriminating against individuals or groups based on their age (Butler, 1969). Approximately a half century ago, Robert Butler, MD, identified this overlooked form of bigotry (Butler, 1969). It is evidenced by a deep-seated uneasiness that manifests as a personal revulsion to and a distaste for growing old. Behind concealed apprehension lies an inadequate appreciation for older people, thus allowing stigmatizing behaviors to threaten their well-being. Even so today, age discrimination persists despite the fact that older workers are not less healthy, less educated, less skillful, nor less productive than their younger counterparts (World Health Organization, 2017). The attention to ageism has increased over the decades because a significant segment of the U.S. population (approximately 77 million individuals born between 1946 and 1964 called “baby boomers”) are now choosing whether to retire or continue working (Nelson, 2016).
Passed by the U.S. Congress and signed by President Lyndon B. Johnson, the Age Discrimination in Employment Act (ADEA) of 1967 is a labor law that prohibits employment discrimination against anyone 40 years of age and older (U.S. Equal Employment Opportunity Commission [USEEOC], 2017). The ADEA applies to employers with 20 or more employees and stipulates that employers are not allowed to hire, terminate, promote, or decide an employee’s compensation based on age. The law also forbids discrimination in other aspects of employment (e.g., wages, job assignments, layoffs, training, and fringe benefits). According to the USEEOC (2017), examples of age discrimination against older workers are: (a) not getting hired because the employer wanted a younger-looking worker to do the job; (b) receiving a negative job evaluation because of not being “flexible” in accepting new projects; (c) being fired because the boss wanted to keep younger, less paid workers; (d) denying a promotion, which went to someone younger hired from outside the company because the boss said the company “needs new blood”; (e) being laid off while a younger worker with less seniority and less on-the-job experience was retained; and (f) before being discharged, the supervisor shared age-related remarks such as older workers are “over-the-hill” or “ancient.”
In 1990, a clause was added to the ADEA that prevented the forced retirement of tenured employees such as college professors. The Older Workers Benefit Protection Act amended the ADEA, prohibiting employers from denying benefits to older employees. Congress recognized that the cost of providing certain benefits to older workers was greater than the cost of providing those same benefits to younger workers (USEEOC, 2017).
The Benefits of Hiring Older Workers
Stamov-Roßnagel and Hertel (2010) found that one of the most concerning social phenomena of this century is the widespread aging of the world’s population, identifying this trend in most nations except African countries. Many organizations have learned to keep their competitive edge while broadening their social role by creating opportunities for the development, performance, and retention of older workers. Aging workers bring valuable resources to the workplace because they have generally been with the company for a long time and have insight gained through longevity (Moore & Moore, 2014). Long-term workers are a valuable source of human capital, especially in regard to experience and education (Kroon, van Selm, ter Hoeven, & Vliegenthart, 2016). Realizing the value of older workers has been translated into a successful hiring strategy at several large American companies. Extracting from a pool of affiliated resources, H&R Block hires former certified public accountants and tax specialists. Home Depot hires older contractors and specialty tradespeople, building an accumulated base of expertise (Cappelli & Novelli, 2010). Vasconcelos (2015) confirmed that employers realize the advantages of hiring older workers because employee engagement appears to increase with age. As a group, aging workers were more satisfied, loyal, reliable, and committed. In addition, older employees reported higher emotional well-being and possess effective cognitive strategies to regulate their feelings; those qualities translated well for businesses that needed individuals who excelled at customer service (Vasconcelos, 2015). Another benefit older workers offer to businesses is flexibility. Many relish the freedom of unconventional hours and are willing to work part-time. In many instances, health care coverage is not essential for these part-time, retirement-age workers who are eligible for Medicare (Cappelli & Novelli, 2010).
Ng and Feldman (2010) examined the relationship between age and job performance. They observed four specific counterproductive workplace behaviors: aggression, on-the-job substance use, tardiness, and absenteeism. Meta-analysis results support the proposition that older workers are less likely to exhibit any of these behaviors. Seniors express more favorable job attitudes than younger workers. They report higher levels of work motivation and job involvement. To reduce turnover, employers sometimes consider hiring older workers.
Safety and Health of Older Workers
Older employees in the work environment present two major problems: chronic health conditions and risk of on-the-job injuries (National Institute for Occupational Safety and Health [NIOSH], 2012). More than two thirds or 21.4 million Medicare beneficiaries have at least two or more chronic health conditions. The most common are hypertension (58%), hyperlipidemia (45%), heart disease (31%), arthritis (29%), diabetes (28%), heart failure (16%), chronic kidney disease (15%), depression (14%), chronic obstructive pulmonary disease (12%), Alzheimer’s disease (11%), atrial fibrillation, cancer, and osteoporosis (8%), respectively, asthma (5%), and stroke (4%). Diabetes management is the costliest; one third of Medicare spending is directed at diabetes (Centers for Medicare & Medicaid Services, 2012).
The prevalence of chronic diseases and comorbidities in older adults has safety implications (NIOSH, 2012). Injuries in this subgroup tend to be more serious, thus requiring more recovery time (NIOSH, 2012). Bohle, Pitts, and Quinlan (2010) reported that some safety risks among older workers arise from age-related physical or psychological changes, while other safety risks reflect exposures to unsafe work or employment conditions. Moore and Moore (2014) found age-related changes in cardiovascular and musculoskeletal systems including bone density impact dexterity, reaction to stress, and strength. Falls from the same or greater heights are more prominent across all occupations for workers aged 65 and over and are more likely to result in a fracture or fatality. Type of occupation is the strongest predictor of occupational injuries (Bohle et al., 2010). According to the U.S. Bureau of Labor Statistics, Current Population Survey, Census of Fatal Occupational Injuries (2016), occupations that have the highest number of injuries and days away from work include tractor-trailer truck drivers, freight movers, nursing assistants and other health care workers, manufacturing workers, retail workers, police officers, firefighters, janitors, teacher assistants, and correctional officers.
Older workers’ physical abilities and job demands are associated with risk of injuries (Fraade-Blanar et al., 2017). A mismatch between physical ability and job demand is associated with a higher risk of occupational injury. If the job has demands that the worker cannot physically meet, unsafe practices and poor health outcomes can result (Fraade-Blanar et al., 2017).
As workers age, their injuries are likely to be more severe. Older workers are at less risk for injury than younger workers, but injuries among older workers are more likely to be fatal (Bohle et al., 2010; Moore & Moore, 2014). Workers ages 65 years and over have the highest fatal injury rate of all: 9.4 per 100,000 full-time workers compared with the all ages worker rate of 3.4 per 100,000 (U.S. Bureau of Labor Statistics, Current Population Survey, Census of Fatal Occupational Injuries, 2016).
Evidence-Based Practices for an Aging Workforce
Chosewood (2012) found that a well-designed workplace with policies and programs to optimize the health of aging workers benefits the employer and the employee. As guidelines, these cost-effective strategies are promoted:
Give workers a say in their schedule, work conditions, location, and tasks. Make flexibility a priority.
Match tasks to abilities. Use self-paced work, self-directed rest breaks, and less repetitive tasks.
Avoid prolonged, sedentary work. Consider sit/stand workstations and walking workstations for workers who traditionally sit all day.
Manage noise hazards, slip/trip hazards, and other physical hazards or conditions that can challenge an aging workforce.
Provide ergo-friendly work environments—workstations, tools, floor surfaces, adjustable seating, illumination as needed, and screens/surfaces with less glare.
Use teams and teamwork strategies for aging-associated problem solving; remembering workers closest to the problem are best equipped to find the solution.
Provide health promotion and lifestyle interventions, including on-site physical activity incentives or connections to low-cost community options, healthy meal options, tobacco cessation assistance, risk factor reduction, screenings, coaching, and on-site health care.
Invest in training and building workers’ skills and competencies at all age levels. Assist older employees to adapt to new technologies.
Proactively manage reasonable accommodations like self-care in the workplace, time away for health care visits, and a return-to-work process after illness or injury absences.
Require aging workforce management skills training for supervisors. Include a focus on the most effective ways to manage a multigenerational workplace (NIOSH, 2012).
A Culture That Embraces Multigenerational Workers
A generation is a large group of individuals born during the same period. Group members share similar life experiences such as economics, political movements, and historical events that shape attitudes, beliefs, and values during their formative years and into adulthood (Green, Eigel, James, Hartmann, & McLean, 2012). Today, in many of America’s workplaces, five generations of individuals are working together. Characteristics of each generation appear in Table 1.
Five U.S. Generational Characteristics
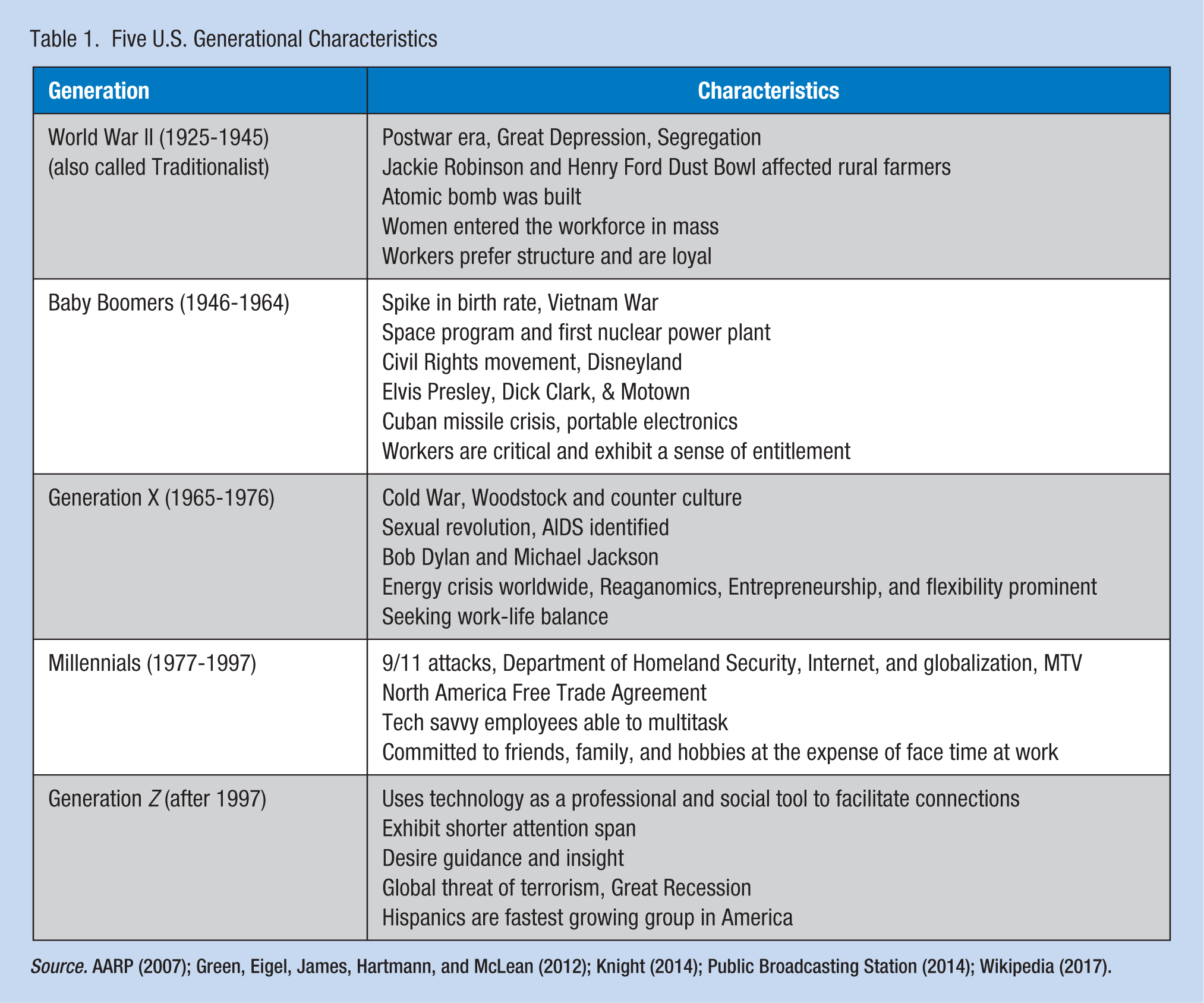
The unprecedented level of age diversity in America’s workplaces has implications related to training, worker motivation, use of technology, recruitment, leadership styles, communication approaches, and teamwork (Rudolph & Zacher, 2015). The workplace is about human interaction and community (Cappelli & Novelli, 2010). Creating a supportive workplace culture involves understanding the generational composition of the workforce, facilitating regular discussions about contemporary issues, and developing programs and policies broad enough to address the needs of all workers. Examples of such interventions include family leave policies that appeal to both younger and older workers and mentoring programs that encourage positive interactions.
According to the Sloan Center on Aging and Work at Boston College (2012), access to flexible work options contributes to overall quality of life for aging workers. Creative scheduling allows employees to work and still attend to personal and family needs. For example, the CVS Caremark Snowbird Program allows workers to change work locations at CVS/pharmacy stores based on seasons, working in northern states during the summer months and southern states in the winter months (Sloan Center on Aging and Work at Boston College, 2012). Proven human resource strategies include fewer days with longer hours, seasonal work based on ebb and flow, flextime, telecommuting options, job sharing, temporary assignments, reduced hours, and phased retirement that is tapered rather than abrupt (Sloan Center on Aging and Work at Boston College, 2012). A fundamental goal of a culture that embraces diversity is to use the unique skills, knowledge, and perspectives of workers in all age groups as a means of developing a more cohesive, productive organization (Rudolph & Zacher, 2015).
Implications for the Occupational Health Nurse
Occupational health nurses play a pivotal role in implementing best practices for adopting workplace cultures that promote aging-friendly workplaces. Placed in the right jobs and integrated properly, America’s expanding pool of senior talent can be advantageous to any business (Sloan Center on Aging and Work at Boston College, 2012). The hiring of aging workers is enhanced by networking with local churches, school systems, civic organizations, and military bases (Cappelli & Novelli, 2010). With the increasing presence of older workers in the workforce, the prevention of occupational injuries and death is paramount (NIOSH, 2012). Older workers must be evaluated to determine their ability to perform specific jobs, and appropriate precautions should be established to maintain safety. Occupational health nurses provide initial and ongoing education regarding workstation hazards and recommend to management needed health and safety improvements (American Association of Occupational Health Nursing [AAOHN], 2017). Another essential duty of the nurse is instructing employees on their responsibility for self-care. The occupational health nurse should encourage employees to develop healthy lifestyle habits related to personal hygiene, use of personal protection equipment, sleep habits, nutrition, weight control, smoking cessation, stress management, psychosocial interventions, immunizations, chronic disease management, and periodic provider visits for health maintenance (AAOHN, 2017). By creating a culture of health in the workplace, the occupational health nurse assists employees in understanding lifestyle choices and the connection between personal health and occupational injuries. Safety improvements benefit workers of all ages (Morrison, 2016).
Applying Research to Practice
Due to the willingness or necessity, older adults are working beyond the traditional retirement age of 65 years. As a result, the American workforce increasingly exhibits an unprecedented level of age diversity spanning five generations. This literature review examines factors associated with changing population demographics, as well as the dynamics related to the presence of older adults in the workplace. Research verifies that the expanding pool of an aging population can be advantageous to both private and public enterprises. Long-term workers are a valuable source of human capital, especially regarding experience, education, and insight gained through longevity in the workforce. Many organizations have learned how to keep their competitive edge while broadening their social role by creating opportunities for the development, performance, and retention of older workers. However, the incidence of chronic disease and comorbidities in aging adults have numerous safety implications. Occupational health nurses play a pivot role in implementing best practices for establishing a culture that promotes safe, aging-friendly workplaces.
Footnotes
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Author Biographies
Mercedia Stevenson White is an MSN student in her final year in the Dual Degree Program Adult Gerontology Primary Care Nurse Practitioner/Occupational Health Nursing at the University of South Florida in Tampa, Florida.
Candace Burns, Colonel (USA Retired), is professor and director of Dual Degree Program Adult Gerontology Primary Care Nurse Practitioner/Occupational Health Nursing, and deputy director of USF Sunshine Education and Research Center (SERC), University of South Florida.
Helen Acree Conlon is an instructor at the College of Nursing and deputy director of Dual Degree Program Adult Gerontology Primary Care Nurse Practitioner/Occupational Health Nursing, USF Sunshine Education and Research Center (SERC), University of South Florida.
