Abstract
This study investigated the current status of infection management for forensic science investigators in South Korea. This study included 104 forensic science investigators, of which 97.1% were exposed to the blood or body fluids of corpses during handling. Of these investigators, 98% claimed they wore gloves, and 12.9% used double-layered gloves. A total of 70.6% of the participants with relevant work experience wore masks to reduce infection risk; 43% wore gowns and goggles when at risk of contracting an infection. Furthermore, 59.8% of the investigators with pertinent work experience sought appropriate first aid and treatment when they experienced contaminated skin cuts or stab wounds. Working conditions and other problems should be analyzed consistently with the cooperation of employees, occupational health practitioners, and relevant organizations to prevent work-associated infections among forensic science investigators.
Forensic science investigators contribute to criminal charges by providing comprehensive examination of corpses suspected of unnatural deaths. More than 20,000 unnatural deaths occur annually in South Korea, and the number continues to increase (National Police Agency, 2012). Violent crimes, which reached an annual minimum of 70,000 in 2002, increased to approximately 270,000 in 2011 (Korean National Statistical Office, 2013). Forensic science investigators usually begin their careers with initial investigation tasks such as collecting evidence and examining the exterior of victims of unnatural death or those suspected thereof. In South Korea, forensic science investigators are responsible for all tasks throughout the investigation process, including postmortem examinations (i.e., autopsies) that determine the cause of death (Kim, 2009; National Police Agency, 2007). While performing their duties, these workers are at high risk for exposure to the blood and body fluids of corpses, including at crime scenes. In particular, stab wounds and cuts occurring during autopsies are likely to cause blood-borne diseases (Hong & Choi, 2008; National Police Agency, 2007; Pfeiffer, 2009). Decomposed bodies are sometimes found several days or even several months after death. Inhalation of gases produced by bacteria or infection from pathogenic microorganisms during decomposition can seriously affect worker health and may even be lethal (Kim, 2009; Korean Society for Nosocomial Infection Control, 2006). Such exposures to pathogenic microorganisms not only affect the health of the exposed individual but may also cause cross-contamination to other individuals in close proximity, such as colleagues and family members. Therefore, establishing systematic, thorough control measures is imperative.
Previous studies of police officers’ exposures to blood and body fluids investigated the rate of exposure incidents (Sonder et al., 2005), risk factors (Averhoff et al., 2002), postexposure management (Dunleavy, Taylor, Gow, Cullen, & Roy, 2010), and tuberculosis infection (Lledó, Gegúndez, Saz, & Beltrán, 2002). Despite the importance of preventing exposures to pathogens while forensic science investigators are working on cases involving communicable blood-borne or respiratory infections (Hong & Choi, 2008; Pfeiffer, 2009), a lack of research has been published on the status of forensic science infection management with evidence-based guidelines (National Police Agency, 2007). Therefore, this study investigated the current status of infection management during forensic science investigations to establish effective disease control measures for these workers.
Method
This descriptive cross-sectional study included forensic science investigators affiliated with the National Forensic Service of the Korea Criminal Investigation Bureau. A questionnaire was distributed to 140 investigators selected from 813 forensic investigators (Park, 2006) via convenience sampling. A total of 104 investigators were included in the study because 36 respondents provided insufficient answers and were excluded.
This study was approved by the Institutional Review Board of Jeju National University. Data were collected from February 2013 to April 2013. After receiving permission from the National Forensic Service of the Korea Criminal Investigation Bureau, the purpose of this study, questionnaire content, and right of refusal were explained to the participants. Questionnaires were subsequently distributed to the forensic investigators who agreed to participate and were collected through the mail. The questionnaire required approximately 20 minutes to complete.
Measures and Definitions
The demographic characteristics of the sample included age, sex, work experience as a police officer, work experience as a forensic science investigator, number of criminal death cases completed, and time taken to investigate a crime scene. The current status of infection management was assessed using a questionnaire developed by the research team on the basis of previous papers (Korean Society for Nosocomial Infection Control, 2011; Ministry of Health & Welfare, 2010). The tool included 22 questions in five categories, including personal protective equipment (six items), hand hygiene and injury (four items), facilities for corpse enshrinement and autopsy rooms (six items), corpse-transportation vehicles (three items), and disinfection and laundry (three items). Provided the investigators had work experience relevant to each item, they responded either “yes” or “no.” Regarding health practices of the study participants, the researchers investigated regular examinations, vaccinations, underlying diseases, desired health education topics, infection management education experience, and infection management education demand. The general characteristics, current status of infection management, and health practices of the investigators were analyzed using descriptive statistical methods.
Results
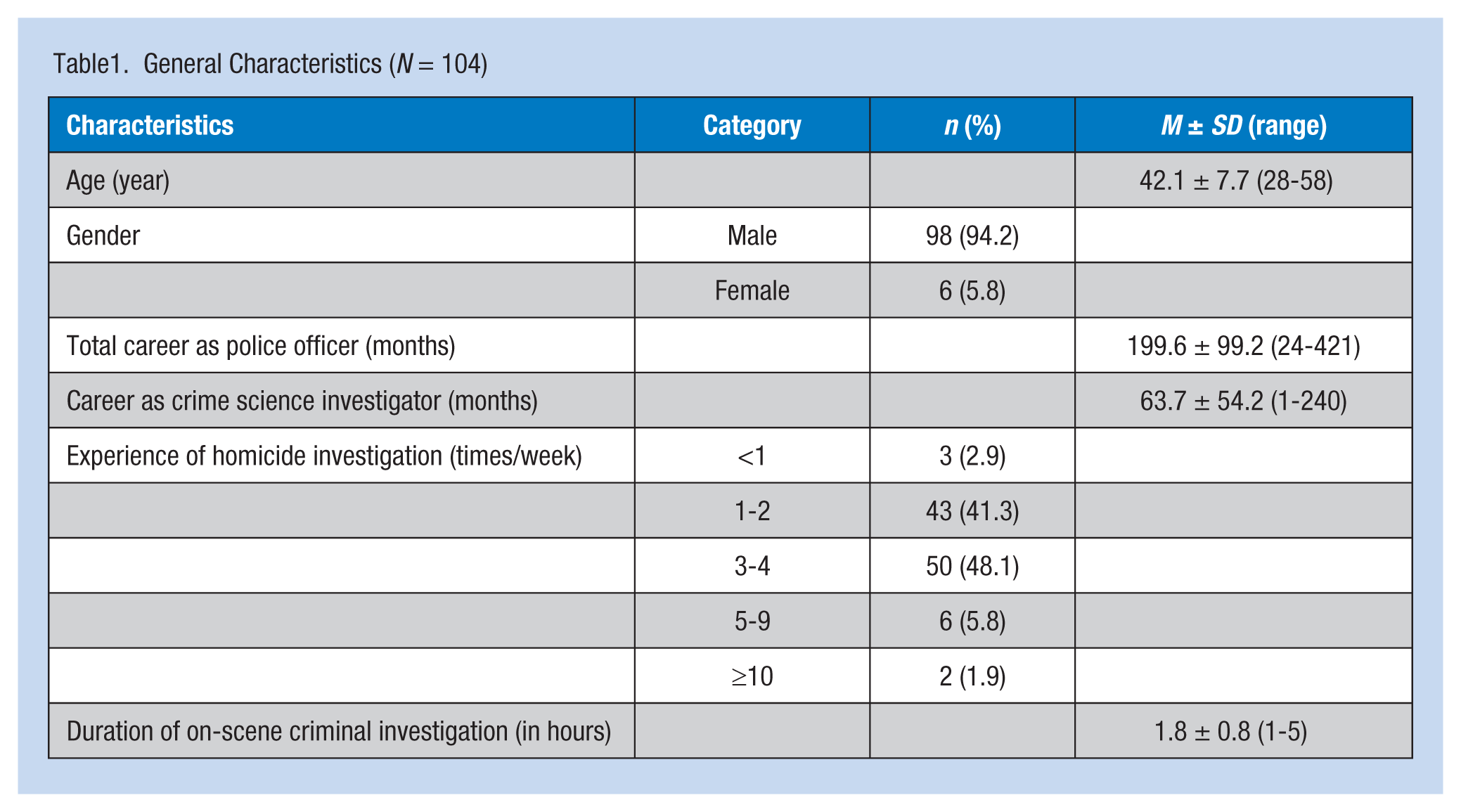
The mean age of the investigators was 42.1 years (range = 28-58 years); 94.2% were men. The average duration of service as a police officer and forensic science investigator was 199.6 months and 63.7 months, respectively. Regarding the number of experiences of criminal death cases, 97.1% of the participants reported more than one case a week. The participants spent an average of 1.8 hours investigating the scene per case (Table 1).
General Characteristics (
Current Infection Management
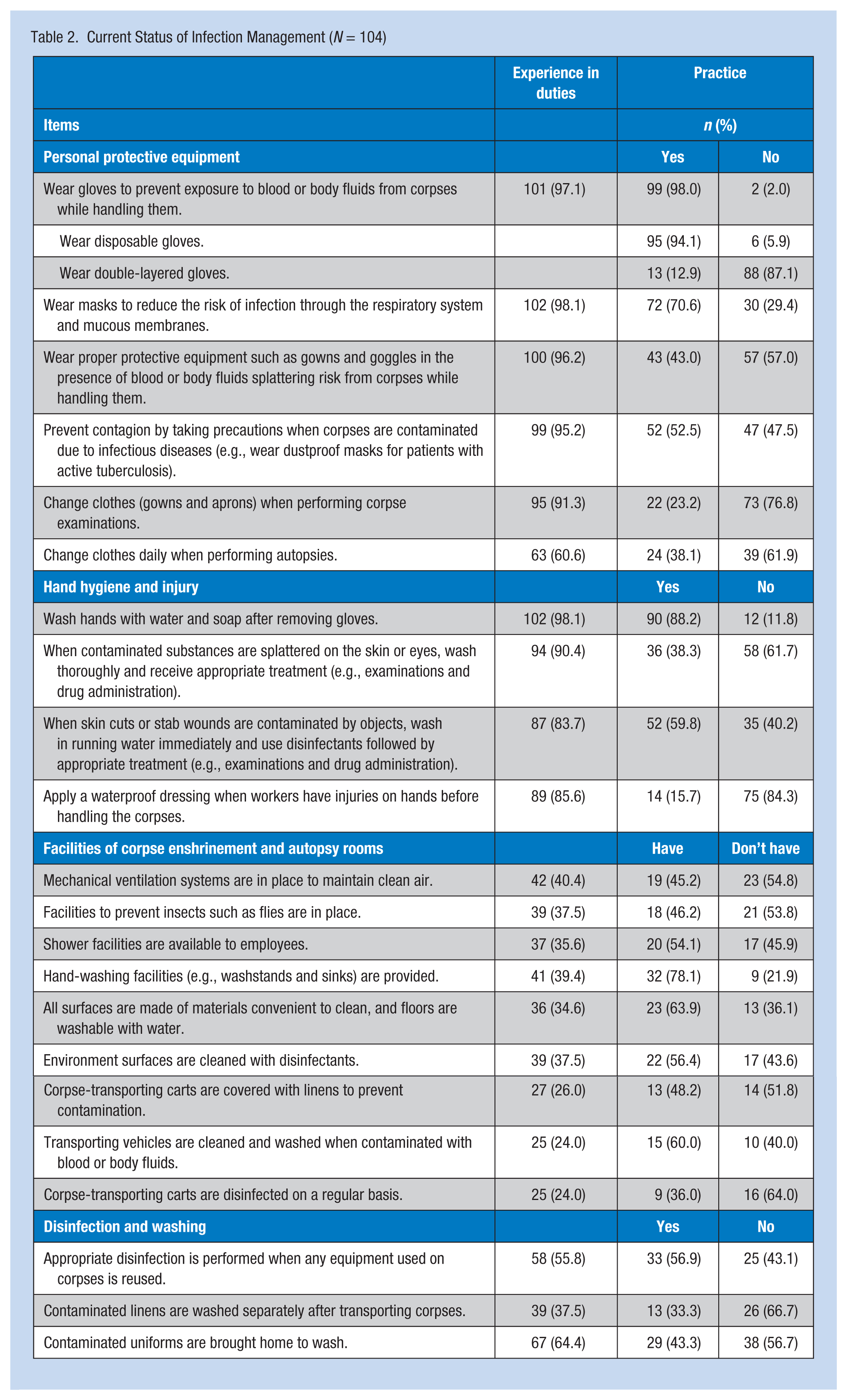
Of the 97.1% of the participants reporting exposure to corpse blood or body fluids while handling them, 98% answered that they “wear gloves” for personal protection. In particular, 94.1% and 12.9% used disposable gloves and double-layered gloves, respectively. A total of 70.6% of the investigators with relevant work experience responded affirmatively to “wear masks to reduce the risk of infection through the respiratory system and mucous membranes.” In addition, 43% of the experienced participants affirmed that they “wear proper protective equipment such as gowns and goggles when at risk for splattering blood or body fluids of corpses while handling them,” and 52.5% of the investigators wore personal protective equipment to “prevent contagion by taking precautions in case the corpses were contaminated by infectious diseases.” Of the 91.3% of the participants responsible for corpse examination, 23.2% responded affirmatively to “change clothes when performing the corpse examination.” Of the investigators participating in autopsies, 38.1% replied affirmatively to “change clothes daily when performing autopsies.”
Hand hygiene
Regarding hand hygiene and injury, 88.2% of the participants with relevant work experience answered affirmatively to “wash hands with water and soap after taking off gloves.” Meanwhile, 38.3% of the respondents with pertinent work experience sought appropriate first aid and treatment when “contaminated substances were splattered on the skin or in eyes,” and 59.8% sought treatment when “there was skin cuts or stabs by contaminated substances.” Furthermore, 15.7% of investigators with pertinent experience responded affirmatively to “apply a waterproof dressing when there are injuries on hands before handling the corpse.”
Facilities and vehicles
Of the participants who work in the corpse enshrinement and autopsy rooms, 45.2% replied affirmatively to “there are mechanical ventilation systems,” and 46.2% affirmed that “there are facilities to prevent insects such as flies.” In addition, 54.1% and 78.1% of the investigators with pertinent work experience answered that there were “shower facilities” and “hand-washing facilities for employees,” respectively. Furthermore, in the corpse enshrinement and autopsy rooms, 63.9% of the experienced investigators affirmed that “all surfaces are made of materials convenient to clean, and floors are washable with water,” and 56.4% reported that “environmental surfaces are disinfected by disinfectants.”
To manage corpse-transportation vehicles, 48.2% of the respondents with relevant work experience (26.0%) responded affirmatively to “cover corpse-transporting carts with linens to prevent contamination.” In addition, 60% of the investigators with relevant work experience responded affirmatively to “transport vehicles are cleaned and washed when contaminated with blood or body fluids,” and 36% reported that “corpse-transporting carts are disinfected on a regular basis.”
A total of 56.9% of experienced investigators responded affirmatively to “appropriate disinfection is performed before any equipment used on corpses is reused,” 33.3% of the participants with relevant work experience responded affirmatively to “contaminated linens are washed separately after transporting corpses,” and 43.3% of experienced investigators reported that contaminated uniforms were washed at home (Table 2).
Current Status of Infection Management (
Health Practices
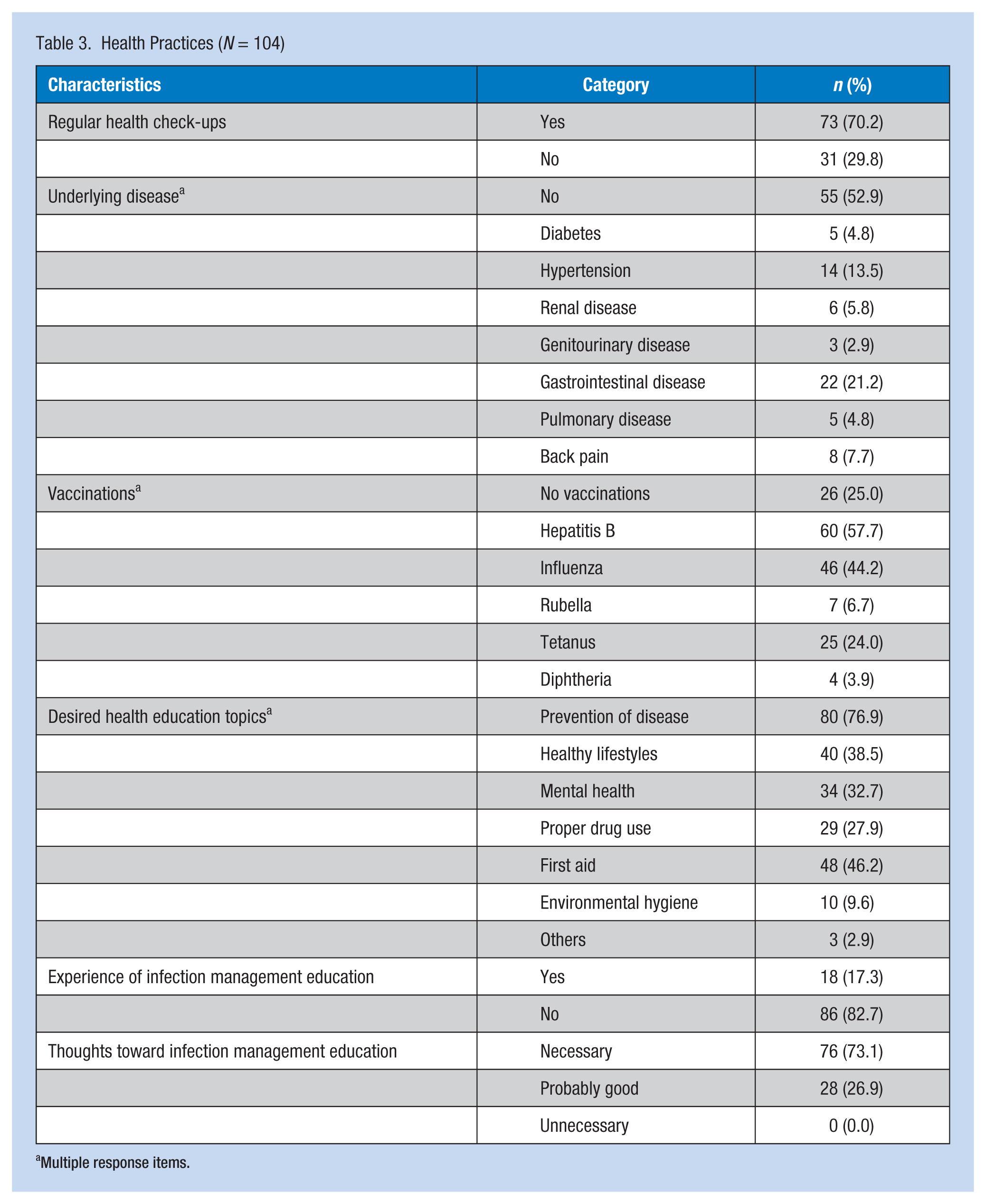
Vaccination rates among the investigators were highest for hepatitis B at 57.7%. Other vaccines had lower rates: influenza (44.2%), tetanus (24%), diphtheria (3.9%), and 25% of the participants did not have any vaccinations. In addition, underlying diseases such as gastrointestinal diseases, hypertension, and diabetes were reported by 47.1% of the participants.
The topic of health education most requested by forensic science investigators was the prevention of diseases (76.9%), followed by first aid (46.2%), healthy lifestyles (38.5%), mental health (32.7%), proper drug use (27.9%), and environmental hygiene (9.6%). Significantly, 82.7% of the investigators had not received infection management education, even though 73.1% and 26.9% replied affirmatively to “infection management education is necessary” and “the education is probably good,” respectively (Table 3).
Health Practices (
Multiple response items.
Discussion
Corpses can be sources of infection, especially for individuals who handle them as part of their work (Burton, 2003). Most of the pathogenic bacteria in corpses can easily be transferred during procedures such as autopsies. Blood-borne diseases, pulmonary tuberculosis, and tetanus are associated with a high risk of infection. The hepatitis B virus can survive more than 7 days in the environment, tetanus can survive in the environment for several years (Beltrami, 2009) and HIV is also known to survive for more than 6 days in a dead body (Nyberg, Suni, & Haltia, 1990). Therefore, pathogenic microorganisms isolated from the blood or body fluids of a corpse can pose significant health threats to forensic science investigators working death scenes.
Crime scenes include a wide range of physical environments, which make it difficult to accurately differentiate between contaminated and non-contaminated materials. Therefore, forensic science investigators must always wear personal protection equipment to prevent exposure to blood or body fluids from a corpse. Sharp pointed objects should be covered with safety caps, and all evidence should be safely collected, wrapped, and transported in protective containers. In particular, special care should be taken to avoid pressure or impact when transporting corpses to avoid contamination with microorganisms from them (Hong & Choi, 2008).
In this study, 97.1% of the participants reported encountering crime-related corpses more than once per week and spending an average of 1.8 hours investigating a scene. Although wearing double-layered gloves is recommended for individuals who handle corpses to reduce the risk of infection due to perforated gloves (Pfeiffer, 2009), an astounding 87.1% of the participants with corpse-handling experience did not. In addition, waterproof dressings are prescribed in the presence of injuries on hands before handling corpses to prevent infectious agents from spreading through the injured skin; however, only 15.7% of experienced investigators complied with this guideline.
Wearing proper personal protective equipment is the most effective way to avoid propagating infections. Waterproof gowns should be worn when blood or body fluids could splatter from a corpse, and masks or safety glasses should be worn in the presence of potential respiratory system and mucous membrane exposures (Pfeiffer, 2009). Nevertheless, the results of this study revealed that only 70.6% of the investigators with relevant work experience wore masks and gowns, and a mere 43% wore goggles. Wearing proper protective equipment while transporting or examining a corpse with a known infectious disease, such as tuberculosis, also had a low compliance rate (52.5%). Microorganisms separate from the decomposed bodies of infectious disease victims leading to colony formation in nasal cavities through droplets or air, resulting in respiratory system infections. Moreover, when dissecting tissues or using saw blades to incise the lungs or pustules during autopsies, wearing appropriate protective equipment for the respiratory system, such as N95 masks, is imperative because contaminated tissues or body fluids from the corpse can disseminate through the air and result in infection spreading through the examiner’s respiratory system (Newsom, Rowlands, Matthews, & Elliot, 1983).
To improve the low utilization of personal protective equipment, awareness of ways to prevent occupational infection exposures should be raised in forensic science investigators, and substantial effort should be made toward implementing such methods.
Forensic science investigators play the most significant role in infection prevention. In other words, forensic investigators should recognize the importance and necessity of infection management, acquire sound knowledge about preventive strategies, and implement such knowledge. Because inconvenience or inadequate personal protective equipment can be reasons why the equipment is not used, easy access and availability of personal protective equipment are crucial. In this regard, kit-type equipment may be useful and can be distributed and ready for use as needed.
In this study, 90.4% of the participants had experienced splattering of contaminated substances on the skin or in the eyes, and 83.7% of these individuals had skin cuts or stab wounds; yet, only 38.3% and 59.8% of the experienced investigators received appropriate first aid or treatment for splattering and cuts or stab wounds, respectively. According to a study by Dunleavy et al. (2010), 71% of police officers reporting blood and body fluid exposure to an occupational health service had exposures via mucous membranes, injured skin, or injuries from sharp objects; 32% of these injuries were contaminated by body fluids containing highly infectious blood. Therefore, occupational health nurses should provide first-aid training for employees to handle occupational high-risk blood or body fluid exposures to reduce the risk of infection. In addition to treatment by health care providers and administration of preventive drugs, greater efforts should be made to educate employees about early detection and disease prevention, including exposure management such as regular antibody and radiological examinations. Furthermore, attention should be paid to the mental health of exposed employees, including resulting stress, depression, and anxiety when they are injured and exposed to infectious microbes at work (Sohn, Kim, Kim, & Han, 2006).
Because microorganisms and the resulting diseases likely spread to colleagues and family members when the hands and clothes of investigators are contaminated while on duty, appropriate hand hygiene and clothing management are critical. Substantial numbers of participants reported a lack of hand-washing facilities (21.9%) and shower facilities (45.9 %). The absence of such basic facilities negatively affects disease prevention.
Morgan et al. (2010) reported that 38.7% of gloves and clothes are contaminated after corpse contact, and the hand contamination rate after hospital workers remove gloves is approximately 5%, indicating that hand hygiene after removing gloves is extremely important. In this study, many investigators were at risk for clothing contamination because only 23.2% and 38.1% of the participants with relevant work experience answered affirmatively to “change clothes for corpse examination” and “change clothes daily for autopsies,” respectively; in addition, 43.3% of experienced investigators responded affirmatively to the statement “bring contaminated uniforms home to wash”; thus, the risk of cross-contamination from work uniforms was high. Because infection can occur not only among forensic science investigators but also among other individuals through direct and indirect contact, special efforts should be made to prevent cross-contamination via hands and clothes. To prevent cross-contamination through contact, protective clothes and gloves are required when examining corpses; contaminated clothes should not be taken outside the workplace and should be washed separately by a designated agency.
Mechanical ventilation systems should be installed in corpse enshrinement and autopsy rooms to prevent infection transmission (Pfeiffer, 2009). In the present study, 54.8% of the participants with work experience responded that mechanical ventilation systems were not installed at their workplaces. In addition, proper sterilization and disinfection should be routine in corpse enshrinement and autopsy rooms as well as in corpse-transporting carts and in corpse-transportation vehicles (Pfeiffer, 2009); however, study results suggest that sterilization and disinfection are currently not routine. Inappropriate environmental management is likely to result in contamination of the surrounding environment and equipment that comes in contact with forensic science investigators during work, thereby increasing the risk of infection among employees and cross-contamination infecting other individuals. Thus, environmental management guidelines should include a list of items requiring disinfection, required disinfectant types and their dilution concentrations, and disinfection cycles. Creating and providing an easy-to-use checklist could maximize this effort.
Given that this study found only 57.7% of the investigators were vaccinated against hepatitis B, which has a high rate of carriers in South Korea, measuring hepatitis B antibodies in forensic science investigators is essential for preventing infection among employees. In addition, tetanus, for which vaccination is recommended for all adults (The Advisory Committee on Immunization Practices Adult Immunization Work Group, Bridges, Woods, Coyne-Beasley, & Centers for Disease Control and Prevention, 2013), can occur due to contaminated wounds, and has a notably high mortality rate. Spores of causative strains inhabit soils, dogs, cats, rodents, and human intestines, and constantly pose a risk for infection (Korea Center for Disease Control and Prevention, 2013).
Fostering a healthy immune system and appropriate prophylaxis and treatment should be expected, even in cases of minor injuries. Immediately providing effective first aid and health care treatment after exposure to blood or body fluids is imperative to prevent infection. Drugs such as immunoglobulin and antiviral agents can be administered to prevent hepatitis B and HIV infection, and the risks of infection can be noticeably reduced through continuous monitoring (Beltrami & Perz, 2009). No preventive drugs for administration at the time of exposure have been developed for hepatitis C; therefore, personal protective equipment should be worn when contact with blood or body fluids is anticipated. Furthermore, besides regular examinations and vaccinations against diphtheria, pertussis, tetanus, influenza, hepatitis A, and hepatitis B, the Korea Center for Disease Control and Prevention recommends vaccination against measles, mumps, rubella, and varicella for those engaged in jobs with risks of exposure to blood and body fluids. Such efforts contribute to the prevention, early detection, and management of occupational diseases that forensic science investigators are likely to contract.
To prevent infections in forensic science investigators attending actual scenes, education about infection management must be required. Despite the finding that all participants in this study desired infection management training, only 17.3% of study participants had received such education. Systematic periodic education on personal health care strategies and environmental management, including the importance and proper use of personal protective equipment, first aid when exposed to blood and body fluids, and vaccinations, must be developed. In addition, continuing and recurring education rather than temporal and formal education should be implemented to facilitate the application of acquired knowledge to real work situations. Public relations campaigns using posters to remind workers of the significance of infection management could also positively affect infection management among employees. In addition to increasing knowledge regarding infection management among forensic science investigators, it is necessary to establish a system that directly observes and continuously monitors their compliance with infection prevention rules. Such a monitoring system could safeguard their health and safety by boosting their awareness of adhering to infection prevention rules as their essential right and duty.
In conclusion, working conditions and problems should be analyzed consistently with the cooperation of the employees, occupational health practitioners, and relevant organizations to prevent work-associated infections in forensic science investigators. Furthermore, continuous efforts should be made to improve preventive measures.
Implications for Practice
Most of the participants who reported exposure to the blood or body fluids of corpses stated that the exposures occurred during handling. The rate of hand hygiene and proper use of personal protective equipment were relatively low, so improvements are needed. Also equipment or facilities management systems in corpse enshrinement and autopsy rooms, and corpse-transporting vehicles were lacking. Therefore, basic facilities and environmental management guidelines should be developed to improve infection control for workers. Appropriate first aid and treatments after exposure to blood or body fluids were also lacking, and vaccination coverage of blood-mediated diseases was low. More occupational health management systems for forensic science investigators are needed. Because forensic investigators should recognize the importance and necessity of infection management, occupational health professionals should focus on providing continuing and recurring education.
Applying Research to Practice
Forensic science investigators reported inadequate equipment or facilities management systems, hand hygiene and proper use of personal protective equipment, vaccination, and management of exposures to blood or body fluids. This survey of the current status of infection management for forensic science investigators should establish needed infection prevention and control strategies.
Footnotes
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Author Biographies
Kyeong-Sook Cha, PhD, RN, is an assistant professor, Department of Nursing Science, Sun Moon University.
Ok-Hee Cho, PhD, RN, is an associate professor, Department of Nursing, College of Nursing and Health, Kongju National University.
Yang-Sook Yoo, PhD, RN, is a professor, College of Nursing, The Catholic University of Korea.
