Abstract
This research study investigated college women’s usage of personal care products and their views on health effects from exposures during the preconception period. Many personal care products and cosmetics contain chemical ingredients that have been known to disrupt human endocrine and neurological systems, and contribute to infertility and adverse birth outcomes. Seventy-two female college students from a single, medium-sized university campus completed a researcher-developed questionnaire. Findings provide insight into the daily exposures young women experience during their reproductive years. Results can inform occupational and environmental health nurses about the personal daily exposures of young women when conducting risk assessments in the workplace or at a school, and can aid in developing interventions that support the environmental health of employees or future employees.
Keywords
Exposures to environmental contaminants have been identified as contributors to adverse health effects for the general population as well as for vulnerable populations such as women of childbearing age. It is estimated that in U.S. homes and workplaces, Americans use more than 83,000 chemicals, and very few of them have been tested for safety; in fact, the U.S. Environmental Protection Agency (EPA) has published evaluation data for only 200 of 83,000 chemicals (Simitian, 2010; Wilson & Schwarzman, 2009). Bio-monitoring studies conducted by the Centers for Disease Control and Prevention (CDC) confirm that measurable levels of several contaminants (e.g., known carcinogens, hormone disruptors, and lead) have been detected in blood and urine samples of the U.S. population including pregnant women (Center for Disease Control and Prevention [CDC], 2011, 2010).
Some chemicals pose a particular threat because they have the potential to linger or bio-accumulate in the environment as well as in the human body, and others, while not suspected to accumulate, are presented as recurrent, low-dose exposures of which the consequences are not fully understood. Evidence suggests that multiple exposures to chemicals that result in the same adverse health outcome may create a greater impact than exposures from individual chemicals acting alone (Woodruff, Zota, & Schwartz, 2011). Individuals may use or come into contact with a wide variety of chemicals and environmental exposures every day. Contaminants can be inhaled, ingested, and absorbed through the skin, and are known to pass through the placenta and breast milk. Chemicals raising specific concerns for childbearing women are those that affect reproduction, fetal development, infant mortality, and birth outcomes, and those linked to hormone disruptions of the thyroid gland, asthma, neurological deficits, and cancers (CDC, 2010, 2011; Chalupka & Chalupka, 2010; Dott, Rasmussen, Hogue, & Refhuis, 2010; Dunagan, Dodson, Rudel, & Brody, 2011; Sutton, et al., 2012; Woodruff et al., 2011). Chemicals passing through the placenta and breast milk amplify exposure risks for infants and children potentially affecting child health (Sutton et al., 2012).
It has been suggested that most consumers give little thought to the personal care products they purchase for daily use, and may assume these products are safe. However, it is estimated that only 10% of the 10,500 chemicals in personal care products have been evaluated for safety by the U.S. Food and Drug Administration (FDA), and the cosmetic industry remains a mostly self-regulated entity in the United States (Goleman, 2010; Houlihan, 2011). The FDA considers cosmetics to be any material that can be rubbed, poured, sprinkled, sprayed, or otherwise applied to the human body for cleansing, beautifying, promoting attractiveness, or altering appearance (U.S. Food and Drug Administration [FDA], 2010). Items generally considered personal care products such as moisturizers, perfumes, lipsticks, fingernail polishes, eye and facial make-up preparations, shampoos, hair colors, toothpastes, and deodorants are usually considered cosmetics by the FDA. The FDA requires cosmetics list ingredients in order of prevalence except those ingredients contained within fragrances and does not require health studies or premarket cosmetic testing (Dodson et al., 2012).
Most consumers are likely unaware of the risks that exposures from using these products pose. A number of personal care products including shampoo, toothpaste, soap, deodorant, hair conditioner, lip balm, lipstick, lotions, shaving products, nail polish, and cosmetics have been found to contain carcinogens, pesticides, reproductive toxins, endocrine disruptors, plasticizers, degreasers, and surfactants (Houlihan, 2011). Women of childbearing age, described as between 18 and 44 years old, are vulnerable to the effects of environmental exposures because of their preconception status and the relationship that current health may have on future health (Sutton et al., 2012). The National Health and Nutrition Examination Survey (NHANES) found that 99% to 100% of pregnant women are exposed to a variety of chemicals, including banned insecticides like dichlorodiphenyltrichloroethane (DDT) that may be harmful to a developing fetus (Woodruff et al., 2011).
Young women may not be aware that daily hygiene habits increase exposure to environmental toxins affecting their personal and reproductive health. For many years, preconception health counseling to promote the health and well-being of prenatal women has centered on the first prenatal visit; however, much of fetal development may have already occurred before this time (CDC, 2006; Delgado, 2008; Frey & Files, 2006; Moos, 2004; Posner, Johnson, Parker, Atrash, & Biermann, 2006). The goal of preconception health care is to identify risks prior to conception and initiate prevention strategies to reduce risks and improve health outcomes for women of childbearing age and their offspring (Moos, 2010). The complex interaction of biological, social, physical, chemical, and environmental factors are thought to contribute to individual and population health, and play a significant role in reproductive health and infant outcomes (Sutton et al., 2012).
The purpose of this study was to examine exposure risks and describe what female college students know about exposures to environmental toxins in personal care products and their possible effects on preconception health. The researchers hypothesized that female college students are unaware of the risk for environmental toxins in personal care products or the effects these toxins may have on preconception health. Variables investigated included the quantity and variety of products students used within a 24-hr period, the frequency of daily applications of personal care products, and the awareness that exposure poses a concern for reproductive health.
Method
Data were collected at a single, medium-sized university campus between February and March, 2013. A non-experimental, descriptive research questionnaire was distributed and included both closed- and open-ended questions. Female students majoring in the top three female-dominated majors at the university (i.e., nursing, psychology, communication science and disorders) were recruited via email to participate in the online or paper survey. Students were also invited to complete the survey at a college wellness fair and through personal contact. The 72 participants who qualified were 18-to-24-year-old, non-pregnant, English-speaking women; 96% were Caucasian. The homogeneity of the university student body was reflected in the study sample. The study included 54 nursing (75%), 11 psychology (15%), and 7 communication science and disorder students (10%). All procedures were approved by the university’s Human Subjects Review Board.
The two key concepts addressed in this study were personal care products and preconception health. Five groups of personal care products included general hygiene products (e.g., soap or body wash, toothpaste, deodorant), hair products (e.g., shampoo, conditioners, gels), cosmetics (e.g., foundation, lipsticks, eye and facial preparations), other products (e.g., lotion, suntan lotion, perfumes), and nail polish and polish removers. The concept of preconception health challenges health providers to promote health for women, infants and families by identifying and addressing risks such as genetic risks, health status and history, lifestyle and exposures to environmental toxins that may significantly affect pregnancy outcomes (Delgado, 2008).
Theoretical Framework
An Integrated Model for Environmental Health Research (Dixon & Dixon, 2002) was used in this investigation to explain young women’s understanding of how toxins in personal care products affect preconception. The model incorporates perspectives from social psychology, toxicology, and health behavior and focuses on the interrelationships of four domains: physiological, vulnerability, epistemological and health protection (Dixon & Dixon, 2002; Harnish, Butterfield, & Hill, 2006). The foundation of the model links scientific knowledge, behavior and the effect of environmental factors and hazardous exposures to the quality of life of individuals and communities. This investigation focused on the first three domains: physiological, vulnerability and epistemological (Figure 1).
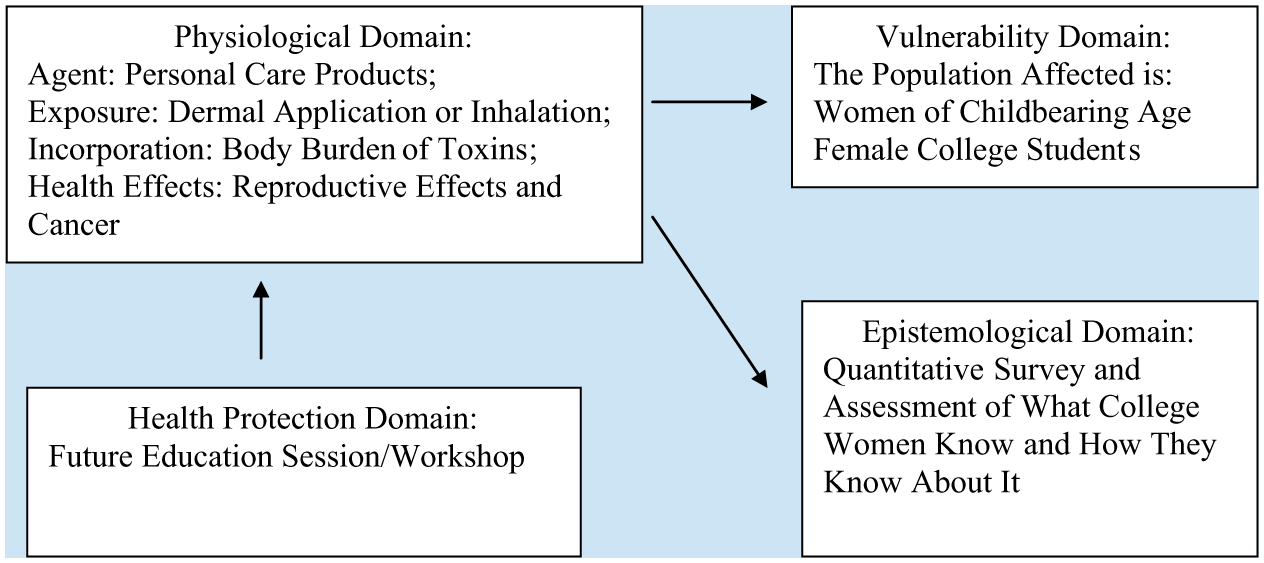
Dixon’s and Dixon’s Integrative Environmental Health Model.
The physiological domain asks, “What is the problem?” and is concerned with chemical and physiological processes by which substances in the environment affect health. This research addresses the problem as daily exposure to chemical toxins from personal care products absorbed and possibly accumulated in body tissues and later linked to adverse reproductive outcomes.
The vulnerability domain asks, “Who is affected?” and focuses on individuals and communities. Young women of childbearing age are susceptible and vulnerable because of their physiology, changes in body tissue, accumulation of toxins in fat tissue, and greater risk of transmission to their children through the placenta and breast milk (Dixon & Dixon, 2002). Because of the importance of optimizing health before pregnancy, this study primarily targeted 18-to-24-year-old female college students.
The epistemological domain asks, “How does everyone know about this?” It asks how women learn about these risks and what they understand about the effects of environmental health on reproduction. This investigation also examined young women’s views on preconception health.
The fourth health protection domain asks, “What do people do about it?” and includes individuals’ concerns, sense of efficacy, and actions taken related to environmental health. Although not addressed in this article, the results of this study were subsequently used to develop a nursing intervention workshop to promote preconception health and healthy lifestyles in young women.
Instrument
Survey questions were derived from concepts and themes identified in the literature and based on the physiological, vulnerability, and epistemological domains of Dixon’s and Dixon’s Integrative Environmental Health Model. (A separate survey was used to collect demographic information.) The survey included both open- and close-ended questions, with multiple statement or categories soliciting multiple responses. Specifically, 8 questions focused on the physiological, 11 questions on the vulnerability, and 4 questions on the epistemological domains. Response bias, format and clarity of the instrument may have affected the accuracy of the study data.
The survey tool was evaluated for validity by three experts in the field who reviewed the survey for content validity and clarity. Three volunteer undergraduate students reviewed the tool for readability and the estimated time of completion. Because this was the first time the tool was used, the tool did not have reliability or validity data from other studies. The questions about instrument effectiveness should be addressed in future studies. Using demographic information, a total of 72 participants qualified for the study. Descriptive statistics were used to analyze the data.
Results
Physiological
The physiological questions asked participants to recall how many cosmetics and personal care products they used during the past 24 hours. Sixty-nine percent of participants used 11 products on a daily basis; more than half (56%) used 12 products. These products included toothpaste, deodorant, hand sanitizer, shampoo, conditioner, soap, lotion, lip gloss/chap stick, face cleansers, foundation, mascara and eyeliner (Figure 2). Students were then asked to count how many times they applied or reapplied each particular product during the past 24-hour period. Items applied less than twice were considered “low-use.” Items reapplied three to four times a day were considered “moderate-use.” Several moderate-use products included toothpaste (40%), lotion (30%), lip gloss/chap stick (27%) and deodorant (24%). Items reapplied more than five times a day were considered “high-use.” The top three high-use products were hand sanitizer (64%), lip gloss or chap stick (24%) and soap (17%; Figure 3).
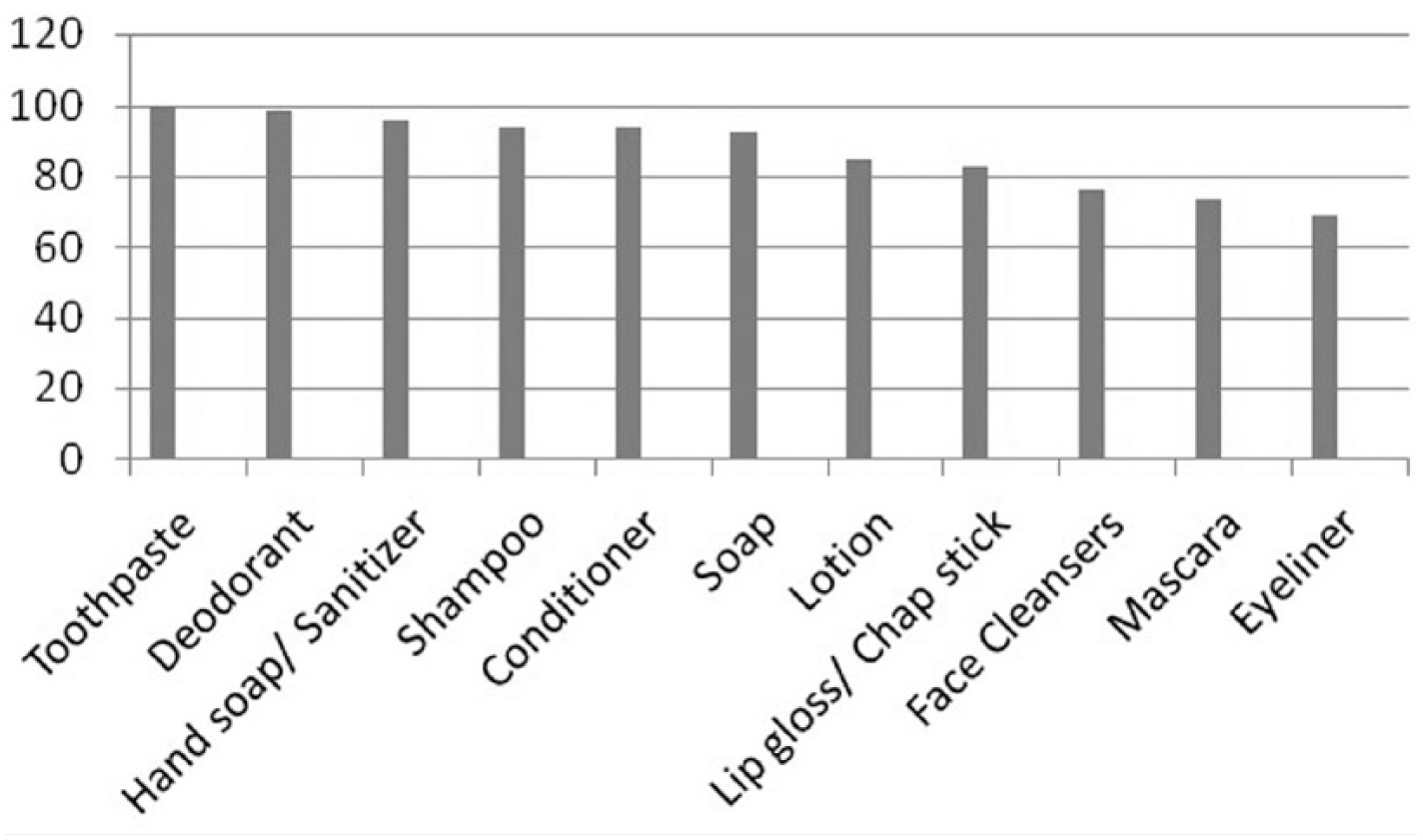
Percentage of female college students who use specific personal care products daily.
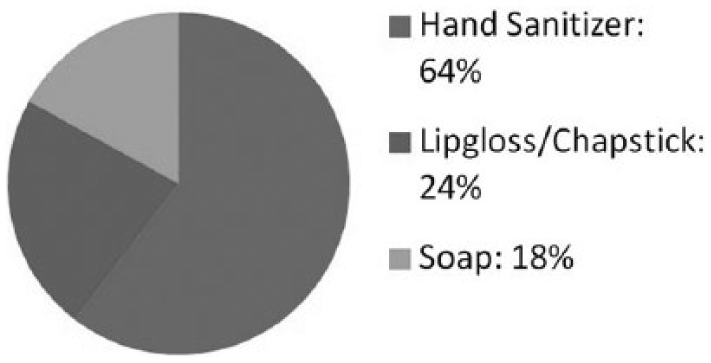
Percentage of high-use products reapplied more than five times in 24 hours.
The remaining physiological questions asked students to rate responses to statements on a Likert-type scale. Only 34.7% of students reported being exposed to toxic chemicals at home or where they live; the remaining participants disagreed (46%) that they were exposed, or were unsure (23.6%). Approximately 42% of students thought using cosmetics was safe, but nearly half (48.6%) the participants were uncertain. More than half (56%) stated they used scented personal care products, 22% said they did not use fragranced products, and 22% were neutral. Scented products are of concern because according to Dodson et al. (2012), fragranced products may contain 3,000 ingredients, including 50 to 300 chemicals linked to adverse health effects.
The majority of students perceived environmental health issues to be related to larger environmental concerns such as poor air quality and pollution (77%) and water contamination (26%) rather than personal care products (3%).
Students were also asked, “What questions or concerns do you have about possible exposure to environmental toxins?” More than half (51%) of students were concerned about the effect that exposure to everyday chemicals could have on their current and future health. Thirty-one percent of students wanted to know where to obtain more information on product safety and regulations, and how to reduce risks. Seventeen percent of students had no concerns about exposures to environmental toxins.
Vulnerability
A majority of students (88%) were concerned that their bodies may not be able to overcome the toxins to which they are exposed. Eighty-seven percent of participants expressed concerns about toxins in the home and in personal care products. Twenty-seven percent of participants did not believe their use of personal care products affected their current health. However, 79% reported that the use of household and personal care products could affect their preconception health.
Eighty-two percent of participants understood that most chronic illnesses arise from a combination of genes and environmental factors, but only 42% connected illness to exposures from environmental toxins and pollution. A larger number of participants (85% to 90%) believed that genes, heredity, diet, personal health, and exposure to air and water pollution were major contributors to preconception health.
Epistemological
Sixty-four percent of participants stated that in the last 6 months they had heard about chemicals in personal care products on TV or the Internet. Almost half (49%) of students discuss personal care purchases with their friends. Students reported receiving information from a variety of sources including the media (85%), class (67%), friends (59%), family (58%), and health care visits (25%). Unfortunately, only 18% sought information about environmental issues from nurses. Many students (67%) stated they would like to learn more about the effects of toxic exposures from personal care products.
Discussion
This study revealed that 69% of female student respondents used 11 cosmetic products per day, and 55% of these students used 12 products daily with several reapplied or repeated more than twice over 24 hours. These data support the 2004 Environmental Working Group (EWG) study, which reported women use on average 12 personal care products per day exposing them to an average of 168 chemicals from daily use of cosmetics and personal care items alone (EWG, 2012). The reapplication of several products increases health risks that could affect personal and reproductive health. Endocrine-disrupting chemicals (EDC) such as phthalates, found in 72% of cosmetic products that contain plastics and fragrances, are suggested to affect fetal development and fertility (Pak & McCauley, 2007). With more than half (55%) the students using scented products, most likely containing phthalates, students may increase exposure risks.
Another alarming finding is the frequent use of products in the moderate and high-use categories such as hand sanitizers and soaps, which may contain triclosan. Triclosan is an antimicrobial agent found in 76% of liquid soaps, in 29% of bar soaps, and in toothpastes, and has been known to disrupt thyroid balance (Dodson et al., 2012). The high-use (64%) of hand sanitizers may reflect the high percentage (75%) of nursing students who participated in the study (Figure 4).
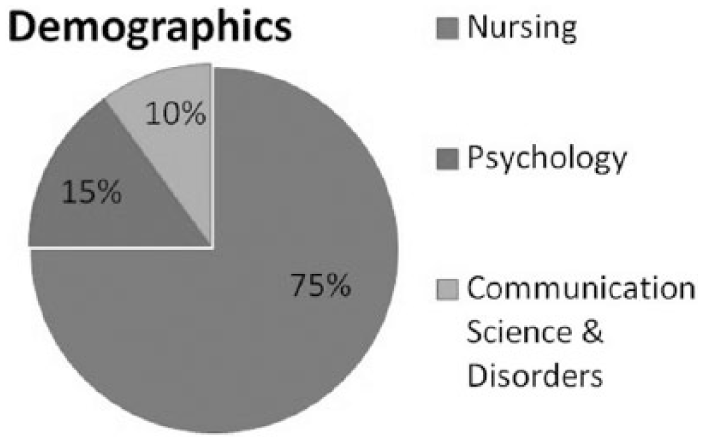
Percentage of nursing, psychology, and communication majors in study sample.
Students demonstrated some awareness and mixed knowledge about exposure risk to environmental toxins, but many seemed more concerned about global environmental issues such as water and air pollution and smoking than toxins in personal care products. Some knowledge deficits existed regarding the health effects of environmental toxins in personal care products and how these toxic effects could negatively affect both current health and preconception health. Because the majority of participants (67%) were interested in receiving more education on the topic, occupational health nurses have an opportunity to provide programs and services to these new employees.
Although data suggest that primary care physicians and nurse practitioners may not be significant sources of information about environmental health for this population, for many years, professional organizations have called on nurses and physicians to incorporate environmental health into their practices; because of their many patient encounters, they have opportunities to reduce health risk, promote health and prevent disease.
Limitations
A major limitation of this study was the use of a convenience sample of female college students recruited from a single, medium-size college campus. Due to the homogeneity of this population, results are less generalizable. In addition, the study sample included only female students from three particular undergraduate majors. Although this focused recruitment strategy saved time and effort, it may have biased the study because of missed data from women in other majors, women in the surrounding community, and diverse community populations. In addition, this survey tool was recently developed and has little reliability and validity data to support its use.
Future studies may overcome these limitations by recruiting a larger more diverse sample from a broader area. Data from the use of the survey tool in other studies may overcome questionable reliability and validity.
Significance to Nursing
Gaps exist in translating scientific findings to the public. The self-regulatory nature of the cosmetic industry and FDA-labeling requirements contribute to misinformation, confusion and knowledge deficits among consumers about the safety of commercial products. Occupational health nurses can play a significant role in improving public awareness and preconception care, translating scientific information to understandable recommendations for health-related behavior, and teaching clients how to best reduce exposures from frequently used products. By focusing on young women at college campuses and in the workplace, occupational health nurses have the opportunity to influence attitudes and behaviors about exposure risks, encourage healthy behaviors before pregnancy, and improve future health outcomes for women and children. Women of childbearing age should be encouraged to reduce personal exposures to a variety of substances by substituting safer products, using less “fragranced” products, and choosing to eliminate products with particular endocrine disrupting compounds.
Occupational and environmental health nurses are encouraged to reduce their own personal exposures at home and in the community, and to use this opportunity to incorporate environmental health education into their practice settings, programs of study, wellness programs and community events. Because of their knowledge and skills, along with their ideal practice setting, occupational and environmental health nurses can make a significant and unique contribution to both worker and community health by identifying individuals most susceptible to environmental hazards, providing worker education about environmental health hazards, recommending appropriate health promotion and protection strategies, and referring workers with environmentally related illnesses to appropriate occupational physicians. Other actions may include promoting environmentally preferable purchasing and toxic use reduction in the workplace, organizing green teams and leading efforts to promote environmental health literacy in the workplace and the community (Chalupka, 2005). Occupational health nurses can also use these opportunities to provide health promotion programs, and advocate for policies that protect workers, their families, and their communities.
Conclusion
This study offers occupational health nurses a broad understanding of college students’ knowledge about exposures to environmental toxins in personal care products during childbearing years. This research study demonstrates that the number of daily exposures to personal care products may be cumulative raising preconception health risks and contributing to chronic illnesses. Although connections have been made between exposures to several chemical ingredients and adverse health effects, more potentially understudied health consequences on the effects of low-dose recurrent exposures that could affect preconception health and contribute to chronic diseases may exist. Opportunities are available for occupational health nurses to raise awareness and educate this vulnerable population through environmental health literacy programs as well as conduct further research in this area. For occupational and environmental health nurses in particular, the effort of educating childbearing women to reduce exposure risks at home and at work could reduce chronic illnesses and absenteeism, lessen pregnancy complications, improve birth outcomes, and decrease employee health care costs.
Applying Research to Practice
Each year, occupational and environmental health nurses care for individual workers with a variety of work-related injuries and illnesses. Some of these occupational injuries and illnesses may be worsened by exposures to environmental toxins in their homes and communities. This study highlights the importance of focusing on the health of childbearing-age women. Occupational and environmental health nurses have the skills to assess and educate this vulnerable population, and conduct further research to better understand the complexity of exposure risks and the importance of improving overall worker health. Occupational and environmental health nurses can be instrumental in advocating for policy changes that promote health for childbearing women in the workforce.
Footnotes
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: I received financial support from Worcester State Foundation Student Research Grant to conduct this research project.
Bios
Lisa M. Chan MS, RN, RNC-OB is a maternity nurse at UMASS Memorial Medical Center in Worcester, MA and a 2014 graduate from Worcester State University’s Master of Science program in Community and Public Health Nursing. She is a 2013 Paul Ambrose Scholar, in which she created an Environmental Health Literacy Workshop for nurses and nursing students. Ms. Chan is currently working with the Alliance of Nurses for a Healthy Environment (ANHE) as the Massachusetts State Coordinator to improve communication with nurses about environmental health matters.
Stephanie M. Chalupka is Associate Dean for Nursing, Worcester State University, Worcester, MA and Visiting Scientist in the Department of Environmental Health, Environmental and Occupational Medicine and Epidemiology Program, Harvard School of Public Health, Boston, MA. Dr. Chalupka was inducted into the National Academies of Practice as a Distinguished Scholar in recognition of her research to reduce and prevent harmful environmental exposures and health risks to children and underserved, disproportionately impacted low income, minority, and tribal communities. Dr. Chalupka serves as an appointed member of the United States Environmental Protection Agency’s Children’s Health Protection Advisory Committee.
Roseann Barrett PhD, RN is the Assistant Dean for Nursing Research and Capstones and Nursing Graduate Program Director at Southern New Hampshire University. She holds a Bachelor’s Degree in nursing from Gwynedd - Mercy College, a Master’s Degree in nursing from Villanova University and a nursing doctorate from Boston College.
