Abstract
Chronic pain is prevalent in the United States, with impact on physical and psychological functioning as well as lost work productivity. Minority and lower socioeconomic populations have increased prevalence of chronic pain with less access to pain care, poorer outcomes, and higher risk of fatal opioid overdose. Acupuncture therapy is effective in treating chronic pain conditions including chronic low back pain, neck pain, shoulder pain, and knee pain from osteoarthritis. Acupuncture therapy, including group acupuncture, is feasible and effective, and specifically so for underserved and diverse populations at risk for health outcome disparities. Acupuncture therapy also encourages patient engagement and activation. As chronic pain improves, there is a natural progression to want and need to increase activity and movement recovery. Diverse movement approaches are important for improving range of motion, maintaining gains, strengthening, and promoting patient engagement and activation. Yoga therapy is an active therapy with proven benefit in musculoskeletal pain disorders and pain associated disability. The aim of this quasi-experimental pilot feasibility trial is to test the bundling of these 2 effective care options for chronic pain, to inform both the design for a larger randomized pragmatic effectiveness trial as well as implementation strategies across underserved settings.
Background/Literature Review
The prevalence of chronic pain problems in the general adult U.S. population is high; estimates have ranged from 10% to 40% in recent large surveys depending on the specific sample.1–4 There is a documented association between pain and impairment in physical and psychological functioning5,6 and lost work productivity. 7 Minority populations differ both in the prevalence and outcomes of chronic pain,2,8–11 wherein race/ethnicity and socioeconomic factors influence access to pain care.10,12–14 Opioids continue to be used for chronic pain with opioid addiction, diversion, and deaths remaining an ongoing epidemic in the U.S. 15 Although opioid overdose deaths began to decrease slightly in 2018, 16 they rose to an all-time high in 201917 and have spiked in the first 4 months of 2020. 18 Opioid fatalities are associated with lower socioeconomic status, 19 making access to nonpharmacologic pain care options a priority in underserved communities where the burden share of health-care costs is also greater—totaling one-third of household spending among lower income Americans. 20 Following Consolidated Standards of Reporting Trials (CONSORT) guidelines, this article will describe a study examining a novel approach to chronic pain which combines group acupuncture with yoga therapy delivered in the primary care setting to an underserved patient population. 21
Acupuncture therapy is effective in the treatment of chronic pain conditions,22–24 including chronic low back pain (cLBP),25–28 neck pain,28–30 shoulder pain, and knee pain from osteoarthritis.31–37 A large individual patient data meta-analysis (39 trials) of 20,827 patients with chronic pain found acupuncture to be significantly better than sham treatment or usual care, with only a 15% loss in treatment effect after 1 year.31,38 Patients with more severe pain at baseline improved more from acupuncture treatment than those with lower levels of pain, compared to sham or non-acupuncture controls. 39
Acupuncture therapy is supported or recommended as part of comprehensive pain care by the U.S. Agency for Healthcare Research and Quality (AHRQ), 40 the U.S. Food and Drug Administration (FDA) 41 and the Joint Commission (TJC).42,43 The National Institutes for Health (NIH) recognizes acupuncture for cLBP and knee OA pain. 44 The American Academy of Family Physicians (AAFP) endorsed the American College of Physicians (ACP) Guidelines recommending acupuncture as a first option for acute, subacute, and cLBP.45,46 A retrospective claims-based study found initial visits to chiropractors, physical therapists, or acupuncturists for new onset LBP substantially decreased early and long-term use of opioids. 47 Active military service members who accessed acupuncture for chronic pain had reduced risk of long-term adverse outcomes. 48
Acupuncture therapy is feasible and effective specifically in an underserved and diverse population at risk for health outcome disparities.49,50 However, cost and access to individual acupuncture treatment continues to pose a barrier to widespread implementation in this patient population. To address these issues, group acupuncture, which is less costly, is being offered in many settings across the U.S. Evidence indicates that acupuncture delivered in a group setting is beneficial for chronic pain.51,52
Yoga therapy is an emerging health-care profession 53 that demonstrates benefit for pain as well as pain-associated function 54 and disability 55 in musculoskeletal pain disorders including back, neck, osteoarthritis, rheumatoid arthritis, and fibromyalgia.56–59 Yoga has also been studied in minority community settings.60–62 Yoga was noninferior to physical therapy for cLBP in underserved patients. 61 The NIH recognizes the evidence and AHRQ and ACP recommend yoga as well as acupuncture for cLBP.40,44,46
Originating in ancient India, yoga has been adapted in the West where practice combines attention and meditation (dhyana), breathing (pranayama), and physical postures (asanas). 15 Chronic pain and related multimorbidities often preclude patients’ access to general yoga classes. Yoga therapy sessions differ from yoga classes in that they are delivered 1-on-1 or in small groups, including a thorough client intake, an individualized plan of care and ongoing assessment of progress. 63 Yoga therapy practitioners have additional specialized training (1000 h) in clinical conditions. Yoga therapy self-management techniques also can aid the chronic pain patient in accessing a public yoga class and modifying practices to their own needs.
Objective: Our Proposed Innovation
Our initial pilot study demonstrated the feasibility of acupuncture therapy for chronic pain given in a group setting with improvement in chronic pain and depression that persisted through the 24-week measure after the completion of an 8-week course of treatment. 51 That study was followed by a larger pragmatic trial focusing on chronic pain in an underserved population that was funded by the Patient Centered Outcomes Research Institute (PCORI). “Acupuncture Approaches to Decrease Disparities in Outcomes of Pain Treatment (AADDOPT-2),” compared 12 sessions of individual practitioner–patient acupuncture to group acupuncture (n = 706) 52 resulting in chronic pain reduction and improved function at 12 weeks in both arms. Qualitative studies to date show that acupuncture treatment in a group setting is highly acceptable to patients64,65 and that the group setting, community-based locations, and low cost of this model help eliminate some of the barriers to access to acupuncture. 66
We noted a natural progression for patients being treated with acupuncture therapy to begin to want and need to engage in more movement as their pain improved, and for acupuncturists to encourage activity and steps in movement recovery. Bundling acupuncture with an effective active therapy may be an optimal progression for recovery. The kind of movement is important both for strengthening and improving range of motion, maintaining gains, and promoting patient activation. As such, it is important to tailor movement to each patient’s needs which can happen in yoga therapy that is delivered to 1 to 3 individuals at a time and designed to accommodate differently-abled participants who would not normally be able to benefit from a general yoga class.
No previous study has evaluated the combination of acupuncture and yoga therapy in patients with chronic pain. Both therapies are effective for chronic pain; both have been shown to be feasible in underserved populations.52,61,67 Yoga and acupuncture have inherent similarities. Both provide patients with counsel on self-care, for example, breathing techniques to mitigate pain. Yoga not only offers specific movement strategies for pain management but also utilizes nonmovement practices that can impact pain processing, emotions associated with pain, and the impact of pain on daily life, for example, breathing, visualization techniques, and relaxation practices. Given the need for patient activation in the context of chronic pain, yoga therapy combined with acupuncture therapy may offer a significant synergy for chronic pain management and recovery. Comprehensive pain care strategies include not only implementation of effective modalities but also aim to maximize their benefit through optimal combinations and bundling of care.15,68–70
Access to nonpharmacologic pain care is minimal in low-resource medical centers; medical providers are seeking effective pain care options in light of the opioid crisis and welcome the ability to refer for effective nonpharmacologic care. Acupuncture therapy in our previous trial was highly acceptable to patient participants as well as medical providers who referred patients. Bundling these therapies at a participant’s primary care site and through PCP referral would likely provide a familiarity that facilitates attendance.
Research Design
Overview of Study
The goal of this project is to assess the feasibility of a low-cost, integrative intervention for chronic pain that can be replicated and implemented in safety net settings across the U.S. Over the course of 18 months, we will recruit at least 150 outpatients with chronic pain from the Institute for Family Health (IFH) Family Medicine sites and Montefiore Medical Group sites. Treatment will consist of 10 consecutive weekly group acupuncture therapy treatments. Yoga therapy treatments will start at Week 3 and will consist of 8 consecutive yoga therapy sessions that occur immediately following in a room adjacent to acupuncture therapy. Sessions are bundled to facilitate attendance that might be affected by 2 separate trips a week for participation. The primary outcome will be pain interference and pain intensity. Secondary outcomes will be pain-free days, depression, functional status, patient activation, and pain medication utilization. These will be used during the preintervention phase, during which patients are receiving usual care only, and compared to the period after patients receive the combined acupuncture and yoga sessions. Data will be collected for 10 days before acupuncture and yoga therapy, and up to 24 weeks following the end of treatment.
Study Design
The study will use a “multiple settings across baseline” quasi-experimental design. This is a repeated measures design, and each study participant will have multiple pre- and postmeasures. The multiple premeasurement points allow us to document and monitor what may be variable patterns of pain preintervention. This design optimizes feasibility and acceptability to patients and participating health centers while still generating meaningful outcome data. Specifically, we have not proposed randomization within the practices, rather allowing sites to offer the intervention to all patients with target diagnoses who meet eligibility criteria. To collect preacupuncture assessments of pain, we will include a 10-day intake run-in period prior to the initial acupuncture session that ensures treatment within a time frame that is consistent with typical time to appointments for many consultations.
Eligibility Criteria
We applied similar eligibility criteria to those used in the AADDOPT-2 trial. 52
Inclusion criteria
Patients 21 years of age or older.
Chronic pain (3 months or more in duration) due to a qualifying diagnosis of back pain, neck pain, and/or osteoarthritis.
Eligible patients must be receiving primary care at a participating IFH or Montefiore Medical Group site.
Participants must understand and be able to provide consent in English or Spanish.
Reliable contact phone numbers must be available to facilitate scheduling.
Availability for up to 10 weekly consecutive treatments.
Availability for follow-up data collection at 24 weeks.
Exclusion criteria
Receipt of acupuncture treatment or yoga instruction/therapy in the 6 months prior to recruitment.
Pregnancy.
Severe psychiatric problems as assessed by the study team (eg, chronic interpersonal problems, cognitive impairment, or active psychosis that is uncontrolled by medication that precludes the ability to provide informed consent or complete the survey instruments).
Setting
Participants will be recruited from IFH sites in Manhattan and the Bronx and 2 Montefiore Medical Group outpatient sites. Treatment groups will take place at Montefiore Medical Group sites the Family Health Center and Williamsbridge Family Practice Center. IFH patients will have the intervention at the Family Health Center of Harlem.
Usual Care and Intervention for Chronic Pain
Usual Care
During the 10-day usual care run-in period, patients will continue to receive clinical services (usual care) for the management of chronic pain as provided by primary care providers. Usual care may include referral for specialty consultation or physical therapy, or use of medication, and does not typically include acupuncture or yoga services. We anticipate that patients will vary substantially in the duration of pain and pain management.
Acupuncture Therapy Component
During the intervention phase, each participant will be given acupuncture therapy delivered in a group setting (seated) in 10 consecutive weekly treatments. Direct practitioner/patient session time will last 30 to 40 minutes. Session time may reach up to 60 minutes, to include time for the participants to arrive and settle in, as well as rest time after treatment. Sessions may be shortened to as little as 15 minutes if participants are late to their scheduled treatment time. Acupuncture treatment precedes the yoga therapy treatments, and the schedules are coordinated wherein lateness may truncate the acupuncture treatment time. Three consecutive weekly sessions of acupuncture will be given before yoga therapy is introduced. This will allow time for acupuncture to reduce chronic pain severity readying the participant to begin an active phase of movement and recovery provided by yoga therapy.
Yoga Therapy Component
At Week 2, a 20- to 25-minute yoga intake will be conducted to assess and inform a yoga plan of care. At Week 3, that plan of care will introduce yoga therapy following the acupuncture therapy. Weeks 3 through 10 will thus be combined interventions of group acupuncture followed by yoga therapy. Participants’ yoga therapy sessions will be 30 to 35 minutes, either individually or in groups of 2 or 3. To foster self-efficacy and sustained benefit, participants will be further directed to practice at home via simple instructions both verbally during the session and with handouts describing the practices in writing and images. Participants will be guided in the yoga philosophy of mindful awareness and non-harming in order to avoid exacerbation of symptoms and ensure optimal safety in home practice.
Acupuncture Therapy Manualization
Acupuncture therapy will be based on the pragmatic intervention manual used in our previous trial52,71 that allows for individualizing treatment from a predetermined set of options adaptable in a group acupuncture setting. Treatment is given primarily to the head, neck, back, and extremities. 71 Through provision of a manual, we have established a methodology for consistent and replicable treatment. Licensed acupuncturists with at least 3 years of practice experience will provide the acupuncture therapy treatment. Acupuncture treatment will consist of palpation, manual techniques: Tui na and/or Gua sha, needling body points and needling auricular acupuncture points, adhesive application of ear seeds for extended auricular therapy. 71 Participants will remain clothed or covered during treatment, with areas of the body accessible by shifting loose clothing.
Yoga Therapy Manualization
A yoga therapy manualization process resulted in a consensus approach for chronic pain in an underserved multimorbid patient population. Yoga positions (asanas) from the low back pain trial
72
will be incorporated along with specific asanas used in trials for upper body/neck pain
73
and for knee OA pain.74,75 To balance the individualization of yoga practices that yoga therapy provides, along with the structure necessary for research study and replication, a list of practices most relevant to the clinical population were agreed on. Yoga therapists are free to choose from the selected practices within each category, beginning with breathing practices and adding new practices at each session as appropriate to the participants' readiness and ability. These included multiple options in the following categories:
Breathing Practices Strengthening Poses Mobilizing Poses Balancing Poses Relaxation Practices Lifestyle Practices
All practices may be modified to the individual, as is standard practice in yoga therapy, using yoga props (blocks, straps, pillows), chairs, the wall, or general pose variations. At the end of the study, we encourage participants to utilize the practices learned as part of self-management options on their own and in the context of accessing a public yoga class and modifying practices to their own needs.
Recruitment and Data Collection
Recruitment will be initiated when primary care providers at the IFH and Montefiore sites make referrals to the study team by paper referral or electronic medical record in-basket. Referring providers will obtain permission from the patient for a clinical research coordinator (CRC) to contact them. The CRC will confirm patient eligibility and consent orally over the phone to be reviewed and confirmed in person. During the 10-day run-in phase, the participant will be contacted to complete run-in 1 using the Brief Pain Inventory (BPI) short form. 76 Timing of data collection is depicted in Table 1.
Interview Content by Time Point.
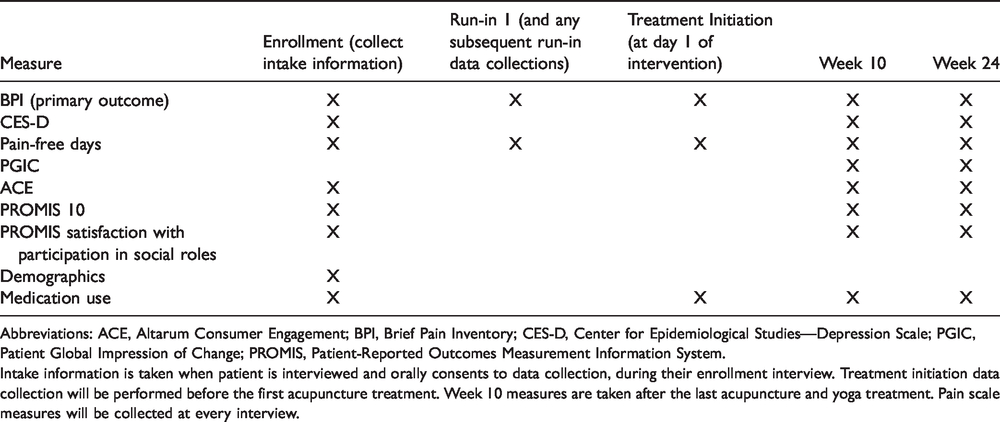
Abbreviations: ACE, Altarum Consumer Engagement; BPI, Brief Pain Inventory; CES-D, Center for Epidemiological Studies—Depression Scale; PGIC, Patient Global Impression of Change; PROMIS, Patient-Reported Outcomes Measurement Information System.
Intake information is taken when patient is interviewed and orally consents to data collection, during their enrollment interview. Treatment initiation data collection will be performed before the first acupuncture treatment. Week 10 measures are taken after the last acupuncture and yoga treatment. Pain scale measures will be collected at every interview.
Incentives
Participants will not receive an incentive to attend treatment sessions but will receive modest incentives to complete the research interviews. Participants will be provided $25 for completing the enrollment interview, $5 for completing the run-in 1 interview (and $5 for subsequent run-in interviews, if necessary), and $15 for completing the treatment initiation interview before the first intervention session. After the intervention, participants will be provided $25 and $30 for completing study interviews at Week 10 and Week 24, respectively.
Outcome Measures
Brief Pain Inventory: Short form (BPI) 76
The BPI is the primary outcome for the study. The BPI is a 9-item measure which that asks patients to indicate how their pain influences function: select aspects of their everyday life including mood, walking, sleep, and their ability to work over the past 24 hours, as well as the level and intensity of pain. This measure will be adapted for use by phone, modifying a question which asks participants to refer to a diagram of the body.
Pain-free days
This self-report measure has been used in previous pain research. 51 Patients will be asked to report the number of pain-free days in the previous 2 weeks. This measure will be used pre- and post-intervention.
Medication utilization
At enrollment and treatment initiation, participants will be asked to report their use of pain medications over the prior 1-week period. At the 10-week interview and 24-week follow-up interview, this information will be collected again, allowing us to analyze the impact of our intervention on analgesic use.
Analysis
Sample Size Calculations
Using an alpha of .05, 2-tailed, and a power of .80, and a clinically meaningful change defined as a 30% improvement on the BPI, we estimate that we will need approximately 134 patients treated through the GAPYOGA (Group Acupuncture Therapy With Yoga Therapy for Chronic Neck, Low Back, and Osteoarthritis Pain in Safety Net Setting for an Underserved Population) trial. As a feasibility study, we are powered only for the primary pain interference outcome but anticipate that our findings will allow us to estimate effect size for a future study for other outcomes. To account for attrition, we based our assessment on the AADDOPT-2 trial where we had complete data at 12 weeks for 84% of the participants. Therefore, for this trial, we plan to recruit 150 participants.
Quantitative Analysis
Prior to any univariate or multivariate analysis, all data will be reviewed to make sure values are in range and that outliers do not reflect typographical or data entry problems. The distributions of all continuous variables will be assessed, and transformations will be considered if the variables are heavily skewed. Baseline data, taken at during the initiation treatment interview, will be described using means, medians, or percentages depending on the variable.
Risks Related to the Intervention and Tracking of Adverse Events
Acupuncture therapy is safe with a “relative” risk that is low. Acupuncture needles are pre-sterilized for single-use only and will be properly discarded. Patients can sometimes feel elated, relaxed, introspective, or tired following acupuncture treatment. In rare instances, an acupuncture point may sting, itch, feel sore, or redden slightly; such symptoms typically resolve shortly after treatment. Similarly, in rare cases, an acupuncture point may bleed due to the nicking of a small blood vessel. In these cases, pressure is applied to the point and the area is cleaned. Rarely, a patient may experience light-headedness or fainting during treatment.
Application of ear seeds is painless. There may be a slight sensation of awareness at areas where Gua sha or Tui na have been applied. This awareness passes immediately or over the next day. Petechiae and ecchymosis from Gua sha also begin to fade immediately and completely after 2 to 4 days. There is a risk of alarm in family members or friends who might see “sha” petechiae and not understand what Gua sha is. Handouts on the Gua sha therapy can be provided so that the subject is able to reassure family members if necessary.
Risks with yoga are minimal. Reported harms associated with yoga for cLBP were mild to moderate,46,83self-limiting joint, and back pain comparable to physical therapy. 61 A systematic review and meta-analysis of randomized controlled trials found yoga to be as safe as usual care and exercise. 50 No association between yoga practice and joint problems was found in a large survey of women aged 62 to 67 years. 51
Serious adverse events are very unlikely given the known safety of acupuncture and yoga. Nevertheless, we will track serious (deaths, illnesses leading to hospitalization) and minor adverse events associated with acupuncture treatment and or yoga sessions. We will review these totals monthly. We anticipate that no serious events will occur during the course of this small study. The number of minor adverse events is expected to be very low.
Data Safety and Monitoring Plan
All electronic data (including all databases) will be protected using encryption software and stored on password protected PCs. The information from the study will be used only in scientific papers and reports that will not contain individual names or identifying information.
Summary
With a high prevalence of chronic pain and disparities in access to adequate pain care for underserved populations in safety net settings, we aim to assess the feasibility of combining 2 effective therapies, acupuncture therapy, and yoga therapy, to enhance the benefits of each for chronic pain. There is a call for research into effective therapy combinations, including investigations of dosage and frequency, to inform options for bundled care as part of comprehensive pain care strategies. A larger pragmatic effectiveness trial may be informed by the outcomes of this feasibility pilot in terms of integrating effective therapies as comprehensive pain care in community health setting.
Footnotes
Authors’ Note
Trial approved by Institution Review Boards (IRB): Albert Einstein College of Medicine, Montefiore Medical Center IRB #2018-9015, Ref: # 059397; Institute for Family Health IRB # 2297. Clinicaltrials.gov # NCT04296344. AN, BJA, MDK, and BJK were investigators on AADDOPT-2 trial and part of original GAPYOGA design team; DMM was a research acupuncturist for AADDOPT-2. RT, SM, EW, DMM, and MM joined team in transition to the pilot. SM worked with yoga team to develop yoga therapy manual. AN responsible for article draft. Each author reviewed and edited article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
