Abstract
Newly graduated nurses represent a crucial human resource for ensuring healthcare safety and quality. This cross-sectional study identified distinct profiles of work adaptation among 611 Chinese NGNs from 17 hospitals throughout nine provinces in China and explored how these profiles relate to key workplace and individual factors. Using latent profile analysis on data concerning work adaptation, we identified three distinct profiles: high adaptation, moderate adaptation and low adaptation. Analyses revealed that, compared to the low adaptation profile, higher levels of self-efficacy, recognized climate, and professional autonomy were significant factors associated with membership in both the moderate adaptation profile and high adaptation profile. Furthermore, male gender and adequate staffing were distinguishing factors specifically for the high adaptation profile. The findings indicate that a substantial majority of NGNs have significant potential to improve their work adaptation. Consequently, nursing managers should prioritize developing tailored, profile-specific interventions, particularly for nurses in the low and moderate adaptation groups, to foster a more successful transition into the workforce.
Introduction
The transition from nursing education to professional practice is a critical yet challenging period for newly graduated nurses (NGNs)—defined as those within their first year of clinical work (Innes & Calleja, 2018). This phase involves a complex adaptation process where NGNs must master necessary skills, internalize professional values, and integrate into their department’s culture and interpersonal networks (Frogeli et al., 2019; Morrison, 2002). Successful adaptation is crucial, as it is linked to increased job satisfaction and a stronger commitment to a long-term nursing career (Kramer et al., 2013; Ulupinar & Aydogan, 2021). Conversely, failure to adapt successfully can lead to burnout, high turnover, and ultimately, compromise patient safety and care quality(Powers et al., 2019; Rudman et al., 2014).
NGNs often face a constellation of challenges during this transition (E. Y. Kim, 2014). They frequently encounter a steep learning curve, dealing with excessive workloads while their practical skills and support systems are still developing (Sin et al., 2014; Walker et al., 2017). The psychological impact is significant, with many experiencing a lack of confidence, low self-esteem, and high levels of stress and exhaustion (Duchscher, 2009; Kumaran & Carney, 2014; Woo & Newman, 2020). Furthermore, adapting to new environments and navigating complex interpersonal relationships, sometimes including bullying or lateral violence, presents additional hurdles (Ellerton & Gregor, 2003; Rush et al., 2014). These factors collectively contribute to the notably high turnover rate observed among NGNs in their first year of practice (Rudman et al., 2014).
A substantial body of research highlights the nursing work environment as a pivotal factor influencing work outcomes. The Job Demands-Resources (JD-R) Model provides a valuable framework for understanding this relationship (Broetje et al., 2020). According to the JD-R model, every work environment comprises job demands (physical, social, or organizational aspects that require sustained effort and are associated with certain physiological and psychological costs) and job resources (aspects that reduce job demands, facilitate the achievement of work goals, and stimulate personal growth and development). In nursing work environment, key job resources include adequate staffing, professional autonomy, supportive managerial and interprofessional relationships, and opportunities for professional development (Lake et al., 2019).
Evidence underscores the importance of these resources for NGN adaptation. Inadequate staffing, a critical job demand, can overwhelm NGNs’ coping capacity and is linked to burnout and diminished care quality (Bhatti et al., 2018; Cho & Han, 2018; S. O. Kim & J. S. Kim, 2021). Conversely, job resources such as professional autonomy in task prioritization enhance job satisfaction and psychological empowerment (Allahbakhshian et al., 2016; Giles et al., 2017), leading to better work quality and patient outcomes (Boamah et al., 2018). A supportive climate, including positive nurse-physician relationships, facilitates organizational integration, reduces stress, and boosts job satisfaction (Göktepe et al., 2020; Shen et al., 2011). Moreover, institutions that invest in professional development tend to achieve higher levels of nurse performance (Sharma & Dhar, 2016).
Beyond the work environment, the psychological resources of NGNs are equally critical. Self-efficacy—an individual's confidence in their ability to handle challenges across diverse situations (Schwarzer & Born, 1997)—is a key personal resource. It correlates with mental health and directly influences behavior (Yu-Hui et al., 2019). For NGNs, higher self-efficacy is associated with improved job performance, greater job satisfaction, and higher quality of care (Kurniawan et al., 2019; Timothy et al., 2007). Another vital psychological factor is organizational identification, which refers to the psychological attachment an individual develops toward their organization. Strong organizational identification enhances morale, strengthens cohesion, and is correlated with increased job satisfaction and employee performance (Katrinli et al., 2010).
Although prior research has established the individual importance of environmental and psychological factors, the NGN population is not homogeneous. Variable-centered approaches may overlook meaningful subgroups with distinct adaptation patterns. Latent Profile Analysis (LPA), a person-centered method, addresses this by identifying latent subgroups based on response patterns across multiple indicators. Applying LPA to NGN adaptation enables a more nuanced understanding of differential adaptation pathways.
Based on the JD-R model and existing evidence, we hypothesize that:
(1) Distinct profiles of work adaptation exist among NGNs.
(2) These profiles will be differentially associated with key job resources (e.g., recognized climate, professional autonomy, staffing adequacy) and personal resources (self-efficacy, organizational identification).
(3) Specific demographic factors may also be associated with profile membership.
Method
Design
This study employed a cross-sectional design to investigate the work environment, self-efficacy, organizational identification, and work adaptation of NGNs. The differences in work environment, self-efficacy, and organizational identification between the latent profiles of work adaptation were tested. STROBE checklist (Supplemental Material S1) was cited in the manuscript.
Participants
From March to April 2022, 611 NGNs working at 17 hospitals throughout nine provinces in China were recruited by convenient sampling. The inclusion criteria included registered nurses who had worked in the hospital for the first time and had no more than 1 year of experience as volunteers to participate in this study. Nurses in non-clinical positions were excluded. Nylund-Gibson and Choi (Nylund-Gibson & Choi, 2018) recommend a minimum sample size of 300 participants for LPA. A total of 645 questionnaires were collected, out of which 34 were excluded due to disqualification, resulting in 611 valid responses (response rate: 94.7%). These responses were appropriately tested using LPA.
Measurements
Nursing Work Environment Scale
The work environment was assessed by the “Nursing Work Environment Scale”(Jing et al., 2016), an instrument developed within the Chinese cultural context to ensure contextual relevance and minimize cultural measurement bias. This scale employs a six-point Likert format (1 = strongly disagree to 6 = strongly agree). It originally contained 26 items measuring seven dimensions: Leadership and Management, Nurse-Physician Relationships, Career Development, Professional Autonomy, Material Reward, Staffing Adequacy, and Recognized Climate. Notably, this instrument incorporates three dimensions (Career Development, Material Reward, and Recognized Climate) that are not explicitly captured in the widely used Practice Work Environment Scale of the Nursing Work Index (PES-NWI), thereby providing a more nuanced assessment relevant to the Chinese hospital setting.
In the present study, the overall scale demonstrated excellent internal consistency, with a Cronbach’s α of .946 and a split-half reliability of .894. All subscales also exhibited good to excellent reliability. The Cronbach’s α values for the subscales ranged from .799 to .896. The corresponding split-half reliability coefficients ranged from .819 to .893. To enhance transparency, example items for key constructs are provided: the Recognized Climate dimension includes items such as “I am affirmed by patients and their families in my work” and “I feel my work is valuable”; the Professional Autonomy dimension includes items such as “I can independently decide on patient care and work-related issues.”
Self-efficacy
The Chinese version of the General Self-Efficacy Scale, developed by Schwarzer (Cheung & Sun, 1999), was used. A four-point Likert scale (1 = strongly disagree; 4 = strongly agree) was used; 10 items measured general self-efficacy. A higher score in this measurement indicates a more optimistic self-belief. The Cronbach’s α of this Scale was .87, and the split-half reliability was .82.
Organizational Identity
The measurement of organizational identification, developed by Ashforth and Mael (Cheung & Sun, 1999), was used. A five-point Likert scale (1 = strongly disagree; 5 = strongly agree) was used; six items measured general self-efficacy. A higher score in this measurement indicates a greater perceived unity and emotional attachment to an organization. The Cronbach's α of the Scale was 0.87.
Work Adaptation Questionnaire
Work adaptation was assessed using the “Work Adaptation Questionnaire”(Lei, n.d.), which a Chinese scholar developed. Since this study would be conducted in a Chinese hospital, we chose a scale developed in a Chinese context to reduce cultural differences. A 4-point Likert scale (1 = strongly disagreed; 4 = strongly agreed) was used. It includes 16 items and four dimensions: task mastery, role clarity, interpersonal relationships, and cultural adaptation. The Cronbach’s α of the Scale was .806.
Demographics
Demographics included age, working time, gender, educational background, hospital rank, and departments.
Data Collection
A convenience sampling method was employed to facilitate participant recruitment across diverse geographic and institutional contexts. The study aimed to include hospitals from nine provinces to capture regional variation. Within each province, the sampling strategy sought to encompass variation in hospital rank by targeting an initial ratio of two tertiary hospitals to one secondary hospital for invitation. This ratio was intentional, as the work adaptation challenges for NGNs are often more pronounced in tertiary hospitals due to their higher workload complexity and patient acuity, making them a key setting for this investigation. Invitations were extended to 27 hospitals (18 tertiary hospitals and 9 secondary hospitals) based on this framework. Ultimately, 17 hospitals (12 tertiary hospitals and 5 secondary hospitals) agreed to participate and were included in the study.
Data were collected via an online questionnaire administered through the Star Questionnaire platform. The nursing directors of the participating hospitals, who agreed to cooperate after being introduced to the study’s aims, received a link to the online questionnaire and the informed consent form. They subsequently distributed these materials to all eligible NGNs within their institutions. Participation was entirely voluntary. Nurses who provided electronic informed consent proceeded to complete the self-reported questionnaires.
Data Analysis
LPA was conducted in M plus 8.3 to identify the unobserved profiles of work adaptation among NGNs (Hagenaars & Mccutcheon, 2002). LPA serves as an analytical framework for identifying homogeneous subgroups within heterogeneous populations. Profile determination incorporated conceptual coherence, minimum profile proportions, entropy values (greater than 0.8 indicating an acceptable classification), and comparative fit indices (AIC, BIC, and adjusted BIC, with lower values indicating a superior fit). Model selection involved likelihood ratio testing, comparing k-profile versus k-1 profile solutions, with significant p-values supporting the more complex model (Asparouhov & Muthén, 2014; Nylund et al., 2007). The lower the value of the information index, the better the fit. In terms of entropy, the larger the entropy value, the more accurate the classification. If the entropy was found to be about .8 or higher, the model was considered acceptable. The model comparison test verified the relative goodness of the model with k potential models and k−1 models. If the p-value is significant, the k potential models are supported. If the p-value is not significant, the k−1 latent profiles are supported (Nylund et al., 2007). Following this, a descriptive analysis of all variables was conducted using IBM SPSS Statistics version 20.0. Finally, multiple logistic regression analysis was used to examine the factors influencing each latent work adaptation profile. Statistical significance was taken as a two-sided p < .05.
Ethics
Institutional Review Board approval was obtained from Xiangya Nursing School, Central South University (approval No. E202236). This cross-sectional survey employed online questionnaires and it guaranteed voluntary participation without penalty to minimize participant risk. Electronic informed consent was secured through an opt-in process where participants reviewed information about this study (the aims, content, potential risks and benefits). Participants need to click “I agree to participate in this study” and sign the informed consent form before answering the questionnaire. To ensure participant privacy and data security throughout the online survey process, no personally identifiable information (e.g., name, IP address, employee ID) was collected. All data were stored on a secure, password-protected server, with access restricted exclusively to the principal investigators. The anonymity of the respondents and the confidentiality of their data were rigorously maintained at all stages of the study. For NGNs, the substantial benefits of generating evidence to improve institutional support systems and nursing practice outcomes decisively outweigh the minimal risks of transient psychological discomfort.
Quality Control
“Each IP address can only answer the questionnaire once and the questionnaire can be submitted after all are completed” was set in Star Questionnaire software. The unified guide language was used in the questionnaire to explain the filling requirements and points. The unqualified questionnaires were eliminated when the proportion of choosing the same option in three or more consecutive items was more than 80% or the answer time was less than 3 min. The requirements of statistical methods were strictly adhered to during the data analysis stage.
Results
General Information
A total of 611 participants’ data (81 men and 530 women) were collected. They had a mean age of 23 years and had worked for an average of 7.5 months. Moreover, 500 (81.8%) and 39 (6.4%) NGNs held bachelor’s degrees and master’s degrees, respectively. In addition, 131 (21.4%) and 149 (24.4%) worked in the surgical department and Internal department, respectively. There were 42 (6.9%) at outpatient clinics, and the same number worked in the operating room. 44(7.2%) and 68(11.1%) worked at emergency departments and ICU respectively. The average scores for self-efficacy and organizational identification were 26.41 and 22.48, respectively.
The Latent Profiles of Work Adaptation
The three-profile solution demonstrated an optimal fit, evidenced by lower AIC/BIC/SABIC values compared to two-profile alternatives and a high entropy value (>0.90). The non-significant LMR test for four-profile solutions confirmed the superiority of the three-profile model. The fit indices of each model are shown in Table 1. Profile 1 (32.1%, n = 196) exhibited uniformly low adaptation scores (Low Adaptation Profile), Profile 2 (53.8%, n = 329) demonstrated intermediate levels (Moderate Adaptation Profile), and Profile 3 (14.1%, n = 86) showed consistently high scores (High Adaptation Profile).
Goodness-of-Fit Statistics for 1 to 5 Profile Solutions.

Note. AIC = Akaike Information Criterion; BIC = Bayesian Information Criterion; SABIC = Sample-Size Adjusted Bayesian Information Criterion; LMRT = Lo-Mendell-Rubin Likelihood Ratio Test; BLRT = Bootstrap Likelihood Ratio Test.
Differences Between LPA Profiles
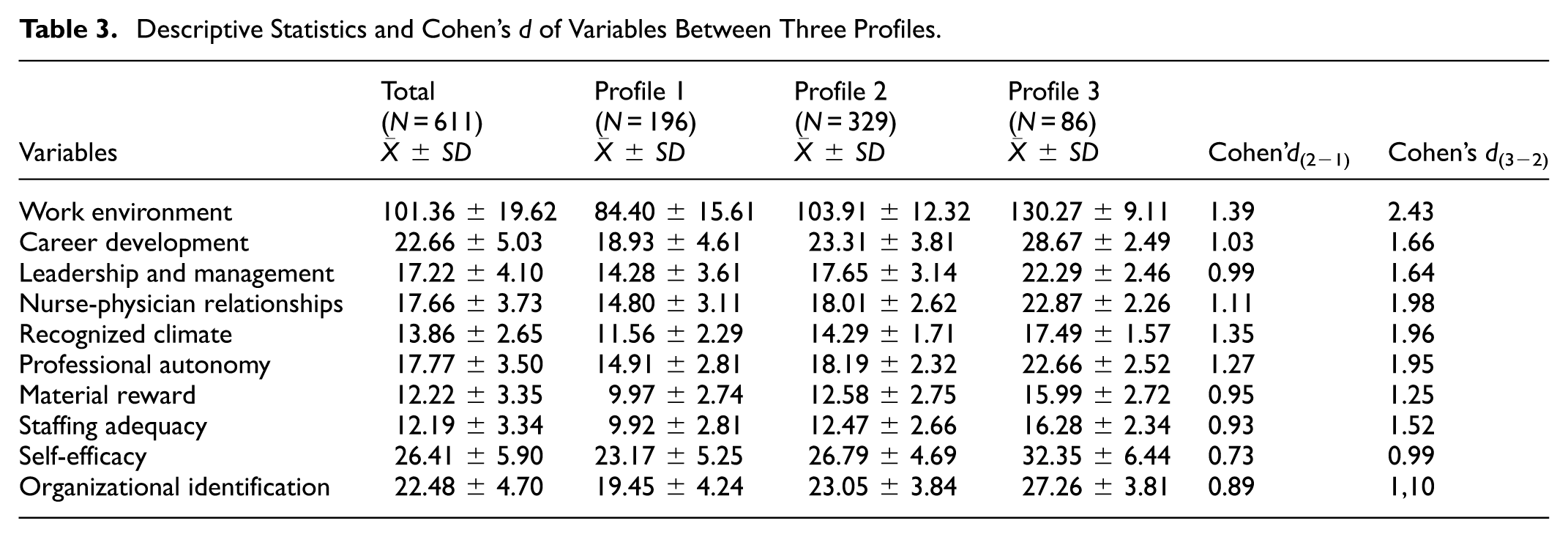
Tables 2 and 3 present the differences in variables between LPA profiles. The average age of NGNs in Profile 3 is older than in Profile 1. The average working time of NGNs in Profile 3 is longer than that in Profile 1. Additionally, in Profile 3, the average scores in the dimensions of work environment, self-efficacy, and organizational identity were the highest, whereas in Profile 1, they were the lowest.
Descriptive Statistics of Demographic Variables and Their Differences Between Three Profiles.

Descriptive Statistics and Cohen’s d of Variables Between Three Profiles.
Influencing Factors of NGNs’ Work Adaptation
Multivariate logistic regression analysis (Table 4) was performed to identify factors associated with profile membership, using Profile 1 (Low Adaptation) as the reference. Male NGNs were significantly more likely to belong to the high adaptation profile (Profile 3) than female NGNs (OR = 8.926, p = .008). Several dimensions of the work environment significantly predicted profile membership: a more favorable recognized climate increased the likelihood of belonging to both Profile 2 (OR = 1.687, p < .001) and Profile 3 (OR = 4.121, p < .001). Similarly, greater professional autonomy was associated with higher odds of membership in Profile 2 (OR = 1.306, p = .001) and Profile 3 (OR = 1.857, p = .001). Adequate staffing was a significant predictor for membership in Profile 3 (OR = 1.709, p = .001). In contrast, material reward did not demonstrate a statistically significant association with profile membership in this model. Higher self-efficacy levels increased the odds of belonging to Profile 2 (OR = 1.064, p = .027) and Profile 3 (OR = 1.130, p = .038). And higher organizational identification was associated with increased likelihood of membership in Profile 2 (OR = 1.096, p = .011).
Multinomial Logistic Regression Predicting Work Adaptation Using Profile 1 as Reference.

Discussion
This study represents the first application of LPA to examine work adaptation typologies among NGNs in China. We identified three distinct profiles: high adaptation, moderate adaptation and low adaptation, revealing meaningful heterogeneity in how NGNs experience the transition to practice. Approximately half of the sample was classified into the moderate adaptation group, while 32.1% (n = 196) fell into the low adaptation group. This distribution suggests that a substantial proportion of NGNs possess significant potential for improved adaptation with targeted support.
A notable and somewhat unexpected finding was that male NGNs were significantly more likely to belong to the high adaptation profile. This contrasts with traditional stereotypes suggesting women are naturally better suited to nursing. This finding may be partially explained by emerging evidence indicating certain advantages for men within the nursing profession. Studies suggest that male nurses often demonstrate greater confidence in their leadership capabilities and perceive themselves as more independent in clinical decision-making and productive compared to their female counterparts (Hoffart et al., 2019). Furthermore, men may be disproportionately drawn to and excel in high-acuity nursing specialties like intensive care and emergency departments, which demand advanced technical skills, quick decision-making, and physical strength (Shah et al., 2017).
Within the framework of JD-R model, factors such as recognized climate, professional autonomy, and adequate staffing function as critical job resources. These resources buffer work-related stressors and foster personal growth, thereby facilitating successful adaptation. The non-significant finding for material reward suggests that, for NGNs in their first year, intrinsic psychosocial resources like recognition and autonomy may be more salient motivators for adaptation than extrinsic financial rewards at this career stage. This aligns with previous studies indicating that professional acknowledgment can be a more powerful retention factor than salary for early-career nurses (Hehman et al., 2025).
Recognized climate emerged as a significant predictor of adaptation. Positive feedback and acknowledgment reinforce self-worth and encourage learning behaviors, thereby supporting professional growth. Conversely, NGNs frequently encounter criticism, belittlement, or unrealistic expectations from supervisors or colleagues which can impair clinical confidence and increase turnover intention (Gazaway et al., 2016; Henderson et al., 2015).
Professional autonomy, defined as involvement in decision-making related to patient care (Varjus et al., 2011), empowers NGNs to exercise initiative and maintain motivation, fostering consistent progress and adaptive competence. Enhancing nurses’ participation in hospital affairs has been linked to increased autonomy, job satisfaction, and reduced turnover intention (Al Sabei et al., 2020). Conversely, authoritarian leadership, ambiguous protocols, and restricted practice control can undermine autonomy (Allahbakhshian et al., 2016). Autonomy is strengthened when NGNs are permitted to schedule tasks and make clinical judgments based on their professional reasoning (Both-Nwabuwe et al., 2019).
Staffing adequacy has been widely established as a predictor of successful NGN adaptation. Nursing environments are inherently complex and stressful (Hinno et al., 2012), and staffing shortages exacerbate these demands, contributing to burnout, reduced productivity, and absenteeism (Whitehead & Myers, 2016). Conversely, improved nurse-to-patient ratios are associated with better outcomes, including reduced medication errors, mortality, and care omissions (Cimiotti et al., 2012; Griffiths et al., 2018). Thus, ensuring adequate staffing adequacy is essential.
Self-efficacy reflects an individual’s perceived capability to mobilize cognitive resources, motivation, and actions necessary to meet the demands of a task (Bandura, 1977). It shapes how NGNs approach challenges and problem-solving. As Wood and Bandura (Blake et al., 1989) emphasized, self-efficacy is foundational to cognitive development and self-reliance. Higher self-efficacy enables NGNs to deploy their skills effectively and pursue more challenging goals (Caruso et al., 2016). Our findings confirm that self-efficacy is indispensable for successful transition during the first year of practice.
Organizational identification, the sense of belonging to an organization, fosters identity and commitment (Haslam et al., 2003). Research consistently links strong organizational identification with higher job satisfaction, motivation, and performance, as well as reduced turnover (Katrinli et al., 2010). The study has also illustrated that organizational identification plays a crucial role in promoting the adaptation of NGNs.
To translate these findings into practice, healthcare administrators should develop intervention programs tailored to each profile. For NGNs in Profile 1, interventions should go beyond enhancing self-efficacy and organizational identification. Structured mentorship programs that pair these NGNs with experienced preceptors can offer individualized psychosocial support and strengthen practical coping skills. Additionally, hospitals should invest strategically in cultivating an inclusive organizational climate, ensures professional autonomy through involvement in decision-making and maintains adequate staffing levels to optimize the work environment as a core job resource. For NGNs in Profile 2, managers should focus on rational staff allocation and gradually increasing task complexity in accordance with their growing competencies. By adopting a profile-specific approach, nursing leaders can more effectively support NGNs’ transition, promoting retention, well-being, and safe patient care.
Conclusion
This study identified three distinct work adaptation profiles (low adaptation, moderate adaptation and high adaptation) among a sample of 611 Chinese NGNs, utilizing Latent Profile Analysis. The findings underscore that a substantial proportion of NGNs exhibit moderate to low adaptation levels during their first year, highlighting a significant opportunity and need for targeted institutional support. Key environmental and psychological factors, including a recognized climate, professional autonomy, self-efficacy, and organizational identification, were significantly associated with membership in more adaptive profiles. Notably, factors such as staffing adequacy and gender demonstrated a more specific association with the high adaptation profile. However, the generalizability of these findings should be interpreted in light of the study's limitations, particularly the use of convenience sampling and its cross-sectional design. While the results provide valuable, profile-specific insights for designing interventions—such as creating supportive climates, ensuring adequate staffing, enhancing autonomy, and fostering self-efficacy—the inferred relationships warrant verification through future longitudinal studies employing more representative sampling methods. Despite these limitations, this study offers a foundational typology of NGN adaptation and empirically derived guidance for healthcare managers to develop tailored, evidence-based support strategies for different NGN subgroups.
Limitation
This study has several limitations that should be considered when interpreting the findings. First, the use of convenience sampling, while pragmatic for recruitment, resulted in a sample that may not be fully representative of the broader population of NGNs in China. Specifically, our sample had a relatively higher proportion of nurses who were female, held bachelor's degrees, and were employed in tertiary hospitals. This overrepresentation may limit the generalizability of our findings, particularly to male nurses, those with different educational backgrounds, and those working in secondary or primary care settings. Second, the reliance on self-reported data introduces the potential for common method bias, such as social desirability or recall bias. Third, as a cross-sectional study, it precludes any causal inferences about the relationships between the identified variables. Furthermore, the findings may be influenced by unmeasured confounders, such as regional healthcare policies, specific hospital cultures, or individual differences in emotional resilience, which were not captured in our model. The cultural context of Chinese work environments, which often emphasize collectivism, might also influence the dynamics of work adaptation in ways that differ from more individualistic cultures, a factor that warrants further cross-cultural investigation. Despite these limitations, this study provides valuable insights. Future research should aim to employ stratified random sampling to enhance representativeness. Longitudinal or intervention studies are strongly recommended to establish temporal precedence and causality. To build a more comprehensive model, incorporating additional variables such as emotional resilience, mentoring support, and specific dimensions of organizational culture would be highly beneficial. Finally, supplementing self-report measures with objective indicators or qualitative data could provide a more robust and multi-faceted understanding of NGN adaptation.
Supplemental Material
sj-docx-1-sgo-10.1177_21582440251410321 – Supplemental material for Work Environment, Self-Efficacy, and Organizational Identity Predict Work Adaptation in NGNs: A Latent Profile Analysis
Supplemental material, sj-docx-1-sgo-10.1177_21582440251410321 for Work Environment, Self-Efficacy, and Organizational Identity Predict Work Adaptation in NGNs: A Latent Profile Analysis by Saiyu Gao, Jingping Zhang and Yun Peng in SAGE Open
Footnotes
Acknowledgements
The authors thank all the nurses who participated in the surveys.
Ethical Considerations
Institutional Review Board approval was obtained from Xiangya Nursing School, Central South University (E202236). This cross-sectional survey employed anonymous online questionnaires to minimize participant risk, with no collection of personally identifiable information and guaranteed voluntary participation without penalty. For NGNs, the substantial benefits of generating evidence to improve institutional support systems and nursing practice outcomes decisively outweigh the minimal risks of transient psychological discomfort.
Consent to Participate
Electronic informed consent was secured through a opt-in process where participants reviewed study information (the aims, content, potential risks, benefits, and privacy protection about this study), clicked “I agree to participate in this study” and signed the informed consent form before questionnaire access. Written informed consent to participate was obtained.
Author Contributions
Saiyu Gao: Conceptualization, Methodology, Data collection, Data analysis and interpretation, Writing - Original Draft, Visualization; Jingping Zhang: Critical revision of the article, Project administration; Yun Peng: Critical revision of the article, Visualization.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data sharing not applicable to this article as no datasets were generated or analyzed during the current study.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
