Abstract
In the context of the Corona Virus Disease 2019 (COVID-19) pandemic, medical staff have experienced traumatic stress events. Research on post-traumatic growth (PTG) was limited. We aimed to assess the relationship between perceived social support and PTG among medical staff 3 weeks after the policy opening of COVID-19 pandemic in Nanjing, China and explore the mediating roles of deliberate rumination. A multicenter study including a total of 842 medical staff was conducted at two general hospitals from December 10, 2022, to December 25, 2022, in Nanjing, China. SPSS was used for statistical description and univariate analysis, and AMOS was used for structural equation modeling (SEM) to analyze the medicating effect of deliberate social support on PTG. In the SEM, the total effect of perceived social support on PTG was significant (β = .332, 95% CI [0.259, 0.408], p < .001). In addition, deliberate rumination played a mediating role between perceived social support and PTG, and the indirect effect of deliberate rumination between perceived social support and PTG was −.036 (95 % CI [−0.059, −0.018], p < .001). Perceived social support has significant direct and indirect effects on PTG. In the context of major public health emergencies, providing medical staff with more social support and guiding them to reflect positively could help medical staff achieve PTG after experiencing a traumatic event.
Introduction
The Corona Virus Disease 2019 (COVID-19) pandemic was first reported in Wuhan, China, in 2019. It spread rapidly around the world at an unprecedented rate of transmission and was the most serious, impactful, and widespread major public health emergency in nearly a century. In several past studies related to public health and mental health, the COVID-19 pandemic was considered a traumatic event that not only negatively impacted social and economic activities, but also medical staff was subjected to greater stress during the COVID-19 pandemic, such as infection of themselves or their families and more difficult working conditions (Liu et al., 2022; Song et al., 2020; H. Xiao et al., 2020). Subsequently, the adverse effects of the COVID-19 epidemic on the mental health among medical staff have gradually emerged (Walton et al., 2020). Evidence demonstrated that medical staff had high levels of anxiety, depression, and post-traumatic stress disorder (PTSD) among medical staff during the COVID-19 pandemic. To be specific, 44% and 78% of medical staff scored above the threshold for depression and anxiety, respectively (Islam et al., 2021; Repon et al., 2021). In addition, a cross-sectional study exhibited that a total of 27.7% of medical staff or public service workers had clinical or subclinical symptoms of PTSD (Johnson et al., 2020). However, with the depth of positive psychology, it has been argued that individuals experience positive and uplifting positive changes after they have encountered and contended with a traumatic event or situation, known as post-traumatic growth (PTG) (Calhoun et al., 2000). Therefore, conducting research on PTG among medical staff is essential to provide them with mental health intervention strategies.
PTG is the ability of an individual to mobilize resources to effectively cope with a traumatic event, enhance psychological stability, and achieve good physical and mental health through a deeper exploration of the strengths of the self after experiencing significant stress (Tedeschi & Calhoun, 1996). According to the PTG model, traumatic and distressing experiences also had the potential to change fundamental life values and worldview of individuals and prompted them to demonstrate positive growth, including reflections on life, personal strengths, new possibilities, relationships with others, and self-transformation (Tedeschi & Calhoun, 1996, 2004). The COVID-19 pandemic as a public health emergency could be considered a traumatic event closely related to medical staff. Previous studies have revealed that a total of 76.8% of medical staff at a tertiary care hospital in New York, USA, recognized moderate or higher PTG associated with COVID-19 pandemic (Feingold et al., 2022). In several other studies, it has been demonstrated that the COVID-19 pandemic also has a positive impact on medical staff, such as experiencing PTG (R. Chen et al., 2021). In addition, an epidemiological study among medical staff indicated that the scores of PTG would change over time (Yilmaz-Karaman et al., 2022). The concentrated outbreak of the COVID-19 pandemic and policy changes in government administration may also have an impact on mental health (Garcia-Prado et al., 2022; Serrano-Alarcon et al., 2022; Yao et al., 2022). As we all know, China has been adopting community-based dynamic control measures to achieve zero COVID-19 cases. With declining mortality and elevated herd immunity, China relaxed its COVID-19 pandemic control measures in December 2022, which led to a short-term surge in COVID-19 incidence, as well as complex psychological changes in individuals (Y. Xiao et al., 2023). Medical staff might face the complexities of infection, overload and psychological relaxation following the liberalization of the policy during this period, which may lead to higher or lower levels of PTG. Therefore, it is essential to monitor and explore in detail influencing factors and impact pathways of PTG among medical staff 3 weeks after the policy opening of COVID-19 pandemic.
Perceived social support is the subjective feeling of social support, the emotional experience and degree of satisfaction of an individual to be supported, respected, and understood in the society, including three dimensions: family support, friend support, and other support, which could be a potential resource to alleviate the psychological stress caused by traumatic events (Birkeland et al., 2021; Kaniasty & Norris, 2008; Norris & Kaniasty, 1996). Social support provides individuals who experiencing post-traumatic events the possibility to express negative emotions and receive help and facilitates the process of overcoming trauma and achieving growth (Harvey et al., 2004). According to the PTG model, perceived social support could help individuals experiencing trauma to see things from different perspectives and develop new patterns (Tedeschi & Calhoun, 2004). In recent years, several studies have revealed that perceived social support has a positive effect on PTG in populations such as college students and cancer patients, with higher levels of perceived social support associated with higher scores of PTG (J.-S. Kim, 2020; Y. Kim et al., 2021). However, in the more than 2 years of the COVID-19 pandemic, medical staff served as a highly representative group, studies confirming the relationship between perceived social support and PTG were limited. In addition, few studies have explored the mediating factors between perceived social support and PTG. Therefore, it is of great interest to further explore the mediating variables and pathways between perceived social support and PTG, specifically 3 weeks after the policy opening of COVID-19 pandemic.
Rumination is a cognitive processing process after an individual experiences a traumatic event, divided into two dimensions: intrusive rumination and deliberate rumination, the former referring to the uncontrollable recollection of trauma-related events, and the latter including active efforts to think about and re-examine the traumatic event (Cann et al., 2011). Research has shown that characteristics of the event, personal qualities, and cognitive processing are associated with PTG (Allen et al., 2022). Therefore, rumination has a crucial role in the process of PTG. Previous researchers have emphasized rumination as a core variable in the PTG model to promote PTG, and some studies have confirmed that individuals with higher levels of deliberate rumination tend to show PTG after experiencing a traumatic event, as the process of re-confrontation and reflection on past traumatic events might be positively reappraised and rewarding (Pan et al., 2022; Su & Chen, 2015; Tedeschi & Calhoun, 2004; Yon, 2015). In addition, in previous studies have revealed that deliberate rumination has a positive predictive effect on PTG (Choi & In, 2020; Huh et al., 2020). Moreover, in a study to investigate the level of rumination and its influencing factors during radiotherapy in nasopharyngeal cancer patients, it was found that negative coping, social support, literacy, and tumors stage were the main influencing factors of deliberate rumination, and the higher the level of social support, the higher the level of deliberate rumination (J. Chen et al., 2019). Since intrusive rumination and deliberate rumination may play different roles in PTG, and few previous studies have investigated the relationship between deliberate rumination and PTG among medical staff during the COVID-19 pandemic, in the present study we focused more on the mediating role of deliberate rumination in the relationship between perceived social support and PTG.
Given that the original study was still inadequate, we conducted this study in a special group of medical staff immediately 3 weeks after the policy opening of COVID-19 pandemic. In anticipation of gaining a deeper understanding of PTG and informing the development of mental health intervention strategies for medical staff. In addition, we proposed the following hypotheses: (1) perceived social support positively correlate with PTG; (2) rumination can mediate the relationship between perceived social support and PTG (Figure 1).

Research theoretical model.
Materials and Methods
Design and Participants
This multicenter cross-sectional design study was conducted 3 weeks after the policy opening of COVID-19 pandemic in Nanjing, China. All recruited participants were medical staff (including doctors, nurses, and other healthcare professionals) working in two general hospitals in Nanjing, China. The inclusion criteria were those who were at least 18 years old and had been engaged in clinical settings for at least 6 months during the COVID-19 pandemic. Medical staff who are not directly engaged in clinical patient treatment and care or are not permanent hospital staff were excluded, such as logistics staff or standardized training medical staff.
Measures
General Information
A general information questionnaire about the participants was developed through a literature review, including gender, type of occupation, department, occupational exposure, and lifestyle-related variables (exercise, smoking, and alcohol consumption).
Multidimensional Scale of Perceived Social Support (MSPSS)
The Chinese version of MPSS was used to assess the social support among medical staff, which have been validated in the Chinese population with good reliability and validity (Chou, 2000). The MSPSS was a 12 items scale which consisted of three dimensions of support from family, friends, and others. Each dimension comprised of four items rated on a 7-point Likert scale ranging from 0 (strongly disagree) to 6 (strongly agree), which total score was 0 to 84 (Zimet et al., 1990). A higher score represented a higher level of perceived social support. In addition, the three dimensions of the Chinese version of MPSS had good composite reliability and convergent validity (CR: .974 to .983, AVE: .903 to .934) and internal consistency (Cronbach’s α: .964 to .977).
Event-Related Rumination Inventory (ERRI)
The Chinese version of ERRI was used to survey the intrusive and deliberate rumination among medical staff after experiencing stressful events 3 weeks after the policy opening of COVID-19 pandemic (Cann et al., 2011). In the Chinese population, the reliability and validity of the Chinese version of the ERRI have been validated (Dong et al., 2013). The scale consisted of 20 items with a total score of 0 to 60 and contained two categories: intrusive rumination (10 items) and deliberate rumination (10 items). Each item was rated on a 4-point Likert scale ranging from 0 (almost never) to 3 (almost always). The sum of all items in two dimensions is the total ERRI score. A higher score indicated a higher level of rumination. According to the focus of this study, only the deliberate rumination dimensions was selected for this study. In present survey, AVE value for deliberate rumination dimensions is .803, while CR value is .976, Cronbach’s α value is .972.
Posttraumatic Growth Inventory (PTGI)
The Chinese version of PTGI was used to evaluate the PTG among medical staff (Tedeschi & Calhoun, 1996). The Chinese version of the scale was validated to have good reliability and validity in the Chinese population (Qin et al., 2021). The PTGI consisted of five dimensions with total 20 items: appreciation of life (six items), personal strength (three items), new possibilities (four items), relating to others (three items), and self-transformation (four items). A total score of PTGI was from 0 to 100 on a six-point Likert scale ranging from 0 (almost never) to 5 (almost always), with higher scores indicating higher levels of PTG. Moreover, in current study, the instrument showed sufficient reliability, convergent validity, and internal consistency demonstrated by acceptable values of composite reliability (CR: .930 to .965), and average variance extracted (AVE: .770 to .895), and Cronbach’s alpha values (Cronbach’s α: .897 to .956), respectively.
Data Collection
This study was conducted via an online survey platform (“SurveyStar,” Changsha Ranxing Science and Technology, Shanghai, China) from December 10, 2022, to December 25, 2022, in Nanjing, China. There were two phase of data collection. In the first phase, we selected two general hospitals through a simple random sampling principle in Nanjing, China. In the second phase, the researchers distributed online questionnaires to medical staff in two general hospitals through the medical office and nursing departments. To avoid duplicate questionnaires, each Internet Protocol Address was limited to fill out once. Furthermore, an intelligent logic check was set up in advance to identify incomplete questionnaires, which were checked again independently by two researchers and finally determined to be validly completed before being automatically entered into the data file by the software. Finally, a total of 842 medical staff validly completed the online questionnaire for present study.
Data Analysis
We conducted descriptive statistics and data analyses by using SPSS 26.0 (IBM, New York, NY, USA). We used the CR value, AVE value, and Cronbach’s alpha to evaluate the sufficient reliability, convergent validity, and internal consistency of the variables in present survey, and we used means ± standard deviations (SD) for continuous variables. Moreover, independent samples t-test and one-way ANOVA were used to compare the differences in score of perceived social support, rumination and PTG between categorical variables. Pearson correlation analysis was utilized for the preliminary analysis of correlations among continuous variables, including perceived social supports, rumination, and PTG. All statistics was considered significant at the level of p < .05 (two-sided).
We conducted structural equation modeling (SEM) by using AMOS 26.0 (IBM, New York, NY, USA) to further identify the mediating effect between perceived social support, rumination, and PTG using the maximum likelihood method. To estimate 95 % confidence intervals for direct and indirect effects, we used the bootstrapping procedure 5,000 resamples from the data (Preacher & Hayes, 2008). Indirect effects were considered significant when the 95% confidence interval does not contain zero. The following multiple fit indices were used to assess the model fit: the value of χ2/df < 3, comparative fit index (CFI > 0.90), incremental fit index (IFI > 0.90), goodness of fit index (GFI > 0.90), Tucker-Lewis index (TLI > 0.90), and the root mean square error of approximation (RMSEA < 0.08) (Hu & Bentler, 1999).
Ethical Statement
This study strictly followed the Declaration of Helsinki. This study obtained approval from the Research Ethics Committee of Jiangsu Provincial People’s Hospital, Nanjing, China. Participants in this survey were asked to read and sign an electronic informed consent form, which gave them the right to withdraw from the survey at any time without giving a reason before accessing the link to complete the questionnaire. Simultaneously, we ensured anonymity by randomly assigning participant numbers to each member of the medical staff.
Results
Demographics Characteristics and Descriptive Analysis
The general characteristics of medical staff and their difference analyses with the score of perceived social support, deliberate rumination and PTG were shown in Table 1. Among 842 medical staff, 80.8% of them were female, 75.4% of them were nurse, 23.3% of them were physician, and 4.4% of them had experienced COVID-19 occupational exposure. In addition, the average score of perceived social support was 58.51 (SD = 13.38), and the average score of deliberate rumination was 8.15 (SD = 7.38), and the average score of PTG was 60.56 (SD = 24.08). It’s essential to note that score of PTG was higher in those who exercised more frequently aerobically (p < .05). Moreover, differences in perceived social support were significant among medical staff by sex, department, smoke, drink, and aerobic exercise.
Demographic Characteristics of the Participants and Univariate Analysis for the Research Variables.

Note. M = mean; SD = standard deviation.
p < .05. **p < .01. ***p < .001.
Correlation Analysis Among Research Variables
The results of correlation analysis among perceived social support, rumination and PTG were represented in Table 2. The Pearson correlation analysis indicated that the correlations between perceived social support, deliberate rumination and PTG were significant. More specifically, perceived social support was significantly negatively correlated to deliberate rumination (r = −.144, p < .001), and significantly positively correlated to PTG (r = .305, p < .001). Deliberate rumination was significantly positively correlated to PTG (r = .185, p < .001).
The Pearson Correlations Between Perceived Social Support, Rumination, and Post-Traumatic Growth.

p < .001.
Mediation Effect Models
The SEM analysis results for deliberate rumination between perceived social support and PTG were illustrated in Figure 2 and Table 3. The direct effects were as follows: the results demonstrated that perceived social support had significant positive effect on PTG (β = .348 SE = 0.034, p < .001), and perceived social support had significant negative effect on deliberate rumination (β = −.145 SE = 0.036, p < .001), and deliberate rumination had significant positive effect on PTG (β = .236 SE = 0.031, p < .001). Much more interesting, in the perceived social support → deliberate rumination → PTG pathway, the indirect effect was −.036 (bias-corrected 95 % confidence interval [−0.059, −0.018], p < .001). Deliberate rumination played a mediating role between perceived social support and PTG. According to the model fit index, the result of SEM demonstrated that the model constructed had a good fit (χ2/df = 2.752, GFI = 0.986, TLI = 0.994, IFI = 0.996, CFI = 0.996, and RMSEA = 0.046).
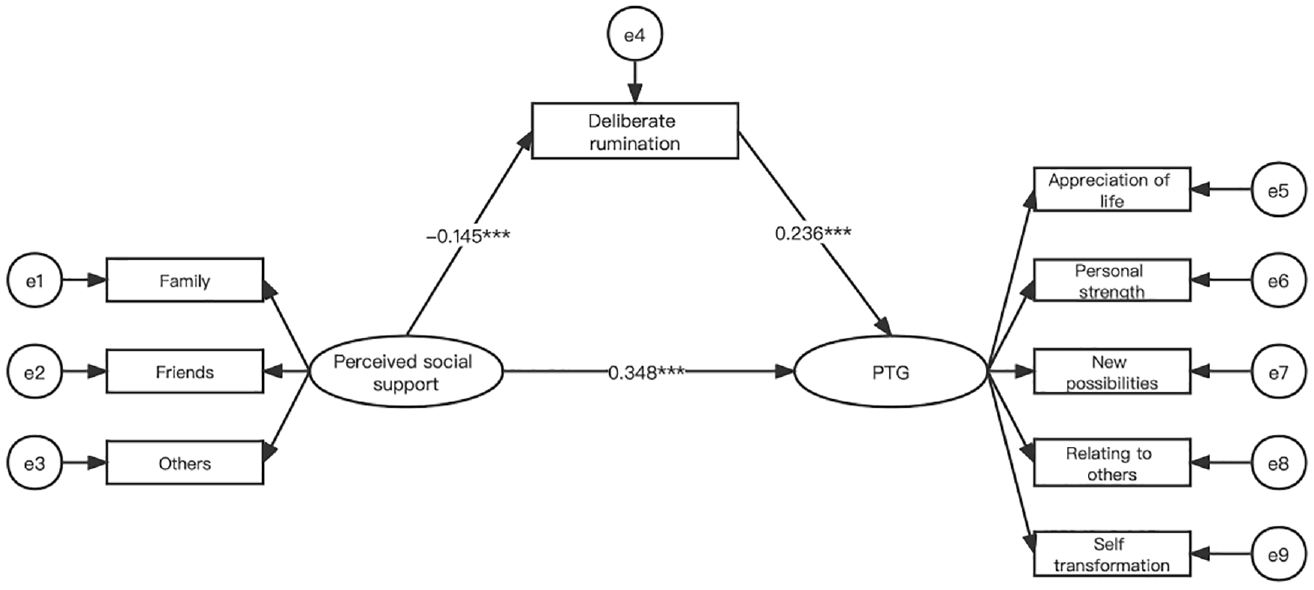
The mediating effect of deliberate rumination in the relationship between perceived social support and post-traumatic growth.
Total, Indirect, and Direct Effects of Perceived Social Support on Post-Traumatic Growth.

Discussion
It is worth pointing out that this study is the first study which investigated the relationships and meditated pathways between perceived social support and PTG among Chinese medical staff the 3 weeks after the policy opening of COVID-19 pandemic. According to above hypothesis, this study found that perceived social support positively associated with PTG. Simultaneously, the mediating relationship hypothesis was supported by our study, which revealed that perceived social support indirectly influenced PTG through the partial mediating effect of deliberate rumination. Although the World Health Organization (WHO) has declared the global emergency of the COVID-19 pandemic to be over, hospital administrations and managers need to pay continued attention to the mental health of medical staff, not only for their well-being but also for the quality of healthcare.
As predicted, this study revealed that the level of PTG among medical staff was significantly positively associated with perceived social support, which was consistent with previous research findings (Cai et al., 2021; Rahimi et al., 2016). This suggested that marvelous perceived social support, including emotional, organizational, and informational support, could give medical staff enough security to help them increase positive psychological behavior. Combined with the results of other studies, perceived social support was the exchange of mental, emotional, and material resources with others through social relationships to meet the needs of individual for coping with stressful events. As providers perceived higher levels of social support, medical staff had more support resources, which goes some way to alleviating the negative emotions associated with a major public health event, promoting emotional expression. This enables medical staff to approach things from a new perspective, which leads to new perceptions, views on life, etc., and ultimately to PTG (Cai et al., 2021). Therefore, any initiative that contributed to the promotion of social support might be helpful in improving the level of PTG.
Moreover, the current result also indicated that deliberate rumination could facilitate PTG among medical staff, which echoed the findings of previous studies (Choi & In, 2020). According to previous research, deliberate rumination refers to the conscious thought process in which individuals try to understand the cause and meaning of event, manifests as proactive and conscious responded to traumatic events and stressors, with greater attention to relevance and problem-solving skills (Wu et al., 2015). Since cognitive processing was an important part of an individual’s posttraumatic adjustment, deliberate rumination was the most significant indicator of cognitive processing. Such thoughtful and purposeful contemplation appeared to have a positive impact on PTG, helping medical staff make sense of traumatic events and engage in meaning seeking. This growth involved a great deal of cognitive effort and played an active role in the process (Hammer et al., 2019; Xu et al., 2021). Consequently, even if the COVID-19 pandemic is no longer a global emergency, actively guiding deliberate rumination among medical staff is conducive to promoting their post-traumatic psychological adjustment and the acquisition of PTG.
The most important implication of the current findings was that deliberate ruminative played a partially mediating role between perceived social support and PTG. The results suggested that higher levels of perceived social support were more conducive to PTG after a traumatic event for medical staff, in addition to influencing PTG through the mediating effect of deliberate rumination. Medical staff with lower levels of perceived social support might be less likely to engage in social activities and had more opportunities and possibilities to ruminate on the causes of the traumatic event, their subjective feelings, and their impact on the future, and therefore were more likely to experience growth such as increased self-empowerment and deeper life perceptions, thus promoting PTG.
Based on above discussion, this study findings provided the following insights for promoting PTG among medical staff. First, in the context of public health emergencies, increasing the level of perceived social support and guiding positive reflection among medical staff could contribute to PTG. Second, governments and organizations should actively respond by providing early detection and diagnosis of the mental health among medical staff, as well as timely assistance and long-term psychological intervention.
We acknowledge the several limitations should be noted in this study. First, the medical staff of two general hospitals were selected by simple random sampling for this study, and medical staff in the emergency and intensive care departments as the population most likely to be exposed to COVID-19 pandemic accounted for only 8.2% of the participants in present study. The generalizability of the results should be noted when interpreting them, and future studies could focus on the PTG of this more representative population. Second, gender, department, smoke, drink, and aerobic exercise as confounding factors should be further controlled for in future studies and explored for their moderating role in the mechanisms of influence on PTG among medical staff. In addition, this study was a cross-sectional study which could not explore in depth the dynamic evolutionary trajectory of PTG among medical staff in the context of the public health emergencies. Moreover, the time and place of this survey have certain particularity, which were closely related to management policies, etc. Therefore, the results of this study should be generalized to other samples with caution. Given these limitations, future multicenter, long-term longitudinal studies are necessary to further explore the influential mechanisms and evolutionary trajectories of PTG among medical staff, in order to identify mental health problems and provide psychological interventions in a timely manner to improve the well-being among medical staff, which would be very meaningful.
Despite these limitations, the present study also has many strengths worth noting. In terms of theoretical significance, this study links perceived social support, deliberate rumination and PTG, extending the literature on the influencing factors and influence pathways for PTG among Chinese medical staff in the context of major public health emergencies. Regarding practice, the relationship between perceived social support, deliberate rumination, and PTG helps to draw the attention of authorities and managers to the fact that medical staff are both rescuers and survivors in major public health emergencies, and the results of this study provide evidence for their provision of interventions.
Conclusion
In conclusion, this study demonstrated that perceived social support could promote PTG among medical staff and that deliberate rumination mediated this process 3 weeks after the policy opening of COVID-19 pandemic. Further, this study might provide an empirical basis for promoting PTG among medical staff who have experienced a traumatic event in the context of a major public health event. Enhancing perceived social support for medical staff and promoting positive reflection are conducive to PTG among medical staff.
Footnotes
Acknowledgements
We thank all staff members and all participants involved in this study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Data Availability Statement
The data supporting the findings of this study are available upon request from the corresponding author.
