Abstract
The incidence of breast cancer among females is increasing and early detection greatly improves patient prognosis and reduces mortality rates. This study aims at evaluating the awareness of these screening measures among adult females in Jordan. A questionnaire was administered to 400 adult women October to December 2018. The majority of women (64.5%) were within the age range 18 to 40 years. Almost all women had ever heard about breast cancer (99.50%) and 86.51% wanted to know more about it. Family history was the most frequently perceived risk factor for breast cancer (45.75%), with lack of awareness regarding other factors. Most participants were aware about breast self-examination (90.50%), but only half of them practiced it (52.75%). Regarding clinical breast examination, 76.0% of the participants have heard about it and a similar proportion recognized it as a method for early detection of breast cancer. However, only 26.33% were aware of the correct frequency of this examination. Screening mammography was acknowledged by 73.75% of participants but was performed by only 14.50%. Most of participants (70%) got their information about breast cancer from media, while only 8.34% got their information from the health centers. Awareness about breast cancer month in Jordan was significantly less among women with less than a university education, married women, and housewives (
Introduction
Cancer incidence and mortality are rapidly growing worldwide for complex reasons, with breast cancer being the most commonly diagnosed cancer and cause of cancer death among females (Bray et al., 2018). The worldwide incidence of breast cancer varies widely across the world, from 27 per 100,000 in Middle Africa and Asia to 92 per 100,000 in Northern America and western Europe (Sancho-Garnier & Colonna, 2019). Risks for breast cancer include female gender, increased age—until menopause-family history of breast cancer, personal history of breast conditions, radiation exposure, and obesity (Fahad Ullah, 2019). The disease leads breast mass, swollen breast with accompanying pain, noticeable changes in nipples. With advances disease stages, metastasis occurs leading to infiltration of adjacent tissues including the overlying skin or underlying muscles with or without locoregional lymph nodes involvement (Simos et al., 2014).
In Jordan, cancer is the second leading cause of death after cardiovascular disease (Abdel-Razeq et al., 2015). According to the 2015 Jordan Cancer Registry, 39.4% of the reported cancer cases in females are due to breast cancer, followed by colorectal and thyroid cancer, with an increase in number of incident cancer cases from 2,100 in 2006, to 2,888 in 2015 (Jordan Cancer Registry (JCR) (2015). The incidence of breast cancer among adult Jordanian females has also increased significantly from 38 to 48.2 per 100,000 people between 1996 and 2009 (Ismail et al., 2013). The median age of breast cancer diagnosis in Jordanian females was 50 years, with about 30.6% of cases occurring in women between 40 to 49 years (Ismail et al., 2013). In this respect, breast cancer represents a significant threat to many Jordanian females.
There has been limited research on breast cancer awareness, with some studies suggesting inadequate levels of awareness of breast cancer among female university students in Jordan. For example, a study was conducted among female students of Jordan, revealed that 83% of them had a poor level of awareness about breast cancer (Kan’an, 2018). Another study targeted female university students suggested limited awareness and inappropriate attitude to recommended BSE practices (Suleiman, 2014). The insufficient breast cancer awareness has a negative impact on the breast cancer screening attendance of women, which could negatively influence the early detection and prognosis of breast cancer (Binhussien & Ghoraba, 2018). Diagnosis at the earlier stages (I, II) of the disease is associated with higher survival rates and lower treatment costs as compared with diagnosis at the late stages (III, IV) of the disease (Wang, 2017). It is thus important to increase the level of breast cancer awareness and screening awareness among women. In this study, breast cancer awareness of disease screening methods was investigated among of adult females in Jordan.
Methods
In this descriptive cross-sectional study, 400 women were recruited using convenience sampling method between October and December 2018. The inclusion criteria were those females aged ≥18 years, with the only exclusion criteria being medical students or a health care provider as they were expected not to represent the general knowledge of women about breast cancer.
A five-sectioned questionnaire developed by the research team, and was based from previous studies (Akhigbe & Omuemu, 2009). The questionnaire was pilot tested to ensure quality and comprehend-ability. Pilot samples were omitted from the final analysis. Reliability coefficient for all item of the survey ranged from 0.64 to 0.81. As for validity, the study survey was content validated via review from experts in the field including senior researchers in the areas of medicine, pharmacology, and public health. The study instrument was adjusted as per comments from those experts. The overall content validity index was derived from the content validity indices of all questionnaire items using the averages of the items approach. Only items with individual content validity indices value of >79% were included in the final questionnaire. Additionally, to ensure content clarity and comprehension, subjects from the pilot sample were asked to provide comments about the way they understood each item of the survey.
The final study questionnaire consisted of five sections. (i) The socio-demographic information; (ii) general awareness of breast cancer including risk factors; (iii) awareness and practice of BSE; (iv) knowledge of clinical breast examination; and (v) awareness and practice of screening mammography.
The study participants were approached by the researchers at the general waiting area of the outpatient clinics of The University of Jordan Hospital (JUH). They were given a description of the study and were asked if they would be willing to participate in the study. Participants were assured that participation is voluntary and that their personal information will be anonymized to ensure confidentiality. If they agreed to participate in the study, participants were asked to read and sign the written informed consent. Then the questionnaire, which was self-administered was used as the data collection instrument. One of the researchers was present during questionnaire filling to answer any questions form the participants. The study questionnaire was distributed in Arabic language and was later carefully translated by the study lead researcher (MA) into English language for data entry and analysis. The English version of the study questionnaire was back translated into Arabic by the same researcher (MA) for accuracy. The filled study questionnaires were entered into a computer database for analysis.
Data Analysis
IBM Statistical Package for Social Sciences software (SPSS) for Windows, Version 22.0 (Armonk, NY: IBM Corp) was used for data processing and analysis. Participant demographics and questionnaire responses were described using frequency distribution. Tests of significance between groups were carried out using Pearson chi-square/Fisher’s exact test. A
Ethical Considerations
The protocol of this study was by the institutional review board of The University of Jordan Hospital (JUH). Written consent was obtained from all participants. Data confidentiality was ensured via anonymizing the questionnaire data, and via storing data of the study at a password protected hard drive.
Results
Socio-Demographic Information
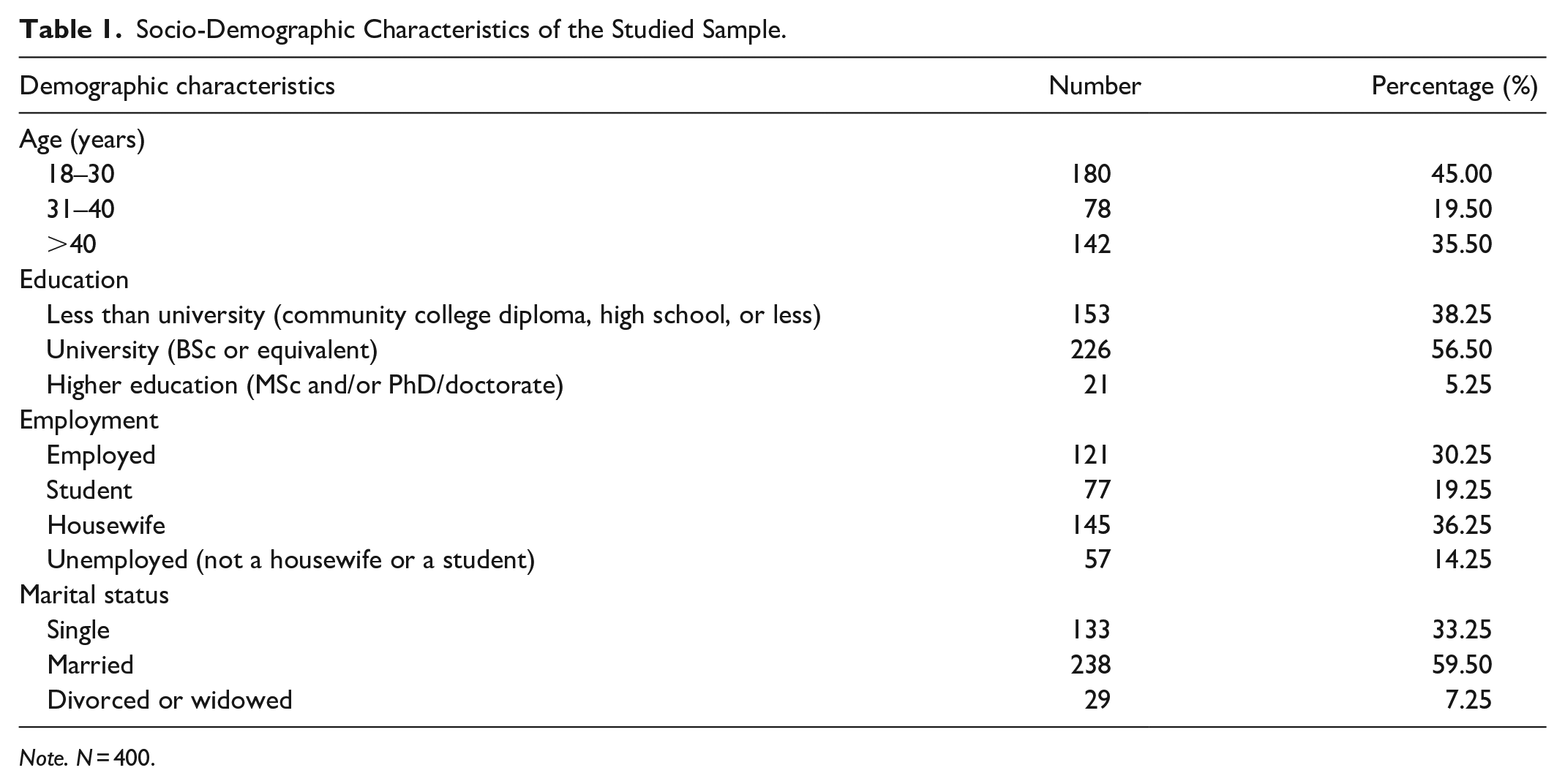
A total of 400 women completed and returned their questionnaires, the majority of which were between the ages of 18 and 40 (64.5%). The majority of participants were married (59.50%), and over half (56.50%) of all participants received a university level of education, while (5.25%) got a higher education level, that is, master and doctorate. Most of women (36.25%) were housewives, while working and studying women formed 30.25% and 19.25%, respectively (Table 1).
Socio-Demographic Characteristics of the Studied Sample.
General Awareness About Breast Cancer
Almost all the participants (99.50%) had heard about breast cancer, and 86.51% wanted to know more about it. Nearly half of participants (49.32%) thought that most breast masses were not malignant, while 35.21% were unsure. More than half of the participants (63.21%) thought that breast cancer was the most common cancer among Jordanian females. This had neither significant relation to different demographic characteristics nor to different sources of information, however, participants with a history of a friend or a relative having breast cancer (44.31%) showed significantly higher knowledge (
The most common perceived risk factor of breast cancer was a positive family history of breast cancer (45.75%), while 20.00% thought it was related to hormonal use. A small percentage (8.25%) attributed breast cancer to smoking and another 8.25% attributed it to radiotherapy. Very few linked ages at menarche or menopause and obesity to risk factors (Table 2).
Perceived Risk Factors for Breast Cancer Among Participants.

When asked whether they were aware of any comprehensive educational awareness program regarding breast cancer in Jordan, 45.18% agreed on that, while 32.81% disagreed. Half of participants (50%) heard about breast cancer awareness month in Jordan, while 35% never heard about that. Most participants (70%) got their information about breast cancer from media, including broadcast media (TV, radio), print media (newspapers, books, street ads, etc.), and social media. Only 11.51% chose friends and relatives as their main source of information, 9.52% from awareness lectures, and 8.34% got their knowledge from health centers. Awareness about breast cancer month in Jordan was significantly less among women receiving their information from their friends (
Awareness and Practice of Breast Self-Examination (BSE)
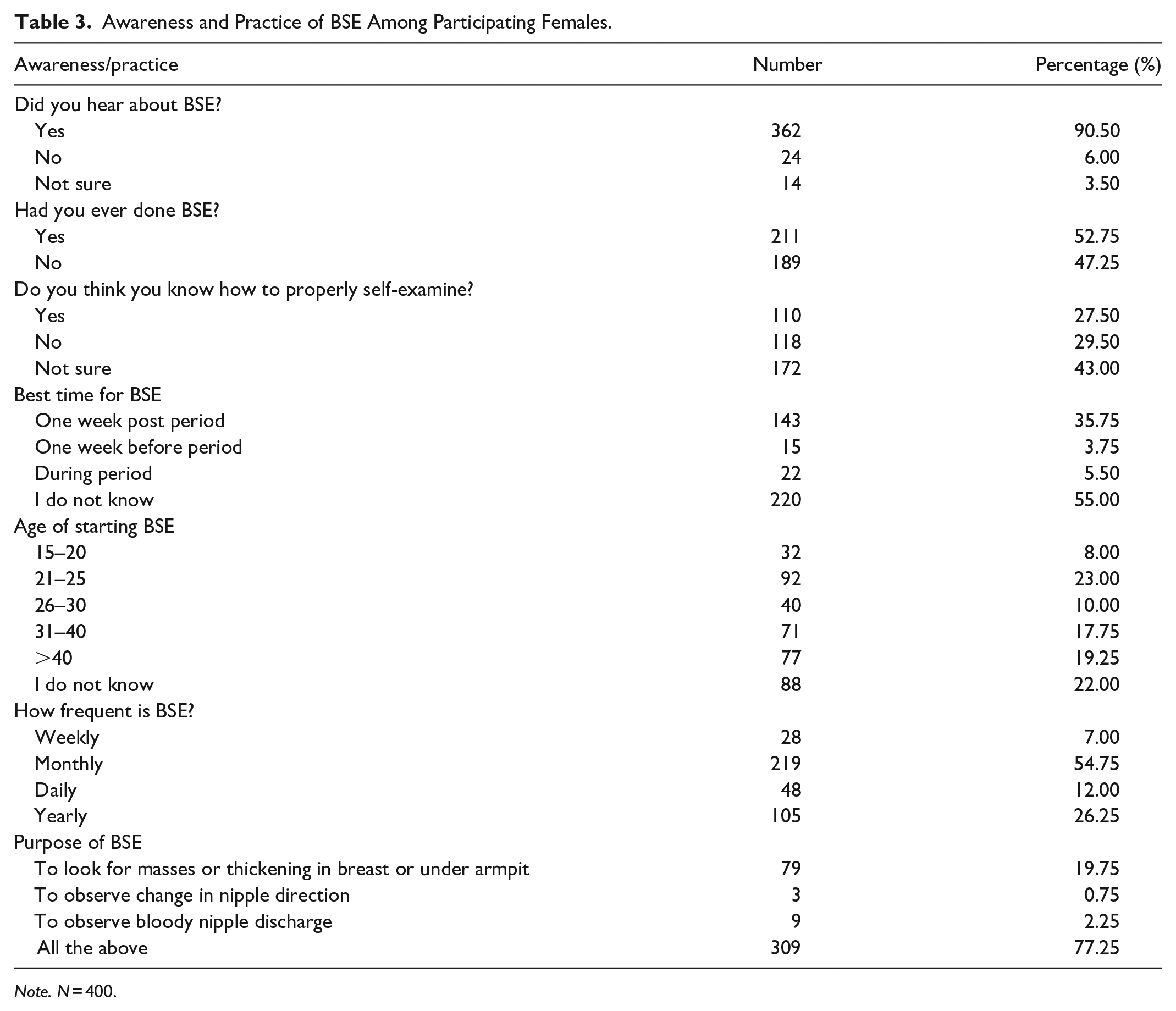
Most of the participants (90.50%) heard about BSE. Of these, two hundred and eleven women (52.75%) reported that they had performed BSE, but only (27.50%) believed that they aware on how to properly self-examine. The majority were not aware of the best time for BSE, but 54.75% said that BSE should be done monthly. Only 23.00% were aware of the proper age of starting BSE. When asked about the purpose of BSE, 77.25% chose all items regarding looking for masses, change in nipple direction and bloody nipple discharge (Table 3).
Awareness and Practice of BSE Among Participating Females.
There was a significant association between level of educational attainment and awareness about BSE, being lowest among those without a university education (
Awareness About Clinical Breast Examination (CBE)
Of the participants, 76.00% have heard about the CBE, and 78.11% of them were aware of CBE as a method for early detection of breast cancer. When asked about the frequency of performing a clinical breast examination, 26.33% said it should be done yearly, while 25.82% thought that it should be done if they noticed any change in the breast during the regular breast self-examination. However, almost 25.02% of the participants were unaware of the answer.
There was a significant association between the educational level and the awareness about clinical breast examination, as women with university education were more knowledgeable about CBE (
Awareness and Practice of Screening Mammography
In this study, it was found that the majority of participants heard about mammography as a method of screening for breast cancer (73.75%). Although 74.75% thought it was useful in early detection of breast cancer, only 14.50% underwent a mammogram examination, most of whom were ≥40 years. Of those who did not have a mammographic screening, 43.75% said that they were busy and a screening for breast cancer was not a priority, while 22.25% said that their ages were not appropriate to start screening mammography (Table 4). The results also revealed that 40.51% of the participants acknowledged the appropriate age to start doing mammography at age 40, but 25.83% were unaware of the starting age of screening. Likewise, 46.31% recognized that it should be done yearly while 30.84% were unaware of the frequency.
Awareness and Practice of Mammography Among the Participants.

Age had a significant effect on the participants’ knowledge about mammography (
Correlation Between Practice of Mammogram and the Sociodemographic Characteristics.

Discussion
In the current study, almost all the participants had heard about breast cancer, but most wanted to hear more. The majority thought that breast cancer was the most common cancer affecting Jordanian females, even though, almost half of them believed that most breast masses were not malignant. This contrasts with a study done in Pakistan, which revealed that 41.4% of Pakistani females considered breast cancer as a rare disease (Masood et al., 2016).
Many participants acknowledged family history, and hormonal use as possible predisposing risk factors of breast cancer. However, only a small minority recognized early menarche, late menopause, and obesity as potential risk factors. These results mirror a study done among Jordanian female university students which showed that low awareness about the risk factors (27.9%), but most of them (60.6%) cited family history as the most common risk factor (Alsaraireh & Darawad, 2018). Similar lack of awareness was also noticed among the university students in Angola, who were generally not aware about risk factors like hormonal therapy and obesity, but nevertheless, majority cited family history of breast cancer as the most known risk factor (Sambanje & Mafuvadze, 2012). Similar findings were also shown in a study from Malaysia, which showed insufficient awareness particularly among older women (Abdul Hadi et al., 2010). Better awareness of the risk factors was noticed among university female students in Oman, although the lowest level of awareness was regarding early menses, being identified by less than 50% of students (Aluko et al., 2014). The result of the current study, like other studies, suggested a need for better education and awareness regarding risk factors. For example, the most commonly cited risk factor in all these studies was a positive family history of breast cancer, which is a known risk factor for breast cancer. Yet, a significant proportion of breast cancer cases lack such a history. Thus, it is important to ensure that women with no known family history of breast cancer still participate in screening activities. Many studies, including ours, also showed low perception of obesity as a potential risk factor, although this can be modified by changing the lifestyle, and likely can help reducing the risk of this increasingly prevalent deadly disease.
In concurrence with the international campaign of breast cancer awareness month, held in October annually, a Jordanian campaign has also been taking place since 2007, accomplished by the Jordan Breast Cancer Program (JBCP), which included awareness material distributed across the media, street advertisements, and awareness lectures throughout the country. Despite that, the majority of the participants thought that awareness and educational programs about breast cancer were inadequate in Jordan. Furthermore, half of them only heard about the national awareness month, being significantly less among married women, housewives, and those with less than university education. This may be explained by the fact that housewives and married women are busy with their house and family affairs and thus, less likely to be engaged in educational and community activities.
The most commonly reported source of information about breast cancer was the media in its different forms (TV, radio, prints, and social media), with a minority receiving information from their friends and noticeably low percentage, from health centers. This was consistent with the findings of other studies (Legesse & Gedif, 2014; Manzour & Gamal Eldin, 2019).
Although most participants heard about BSE, only about a quarter of them were aware on how to properly self-examine, and more than half of them did not know the best time for BSE as well. This is consistent with other studies from Jordan (Alsaraireh & Darawad, 2018). Yet, lower awareness about BSE were reported from Malaysia and Saudi Arabia (Akhtari-Zavare et al., 2015; Ravichandran et al., 2011). However, very good awareness and practice of BSE was found among Omani university female students (Al Junaibi & Khan, 2011). In the current study, higher percentage of women with educational level of less than university were unaware about BSE compared to other educational groups with no influence of age, marital status, job, or having a known one with breast cancer. No influence of source of information was found on the awareness about BSE in the current study, which was opposite to the finding in the study of Ayed et al. and Noroozi et al., where mass media was the major source of information about BSE (Ayed, 2015; Noroozi & Tahmasebi, 2011). Anyhow, the American Cancer Society does not recommend women to perform BSE, but recommend them, nevertheless, to be more aware with the appearances and feelings of their breasts, and to report any change in them to their health care providers immediately.
Clinical breast examination is one of the screening methods used for breast cancer detection. This is because CBE could detect about 60% of breast cancer detected by mammography, as well as some breast cancer not detected by mammography (Provencher et al., 2016). Controversy regarding CBE in a screening context still exists. The American Cancer Society, the U.K. National Health Services, and the World Health Organization no longer recommend CBE screening, while U.S. National Comprehensive Cancer Network and the American College of Obstetricians and Gynecologists still adhere to it in their guidelines (American Cancer Society, 2021). The current study revealed that majority of the participants have ever heard about CBE and majority were aware of it as a method of early detection of breast cancer. Only a proportion of the participants answered correctly about the annual frequency of CBE, while another proportion believed that it should be done if they noticed any change during BSE. In contrast, a previous study from Jordan showed that 53% of them reported the annual frequency of CBE, and only 4.5% of women did it for pain or unusual feeling in their breasts (Othman et al., 2015). This difference in participant responses between both studies may be related to different age ranges and educational levels of the surveyed women. In the current study, better awareness about CBE was found among university educated participants with no differences regarding the rest of sociodemographic characteristics. Interestingly, no difference was found in a study from Iran regarding adherence to CBE between two classes with significant differences in socioeconomic and educational background (Kadivar et al., 2012).
More than two thirds of women in the current study were aware of screening mammography. Despite that, a minority have had a mammographic examination. Less than half of them acknowledged the appropriate starting age and frequency of screening mammography. Variable excuses for not doing mammography were cited, with majority claiming being busy and considering the exam a non-priority. However, the reported awareness and performance rate of mammography, in the current study are much higher than those of a study from Northern Ethiopia, which showed a knowledge about and performance of mammography in only 4.6% and 2.7% of participants respectively (Legesse & Gedif, 2014). In the current study, awareness about mammography was only significantly higher among older age group (≥40) and among university and higher educated women. On the other hand, performance of mammography was significantly higher among the older age group—the target population—and among the housewives but was lowest among single ones and those with university education. In a study done among young adult female university students in Egypt, most of study participants had correct information about mammography (Manzour & Gamal Eldin, 2019). Such variation among studies could be related to differences in the sampled population (university students vs. general population, and methods of sampling (convince vs. random sampling).
This study has some limitations. They include the use of convenience sampling method and the collection of the study sample only from one medical center. Additionally, the current study used a self-administered questionnaire, which has embedded issue of self-idealism. A more comprehensive theory-based study that utilizes random sampling is, thus, recommended.
Conclusion
This study showed a suboptimal awareness about breast CA among Jordanian females, although they had better overall awareness and practices of breast cancer screening compared to other communities. This suggests that breast CA educational programs in Jordan are inadequate to significantly promote women participation in the different screening activities including BSE, CBE, and screening mammography. This implicates that the relevant policy makers and breast cancer authorities to adopt more innovative methods and broad reaching strategies to disseminate more effective knowledge about this increasingly incident, young involving deadly disease. Health care providers are suggested to be more proactive in promoting patients’ awareness and are encouraged to spend more time delivering convincing information to their patients to get involved in efficient screening practices. Finally, the widespread exposure to social media, helped by the widespread availability of mobile phones and internet access, may be more effectively exploited to draw attention to an alarming health issue that affects relatively young ladies in Jordan and to promote more public awareness.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
Approval to this study was obtained from IRB of the University of Jordan.
Consent to Participate
Written consent was obtained from all participants.
Availability of Data and Material
Data is available via contacting the corresponding author.
