Abstract
This study examined the perceived risks of breast cancer (BC) and its influence on the BC screening behavior of 992 women residing in rural, urban, and semi-urban communities in five randomly selected local government areas (LGAs) in Ogun State, Nigeria. The article attempts to examine women’s perception of BC risk and how this may influence their behavioral disposition to breast screening. Cross-sectional survey and in-depth interviews were utilized to elicit quantitative and qualitative data from respondents. It was found that, although a positive association exists between risk perception of BC and BC screening attendance (β = .411), the association is not statistically significant:
Introduction
Breast cancer (BC) has been considered to be one of the most commonly diagnosed, and leading cause of cancer-related deaths among women globally (MacDonald, Sarna, Uman, Grant, & Weitzel, 2005; Norman & Brain, 2005; Phaswana-Mafuya & Peltzer, 2018; George, Allo, Amoo & Olonode, 2019). In the past, deaths among Nigerian women was often attributable to obstetrics complications and communicable diseases, whereas cancer-related death was less common (Ogunsiji, Kwok, & Chun Fan, 2017; Phaswana-Mafuya & Peltzer, 2018). Today, BC has become the commonest form of cancer morbidity and mortality among these women (Globocan 2002; Lawal, Murphy, Hogg, Irurhe, & Nightingale, 2015; Okobia & Aligbe, 2005).
Approximately 45% of BC diagnosis and 60% of BC deaths occurred in middle-to-low-income countries, and statistics for African countries such as Nigeria, Kenya, South Africa, and the rest revealed that BC has steadily surpassed cervical cancer as the most fatal cancer among women (Amoo, Ajayi, Samuel, Adekeye, & Odewale, 2017; Amoo et al., 2018; Jemal et al., 2011; Ogunsiji, Kwok, & Chun Fan, 2017; Parkin & Fernandez, 2006). In Nigeria at present, BC has been reported to have accounted for 56.6% of all cancer diagnosis, with about 70% of Nigerian women presenting late with advanced stage of the disease (Amoo et al., 2018; Lawal et al., 2015; Mandong, Madaki, & Manasseh, 2004; Ogunsiji et al., 2017). The estimated 5-year survival rate of BC is still less than 10% in Nigeria when compared with Western Europe and North America that have been experiencing over 70% survival rate (Amoo et al., 2017; Anyanwu, 2000; Lawal et al., 2015; Okobia & Osime, 2001).
The burden of BC in Nigeria is, however, unknown and this is largely due to missed diagnosis and inaccurate data from poorly funded cancer registries that produce mainly hospital-based data (Abdul-kareem, 2009; Akinkugbe, Lucas, Onyemelukwe, Yahaya, & Saka, 2010; Amoo et al., 2018). Nonetheless, existing data from different parts of the country revealed a growing increase in female cancers with BC taking the lead (Amoo et al., 2018; Mohammed, Ezino, Ochicha, Gwarzo, & Samaila, 2008; Okobia & Aligbe, 2005).
Women’s perception of risk or vulnerability to BC is also inaccurate either in the form of overestimation or underestimation (Black, Nease, & Tosteson, 1995; Brenes, Case, & Paskett, 2001; Buxton, Bottorff, Balneaves, & Richardson, 2003; Hopwood, 2000; Hopwood, Howell, Lalloo, & Evans, 2003; Hopwood, Shenton, Lalloo, Evans, & Howell, 2001; Iglehart et al 1998). It is also sometimes misguided, erroneous, and often shrouded in anxiety about cancer (Amoo et al., 2017; Hopwood, 2000).
Perceived risks, also known as perceived vulnerability, has been viewed as an individual’s recognition of the risks or the chances of developing a health condition, and it includes an appraisal of one’s susceptibility to illnesses in general (Rosenstock, Strecher, & Becker, 1994; Witte, 1992). There is limited information about what determines perceived risk, especially as it relates to most types of illness behavior. However, personal health risk perception has been viewed as an important determinant of specific health-related behavior (de Hoog, Stroebe, & John, 2005). Unfortunately, women, notably of African descent continue to overlook their chances of being at risk of BC. A lot of factors have been discovered to impact on women’s understanding of BC, such as their understanding of cancer as lethal, inadequate knowledge of BC screening (Pham & McPhee, 1992), and inadequate knowledge about the importance and practice of breast self-examination (BSE), clinical breast examination, and mammography as a form of early detection strategy (George et al., 2019; Rashidi & Rajaram, 2000).
In this article, the authors made an assumption that, low levels of perceived risk of developing BC among African women, especially among Nigerian women may be the reason for their poor attitude toward BC screening. Past studies have suggested that Black African women generally underprioritize their health thereby underestimating their risk of BC. They may also likely put the needs of their extended family members before their own, and when it comes to BC, many dismiss it as a Western disease just so to justify their underutilization of preventive services (Ogunsiji et al., 2017). In Ghana, for instance, the rate of mammography screening services usage was as low as 2% in 2012 (Opoku, Benwell, & Yarney, 2012). In a recent study conducted among South African women in 2018, the prevalence rate of mammography participation was 13.4% (Phaswana-Mafuya & Peltzer, 2018). This showed some appreciable increase when compared with the statistics from Ghana, albeit, these figures are low when compared with Western developed countries. In the case of Nigeria, studies have shown that an extremely low participation rate exist for BC screening (Lawal et al., 2015), and this could be largely attributable to low risk perception.
Study Objectives
This study seeks to examine women’s perception of BC risk, and how this may influence their behavioral disposition to screening.
Research Questions
Data and Methods
Study Design
This study employed a descriptive cross-sectional research design. The survey method was used to collect quantitative data through the use of the questionnaire, whereas the in-depth interview method was employed to gather qualitative data on the subject of interest.
The survey method was adopted for this study because of its high propensity for representativeness and its ability to extract data that are near to the exact attribute of the study population. The in-depth interview method was utilized as a complementary research method for eliciting in-depth information from selected health care providers and persons who have had a relation or friend that has ever been diagnosed with BC.
Study Location
The area under investigation with regard to this study is Ogun State. Ogun State, also known as the “Gateway State” is located in the South-western region and is one of the 36 states in the Federal Republic of Nigeria. Often ranked as the 24th largest state out of the 36 states in Nigeria in terms of land mass, Ogun State consists of three senatorial districts, nine Federal constituencies, 27 state constituencies, and 20 local government areas (LGAs; Oke, 2012).
Study Population
The population of interest constituted premenopausal and postmenopausal women aged 15 years to 69 years selected from over 880,970 regular households distributed unevenly across the 20 LGAs in Ogun state (National Population Commission [NPC], 2010).
For the survey, a sample of 1,000 women was drawn from five wards located in five randomly selected LGAs out of the 20 identified LGAs in Ogun State using the multistage sampling technique. The selected LGAs include Ado-Odo Ota, Abeokuta South, Sagamu, Obafemi Owode, and Ijebu Ode, whereas the wards visited in these LGAs include Sango Ota, Ake, Ogijo, Mowe, and Irewon. Opinions were sampled from women residing in rural, urban, and semiurban areas in these five wards. The inclusion criteria for selecting an area as urban, semiurban, or rural with regard to this study were simply based on size, population density, social distance, and economic activities in these areas.
The study area was first stratified into LGAs, and then into wards. Using the lottery method, one ward (each) was randomly selected across all five selected LGAs making a total of five wards. Out of the five selected wards, 32 streets were selected in all using the purposive sampling method, whereas the systematic sampling method was adopted in the selection of residential houses in selected streets. One household was selected in every fifth house to ensure that every woman was given an equal nonzero chance of being selected.
The final stage of the sampling process involved the selection of one female respondent per selected household.
The number of respondents sampled from each LGAs was proportional to the total female population size of each LGAs according to the data obtained from the NPC (2010; Table 1).
Female Population Distribution According to Selected LGAs.

The number of females sampled from each LGA was determined through the Taro Yamane’s formula for sample size calculation:

where
Therefore, to determine the sample size using Taro Yamane’s formula,

The suggested sample size (400) was increased by 150%, which gave a total of 1,000 as it is argued that, the larger a sample size, the more representative it is using the appropriate sampling technique.
Proportionate representation from each of the selected LGAs was ensured as follows:
Two in-depth interview sessions were also constituted in each ward of the five selected LGAs, making a total of 10 interview sessions. Two persons were selected from each ward using the purposive and snowball sampling method. The inclusion criteria for making this selection was based on the condition that, they are either a female health care provider (doctor/nurse) from any of the health care facilities in the ward, and/or a female who have had a close relation or friend diagnosed with BC.
Data Measurement
A 58-item, study-specific self-administered questionnaire was used to elicit quantitative data from the population of interest, and, in a situation where respondents could not read or write, the interviewer-administered method was adopted. A pretest was conducted on the research instrument before its final adoption. The test of reliability of the instrument for this study using standardized Cronbach’s alpha was obtained as (.778) > .70 threshold value. The validation of the reliability results of the instruments was carried out using ANOVA to test if there is a significant variation on how the respondents rated the items in the instrument. The result suggests that there is no variation on the rating of the items by respondents at
A total of 1,100 copies of questionnaire were administered on the study population with 992 returned and adjudged suitable for analysis. The attrition rate was 9.8%. The questionnaire administration was done by a team of research assistants who were trained before the commencement of the study and who could communicate fluently and effectively in both English and Yoruba languages depending on the preference of respondents. The questionnaire gathered information on sociodemographic characteristics of respondents, their general knowledge and awareness of BC, if they think they may be at risk of getting BC and if they will go for a voluntary BC mammography screening.
An in-depth interview guide was also utilized to elicit qualitative data to complement and support the survey method.
Data Analysis Procedures
Quantitative data analysis was done using the Statistical Package for the Social Sciences (SPSS) 16.0. Univariate analysis was conducted with the use of frequency tables to assess and describe the sociodemographic characteristics of respondents and other variables of interest, while the binary logistic regression (BLR) was used to estimate the log of likelihood
Qualitative data analysis was done by categorizing the recurrent or common themes identified in each of the participant’s responses using the “scissors and paste” approach (Green & Thorogood, 2004). Relevant striking statements were noted and were reported verbatim.
Results
Sociodemographic Profile of Respondents
A total of 992 women were surveyed across the five selected LGAs and wards: 30.8% from rural areas, 55.1% from urban areas, and 14.01% from semiurban areas. Wards that are seemingly urban were visited in Ado-odo Ota and Abeokuta South, those that have some rural characteristics were visited in Sagamu and Ijebu Ode, and those having semiurban features were targeted in Obafemi Owode LGA. The selection was done based on size, population density, social distance, and economic activities in these areas.
A larger percentage of the sampled population is of the Yoruba Ethnic group, their mean ages were as follows: 30.8% for rural, 31.8% for urban, and 27.89% for semiurban. Most of the respondents had some form of education with only 8.6% having no Western education. They are mostly single and married women, and majority belonged to the Christian faith (rural = 69.0%, urban = 67.8%, semiurban = 74.8%) as shown in Table 2.
Percentage Distribution of Respondents by Sociodemographic Characteristics.

BC Knowledge and Awareness
Almost all the respondents in the study area have heard about BC: rural = 90.55%, urban = 90.7%, semiurban = 83.5%, with only a fraction admitting otherwise. An appreciable number have also heard of BSE: 70.6% in the rural, 72.8% in urban, and 64.0% in semiurban. However, when asked about how to carry out the BSE procedure, just about half of the total respondents answered in the affirmative: rural = 56.2%, urban = 57.6%, and semiurban = 40.3%. This result revealed that, although a higher proportion of the study population have heard about BC and BSE, the knowledge about the performance of the BSE procedure is still low (Table 3).
Percentage Distribution of Respondent’s by Breast Cancer Knowledge and Awareness.

Perceived Risk of BC
Respondent’s perceived risk of BC was analyzed in this section. It was assumed that a woman’s perception of her risk of getting BC may prompt her into taking steps that may protect her from the disease.
Respondents’ opinion were sampled based on their knowledge of someone who have had BC, if they viewed BC as threat, if they ever worried about getting it, and if they think they may be at risk of getting BC.
Given the fatality of the disease, many respondents took offense when asked all of these questions and only a fraction hesitatingly answered the question. Analysis revealed that 29.4% of the total respondents from rural areas knew someone who have had BC; 30.2% knew from urban areas, and 24.5% knew from semiurban areas. In addition, of the total respondents sampled in the rural area, 37.3% viewed BC as threat, 37.3% also viewed it as threat in the urban area, and 25.2% saw BC as threat in the semiurban area.
For those respondents who claimed to have ever been worried about getting diagnosed with BC, 16.3% are from rural areas, 16.1% are from urban, and 11.5% are from the semiurban area. When asked if they think they could be at risk of being diagnosed with BC, respondents who answered in the affirmative from the rural area are 17.6%, 15.2% are from the urban area, and 12.2% are from the semiurban area. Going by all of these responses, it is clear that majority of the respondents do not perceive themselves at risk of BC and the perception of all the respondents about BC are nearly the same in spite of their locality. These findings may have a negative implication for the curtailment of the disease as low risk perception may reduce the likelihood of engaging in a preventive and protective action against the disease.
Perceived Risk of BC and Behavioral Disposition to Mammography Screening
The statistical tool in use here is the BLR. The BLR tested respondent’s behavioral disposition to BC screening attendance against some selected independent variables: at risk of getting BC, age, locality, religion, marital status, education, and occupation.
The hypothesis estimated the log of likelihood
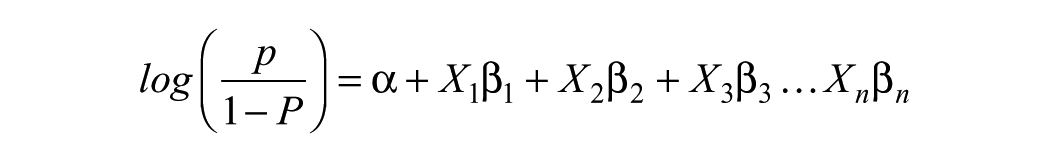
where β = coefficient.
Table 4 presents the behavioral disposition of respondents toward “breast cancer screening attendance,” and their “perceived risk of breast cancer.” As illustrated in the table, there is a positive association between respondents who think they can be at risk of BC and BC screening attendance (β = .411). That is, women who think they can be at risk of BC will be 1.508 times more likely to attend BC screening compared with women who think differently. The association is, however, not statistically significant,
Binary Logistic Regression Model Illustrating Relationship Between Respondent’s Perceived Risks of BC and Behavioral Disposition to BC Screening.

Looking at the age of respondents, a positive relationship can be observed between women aged 25 years and 39 years and screening attendance (β = .015). They will also be 1.015 times more likely to go for BC screening when compared with women <25 years. The relationship is not statistically significant,
In the same vein, locality showed a positive association in relation to screening attendance (β = .168 and .136), meaning women residing in semiurban and rural areas are 1.649 and 1.658 times more likely to go for BC screening when compared with those residing in urban areas, but the relationship is not significant at
As regards religion, there exists a positive relationship between screening attendance and Islamic and traditional religion (β = .313 and .079), meaning, women belonging to these categories of religion will be 1.368 and 1.082 times more likely to go for BC screening compared with Christians. The relationship is not significant at
With reference to marital status, a positive association could be detected between screening attendance and women belonging to all categories of marriage (0.893, 0.614, and 0.789), “except ‘separated’” (β = −.047). This is suggesting that, women belonging to these categories except “separated” will be 2.442, 1.848, and 2.201 times more likely to go for BC screening when compared with single women, whereas separated women will be 0.954 times less likely to go for BC screening. The relationship between married women and screening attendance is statistically significant at
A positive association was also noted in all the categories of education (β = .479, .371, and .122) implying that, they will all be 1.615, 1.450, and 1.885 times more likely to go for BC screening compared with women without a formal education, but there was no statistical significance observed in all the categories,
With respect to occupation, a negative relationship was detected in all categories of occupation as shown in Table 5, implying that women engaged in all the listed occupation will be 0.412, 0.576, 0.268, 0.412, and 0.451 times less likely to go for BC screening when compared with unemployed women. Statistical significance was also noted under farming,
Percentage Distribution of Respondents by Perceived Risk of BC.

The model summary indicated overall percentage of 73.2 indicating that the model is 73.2% sufficient to answer the research questions. However, the Cox and Snell
It, therefore, suffices to conclude that there is no enough statistical evidence to validate the assumption that women’s attitude toward BC screening is determined by their perception risk given the result of analysis as revealed in the model. Consequently, it can be said that women’s attitude to BC screening is not determined by their perception of BC risk.
Results from the in-depth interviews conducted to complement and support the survey method for this study, however, revealed that the women in the study area were excessively fatalistic in nature and were quick to arrogate their health problems to spiritual causal factors. It was also observed that they possessed deep-seated traditional health beliefs. Excerpts from the IDI sessions have been categorized under the following themes: perceived risk of developing BC and BC screening attendance.
Perceived Risk of Developing BC
Across the five selected LGAs and wards, low levels of BC risk perception were observed. Excerpts presented here represented the views of close family members and close acquaintances of a cancer patient.
Questions on whether BC is perceived as threat and whether interviewees think they could be at risk of developing the disease were asked and many of them were quick to respond with “God forbid!.” Below are some excerpts.
. . . I don’t see it as a threat to my health because I see it as the disease of the Egyptians and God has promised not to bring it near me so I cannot have it. (Close family member of a cancer patient from Obafemi Owode LGA). . . . God will not allow me to contract a disease that will have no cure. God should have mercy on us and should not kill us small small . . . (Close acquaintance of a BC patient from Sango Ota).
In the same vein, health care providers also presented their own perspective on some of their patient’s attitude toward BC risk perception: . . . women around here are more influenced by their religion. They belief breast cancer is an attack, they don’t know much about health, but they belief there are forces responsible for it. You see these people from polygamous homes, they will say it is one woman that is after them. They don’t normally belief that it is something medical. . . (Matron, State Hospital Ota, Ijebu Ode/ Female surgical ward)
BC Screening Attendance
With regard to BC screening attendance, below are excerpts from both close family members/acquaintances of a cancer patient and health care providers: . . . for me, I don’t think I can use my money to go and do breast cancer screening because I believe I cannot have it. But if there is a free screening I will go for it if the queue is not much. And for those that discover it I believe they will go spiritual. I remember a lady back in school, she began to show symptoms, she had lumps and she believed God for her healing and God healed her. . . . some people don’t even want to hear about breast cancer! They believe they cannot have it. Someone said it is a demon and a demon cannot reside in her body. . . (Close acquaintance of a cancer patient in Obafemi Owode) . . . last year we had one programme in this hospital, and cancer screening exercise was taken to different local governments in this Sagamu. And some of them came for removal of breast lumps. And the government paid for this screening exercise, but it’s their attitude towards it. Some of them have “I don’t care attitude” that, it doesn’t matter. Then, number two, their religious beliefs, some believe that once you have it you can go to church. And some prophets even use to deceive them by saying to them “don’t worry, it will melt.” Then, apart from church, some believe in
Discussion
To engage in a healthy lifestyle behavior, there is a need for a perception of personal risk or vulnerability, and to accurately measure risk, individuals should be able to feel susceptible to a particular threat and must also perceive the threat as severe. This will inform the actions they take to salvage or treat a health condition. This study on the contrary found that, perceptions of risk, although an important component of behavioral change paradigm, is not a sufficient enough variable that is capable of affecting on women’s behavior and disposition toward BC screening in the study areas. Considering the results from the IDI conducted to support the quantitative method for this study, issues surrounding cultural/traditional beliefs and religion stood out as major determinants of attitude toward BC screening. Other issues raised by interviewees include cost, time, and discouraging long queues at screening centers.
Several studies supported the findings from this study. In one study that examined beliefs and attitudes about BC and screening practices among Arab women living in Qatar, it was reported that many complex beliefs, values, and attitudes influences Arab women’s behavioral disposition toward BC (Donnelly et al., 2013). Cultural values, beliefs, and attitudes were seen as major determinants of perception of BC risk, and having a cancer diagnosis was often accompanied by social stigma. In some societies, a cancer diagnosis was seen as carrying a significant amount of stigma, myth, and taboos, while culture was also viewed as having a major influence on patients’ and communities’ perceptions of cancer risks (Daher, 2012; Kagawa-Singer, Dadia, Yu, & Surbone, 2010).
Donnelly et al. (2013) further found that BC screening among Arab women remained low in spite of the rising BC incidence and mortality rates. Some factors they identified as affecting negatively on Arab women’s disposition toward BC particularly BC screening include low perceived risk of cancer, preference for a female health professional, time, cost, lack of a physician’s recommendation, fear of the BC screening procedure, fear of finding cancer and embarrassment related to the BC screening procedure.
Opoku et al. (2012) have also linked the poor participation of African women in screening to cultural factors and fatalistic beliefs, and a study of African migrants in the United Kingdom by Jones et al. (2015) have revealed that African women migrants regard BC as a curse that was inflicted by an evil spirit and that any woman diagnosed with the disease must have done something bad to deserve it.
Other interesting findings from literature have also recounted how many women, particularly in sub-Saharan Africa often live in denial of their risk majorly because of fear of death and deformation from mastectomy and chemotherapy treatment. There are also reports of high patronage of quacks and traditional medical practitioners (Akinyemi & Isiugo-Abanihe, 2014), which makes women evade diagnosis and delay treatment (Clegg-Lamptey, Dakubo, & Attobra, 2009; Fregene & Newman, 2005; Mdondolo, de Villiers, & Ehlers, 2004).
Conclusion and Recommendations
The study concludes that the likelihood of going for BC screening among the women in the study area, rather than being determined by their perceived risks of BC are on the contrary influenced by traditional health beliefs and religious idiosyncrasies. Issues that bother around perceived risks of BC and its cancer screening are thus better understood from a sociocultural and spiritual perspectives rather than from psychosocial and analytical perspectives.
The sociocultural milieu and religious idiosyncrasies of Nigerian women may be considered when developing interventions to encourage mammography screening.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Approval was sought from the Covenant University Health Research Ethics Committee (CUHREC) of the University, and the informed consent of participants for both the survey and in-depth interviews were duly obtained. Participants were debriefed about the aim and objectives of the study before the data collection process commenced. Participants were also assured of privacy, anonymity, and confidentiality of information supplied.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The authors acknowledges Covenant University Center for Research, Innovation and Discovery (CUCRID) for their financial support.
