Abstract
Systematic reviews have provided some insight into the impact of interprofessional collaborative practice on patient outcomes. Despite strong interest in interprofessional collaborative practice, relatively little is known about its impact in primary care settings. This scoping literature review describes the essential elements of an interprofessional primary care practice and explores what is known about its impact on patient care including clinical, humanistic, and economic outcomes. We completed a review of the literature examining the breadth of knowledge related to interprofessional collaborative practice in primary care settings. A search was conducted to identify studies based on predefined criteria. A total of 51 studies met the criteria. A total of 27 studies reported a significantly positive clinical outcome with the interprofessional collaborative practice model, 27 studies reported no difference, and one study reported negative outcome in mortality. A total of 15 studies reported a significantly positive humanistic outcome. There was little to no difference in economic outcomes. This study provides new insights for future research that examines the impact of interprofessional primary care practice.
Keywords
Introduction
With growing demand for health care services and an aging population, management of chronic illness in primary care settings is an increasingly important aspect of health care delivery. Many models of primary care delivery have been proposed and most industrialized nations have adopted one or more of these models (Spenceley et al., 2015). The patient-centered medical home (PCMH) model has been proposed as one of the featured models in a reformed United States health care system. This model is patient-centered and physician-directed but also encourages a team approach to care for patients. Patient-centered care is defined as shared responsibility of patient care between the physician and the patient. However, physician-directed care is defined as a physician who coordinates the care for the patient and leads the medical team. The authors reported the patient-centered and physician-directed care to be more accessible, higher quality, more satisfying, and less costly than other models of care. The main feature of this system includes getting patients to the correct care location to be seen by the appropriate specialists in a timely manner. PCMH model has shown to decrease mortality, morbidity, emergency room utilization, hospitalization, and cost per patient (Epperly, 2011). In addition, the PCMH model using interprofessional team care has shown to increase patient and physician satisfaction with care as well as improve patient access and quality of care (Epperly, 2011).
The World Health Organization (WHO, 2010) defines interprofessional collaborative practice (ICP) as “when multiple health workers from different professional backgrounds work together with patients, families, carers, and communities to deliver the highest quality of care.” This model of care differs from other practices because it requires teamwork and patient involvement compared with other models where usually one provider takes leadership working solo (e.g., primary care physician, nurse practitioner, physician assistant) to care for the patient and makes most medical decisions without involving the patient. Since the 1970s, ICP has been shown to play a very important role in improving access to health care services (Brandt et al., 2014). In 2010, the WHO reinforced its support to ICP by creating the Framework for Action on Interprofessional Education and Collaborative Practice (Brandt et al., 2014). WHO’s report described the connection between interprofessional health care teams and patient outcomes (Brandt et al., 2014). Similarly, the “Triple Aim” of improving quality, enhancing the patient’s experience, and lowering costs might be achieved by ICP and has been the focus of health care delivery reform in the United States (Brandt et al., 2014).
Activities performed within the traditional scope of primary care practice include health promotion, disease prevention, and management of common chronic and acute conditions (Hogg et al., 2008). It is reasonable to conclude that it is important to formally research the connection between primary care delivery and the ICP model.
Some reviews have been conducted (Brandt et al., 2014; Reeves et al., 2017; Zwarenstein et al., 2009) to assess the effect of ICP on the triple aim and health care outcomes in a hospital setting; however, to our knowledge, no review has described comprehensively the impact of ICP on patient outcomes in the primary care setting. The objective of this scoping review was to identify and summarize the available literature regarding the composition and functions of interprofessional care teams in primary care settings as well as to determine the known impact of this model of care on patient outcomes (e.g., clinical, humanistic, and economic) when implemented in primary care settings.
Method
This scoping review followed a structured framework for conducting scoping reviews (Arksey & O’Malley, 2005; Levac et al., 2010), composed of six steps: (a) identify the research question; (b) identify relevant studies; (c) select studies; (d) chart the data; (e) collate, summarize, and report results; and (f) seek consultation. The research team was interprofessional (e.g., medical librarian, pharmacists, primary care physician, and a researcher with background in health services and nursing) from various countries (e.g., the United States, Canada, and Australia) and held diverse health system perspectives.
Definitions and Search Strategies
For the purposes of this scoping review, an interprofessional team was defined as a group composed of at least three health workers from different professional backgrounds who communicate and collaborate to provide services to patients, families, caregivers, and communities. At least one team member must have been a primary care provider (e.g., a physician, physician assistant, or nurse practitioner) with the authority to diagnose and initiate treatment based on the scope of practice governing health professional practice in the state or country in which the study was conducted (Canadian Interprofessional Health Collaborative, 2010; Department of Health, 2007; The Interprofessional Curriculum Renewal Consortium, Australia, 2013; WHO, 2010). The Starfield definition of primary care was used, which defines key features of primary care as being the first point of entry to a health care system, person-focused (not disease oriented), and integrates care from outside providers (Starfield, 1998; Valaitis et al., 2012). Four unique features of primary care service delivery include access, continuity, integration, and comprehensiveness. The description of each of these features are explained in Supplemental Appendix A (Hogg et al., 2008).
Literature Search
A comprehensive literature search was conducted by a medical research librarian (A.A.S.). Database searches were conducted in July 2013. Search results were limited to articles published between 2000 and 2013. We selected this time frame because more studies in the area of ICP started to emerge in 2000. The following databases and research registries were searched: Ovid MEDLINE, Ovid MEDLINE In-Process and Other Non-Indexed Citations, Ovid MEDLINE Daily, and Ovid OLDMEDLINE; Embase.com Embase; Wiley Cochrane Library: Cochrane Central Register of Controlled Trials (Issue 6 of 12, June 2013), Cochrane Database of Systematic Reviews (Issue 7 of 12, July 2013), NHS Economic Evaluation Database (Issue 2 of 4, April 2013), Health Technology Assessment Database (Issue 2 of 4, April 2013), Database of Abstracts of Reviews of Effect (Issue 2 of 4, April 2013); Thomson Reuters Web of Science: Science Citation Index, Social Sciences Citation Index, Conference Proceedings Citation Index Science, Conference Proceedings Citation Index-Social Sciences & Humanities, EBSCOhost CINAHL, OvidSP IPA, ClinicalTrials.gov, and HSRProj. A copy of the search strategy is included in Supplemental Appendix B. In addition, we wanted to ensure we searched articles from most journals related to ICP; therefore, we handsearched for articles from journals our team recommended or found via Google search related to the field of ICP. Handsearching was conducted in the following journals:
Study Selection
Following the removal of duplicates, the title and abstract of each record was screened by one investigator (Figure 1). During this initial screening phase, citations were excluded if they did not appear to be relevant or related to the topic of ICP. If the abstract had a topic totally unrelated to ICP such as it did not mention keywords “interprofessional, multidisciplinary, interdisciplinary, and team,” it was excluded.

Article selection flowchart.
Following title/abstract screening, two investigators independently screened the full text of the first 60 studies using an inclusion criteria screening form (Supplemental Appendix C), developed and pilot-tested by the investigators. They compared the results to determine whether the approach to screening was consistent with the research question and purpose (Arksey & O’Malley, 2005; Levac et al., 2010). Disagreements were resolved by consensus or by arbitration by one of the other investigators when no consensus was reached. All remaining articles were screened by one investigator. Studies included in the analysis were conducted in a primary care setting, had an interprofessional team with a team member who provided a range of primary care services, reported patient-related outcomes, and had a comparison group. Studies that did not meet the inclusion criteria from Supplemental Appendix C were excluded. Only studies published in English after 2000 were included. Commentaries, editorials, literature reviews, theoretical models, and descriptive reports were excluded.
Charting the Data
Data from the included studies were extracted using a detailed charting form (form available on request from the corresponding author) (Levac et al., 2010). This form was created using Google forms and piloted with the first 30 studies extracted independently by two investigators (Arksey & O’Malley, 2005; Levac et al., 2010). Once consistency of data extraction was established, the form was refined and finalized. All remaining articles were extracted independently by one investigator.
Data extracted included the study design; team composition, activities, structures, and features; study setting; and patient population. In addition, specific patient-related outcomes were extracted.
Collating, Summarizing, and Reporting Results
Extracted data obtained from the charting process were coded and categorized into common themes in QSR International’s NVivo 10 software for data analysis. Results focusing on the most relevant themes are reported.
Results
A total of 36,161 articles were included after removal of duplicates (Figure 1). After screening the titles and abstracts for relevance, 612 articles were identified for full-text review from which 51 articles were ultimately selected for inclusion based on the inclusion and exclusion criteria.
Study Design, Characteristics, and Outcomes Assessed by Included Articles
Table 1 describes relevant information on the included articles. The majority of the studies included were conducted in the United States (
Characteristics, Study Design, and Outcomes of Included Studies.
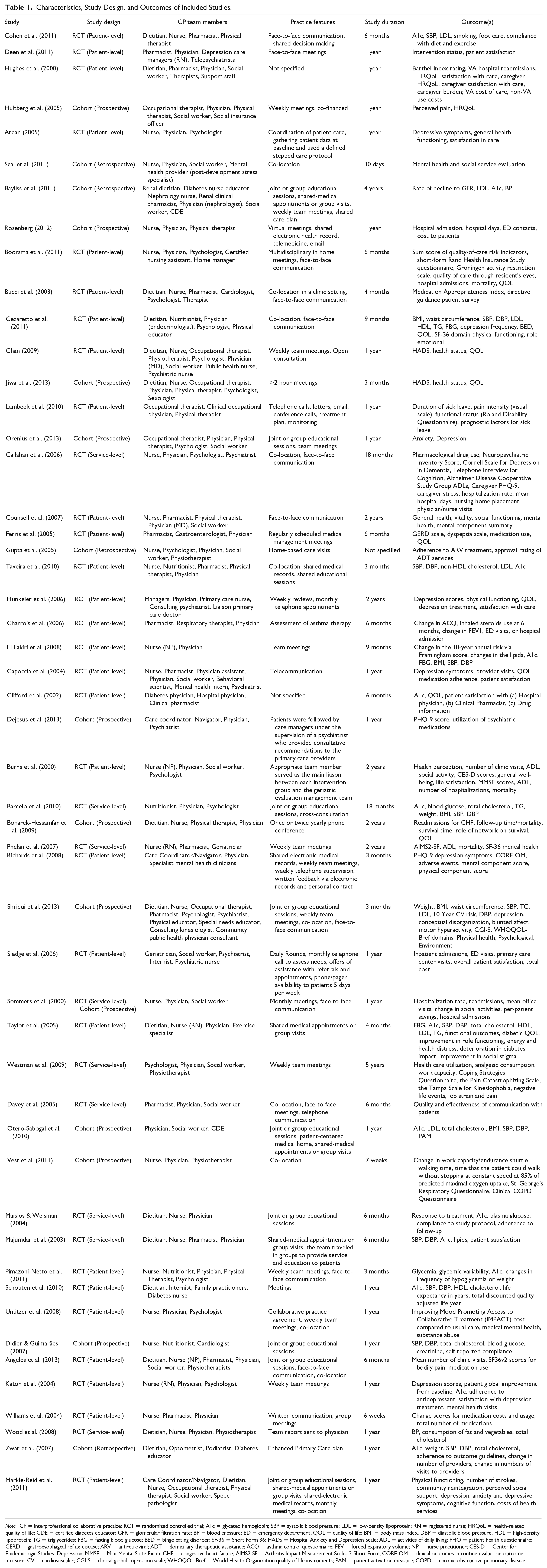
Interprofessional team composition varied widely. The professionals most often included on interprofessional primary care teams were physicians, nurses, therapists (occupational and physical therapist), mental health professionals, dietitian/nutritionists, pharmacists, and social workers (Table 2). The professionals included on interprofessional teams showing significantly positive impact were physicians (
Health care Professionals Represented,

Interprofessional Team Features and Strategies,

Team collaboration most commonly focused on patient education and counseling, and chronic disease management (Table 3).
Effect of Intervention on Clinical Outcomes
Out of 51 studies included, a total of 41 studies reported clinical outcomes including cardiovascular, psychiatric, mortality, pain, renal function, smoking, functional status, health perception, median survival time, patient global improvement, social activity, among others (Table 1).
Twenty-seven studies out of those 41 studies reported a significantly positive clinical outcome when interprofessional primary care teams’ collaborative interventions were implemented, when compared with the control group (e.g., Angeles et al., 2013; Barcelo et al., 2010). Cardiovascular and psychiatric outcomes were the most frequently reported. Specifically, 15 out of 27 studies reported clinical outcomes related to cardiovascular disease with 10 showing significant positive difference in blood pressure (BP), eight in glycated hemoglobin (A1c) and blood glucose, and seven in serum cholesterol (low-density lipoprotein [LDL], high-density lipoprotein [HDL], and total cholesterol [TC]) (Table 4). In addition, 10 out of 27 studies were related to psychiatric illnesses with six showing significant positive difference in depression (frequency of depression, depression scores, caregivers’ Patient Health Questionnaire-9, Center for Epidemiologic Studies–Depression [CES-D], Hopkins Symptom Checklist-90 (SCL-90) mean depression scores, symptom checklist depression scale (SCL-20), remission of depression) (Table 5). Some studies reported multiple clinical outcomes. For example, there were 35 outcomes reported in the 15 studies related to cardiovascular disease and 22 outcomes reported in the 10 studies related to psychiatric illness. See Tables 4 and 5 for further details on cardiovascular and psychiatric outcomes, respectively.
Significant Positive Cardiovascular Clinical Outcomes With ICP Intervention Versus Control (No. of Studies = 15).

Significant Positive Psychiatry Clinical Outcomes With ICP intervention Versus Control (No. of Studies = 10).
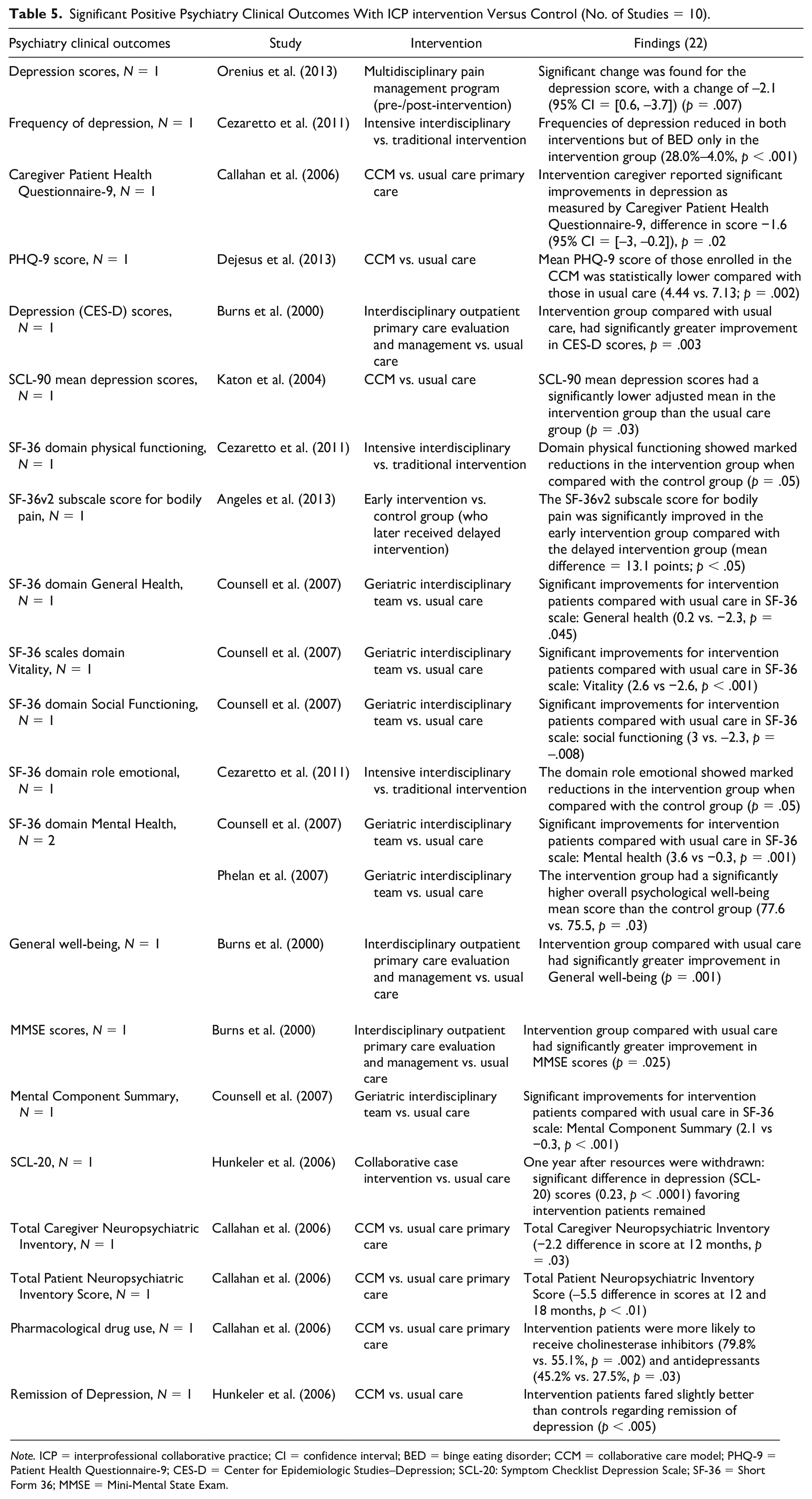

Thirteen studies reported different types of clinical outcomes that were significantly positive and other outcomes that showed no difference (Bayliss et al., 2011; Burns et al., 2000; Callahan et al., 2006; Charrois et al., 2006; Cohen et al., 2011; Didier & Guimarães, 2007; Katon et al., 2004; Majumdar et al., 2003; Otero-Sabogal et al., 2010; Pimazoni-Netto et al., 2011; Shriqui et al., 2013; Taveira et al., 2010; Taylor et al., 2005). Twenty-seven studies reported no difference in clinical outcomes when comparing intervention and control groups. Specifically, 15 out of 27 studies assessing clinical outcomes were for cardiovascular disease with eight showing no difference in serum cholesterol (LDL, HDL, TC, triglyceride [TG]) (Bayliss et al., 2011; Cohen et al., 2011; El Fakiri et al., 2008; Majumdar et al., 2003; Shriqui et al., 2013; Taveira et al., 2010; Taylor et al., 2005), six in A1c and blood glucose (Bayliss et al., 2011; Clifford et al., 2002; Didier & Guimarães, 2007; Katon et al., 2004; Majumdar et al., 2003; Taylor et al., 2005), and three in blood pressure (Otero-Sabogal et al., 2010; Shriqui et al., 2013; Taylor et al., 2005). Nine out of 27 studies focused on psychiatric outcomes with five showing no difference in depression symptoms (Cornell Scale for Depression in Dementia, Recovery from depression, Effect Size on PHQ-9 Depression Symptoms, Hospital Anxiety and Depression Scale (HADS); Callahan et al., 2006; Chan, 2009; Jiwa et al., 2013; Katon et al., 2004; Richards et al., 2008).
One RCT reported negative clinical outcomes in mortality and no difference in activities of daily living (ADLs) disability and Arthritis Impact Measurement Scale 2-Short Form (AIMS2-SF) physical and affect subscales (Phelan et al., 2007). Phelan et al. found that an interprofessional team of geriatrics specialists providing care for 433 patients, compared with 441 patients receiving usual care, resulted in increased mortality in the intervention group at 24 months (11.4% vs. 7.1%,
Effect of the Intervention on Humanistic Outcome
Out of 51 studies included, a total of 25 studies reported humanistic outcomes including measures of patient and caregiver satisfaction, quality of life measures, and treatment adherence. Fifteen out of 25 studies reported a significantly positive humanistic outcome with the ICP model (e.g., Orenius et al., 2013; Shriqui et al., 2013). Of note, six studies reported improved satisfaction with medical care (Arean et al., 2005; Deen et al., 2011; Hughes et al., 2000; Hunkeler et al., 2006; Katon et al., 2004; Majumdar et al., 2003), and five studies reported an improvement in quality of life (Angeles et al., 2013; Hughes et al., 2000; Hunkeler et al., 2006; Lambeek et al., 2010; Orenius et al., 2013). There was also an increase in adherence to medications in two studies (Gupta et al., 2005; Katon et al., 2004). An increase in adherence, specifically with anti-retroviral therapies in the setting of HIV+ patients, was shown in one study by Gupta et al. (2005) when an interprofessional team consisting of a physician, nurse, social worker, physiotherapist, and psychologist provided care to the patient compared with usual care. Another study showed an increase in adherence to antidepressant treatment in the intervention group (Katon et al., 2004).
Three studies had different types of humanistic outcomes that were significantly positive and other outcomes that showed no difference. The significantly positive outcomes included patient satisfaction with drug information; patient satisfaction with care; patient and caregiver health-related quality of life (medical outcomes study, short-form, 36 items); and patient and caregiver satisfaction with care. Outcomes that showed no difference included quality of life; intervention status on the patient ratings of patient respect, being informed about self-help or support groups, being involved in care, feeling safe and the protection of confidentiality; patient and caregiver Barthel Index rating (Clifford et al., 2002; Deen et al., 2011; Hughes et al., 2000). Thirteen studies reported no difference in humanistic outcome with the ICP model compared with the control group. Specifically, six out of 13 studies reported no difference in quality of life (Boorsma et al., 2011; Capoccia et al., 2004; Chan, 2009; Clifford et al., 2002; Ferris et al., 2005; Jiwa et al., 2013). Finally, one study by Angeles et al. reported a negative outcome in quality of life SF-36v2 physical component in the intervention group (15.3 decrease) versus the control group (3.4 increase,
Effect of the Intervention on Economic Outcome
Out of 51 studies included, only six studies evaluated economic outcomes. One study by Williams and colleagues (2004) measured the effect on monthly medication cost when a medication review was conducted by an interprofessional team. This study reported savings in wholesale medication cost of US$26.92 per month for patients in the intervention group versus US$6.75 in the control group (
Discussion
We will be discussing the main findings of clinical, humanistic, and economic outcomes from the studies included in this scoping review. Out of 51 studies included, many studies (
One RCT reported a significantly negative clinical outcome (Phelan et al., 2007). Mortality was increased in the intervention group at 2 years. The study hypothesized that the cause for increased mortality could have been associated with greater disease severity among intervention participants, although the investigators did not collect this data. Another explanation hypothesized was patient confusion as to who (geriatric care team vs. primary care physician) was to make clinical decisions. The authors concluded that ICP is not an appropriate model of care for older adults in primary care. It is uncertain what caused this unnerving result and this outcome should be further analyzed. Although the authors reported mortality being higher in year 2 in the intervention group, life expectancy may have been positively influenced in the intervention group compared with controls. The average age in both groups was the same and mortality was higher in the control group at 12 months. Nevertheless, it is important to point out that open communication is key between health care professionals when caring for patients, to prevent confusion, which was one of the possible causes for the negative outcome reported by the authors.
Overall, a majority of studies reporting humanistic outcomes showed significantly positive results with ICP compared with usual care, specifically for satisfaction with care and adherence to medications. In one study that reported a negative humanistic outcome in quality of life, the authors doubted they had used the most appropriate measurement tool, as their results contradicted the overall positive qualitative comments from patients (Angeles et al., 2013). Therefore, this result should be considered less reliable.
There were only a small number of studies (
Given that it is not possible to conduct a meta-analysis of these data due to the heterogeneity of the study designs, patient populations, interprofessional team composition, and outcome measures, we chose to use a scoping literature review approach. In addition, we did not perform a risk of bias assessment, because that is generally not conducted in scoping reviews (Munn et al., 2018). Our review differs from other reviews in several ways. Our definition for ICP required the team to have at least three different health professionals involved in the patient care. Other investigators included studies with two or more health care professionals (Reeves et al., 2017). A major strength of our scoping review is that we searched a broad range of databases and gray literature as part of our literature search, which resulted in the inclusion of a larger number of studies compared with previous reviews (Reeves et al., 2011, 2017).
There are some limitations to this scoping review that are important to note. While we attempted to include all the studies available from 2000 to 2013, it is possible some relevant studies were missed. Our review did not include studies after the year 2013 and some important new work may have been published since then. Therefore, as there is still no other scoping review similar to this one published to date, these data would still help future researchers gain knowledge and perspective of the impact of interprofessional care on patient outcomes during the period of 2000–2013.
In addition, it was not possible to clearly identify which studies used shared decision making as part of their ICP model, which may be an important element of high-quality interprofessional team-based care. Shared decision making was not discussed or defined in a majority of the studies. As this was a scoping review with a focus on reporting the main themes that emerged, the studies that showed no difference in outcomes and the possible reasons for such results were not fully investigated. Finally, another limitation is that we did not separate out the different outcomes based on countries; however, this may be something other researchers may be interested in doing in the future and could find this scoping review helpful to get started.
Despite positive results in the majority of papers, several studies reported no difference when comparing ICP to usual care. These results should be further analyzed to identify the lessons learned and aspects of interventions needed to improve the ICP model. Rarely studies reported significant negative patient outcomes with the ICP model, but these results should be carefully considered.
Conclusion
Our findings reveal that there are studies showing that ICP in primary care settings can positively impact clinical and humanistic outcomes. Future studies should identify unique activities and interventions that were highly successful among ICP teams with positive impact on patient outcomes. In addition, studies should aim to define shared decision making clearly within their study and the process of how it is implemented. Furthermore, more studies are needed to determine the impact of ICP on humanistic and economic outcomes in the primary care setting. Beyond cardiovascular and psychiatric outcomes, other common diseases seen within primary care settings should be further explored to determine the impact of the ICP model.
Supplemental Material
Appendix_A-Features_of_Primary_Care_Service_Delivery – Supplemental material for Impact of Interprofessional Primary Care Practice on Patient Outcomes: A Scoping Review
Supplemental material, Appendix_A-Features_of_Primary_Care_Service_Delivery for Impact of Interprofessional Primary Care Practice on Patient Outcomes: A Scoping Review by Livia R. M. McCutcheon, Stuart T. Haines, Ruta Valaitis, Deborah A. Sturpe, Grant Russell, Ahlam A. Saleh, Kevin A. Clauson and Jeannie K. Lee in SAGE Open
Supplemental Material
Appendix_B-_Search_Strategy – Supplemental material for Impact of Interprofessional Primary Care Practice on Patient Outcomes: A Scoping Review
Supplemental material, Appendix_B-_Search_Strategy for Impact of Interprofessional Primary Care Practice on Patient Outcomes: A Scoping Review by Livia R. M. McCutcheon, Stuart T. Haines, Ruta Valaitis, Deborah A. Sturpe, Grant Russell, Ahlam A. Saleh, Kevin A. Clauson and Jeannie K. Lee in SAGE Open
Supplemental Material
Appendix_C-_Inclusion_Criteria_Screening_Form – Supplemental material for Impact of Interprofessional Primary Care Practice on Patient Outcomes: A Scoping Review
Supplemental material, Appendix_C-_Inclusion_Criteria_Screening_Form for Impact of Interprofessional Primary Care Practice on Patient Outcomes: A Scoping Review by Livia R. M. McCutcheon, Stuart T. Haines, Ruta Valaitis, Deborah A. Sturpe, Grant Russell, Ahlam A. Saleh, Kevin A. Clauson and Jeannie K. Lee in SAGE Open
Footnotes
Acknowledgements
The authors thank Drs. Miguel Franquiz, Suhl Choi, Susan Williams, Janice Lee, and Erica Wilson for their assistance during various phases of this research project.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
