Abstract
To address the prevalence of chronic diseases in Newfoundland and Labrador, the province has committed to primary health care reform, including implementing interdisciplinary primary care (PC) teams. To inform discussions regarding integrating nurse practitioners (NPs), registered nurses (RNs), and licensed practical nurses (LPNs) into these teams, better understanding of their roles in PC is needed. A scoping review was conducted to examine and synthesize existing evidence related to nursing roles and resources in PC settings across Atlantic Canada (Newfoundland and Labrador, New Brunswick, Nova Scotia, Prince Edward Island), and associated contributions to patient care. Joanna Briggs Institute scoping review methodology was used. The Nursing Role Effectiveness Model guided the review. Twenty articles met inclusion criteria. Roles of RNs and NPs in PC included chronic disease management, education, and health promotion. No literature focused on LPNs. Interdisciplinary collaboration was evident across studies. However, nurses’ functions within teams were limited by institutional constraints and other providers. PC settings with nurses had positive clinical outcomes, improved access to services, and high patient satisfaction. The prevalence of nursing in PC throughout Atlantic Canada and how nurses’ roles are enacted is unclear. There is opportunity for future inquiry into specific attributes of nursing and PC teams that result in positive patient and system outcomes.
Background and Purpose
Newfoundland and Labrador ranks among the highest in Canada for the prevalence of chronic diseases (Government of Newfoundland and Labrador, 2011) and modifiable risk factors for chronic diseases (Government of Newfoundland and Labrador, 2002). Individuals living with chronic diseases in Newfoundland and Labrador access health care services primarily through family physicians (Government of Newfoundland and Labrador, 2002). However, high rates of family physician turnover have created a barrier to access and lack of continuity of care for many individuals in the province, particularly in rural areas (Mathews, Edwards, & Rourke, 2008; Mathews & Park, 2007). In response to the prevalence and burden of chronic diseases, the Government of Newfoundland and Labrador (2011) published a policy framework aimed at preventing and managing chronic diseases in the province. The framework outlined a commitment to optimize health service delivery, citing interdisciplinary team–based primary health care as a potential strategy. Interdisciplinary primary care (PC) teams have been found to improve outcomes for individuals with chronic diseases and reduce the economic burden of illness (Aggarwal & Hutchison, 2012; Health Council of Canada, 2009).
In Canada, there are three licensure categories for nurses; nurse practitioners (NPs), registered nurses (RNs), and licensed practical nurses (LPNs; known as registered practical nurses in Ontario). Emerging evidence suggests the presence of nurses in PC settings is associated with positive outcomes for patients and the health care system. Higher levels of nurse staffing in PC settings is associated with favorable clinical outcomes and higher rated care, particularly for patients with chronic diseases (Griffiths, Maben, & Murrells, 2011; Griffiths, Murrells, Maben, Jones, & Ashworth, 2010; Lukewich, Williamson, Edge, VanDenKerkhof, & Tranmer, 2016). Furthermore, patients cared for by nurses in PC settings received more teaching (Laurant et al., 2005; Swan, Ferguson, Chang, Larson, & Smaldone, 2015) and reported higher satisfaction with care (Horrocks, Anderson, & Salisbury, 2002; Laurant et al., 2005) than those cared for by other providers, such as physicians. Health outcomes were found to be equal between patients seen by PC NPs or in nurse-led PC centers when compared with those seen by physicians (Keleher, Parker, Abdulwadud, & Francis, 2009; Laurant et al., 2005; Swan et al., 2015). However, there is evidence that nurse-led care is more cost-effective (Swan et al., 2015), which highlights potential for greater emphasis on PC nursing services to reduce health care costs.
As Canadian health care systems transition to interdisciplinary models of care, there is a need to explore and synthesize available information related to nursing in PC. Although nurses are essential to the interdisciplinary team, their role in PC settings is not well understood (Lukewich, Edge, VanDenKerkhof, & Tranmer, 2014; Martin-Misener et al., 2014). A comprehensive summary of available information related to nursing roles and associated outcomes are needed to contribute to resources used to inform discussions related to PC models that incorporate nurses, particularly within Newfoundland and Labrador where PC is currently largely provided by physicians.
The research question guiding this review was as follows:
The Nursing Role Effectiveness Model guided the study. This model is adapted from Donabedian’s (1980) model of quality care, and depicts a structure–process–outcome approach that can be used to guide assessment of nursing contributions to health care (Irvine, Sidani, & McGillis Hall, 1998). Structural variables include characteristics of patients (e.g., age, physical condition), nurses (e.g., education, designation, skill level), and organizations (e.g., staffing patterns, models of care) that purportedly affect nurses’ ability to perform their role functions. The process component of the model includes nurses’ functions categorized as independent, interdependent, and medical-related roles. According to the Nursing Role Effectiveness Model, structure and process variables influence patient and system outcomes, including physical and functional health outcomes, knowledge, satisfaction, and cost (Irvine et al., 1998). The Nursing Role Effectiveness Model has been used as a framework for several recent studies of nursing within a variety of practice settings (Doran et al., 2014; Rondinelli, Omery, Crawford, & Johnson, 2014; White, Jackson, Besner, & Norris, 2015).
Methods and Procedures
This study was conducted using the Joanna Briggs Institute (JBI; 2015) scoping review methodology. Scoping reviews are appropriate when review authors aim to assess the size, scope, and characteristics of available research on a topic, and to identify key concepts within the extant literature (Arksey & O’Malley, 2005; Grant & Booth, 2009; JBI, 2015).
A preliminary scan of the literature revealed a small volume of heterogeneous literature from Newfoundland and Labrador. In consultation with a librarian, it was determined that a comprehensive examination of relevant literature would be best achieved if the search was expanded to include all four Atlantic Canadian provinces (i.e., Newfoundland and Labrador, Nova Scotia, New Brunswick, Prince Edward Island). The search was conducted from September to November, 2016. A three-step search strategy was used to find both published and unpublished studies (JBI, 2015). An initial limited search of PubMed and the Cumulative Index to Nursing and Allied Health Literature (CINAHL) was conducted using the following search terms: nurs* AND primary care AND Newfoundland and Labrador OR New Brunswick OR Nova Scotia OR Prince Edward Island. Next, words contained in titles and abstracts and subject headings, which are used to describe articles, were analyzed and a second search using identified terms was undertaken across all included databases (Table 1). The databases searched included PubMed, CINAHL, Embase, AMED, JBI Database, Cochrane Database, Sociological Abstracts, OT Seeker, Google Scholar, and PEDro. Third, the reference lists of all included reports and articles were searched for key studies, authors, and organizations. In addition, 19 relevant websites were searched, including the Canadian Nurses Association, Canadian Family Practice Nurses Association, provincial nursing regulatory bodies, and provincial ministries of health.
Scoping Review Phase 2 Search Terms.

Note. EBP = evidence-based practice; CINAHL = cumulative index to nursing and allied health literature; PEDro = physiotherapy evidence database.
Inclusion Criteria
All articles retrieved were reviewed independently by two reviewers for relevance and inclusion in the review. The review included published literature, including qualitative and quantitative primary research studies, reports, and discussion papers; and unpublished literature, including expert opinions, discussion papers, position papers, and reports. The scoping review included literature that pertained to NPs, RNs, or LPNs working in a PC setting and/or as part of a PC team in any Atlantic province (i.e., Newfoundland and Labrador, Nova Scotia, New Brunswick, Prince Edward Island). Literature pertaining to settings/services other than PC, such as acute care, long-term care, and emergency services were excluded. Articles were considered for inclusion if they were related to variables outlined within the Nursing Role Effectiveness Model (Irvine et al., 1998). All literature available as of November, 2016 was considered, as historical trends were considered relevant to overall findings. Only English language articles were considered eligible for review. As per JBI (2015) scoping review methodology, the quality of literature was not a factor in determining eligibility for inclusion.
Results
A summary of search results is included in Figure 1. Once duplicates were removed, the database search returned 114 results. Defined inclusion and exclusion criteria were applied and 17 articles were deemed eligible for inclusion. The web search resulted in inclusion of two additional reports (Health Council of Canada, 2009; Labrosse, 2016) and perusal of reference lists of eligible articles resulted in the inclusion of one additional research article (Goss Gilroy Inc, 2001). An additional four articles were potentially eligible; however, despite requesting access from the authors, full-text articles could not be obtained. After all inclusion and exclusion criteria were applied, a total of 20 articles were eligible for inclusion and were reviewed. Data extraction was guided by available JBI data extraction forms.

Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) diagram for scoping review.
Included literature (Table 2) consisted of 11 primary research studies (Barrett et al., 2011; Chambers, Bruce-Lockhart, Black, Sampson, & Burke, 1977; Chambers & West, 1978; Goss Gilroy Inc, 2001; Graham, Sketris, Burge, & Edwards, 2006; Lawson, Dicks, Macdonald, & Burge, 2012; Martin-Misener, Downe-Wamboldt, Cain, & Girouard, 2009; Martin-Misener, Reilly, & Vollman, 2010; Murphy, Martin-Misener, Cooke, & Sketris, 2009; Paterson, Duffett-Leger, & Cruttenden, 2009; Todd, Howlett, MacKay, & Lawson, 2007), three position papers (Agnew, 1974; Bristow et al., 1974; Faculty of Nursing University of New Brunswick [UNB], 1974), two feature columns (Jaimet, 2012; Magee, Hodder-Malloy, & Mason, 2011), and four reports (Health Council of Canada, 2009; Jones, 2015; Labrosse, 2016; Martin-Misener, McNab, Sketris, & Edwards, 2004).
Summary of Included Literature (n = 20).
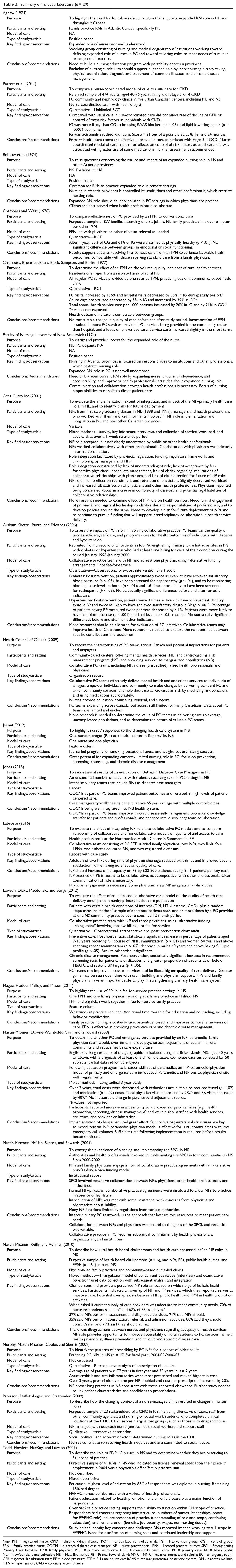
Note. RN = registered nurse; CKD = chronic kidney disease; RCT = randomized controlled trials; IG = intervention group; CG = control group; FPN = family practice nurse; ODCM = outreach diabetes case manager; NP = nurse practitioner; LPNs = licensed practical nurses; SPCI = Strengthening Primary Care Initiative; FP = family physician; PHC = primary health care; CHC = community health clinic; PC = primary care; NS = Nova Scotia; NL = Newfoundland and Labrador; NB = New Brunswick; PE = Prince Edward Island; MMR = MMR = measles, mumps, and rubella; ER = emergency room; GFR = glomerular filtration rate; BP = blood pressure; FTE = full time equivalent; RAAS = renin-angiotensin-aldosterone system; DM - diabetes mellitus, HTN = hypertension; CAD = coronary artery disease.
Nova Scotia had the greatest amount of literature related to nursing within PC settings (n = 11) compared with other Atlantic provinces, including four quantitative (Barrett et al., 2011; Graham et al., 2006; Lawson et al., 2012; Murphy et al., 2009) and three mixed methods (Martin-Misener et al., 2009; Martin-Misener et al., 2010; Todd et al., 2007) research studies, and four nonresearch articles (Bristow et al., 1974; Health Council of Canada, 2009; Magee et al., 2011; Martin-Misener et al., 2004). Six articles were from Newfoundland and Labrador (Agnew, 1974; Barrett et al., 2011; Chambers et al., 1977; Chambers & West, 1978; Goss Gilroy Inc, 2001; Health Council of Canada, 2009) and five articles were from New Brunswick (Faculty of Nursing UNB, 1974; Health Council of Canada, 2009; Jaimet, 2012; Jones, 2015; Paterson et al., 2009). New Brunswick was represented in only one primary research study, which was qualitative (Paterson et al., 2009), whereas PC nursing in Newfoundland and Labrador was studied in three randomized controlled trials (RCT; Barrett et al., 2011; Chambers et al., 1977; Chambers & West, 1978) and a mixed methods study (Goss Gilroy Inc, 2001). Prince Edward Island was represented in one report discussing the role of NPs in PC (Labrosse, 2016). In the RCT by Barrett et al. (2011) and the report by the Health Council of Canada (2009), more than one Atlantic province was examined.
Nurse Structural Variables in PC Settings
The RN and NP designations were most represented in PC literature from Atlantic Canada. Nurses within the RN and NP designations were the focus in 10 articles each. Specifically, the role of the RN as a family practice nurse (FPN) was explored in five articles (Agnew, 1974; Chambers et al., 1977; Chambers & West, 1978; Magee et al., 2011; Todd et al., 2007). No articles focused on LPNs. LPNs were mentioned as part of a PC team in a case study of one clinic (Labrosse, 2016). However, the report focused only on the NPs working on the team. In three articles, the term “nurse” was used to refer to a group of nurses without specifying designation (Barrett et al., 2011; Health Council of Canada, 2009; Paterson et al., 2009), and some articles focused on more than one nursing designation (Health Council of Canada, 2009; Martin-Misener et al., 2010; Paterson et al., 2009). There were no studies that explored the relationships between nursing designation and education level on patient or system outcomes.
In early publications, there was emphasis on promoting baccalaureate education for RNs in the Atlantic provinces and expanding nursing curricula to include additional clinical skills (Agnew, 1974; Bristow et al., 1974). This enhanced knowledge and skill translated to an “expanded nursing role” (Agnew, 1974; Bristow et al., 1974; Faculty of Nursing UNB, 1974) that became pivotal in PC in Atlantic Canada (Chambers et al., 1977; Chambers & West, 1978). However, the current overall education level of nurses in PC and how it relates to nursing roles or patient and system outcomes is unclear. A survey of a small sample of 41 participants by Todd and colleagues (2007) reported that 85% of family practice RNs in Nova Scotia had a diploma in nursing, whereas the remaining 15% had a baccalaureate degree. However, the data were purely descriptive. No such data were reported for NPs, LPNs, or RNs working in other Atlantic provinces.
Organizational Structure: Models of PC Delivery
Interdisciplinary collaboration between nurses, physicians, and other health professionals was evident throughout the literature. There was a variety of interdisciplinary PC team models discussed. Nurse-led care by NPs (Goss Gilroy Inc, 2001; Paterson et al., 2009), RNs (Chambers & West, 1978), or unspecified nurses (Barrett et al., 2011; Health Council of Canada) in consultation with physicians and other professionals was identified in Newfoundland and Labrador and New Brunswick. Alternatively, NPs and physicians in Nova Scotia engaged in formal collaborative practice agreements (Graham et al., 2006; Lawson et al., 2012; Martin-Misener et al., 2004). An innovative NP–physician paramedic model for providing PC to a remote location in Nova Scotia was examined in a longitudinal mixed method study by Martin-Misener et al. (2009). Findings from this study indicated this model reduced emergency room visits, improved patient satisfaction, and reduced health care costs over a 3-year period.
Historically in Atlantic Canada, nurse autonomy was exercised almost exclusively in areas where no other PC provider was available (Agnew, 1974; Chambers et al., 1977). The expanded nursing role of the 1970s was expected to enhance nurse autonomy and oppose the hierarchical structure of health care (Bristow et al., 1974; Faculty of Nursing UNB, 1974). Nurses began to practice independently or in collaboration with physicians (Chambers et al., 1977; Chambers & West, 1978). PC practice environments have continued to evolve to promote nurse autonomy and nurse-led models of care (Barrett et al., 2011; Chambers et al., 1977; Chambers & West, 1978; Goss Gilroy Inc, 2001; Jaimet, 2012; Paterson et al., 2009). Yet, placement of nurses in PC continues to be motivated by a need to improve access to PC practitioners, particularly in response to challenges with recruiting and retaining family physicians (Chambers et al., 1977; Goss Gilroy Inc, 2001; Labrosse, 2016; Martin-Misener et al., 2009). Goss Gilroy Inc (2001) reported NPs had no effect on recruitment and retention of other care providers in Newfoundland and Labrador, and that settings in which NPs reported practicing autonomously were primarily those without family physicians.
Nurse Process Variables: Nursing Roles in PC
The reported role of RNs and “nurses” in PC principally involved managing chronic diseases (Barrett et al., 2011; Health Council of Canada, 2009; Jones, 2015; Magee et al., 2011) and providing education and counseling to patients (Health Council of Canada, 2009; Jaimet, 2012; Jones, 2015; Magee et al., 2011; Todd et al., 2007). In particular, risk factor modification (Barrett et al., 2011; Health Council of Canada, 2009; Jones, 2015; Magee et al., 2011) and promoting self-management (Barrett et al., 2011; Health Council of Canada, 2009; Jones, 2015) were cited as aspects of nurses’ roles in chronic disease management. Patient education and counseling roles included diabetes education (Jones, 2015), one-on-one smoking cessation counseling (Jaimet, 2012), behavior modification (Magee et al., 2011), and general provision of health-related information (Magee et al., 2011; Todd et al., 2007). Other nursing roles included advocating for social justice for marginalized populations (Health Council of Canada, 2009; Paterson et al., 2009), facilitating clinician education (Jones, 2015), organizing health and fitness programs (Jaimet, 2012), and providing direct interventions, such as screening tests and medication administration (Martin-Misener et al., 2010; Todd et al., 2007).
With respect to NPs, specifically, literature described their role in diagnosing, treating, and managing chronic diseases, including diabetes, pulmonary disease, kidney disease, mental illness, and cardiovascular disease; and episodic illnesses, such as infections (Goss Gilroy Inc, 2001; Graham et al., 2006; Labrosse, 2016; Lawson et al., 2012; Martin-Misener et al., 2009; Martin-Misener et al., 2004; Martin-Misener et al., 2010; Murphy et al., 2009). Prescribing and managing medications and monitoring clinical outcomes were also cited as part of the NP role (Goss Gilroy Inc, 2001; Lawson et al., 2012; Martin-Misener et al., 2010).
Nurse role implementation and integration into PC settings was affected by various governmental, financial, and sociopolitical factors (Goss Gilroy Inc, 2001; Martin-Misener et al., 2004; Paterson et al., 2009). Nursing roles were found to be responsive to the needs of populations and communities (Paterson et al., 2009). Based on qualitative data, strong governmental support, in the form of regulation, legislation, and funding, facilitated nurses’ roles in practice (Goss Gilroy Inc, 2001; Martin-Misener et al., 2004). Barriers to performing role functions included financial constraints (Paterson et al., 2009), lack of understanding and acceptance of roles (Goss Gilroy Inc, 2001; Martin-Misener et al., 2004), and lack of substantial planning for the future direction of nurse roles (Goss Gilroy Inc, 2001). In collaborative settings, lack of role clarity led to concerns about potential effects on the roles and responsibilities of other professionals. In particular, concerns from physicians regarding the scope of practice of NPs and the legal implications of collaborative practice were identified (Goss Gilroy Inc, 2001; Martin-Misener et al., 2004). Although the NP role was expected to alleviate some of the pressure on family physicians, some physicians found the NP role disruptive to their practice (Goss Gilroy Inc, 2001; Labrosse, 2016). In a survey conducted by Goss Gilroy Inc (2001), physicians cited concerns such as increased complexity of caseload as NPs took on patients with less complicated conditions. Martin-Misener et al. (2010) noted that differences in attitudes of nurses and family physicians toward the perceived adequacy of health services could also affect nursing roles within PC settings. When they asked participants whether the current supply of health care practitioners was adequate to meet community needs, 70% of nurse respondents replied “no,” whereas 62% of family physicians said “yes.”
Patient and System Outcomes
Eleven articles discussed patient and system outcomes related to nurses within PC. In Atlantic Canada, PC settings that incorporate nurses have resulted in better (Chambers et al., 1977; Chambers & West, 1978; Graham et al., 2006; Jones, 2015; Lawson et al., 2012) or equal (Barrett et al., 2011; Chambers & West, 1978; Labrosse, 2016; Lawson et al., 2012) patient health outcomes when compared with settings that do not include nurses. In particular, many clinical outcome measures for patients with chronic diseases were improved (Barrett et al., 2011; Graham et al., 2006; Jones, 2015; Lawson et al., 2012) or unchanged (Barrett et al., 2011) with the addition of nurses when compared with usual care. Notably, patients with chronic diseases had increased odds of having satisfactory blood pressure (Graham et al., 2006; Lawson et al., 2012) and hemoglobin A1C levels (Lawson et al., 2012); receiving certain recommended medications (Barrett et al., 2011); and participating in many recommended screening and monitoring practices (Graham et al., 2006; Lawson et al., 2012) when nurses were added to models of care. Nurses in PC settings are also associated with improved access to health services, as evidenced by increased PC visits (Chambers et al., 1977), decreased hospital or emergency department visits (Chambers et al., 1977; Martin-Misener et al., 2009), shorter wait times (Labrosse, 2016; Magee et al., 2011), and greater frequencies of recommended screening and monitoring practices (Graham et al., 2006; Lawson et al., 2012). Patients reported increased accessibility of a broader range of health services (Martin-Misener et al., 2009) and high levels of satisfaction (Barrett et al., 2011; Health Council of Canada, 2009; Jones, 2015; Labrosse, 2016; Martin-Misener et al., 2009) with models of PC that incorporate nurses. Reports suggested implementing interdisciplinary PC teams with nurses increased initial health care expenditures (Chambers et al., 1977; Labrosse, 2016; Martin-Misener et al., 2009; Murphy et al., 2009). Only one study examined costs longitudinally, and overall costs were found to decrease over a 3-year period (Martin-Misener et al., 2009). Many of these studies identified reliance on chart abstraction of existing health records as a limitation to conducting research of this nature (Chambers et al., 1977; Graham et al., 2006; Labrosse, 2016; Lawson et al., 2012; Murphy et al., 2009).
Discussion
Overall, there was limited evidence related to nursing within PC in Atlantic Canada. Consistent with JBI (2015) scoping review methodology, comprehensive quality appraisal of literature was not performed. However, many limitations within the body of evidence were recognized throughout the processes of data extraction and analysis. Much of the literature consisted of position papers and reports that did not provide new evidence, or did not clearly outline the sources and methods from which information was derived. Only 11 out of 20 articles reviewed were primary research studies. Of these, only three were experimental studies (Barrett et al., 2011; Chambers et al., 1977; Chambers & West, 1978), two of which were nearly 40 years old. In addition, many methodological limitations, such as small sample sizes and vague statistical reporting (e.g., unreported p values and odds ratios) were noted in studies. The lack of high quality, strongly designed literature limits the extent to which decisions about policy and practice throughout Newfoundland and Labrador and Atlantic Canada can be informed. This scoping review highlights the need for more rigorous research related to nursing within PC, and it is a necessary first step in guiding the direction of research in this area.
The literature was well dispersed over three of the four Atlantic provinces. Prince Edward Island was considerably underrepresented in the literature. This may be due in part to the comparatively small population and geographic area of Prince Edward Island in relation to the other provinces. Also, it is noteworthy that Newfoundland and Labrador, New Brunswick, and Nova Scotia have all released frameworks for or developed initiatives to improve PC using interdisciplinary health care teams that include nurses (Government of New Brunswick, n.d.; Government of Newfoundland and Labrador, 2015; Martin-Misener et al., 2004), whereas Prince Edward Island has not. In addition to the Strengthening Primary Care Initiative, a provincial initiative aimed at reforming PC delivery using interdisciplinary health care teams across the province (Graham et al., 2006; Lawson et al., 2012; Martin-Misener et al., 2004), the large number of articles from Nova Scotia may be related to the existence of the Family Practice Nurses Association of Nova Scotia (a provincial affiliated group of the Canadian Family Practice Nurses Association), and the availability of a Family Practice Nursing Education Program offered through the Registered Nurses Professional Development Centre (Canadian Family Practice Nurses Association, 2016; Registered Nurses Professional Development Centre, n.d.).
Nurses’ roles in health promotion and preventive care, particularly for individuals with chronic diseases, aligns well with the Government of Newfoundland and Labrador’s (2002, 2011, 2015) plans for addressing pressing health system challenges. RNs and NPs are currently involved in these roles in PC across Atlantic Canada. It is conceivable that LPNs may also be among the cohort of nurses in PC in Atlantic Canada, as they are in other locations (Freund et al., 2015). However, LPNs were not identified as participants in any literature. We cannot rule them out as participants, as some articles discussed “nurses” without specifying a designation (Barrett et al., 2011; Health Council of Canada, 2009; Paterson et al., 2009). Because the scopes of practice, roles, and responsibilities of each nursing designation are different, future studies should attempt to be clear about designations when designing and reporting studies of nurses. LPNs are the lowest paid of the three nursing regulatory designations, making them attractive to governments and employers who are interested in reducing or controlling expenditures. But, the applicability of research findings to LPN practice within PC teams is limited by the lack of LPN-specific data. There is a need for future research to examine the contribution of this group of nurses to PC, especially in Newfoundland and Labrador, where current budgetary constraints demand prudence.
The findings related to barriers and facilitators of nursing role implementation and integration in PC are consistent with the greater Canadian and international literature. Financial constraints (DiCenso & Matthews, 2005), legislation, health care provider attitudes (Cashin, Theophilos, & Green, 2017; DiCenso & Matthews, 2005), and lack of understanding of roles (Cashin et al., 2017; van Soeren, Hurlock-Chorostecki, Goodwin, & Baker, 2009) are cited as barriers throughout the literature. Although there is limited discussion of facilitators to RN and LPN role implementation and integration in PC, the greater body of literature indicates teamwork between NPs and other health care professionals is facilitated by positive, supportive relationships between professionals and their management teams (Poghosyan & Liu, 2016; Reay, Golden-Biddle, & Germann, 2003; Sangster-Gormley, Martin-Misener, Downe-Wamboldt, & DiCenso, 2011). Furthermore, a structural approach that fosters active participation by health care providers in the planning and implementation process (Reay et al., 2003; Sangster-Gormley et al., 2011) and includes clear policies and practice protocols to minimize role confusion (Norful, Martsolf, de Jacq, & Poghosyan, 2017; Reay et al., 2003) can facilitate NP and RN role implementation and integration in PC. The transition to collaborative practice teams in Atlantic Canada has required extensive commitment from government, institutions, and professionals (Health Council of Canada, 2009; Martin-Misener et al., 2009; Martin-Misener et al., 2004), and much work remains to be done. Although outcomes are promising, there is resistance and perceived lack of support by some stakeholders concerning integration of nursing roles into PC teams. It is in the best interest of professionals, authorities, and the public to explore means of identifying and addressing issues of resistance (Sangster-Gormley et al., 2011). However, the literature did not indicate what, if any, strategies have been implemented to address this issue. Furthermore, many of the articles included in the review were written at times when nurses were being transitioned into PC settings or into new roles within their current settings. To best inform future decisions about nursing role implementation and integration within PC in Atlantic Canada, it would be prudent to re-examine stakeholder attitudes once nurse roles have been in place for some time.
Consistent with other Canadian and international literature (Griffiths et al., 2011; Griffiths et al., 2010; Horrocks et al., 2002; Keleher et al., 2009; Laurant et al., 2005; Lukewich et al., 2016; Swan et al., 2015), the findings of studies included in the review indicated the presence of nurses in PC settings is associated with positive patient and system outcomes. Most notably, there is some evidence in the Atlantic Canadian literature to support that PC teams that incorporate nurses can improve access to health care and improve health outcomes from individuals living with chronic diseases. Studies that examined the relationship between nursing care and patient outcomes found that outcome measures were improved or comparable when measured against care models that did not incorporate nurses. However, researchers did not attempt to identify specific nursing resources and attributes of PC teams that contribute to outcomes. Incorporating a structure–process–outcome framework, such as the Nursing Role Effectiveness Model, into future studies would help clarify the nature of relationships between variables. Furthermore, there were only six published, peer-reviewed research studies examining the relationships between nursing and patient or system outcomes in PC settings. These points represent substantial gaps in evidence in this field and important opportunities for future research.
Limitations
Although the authors attempted to retrieve all available literature, it is possible that additional studies and articles exist that could further enhance our understanding of the use of nursing resources within PC settings in Atlantic Canada. Consistent with JBI (2015) scoping review methodology, we did not conduct comprehensive appraisal of studies or exclude any literature based on methodological quality. Therefore, results cannot be assumed to be generalizable and should not be used alone to inform policy and practice (Arksey & O’Malley, 2005; Grant & Booth, 2009; JBI, 2015).
Conclusion
This scoping review has examined literature related to nursing roles and resources within PC settings in Atlantic Canada. Nurses are present and active in PC settings, particularly as members of collaborative teams. However, the extent to which nursing roles and resources are being utilized remains unclear. Emerging evidence suggests nurses in PC settings positively affect patient outcomes and improve access to health care; and thus, may contribute to necessary improvements within Atlantic Canadian health care systems. Continued commitment by health professionals, health authorities, and provincial governments is needed to support optimization of nursing resource utilization in PC. For this to be accomplished, further inquiry is needed to enhance understanding of the value of nursing roles and resources in achieving desired patient and system outcomes. There is potential for greater understanding of the relationships between variables identified in this review using the Nursing Role Effectiveness Model in research frameworks.
Footnotes
Acknowledgements
The authors are grateful to Ms. Michelle Swab, Public Services Librarian at Memorial University Health Sciences Library, for her contributions to developing the scoping review protocol; and to Ms. Samantha Taylor, research assistant and Bachelor of Nursing (Collaborative) student at Memorial University School of Nursing, for her assistance with reviewing articles.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the Memorial University of Newfoundland School of Nursing Research Fund. Deanne Curnew received financial support as a Master of Nursing student through the Canadian Institutes of Health Research (CIHR), Association of Registered Nurses of Newfoundland and Labrador (ARNNL) Education and Research Trust, Health Care Foundation, and Memorial University of Newfoundland School of Graduate Studies.
