Abstract
Articulated education pathways between the vocational education training sector and universities provide opportunities for students wishing to progress to higher qualifications. Enrolled nurses seeking to advance their career in nursing can choose to enter baccalaureate degree programs through such alternative entry routes. Awarding of credit for prior studies is dependent on accurate assessment of the existing qualification against that which is sought. This study employed a modified Delphi method to inform the development of an evidence-based, structured approach to mapping the pathway from the nationally consistent training package of the Diploma of Nursing to the diversity of baccalaureate nursing programs across Australia. The findings of this study reflect the practical nature of the role of the enrolled nurse, particularly the greater emphasis placed on direct care activities as opposed to those related to professional development and the generation and use of evidence. These findings provide a valuable summative overview of the relationship between the Diploma of Nursing and the expectations of the registered nurse role.
Keywords
Introduction
Tertiary education in Australia is a two-tiered system that provides students with the opportunity to articulate from the Vocational Education and Training (VET) sector to the higher education (HE) sector. This pathway is most commonly used to step from certificate and diploma qualifications to a degree qualification, although evidence suggests student movement between the VET and HE sectors remains relatively modest in Australia (Curtis, 2006; Langworthy & Johns, 2012).
Articulation arrangements between these sectors broaden access to HE (Langworthy & Johns, 2012). This is particularly the case for students who come from disadvantaged backgrounds (Hoelscher, Hayward, Ertl, & Dunbar-Goddet, 2008; Moodie, 2010). Successful inter-sectorial pathways are characterized by high levels of student awareness, motivation, and self-esteem as well as close relationships between institutions and formalized articulation agreements (Santiago, Tremblay, Basri, & Arnal, 2008). Articulation agreements aim to optimize the legitimate application of credit to recognize students’ previous formal learning. This process involves the linking of one qualification to another, often higher level qualification, and requires that an equivalence of content and learning outcomes be established (Australian Qualifications Framework Council, 2013). Appropriate recognition of prior learning (RPL) and the awarding of credit for previous study and experience underpin this system.
Articulated pathways are particularly common in nursing, where career advancement is often seen as being contingent on securing a baccalaureate qualification (Moodie, 2010; Ralph, Birks, Chapman, Muldoon, & McPherson, 2013). Nursing care in most Australian practice contexts is delivered by two levels of nurse—registered (RN) and enrolled (EN) nurses. Whereas the scope of practice and supervisory requirements of each role differ, both require registration with the Nursing and Midwifery Board of Australia (NMBA). The registered nurse practices both independently and as part of a multidisciplinary team (NMBA, 2006), whereas the enrolled nurse functions in an associate role, providing supervised nursing care as delegated by the registered nurse (Australian Nursing and Midwifery Council, 2002; Hutchinson, Mitchell, & St John, 2011).
In Australia, both enrolled and registered nurses were originally educated in hospital training schools where they were employed and paid as students, reflecting an apprenticeship training model. From the late 1970s, registered nurses commenced education in the tertiary sector with an initial qualification of Diploma, eventually becoming a baccalaureate qualification in the late 1980s (Russell, 1990). This move recognized the tension between the needs of the training hospital to provide patient care and the educational needs of the student nurse (Sellers & Deans, 1999). Changes in health technology and knowledge, consumer expectations, and evolving standards of nursing practice also fed the impetus for this change (Lindeman, 2000; National Nursing and Nursing Education Taskforce, 2006). The move to HE provided the expanded theoretical input that was not available in hospital training. Enrolled nurse education followed with the transition into the VET sector in the late 1990s (McKenna, Sadler, Long, & Burke, 2001), with both the Certificate IV and Diploma of Nursing endorsed as qualifications for registration as an enrolled nurse (Jacob, Barnett, Sellick, & McKenna, 2013). Since 2010, the minimum qualification for entry to the register as an enrolled nurse in Australia has been a Diploma of Nursing.
The 18-month Diploma of Nursing is a national qualification offered predominately in the VET sector. The qualification consists of 21 core Units of Competency (UoCs), plus five elective units. This package was designed to impart the necessary knowledge, skills, and professional attitudes described in the National Competency Standards for the Enrolled Nurse (Australian Nursing and Midwifery Council, 2002). The UoCs are largely consistent across Australia irrespective of VET institution. In contrast, the 3-year baccalaureate degree programs in nursing offered by HE institutions demonstrate greater variation in design and delivery (Ralph et al., 2013). These programs are subject to professional accreditation to ensure that students demonstrate achievement of the NMBA National Competency Standards for the Registered Nurse (2006).
When graduates with a Diploma of Nursing pursue RPL, the HE institution from which the student seeks that RPL makes decisions in respect of the awarding of credit. In the case of nursing, such decisions must comply with both institutional policies and the standards for accreditation established by the Australian Nursing and Midwifery Accreditation Council (ANMAC; 2012), the body endorsed by the NMBA to accredit nursing qualifications that lead to registration as a nurse. Significant differences exist in the structure, intent, and educational modalities between HE and VET sector organizations, making the process of determining and awarding credit particularly complex.
A recent Commonwealth-funded project undertaken by the Australian Nursing and Midwifery Federation (2014) sought to map articulation pathways in nursing. This project identified inconsistencies in the processes and amount of credit awarded to nurses who held a diploma qualification. Up to 1 year of credit (or equivalent) for entry into a nursing baccalaureate program was given in most instances (Australian Nursing and Midwifery Federation, 2014; Hutchinson et al., 2011), although anecdotal evidence suggests it could be as much as 18 months. This credit may be applied to all subjects in a single year or distributed across more than 1 year. Commonly, students transitioning with a diploma of nursing are only required to complete the final 2 years of a nursing degree program. The process is fraught with inconsistency and, despite the guidance provided by the Australian Qualifications Framework (AQF) and the respective accreditation standards, there appears to be little uniformity in how institutions facilitate articulation between the diploma and degree level programs.
A key challenge when awarding credit for students entering baccalaureate nursing programs is determining how their prior learning maps against the learning outcomes for that degree program. Most commonly, institutions directly map their degree program against the Diploma of Nursing to identify areas of overlap, usually requiring a minimum of 80% content alignment. This minimum is legitimate given that it is not necessary for content and learning outcomes to be exactly the same; rather, it is enough for the scope and focus of learning to be similar or comparable to support the awarding of credit (Australian Qualifications Framework Council, 2013). The direct mapping of the Diploma against the individual program involves considerable work for each university and requires that those allocating credit for prior learning have a detailed understanding of both their own degree program and the Diploma of Nursing. Assessment generally involves a superficial qualitative comparison of learning in specific areas, and may not appropriately measure depth of cognition or degree of exposure to a particular topic in a quantitative sense. This may expose the process of credit application to significant subjective interpretation and therefore variability. Diploma graduates may be given credit for a content area they have had some experience with, but not sufficiently to produce an equivalent depth of understanding to that of a baccalaureate student. As a result, students face further difficulties in what is already a challenging first year of study at university (Birks et al., 2013; Ralph et al., 2013).
The authors of this article sought to develop a method of identifying and mapping overlap between diploma and baccalaureate programs to address many of the shortfalls that exist in the current process. This need arises in the absence of existing work in the area. Considerable literature exists that explores various aspects of the transition of ENs to the RN role in Australia (see, for example, Cubit & Lopez, 2012; Kenny & Duckett, 2005; Nayda & Cheri, 2008; Ralph et al., 2013) and overseas (Gordon & Melrose, 2010; Hylton, 2005; Melrose & Wishart, 2013). This work primarily focuses on issues related to the experience of the transition process. Much work has also been completed in respect of the scope of practice of the enrolled nurse role (Corazzini, Anderson, Mueller, Thorpe, & McConnell, 2013; Cox & Prendergast, 2014; Hoodless & Bourke, 2009; Jacob et al., 2013; McEwan, 2008) and comparisons with the RN role (Chaboyer et al., 2008; Eagar, Cowin, Gregory, & Firtko, 2010; Jacob, Sellick, & McKenna, 2012). Two studies were identified that specifically explore the transition of enrolled nurses to baccalaureate programs in Australia (Hutchinson et al., 2011; Laming & Kelly, 2013; Pryor, 2012). Only one study was identified that compares enrolled nurse and registered nurse preparation in the current context (Jacob, McKenna, & D’Amore, 2014). No previous work has been identified in either the local or international literature that describes or explores processes associated with mapping curricula with the aim of facilitating the transition of diploma qualified nurses into baccalaureate programs of study.
Whereas the ultimate purpose of this study was to produce a software package to facilitate the process of mapping the Diploma of Nursing to baccalaureate nursing programs, the aim of the research described in this article was to produce a standardized framework that aligns these curricula and identifies where credit should be assigned for students moving through this pathway. This aim was achieved through the methods outlined in the following section with the outcomes described and discussed later in this article.
Method
Delphi is a systematic technique that seeks to obtain expert input using a series of evolving questionnaires while allowing for anonymity and asynchronous participation (Linstone & Turoff, 2011). The Delphi method is a widely accepted research technique (Landeta, Barrutia, & Lertxundi, 2011; Linstone & Turoff, 1975; Rowe & Wright, 2011), particularly in studies seeking to quantify consensus and dissensus on a given issue (Rowe & Wright, 2011). This study employed a modified Delphi approach to build a collaborative structural model. Structural models developed from an expert cohort allow the user to make subjective estimates about a problem (Linstone & Turoff, 2011). In this case, a structural model was developed with the intent of assisting the process of calculating credit between the Diploma of Nursing and the various baccalaureate nursing degrees offered across Australia. The actual process of using this structural model to translate learning achievements from the Diploma to credit in a baccalaureate nursing program is undertaken using a computer program developed specifically for this purpose. A detailed description of the functionality of that software program is the focus of a subsequent article.
Development of the structural model involved the mapping of diploma and degree programs to a common reference point. The common reference point chosen for this study was the National Competency Standards for the Registered Nurse (RN competencies). This project involved the mapping of the national Diploma of Nursing core Units of Competency to these RN competencies. This approach established a link between the diploma content and their potential contribution to student achievement of the RN competencies. Subsequently, each baccalaureate program team need only map their own program to the RN competencies to establish potential curriculum overlap with the diploma. This process enables the identification of baccalaureate program content that most closely resembles the learning achieved in the Diploma of Nursing. Credit can then be allocated where equivalence is identified.
Following approval to conduct the study from the university Human Research Ethics Committee, a two-phase study design was implemented. During the first phase, three consultants with recent experience in both the Diploma of Nursing UoCs and RN competencies produced a matrix proposing the potential contribution of the Diploma UoCs to the RN competencies. The matrix took the form of a two-axis table with the 21 core diploma UoCs on the vertical axis and the 45 RN competencies on the horizontal axis. The elective Diploma of Nursing UoCs were not mapped in the matrix given the significant variability across the 21 electives from which a student could choose. Simultaneously, the consultants indicated the cognitive developmental level expected to be reached using categories derived from those originally described by Bloom (1956). Two consultants worked together, and one independently to produce two draft matrices describing the potential contribution of the Diploma UoCs to the RN competencies. Members of the project team reviewed the matrices, and the more conservative of these was used in Phase 2 of the study.
The second phase employed a modified Delphi process. During this phase, a panel of experts examined the matrix developed in Phase 1. The aim of the second phase was to refine the quantitative association between the Diploma UoCs and the 45 standards that comprise the RN competencies to qualify consensus or dissensus. An acceptable panel size (Habibi, Sarafrazi, & Izadyar, 2014) of six was determined and senior nursing academics with expertise in nursing education at diploma or degree level, or both, were invited to take part. Participants were sought from various stakeholder groups in diverse locations, with the final sample being drawn from professional and accreditation organizations, registered training organizations, and universities across three Australian states.
Each member of the expert panel individually undertook the extensive task of reviewing the matrix developed during Phase 1, a process that took a number of hours. Expert panel members were asked to review the alignment between the UoCs and the RN standards and associated developmental level and indicate either agreement or non-agreement. Non-agreement was indicated by modification of the matrix. The returned matrices were collated using a count-based method. The count was converted to a common metric of study hours and the mean and range of responses were subsequently calculated. These data were then graphed for each of the RN standards. The resulting structural model (Figure 1) graphically displays the relative contribution of the diploma to each of the RN standards.

Structural model.
In response to expert panel feedback on the magnitude of the task, the planned second modified Delphi round was adjusted. Data from the first phase in conjunction with the draft structural model (Figure 1) were analyzed to produce a narrative abstract addressing each of the 10 RN competencies. These narratives were piloted and modified to form an abstract statement that reflected a summary of the findings from the first round. The resultant 10 “summary statements” are presented in Box 1.
Summary Statements.

Note. EN = enrolled nurse.
In the second modified Delphi round, the summary statements were returned to the expert panel with the draft structural model (Figure 1) showing mean responses and range. This was done using an online survey. Participants were asked to review each statement in conjunction with the associated segment of the graph and indicate their level of agreement on a 5-point Likert-type scale ranging from strongly agree to strongly disagree. Participants were also asked to make an open-text response to the statements and data if necessary. In preparation for determining level of consensus, and to increase sensitivity, the strongly agree and agree categories were collapsed into a % agree category, and the disagree and strongly disagree categories were collapsed into a % disagree category (Smithson, Birks, Harrison, Nair, & Hitchins, 2015). For the purpose of this study, a simple method of defining consensus was that which is greater than 80%, an approach supported by Hsu and Sandford (2007) and Von der Gracht (2012). Free-text comments were employed to assist in interpretation of quantitative responses. Consensus on all items was reached after two rounds.
It should be noted that the mapping process was complex and influenced by numerous factors. To promote validity and reliability in this process, progressive analysis was underpinned by three assumptions, all of which were disclosed to participants. First, 1 hr of student work (class time, assignment work, practical, etc.) in the Diploma of Nursing is equivalent to 1 hr of student work in a nursing baccalaureate. This assumption reflected the nominated contact hours in the Diploma of Nursing, the volume of learning of a diploma as described in the Australian Qualifications Framework (AQF), and current practice for the application of credit for the Diploma of Nursing in a nursing degree program in a majority of institutions. Second, where a diploma UoC contributes to more than one RN competency, its contribution was evenly distributed across any associated standards to a maximum of its associated contact hours. Third, all content in a UoC could potentially contribute toward credit in a nursing baccalaureate program.
A summary of the method used in this study is presented in Figure 2.

Study method.
Results
The following results describe the outcome of analysis of the diverse modified Delphi approach employed in this study. Participants’ opinion as to the relative contribution (in hours) of the Diploma of Nursing UoCs to the RN competencies is summarized in accordance with each of the 10 competency standards.
Competency 1
Standards within this competency relate to the requirement that the registered nurse “practices in accordance with legislation affecting nursing practice and health care.” The mean relative hourly contribution and the associated range for each standard, as reported by participants, are presented in Table 1.
National Competency Standards for the Registered Nurse—Competency 1.
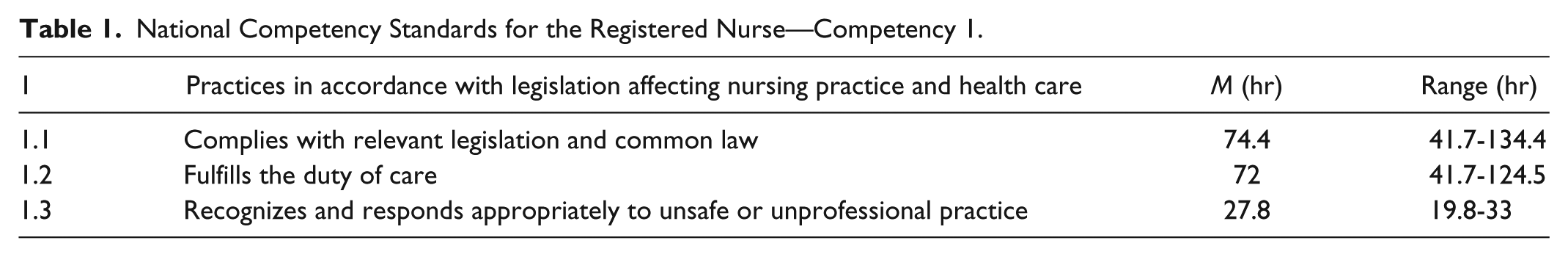
The data suggested variance of opinion about the contribution of the Diploma of Nursing to these standards, as evidenced by the large range for Standards 1.1 and 1.2, as well as a lack of concordance in the free-text responses for Standard 1.1 and 1.2: The Diploma of Nursing covers these elements, but with the resultant lower hours and content. I don’t think they have any less responsibility to report unsafe or unprofessional behavior. In some areas (aged care) . . . are key to this area due to lack of RNs. I think 1.1 and 1.2 are a bit low. RNs are required to respond appropriately to unsafe and unprofessional conduct. This is missing from EN programs although is a major professional problem with ENs recognizing problems but not having the confidence or understanding of how to deal with them.
Nevertheless, there seemed adequate concordance for Standard 1.3, reflected in the narrower range and free-text response: Certainly there is little direct evidence of competency standard 1.3 appearing overtly in the elements of the Diploma of Nursing.
Census was determined for Summary Statement 1 with 83.3% agreeing and 16.6% in disagreement.
Competency 2
Competency 2 contains standards that ensure that the registered nurse “practices within a professional and ethical nursing framework.” Table 2 presents the mean relative hourly contribution and range for these standards.
National Competency Standards for the Registered Nurse—Competency 2.

These data suggested less variance of opinion about the contribution of the Diploma of Nursing to these RN competencies, which was evidenced by the converging range and the universal (100%) acceptance of Summary Statement 2.
Competency 3
This competency recognizes the need for the registered nurse to demonstrate that he or she “practices within an evidence-based framework” (Table 3).
National Competency Standards for the Registered Nurse—Competency 3.

The data in Table 3 suggested limited variance of opinion about the extent that the diploma contributed to these standards, as evidenced by the converging range (compared with other competencies), universal acceptance of Summary Statement 3 and free-text responses: ENs often struggle to make connections between even minor research approaches and any aspect of practice. This is for me the most significant difference between programs of study. The term “relevance” could be looked at further. I would agree that there is less emphasis with regard to volume of content that appears in the elements of the Diploma of Nursing on the areas referred to. There is an elective unit: “HLTEN514B—Apply research skills within a contemporary health environment” that can be packaged into the Diploma of Nursing as part of the 5 electives required to achieve the qualification. This elective does relate to competency standard 3, but again the volume of content would be lower in comparison. I agree, but the use of evidenced based practice has improved and continues [to] increase in the curriculum.
Competency 4
Competency 4 seeks to ensure that the registered nurse “practices in ongoing professional development of self and others” (Table 4).
National Competency Standards for the Registered Nurse—Competency 4.
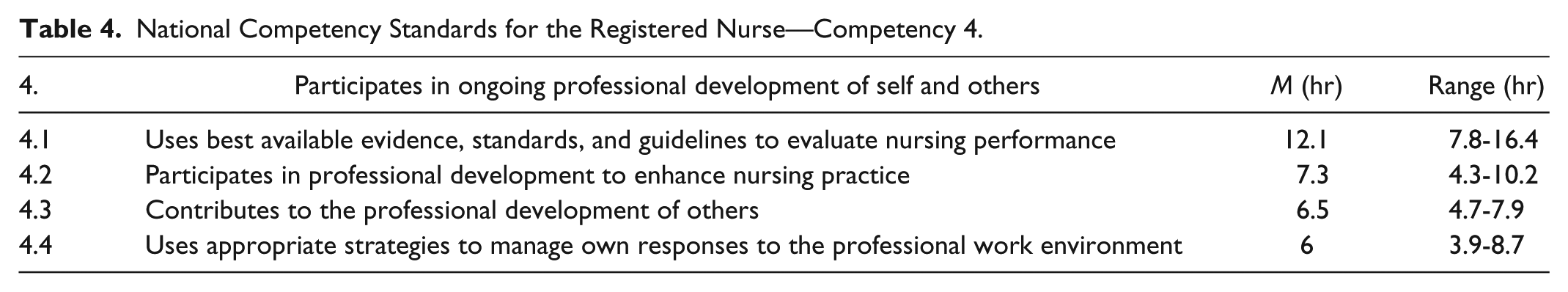
Limited variance of opinion is suggested by these data, an assertion further evidenced by the narrower range and universal acceptance of Summary Statement 4.
Competency 5
Standards contained in Competency 5 are focused on ensuring that the registered nurse, as an element of care coordination and provision, “conducts a comprehensive and systematic nursing assessment” (Table 5).
National Competency Standards for the Registered Nurse—Competency 5.

These data suggested some variance of opinion about the relative contribution of the diploma to the standards within this competency, but overall, there is general agreement. The variable range of contribution evidenced this conclusion across Competency 5 and an 83.3% acceptance rate of Summary Statement 5: Other than research the most glaring issue is that while [the] EN may have some older person assessment skills despite the emphasis noted above, there is a need for greater exposure and opportunity to consider broader concepts of nursing assessment.
Competency 6
Standards within Competency 6 address the requirement that the registered nurse “plans nursing care in consultation with individuals/groups, significant others, and the interdisciplinary health care team” (Table 6).
National Competency Standards for the Registered Nurse—Competency 6.

Less variance of opinion is suggested by the data in Table 6. The converging range and the universal acceptance of Summary Statement 6 further supported this assertion.
Competency 7
Competency 7 seeks to ensure that the registered nurse “provides comprehensive, safe, and effective evidence-based nursing care to achieve identified individual/group health outcomes” (Table 7).
National Competency Standards for the Registered Nurse—Competency 7.

These data suggested limited variance of opinion in respect of the contribution that the Diploma of Nursing made to the standards that fall within this competency. The tighter range (except for 7.1) supported this, as does the universal acceptance of Summary Statement 7 and the free-text response: 7.5 and 7.6 are appropriately identified as having minimal relationship.
Competency 8
Standards within this competency relate to the requirement that the registered nurse “evaluates progress toward expected individual/group health outcomes in consultation with individuals/groups, significant others, and interdisciplinary health care team” (Table 8).
National Competency Standards for the Registered Nurse—Competency 8.

These data suggested an acceptable variance of opinion evidenced by the converging range and an acceptance rate (83.3%) of Summary Statement 8. The one free-text comment in response to this competency suggested, This may be slightly overestimated in terms of significance.
Competency 9
Competency 9 contains those standards that dictate that the registered nurse “establishes, maintains, and appropriately concludes therapeutic relationships” (Table 9).
National Competency Standards for the Registered Nurse—Competency 9.

The data in Table 9 suggested limited variance of opinion in respect of the relative contribution of the Diploma of Nursing to this competency, as evidenced by the narrower range and broad acceptance of Summary Statement 9 (83.3%).
Competency 10
The final competency maintains that the registered nurse “collaborates with the interdisciplinary health care team to provide comprehensive nursing care” (Table 10).
National Competency Standards for the Registered Nurse—Competency 10.

Participants demonstrated limited variance of opinion about the contribution of the Diploma of Nursing to the standards contained in this competency. This conclusion was further evidenced by the converging range and universal acceptance of Summary Statement 10 (83.3%). As one participant indicated, I think this estimation is made more stark by the drive (slowly) towards a greater level of interdisciplinary communication and I would suspect future curricula will need to accommodate this.
Discussion
Articulated pathways increase accessibility to HE (Watson, Hagel, & Chesters, 2013). Individual institutions have the autonomy to award credit for prior studies and experience. Such decisions are often influenced by commercial and competitive factors, pedagogical rationales, professional judgment, and accrediting bodies. To some extent, these factors compete against one another. The process of awarding credit should be designed to build on existing skills and knowledge, reduce repetition of content, minimize the cost of gaining qualifications, and allow for successful transition through, and completion of, the new qualification. In the case of nursing, implementing a consistent and measurable approach to application of credit is difficult and involves significant professional judgment and interpretation, this complexity being a consequence of the diversity inherent in baccalaureate nursing programs across Australia (Ralph et al., 2013).
A standardized approach to the assessment and application of credit is essential to ensure it is awarded appropriately, recognizes prior learning, and positions the student to meet the required outcomes of successive qualifications. Indeed, Ralph et al. (2013) suggest that institutions are mandated to ensure rigor in this process. Both anecdotal and empirical evidence indicates that ENs making the transition to baccalaureate studies have difficulties with this process. Often these struggles relate to the technical aspects of the student role such as academic writing and computer literacy (Laming & Kelly, 2013), whereas specific subject matter such as science (Pryor, 2012) frequently presents a hurdle for students. Approaches to mapping programs of study such as the one described in this article have the potential to guide and influence the design or redesign of qualifications to properly support students in the articulation from one completed qualification to another. Furthermore, they enable universities to be responsive to student educational needs.
For participants in this study, it is likely that the more tangible aspect of the baccalaureate nursing curriculum is more easily measured and therefore responsible for the higher levels of agreement in respect of those content areas. For example, the relevance of research, evidence-based practice, evaluation of research evidence, patient assessment and the performance of procedures and activities often feature as easily identifiable elements in degree curricula. The standards that reflected these elements often enjoyed the highest levels of agreement and demonstrated narrower ranges in the study. Conversely, compliance with legislation and ethical and culturally appropriate practice is often ubiquitous and highly integrated throughout the program. These aspects of the role were therefore less easy to identify and quantify. The standards that reflected these elements had a broader range of responses in the findings presented.
The findings of this study provide a valuable summative overview of the relationship between the Diploma of Nursing and the expectations of the registered nurse role, through the prism of the RN competencies. These findings reflect the nature of the role of the enrolled nurse, both in theory (Australian Nursing and Midwifery Council, 2002) and in practice. In particular, subject matter relating to those elements of the role that address professional development of self and others, knowledge generation and application, policy and regulation, and decision making were found to have least emphasis in the Diploma of Nursing. Conversely, direct care activities such as assessment, documentation, establishing therapeutic relationships, and communication receive greater attention, as reflected in the relatively larger proportion of contact time. This finding is in conflict with Jacob et al. (2014) who found similarities in content between EN and RN preparatory programs. Those authors suggest that actual variation in the ability of graduates from each was more a result of factors such as the qualifications of educators and number of clinical hours. Recognition of these less tangible elements of the RN role supports the need for a holistic approach to the assessment and application of credit for those making the transition to this qualification through an articulated pathway.
The main limitation of this study was the small sample size. This sample does, however, reflect the limited number of individuals with the necessary expertise for a multifaceted study such as this. The resultant structural model provides a significant advancement toward a foundational framework. This framework will benefit from further research and testing, with a view to extending its functionality both within and beyond nursing education.
Conclusion
The untapped potential for articulated educational pathways to increase educational opportunities for those who would otherwise be denied access to HE is significant. Diversity of nursing curricula nationally serves numerous purposes, including providing variety for students and enabling universities to develop programs that meet the needs of the communities they serve. Whereas this diversity creates the potential for inconsistency in the awarding of credit for prior learning, the development of innovative approaches to mapping content and outcomes can assist in ensuring that students entering nursing programs from various pathways have the best chance of success. Ensuring an efficient and scaffolded progression from one qualification to the next is dependent on accurate and detailed mapping of both the qualitative and quantitative elements of the outcomes students are expected to achieve at each level of education. Engagement in the discussion about equivalence of outcomes from different programs of study is difficult in the absence of a framework that allows comparability. This article has described a study that sought to develop an evidence-based, structured approach to mapping the pathway from the national Diploma of Nursing to nursing degree programs across Australia. Future work in respect of extending and testing this framework will expand its potential both within nursing and other health care professions.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research and/or authorship of this article: This work was supported under the Nurse Pathways Project, managed by the Australian Nursing and Midwifery Federation (ANMF) on behalf of the Community Services and Health Industry Skills Council. This project was funded by the Commonwealth Government through the Department of Industry, as part of the Aged Care Workforce Innovation Project.
