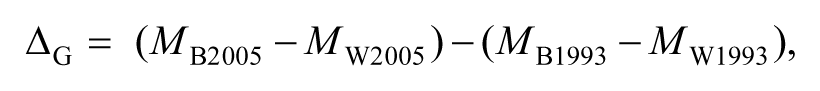Abstract
Our study aim was to determine whether local health department (LHD) services were associated with U.S. racial disparities in 1993-to-2005 mortality rates. In a national sample of LHDs, we examined 10 LHD service domains and gaps in Black–White all-cause mortality rates, drawing data from the National Association of County and City Health Officials’ National Profile of Local Health Departments surveys, as well as mortality and other public data files. Two service domains, maternal/child health and other activities, were significantly associated with decreases in the Black–White mortality gap for 15- to 44-year-olds. The health services domain approached significance in decreasing this gap. Screening was associated unexpectedly with a significant increase in the Black–White mortality gap for 15- to 44-year-olds. Selected LHD services that are provided directly to individuals and are allocated by need may have particular benefit for reducing Black–White mortality disparities for U.S. adults aged 15 to 44.
Keywords
Introduction
An emerging national Public Health Services and Systems Research (PHSSR) agenda in the United States recognizes the crucial role that local public health departments (LHDs) have in reducing disparities in morbidity and mortality in populations (Henry, Scutchfield, & Perez, 2008). LHDs are the governmental entities expected to conduct population-level activities that monitor differential rates of death, disease, and disability, and LHDs address disparities by assuring the availability of appropriate, effective, and accessible resources and services to vulnerable populations by creating healthy living conditions (National Association of County and City Health Officials [NACCHO], 2005b). These resources and services “vary tremendously” among LHDs (Erwin, 2008), have been changing dramatically in recent decades, and involve activities focused on prevention and delivered at a population level, as well as intensive direct services targeting groups at risk (E. L. Baker et al., 2005; Erwin, 2008; Henry et al., 2008; Thiede, Duchin, Hartfield, & Fleming, 2012).
In this era of public health system change, Black–White mortality disparities have also been changing. Harper, Lynch, Burris, and Davey Smith (2007) report that from 1983 to 1993, Black–White gaps in life expectancy were increasing, mainly from slower declines in heart disease among Blacks and greater increases in human immunodeficiency virus (HIV) and homicide, particularly among males aged 15 to 49. However, from 1993 to 2003, the Black–White mortality gap declined mainly because of rapid declines in HIV following widespread adoption of effective antiretroviral therapy as well as reductions in homicide and unintentional injuries, particularly among Black males aged 15 to 49. In the wake of great change among U.S. public health systems and in light of the critical role LHDs are expected to play in reducing health disparities, we know little about the relationship between LHD services and Black–White disparities in mortality (Bombard et al., 2012; Grembowski, Bekemeier, Conrad, & Kreuter, 2010)
Our study purpose was to examine whether changes in the breadth of specific population-level, screening, and direct LHD services over a 13-year period (1993-2005) were associated with changes in Black–White disparities in mortality.
Context
Recent U.S. changes in LHD service delivery are attributable to multiple historical forces. In 1988, the nation’s prestigious Institute of Medicine (IOM) produced the first of its public health reports proclaiming a “call to action” toward strengthening the public health system. This report sparked groundbreaking work that began to define public health practice, identify essential public health services, measure system performance, and develop a stronger evidence base for practice (IOM, 1988). During this period, new tools such as the National Public Health Performance Standards Instruments were developed for measuring public health agency performance, and the importance of PHSSR gained national attention (Scutchfield, Mays, & Lurie, 2009). Lenaway and colleagues (2006) suggest that the “pace of change” in public health practice in the United States further accelerated in the beginning of this century with the emergence of population health threats, such as an obesity epidemic and bioterrorism, and with related “dramatic shifts” in funding toward chronic disease programs, emergency preparedness activities, and enhanced epidemiological surveillance. These historical changes were also linked to a national trend in the United States toward placing a greater emphasis on population-level LHD activities, such as community assessment and health-promoting policy change, while decreasing the emphasis among LHDs on individually oriented “direct” clinical services (Keane, Marx, & Ricci, 2003; NACCHO, 2010). As a result of these systematic efforts to strengthen public health systems and external pressures with new demands, the activities of local public health agencies changed substantially, and a considerable variation in practice among the nation’s LHDs remains.
Service Breadth and Racial Disparities in Mortality
LHDs typically provide several domains of services, such as screening for diseases, maternal and child health promotion, and disease surveillance. In general, if the breadth of LHD service domains increased from 1993 to 2005, we might expect that Black–White disparities in mortality would subsequently decrease across LHDs. The underlying assumption is that services are more effective when they target the health needs of specific populations, and that LHDs that offer a greater breadth of comprehensive service are more likely to be successful in achieving their goals and reducing Black–White mortality gaps (Mete, Cioffi, & Lichtveld, 2003). In one national study, LHDs that conducted a community needs assessment in the last 3 years were more likely to provide a greater diversity of activities to reduce health disparities (Yang & Bekemeier, 2013). In another study, specific LHD revenues for the Special Supplemental Nutrition for Women, Infants, and Children (WIC) program—a program for which federal funding formulas dictate that services are delivered based on local need—showed that changes in local need were correlated positively with changes in LHD funding for WIC services provided (Bekemeier, Dunbar, Bryan, & Morris, 2012).
If service breadth is correlated positively with need and the services are effective, the services may impact racial health disparities in a variety of ways, but these relationships have not been well examined and remain poorly understood (Bombard et al., 2012). With a focus on primary prevention and health disparities, and by favoring population-based services over individually oriented services, LHDs tend to provide services benefiting populations of children and childbearing adults “upstream” in the life course trajectory. This focus is intended to reduce the “downstream” burden of disease and disability later in life and the disproportionate impact of this burden on the poor and among minority groups. LHD preventive services, therefore, ideally weaken the impact of poverty and race on increased mortality—particularly among populations during their working and childbearing years (Bombard et al., 2012). In their review of downstream disparities in health care, Franks and Fiscella (2008) argue that health disparities can be reduced by tailored program improvements and intensive outreach targeting specific groups at risk. In general, LHD direct services also have similar tailoring and outreach components, suggesting these focused activities might conceivably reduce premature mortality and disparities over the life course (White, 2009).
However, 1993-to-2005 changes in the breadth of services may be unrelated to 1993-to-2005 changes in Black–White mortality disparities for three reasons. First, sometimes LHD services are not allocated based on community needs (Bekemeier, Chen, Kawakyu, & Yang, 2013). Funding restrictions and legal programmatic mandates frequently trump factors such as research evidence and community needs in LHD resource allocations. Second, when performed correctly, a LHD’s community assessment and epidemiological services may be critical factors in reducing disparities by targeting services toward social groups with the greatest need. However, little is known about which LHD services favorably impact health outcomes for vulnerable populations, and consequently, practice-level decisions about prioritizing delivery of various types of public health services remain largely based on “conventional wisdom or expert opinion” (Van Wave, Scutchfield, & Honoré, 2010).
Third, when LHD services are not aligned tightly with community need, the expected relationships between service breadth and Black–White mortality disparities may erode through several mechanisms. LHD services that depend on voluntary participation may actually increase disparities because people with more resources and less need are more likely to take advantage of them (Link & Phelan, 2005; Starfield, 2007). White, Adams, and Heywood (2009) also note that LHDs may inadvertently introduce inequalities in service that result in increasing health disparities—for example, when socioeconomic variation is not identified during assessment of local need or when there is underestimation of risk in disadvantaged groups. For these reasons, it is unclear whether the expected associations exist between increased service breadth and reduced Black–White mortality disparities.
Method
Design and Sample
Secondary data, compiled from national U.S. data sets, were used in a time-trend ecologic study design to estimate the association between 1993-to-2005 changes in the breadth of LHD services and 1993-to-2005 changes in Black–White disparities in all-cause mortality rates for U.S. counties, controlling for other factors (Morgenstern, 1998). This research was approved by the study’s academic Institutional Review Board.
The primary sample consisted of 558 county or multi-county “common local areas,” or jurisdictions, with statistically measurable Black mortality, and with LHDs that responded to the NACCHO National Profile of Local Health Departments (Profile) surveys in both 1993 and 2005. Counties in the United States serve as relatively standard administrative subdivisions of a state. They typically have their own local government and often have their own LHD, serving as the administrative public health authority over the population in that geographic jurisdiction and with a governmental public health official providing leadership. Our study relied mainly on county-level data sources, and most LHDs had county jurisdictions (82.4%, n = 460 areas). If a county had two or more municipal LHDs, we aggregated the LHD data up to the county level (11.5%, n = 64 areas). If a LHD served multiple counties, we combined the county data to create multi-county LHD jurisdictions (4.8%, n = 27 areas). The remaining LHDs (1.3%, n = 7 areas) did not fit standard county or municipal designations, for example, a municipal LHD that crossed two counties or a county LHD that excluded a city LHD within its borders—these types of jurisdictions were combined into multi-county or county levels respectively. We gave the name common local areas to the jurisdictions that represented the universe of the county, multi-county, aggregated municipal LHDs, and other geographic regions that made up our sample. In the multivariate analyses, only common local areas with complete data over time were examined, which yielded a maximum sample of 423 areas.
Measures and Data Sources
Data from the Centers for Disease Control and Prevention (CDC) Wonder Database were used to measure county-level, all-cause, age-adjusted Black and White mortality rates in 1993 and in 2005 for the following population groups: (a) all-age Black residents, (b) all-age White residents, (c) 15- to 44-aged Black residents, and (d) 15- to 44-aged White residents. We chose mortality because few race-specific health measures existed at the county level. Our study is limited to Black–White racial disparities because data sources did not provide mortality rates for other racial groups at a similar level of aggregation across all U.S. counties. Annual Black mortality rates did not exist for counties with less than 20 Black deaths due to measurement unreliability. CDC Wonder also suppressed annual mortality rates for counties with less than 100,000 population and less than five deaths. We examined age 15-to-44 subgroups as previous studies indicate that this age group contains some of the biggest differences in Black and White mortality, while also being among the groups most likely to benefit from LHD investments (Grembowski et al., 2010; Harper et al., 2007).
Differences between the 2005 gap in Black–White mortality rates and the 1993 gap in Black–White mortality rates (the difference in annual differences, ΔG), were calculated as shown in the equation below (Grembowski et al., 2010):
where ΔG represents change in the mortality gap and M captures the mortality rate subscript by race and year.
Positive scores in the 2005-to-1993 difference in the annual Black–White gap indicated increasing disparity, while negative scores in the 2005-to-1993 difference indicated decreasing disparity. We also examined 2005-to-1993 changes in local mortality rates for each racial group to acknowledge race-specific mortality changes that might underlie changes in the above equation. Counties where Black mortality was lower than White mortality in both years (n = 47) were excluded, because our policy interest was the typical pattern of higher mortality in Black than in White populations.
Comparable data from the 1993 and 2005 NACCHO Profile surveys were used to measure breadth of LHD services provided directly by LHDs in each of 11 domains of service in 1993 and 2005 (see Table 1). Breadth of service in a domain was computed as the sum of the number of individual activity items arrayed in a specific domain, with 1 to 7 individual activities in each domain. Examples of the activities in each domain include Family Planning and Prenatal Care among the activities in the Maternal/Child Health domain and Vector Control and Groundwater Protection among the activities in Environmental Health. Domains were based on how activities were functionally grouped together in the 1993 and 2005 Profile surveys and reflect the typical array of types of services provided by a LHD (NACCHO, 2005a). Categorical measures were also created for each domain to depict whether the breadth of service increased, decreased, or stayed the same in 1993 to 2005. Some or all these service domains could be expected to contribute to the critical function that LHDs are expected to play in addressing health disparities (NACCHO, 2005b). The Profile surveys do not collect information about the amount of service delivered or number of clients served relative to a service activity or the activities within a service domain.
Number and Mean of Local Health Department Services by Domain (1993, 2005).

p < .1. **p < .05. ***p < .01.
We obtained data from the U.S. Census Bureau and the Bureau of Health Professions’ Area Resource File to measure five sets of contextual factors that were related to LHD performance, population health, or health disparities in prior studies (Hajat et al., 2009; Rajaratnam, Burke, & O’Campo, 2006; Robert & Reither, 2004). The first set of factors was county-level 1990-to-2000 changes in community characteristics: percentage of foreign born residents, of Black residents, and of residents with a high school diploma (Hajat et al., 2009; Rajaratnam et al., 2006; Robert & Reither, 2004).
A second set of factors measured 1990-to-2000 change in community disadvantage, using Robert and Reither’s community socioeconomic disadvantage index (SDI), or the sum of the percentage of county households on public assistance, of families below the county median family income, and of adults unemployed (Mete et al., 2003; Robert & Reither, 2004). A third set of factors represented change in countywide health resources or 1990 to 2005 change in density of nurses and primary care physicians (Bigbee, 2008).
A fourth set of variables were LHD characteristics that have been found to be associated with LHD performance and included governance by a local Board of Health (Mays et al., 2006; Mays & Smith, 2011), change in the number of full-time-equivalent (FTE) staff, and change in the discipline of the LHD lead executive (Bekemeier, Grembowski, Yang, & Herting, 2012; Bekemeier & Jones, 2010; Keane, Marx, & Ricci, 2001; Keane et al., 2003). We included number of FTEs as a measure of LHD size, supported by evidence that larger sized LHDs appear to have higher performance (Mays et al., 2006). The 1993 Profile data had substantial missing values in our sample (12.2%, n = 68 missing cases) for “number of FTEs,” and estimates were calculated for missing data based on jurisdiction size. The discipline of the lead executive was defined as a change in or maintenance of the type of lead executive as a clinician (i.e., nurse, physician, veterinarian, dentist) or non-clinician, measured through three binary (0,1) variables: (a) clinician executive in both Profiles, (b) change from 1993 clinician to 2005 non-clinician executive, and (c) change from 1993 non-clinician to 2005 clinician executive (omitted category: non-clinician executive in both Profiles; Bekemeier, Grembowski, Yang, & Herting, 2012; Bekemeier & Jones, 2010; Keane et al., 2001, 2003). Local Board of Health was measured by a binary variable coded 1 if the LHD was ever governed by a Board of Health in the 1993 or 2005 Profiles and 0 otherwise.
Last, we used the geographic 2003 Rural-Urban Commuting Area (RUCA) Code classifications for rural versus urban differences (Santerre, 2009). The seven RUCA categories were combined into three binary variables delineating large urban areas, medium-sized population areas with a large town of at least 10,000 persons, and small rural areas (Grembowski et al., 2010; NACCHO, 2007).
Analytic Strategy
We screened variables for outliers and general distribution and computed descriptive statistics for all measures. Correlations were also examined across domains and between service domains and local characteristics.
Regression models were estimated using general estimating equations (GEE) to adjust for clustering of local areas within federal regions. For each mortality measure, multiple regression models were estimated to determine if a 1993-to-2005 change in the breadth of a LHD service domain was significantly related to 1993-to-2005 change in mortality (as defined in the previous equation), while controlling for changes in other factors and rural–urban setting. We included all service domain measures in each model. The Immunization service domain, however, was omitted from the model due to lack of variation (almost all LHDs provided this service). We reviewed regression models for assumptions of linearity and homoscedasticity, and no violations were evident.
Results
The sample largely represented large urban areas (65.9%, n = 368) and 59 (10.6%) areas were small town rural jurisdictions (<10,000 residents). Locations in the southern U.S. were over-represented (see Table 2). Compared with the nation, our study’s “common local areas” at baseline had similar rates of unemployment and residents with high school diplomas, a smaller percentage of families with less than median family income, higher percentages of households on public assistance and of foreign born and Black residents, and greater densities of nurses and primary care physicians. Average mortality rates tended to be similar to the nation as a whole (see Table 3).
Distribution of Local Health Departments in Federal Regions, Characteristics of Communities, and Characteristics of the Local Health Departments.

Note. LHD = local health department; FTE = full-time-equivalent; MD = primary care physicians; RN = registered nurses; BSN = bachelor of science nurses.
Descriptive Statistics of 1993, 2005, and 1993-to-2005 Change in All-Cause, Age-Adjusted Mortality Rates per 100,000.

Overall, the mortality gap, or the differences in the annual 2005 and 1993 Black–White differences in mortality, was on average −82 for all-ages and −83 for 15- to 44-aged residents (see Table 3), with a median of −80 and −76, respectively, and both were normally distributed. Black–White relative rates changed in a similar pattern: The relative rates for all-cause/all age mortality declined from 1.31 (1236/942) to 1.25 (1075/863) from 1993 to 20015, and for all-cause/age 15 to 44 mortality from 2.24 to 1.71.
For the LHD service domains, the breadth of service in most of the domains changed significantly between 1993 and 2005 (Table 1). Maternal/Child Health (t = 15.216, p < .001), Health Services (t = 9.707, p < .001), Regulation (t = 5.699, p < .001), and Environmental Health (t = 9.123, p < .001) had significant decreases in breadth of service from 1993 to 2005. The breadth of service in the Epidemiology (t = −5.792, p < .001), Population-Based Primary Prevention (t = −4.463, p < .001), and Assessment and Planning (t = −3.352, p = .001) domains significantly increased by 2005. Pearson correlation tests indicated that domains of service were correlated significantly with each other, but all correlations were less than .5.
Among the 10 service domains examined in the regression analyses, only three were significantly associated with changes in the gap in Black–White mortality and only for 15- to 44-year-old residents (see Table 4). Two service domains, Maternal/Child Health and Other Activities, were significantly associated with a decrease in the Black–White mortality gap for 15- to 44-year-olds, although the association for Maternal/Child Health has marginal significance (p < .10). For example, Maternal/Child Health consisted of five activities (see Table 1); Table 4 associations (coefficients) imply that for each activity added to the breadth of Maternal/Child Health service in 1993 to 2005, the Black–White mortality gap narrowed by 11.407 deaths, controlling for changes in other factors. Increases in the breadth of Health Services (t = −1.37, p = .179) also approached significance with a decrease in the 15- to 44-year-old mortality gap. Screening was the only domain associated with a significant increase in the age 15 to 44 Black–White mortality gap.
Regression Coefficients Indicating the Associations Between 2005-to-1993 Change in the Breadth of a Service and 2005-to-1993 Change in Mortality for Black Residents, White Residents, and for the Black–White Mortality “Gap” (ΔG).

Note. The control variables in each model were 2000-to-1990 change in socioeconomic disadvantage index (SDI); 2005-to-1993 change in local health department (LHD) characteristics (full-time-equivalent staffs, Board of Health, Leadership—clinician vs. non-clinician); 2000-to-1990 change in community characteristics (% foreign born, % Black, % with high school diploma); 2005-to-1990 change in health care resources (MDs and RNs per 100,000 population); and geography (Rural-Urban Commuting Area (RUCA), Federal Region).
The number of areas in the sample reflects those areas with a sufficient population size and number of Black and White deaths in this age group to calculate an annual mortality rate.
p < .1. **p < .05. ***p < .01.
While the Health Services and Regulation domains were associated significantly with a decrease in all-age White mortality, no service domains were significantly associated with a change in all-age Black mortality. Correspondingly, no service domain strongly drove differences in the Black–White mortality gap for the all-age group.
An increase in breadth of Health Services (which included activities such as primary care, mental health services, and substance abuse care) was significantly associated with decreases in mortality for 15- to 44-year-old Black residents and for 15- to 44-year-old White residents. In each of two service domains, an increase in breadth was significantly associated with race-specific mortality increases for 15- to 44-year-olds that did not impact the mortality gap—Treatment and White mortality, Regulation and Black mortality.
Discussion
Our findings contribute to the small amount of existing literature examining whether public health systems contribute to improvements in population health and reductions in health disparities across social groups. In general, we found that 1993-to-2005 changes in the breadth of services in 10 LHD service domains were not associated with 1993-to-2005 changes in Black–White disparities in mortality for all ages. Two LHD direct service domains, however, were found to potentially contribute to reducing disparities in Black–White mortality rates for U.S. adults aged 15 to 44. Increases in the breadth of Maternal/Child Health services and Other Activities were each associated with decreases in the Black–White mortality gap for ages 15 to 44. Increases in the breadth of Health Services were associated with decreases in Black mortality and White mortality for ages 15 to 44 but did not close the Black–White mortality gap.
The expected, negative association for Maternal/Child Health is noteworthy because LHDs receive some Maternal/Child Health funds, such as for WIC, with funding formulas that explicitly require allocation of resources based on local need. Mete and colleagues (2003) and fundamental cause principles (Link & Phelan, 2005) suggest that when funding is not allocated relative to need, LHD services could potentially benefit wealthier populations with less need and, consequently, be less likely to close racial disparities in health. In terms of maternal and child health services, Bekemeier and colleagues (Bekemeier, Grembowski, et al., 2012) found that LHD-provided prenatal care and family planning services were associated specifically with reductions in Black–White mortality rate disparities.
Having a breadth of Maternal/Child Health and Health Services suggests that a wide range of direct services provided by LHDs may be markers for broader community-wide investment in a comprehensive safety net and/or early childhood development targeting social groups with high needs, which may ultimately yield long term health benefits. These more “traditional” direct services (such as maternal/child health activities, primary care, and school health) were likely in place among LHDs well before the 1993 Profile survey. Established and targeted community-wide investments such as these may have benefited children prior to 1993 and contributed to our findings for 15- to 44-year-olds over the life course—particularly in communities where impoverished, uninsured Black populations may have been more dependent on LHD than the White residents (Keane et al., 2003; U.S. Department of Health and Human Services of the Assistant Secretary for Planning and Evaluation, 2005).
LHDs providing Maternal/Child Health and Health Services also may produce health benefits through a variety of channels. The LHD Health Services domain, for example, includes activities such as “substance abuse services,” which have been found to reduce gun-related homicide rates (Cerda et al., 2010). LHD activities related to maternal and child health services may reduce neonatal and cardiovascular-related risk behaviors such as tobacco smoking (Reichman, Corman, Noonan, & Schwartz-Soicher, 2010).
We also found that Other Activities were significantly associated with a decrease in the Black–White mortality gap for 15- to 44-year-olds. This domain consisted of the following six heterogeneous activities: animal control, emergency medical services, occupational health services, occupation health laboratory services, school-based clinics, and school health. From 1993 to 2005, LHDs generally reduced Other Activities. Compared with the 1993 Profile, four of the six activities were less likely to be performed directly by LHDs in the 2005 Profile survey: animal control, occupational health services, school health, and school-based clinics (p < .01). This pattern implies that the Black–White mortality gap increased in LHDs that decreased the breadth (number) of these activities, but this association is probably not causal. Instead, LHD provision of all Other Activities in both 1993 and 2005 may simply be a proxy measure for LHDs that have greater resources, and that LHDs with greater resources may be more likely to reduce Black–White mortality gaps (Grembowski et al., 2010).
Many of the screening activities provided by LHDs during the study period were new or expanding (e.g., mammography promotion; Breen & Kessler, 1994), were focused on particularly vulnerable populations, and were intended to reduce morbidity and early mortality disparities from specific infectious (e.g., HIV/AIDs) and chronic diseases (e.g., cardiovascular disease, breast and cervical cancer) (Smith, Cokkinides, & Eyre, 2004). The positive relationship found between the breadth of screening activities and increases in Black–White 15- to 44-year-old mortality disparities during the study period may reflect a responsiveness of LHDs to expand their screening services in relation to advances in cancer and infectious disease screening, the HIV/AIDS epidemic, and local disparities that may have been identified as on the rise. Screening activities initiated in the 1990s may still ultimately reduce Black–White mortality disparities, but beyond the period we examined. This delayed population-level benefit from screening is supported by the review of chronic disease disparities intervention research by Franks and Fiscella (2008) and also by D. Baker and Middleton (2003) who found that increased, targeted cervical cancer screening provided in response to specific disparities did appear to ultimately reduce mortality disparities attributed to cervical cancer.
The lack of significant relationships identified between the Black–White mortality gap and population-level practice domains such as assessment and planning, epidemiology and surveillance, and population-based primary prevention in our study can conceivably be attributed to a combination of factors. These factors include the more recent emphasis of LHDs on these domains of practice, since the early 1990s, and the long trajectory for population-level and prevention interventions to impact distal mortality outcomes.
Compared with cross-sectional studies, time-trend designs can provide stronger evidence that changes in breadth of LHD services may be associated with changes in mortality disparities because alternative explanations for an observed relationship between change in service breadth and change in mortality rates are reduced (but not eliminated) in time-trend designs (Gordon & Heinrich, 2004; Morgenstern, 1998). Such associations are not evidence of cause and effect, however, and two-way causation may exist. This study also lacks information regarding the amount and quality of services provided by LHDs and how LHDs changed in the years between 1993 and 2005, as well as other unmeasured societal factors, such as racism, that differentially impact Black mortality rates. Further study with richer LHD service data (as they become available), proximal health indicators, and study designs with fewer confounders will allow for stronger inferences regarding the effects of specific public health services on population health and health disparities. The generalizability of these findings is also limited by the sample of jurisdictions, over representing the south and urban United States, and by the examination of only two racial groups.
Implications
The recent economic crisis and slow recovery has resulted in a much more “crippling” and sudden “elimination of essential public health services” (NACCHO, 2010). A NACCHO study indicated that the LHD program areas most affected by budget cuts in 2009 were population-based primary prevention, maternal and child health, clinical health, and chronic disease screening and treatment services (NACCHO, 2011). By 2012, these same services were among the program areas most likely to be still experiencing reductions or elimination (NACCHO, 2013). Studies examining previous economic crises indicate that such sudden and major budget cuts to public health programs and social policies may exacerbate health disparities (Edwards, 2008). We found that decreases in maternal/child health services were associated with increases in the Black–White mortality gap for 15- to 44-year-olds. These findings suggest that caution, assessment, and thoughtful planning are needed for services that comprise a community’s “safety net” and meet the needs of vulnerable populations (Jacobson, Dalton, Berson-Grand, & Weisman, 2005).
Our findings illustrate the complexities of identifying an effective constellation of LHD programs for reducing health disparities. It is likely that no one constellation exists, but rather effective public health practice is more nuanced relative to other local factors and existing capacity and closely tied to the health needs of social groups. Research is needed to monitor the outcomes of practice variation over time and to elucidate these nuances to reduce unnecessary variation, provide direction to practice, reduce health disparities, and avert unintended consequences from changes to services that could exacerbate health disparities.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research and/or authorship of this article: Funding support was provided from Pfizer Scholars Grants in Public Health to Professor Bekemeier.