Abstract
Many studies have investigated the efficacy of Endostar combined with transcatheter arterial chemoembolization (TACE) versus TACE alone for hepatocellular carcinoma (HCC). A systematic review was conducted to evaluate the efficacy of Endostar. PubMed, Embase, and other databases were searched, and meta-analysis was performed using RevMan 5.3 software. Nine studies, all of which were clinical randomized controlled trials, involving 411 participants were included. The overall response rate, disease control rate and α-fetoprotein negative conversion ratio, and the 6- and 12-month survival rate of HCC patients treated with combined Endostar and TACE were higher than those treated with TACE alone (P < .01). Furthermore, the incidence of tumor progression was low after Endostar treatment (P = .005). The incidence of adverse effects (leukocytopenia, liver function damage, and vomiting) was similar in Endostar with TACE and in TACE alone (P > .05). However, large studies and more randomized trials are necessary to determine the effects of Endostar on HCC.
Hepatocellular carcinoma (HCC) is among the primary causes of cancer-related deaths. Although some patients can be treated via surgical resection, which results in long-term resolution of clinical symptoms and long-term survival, 1 the majority are not eligible for surgery because of either the progressive nature of disease or other serious comorbidities. Transcatheter arterial chemoembolization (TACE) is the preferred and widely used interventional therapy for HCC patients who cannot receive radical surgery. Several research studies have proven that it can remarkably improve the short-term survival rate (SR) and the quality of life (QOL) of the patients. 2 In TACE therapy, chemotherapy (chemotherapy drugs plus lipiodol) and embolization have synergistic antitumor effects. Drug selection in traditional chemotherapy does not follow any uniform standard. At present, the primary chemotherapy drugs are categorized into the following: (a) doxorubicin-based drugs, such as Adriamycin (ADM) and pirarubicin (THP); (b) platinum-based drugs, such as cisplatin (DDP), carboplatin (CBP), and oxaliplatin (OXA); and (c) fluorouracil-based drugs, such as 5-fluorouracil (5-FU) and floxuridine (FUDR). Traditional chemotherapy uses 1 of these 3 chemotherapy drugs along with one or more other kinds of chemotherapeutics. The study by Poon et al 3 has statistically proven that triple-drug chemotherapy with embolization significantly improves tumor response and survival compared with single-drug chemolipiodolization with embolization in patients with either intermediate or advanced HCC. Thus, studies with 2 or more than 2 kinds of chemotherapy drugs in treatment were selected and divided into 2 groups: (a) fluorouracil and Adriamycin-based (FUDR and ADM-based) chemotherapy, which abbreviated as FA-based chemotherapy and (b) platinum and Adriamycin-based (DDP and ADM-based) chemotherapy, which abbreviated as PA-based chemotherapy.
Collagen XVIII is a protein located in most basement membranes in the body such as vascular basement membrane. 4 Meanwhile, endostatin is a peptide fragment with a relative molecular weight of 20 kDa that is cleaved by various proteinases from the C-terminal of collagen XVIII during proteolysis mechanisms. 5 Increasing studies have described the antiangiogenic activity of endostatin, and it was applied to tumor antiangiogenesis gene therapy recently. The antiangiogenic activity of endostatin can be estimated by several mechanisms, including inducing the endothelial cell apoptosis, inhibiting the proliferation and migration of endothelial cell, inhibiting the actions of angiogenic inducers, and inhibiting protease activity and the angiogenic signaling pathways. 6,7 Endostar (YH-16) is a novel recombinant human endostatin expressed and purified in Escherichia coli. It was approved by China’s State Food and Drug Administration for the treatment of non–small-cell lung cancer in 2005. 8 Recently, numerous studies have focused on applying Endostar in other solid tumors, such as hepatocellular carcinoma and nasopharyngeal carcinoma. 9 To date, several studies discussed the efficacy and safety of Endostar in treating advanced HCC. 10 –12 A reliable assessment of Endostar treatment in HCC is important and urgent. The current study presents a systematic review to quantify the toxicities and clinical benefits of Endostar combined with FA-based or PA-based TACE versus TACE alone for treating advanced HCC.
Methods
Search Strategy
Literature published in the databases of PubMed, Embase, Cochrane Library, Web of Science, Chinese National Knowledge Infrastructure, and Chinese biomedicine were searched electronically using free-word retrieval and Medical Subject Heading terms. The search strategy used the following main search terms in combination: terms that described the disease (“hepatocellular carcinoma” or “liver cancer” or “liver tumor” or “liver carcinoma” or “hepatic cancer” or “hepatic tumor” or “hepatic carcinoma” or “HCC”), treatment (“rh-endostatin” or “endostatin” or “YH-16” or “Endostar” or “recombinant human endostatin”), control treatment (“TACE” and “transcatheter arterial chemoembolization”), and the type of studies (“randomized controlled trials” or “RCT” or random*). The search period was from the start of each database up to December 31, 2016 without language restrictions. Moreover, other websites, such as http://scholar.google.com/, were researched for completed but not yet published studies. However, more studies in this category were not found. Furthermore, reference papers were also identified by personally contacting the authors using email and telephone as necessary.
Inclusion and Exclusion Criteria
The inclusion criteria were as follows: (a) patients with HCC without metastasis; (b) trials that compare Endostar combined with TACE to TACE alone; (c) chemotherapy drugs in the TACE that include at least 2 of the following three drugs: Adriamycin-based, platinum-based, and fluorouracil-based drug; (d) studies that report on at least 1 of the outcome indicators mentioned in the succeeding portion; and (e) studies with total number of cases greater than or equal to 40. Studies in which patients had comorbidities or additional treatments and with non-human trials were excluded. In addition, abstracts without full text, letters, expert opinions, reviews, conference abstracts without original data, and single case reports were excluded. Full-text papers that meet the inclusion criteria, and their references, were independently assessed by two reviewers, (Y-QZ and FZ). Disagreements were resolved by consulting with a third reviewer (LS).
Data Extraction
For each study, the following information were recorded: general information (title, author, year of publication, and study design), patient data (number, sex, age, Child-Pugh stage, and TNM grade), intervention data (the method and dose of chemotherapeutic drugs), and outcome data (overall response rate [ORR], disease control rate [DCR], survival rate [SR], tumor progression [TP], α-fetoprotein negative conversion ratio [AFP-NCR], and adverse effects [AEs], such as leukocytopenia, liver function damage, and nausea/vomiting). Data extraction was independently conducted by 2 reviewers using a standardized approach. Disagreement was adjudicated by a third reviewer after a review of the original publications.
Methodological Quality Assessment
The methodological quality assessment of the randomized controlled trials (RCTs) in the studies was done using the criteria from the Cochrane Handbook for Systematic Reviews of Interventions (version 5.3), including the following aspects: adequacy of the generation of allocation sequence, allocation concealment, blinding, and the presence of incomplete outcome data, selective outcome, or other sources of bias. The risk for each important outcome quality of trials was categorized into low risk of bias, unclear risk of bias, or high risk of bias. If lost cases appeared in the studies, then the intention-to-treat analysis was also performed.
Statistical Analysis
Dichotomous variables were analyzed by estimating odds ratio (OR) and risk ratio (RR) with a 95% confidence interval (CI) and calculated using the Mantel-Haenszel method. Heterogeneity was evaluated through chi-square (χ2) and I 2 tests. I 2 statistic values of 25%, 50%, and 75% can be interpreted as low, moderate, and high heterogeneity, respectively. When the heterogeneity was low, a pooled effect was calculated using the fixed effects model; otherwise, the random effects model was used. If data analysis reported significant heterogeneity, then summary results obtained from study subsets grouped according to the drug used were compared to explore the source of heterogeneity. Interaction tests were performed to compare the differences between two estimates, which were based on Student’s t distribution rather than on normal distribution because the number of inclusive studies was small. All values were 2 sided, and P < .05 was considered statistically significant. All statistical analyses were conducted using the Cochrane RevMan 5.3 software (Copenhagen: The Nordic Cochrane Centre).
Results
Included Studies
A total of 286 potentially relevant articles were searched, of which 228 were excluded by identifying titles and abstracts. Of the remaining 58 studies, 51 were excluded after strict screening because of the following reasons: limited cases (n < 40), repeat study, full text was not obtained, no controlled trials, required outcome indicators were not reported, only one kind of chemotherapy drug was used, unclear intervention, combination of other therapy, and incomplete data. Finally, 9 studies 13 –21 (7 in Chinese and 2 in English) published between 2009 and 2013 matching the inclusion criteria were included (Figure 1). Except 1 study, patient information was available in all other selected articles. Table 1 shows the baseline demographic factors of the patients. The eligible studies comprised 411 patients, 210 in the experimental group and 201 in the control group. The sample sizes varied between 20 and 60 patients, and the patient age ranged from 25 to 83 years. All studies were designed clinical RCTs of Endostar combined with TACE versus TACE alone for treating HCC. However, the type of interventions was categorized into 2 subgroups according to the different chemotherapy drugs used: (a) Endostar + FA-based TACE versus FA-based TACE alone and (b) Endostar +PA-based TACE versus PA-based TACE alone.

Flowchart of literature search of randomized controlled trials (RCTs).
Baseline Characteristics of the Studies Included in the Systematic Review.

Abbreviations: FA, fluorouracil and Adriamycin-based transcatheter arterial chemoembolization; PA, platinum and Adriamycin-based transcatheter arterial chemoembolization; M, mitoxantrone; H, hydroxycamptothecine; E, Endostar; NA, not available; KPS, karnofsky score.
Quality of Study
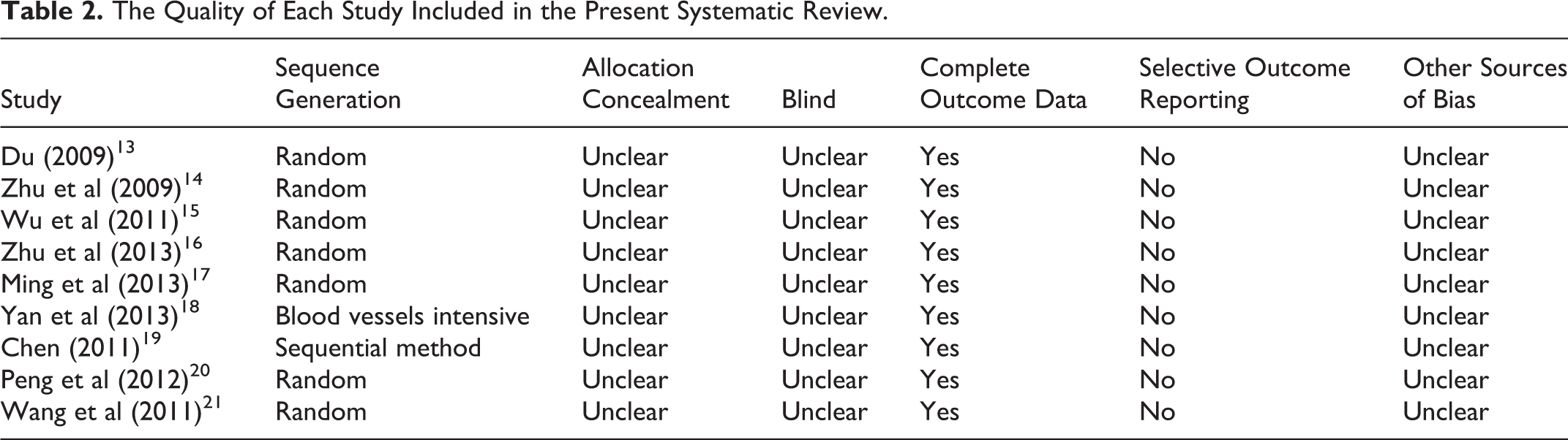
The included studies were assessed independently by two authors based on the criteria from the Cochrane Handbook for Systematic Reviews of Interventions (version 5.3). In terms of the generation of allocation sequence, all studies mentioned “random,” but only 2 articles described specific randomization methods. No studies mentioned blinding and allocation concealment. As the particularity of clinical RCTs, patients will be informed of all therapeutic measures before treatment. Blinding and allocation concealment are difficult to achieve in clinical practice. All studies had complete follow-up data of HCC patients. Eight papers did not report any funding and conflicts of interest. Table 2 shows the quality of each study included in the present systematic review.
The Quality of Each Study Included in the Present Systematic Review.
Comparison of Overall Response Rate (ORR)
All 9 studies had comparison data on ORR, which was divided into two subgroups, namely, FA-based TACE and PA-based TACE, according to different chemotherapy regimens. The meta-analysis result showed that OR = 3.26 (95% CI = 2.14-4.95); test for heterogeneity = 3.88; and I 2 = 0%. The ORR of Endostar combined with TACE for treating HCC was significantly higher than that of TACE alone, and the difference was statistically significant (P < .00001) (Figure 2). Although all the included studies were small sample trials, the sensitivity analysis was considered. The heterogeneity test results of the 2 subgroups both showed P > .05, I 2 = 0%. Finally, fixed effects model was chosen. However, the differences noted between the 2 subgroups must be verified in more large-sample studies.

Comparison of ORR between Endostar combined with TACE and TACE alone. ORR, overall response rate; TACE, transcatheter arterial chemoembolization.
Comparison of Disease Control Rate (DCR)
As shown in Figure 3, out of the 9 published studies, three had comparison data on DCR. The results of the fixed effects model showed that the OR was 3.50 (95% CI = 1.51-8.11). The DCR of Endostar combined with TACE for treating HCC was significantly higher than that of TACE alone, and the difference was statistically significant (P = .003).

Comparison of DCR between Endostar combined with TACE and TACE alone. DCR, disease control rate; TACE, transcatheter arterial chemoembolization.
Comparison of AFP Negative Conversion Ratio (AFP-NCR)
Three studies compared the AFP-NCR between Endostar combined with TACE and TACE alone, and their chemotherapy measure all belong to FA-based TACE. The RR was 1.81 (95% CI, 1.15-2.85) and test for heterogeneity: I 2 = 0%; test for overall effect: Z = 2.56, P = .01. The AFP-NCR of Endostar combined with TACE for treating HCC was higher than that of TACE alone, and difference was statistically significant (Figure 4).

Comparison of AFP-NCR between Endostar combined with TACE and TACE alone. AFP-NCR, α-fetoprotein negative conversion ratio; TACE, transcatheter arterial chemoembolization.
Adverse Reaction (AE) Analysis
The included studies assessed 10 severe AEs, the most common being gastrointestinal reactions, hepatic and renal function, and hematologic diseases. Four studies, 3 of which belong to the PA-based TACE and 1 belongs to the FA-based TACE, compared leukopenia between patients treated with Endostar combined with TACE and TACE alone. No difference in leukopenia incidence was found between Endostar combined with TACE and TACE alone (OR = 1.19; 95% CI = 0.58-2.44; P = .40) (Figure 5). Random effects model was chosen because all studies had small sample sizes. Similarly, no significant differences in incidence and severity were found between Endostar combined with TACE and TACE alone (Figure 6) in 4 studies comparing hepatic function damage (OR = 0.91; 95% CI = 0.49-1.71; P = .79) and in 4 studies comparing nausea/vomiting (OR = 1.00; 95% CI = 0.51-1.97; P = .46) (Figure 7).
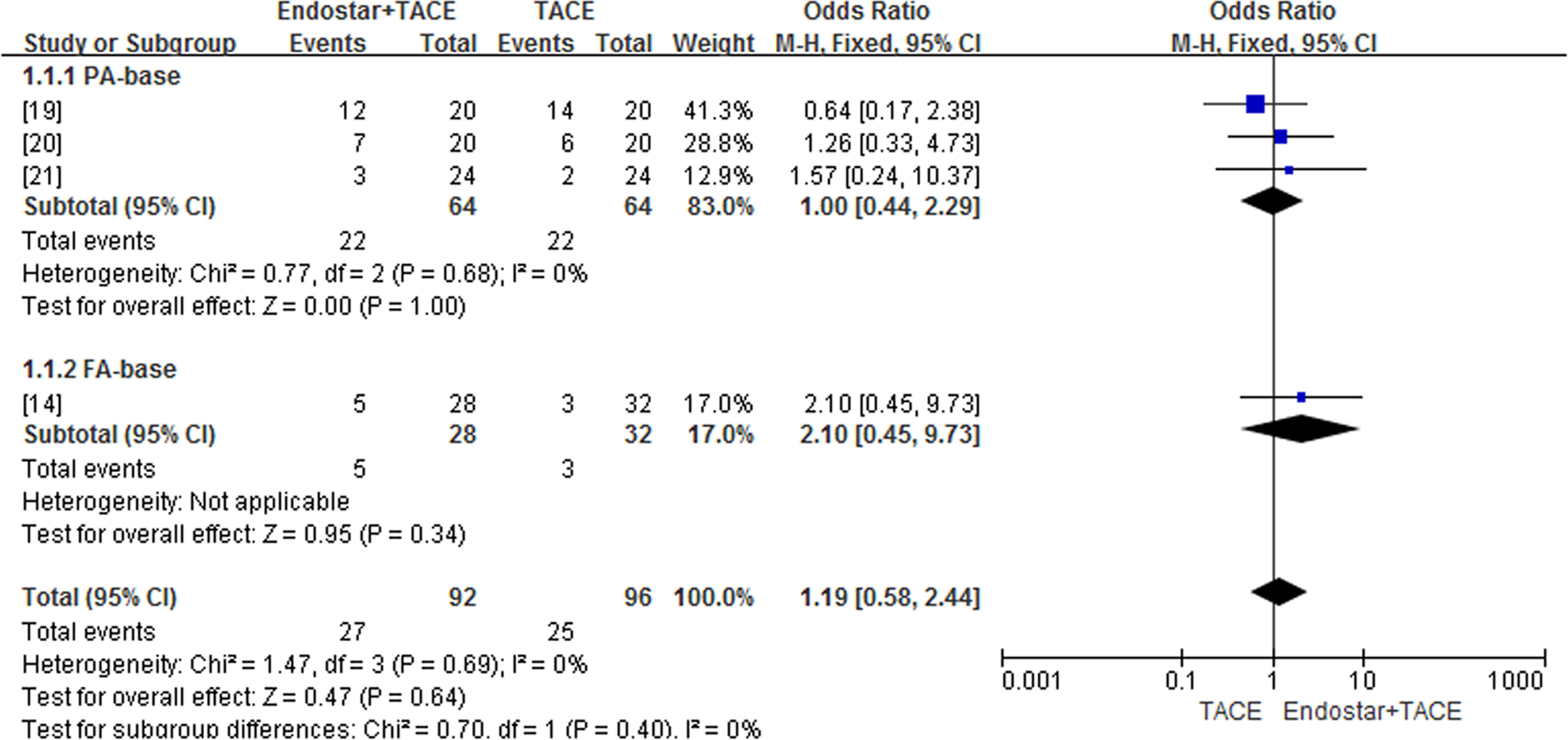
Comparison of leukopenia incidence between Endostar combined with TACE and TACE alone. TACE, transcatheter arterial chemoembolization.
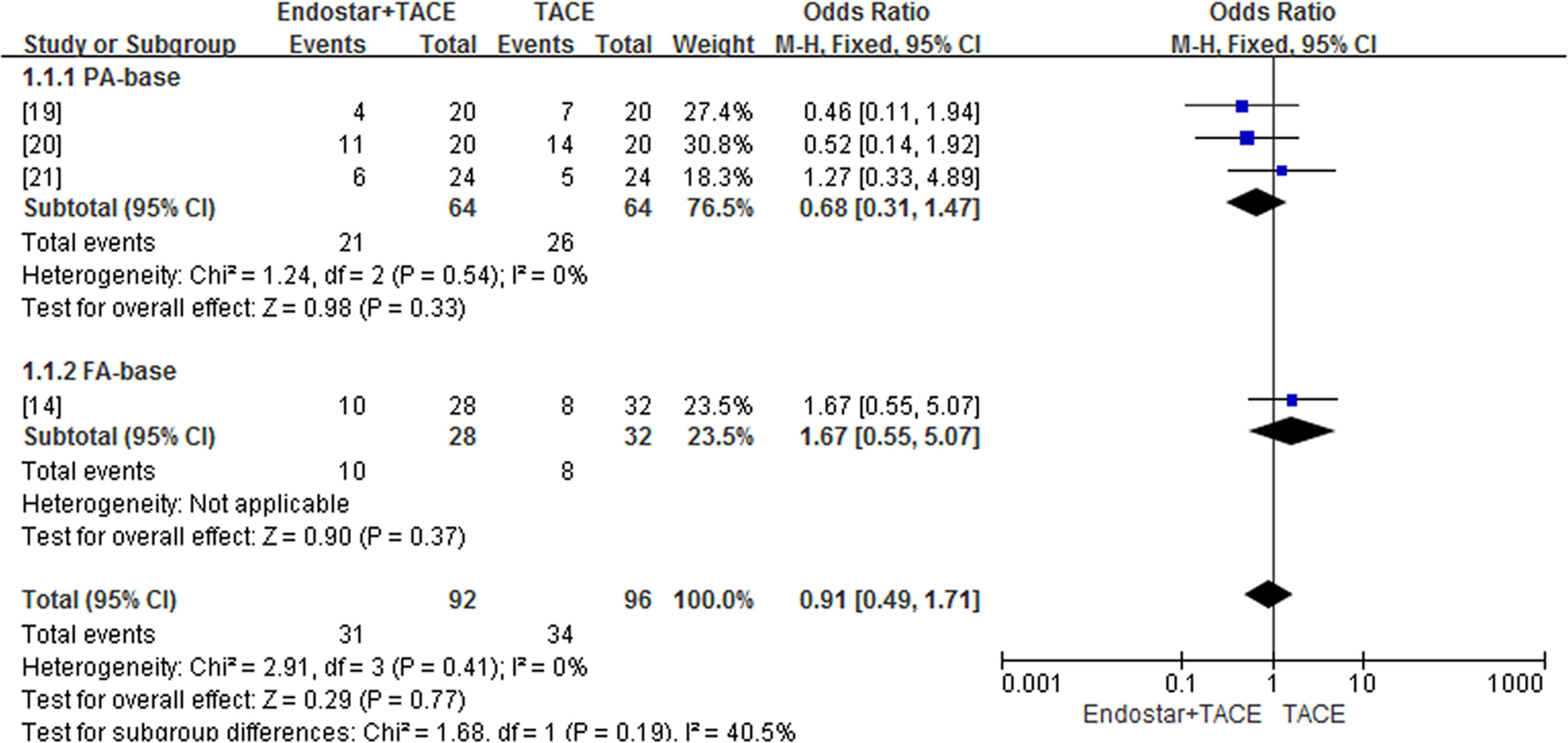
Comparison of hepatic function damage between Endostar combined with TACE and TACE alone. TACE, transcatheter arterial chemoembolization.

Comparison of nausea/vomiting between Endostar combined with TACE and TACE alone. TACE, transcatheter arterial chemoembolization.
Comparison of Tumor Progression (TP)
Two studies reported that tumor angiogenesis was revealed through digital subtraction angiography examination 6 months after treatment. Random effects model was chosen to combine the effect size. The analysis results show that OR is 0.14 (95% CI = 0.03-0.54; P = .005). The TP of Endostar combined with TACE for treating HCC was significantly lower than that of TACE alone, and the difference was statistically significant (Figure 8).

Comparison of tumor progression between Endostar combined with TACE and TACE alone. TACE, transcatheter arterial chemoembolization.
Comparison of Survival Rates (SR)
Two studies, both belonging to PA-based TACE, reported the number of patient who survived 6 months after treatment A fixed effects model was used, and the analysis results show OR is 3.58 (95% CI = 1.10-11.70; P = .03) (Figure 9). The 6-month survival rates of Endostar combined with TACE for treating HCC was significantly higher than that of TACE alone, and the difference was statistically significant. Another 2 studies reported the number of patient who survived 12 months after treatment. The analysis results show OR is 2.94 (95% CI = 1.09-7.93; P = .04) (Figure 9).

Comparison of SRs between Endostar combined with TACE and TACE alone (1.1.1. 6 months SR; 1.1.2. 12 months SR). SR, survival rate; TACE, transcatheter arterial chemoembolization.
Discussion
As a new type of antiangiogenesis drug, an increasing number of researchers have been concerned with the role of Endostar in recent years; several studies have reported on the efficacy and safety of Endostar in the treatment of solid tumors. 22 This systematic review was performed to better quantify the benefits and adverse effects of Endostar combined with TACE versus TACE alone for treating advanced HCC. In this review, 9 clinical randomized trials were identified. Four studies were based on FA (5-FU and ADM/THP) chemotherapy TACE, whereas the other 5 were based on PA (DDP/OXA and ADM/THP) chemotherapy TACE. A significant benefit of Endostar plus TACE in ORR was found (OR = 3.26). Data analysis in these 2 subgroups shows that they have less heterogeneity (I 2 = 0%). However, the differences between the 2 subgroups have to be verified in more large-sample studies. In 3 of the selected studies, the DCR and AFP-NCR in the Endostar plus TACE groups was higher than that in TACE alone, and the difference was statistically significant (P < .01). In addition, the TP of Endostar combined with TACE for treating HCC in 6 and 12 months after treatment was significantly lower than that of TACE alone (P < .01). Analysis results indicated that the Endostar combined with TACE group has a higher survival rate than that of the TACE alone group, and the difference was significant (P < .05). However, only 4 trials providing relative data were included, which were insufficient to reach a decisive conclusion. Therefore, more research is required to better understanding the probability of Endostar with TACE being better in treating HCC. The AEs found in the present review were mainly leukocytopenia, liver function damage, and nausea/vomiting. The results supported that AEs were similar in Endostar combined with TACE and in TACE alone. No significant differences were found in the incidence of all 3 AEs between the 2 groups (P > .5). Whether Endostar combination could relieve the AEs of treatment should be assessed in future studies. Overall, these results indicate that the potential benefit of Endostar may be widely applicable to a patient population closely resembling clinical characteristics of advanced HCC.
Considering the quality of the evidence in included studies is one of the most important aspects of systematic reviews. Bias might affect the conclusions of the meta-analysis, and bias reduction depends on the experimental design. Moderate bias likely occurred in the nine included studies. They are all clinical RCTs, and only 2 studies reported a specific method of random allocation. Total randomization, blinding, and allocation concealment is difficult in clinical research because of the characteristics of surgical tumor treatment. As such, the biases in the included research were acceptable in drug treatment for clinical cancer studies. Funnel chart showed that certain publishing bias occurred. More clinical studies with RCTs are needed to provide sufficient supporting evidence.
In this review, the included studies were carefully assessed, and the heterogeneity of different chemotherapy regimens was considered. However, some deficiencies in the present meta-analysis were found. First, the quality of subgroup analysis according to the different agents (Endostar plus TACE compared with TACE alone) was lacking because the subgroup data (eg, age, sex, Child-Pugh stage, TNM grade, and QOL) were only from a few trials. The number of studies with subgroup analysis was limited and insufficient to reach a definite conclusion. Second, the number of available cases was relatively small, and most of the included studies were published in Chinese, with heterogeneous data and analysis methods (eg, different methods for tumor classification were used for assessment). In addition, the benefit of chemotherapy in incurable cancers needs to be assessed directly through validated health-related QOL instruments rather than only inferred from ORR, DCR, SR, and other traditional endpoints. 23 However, the studies included in this review lacked related indicators, such as QOL and MST. Meanwhile, other indicators, such as SR, TP, AFP-NCR, and AEs, have been reported but not detailed data in every article. Although such studies were reported to be of low quality, they still provide credible evidence regarding the efficacy of Endostar combined with TACE. However, more RCTs are needed to confirm that Endostar combined with TACE is better than TACE alone.
Conclusion
The results showed that Endostar combined with TACE was associated with high ORR, DCR, and AFP-NCR as well as superior SR (6 and 12 months) profiles compared with TACE alone. Moreover, AEs in Endostar combined with TACE was shown to be similar with that in TACE alone. Endostar combined with TACE exhibited superior efficacy and safety in antiangiogenic therapy compared with TACE alone in tumor therapy. However, several issues regarding Endostar, as a new strategy, still need to be resolved in further studies. The notable efficacy and antiangiogenic activity of Endostar in combination with TACE suggest that this regimen may have a value in the treatment of previously untreated patients, including those who cannot tolerate more aggressive therapies, such as surgery. However, confirmation of these conclusions in rigorously controlled randomized trials with large sample is required before definite conclusions about this therapy can be drawn.
Footnotes
Acknowledgments
Our sincere appreciation goes to the Evidence-Based Medicine Center, School of Basic Medical Sciences, Lanzhou University, Lanzhou, China.
Author Contributions
YQZ contributed towards conception of study design, literature retrieval, data extraction and analysis, statistical analysis, manuscript writing and editing. FZ contributed towards conception of study design, literature retrieval and literature screening, data extraction and analysis, statistical analysis, manuscript writing and editing, and manuscript revision/review. LS contributed towards conception of literature screening and statistical analysis. HYG contributed towards conception of data extraction and analysis. XFX contributed towards conception of data extraction and analysis.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the Science Technology Project of Lanzhou City (Nos.2016-3-37; 2015-3-132) and the Fundamental Research Funds for the Central Universities of Northwest Minzu University (No.31920140070;31920160009;31920150045).
Ethical Approval
The project received approval from the School of Medicine, Northwest Minzu University, Lanzhou, China.
