Abstract
Transcatheter arterial chemoembolization (TACE) has become one of the first-line standard treatments for intermediate-advanced hepatocellular carcinoma, as well as an effective treatment for metastatic hepatic carcinoma. The majority of TACE-related complications are mild and acceptable to patients. Compared with conventional (C)-TACE, drug-eluting bead (DEB)-TACE allows permanent embolization of blood vessels, a slow continuous release of anti-tumour drugs in a locally targeted manner, and reduction of the systemic release of anti-tumour drugs, so that their adverse effects are significantly reduced. The general consensus is that DEB-TACE is safer and better tolerated by patients than C-TACE because serious complications after DEB-TACE are rarely reported. This current case report describes a rare case of diffuse biliary peritonitis secondary to rupture of a hepatic tumour after DEB-TACE. After the procedure, the patient presented with progressively worsening upper abdominal pain. As conventional management methods for the suspected tumour rupture failed, an emergency laparotomy was performed to remove the metastatic mass of differentiated hepatic adenocarcinoma. The patient remains under surveillance with no further complications. In our opinion, although DEB-TACE is safe and rarely has serious complications, caution should be exercised when this method is used to treat tumours that are located close to the liver surface.
Keywords
Introduction
With the increasing incidence of primary and metastatic tumours in the liver, the clinical application of transcatheter arterial chemoembolization (TACE) has increased. 1 It has become one of the first-line standard treatments for intermediate-advanced hepatocellular carcinoma, as well as an effective treatment for metastatic hepatic carcinoma. 2 Compared with traditional surgical treatment methods, TACE has the advantages of causing less trauma, fewer complications and having good patient tolerance; and is one of the most effective treatment methods for primary and metastatic tumours of the liver. 2 The incidence of minor complications after TACE is 10–12%,3,4 while that of serious complications is 2.6–5.3%,3,5 and the mortality rate is 0.5–4.1%.6,7 It is reported that the incidence of rupture of hepatic tumours after conventional (C)-TACE is 0.1–1.5% and the main clinical manifestation after the rupture is haemorrhagic shock due to intra-abdominal haemorrhage.5,6,8 Drug-eluting bead (DEB)-TACE is a new type of drug-eluting embolization and is believed to have higher safety and patient tolerance than C-TACE. 9 Therefore, reports of serious complications after DEB-TACE are rare. 3 This current case report describes an extremely rare case of diffuse biliary peritonitis secondary to the rupture of hepatic tumours after DEB-TACE.
Case report
A 64-year-old male patient was diagnosed with antral gastric cancer by gastroscopic biopsy and underwent radical gastrectomy (total gastrectomy + D2 lymph node dissection + Roux-y oesophagojejunostomy) on 14 May 2015 at the Department of Hepatobiliary Surgery, Beilun District People's Hospital, Ningbo, Zhejiang Province, China. Pathological examination after radical gastrectomy revealed an ulcerated adenocarcinoma, with moderate to highly differentiated adenocarcinoma in some parts of the specimen (approximately 70%) and moderate to slightly differentiated adenocarcinoma in other parts (approximately 30%), and a small amount of neuroendocrine differentiation and lymph node metastatic carcinoma (lymph node metastasis in five out of 25 specimens). After surgery, the patient underwent chemotherapy with 120 mg tegafur, gimeracil and oteracil potassium capsule twice daily, oral administration, repeated every 3 weeks, for 12 months and was followed up, showing normal levels of carcinoembryonic antigen (CEA) (<5 ng/ml) and carbohydrate antigen (CA) 19-9 (<37 U/ml).
On 10 May 2018, a mass in the upper abdomen, approximately the size of a small egg, was detected. A plain magnetic resonance imaging (MRI) scan, a diffusion-weighted MRI scan and a contrast-enhanced MRI scan of the upper abdomen revealed an abnormal signal lesion (43 mm × 40 mm) in the left lobe of the liver. The lesion had low T1-weighted signals (Figure 1a) and slightly higher T2-weightedsignals (Figure 1b), with a longer T2 signal shadow appearing at the centre of the lesion. Diffuse-weighted imaging signals of the lesion were high and the internal signals were homogeneous with a clear boundary. Progressively enhanced signals were observed in contrast-enhanced MRI, indicating that a space-occupying lesion was present in the left liver lobe, and that the likelihood of the lesion being a metastatic tumour should be considered first. Tumour marker analysis revealed the following: CEA, 24.4 ng/ml and CA 19-9, 1555.15 U/ml. The liver and kidney functions were normal, with cirrhosis of Child-Pugh class A.

Magnetic resonance imaging scans of the upper abdomen of a 67-year-old male patient revealed an abnormal signal lesion (43 mm × 40 mm) in the left lobe of the liver. The lesion had low T1-weighted signals (a) and slightly higher T2-weighted signals (b).
The patient refused surgery, so TACE was performed on 6 July 2018 after two rounds of chemotherapy with the XELOX regimen (3000 mg capecitabine tablets, oral administration 1–14 days, twice daily, repeated every 3 weeks; 190 mg oxaliplatin, intravenous administration on day 1, repeated every 3 weeks) conducted on 22 May 2018 and 12 June 2018, respectively. The TACE procedure was as follows: the Seldinger technique was used to puncture the right femoral artery for catheterization and digital subtraction angiography (DSA) of the celiac artery showed a slight thickening of the left hepatic artery. In the parenchymal phase, nodular tumour staining in the left lateral section of the liver was observed (Figure 2a). Super-selective catheterization with a 3F microcatheter was performed on the tumour artery in the left lateral section of the liver; and 10 mg dexamethasone and 5 mg tropisetron diluted with 100 mg oxaliplatin in a total volume of 50 ml were injected through the catheter for left-lobe and right-lobe perfusion. Gelatin sponge strips were used for protective embolization of part of the vascular branches in the left lateral section of the liver. After Dyna-CT (Siemens Medical Solutions, Malvern, PA, USA) computed tomography (CT) scanning confirmed the tumour-feeding artery and its staining, embolization was performed with 100–300 μm CalliSpheres® drug-eluting beads (loaded with 80 mg epirubicin; Suzhou Hengrui Jialisheng Biological Medicine Technology, Suzhou, China) in a total volume of 10 ml, after which DSA was conducted again to reveal that the staining of the left lobe tumour had disappeared (Figure 2b). DSA and Dyna-CT scanning after a second super-selective catheterization in the vascular branches in the left lateral section of the liver showed no other vascular branches feeding the tumour, and therefore, the surgery was terminated.

Digital subtraction angiography showed significant nodular tumour staining in the left lateral section of the liver (a); and the disappearance of the tumour vascularity confirmed complete tumour embolization following transcatheter arterial chemoembolization using 100–300 µm CalliSpheres® drug-eluting beads (b).
On the first day after DEB-TACE, the patient felt a slight dull pain and discomfort in the right upper abdomen. On the 4th day after surgery, he felt gradually increasing abdominal pain and bloating, and there was a low fever. Physical examination revealed that the patient showed a painful acute sickly appearance and suffered from total abdominal tenderness with rebound pain, and the pain was obvious in the upper abdomen, with tense abdominal muscles and negative shifting dullness. Abdominal CT examination revealed that there were flake-like mixed-density shadows in the left lobe with visible gas shadows inside (Figure 3a). A few arch-shaped liquid density shadows were observed under the capsule of the liver, with a small amount of free gas shadows in the abdominal cavity at the leading edge of the liver (Figure 3b). Considering tumour rupture with peritonitis, symptomatic treatment was administered to the patient, which included fasting, gastrointestinal decompression, anti-inflammatory drugs, inhibition of digestive gland secretion and fluid infusion. However, this treatment was not effective and the patient showed progressive abdominal pain accompanied by high fever. On 11 July 2018, the patient underwent emergency laparotomy, in which the abdominal cavity and pelvic cavity were found to contain approximately 800 ml of yellow turbid liquid and the left lateral section of the liver contained a tumour mass measuring approximately 4.5 cm × 4.0 cm with a soft texture. On the surface of the tumour, there was a gap with a diameter of approximately 1 cm, with bile flowing out of the gap (Figure 4a and 4b). Therefore, left hepatic lobectomy was performed. Postoperative pathology revealed the occurrence of invasion/metastasis of differentiated adenocarcinoma in the left lateral section of the liver (Figure 5a and 5b). Immunohistochemistry revealed the following: CEA (+), cytokeratin (CK) 19 (+), CK7 (+), CD34 (vascular +), alpha-fetoprotein (–), hepatocyte (–), CK20 (–) and chromogranin A (–). The patient recovered satisfactorily after surgery and was discharged from hospital. The patient underwent treatment with the XELOX regimen as described above four times after surgery. The patient is still under follow-up without signs of recurrence or metastasis.
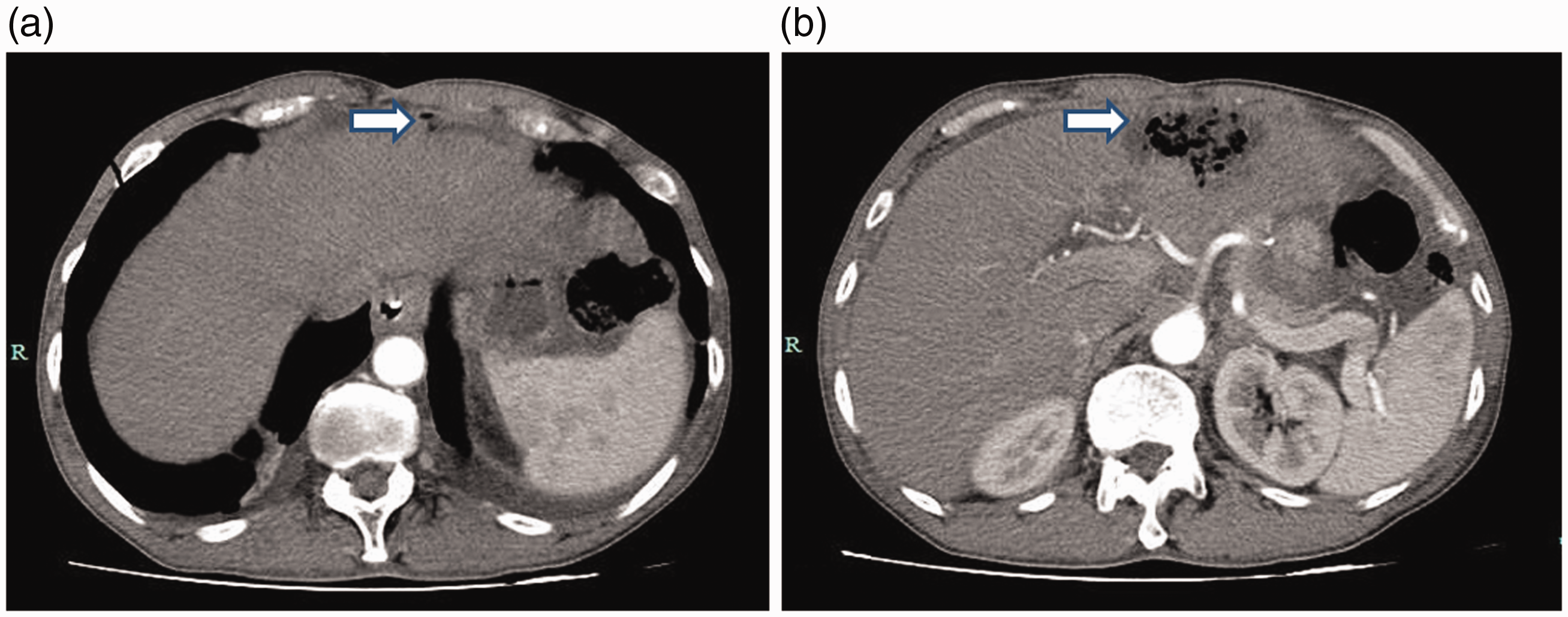
Preoperative axial contrast-enhanced computed tomography (CT) scan images of the abdomen. (a) The left lobe of the liver shows elliptical low-density shadows with visible gas shadows inside. Signals are not obviously enhanced in the contrast-enhanced CT. (b) A few arch-shaped liquid density shadows are seen in the liver, with a few free gas shadows appearing at the leading edge of the liver (white arrow).
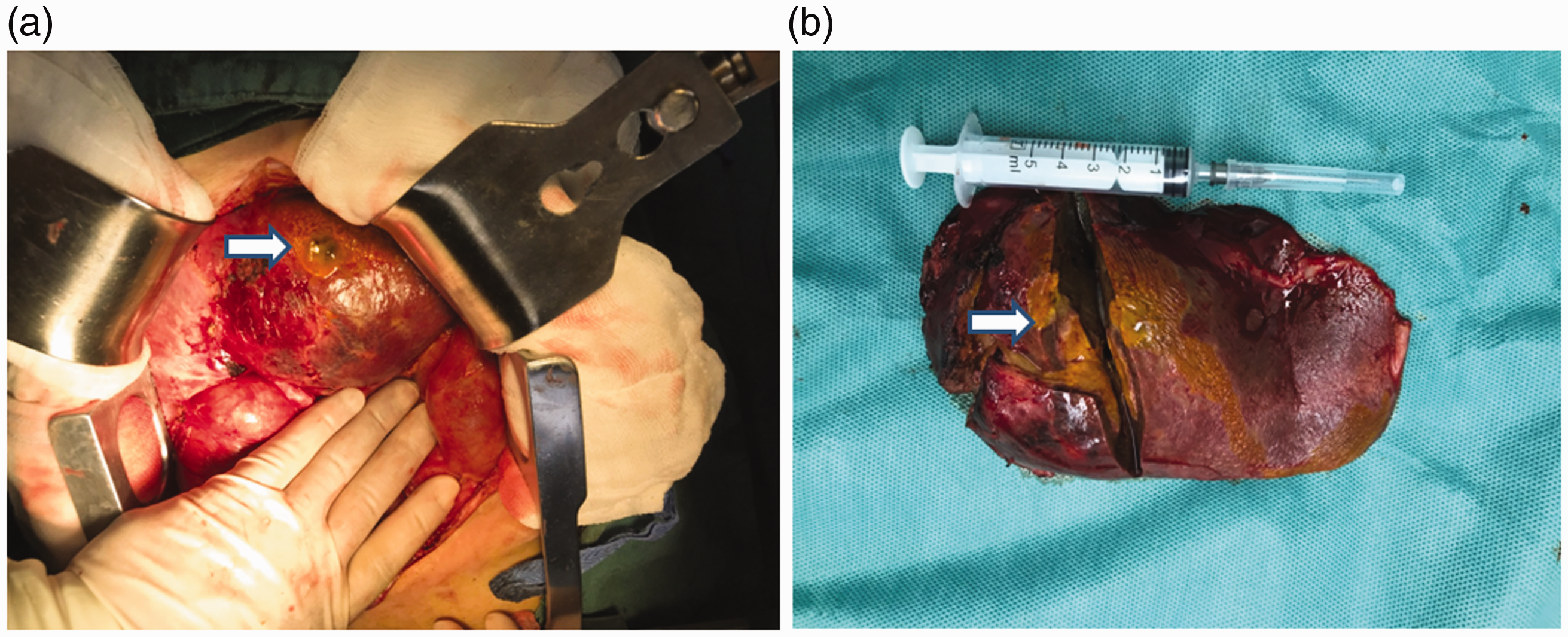
Following a deterioration in the patient’s symptoms, he underwent an emergency laparotomy, in which the abdominal cavity and pelvic cavity were found to contain approximately 800 ml of yellow turbid liquid and the left lateral section of the liver contained a tumour mass measuring approximately 4.5 cm × 4.0 cm with a soft texture (a). There was a gap with a diameter of approximately 1 cm on the tumour surface, with bile flowing out of the gap (the white arrow denotes the gap). Dissection of the excision specimens revealed that the gap was linked to the tumour mass and the tumour section was yellow with most of the tissues being necrotic (white arrow) (b). The colour version of this figure is available at: http://imr.sagepub.com.

A left hepatic lobectomy was performed and postoperative pathology revealed the occurrence of invasion/metastasis of differentiated adenocarcinoma in the left lateral section of the liver (a) and a large amount of coagulative necrosis in the left lateral section of the liver (b) (haematoxylin and eosin). Scale bar, 50 µm. The colour version of this figure is available at: http://imr.sagepub.com.
The Ethics Committee of Beilun District People's Hospital approved this study. The analysis was performed in accordance with the ethical standards of the hospital and the tenets of the Declaration of Helsinki/Declaration of Istanbul. The patient reported in this study provided written informed consent.
Discussion
This current case report describes a rare case of complications occurring after DEB-TACE, when the patient presented with progressively worsening upper abdominal pain. As conventional management methods for the suspected tumour rupture did not work, an emergency laparotomy was performed to remove the metastatic mass of differentiated hepatic adenocarcinoma.
The incidence of severe complications after TACE is 2.6–5.3%, including liver failure, hepatic encephalopathy, abscess formation, acute renal failure, bile duct injury, upper gastrointestinal bleeding, embolic cholecystitis, pulmonary embolism and hepatic artery spasm.3,5 Due to advances in technology and improvements in equipment, mortality associated with TACE treatment has declined from 4.1% to 0.5% over the past 20 years.6,7 The correct understanding and treatment of these complications have important practical implications for using TACE in a better manner to treat liver cancer.
Conventional TACE involves iodized oil as the embolic material with poor long-term embolization efficacy and significant systemic side-effects. 9 DEB-TACE is a novel drug-eluting embolization technique, which is characterized by its ability to allow permanent embolization of blood vessels, a slow continuous release of anti-tumour drugs in a locally targeted manner and reduction of side-effects caused by the systemic release of anti-tumour drugs. 9 At present, most physicians believe that the short- and long-term therapeutic efficacies of DEB-TACE are not significantly different from those of C-TACE, but the former method has a better safety and higher patient tolerance than the latter. 9 A series of small-sample studies reported an incidence of hepatic tumour rupture after C-TACE of approximately 4.0%,5,6,8 although the overall incidence of such ruptures is reported to be 0.1–1.5%. 3
Drug-eluting bead TACE has a high safety record when used to treat liver cancer and severe postoperative complications are rarely reported. 10 In particular, cases of diffuse biliary peritonitis secondary to postoperative rupture of hepatic tumour have not been reported. In this current case, after DEB-TACE, the patient felt dull pain and discomfort in the right upper abdominal region, indicative of post-TACE syndrome, but the patient’s dull pain in the right upper abdominal region persisted and gradually worsened. Abdominal CT revealed the presence of free gas in the abdominal cavity, indicative of tumour rupture. Therefore, when severe right upper abdominal dull pain appears after DEB-TACE, it should be differentiated from post-TACE syndrome. In particular, if the right upper abdominal pain after TACE first improves and then suddenly reappears or even worsens, it is highly indicative of the possibility of tumour rupture or bleeding. If necessary, CT or ultrasonography should be performed.
Tumour rupture after C-TACE in liver cancer patients may be related to the following factors:7,8,11 (i) tumour location – the tumour is located on the surface of the liver or is protruding outward; (ii) tumour diameter – the tumour is large and there is ischaemic necrosis inside the tumour with increased pressure; and (iii) embolization – iodized oil embolization is conducted at too large a dose. In this current case, the patient’s tumour was large and close to the surface of the left liver lobe, which increased the probability of post-TACE rupture.
Usually, liver tumour rupture presents with bleeding and not biliary leakage. However, the arterial embolization was performed successfully in the current case with the tumour-feeding vessels near the tumour being entirely embolized, so that even after the liver rupture, there was no intra-abdominal haemorrhage. The specific cause of bile leakage in this current patient remains unknown but does not exclude the possibility of rupture after the formation of bilioma. Bile ducts are fed exclusively by the hepatic artery and do not have a dual blood supply. 12 After arterial embolization, it is easy to cause severe ischaemia, necrosis and rupture of the peripheral bile duct, leading to bile leakage and accumulation in liver tissues, forming bilioma. CT and MRI scans might help to diagnose bile duct injuries by showing bile duct dilatation. 12 Although no peripheral bile duct dilatation was found on preoperative CT images for this patient, there was no specific imaging manifestation of small bile duct necrosis. Therefore, the possibility of bile peritonitis caused by rupture of bilioma after TACE still exists in this patient.
Based on the experiences of this case, the authors propose that in patients whose liver tumours are close to the lobe surface and are not encapsulated by normal liver tissues of a certain thickness, it is necessary to administer an optimum dose of the embolic agent to ensure adequate embolism. Alternatively, DEB-TACE can be performed for a second time to improve treatment efficacy, which may significantly reduce the risk of tumour rupture. In the event of rupture of hepatic tumours after DEB-TACE, conservative medical management is sufficient if there is only localized peritonitis, except in the case of active bleeding. If the inflammation is confined, abscess drainage may be considered. Given that the current patient developed diffuse peritonitis with obvious signs and symptoms, laparotomy was performed, and the left lateral section of the liver was removed.
In conclusion, this current case report describes an extremely rare case of diffuse biliary peritonitis secondary to rupture of a hepatic tumour after DEB-TACE. It is our opinion that although DEB-TACE is safe and rarely has serious complications, caution should be exercised when this method is used to treat tumours that are located close to the liver surface and the dose of the embolic agent should be controlled at an optimum level so as to ensure an appropriate degree of embolization. Alternatively, DEB-TACE may be performed for a second time to strengthen the therapeutic efficacy. In the event of diffuse biliary peritonitis secondary to postoperative rupture of hepatic tumours, emergency surgery is the preferred treatment.
Footnotes
Authors’ contributions
Lin-Bo Zhu drafted this manuscript. Tie-Feng Li, Jun-Qiang Li, Peng-Bin Zhang, Hua-Bin Wu and Rong Xv were involved in the acquisition of data and preparing the figures. Peng-Fei Li conceived of the study and revised the manuscript. All authors read and approved the final manuscript. All data and materials are freely available upon request. For further information, please contact Dr Peng-Fei Li (
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
The work was supported by grants from the Foundation for the Health and Family Planning Commission of Zhejiang Province, China (no.2018KY747) and the Medical Science and Technology Project of Ningbo, Zhejiang, China (no. 2016A05).
