Abstract
Appropriate hydration and skin surface pH are of fundamental importance in preventing areola skin barrier damage and breastfeeding success. We studied the dermal effects of emu oil on areola skin soon after birth in 70 at-term breastfeeding mothers by noninvasive bioengineering method. Emu oil–based cream was found to be effective in improving stratum corneum hydration of breast areolae (mean ± standard deviation, from 56.9 ± 18.2 to 65.0 ± 17.2 conventional units, P < .003) and did not affect skin pH, temperature, or elasticity. The significant improvement in hydration values was more pronounced in the puerperae presenting with basal hydration in the lower quartiles (mean ± standard deviation, from 41.6 ± 17.2 to 59.6 ± 21.2 conventional units, P < .001). Further studies are warranted to confirm the long-term beneficial effects of this preparation in a very sensitive patient population.
Introduction
The human female’s nipple-areola complex (NAC) is of particular interest in view of its crucial role in the natural progression of the birth to breastfeeding continuum. 1 In newborn mammals, the nipples provide access to colostrum and milk and is the source of thermal (V. Zanardo and G. Straface, 2014, unpublished data) and chemical 2 signals that appear to be specifically salient, facilitating early breastfeeding attempts and the probability of successful nipple grasping and feeding. 1,3
When newborns latch on to the breast, mothers often experience pain, which is caused by all or parts of the nipple being pulled into the baby’s mouth. 4 The first days after birth are often characterized by breast discomfort due to rough treatment of the tender area and other causes such as engorgement or dryness. Sore, cracked nipples are, in fact, a common problem early into breastfeeding, with an incidence ranging from 11% to 96%, and can be so severe as to lead to extreme nipple pain and premature weaning. 4,5
One of the most common causes of sore, damaged nipples is the infant’s poor attachment to the breast and this can usually be corrected if the suggestions of breastfeeding experts are followed. 6 Many women, however, delay seeking treatment until substantial damage has already occurred and this can delay the healing process. 7 The NAC is repeatedly exposed to the rough treatment and wet environment of the infant’s mouth; after feedings, mothers may not use the best technique to dry the nipple, and mother’s clothing between feedings may not permit air to circulate. In addition, traumatized nipples, exposed not only to maternal skin flora but also to the infant’s oral flora, readily become infected by bacteria or yeast infections, which can delay and impede healing. 8
The surface of the skin is covered with a protective acidic hydrolipid film with pH 4.5 to 5.5, which is an emulsion of substances dissolved in water, composed of sebaceous and sweat gland secretion and products of decomposed corneocytes, whose bactericidal and fungicidal properties are based on mild acidity. 9 –11 This emulsion also prevents evaporation of water from the surface of the skin, thus contributing to the maintenance of stratum corneum hydration. 12
Appropriate areola hydration is a key factor in preventing and treating sore, cracked nipples, mastitis, and breast abscesses secondary to skin barrier damage. 13,14 Emu oil is a commercially available product in various countries that possesses various beneficial activities such as anti-inflammatory, skin permeation enhancing, moisturizing and cosmetic properties, and has been used for the treatment of various ailments since decades. 15,16 Topical use of emu oil, containing high quantities of polyunsaturated fatty acids and antioxidants 15 seems to have potent anti-inflammatory effects. 16,17 Its mechanisms of action are, however, not entirely clear and have not, until now, been extensively studied. 18
Therefore, the aim of this investigation was to prospectively study the dermal effects of a new emu oil–based cream on areola skin hydration soon after birth in breastfeeding mothers. The study’s secondary aims were to test related physiological characteristics of areola skin, pH, temperature, and elasticity.
Methods
This prospective, open-label, controlled clinical trial was carried out from January 1 to February 28, 2014 at the Policlinico Abano Terme and was certified by the National Observatory on Women’s Health, an association dedicated to raising awareness on the importance of preventing and caring for illnesses afflicting women. The trial focused on the hydrating properties of an emu oil–based cream in 70 at-term, breastfeeding puerperae early after delivery. Institutional review board (Policlinico Abano Terme, Abano Terme, Italy) approval was obtained before the study began.
The commercial name of the product being examined is Clemulina Pus cream (Sitar Laboratories, Padua, Italy), which contains 30% of pure emu oil. 19 Emu oil preparations that contain high levels of omega-3 and omega-6 have been shown to possess a variety of beneficial features such as anti-inflammatory and antioxidant properties. 15 –17
The study’s eligibility criteria included being a healthy woman older than 18 years who spoke Italian, experienced a low-risk pregnancy, delivered a singleton infant who completed at least 37 weeks of gestation with no neonatal complications. Exclusion criteria were breast and/or nipple anomalies, chronic illness, and/or nipple dermatitis.
Women who fulfilled the eligibility criteria were approached in the maternity ward by a researcher and invited to take part in the trial. Those who agreed and signed consent forms were enrolled and received instructions. There was a postpartum washout period of 6 to 12 hours depending, respectively, if the delivery had been vaginal or caesarean section; baseline measurements were then taken. Participants who were prevalently right-handed were instructed to apply the cream on their left breast and nothing on the right one; those who were prevalently left-handed were instructed to apply the cream on their right breast and nothing on the left one. Thus each woman formed both part of the study and control population. All the women were instructed to wash their hands with warm water and soap prior to breastfeeding and to massage a few drops of the emu oil–based cream on the appropriate breast after each feeding; the participants were instructed to allow the NAC to air-dry naturally.
The study was carried out within the context of the hospital’s ordinary care protocol. In accordance with the hospital’s standard practice, following an uneventful delivery, infants are placed on the mother’s chest for about 15 minutes during which time the midwife assists with the first suckling episode. Infants are then dried, receive umbilical care, and are weighed before their first bath. During the subsequent 2 days in our ward, newborns room-in with their mothers, who are encouraged to demand-feed them (with no more than 3-hour interfeeding intervals). The infants receive complementary formula milk if breast milk intake is judged insufficient by the midwives. The definition of breastfeeding patterns used in this study were based on those outlined by the World Health Organization (exclusive breastfeeding was defined as feeding only maternal milk and nothing else; complementary breastfeeding was defined as offering breast milk and infant formulas; and exclusive formula feeding was defined as offering exclusively bottle-fed formula).
The areolae were assessed between feedings by a single physician (VZ) using noninvasive bioengineering methods. The Soft Plus 5.5 (Callegari SPA, Parma, Italy) corneometer, which measures electrical capacitance of the skin surface expressed in conventional units (c.u.), was used to assess hydration values (field, 0-100 c.u.; resolution, 1 c.u.; precision, ±5%; operating conditions—temperature 15°C to 35°C; maximum relative humidity, 80% [uncondensed]; the probe is placed onto a hairless area, making sure that the whole sensor is in contact with the skin). 20
Testing was performed at a fixed point, defined as areolar corresponding to the internal quadrant skin of both breasts, and included pH, temperature, and elasticity measurements, as previously reported (V. Zanardo and G. Straface, 2014, unpublished data).
The size of the sample population was calculated on the basis of a previous study that showed a mean areolar hydration of 57.9% (standard deviation [SD] = 19.3%) in breastfeeding mothers. To identify a 10% hydration difference with a power of 0.80 and type 1 error of 0.05, the minimum sample size was estimated at 57 puerperae for each group.
A descriptive analysis was used to construct a qualitative evaluation of clinical data. Continuous data were expressed as means and standard deviations or medians and interquartile ranges (IQRs). Categorical data were compared using Fisher’s exact test, while continuous data were compared using the Student’s t test. A P value less than .05 was considered significant. Statistical analysis was performed using R 2.12 software.
Results
In accordance with the population sample estimated (n = 57), a total of 70 women were enrolled in the study, 70% primiparae. The mean age of the mothers was approximately 33 years; about 22% underwent caesarean section, 60% of these were elective. All the mothers were breastfeeding exclusively at the time they were enrolled in the study. At discharge, most of the mothers were exclusively breastfeeding; only 3 (6%) were giving their infants some formula milk. Infants’ mean body weight at discharge was 5.9% inferior with respect to their mean birth weight. After testing, the mothers left the emu–oil based cream on their NAC.
Baseline and posttreatment areola skin hydration and dermatological characteristics are outlined in Table 1.
Baseline and Posttreatment Hydration and Related Dermatological Characteristics of Areolae in Early Postpartum Breastfeeding Women.a
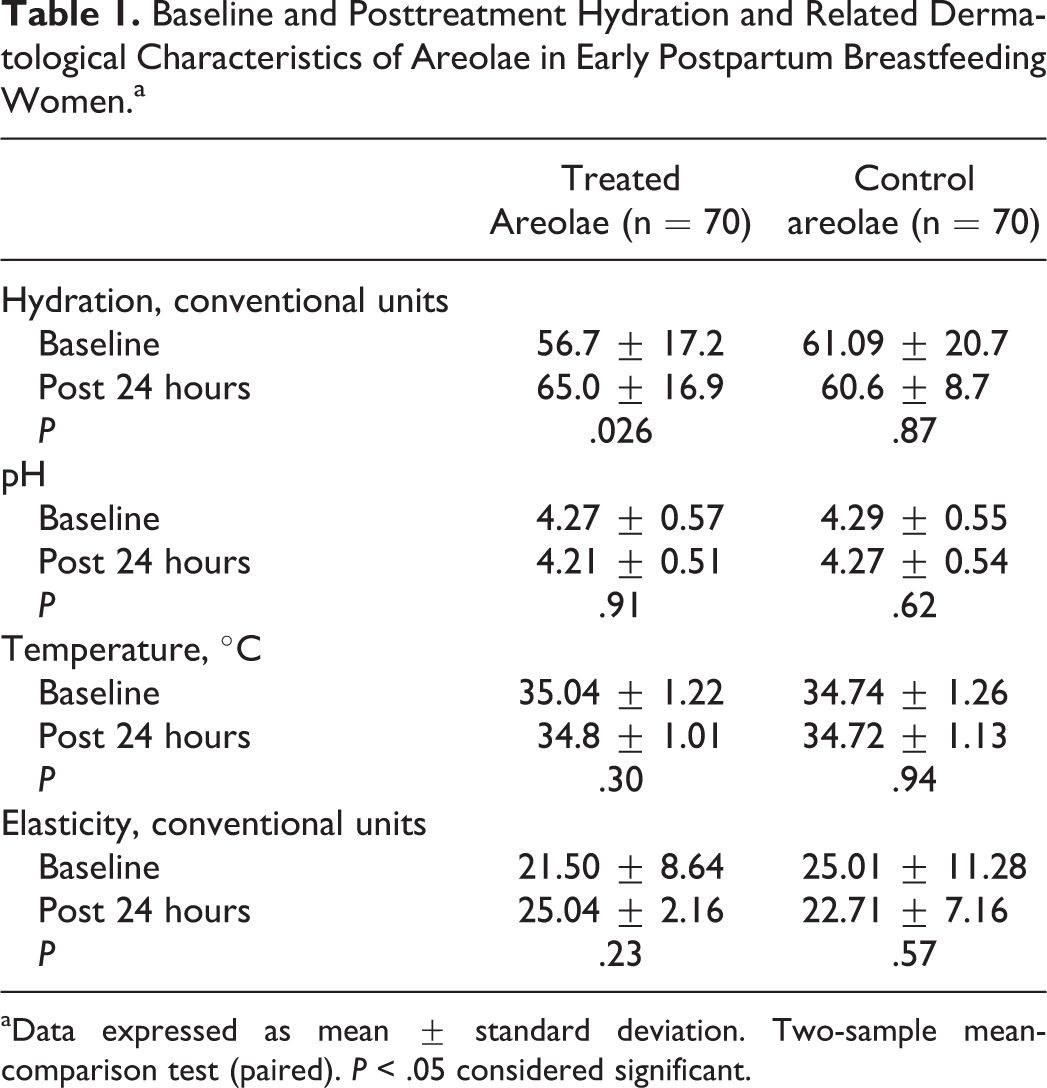
aData expressed as mean ± standard deviation. Two-sample mean-comparison test (paired). P < .05 considered significant.
The baseline median (IQR) hydration was 60.0 (44.8-73.0) c.u.; the values were normally distributed. Posttreatment hydration significantly increased (mean ± SD, from 56.7 ± 17.2 to 65.0 ± 16.9 c.u., P < .026). The significant improvement in hydration values was more pronounced in the puerperae presenting with basal hydration in the lower quartiles (mean ± SD, from 41.62 ± 17.2 to 59.6 ± 21.2 c.u., P < .001).
The posttreatment values of hydration vales were not correlated to areola skin pH (r = −0.08, P = .629).
Twenty-four hours after Emu oil application was first begun, the pH, temperature, and elasticity of the areolae of the mothers studied were unvaried.
Discussion
Nipple trauma associated with breastfeeding onset is commonplace and mothers cite it as one of the main reasons for painful, cracked, or bleeding nipples, and early cessation of breastfeeding. 4,5 Discomfort becomes particularly pronounced on the third postpartum day as breasts fill to the engorgement stage of lactogenesis. 21 Preventing and treating traumatized, sore nipples quickly and effectively is crucial to ensure that the bonding experience is a pleasant one and to encourage mothers to continue in the face of further complications and difficulties. 7,22
The results of this prospective open-label dermatologic trial found that 24 hours after emu oil–based cream applications (initiated shortly after delivery) were begun, there was an improvement in the level of stratum corneum hydration of the breast areolae; skin pH, temperature, and elasticity were, instead, unvaried. The marked improvement in hydration was more pronounced in the puerperae presenting with basal hydration in the lower quartiles.
A variety of interventions have been used to prevent or to treat nipple trauma and/or pain associated with breastfeeding. These include topical creams, solutions, or sprays, restricting the infant’s time at the breast, exposure of the nipples to dry heat or ultraviolet light and air-drying, hardening of the nipple skin, and pre- or postnatal breastfeeding education. 7 None of these measures appear to be particularly efficacious; nor have they been investigated scientifically.
It is well known that skin barrier function, which represents protection from water loss from the body, depends on several factors, including the level of hydration, the cellular properties of the corneocytes, the association and turnover of these cells in the stratum corneum, the amount and composition of intercellular lipids, and skin surface pH (a protective acid mantle). 11 Moreover, the water content of the stratum corneum and skin surface lipids form a balance that is very important for skin function and integrity. 23
Although no scientific studies have as yet been designed to investigate emu oil’s effect on breast hydration, topical treatments have been demonstrated to have potent anti-inflammatory activities and to lower proinflammatory cytokine levels in the tissue; this leads to improved wound healing and recovery of damaged skin. In an experimental animal model, Lagniel, Politis, and Dmytrowich demonstrated the anti-inflammatory properties of transdermal emu oil applications that were found to be as effective as orally administered ibuprofen. 24,25 In addition, emu oil contains variable levels of several compounds with antioxidant properties. 26
Although this study was originally designed to meet the methodological criteria of a prospective controlled trial, in the end we decided against using a randomized selection method. To facilitate the use of the cream, the women who prevalently used their right hand were instructed to apply the cream on their left breast (and nothing on the other); those who prevalently used their left hand were instructed to apply the cream on the right breast (and nothing on the other). Double blinding also proved difficult in this particular context. As a result, a single-blind design was used and data was collected and analyzed by “unblind” investigators. Another study limit was omission of information concerning the quantity of the cream used and therapy compliance.
In conclusion, despite the trial’s limits, prophylactic emu oil–based cream in early breastfeeding women is associated with hydration improvement. It could be recommended for prevention of nipple crack along with teaching better breastfeeding technique at the initiation of breastfeeding. Further long-term studies are warranted to confirm the beneficial effects on areola skin barrier of this preparation in a very sensitive patient population.
Footnotes
Author Contributions
VZ carried out the dermatologic study, DG participated in the design of the study, and GS performed the statistical analysis. LM conceived of the study, and participated in its design and coordination and helped to draft the manuscript. All authors read and approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
All tests were performed with ethical approval from the ethics committees of the Policlinico Abano Terme.
